Abstract
Introduction:
India’s tribal communities face significant public health issues, with tuberculosis (TB) being a major concern. These populations experience a higher TB burden due to limited healthcare access, socioeconomic inequalities, and distinct cultural practices. This study focuses on the prevalence and impact of TB among these communities.
Methods:
A comprehensive review of literature from databases such as PubMed, Scopus, ResearchGate, and Google Scholar was conducted to analyze the health challenges, particularly TB, affecting India’s tribal populations.
Results:
The review highlights a significant disparity in TB prevalence between tribal and non-tribal populations. Factors like inadequate healthcare infrastructure, limited medical access, and socioeconomic inequalities, along with cultural practices, complicate TB transmission and treatment, emphasizing the need for culturally tailored interventions.
Conclusion:
Addressing the TB crisis in India’s tribal communities requires a holistic and culturally sensitive approach. Collaborative efforts among healthcare providers, policymakers, and tribal communities are crucial to improving health outcomes and preserving cultural heritage for a sustainable future.
Keywords
Introduction
India’s tribal population, often called Adivasis, represents a vital and integral component of the nation’s prosperous cultural heritage.[1] These indigenous communities constitute a tapestry of ethnic, linguistic, and cultural groups that have inhabited the Indian subcontinent for centuries, forming a diverse and vibrant mosaic within the country.[2] Their unique customs, traditions, and belief systems are woven into the very fabric of India’s profound cultural diversity, adding depth and colour to the nation’s identity.[1] On the other hand, the intricate examination of the Indian tribal population’s characteristics in the context of health issues, particularly tuberculosis (TB), offers valuable insights into the socio-cultural and economic challenges they face. This analysis serves as a valuable model for studying population health, not only in relation to TB but also for understanding various other chronic conditions like diabetes, mental health disorders, and even rare genetic ailments.
As of the 2011 census, India’s tribal population exceeded 104 million, constituting 8.6% of the country’s total population—an increase from 8.2% in the 2001 census.[3,4] This tribal population comprises 705 distinct ethnic groups spread across India’s 30 states and union territories, each with unique cultural and living practices.[5] Predominantly residing in rural and remote areas, tribal people represent one of the most disadvantaged and neglected segments of society, facing disparities in various social, health and developmental indicators. Their access to healthcare delivery networks is notably limited.[2-3,6]
Despite their significant contributions to India’s cultural landscape, tribal populations confront a range of substantial public health challenges that not only imperil their well-being but also undermine the preservation of their way of life.[2]
Throughout history, tribal populations have confronted numerous health challenges, including issues related to infant and maternal mortality, malnutrition, anaemia, malaria and other communicable diseases; however, ‘Tuberculosis’, a pressing and alarming health concern, significantly affects tribal communities in India, with over 1.9 million new cases reported annually, constituting the highest TB burden in the country[3] and population health in chronic illnesses, encompassing prevalent conditions such as diabetes mellitus and mental health disorders, along with rare or uncommon genetic and inherited conditions.
India accounts for one-fifth of all new TB cases globally, with two-thirds occurring in Southeast Asia.[3,7] The gravity of the situation becomes evident when considering that the prevalence of TB in these communities is estimated to be a staggering 703 cases per 100,000 population.[3] This prevalence rate is substantially higher than the national average, which stands at 256 cases per 100,000 population, as the World Health Organization reported in 2022.[4]
This elevated incidence of TB in tribal communities can be attributed to a complex interplay of multiple factors. These factors encompass limited healthcare access, inadequate healthcare infrastructure, stark socioeconomic disparities, and the influence of unique cultural practices and belief systems within these communities.[1]
For instance, language barriers and cultural differences pose formidable obstacles for tribal attempting to access and comprehend TB care services.[5] These challenges can lead to miscommunication, misdiagnosis and delayed treatment, exacerbating the TB crisis in these communities. Furthermore, traditional healing practices, deeply rooted in tribal cultures, may inadvertently delay or even deter individuals from seeking essential medical care, particularly for diseases as debilitating as TB.[1]
In light of these intricate dynamics, addressing TB within India’s tribal communities demands a multifaceted and culturally sensitive approach that not only targets the disease but also acknowledges and respects the unique identities and practices of these indigenous groups.[1] However, addressing TB in tribal communities requires a multi-pronged approach that includes:
Therefore, this present study aims to comprehensively examine the public health challenges confronting India’s tribal communities, with exclusive attention to the pervasive issue of TB.[3] By examining these dimensions and adopting a multifaceted approach, this study aims to raise awareness and inspire concrete actions and policies that address the critical health challenges faced by India’s tribal communities. The ultimate goal is to contribute to a healthier, more sustainable future for these indigenous groups, preserving their cultural richness while mitigating public health disparities, with TB at the forefront of this endeavour.[1]
Tribal Populations and their Substantial Numbers and Diverse Culture
Tribal populations in India are indeed substantial, constituting a significant portion of the country’s total population.[6] According to the 2022 Annual Report of the Ministry of Tribal Affairs, Government of India, there are over 700 tribal communities in India, accounting for 8.6% of the country’s total population.[7] This translates to over 104 million tribal people in India, making it one of the largest indigenous populations globally.[8]
Distributed across various regions of India, tribal populations have a significant presence in states like Jharkhand, Chhattisgarh, Odisha and the northeastern states, contributing to the country’s cultural diversity. Each community boasts its languages, traditions and ways of life.[9] India hosts the world’s second-largest concentration of tribal people, comprising about 8.3% of the population. The current survey identifies 635 tribes distributed across five major tribal belts, residing in hilly and plain forest regions. Mizoram, Lakshadweep, Meghalaya and Nagaland have the highest tribal settlements, with percentages ranging from 86.1% to 94.4%. Noteworthy tribal populations exist in states like Madhya Pradesh, Orissa, Maharashtra, Rajasthan, Chhattisgarh, Assam and West Bengal.
Prominent Indian tribes include the Gonds, Bhils (or Bheels), Santhal, Munda, Khasi, Garo, Angami, Bhutia, Chenchu, Kodaba and the Great Andamanese Tribes. The Bhil tribal group, according to the 2011 census, stands as India’s most significant, accounting for over a third of the country’s total scheduled tribal population. However, tribal populations are sparse in certain regions, including Haryana, Punjab, Chandigarh, Delhi, Goa and Puducherry. The remaining states and union territories exhibit substantial tribal populations, with Madhya Pradesh being the state with the highest number of tribes, categorised into four zones based on their geographical distribution (Table 1):
The tribal groups mentioned are based on the regions they primarily inhabit
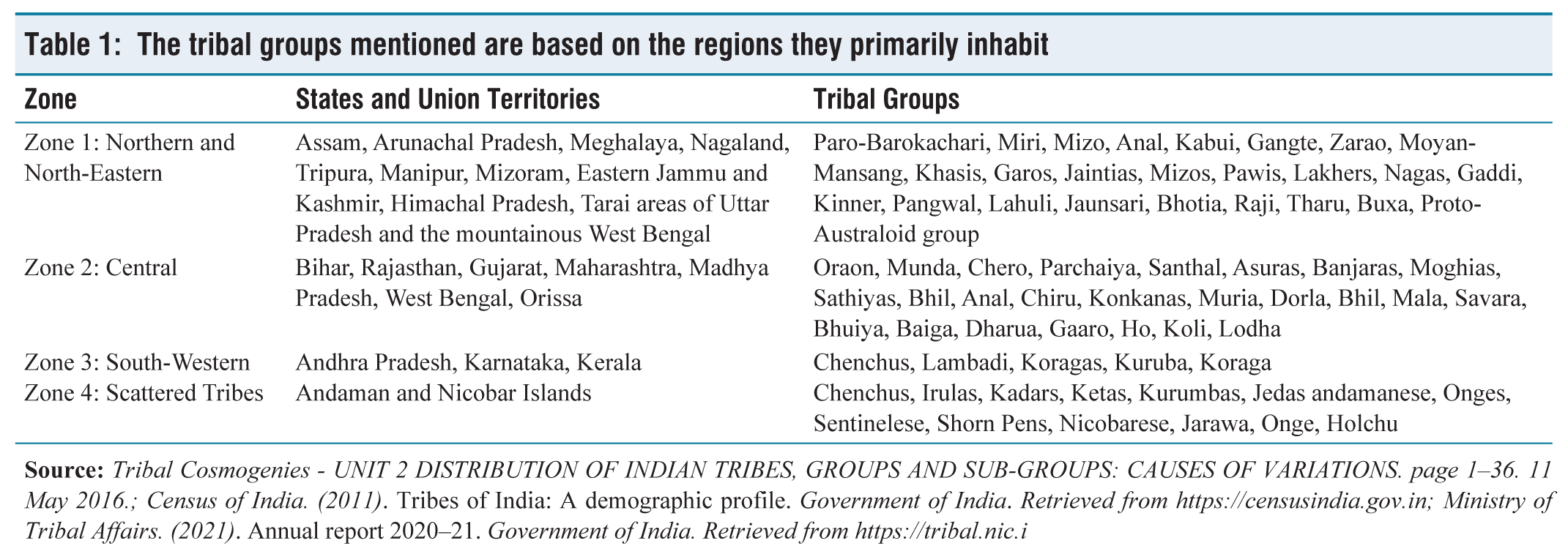
Zone 1: Northern and North-Eastern.
Zone 2: Central.
Zone 3: South-Western.
Zone 4: Scattered Tribes of Andaman and Nicobar.
The substantial number of tribal populations in India makes it crucial to address their unique public health challenges, which can significantly impact the nation’s overall health landscape. For example, tribal populations are more likely to experience poverty, malnutrition and infectious diseases.[10] They also face barriers to accessing healthcare services and education.
To improve the health and well-being of tribal populations in India, it is essential to develop and implement culturally sensitive and appropriate public health interventions. This includes addressing the social determinants of health, such as poverty and education, and ensuring that tribal communities have access to quality healthcare.[6]
Importance of the TB Emergency in Tribal Communities
The prevalence of TB within India’s tribal communities is a crisis that demands immediate attention. The TB crisis in tribal communities not only poses a severe threat to the health of individuals but also hampers the overall well-being of these populations. The disease can lead to economic hardships, loss of productivity, and social stigma, further emphasising the urgent need for interventions. This part of the study underscores the gravity of the TB problem within these populations and its far-reaching implications.
Elevated Prevalence
TB is a pervasive issue among tribal communities, with significantly higher prevalence rates compared to the national average.[3] According to the Tribal TB Initiative by the Ministry of Tribal Affairs, Government of India (2021), the prevalence of TB in these communities stands at a staggering 703 cases per 100,000 population, in stark contrast to the national average of 256 cases per 100,000 population, as reported by the World Health Organization in 2022.[4] These figures vividly illustrate the extent of the TB crisis.
Complex Factors
The high prevalence of TB within tribal communities can be attributed to a complex interplay of multiple factors.[1] Limited healthcare access, inadequate healthcare infrastructure, socioeconomic disparities, and the influence of unique cultural practices and belief systems are some of the critical factors that contribute to the TB crisis.
Healthcare Access Barriers
Language barriers and cultural differences further exacerbate the TB problem by making it challenging for tribal individuals to access and understand TB care services.[5] These obstacles can result in miscommunication, misdiagnosis and delayed treatment, thereby compounding the TB crisis.
Cultural Practices
Traditional healing practices deeply rooted in tribal cultures can inadvertently deter individuals from seeking essential medical care, especially for diseases as debilitating as TB.[1] The persistence of such practices can delay diagnosis and treatment, contributing to the high TB prevalence.
However, addressing the TB crisis in tribal communities requires a multi-pronged approach that includes improving healthcare access and infrastructure, addressing socioeconomic determinants of health, promoting culturally sensitive interventions, and engaging tribal communities in the decision-making process. Additionally, raising awareness, reducing stigma, and building healthcare capacity within tribal areas are essential components of any effective strategy to combat the TB crisis. Recognising the unique challenges tribal communities face and tailoring interventions to their specific needs.[1]
Understanding Health Challenges: Poverty and Malnutrition Among Tribal Population
Poverty and malnutrition are two of the biggest challenges faced by tribal populations in India. Tribal communities are disproportionately affected by poverty, with an estimated 47% of tribal people living below the poverty line—significantly higher than the national average of 22%.[1] Malnutrition is also a severe problem among tribal populations, with 43% of tribal children under five being stunted and 20% wasted, compared to 36% and 15% of non-tribal children, respectively.[2] Stunted and wasted children are more likely to experience a range of health problems, both in the short-term and long-term. Stunting can lead to cognitive impairment, reduced physical capacity, and an increased risk of chronic diseases in adulthood.[3] Wasting can lead to weakened immunity and an increased risk of death.[4]
Tribal populations are more likely to contract communicable diseases such as malaria, TB and diarrhoea. This is due to poor sanitation and hygiene and limited access to clean water.[1] For example, a 2020 study by the Indian Council of Medical Research found that the prevalence of malaria among tribal populations is 2.5 times higher than the general population.[5]
Several factors contribute to poverty and malnutrition among tribal populations in India, including limited access to land and other natural resources, lack of education and employment opportunities, and social discrimination and exclusion.[1] The consequences of poverty and malnutrition for tribal populations are severe, with malnourished children more likely to experience health problems, leading to poor academic performance and reduced productivity as adults, thus perpetuating the cycle of poverty and malnutrition.[3]
Implementation
Several measures can be taken to address poverty and malnutrition among tribal populations in India. These include improving access to land and other natural resources, investing in education and employment opportunities, and addressing social discrimination and exclusion.[1] Additionally, ensuring access to quality healthcare and nutrition services is crucial. This involves providing tribal villages with healthcare facilities’ trained personnel and implementing nutrition programmes to address malnutrition among tribal children and women.[1] By addressing these challenges, India can make significant progress towards achieving its sustainable development goals (SDGs), including goals to end poverty and hunger and ensure healthy lives and well-being for all.
Challenges in Healthcare Access for Tribal Communities
The health challenges encountered by these indigenous groups, such as Adivasi communities in India, are complex and often intertwined with their unique cultural, social and geographical circumstances.[6] One of the most significant challenges is limited access to healthcare services, exacerbated by residing in remote, hilly, or forested areas far from urban centres with medical facilities.[7] Geographical isolation contributes to delayed or inadequate medical attention, further intensified by a shortage of healthcare infrastructure, including hospitals, clinics and trained professionals.[7]
The most pressing health challenge tribal communities faces in India is the substantial lack of access to quality healthcare.[7] Living in remote and underserviced areas, tribal populations encounter formidable barriers that hinder their ability to reach medical facilities, resulting in limited access to essential healthcare services. This issue particularly impacts the timely diagnosis and treatment of diseases, with TB being a significant concern.
Tribal communities often reside in remote areas with restricted access to healthcare facilities and a scarcity of trained healthcare personnel. This geographical isolation and healthcare scarcity exacerbate their healthcare access challenges, particularly in the context of chronic diseases.
Reported Data from the Ministry of Tribal Affairs, Government of India (2022), underscores the gravity of the situation. It reveals that only 38% of tribal villages have sub-centres, which serve as the most basic form of healthcare facilities, in contrast to 68% in non-tribal villages. Furthermore, only 28% of tribal villages have primary health centres, in contrast to 52% in non-tribal areas.[7] An acute shortage of trained healthcare professionals further compounds the deficiency of healthcare infrastructure in tribal regions. Research by the National Tribal Commission (2021) underscores this issue, indicating a lack of doctors, nurses and other vital healthcare workers in tribal areas. This shortage is attributed to numerous factors, including challenging working conditions and a lack of incentives for healthcare professionals to serve in remote areas.
Consequently, limited healthcare access translates into higher rates of morbidity and mortality among tribal populations compared to their non-tribal counterparts. For instance, the maternal mortality rate among tribal women is 2.5 times higher than the national average, as reported by the Ministry of Tribal Affairs, Government of India (2022). Additionally, tribal children are more vulnerable to preventable diseases like diarrhoea and malaria, according to the National Tribal Commission (2021).
The consequences of limited healthcare access extend beyond health outcomes alone. They significantly affect the productivity and overall well-being of tribal communities. Illness prevents community members from engaging in gainful activities, resulting in decreased household income and a lower quality of life. The pressing need to address these healthcare access challenges for tribal populations is evident, as it has profound implications for health and socioeconomic development in these communities.
Implementation
Several things can be done to improve access to healthcare for tribal populations in India. These include: (a) Increasing the number of healthcare facilities in tribal areas could involve building new healthcare facilities and upgrading existing facilities.[1] (b) Recruiting and training more healthcare workers to work in tribal areas: This could involve incentives for healthcare workers to work in remote areas and offering specialised training programmes for healthcare workers who want to work with tribal populations.[1] (c) Making healthcare more affordable for tribal populations: This could involve providing subsidies for healthcare services and offering free or low-cost health insurance to tribal people.[1] (d) Improving transportation and communication networks in tribal areas: This would make it easier for tribal people to reach healthcare facilities and communicate with healthcare providers.[1] In addition to these strategies, it is imperative to tackle the social determinants of health that profoundly influence the well-being of tribal populations, encompassing factors such as poverty, education and sanitation.[1] These determinants play a pivotal role in shaping health outcomes and must be addressed comprehensively to effect lasting improvements in the health of tribal communities. By enhancing healthcare accessibility and addressing the socioeconomic determinants of health, India can take substantial strides toward realising its SDGs. These SDGs encompass vital objectives to ensure healthy lives and well-being for all, as set forth by the United Nations.[2] This synergy between improved healthcare access and broader development goals underscores the potential for positive and transformative change in the health and quality of life for tribal populations in India.
Socioeconomic Disparities and Their Impact on TB in Tribal Communities
Tribal communities in India confront significant socioeconomic disparities that are intrinsically connected to the elevated prevalence and severity of TB within these populations. These disparities are the outcome of a multifaceted interplay of historical, geographical and socioeconomic factors, establishing them as a pivotal element in the TB crisis among tribal groups. Tribal populations frequently contend with heightened poverty levels and lower literacy rates, factors that amplify existing health disparities.[6] These socioeconomic determinants contribute to malnutrition and compromised immune systems, intensifying the vulnerability to diseases, including TB. As such, addressing the TB crisis in tribal communities necessitates not only targeted healthcare interventions but also comprehensive efforts to uplift socioeconomic well-being, ultimately mitigating the impact of socioeconomic disparities on health outcomes within these populations.
Cultural Practices and Beliefs
In tribal communities in India, cultural practices, beliefs and traditions wield a considerable influence on the dynamics of TB, both in terms of transmission and management. As highlighted by Gupta et al. in their 2023 study,[6] these cultural elements contribute to the complexities of the TB crisis in these populations in the following ways:
Communal Living Arrangements
Many tribal communities practice communal living arrangements, where extended families or multiple households share living spaces. While these practices foster strong social bonds, they can inadvertently facilitate the transmission of infectious diseases like TB. The proximity within these communal settings can expedite the spread of the bacteria, posing a significant challenge in disease containment.[6]
Traditional Healing Practices
Within tribal cultures, traditional healing practices hold deep-rooted significance. These practices often involve using herbs, rituals and spiritual beliefs to address health issues. While these customs are integral to tribal identity, they may inadvertently delay or even deter individuals from seeking timely medical treatment, particularly for diseases as debilitating as TB.[6] Such delays in seeking appropriate medical care can lead to the progression of the disease and contribute to its persistence within tribal communities.
Challenges of TB Control in Tribal Communities
Tribal communities in India face several challenges in the prevention and control of TB, including (a) Language and communication barriers. Healthcare providers and tribal communities may speak different languages, which can hinder effective communication and the understanding of health information. This can lead to misdiagnosis, non-compliance with treatment, and a lack of awareness about TB.[6] (b) High prevalence of TB: TB is a significant public health concern within tribal communities, with a prevalence rate that is often higher than in non-tribal areas. This is partly due to the abovementioned factors, such as crowded living conditions, malnutrition, and limited access to healthcare.[7,9] (c) Stigma and discrimination: Stigma associated with TB can be particularly harmful in tribal communities, where it may lead to delayed diagnosis and treatment. Fear of social isolation and discrimination can discourage individuals from seeking the care they need.[6,10] (d) Healthcare infrastructure: Inadequate healthcare infrastructure in tribal areas, including a shortage of healthcare workers and facilities, poses a significant challenge in diagnosing and treating TB effectively.[8,11,12] (e) Lack of awareness and education: Limited access to education and health awareness programmes in tribal areas results in a lack of knowledge about TB, its transmission, and prevention measures.[6,13,14] Cultural factors such as traditional healing practices and communal living arrangements can also influence TB control efforts in tribal communities.[8,9,15,17] In addition, implementing holistic methods is essential for addressing the health challenges of tribal communities effectively. This involves cultural sensitivity, community engagement, interdisciplinary collaboration, empowerment, improved healthcare access, socioeconomic development, and environmental sustainability. By adopting these approaches, stakeholders can create sustainable solutions tailored to the specific needs of tribal populations.
Addressing TB in Tribal Communities
Given these challenges, addressing TB in tribal communities requires a multifaceted approach. It should involve improving healthcare access and infrastructure and promoting culturally sensitive interventions, community engagement, and awareness campaigns tailored to the unique needs and perspectives of these indigenous populations.
Some specific measures that can be taken include:
Improving access to healthcare services: This could involve building new healthcare facilities in tribal areas, recruiting more healthcare workers, and providing transportation and financial assistance to help tribal people reach healthcare facilities.[16] Promoting culturally sensitive interventions: This could involve developing TB prevention and control programmes that are tailored to the cultural needs and beliefs of tribal communities. For example, it is essential to involve tribal leaders and traditional healers in these programmes.[7-10] Encouraging community engagement: Tribal communities should be actively involved in the planning and implementing TB prevention and control programmes. This helps to ensure that the programmes are responsive to the community’s needs and more likely to be successful.[8,11,14] Raising awareness and education: TB awareness and education campaigns should be conducted in tribal communities in local languages. These campaigns should focus on the signs and symptoms of TB, the importance of early diagnosis and treatment, and ways to prevent the spread of the disease.[13-18] By addressing the challenges of TB control in tribal communities, India can make significant progress towards achieving its goal of ending TB by 2025.
Conclusion
The health challenges faced by tribal communities in India, with a particular emphasis on TB, are both pressing and intricate. These challenges, deeply rooted in socioeconomic disparities, limited healthcare access, and cultural practices, have significant implications for the well-being of tribal populations. The high prevalence of TB within these communities, far exceeding national averages, calls for immediate attention and multifaceted interventions.
To address these challenges effectively, a holistic approach is paramount. This approach must include improving healthcare access and infrastructure, addressing socioeconomic determinants of health, promoting culturally sensitive interventions, and actively engaging tribal communities in healthcare decision-making. Moreover, it requires a concerted effort to build healthcare capacity and establish robust monitoring systems to measure progress accurately.
Recognising the cultural diversity and unique identities of tribal populations is integral to any successful intervention. While modern healthcare solutions are essential, they must be harmonised with traditional practices and beliefs to respect the cultural heritage of these communities.
Ultimately, the aim is to reduce the prevalence of TB in tribal communities, bridging the gap with national averages while concurrently preserving their rich cultural diversity. The overarching objective is to alleviate the TB burden and foster a healthier, more sustainable future for India’s tribal populations. This endeavour underscores the importance of a comprehensive strategy that considers the complexities of these communities’ lives and health challenges, striving for a future where health disparities no longer cast shadows over the unique cultural identities of India’s tribal populations.
Future Aspects
As we consider the future of addressing health challenges, particularly TB, in India’s tribal communities, several vital aspects come into focus:
In the coming years, concerted efforts should be made to ensure that TB, along with broader health issues, no longer cast shadows over the unique cultural identities of India’s tribal communities. The future promises healthier and more sustainable lives for these indigenous groups, guided by multifaceted strategies and a deep respect for their cultural richness.
Footnotes
Acknowledgements
The acknowledgements for this study are extended to those who have previously contributed to and conducted research on the same topic. This recognition acknowledges the existing body of work and the collective efforts of researchers in the field. The author expresses gratitude to those who contributed to the development and execution of this research, acknowledging their invaluable support and collaboration. AI plagiarism detection tools were employed to ensure the authenticity of the acknowledgements and avoid any instances of plagiarism.
Consent for publication
The article adheres to ethical principles rooted in the Declaration of Helsinki.
Declaration of conflicting interests
The author declared no potential conflicts of interest with respect to the research, authorship and/or publication of this article.
Funding
The author received no financial support for the research, authorship and/or publication of this article.
Institutional ethical committee approval number
Given that this is a literature-based study, it is important to note that strict adherence to ethical principles and guidelines was not required. The research primarily involved the examination of existing literature and did not directly involve human subjects.
Credit author statement
RK contributed to the conception, literature search, and manuscript drafting.
Data availability
Rinki Kumari, the author, maintains a commitment to transparency in presenting data in this literature-based study. All information and findings shared in this work are authentic and accurately represent the research conducted. Any potential conflicts of interest have been meticulously disclosed to ensure transparency.
Use of Artificial Intelligence
Artificial intelligence was not used.
