Abstract
Background
Liquiritin, a flavonoid present in the traditional Chinese medicine Radix Glycyrrhizae, reduces myocardial damage and improves cardiac function. However, it remains unclear what effect it has on the thoracic aortic rings.
Objectives
Use of rat thoracic aortic rings to study the vasodilatory effects of liquiritin and its associated mechanisms.
Materials and Methods
The arterial tension of rat thoracic aortic rings was measured in vitro using the perfusion method. Precontraction of the thoracic aortic rings with phenylephrine (PE) 1 µM and changes in vascular ring tension were observed and recorded after cumulative administration of liquiritin (1, 3, 10, 30, 100, and 300 µM). The effects of liquiritin on the tension of thoracic aortic rings with intact or denuded endothelial that were precontracted with PE or potassium chloride were determined, as well as how NG-nitro-
Results
Liquiritin exerts a diastolic effect on PE-induced contraction of the thoracic aortic ring, and this effect is independent of the integrity of the vascular endothelium. L-NAME and INDO pretreatment also did not influence the vasodilatory function of liquiritin, illustrating that it might not be endothelium-dependent. Furthermore, pretreatment with TEA, a Ca2+-activated K+ channel inhibitor, and BaCl2, an inwardly rectifying K+ channel inhibitor, did not affect the vasodilatory effects of liquiritin. Nevertheless, pretreatment with the voltage-dependent K+ (Kv) channel inhibitor, 4-AP, and the ATP-sensitive K+ (KATP) channel inhibitor, Gli, significantly reduced the vasodilatory effect of liquiritin, indicating that the vasodilatory effects of liquiritin may have a bearing on the activation of Kv and KATP channels.
Conclusion
Overall, we confirmed for the first time that liquiritin has vasodilatory effects that are endothelium-independent, and the mechanism of its vasodilatory effect may include activation of Kv and KATP channels.
Keywords
Introduction
Hypertension is a cardiovascular disease that seriously endangers human health, with the main manifestation being increased arterial pressure in the body (Ito et al., 2022; Schiffrin, 2020). Long-term surges in blood pressure can affect the functions of the heart, brain, kidneys, and other important organs, posing a serious threat to human health (Arguedas et al., 2020; Di Palo & Barone, 2022). Studies have shown that lowering blood pressure and controlling its stability can effectively improve cardiovascular and cerebrovascular complications caused by elevated blood pressure. Vasodilation is one of the most common and effective clinical treatment strategies for hypertension (O’Rourke et al., 2009). It has been found that the development of hypertension is usually linked to endothelial dysfunction, impaired endothelium-dependent vasodilatation, and altered vascular smooth muscle tone (Amssayef & Eddouks, 2023; McComb et al., 2016). Commercially available vasodilators are often limited by their adverse effects, and thus patient compliance (Krum & Pellizzer, 1998). Therefore, the search for ideal vasodilators could have far-reaching implications for the treatment of hypertension.
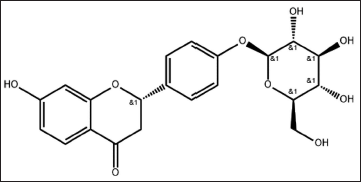
Traditional Chinese medicine is widely used to treat illnesses because it is based on many different sources: low toxicity, few side effects, low cost, and easy availability (El-Saber et al., 2020; Kwon et al., 2020; Yang et al., 2018). Therefore, exploring effective vasodilators in natural herbal medicines has become a new research prospect. Liquiritin (LQ; Figure 1), a flavonoid extracted from the Chinese medicine Radix Glycyrrhizae, possesses a wide range of pharmacological activities, including significant antioxidant, inflammation and neuroprotective effects, where its antioxidant and anti-inflammatory effects protect the heart from myocardial damage and improve cardiac function (Qin et al., 2022). It has been shown that the ethanolic extract of Glycyrrhizae has the strongest vasodilatory activity and can relax thoracic aortic rings precontracted with norepinephrine (Tan et al., 2017). Our group found that 18β-glycyrrhetinic acid, a major component of Glycyrrhizae, could induce vasodilation in thoracic aortic rings by influencing the opening of Ca2+ and K+ channels (Zhang et al., 2019). Meanwhile, 18β-glycyrrhetinic acid has a good therapeutic effect on pulmonary arterial hypertension by regulating oxidative stress levels and pulmonary artery (PA) smooth muscle cell proliferation (Zhang, Chang, & Zhang et al., 2019; Zhang, Chang, & Zhao et al., 2019). However, the effect of LQ, another major component of Glycyrrhizae, on the thoracic aortic ring is not yet reported.
The present study aimed to investigate the vasodilatory effect of LQ on isolated rat thoracic aortic rings and the possible mechanisms involved, as well as to provide an experimental and theoretical basis for the screening of drugs against cardiovascular diseases.
Materials and Methods
Animals and Reagents
Sixty Sprague-Dawley (SD) rats (220–280 g) were provided by the Experimental Animal Center of Ningxia Medical University (Ningxia, China). Rats were maintained in separate cages in an SPF environment at 22±3℃ with free access to food and water.
LQ (>98% purity) (Batch No.: Z28M10X84164; Shanghai, China). Phenylephrine (PE) was purchased from Shanghai (Batch No.: 07150801; China). NG-nitro-
Isolated thoracic aortic rings from SD rats were retained in a Krebs–Henseleit (K–H) solution (NaCl, 118.96 mmol/L; KCl, 4.73 mmol/L; NaHCO3, 25 mmol/L; CaCl2·2H2O, 2.54 mmol/L; KH2PO4, 1.17 mmol/L; MgSO4·7H2O, 1.17 mmol/L; glucose, 11.1 mmol/L; pH, 7.4; temperature, 37°C) with a standard gas mix comprising 95% O2 and 5% CO2.
Rat Thoracic Aortic Ring Preparation
Male SD rats were anesthetized intraperitoneally with 10% urethane (10 mL·kg-1), fixed on a surgical plate, and cut in the center of the chest to immediately separate the thoracic aorta. The isolated thoracic aorta was quickly transferred into a K–H solution containing 95% O2 and 5% CO2. The rings were carefully trimmed to approximately 3–4 mm by removing perivascular fat and connective tissue. A model in which endothelial vascular rings were removed was prepared by rubbing the endothelial surfaces of some vascular rings with cotton swabs. The isolated thoracic aortic rings were floated in a 10 mL bath preheated to 37°C, where an m-type hook was fixed at one end and the other end connected to a bio-information acquisition system via a tension transducer. After passing the rings through the mixed gas solution, the resting tension was adjusted to 2.0 g, and the solution was changed once every 15 minutes for 60 minutes. The vascular ring was precontracted using KCl (40 mmol⋅L-1), which was repeated twice, and the difference in KCl contraction amplitude between the two contractions was less than 10%. To validate endothelial integrity, add 1 µM constrictor PE to constrict blood vessels, stimulate until the plateau phase, and add Ach 10 µM after it stabilizes. Diastolic 2 minutes, endothelial integrity was considered when the vasodilation amplitude was greater than 70%. When Ach does not produce a diastolic effect or the diastolic amplitude is less than 10% of precontraction, it is considered that endothelial function is incomplete and belongs to the de-endothelial group.
Influence of LQ on the Resting Tension of Thoracic Aortic Rings
Separated rat thoracic aorta vascular rings with intact endothelia were divided into control and administration groups. After stabilization, cumulative concentrations of LQ were added every 2 minutes. The final concentrations were 1, 3, 10, 30, 100, and 300 µM. Equal volumes of K–H nutrient solution were added to the control group to observe changes in vascular tension.
Effect of LQ on PE Pre-contracted Thoracic Aortic Rings
Isolated rat thoracic aorta vascular rings with intact and denuded endothelia were divided into blank control and administration groups. PE (1 µM) was used to induce a steady contraction in the aortic ring. After stabilization, LQ was added every 2 minutes with final cumulative concentrations of 1, 3, 10, 30, 100, and 300 µM. Equal volumes of K–H nutrient solution were added to the blank control group to observe changes in vascular tension. Vascular tension in the rings was recorded as follows.
Effect of LQ on L-NAME and INDO Pretreated Thoracic Aortic Ring Tension
The isolated thoracic aortic rings were divided into experimental and control groups after stabilization in K–H solution at 37°C for 1 hour. In the experimental group, the thoracic aortic rings were excited with L-NAME (0.1 mmol/L) and INDO (10 µmol/L) for 20 minutes, and PE (1 µM) was applied to precontract the rings. After the vessels reached a stable contraction, LQ was added every 2 minutes until concentrations of 1, 3, 10, 30, 100, and 300 µM and equal amounts of K–H solution were added to the control group. The rate of vasodilation in each group was computed from the amplitude of PE-induced vascular tone measured after drug administration.
Effect of LQ on Tension of K+ Channel Inhibitor Pretreated Thoracic Aortic Rings
To investigate whether K+ channels affect the vasodilator action of LQ, thoracic aortas were incubated with BaCl2 (1.0 mmol/L), TEA (10 mmol/L), 4-AP (5.0 mmol/L), and Gli (0.01 mmol/L) for 20 minutes after precontraction with PE (1 µM). After the vasculature reaches a stable constriction, add LQ or K–H solutions of different concentrations.
Statistical Analysis
Data were processed and analyzed using SPSS 26.0 and GraphPad Prism statistical analysis software, and results were expressed as mean ± SEM. Results were compared between two samples using independent samples t-test. p < 0.05 was considered statistically significant.
Results
Effect of LQ on the Resting Tension of Thoracic Aortic Rings
Compared to the control group, there was no significant impact of LQ administration on the resting endothelial tension of the vascular ring (p > 0.05; Figure 2), suggesting that it had no effect on the normal vascular ring.
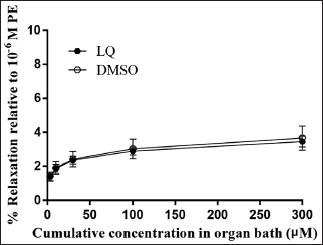
Effect of LQ on PE Precontracted Thoracic Aortic Rings
Compared with the control group, LQ exerted a dose-related vasorelaxation effect on isolated rat thoracic aortic rings with intact and denuded endothelium that were precontracted with PE (p < 0.001; Figure 3A–B). The relaxation effects of LQ on isolated rat thoracic aortic rings with intact and stripped endothelium were not significantly different (p > 0.05; Figure 3C).
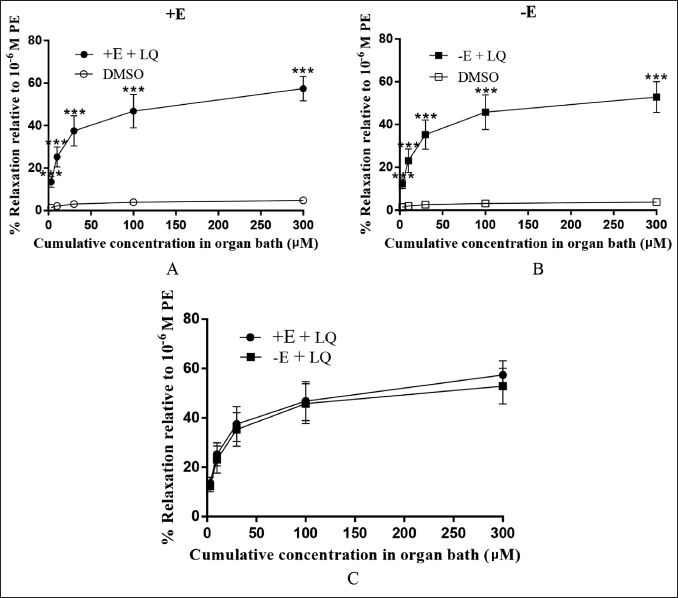
Effect of LQ on L-NAME and INDO Pretreated Thoracic Aortic Ring Tension
Compared with the control group, L-NAME and INDO incubation groups failed to inhibit the effect, indicating that the vasorelaxation effect by LQ on the vascular rings was not affected by L-NAME and INDO (p > 0.05; Figure 4A–B).
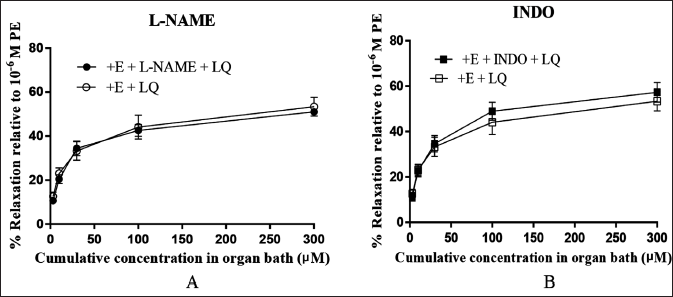
Effect of LQ on Tension of K+ Channel Inhibitor Pretreated Thoracic Aortic Rings
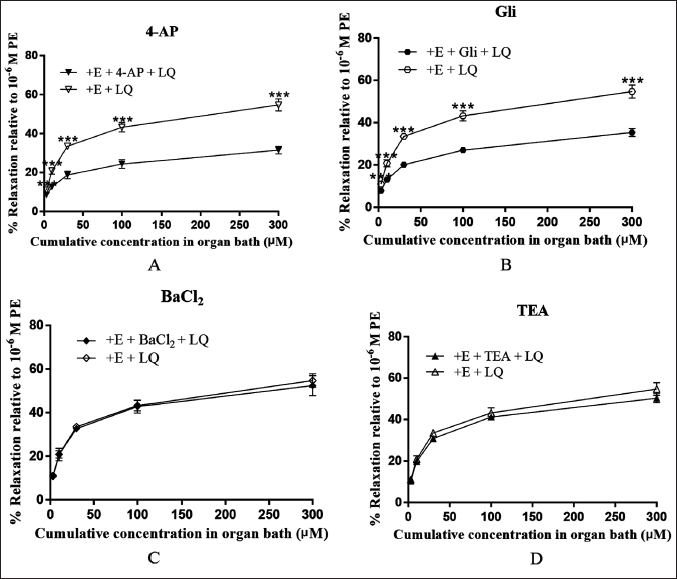
In comparison with the control group, 4-AP and Gli significantly inhibited the vasorelaxation effect of LQ (p < 0.001; Figure 5A–B). However, this vasorelaxant effect was not inhibited by BaCl2 and TEA (p > 0.05; Figure 5C–D).
Discussion
Hypertension is a chronic noncommunicable disease characterized by an increase in blood pressure in the arteries of the body circulation (Aryal et al., 2020; Feng et al., 2021; Ito et al., 2022). In the treatment of hypertension, it is vital to lower blood pressure and control its stability, with vasodilation being a common and effective strategy for lowering blood pressure (Arguedas et al., 2020; O’Rourke et al., 2009). Radix Glycyrrhizae is one of the most common local herbs in Ningxia and is used to treat various diseases because it is grown in large quantities and is easily available (Zhang, Chang, & Zhao et al., 2019; Zong et al., 2013). LQ is an important flavonoid extracted from Glycyrrhizae. In this study, LQ was found to have a vasoconstrictive effect on isolated rat thoracic aorta following vascular tension assays and showed varying degrees of relaxation effects on PE-induced vasoconstriction. Thus, the blood pressure lowering and stabilizing effect of LQ was hypothesized to be related to its modulation of vascular tension. Owing to this, we researched the diastolic effect of LQ on rat thoracic aortic rings and its possible mechanism.
In order to evaluate whether LQ has a diastolic effect on normal vascular rings, the impact of LQ on the resting tension of thoracic aortic rings was investigated in this experiment, and the results indicated that LQ did not have any effect on the normal rings of blood vessels, which can be further investigated to see whether LQ has a diastolic effect on preconstricted vascular rings in PE. The results showed that LQ had a dose-dependent vasodilatory effect on PE-preconstricted endothelium-intact and detached isolated rat thoracic aortic rings, suggesting that LQ may play a role in blood pressure reduction by vasodilating the blood vessels, resulting in a decrease in peripheral and central vascular resistance, which is expected to be a potential new drug for the treatment of cardiovascular diseases. Recent studies have shown that vascular smooth muscle and vascular endothelial cells play an instrumental role in regulating vascular tone (Qiu et al., 2017). Therefore, exploring the mechanisms of vasodilation and contraction of vascular smooth muscle and endothelial cells may provide new solutions for clinical antihypertensive therapy. Numerous reports have found that the vascular endothelium has an important role to play in modulating vascular tone and maintaining the balance between vasodilation and contraction by interacting with vascular smooth muscle cells (Púzserová et al., 2010; Triggle et al., 2012). Vasodilator drugs can be classified as endothelium-dependent or endothelium-independent, and there is a close relationship between vascular endothelial incompleteness, endothelial functional impairment, and the development of cardiovascular diseases (Goon et al., 2006).
Vascular endothelial cells regulate vasodilation by synthesizing and secreting vasoactive substances (nitric oxide (NO) and prostaglandin (PGI2)) that act on the vascular smooth muscle cells (Liu & Khalil, 2018). Currently, there are two main mechanisms of vascular dependence on endothelial diastole: the NO and PGI2 pathways (Godo & Shimokawa, 2017). The strongest vasodilatory factor, NO, released by the endothelium is produced by the oxidation of
In addition to the regulation of vasodilation by endothelium-derived diastolic substances, ion channels in vascular smooth muscle cell membranes are key factors in the regulation of vasoconstriction and diastole. K+ channels affect vascular smooth muscle contraction and diastole by altering the cell membrane potential (Khan et al., 2012). When K+ channels in vascular smooth muscle cell membranes are activated, K+ efflux causes cell membrane hyperpolarization and reduces the intracellular Ca2+ concentration, resulting in vasodilation (Yang et al., 2022). Four main types of K+ channels exist in vascular smooth muscle cell membranes: inwardly rectifying K+ (Kir), ATP-sensitive K+ (KATP), Ca2+-activated K+ (KCa2+), and voltage-sensitive K+ channels (Kv) (Boz et al., 2016; Hessler et al., 2019; Sorrentino et al., 1999). This study found that the diastolic effects of LQ on vascular rings after preincubation with the Kir inhibitor, BaCl2, and the KCa2+ inhibitor, TEA, were not significantly different from those in the control group. In contrast, the Kv inhibitor 4-AP and the KATP inhibitor Gli antagonized the diastolic effect of LQ on thoracic aortic vascular rings after preincubation, suggesting that the Kv and KATP pathways may be involved. Both Kv and KATP channels are essential for the maintenance of normal vascular function and for the differentiation and maturation of vascular cells (Jackson, 2017). The opening and closing of Kv channels are regulated by changes in cell membrane potential and open during depolarization, permitting the efflux of potassium ions, which is essential for repolarization and for the regulation of neuronal excitability (Xiong et al., 2013). KATP channels are sensitive to the intracellular ratio of ATP to ADP and usually open when ATP levels fall, helping to regulate the heart’s auto-rhythm (Dogan et al., 2019). Stimulation of IKCa (calcium-activated potassium channel) channels on vascular smooth muscle cells in human atherosclerotic vessels has been found to result in vascular smooth muscle cell proliferation and spindle cell morphology (King et al., 2015; Rojas et al., 2020). The levels of functional expression of BKCa channels in vascular smooth muscle cells are increased in hypertension, suggesting that BKCa channels may be a novel hypertension treatment target (Guan et al., 2016). The results of this experiment suggest that LQ may have a regulatory role in cardiovascular disease by acting on the Kv and KATP pathways, and its role needs to be further verified.
Recent studies have shown that betaine has a dose-dependent vasodilation effect on a PE-precontracted PA of rats with pulmonary hypertension, whereas pretreatment with the KCNQ inhibitor linopirdine markedly prevented the vasodilatory effect, suggesting that betaine can induce stable vasodilation in normal and reconstructed PA rings by activating the KCNQ channel (Shan et al., 2023). The difference between this aforementioned experiment and ours is that only a single pathway inhibitor was used in the former; however, the study was conducted on a control and pulmonary hypertension model, providing new research avenues for subsequent experiments. The advantage of our study is that multiple pathway inhibitors were used to explore the vasodilation mechanism of glycyrrhizin. Vasodilatory effects have also been reported for three extracts of Glycyrrhiza uralensis and found that 50% ethanol extract (EFG) had the strongest vasodilatory effect and that the vasodilatory effect of EFG was partly due to the participation of Kv and KATP channels. Approximately 38% of vasodilation was inhibited by the blocker Gli, suggesting that EFG primarily uses KATP channels as one pathway to exert vasodilation. Additionally, approximately 15% reduction in vasodilatory impacts strongly suggests that Kv channels are involved in these effects (Tan et al., 2017). The above studies suggest that LQ and EFG may exert vasodilatory effects through the same ion channels.
Conclusion
LQ vasodilates non-endothelium-dependently in isolated rat thoracic aortic rings, and the mechanism of LQ-induced vasodilation may be associated with the activation of Kv and KATP channels. Taken together, our results support the potential of LQ as an alternative naturally derived vasodilator, and unravel the potential mechanism of LQ-induced vasodilation in aortic rings. For a more comprehensive understanding of the vasodilatory potential of LQ, further studies should be conducted in animal models of diseases.
Footnotes
Abbreviations
LQ: Liquiritin; PE: Phenylephrine; L-NAME: NG-nitro-
Acknowledgments
The authors are indebted to the staff of the Animal Center and the Science and Technology Centre at Ningxia Medical University (Ningxia, China) who assisted us during this study.
Authors’ Contributions
XY and ZW performed the literature search. Y-WB and YY performed data curation. RZ and Q-BX carried out project management. Y-LC and M-XM wrote the original draft of the manuscript. RZ and Y-LC reviewed and edited the manuscript. All the authors reviewed and approved the final draft.
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship and/or publication of this article.
Ethical Approval
All experimental procedures using rats were reviewed and approved by the Ethics Review Committee of Ningxia Medical University (Certificate No.: SCXK Ningxia 2020-0001).
Funding
The authors disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This project was supported by the 2019 College Students’ Innovation and Entrepreneurship Training Program (S201910752002).
