Abstract

Dear Editor:
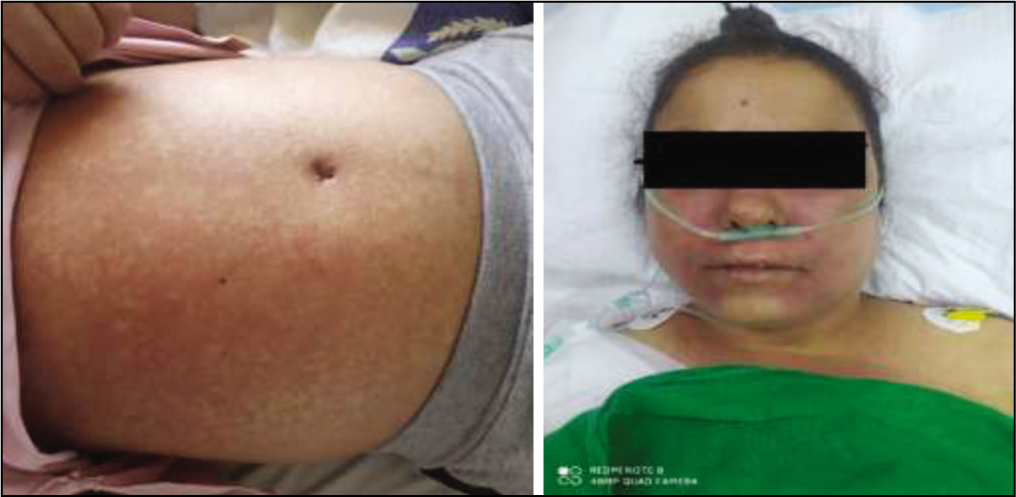
Drug Reaction with Eosinophilia and Systemic Symptoms (DRESS) is a rare severe drug reaction that can be life-threatening. Acute visceral involvement is well documented, but little is known about long-term complications. 1 Autoimmune diseases have been documented to occur rarely months or years after recovery from DRESS such as type one diabetes, alopecia areata, thyroid disease, rheumatoid arthritis, systemic lupus erythematosus and scleroderma A thyroid diseases. 2 Here, we documented a case of surprising multiple delayed autoimmune complications in a patient with DRESS syndrome. A-35-year-old female with a past diagnosis of nonspecific arthritis on sulfasalazine, presented to the emergency department with a fever, facial oedema, generalised macular rash on the face, trunk and extremities (Figure 1), jaundice and abdominal pain of a two-week duration. Laboratory tests showed leucocytosis, anaemia, Eosinophilia, elevated liver enzymes with marked elevation of c reactive protein (CRP) and erythrocyte sedimentation rate (ESR) (ANA, anti-DNAds, anti-RO, anti-LA, anti-ccp, and RF) were negative. Diagnosis of DRESS syndrome was made, and the patient was started on intravenous methylprednisolone 1 g/day for three days, followed by oral prednisolone 60 mg/day and cyclosporine with significant improvement. During follow-up, seven months after recovery of DRESS syndrome, the patient suffered from painful grouped herpetiform vesicles on an erythematous base on the left side of the chest. The rash is associated with a mild fever (38 c), tiredness, and headache. She was diagnosed with herpes zoster. Three months later, the patient suffered from alopecia areata with generalised hypopigmentation on the face and trunk consistent with vitiligo universalis (Figure 2). Two months later, during usual monitoring for thyroid function, thyroid stimulating hormone (TSH) was 0.04, {normal: 0.35–5.1 (mIU/L)}. further investigation demonstrated elevated Anti-TPO 520,09 (reference range: 0–9 IU/l), normal T3: 2.58 (reference range 2–7 pmol/L), normal FT4: 0.96 (reference range 0.5–1.4 ng/dL), these findings suggested the diagnosis of subclinical hyperthyroidism.
A 30-year-old Syrian Woman with DRESS Syndrome Showing Generalised Macular Rash on the Face, Trunk and Extremities.
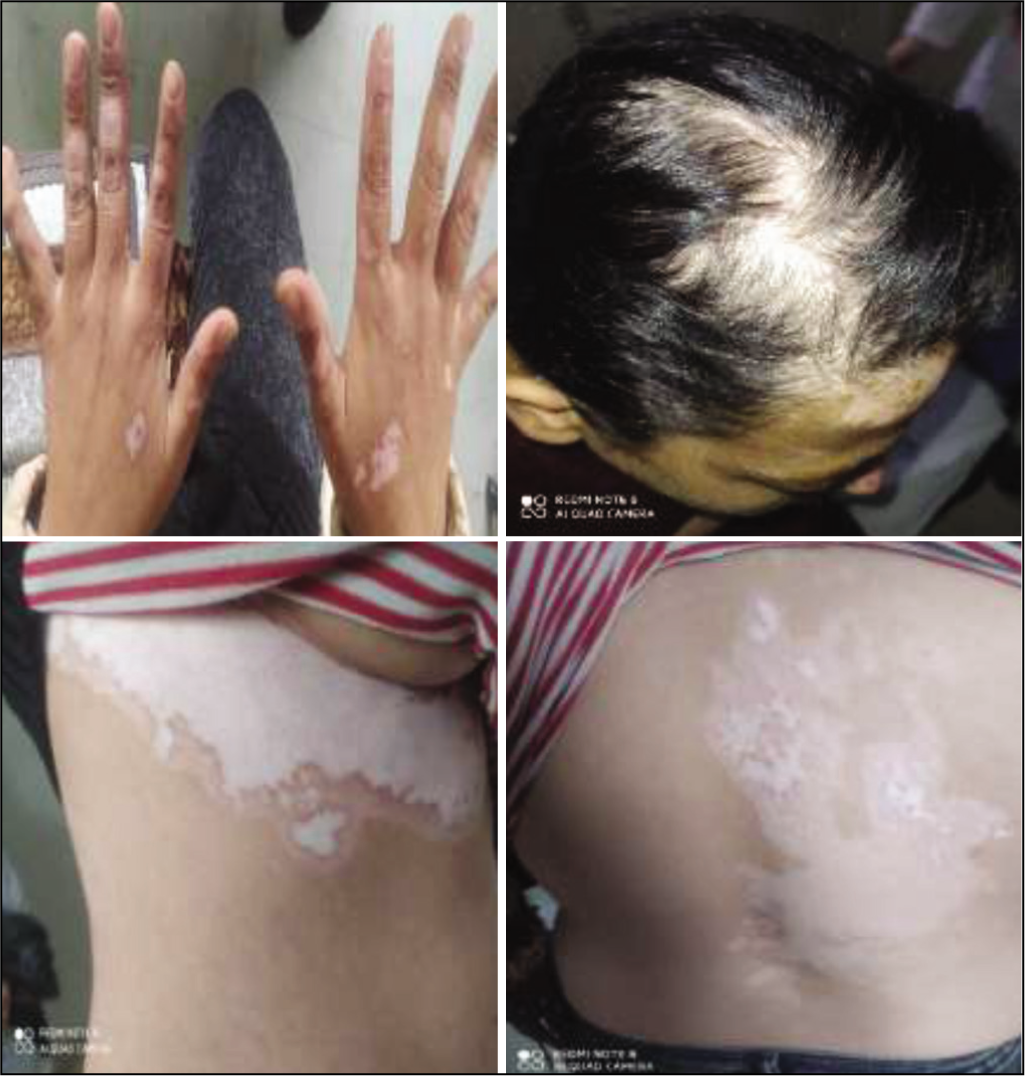
A 30-year-old-Syrian Woman with DRESS Syndrome Showing Generalised Vitiligo on the Trunk and Hands with Alopecia.
During the patient’s last visit to our rheumatology department, she complained of dry eyes and mouth with symmetric polyarthritis. Blood tests revealed leukopenia (3000 per microliter), lymphopenia (900 /ref: 1100–3700 per microliter), elevated ESR (111 mm/h) and CRP (54 g/d), rheumatoid factor was positive, while anti-citrullinated peptide (Anti-CCP) was negative. ANA was positive (1/640), anti-DNAds was positive (1/320), anti-RO(SSA) and anti-LA(SSB) were positive, and optic examination revealed dry eyes (Schirmer test was 3 mm (normal >5 mm)). Hence, the patient was diagnosed with SLE and secondary Sjogren syndrome. The mechanism of the development of these autoimmune complications is not well understood, with the possibility of a herpes virus role, genetic susceptibility, and the functional defect of Treg cells. in summary, long-term delayed autoimmune complications may be overlooked because of the long asymptomatic period after the resolution of the acute phase. Therefore, rheumatologists and dermatologists should be aware and vigilant for any suggestive manifestations during follow-up.
Footnotes
Author Contributions
All the authors contributed equally in writing, reviewing the manuscript and literature review.
Availability of Supporting Data
Data and materials are available in the Department of Rheumatology and immunology – Tishreen hospital, Damascus, Syria.
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship and/or publication of this article.
Ethical Approval
Ethical permission was not applicable for this article, as this is a review article drafted from various research articles and not from patients directly.
Funding
The authors received no financial support for the research, authorship and/or publication of this article.
Patient Consent
Written informed consent was obtained from the patient for publication of this case report and accompanying images. A copy of the written consent is available for review by Editor in-Chief of this journal.
