Abstract
Background
Hypothyroidism (HT) is the most prevalent endocrine disorder, affecting approximately one in 10 out of 35 adults, with a higher prevalence in females and the elderly.
Purpose
This systematic review (SR) aimed to discuss the effects of yoga on markers and comorbid conditions of HT.
Methods
The SR was registered with the PROSPERO (PROSPERO 2022 CRD42022312990). Google Scholar, PubMed, Cochrane, and EMBASE were searched for the relevant English language interventional studies published from 31 December 1947 to 31 December 2023 by using the keywords ‘meditation OR breath regulation OR yoga OR yoga nidra AND hypothyroidism OR hypothyreosis OR underactive thyroid OR low thyroid’. Of the 4078 screened studies, eight eligible studies (three RCTs, two pilot studies, two pre-post trials, and one case study) with 421 HT patients (392 females and 29 males) and three to six-month yoga interventions were included. Two independent review authors extracted study characteristics and synthesised them descriptively. RCTs and NRSIs were assessed for risk-of-bias (RoB) using Cochrane tools RoB2 and ROBINS-1.
Results
The findings suggest that yoga effectively improves the thyroid profile, lipid profile, heart rate variability, pulmonary functions, anxiety, depression, and quality of life among HT patients.
Conclusion
Yoga may be an inexpensive add-on preventive and therapeutic option for HT. The clinical and methodological heterogeneity among the studies did not allow for meta-analysis (MA). Well-designed MAs are warranted by including rigorous RCTs to draw valid conclusions and defined mechanisms regarding the efficacy of yoga practices/interventions on HT.
Introduction
Hypothyroidism (HT) is the most prevalent endocrine disorder, affecting approximately one in 10 out of 35 adults, showing its higher prevalence in females and the elderly.1, 2 In the USA, HT prevalence grew from 9.5% in 2012 to 11.7% in 2019. 3 In India, 11% of people have HT, compared to 2% in the UK and 4·6% in the USA. 4 Women are affected approximately six times more often than men with an underactive thyroid, 1 which may be due to autoimmune disorders, nutritional deficiencies, or hormonal imbalances. HT is the under-secretion of thyroid hormones (THs) from thyroid glands/impaired resistance of peripheral tissues to the effects of THs, resulting in a hypometabolic clinical state. 5 The signs and symptoms of HT include fatigue, weakness, dry skin, feeling cold, rapid heartbeat, thinning hair, trouble focusing, lousy memory, constipation, obesity, weak appetite, menorrhagia, dyspnoea, hearing impairment, myxoedema, bradycardia, diffuse alopecia, and peripheral oedema. 6 If left untreated, it may lead to hypertension, dyslipidaemia, infertility, cognitive impairment, neuromuscular dysfunction,4, 6, 7 and comorbidities, such as coronary artery disease, obesity, osteoporosis, depression, and sleep apnoea 8 . The treatment of HT focuses mainly on substituting the deficient hormone, and over 78% of HT patients receive thyroxine (T4) monotherapy—levothyroxine (LT4) to reach a euthyroid state.3, 9, 10 Persistent intake of synthetic levothyroxine (levothyroxine, synthroid, and others) might make patients drug-dependent and induce adverse effects.3, 5 Patients need to switch to alternative therapies to control the overall impact of HT on their lives. 11
Yoga is an ancient oriental practice that aims to purify the body, breath, bioenergy, cognition, and emotion to promote holistic wellness as an indispensable foundation for spiritual elevation.12, 13 Yoga includes an array of practices─cleansing technique (shatkarma), pose (asana), conscious breath regulation (pranayama), neuromuscular lock (bandha), seal (mudra), sensory withdrawal (pratyahara), concentration/mindfulness (dharana), and meditation (dhyana).14, 15 Yoga improves psychosomatic health by optimising psycho-neuroendocrine interactions, musculoskeletal health, immune system, cardiopulmonary functions, metabolic processes, bioenergy, and worldly outlook. Yoga is also a psychosomatic intervention for thyroid disorders that can be practised by all age groups and genders with minor side effects. 16 Yoga is a cost-effective and easy option for several physical and mental ailments.17, 18 The American College of Sports Medicine (ACSM) and the American Heart Association (AHA) reported that moderate to low-intensity yoga exercises can mitigate underactive thyroid symptoms. 19 A study consistently showed that a 50-minute yoga session for 10 days significantly decreased body weight, body mass index (BMI), waist circumference, lipid profile, and thyroid-stimulating hormone (TSH) levels 20 of underactive thyroid patients. The untested hypothesis asserts that yoga poses such as sarvangasana, bhujangasana, halasana, surya namaskar, marjariasana, and vipritkarani mitigate thyroid disorders, including HT by inducing mechanical effect and vascular supply on the thyroid. 20 However, no systematic reviews (SRs) and meta-analyses (MAs) synthesise the reported results regarding the effectiveness of yoga interventions in improving primary/secondary markers and comorbid conditions of HT. Therefore, this SR aimed to discuss the impacts of yoga interventions on primary/secondary markers of HT by synthesising the reported effects in the eight interventional studies.
Methods
Registration
This SR followed Preferred Reporting Items for Systematic Reviews and Meta-analyses (PRISMA) guidelines and was registered with the International Prospective Register of Systematic Reviews (PROSPERO) with registration number PROSPERO 2022 CRD42022312990.
Eligibility Criteria
In this SR, all the full-text interventional studies evaluating the effect of yoga on HT and published in the English language were included. The selection of studies was based on the Population Intervention Comparison Outcome (PICO) statement, as depicted in Table 1.
PICO Statement.
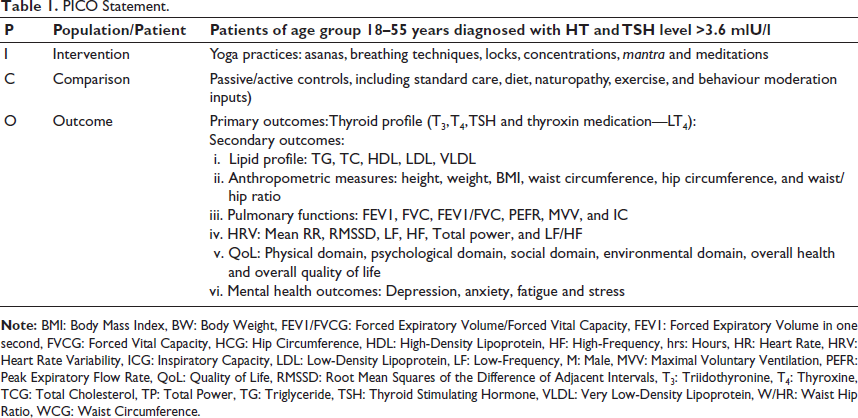

Search Strategy
PubMed, Cochrane, EMBASE, and Google Scholar were searched to identify the relevant studies published from 31 December 1947 to 31 December 2023. Meditation OR breath regulation OR yoga OR yoga Nidra AND hypothyroidism OR hypothyreosis OR low thyroid were used as search keywords. Only articles in the English language were included in the studies. The search was limited and filtered by selecting only interventional studies that mainly assessed the effect of yoga therapy on HT. The detailed search strategy is depicted in Table 2.
Detailed Search Strategy.
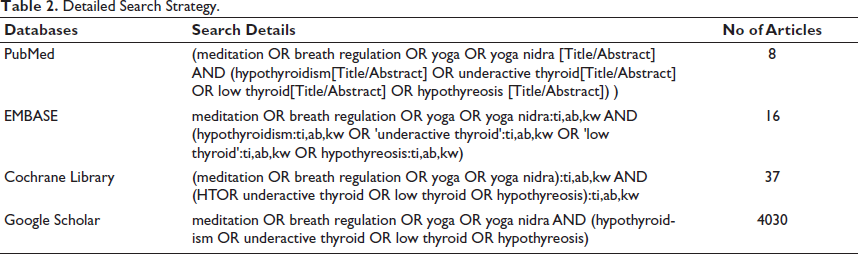
Study Selection and Data Extraction
The studies were searched from the above-stated databases, and the search engine was exported to the citation manager, Mendley version 1.19.8. The duplicates were filtered and removed. The retrieved articles were screened individually for titles and abstracts by two independent review authors to verify their eligibility for inclusion. The study characteristics, including author, publication year, country, study design, sample characteristics, intervention, comparator, measures, outcome variables, results, and findings, were extracted from each study and condensed into tabular form.
Risk of Bias in Individual Studies
The quality of studies included in the review was assessed using the Revised Cochrane risk-of-bias tools for randomised controlled trials (RoB2) and non-randomised studies of interventions (ROBINS-I).
Study Selection
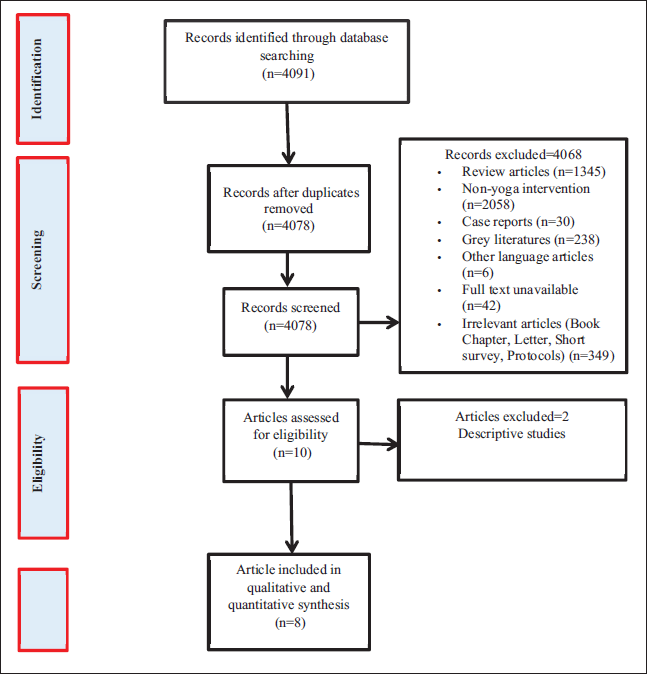
A total of 4091 records with 13 duplicates identified from one search engine (Google Scholar = 4030) and three databases (Cochrane = 37, PubMed = 08, EMBASE = 16) were exported to a citation manager, Mendley version 1.19.8. The remaining 4078 records were then screened for irrelevant studies. The screening yielded 10 studies, which were further assessed for eligibility. Of the 10, two descriptive studies were excluded. Finally, eight studies were eligible for this review, as shown in Figure 1.
PRISMA Flow Diagram for Study Selection.
Study Characteristics
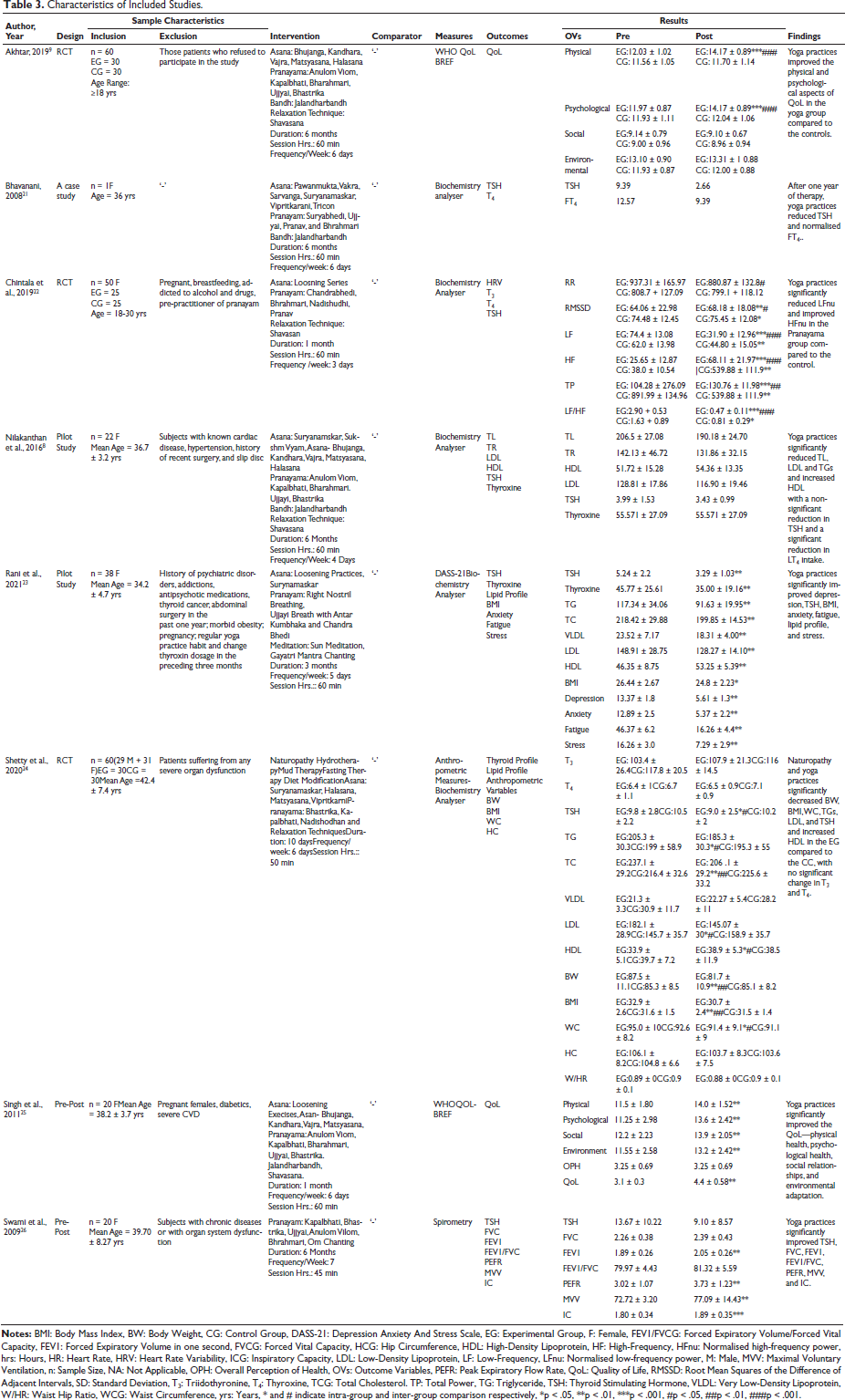
Eight studies (three RCTs, two pilot studies, two pre-post clinical trials, and one case study) were eligible to be included in this review. The studies had 421 participants (392 females and 29 males) diagnosed with HT. Yoga therapy for three to six months was the intervention. Table 3 provides a detailed description of the study characteristics.
Characteristics of Included Studies.
Results
RoB in Studies
All three RCTs were assessed with moderate overall RoB. All NRSIs were assessed with unclear overall RoB. Summary of RoBs regarding included RCTs and NRSIs are shown in Figures 2 and 3.
Summary of RoB for RCTs.
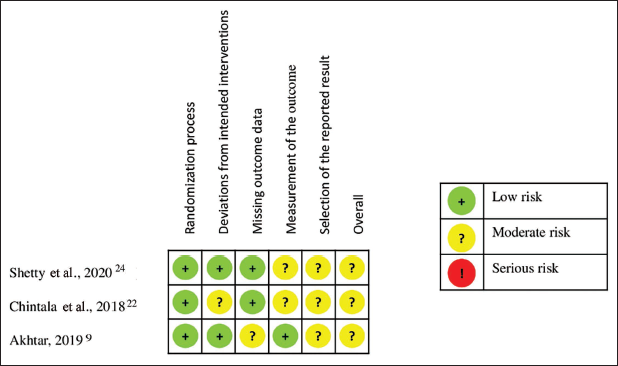
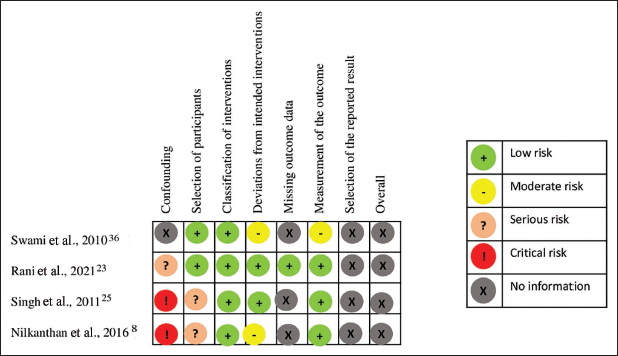
Summary of RoB for NRSIs.
Thyroid Profile and LT4
Four studies8, 23, 24, 26 indicated that yoga interventions significantly improve HT by decreasing TSH levels and doses of LT4 and increasing T3 and T4 levels. Two NRSIs with six-month yoga interventions showed significant effects on reducing doses of LT4.8, 23
Lipid Profile
Three studies8, 23, 24 reported a significant positive effect of yoga intervention incorporating yoga asanas with varied durations from 10 days 24 to 6 months8, 23 in improving lipid profiles, TC, LDL, VLDL, TG and HDL compared to standard care.
Anthropometric Outcomes
Two studies23, 24 indicated the significant effect of yoga interventions on decreasing BMI, BW, WC, HC, and W/HR of underactive thyroid patients after intra and inter-group comparisons.
Pulmonary Functions
One study 26 indicated the significant effect of a six-month yoga intervention on pulmonary functions by increasing FEV1, PEFR, MVV, and IC of underactive thyroid patients.
Heart Rate Variability
One study 22 showed the significant effect of yoga intervention on HRV by increasing RMSSD, HF, and total power and decreasing LF and LF/HF.
Quality of Life Outcomes
Two studies9, 25 indicated a significant effect of the yoga intervention to improve QoL (with an increase in physical, psychological, and environmental aspects but a slight decrease in social aspects). However, Singh et al.’s study 25 showed a significant effect of yoga intervention in improving overall QoL with no difference in overall perception of health.
Mental Health Outcomes
One case study 23 showed the significant positive effect of 6-month yoga intervention on the mental health (rated in terms of depression, anxiety, fatigue, and stress) of HT patients.
Discussion
This SR aimed to investigate the effects of yoga interventions on primary, secondary, and comorbid outcomes of HT. The synthesis of results reported in eight studies8, 9, 21–26 substantiated the beneficial effect of yoga practices in improving TSH, T3, T4, LT4, lipid profile, anthropometric outcomes (BW, BMI, HC), pulmonary functions, HRV, QoL, and mental health outcomes (depression, anxiety, fatigue, and stress) of hypoactive thyroid patients without reporting their adverse effects.
The three RCTs in the SR suggest favourable effects of yoga interventions on thyroid profile and LT4. Six-month yoga nidra practice significantly decreased TSH levels. 23 The actual mechanism underlying these results remains unknown. Studies have shown that breathing exercises, relaxation techniques, and meditation can reduce stress and balance the hypothalamic-pituitary-adrenal axis (HPA axis). 27 Yoga regulates the HPA system, lowers cortisol,28, 29 epinephrine, and norepinephrine, boost immunity (by increasing T cells, NK cells, and CD4 cells)30, 31, increases HRV 32 , empowers pulmonary functions 33 , strengthens glucose tolerance and reduces LDL.31, 34, 35 Regular yoga lowered IL-6, TNF-α 36 , and CRP and increased NK cells, T cells, B cells, and CD4 37 as an indication of inexpensive add-on therapy for HT and comorbid psychological problems. Regularly practicing bhujangasana, sarvangasana, vipritkarani, and halasana may impact the hypothalamic-pituitary-thyroid (HPT) axis and reduce blood TSH. 38 T4 and T3, which comprise just 20% of the circulating T3 in the blood, are the two main hormones secreted by the thyroid gland. Ujjayi breathing increases the intrathoracic pressure due to a slight contraction of the thyroid gland, potentially resulting in the increased secretion of T3 and T4. 39 The remainder of the T3 is created by peripheral tissues, including skeletal muscle, activating enzymes of both types 1 and 2 of iodothyronine deiodinase –DIO1 and DIO2, which split an iodine atom from T4. These yoga poses may affect skeletal muscle and peripheral tissue to activate DIO1 and DIO2, which split an iodine atom from T4. Omkar meditation enhances the circadian rhythm, induces plasma melatonin 33 , and may modulate serum TSH levels.
The two included trials24, 40 showed positive effects of yoga interventions in reducing TG, TC, LDL, and VLDL of hypoactive thyroid patients. Yoga practice stimulates the thyroid gland to secrete THs—T3 and T4. Increased TH lowers plasma levels of phospholipids, TGs, and cholesterol. Conversely, decreased thyroid secretion significantly increases cholesterol, phospholipids, and triglyceride plasma concentrations. THs lower plasma cholesterol levels by several processes, one of which is a marked increase in bile secretion of cholesterol and the resulting loss of cholesterol in feces. THs may cause an increase in LDL receptors in the liver cells, which in turn causes the liver to quickly remove LDL from plasma and secrete cholesterol in these lipoproteins by the liver cells. The consequences are the same as Nilakanthan et al.’s study finding, which reported a significant decrease in lipid profile outcomes after 16 weeks of yoga intervention. 8 An RCT showed a significant reduction in lipid profile after five months of YT.22, 23 Increased postural activity may have contributed to a decrease in TGs, TC, LDL, and an increase in HDL.28, 41 The increase in hepatic lipase and lipoprotein lipase, which can enhance the absorption of TGs by adipose tissue and impact lipoprotein metabolism, may cause a change in lipid profile followed by yoga practice. 20
Yoga interventions significantly improved anthropometric outcomes—BW, BMI, HC, WC, and W/HR-significantly. 24 Another study has shown that bhujangasana (cobra pose), bhastrika (periodic breathing), and kapalabhati (deep breathing) pranayama stimulate metabolic rate and oxygen consumption 42 by reducing body weight. Various studies found that being overweight is associated with overstimulation of the HPA axis, which alters the diurnal cortisol secretion. 43 Abnormal regulation of the HPA axis and perceived stress-dependent cortisol levels are strongly related to perturbations of the endocrine axis. 44 Consistently, an SR and MA including 44 RCTs with a total of 3168 participants reported a significant effect of yoga on improving blood pressure, heart rate, breath rate, waist circumference, waist/hip ratio, total cholesterol, HDL, VLDL, TGs, glycosylated haemoglobin (HbA1c), and insulin resistance in the general population and high cardiovascular risk groups compared to usual care and no intervention. 45
A study showed that yoga intervention significantly impacts pulmonary functions in hypothyroid patients. 26 The three-month practice of Hatha yogic postures, pranayams (nadisodhan, bhastrika, bhramari, sheetali, and shitkari), and omkar meditation divided into two sessions—morning and evening, a day improved cardiorespiratory performance (heart rate, blood pressure, mean arterial pressure, respiratory rate, FVC, FEV1, FEV%, PEFR, and MVV), and psychologic profile (anxiety, depression, and well-being) along with an increase in plasma melatonin level. 33 The improvement in pulmonary functions may be due to better respiratory muscle strength, improved thoracic mobility, and the balance between lung and chest elasticity, which yoga practitioners may have gained from regular yoga practice. 46
A study indicated yoga intervention’s highly significant positive effect on HRV in hypothyroid patients. 22 The increased HRV at rest after practising pranayam indicated a stimulated parasympathetic tone that might reduce the risk of symptoms. 47 Cyclic meditation/mindfulness followed by yoga poses consistently increased HRV by stimulating the parasympathetic tone.28, 32 HRV is decreased mainly because of a significant decrease in vagal activity. 48 Some studies suggest that TSH stimulates sympathetic output from the central nervous system and acts as a neurotransmitter, critical in determining sympathovagal imbalance. 49 Decreased vagal tone and increased sympathetic activity in HT have important clinical implications. Catecholamine receptor desensitisation decreases cardiac output, leading to a compensatory increase in norepinephrine release. 50 Indeed, patients with low vagal tone are more susceptible to cardiovascular diseases such as myocardial infarction, rhythm disorders, and hypertension. 51 Pranayama appears to alter autonomic responses by breath-holding, increasing vagal tone, decreasing sympathetic discharge, and causing relaxation. 52 Various studies have found that slow breathing increases blood pressure oscillations and HRV amplitudes, particularly at a respiration rate of six breaths per minute (0.1 Hz).53, 54
An RCT showed significant improvement in the physical, physiological, social, and environmental domains of QoL 9 , like Cramer et al.’s findings. 16 Rani et al. (2021) reported a significant effect of yoga practices on comorbid psychological conditions of HT—depression, anxiety, fatigue, and stress, aligned with Streeter’s findings that assert a significant effect of yoga to increase thalamic GABA and improve anxiety. 55 The two qualitative studies conducted by Cartwright et al. (2023) and Park et al. (2014) also consistently reported that yoga improved stress, mindfulness, emotional regulation, self-regulation, inclusiveness, social relation and spiritual pursuit.56, 57 Sudarshan kriya yoga (SKY) (including a set of breath regulatory practices ujjayi, bhastrika, pranav, and cyclical breathing) 58 is found supportive of mitigating neuropsychiatric illnesses—depression, anxiety, and stress, by upregulating gene expression—cyclooxygenase-2 gene, antiapoptotic BCL-2 gene, heat shock protein 70, and telomerase reverse transcriptase (hTERT) resulting in robust immune functions 59 ; decreased ACTH and cortisol28, 60; and increased prolactin 61 and oxytocin. 62 SKY also elevates antioxidant markers—superoxide dismutase (SOD) 63 and glutathione peroxidase. 59 Carlson et al. (2004) also reported that a mindfulness-based stress reduction (MBSR) programme comprised of relaxation, meditation, gentle yoga poses, and daily home practice significantly improved overall QoL, stress, and sleep quality and reduced cortisol levels in breast and prostate cancer patients. 64 Yogic breathing practices—ujjayi (breathing against airway resistance) and bhastrika (forceful nasal breathing), initiate adequate interhemispheric synchronisation and generate a dominant global brain rhythm with high-frequency cerebral activity and have been accepted for improving and maintaining physical and emotional health via down-regulation of the HPA axis resulting in enhanced autonomic and emotional control, cognitive functions and the QoL in all age groups.65, 66
The mechanical and vascular effects developed on thyroid by the practice of yoga poses and locks (suryanamaskar, bhujanga, sarvanga, matsya, kandhra, vipritkarani, halasana, tricon, vakra, ardhamatsyendra, jalandharbandh); parasympathetic tone and immunomodulation induced by the practice of ujjayi, bhramari, chandrabhedi, solar meditation, om/Gayatri mantra chanting, and corpse pose; and improved cardiopulmonary function and weight reduction caused by the practice of bhastrika, kpalbhati, suryabhedi, loosening poses, and alternate nostril breathing may prevent and mitigate the HT. The mechanisms of yoga practices’ effects on HT are yet unclear and need to be explored and tested in further studies.
Conclusion
Duly designed yoga interventions, including yoga poses, breath regulations, locks, concentrations, and meditations, may improve thyroid profile, lipid profile, cardiopulmonary functions, anthropometric outcomes, quality of life, and mental health of hypothyroid patients as inexpensive add-on therapy with minimal risk. Definite yoga practices with a detailed mechanism of positive effects on thyroid disorders are still unclear, warranting the need for further explanatory research regarding specific yoga practices versus hypothyroidism.
Limitations and Recommendations
The included eight studies had considerable clinical and methodological heterogeneity. This created a fragile base to conclude the positive effects of yoga interventions on primary/secondary markers and comorbid conditions of hypothyroidism. Moreover, inclusion, discussion, and derived conclusions regarding the impact of yoga on hypothyroidism inferred from more NRSIs warrant the future conduct of more rigorously designed RCTs and their inclusion in SRs and MAs to reach more definite and valid conclusions regarding the effects of yoga interventions on hypothyroidism.
Footnotes
Acknowledgements
The authors thankfully acknowledge the Honorable Acharya Balkrishna, Vice Chancellor, for constant administrative support and motivation and the Department of Yoga Science, University of Patanjali, for academic support.
Authors’ Contribution
R.B.B.: Conceptualization, Supervision, Methodology, Writing-original draft, Writing-review and editing, Validation, Visualization, Project Administration. P. K. M.: Data Curation, Formal Analysis, Writing.
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship and/or publication of this article.
Funding
The authors received no financial support for the research, authorship and/or publication of this article.
Statement of Ethics
Ethical permission was not applicable for this article, as this is a review article drafted from various research articles and not from patients directly.
