Abstract
Background
Sleep and immune function are interconnected aspects of health that mutually impact each other in disease development and inflammatory homeostasis. Different aspects of immunology are regulated by different sleep characteristics, impacting on specific aspects of immune function including cytokine production and T-cell activity. Ongoing disruptions of sleep have been linked to heightened inflammation and are suspected in the pathogenesis and disease course of a range of life-style-related illnesses, including diabetes and neurodegenerative diseases.
Summary
This review provides a comprehensive overview of knowledge on the interaction of sleep with the immune system, its modulation of inflammatory balance, and the pathogenesis of many diseases. It emphasizes how sleep deficiency compromises immune function by means of a systemic, low-grade inflammatory response, while adequate sleep promotes intense immune responses and thus enables efficient pathogen clearance and the maintenance of immune memory. The mutual influence of sleep on the immune system underlines its critical involvement in health preservation and the course of disease.
Key Message
Sleep plays an indispensable role in immune health, mediating the efficiency of immune responses and the course of the regulation of inflammation. Chronic sleep deprivation can result in a low-grade inflammation that substantially contributes to the onset and exacerbation of metabolic and neurodegenerative disorders. The intimate linkage between sleep and immune function can be one strategic approach to therapy, improving health outcomes by leveraging this sleep-immune connection.
Introduction
The interactions of our sleep and the immune system can be observed in everyday life. The amount of sleep increases to improve the recovery rate whenever an individual is infected or catches up viral. Good sleep is significant in boosting the strength and immunity of an individual.
The daily bodily needs are modulated with the help of time perception, an essential aspect of the body mechanisms to work. To maintain these body requirements, various cycles oscillate hormones as in the neuroendocrine system, temperature, and sleep-wakefulness as observed in the circadian rhythm. These biological cycles, when disrupted, can lead to health problems. When the sleep-wakefulness cycle is disrupted, it can be a potential risk factor for metabolic diseases like diabetes, cancer, and cardiovascular anomalies. 1 During sleep, it is seen that there is functional activation of particular brain regions, which is a result of the inert withdrawal of all afferent stimuli. Sleep is, therefore, not a simple process; it modulates memory consolidation, mood, concentration, and temperature, along with modulating the immunological response and immunity. Hence immunity is affected due to lack of sleep which leads to more probability of getting or acquiring a disease. Various field studies have observed changes in sleep patterns due to chronic immune system activation. 2
According to many studies, disturbed or improper sleep (short duration) increases the chances of viral infections (common cold). 3 Mental health and everyday behaviour are negatively altered due to lack of sleep. 4 Healing is known to be modulated by sleep. Scientific evidence from the last 1.5 decades of neuroimmunology research suggests that immunity and immunological defence are increased with the help of sleep. Many particular physio-anatomical conditions are the basis of such neuro-immunological defence.
These conditions include:
Blood pressure, blood flow, and lymph flow are affected indirectly, while hormones are affected directly when the autonomic nervous system (ANS) and the neuroendocrine system regulate the immune system.
5
Peptidergic, sympathetic and sensory nerve fibres innervate the thymus and bone marrow and mucosa-associated lymphatic tissue, lymph nodes, and spleen.
6
Chemokine and cytokines, hormones, neuromodulators, and neurotransmitters are the intercellular signals which are commonly shared by glial cells, immune cells, neurons, and receptors are expressed for such signals.
7
These intercellular signals have the ability to cross the blood-brain barrier (BBB) from either direction.
8
Brain parenchyma, nerve endings, and meningeal borders all over the body have traffic of immune cells.
9
This review discusses the involvement of several inflammatory mediators in natural, normal sleep in the presence of viral inflammatory conditions. Research focuses on both sudden and long-term immune responses to infections and inflammation. Recent studies have elucidated critical connections between sleep and immune system function. Research indicates that sleep enhances the efficiency of immune responses by promoting the production of cytokines and supporting T-cell activity.10, 11 Chronic sleep deprivation has been linked to increased inflammation and impaired immune responses, contributing to conditions such as diabetes and neurodegenerative diseases.11–13 Additionally, studies have highlighted the role of sleep in modulating the gut microbiome, which in turn influences immune homeostasis.14, 15 These findings underscore the bidirectional relationship between sleep and immune function, emphasising the importance of adequate sleep for maintaining health and preventing disease. With this review we aim to synthesise current knowledge on the interplay between sleep and immune function, highlighting recent advancements and identifying gaps in the literature. As there is a growing evidence of sleep’s crucial role in immune regulation and its impact on inflammatory diseases, a comprehensive review is essential. By consolidating these findings, we seek to provide a clearer understanding of the mechanisms involved and to underscore the importance of adequate sleep for maintaining immune health and preventing disease. This synthesis will aid researchers and clinicians in developing targeted interventions and inform future research directions.
Methodology
Search Strategy
We conducted a comprehensive literature search using databases such as PubMed, Google Scholar, and Scopus. Keywords included ‘sleep’, ‘immune system’, ‘cytokines’, ‘inflammation’ and ‘immune regulation’.
Inclusion Criteria
We included peer-reviewed articles published in the last 10 years that focused on the interactions between sleep and the immune system. Both human and animal studies were considered.
Analysis Methods
Selected studies were analysed for relevance, methodological rigour, and findings. Data were synthesised to highlight key mechanisms and the impact of sleep on immune responses and inflammatory homeostasis.
Stages of Sleep and Assessment Methods
Sleep comprises two phases in general, that is, rapid eye movement (REM) stage and non-REM (NREM) sleep. NREM further consists of three stages, the N1, N2 and N3, also called as slow wave sleep (SWS). Whereas REM sleep includes REM sleep amount, REM latency, REM density, and REM duration. REM sleep is characterised by the presence of REM and low muscle tone. 16 Total sleep time and sleep efficiency, waking up after sleep onset, and total sleep latency are measures of total sleep continuity. Imaging techniques like electroencephalography (EEG), electromyography (EMG), and electrooculography (EOG) are used to understand the substrates that make the sleep cycle complete. These methods allow the observer to note different stages of sleep leading to REM sleep. In addition, the multiple electrodes of the EEG or EMG will enable one to know the stage of sleep or wakefulness. EOG accesses the random eye movements and EMG the muscle tone. 17
Spectral analysis is the mathematical tool used to study the EEG waveforms to further understand sleep components. They are used to deconstruct complex EEG waveforms into their constituent frequency waveforms to study the graph. In sleep medicine and preclinical trials, an algorithm-based method called Fast Fourier transformation is usually employed. For select frequency bands, Fast Fourier transformation of the EEG yields units of power. Frequency bands that are reported in sleep studies include slow frequency observed as less than 5Hz known (delta frequency), faster bands, that is, theta 6–9 Hz or beta 12–14 Hz and spindle frequency activity. 17
The frequency of these bands is associated with NREM sleep (spindle frequency and delta frequency bands). REM sleep has theta frequency bands. From wakefulness to NREM sleep, the brain waveforms transition from higher to lower frequency waveforms, and the amplitude increases the delta waveform. In contrast to this, during the transition from NREM to REM sleep, the amplitude of the EEG waveform decreases, and the low frequency of the wave is exchanged with high-frequency theta waves and spindle activity. During REM sleep, the EMG drops to the lowest level, depicting low striated muscle activity levels and general activity absences. 17 The sensitivity of spectral analysis takes into account factors such as age, insomnia complaints, and medication, which can further delineate discrepancies between subjective and objective measures of sleep. 17
Borbély and Achermann 17 stated that the longer one stays awake, the larger the homeostatic drive to sleep, that is, the sleepier one becomes. When wakefulness is prolonged, humans and animals sleep longer during the recovery night yet do not fully recover all the lost sleep. Delta waves characterise the recovery night, deep sleep, and EEG waves are slow activity. Sleep loss during prolonged wakefulness may partly be recovered by sleeping for a longer duration with higher intensity, but certain population groups like adults and patients with depression find it hard to recover NREM sleep, whereas REM sleep is retrieved more than what was lost by sleeping for longer. 17
Immune System Cells in Host Defence
Our body protects itself due to the presence of a defence system present within called the immune system. It serves the function of detecting foreign particles and eliminating the threat in order to prevent any disease or infections in the body. Various molecules and cells are located in specific regions, such as white blood cells (WBCs) or macrophages which act as the barrier to any molecular invasion. The body’s outer surface comprises physical obstacles like mucosa or epithelium layer to prevent bacterial invasion. Macrophages break down the pathogens crossing the physical barrier layer through specific receptors. These pattern recognition receptors (PRPs) induce activating signals to inflammatory mediators to generate a signalling cascade. 2
WBCs also known as leukocytes are of different forms depending on their maturation site as in bone marrow for B cells and thymus for T cells, antigen specificity as in antigen-specific T and B cells or plasmacytoid dendritic cells (pDC) and natural killer cells (NK), cytokine profile like Th1, Th2, Th17 development as in adaptive or innate, the primary site of action, function as in T helper (Th) cells, regulatory T cells, memory cells, cytotoxic T lymphocytes (CTLs), antigen-presenting cells (APCs), NK cells and haematopoietic lineage as in lymphoid or myeloid lineage (Figure 1). Cytokines and other molecules act as mediators between immune and non-immune cells. 2
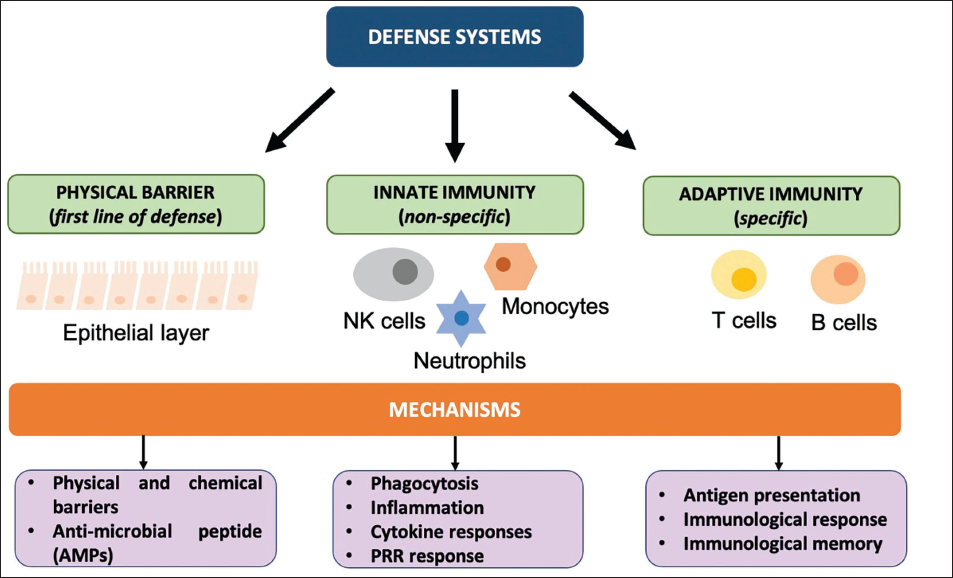
An abnormal state of the body due to infectious agents causes central nervous system (CNS) responses such as fever 18 and other symptoms, including fatigue, sleepiness, social withdrawal, negative mood (depression, anxiety), pain hypersensitivity, and decreased appetite. 19 These symptoms are considered to aid in the recovery of the body from the abnormal state and can be considered adaptive responses carried out by the CNS. For example, fever promotes the body’s action against the infectious agent by trying to weaken it or eliminate it. It has been established that fever and sickness are responses to infection and inflammatory diseases which are marked and mediated by inflammatory mediators, including cytokines and prostaglandins (PGs) that signal to the brain.19, 20 On the other hand, it has been observed that ageing and physiological conditions negatively affect neurological and immunological health.21–25 In this article, the importance of these mediators will be reviewed in the context of spontaneous, physiological sleep in the case of infectious inflammatory changes. We studied acute changes and also chronic activation for infectious and inflammatory changes.
Immunological Response and Memory Consolidation in Effect
All the altered self-antigens and the foreign antigens represented by cells or molecules are first detected and then eliminated by all the immune defence cells.26, 27 When a foreign antigen invades, adaptive immune system is activated. APCs like dendritic cells (DC) B cells, and macrophages bind to the foreign invading antigen. APCs present the foreign antigen to the T cell receptor and an immunological synapse is formed with the Th cells after APCs are migrated via afferent lymphatics to draining lymph nodes. 28 Because of antigen presentation, Th cell’s progeny is produced as Th cells activate, then proliferate, and finally differentiate into two subcategories Th1 or Th2 cells. This helps in the antibody production (from the B cells) which supports the CTL and macrophages after leaving the lymph nodes, which then eliminates the foreign antigen/pathogen. Immunological memory is formed when B cells, Th cells, and CTL which are antigen-specific survive. This immunological memory helps in a faster immune system response when the same foreign particle invades. Major histocompatibility complexes keep control of the immune system activation, and this is done by counter-regulatory and co-stimulatory signals as in the anti-inflammatory and pro-inflammatory signalling. When such signalling is altered, it results in many different conditions like allergies, immunodeficiencies, autoimmunity, and septic shock. In the case of memory, both the CNS and the immune system share one aspect which is memory. During this memory consolidation in both systems synapses are formed and include cell-to-cell contacts. 29 The synapse which is involved in the immune system is called the immunological synapse, and it is formed between T cells and APCs.28, 30 There are different stages of immunological memory, including the encoding phase, as in the antigen presentation, the consolidation phase, and the recall phase, which helps mediate the immune response when the antigen is re-encountered. These two systems are different, but the formation of neurobiological memory is regulated by sleep. 31 This suggests that immune response is also regulated with the help of sleep and can be inferred as immunological memory formation is regulated and enhanced with sleep.
Immune System and Sleep-wake Cycle
The bodily functions and behaviour are regulated with the help of circadian rhythm which is controlled by the suprachiasmatic nuclei (SCN) situated in the hypothalamus and is also known as the ‘hypothalamic pacemaker’. Circadian rhythm determines the sleep-wake cycle regulated by different clock genes controlling sleep and circadian rhythm. Cytokine production and leukocyte proliferation are the immune functions that are also regulated with the help of the sleep-wake cycle besides the cardiovascular function, mental or physical activity, and temperature regulation which coincide.
Sleep deprivation directly influences inflammatory markers and cytokine levels, primarily affecting cortisol production. SCN controls the behaviour of cortisol secretion on a daily basis which can be altered due to complications in circadian rhythm via the hypothalamic pituitary adrenal (HPA) axis and sleep-wake cycle. Changes in both pro-inflammatory proteins (TNF- α) and anti-inflammatory proteins were also recorded. 32 Tumour necrosis factor (TNF)-α and interleukin (IL) are key factors to induce alterations in NREM sleep period and sleep-wake cycle (Figure 2). Studies have concluded that anti-TNF-based therapy has shown positive results in terms of REM sleep enhancement with increased higher efficiency of sleep. 2
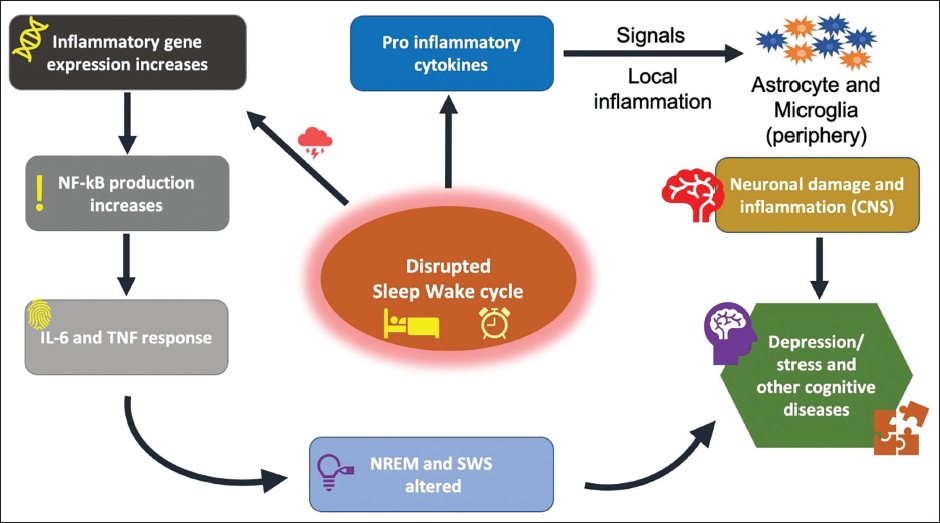
A Pro-inflammatory State is seen During the Resting Period
It is well reported that in humans during normal sleep there are decreased levels of norepinephrine, cortisol, and epinephrine in the blood, increased levels of melatonin, prolactin, GH (growth hormone) released from the pituitary, and along with this SNS (sympathetic nervous system) and HPA axis are also down-regulated.33–35 The adipocytes inhibit hunger with enhanced secretion of leptin during sleep. 36 All these factors interdependently act on sleep and the immune system. The pro-inflammatory cytokines are produced when the immune cells activate, proliferate, and differentiate in the presence of pro-inflammatory signals. 37 These pro-inflammatory cytokines include tumour necrosis factor (TNF)-α, interleukin (IL)-12, IL-1, and interferon (IFN)-γ.38–42 Anti-inflammatory signals such as catecholamines and cortisol inhibit immune function.43, 44 Hence there, it was inferred that during sleep (nocturnal) inflammatory peak is reached, which is regulated by close coordination of the immune system and the endocrine system suggesting that the pro-inflammatory signals increase, and along with this, during wakefulness, anti-inflammatory signalling activity is enhanced.45, 46
During the SWS phase, it is seen that cytokines, as well as pro-inflammatory signals, are enhanced on the level of protein and mRNA in plasma,47–50 peripheral blood cells,51–57 splenic macrophages,58, 59 lymph nodes, 40 brain 49 and adipose tissue. 49 The pro-inflammatory signals help in regulating the adaptive immune responses as they act to eliminate the endogenous danger signals like metabolism, cell injury, physical activity, synaptic transmission, ATP (nucleotides), ROS (reactive oxygen species), and HSP (heat shock proteins) and the exogenous danger signals like LPS (lipopolysaccharide), toll-like receptor ligands, which produced pro-inflammatory signals with the help of APCs.38–42, 60
In vitro, the production of pro-inflammatory cytokines is regulated by their cellular clocks (intrinsic) which include peripheral Th cells splenic macrophages and peritoneal macrophages.59, 60
Immune activation is enhanced with the help of intrinsic clock gene activity along with the exogenous danger signal and the endogenous danger signal. Besides this, the neuroendocrine system enhances immune activation during the early SWS period, which decreases the release of anti-inflammatory hormones and promotes the release of pro-inflammatory hormones. At the time of vaccination, this function of sleep as in the pro-inflammatory function of sleep, helps in achieving adaptive immunity. 59
The Peak of Immune Cell Differentiation During the Sleep Phase in Lymph Nodes and Peripheral Blood
New immune cells are continuously released in the blood circulation from the bone marrow, conducting the migration of immune cells. Neutrophils, macrophages, and DC extravasate to the periphery, whereas B cells and T cells are readily present as they circulate in the blood and start acting the immune response when any antigen is encountered in the lymphatic tissue (secondary lymphatic tissue). To reach the lymph nodes and later return to circulation through the thoracic duct and efferent lymphatics, CD62L-expressing T cells exit the blood with the help of HEVs (high endothelial venules) in humans. 61 Circadian rhythms in these cells are visible in peripheral blood and during the early rest period of sleep, and equilibrium is maintained between the lymphatic system and the blood as these immune cells show a peak, and this rhythm is seen in Th cells and T cells in the lymph nodes.62, 63 Along with these, studies have shown that sleep seems to be related to lymphocyte accumulation/collection in lymph nodes.64, 65 Rhythms of cortisol hormone in blood also affect the rhythms of T cells inversely as the peak of cortisol in blood inhibits the elevation of T cells rhythm, and with the help of increased expression of CXCR4, this cortisol-mediated redirection of T cells is mediated. 63 CXCL12 is the ligand expressed by the bone marrow which is produced throughout the active period of sleep and reaches its peak. The SNS and the clock genes regulate these rhythms. 66 Haematopoietic stem cells also express CXCR4, which the excessively into the peripheral bloodstream and includes memory T cells and naive T cells. 67 T cells expressing CXCR4 are known as the CXCR4+ T cells and are released from the bone marrow during the resting period of sleep while the HPA axis and cortisol are inhibited. These CXCR4+ T cells have the purpose of getting distributed to other areas where immune action is needed. As T cells extravasation is modulated with the help of low levels of cortisol and the extravasated to the lymph nodes from the blood. It is seen that migration of T lymphocytes from the HEV is obstructed due to glucocorticoids. 68 The lymph node rhythm of immune cells is regulated with different species-specific regulators in various animals, as seen in many animal studies. 69 Throughout early sleep, it is seen that lymph nodes have accumulated lymphocytes due to inhibited activity of SNS and enhanced GH levels.70–72
All the studies inferred that APCs, pro-inflammatory signals, central memory T cells, and naive T cells in lymph nodes are activated and proliferated during the resting period of sleep. It is still unclear that the immune rhythms are time-regulated. Pain, fatigue, immobility, malaise, mental illness, and cognitive impairment are common symptoms of inflammation during the awake stage. 73 The neuroendocrine modulations while sleeping regulate the insulin-dependent tissues, allowing the distribution of energy consumed by the proliferation of cells, resulting in immune activation.34, 47 The oxidative stress and cell damage caused by inflammation may be successfully controlled by melatonin, which is regulated by the haematopoietic stem cells and the free radicals that eventually provide cellular energy.
The association of pro-inflammatory cytokines and initiation of adaptive immunity are regulated with the reasons listed above, supported by the circadian rhythm’s particular time.
Sleep is Regulated by Inflammatory Mediators which Include
Discussion
The complex interaction between sleep and the immune system has a major impact on both the aetiology of disease and general health. The current review synthesises recent knowledge on how sleep modulates immune functions, emphasising the roles of cytokines, hormones, and neurotransmitters in maintaining inflammatory homeostasis. By integrating the findings on common mechanisms, our review highlights the complex yet essential role of sleep in immune regulation and its broader implications for health and disease management. This comprehensive synthesis underscores the critical need for further research to explore therapeutic interventions that leverage the sleep-immune connection to improve health outcomes.
We discussed how different cytokines play a crucial role in the bidirectional relationship between sleep and the immune system. Pro-inflammatory cytokines such as IL-1β and TNF-α promote sleep, particularly NREM sleep, by acting on specific brain regions like the hypothalamus. These cytokines are typically elevated during infections and inflammatory responses, leading to increased sleepiness, which is thought to facilitate recovery. Conversely, chronic sleep deprivation has been shown to increase the production of these cytokines, contributing to a state of low-grade inflammation that can exacerbate various health conditions, including metabolic and cardiovascular diseases.
Importantly, hormones such as cortisol and melatonin are integral to the regulation of sleep and immune functions. Cortisol, a glucocorticoid hormone released by the adrenal cortex, follows a circadian rhythm, peaking in the early morning and decreasing throughout the day. It has immunosuppressive effects, reducing inflammation and modulating immune responses. Prolonged sleep deprivation disrupts cortisol rhythms, potentially leading to immune dysregulation and increased susceptibility to infections. Melatonin, produced by the pineal gland during darkness, supports immune function by enhancing the activity of NKs and T lymphocytes. It also possesses antioxidant properties that protect immune cells from oxidative stress.
Nevertheless, neurotransmitters, like serotonin and gamma-aminobutyric acid (GABA), are pivotal in the sleep-immune interaction. Serotonin, primarily known for its role in mood regulation, also influences immune function by modulating the activity of various immune cells, such as T cells and macrophages. It helps regulate sleep by converting to melatonin in the pineal gland. GABA, the primary inhibitory neurotransmitter in the CNS, promotes sleep by reducing neuronal excitability. It also affects immune function by inhibiting the release of pro-inflammatory cytokines. Alterations in GABAergic activity due to sleep disturbances can therefore impact both sleep quality and immune responses.
As thoroughly discussed in the article, the interplay between sleep and the immune system is inherently bidirectional. Immune activation, through cytokine release, can alter sleep patterns, increasing the need for restorative sleep during illness. Conversely, adequate sleep enhances immune surveillance and response, facilitating efficient pathogen clearance and immune memory consolidation. This dynamic relationship underscores the importance of maintaining healthy sleep patterns for optimal immune function. The common mechanisms discussed have significant implications for understanding the pathogenesis of various diseases. For instance, chronic sleep deprivation-induced inflammation is linked to the development and progression of metabolic disorders, cardiovascular diseases, and neurodegenerative conditions. Understanding these mechanisms provides insights into potential therapeutic targets, such as cytokine modulation, hormone regulation, and neurotransmitter balance, to mitigate the adverse effects of sleep disturbances on health.
Strengths and Weaknesses of this Review
One of the key strengths of our review is the comprehensive synthesis of recent findings on the interplay between sleep and the immune system. By integrating a wide range of studies, we provide a detailed overview of the roles of cytokines, hormones, and neurotransmitters in this interaction. Our systematic approach to literature selection ensures that the most relevant and up-to-date research is included, enhancing the robustness of our conclusions.
However, there are also some limitations. Despite our efforts to be thorough, some relevant studies may have been inadvertently excluded due to search strategy constraints or publication bias. Additionally, the inherent variability in study designs, populations, and methodologies among the reviewed studies presents challenges in drawing definitive conclusions. Potential biases in the selected studies, such as small sample sizes or lack of longitudinal data, may also influence our findings. Future research with standardised methodologies and larger, more diverse populations will be crucial to further validate and expand upon our conclusions.
Conclusion and Future Directions
In the immunological processes, maintaining sleep cycle patterns, circadian rhythm plays a major role. It also plays an essential role in determining the bidirectional communication established between the immune system and the CNS via shared signals (such as neurotransmitters, hormones, and cytokines) and by the ANS in the form of direct interventions. Many immune functions work in tandem with the 24-hour circadian rhythm and sleep, thus showing a relation between the sleep and sleep-wake cycle with the immune system. The immediate effector cells of the immune system, such as cytotoxic NK cells and terminally differentiated CTL are most active during the awake period of circadian rhythm to allow an immediate response to any pathogen which can be virulent or any other form of antigen. This also allows for faster repair of the damaged tissue due to the activity during the wake cycle. Adaptive immunity is generally more active during the night as the undifferentiated or less differentiated cells like naïve, and memory T cells peak during the night. During the nighttime sleep and especially the SWS phase of sleep, the anti-inflammatory action of cortisol and catecholamines are at the lowest level. In contrast, nighttime sleep promotes the release of GH and prolactin. The endocrine milieu during early sleep critically supports the enhanced production of IL-12 and increases the interaction between APC and T cells as shown by the evidence. The cytokine balance shifts towards Th1 Cytokines. Th1 cell proliferation is increased. There’s a possibility that it might also facilitate the migration of naive T cells to lymph nodes. The endocrine milieu thereby supports longer-lasting immune memory responses during early sleep stages (because Th1 endorses the formation of long immunological memories). Chronic lack of sleep leads to stress and causes the release of persistent unspecific pro-inflammatory substances, which can best be described as chronic low-grade inflammation and produces immunodeficiency, which is detrimental to health.
Although the exact relationship between the activation of adaptive and innate immunity with the circadian rhythm is unknown, we know that innate immunity is active during the day and adaptive immunity is active during the night. The exact mechanism of interaction with the immune system, endocrine system, and CNS has to be uncovered so that we can understand and develop medicines that act with best efficiency according to the circadian rhythm.
This review uniquely consolidates recent findings on the intricate crosstalk between sleep and the immune system, providing a holistic overview of how sleep influences immune function and inflammatory homeostasis. Our synthesis highlights novel insights into the role of sleep in modulating specific cytokines, immune cell activity, and the gut microbiome. Additionally, we explore the bidirectional nature of sleep and immune interactions, emphasising the implications for lifestyle-related diseases. By integrating these diverse aspects, our review offers new perspectives on potential therapeutic approaches and underscores the critical importance of sleep in maintaining immune health and preventing chronic diseases.
Abbreviations
APCs, antigen-presenting cells; ANS, autonomic nervous system; REM, rapid eye movement; NREM, non-rapid eye movement; SWS, slow wave sleep; EEG, electroencephalography; EMG, electromyography; EOG, electrooculography; WBCs, white blood cells; PRPs, pattern recognition receptors; pDC, plasmacytoid dendritic cells; NK, natural killer cells; CTLs, cytotoxic T lymphocytes; CNS, central nervous system; PGs, prostaglandins; DC, dendritic cells; SCN, suprachiasmatic nuclei; HPA, hypothalamic-pituitary-adrenal; TNF, tumor necrosis factor; SNS, sympathetic nervous system; IL, interleukin; GH, growth hormone; ROS, reactive oxygen species; LPS, lipopolysaccharide; HEVs, high endothelial venules; NSAIDs, non-steroidal anti-inflammatory drugs.
Footnotes
Acknowledgement
JKS and SG acknowledge the research support from International Brain Research Organisation (IBRO).
Author’ Contribution
The conceptualization was done by KKS, SG, AB and JKS. The initial draft was written by AB, KKS and SG. The later version and diagrams were compiled and completed in its final form by all the authors.
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship and/or publication of this article.
Funding
The authors received no financial support for the research, authorship and/or publication of this article.
ICMJE Statement
All authors have contributed significantly in manuscript preparation and submission.
Statement of Ethics
Not applicable.
