Abstract
Background
Hypertension (HTN) has a genetic predisposition and it also impairs microcirculation, thereby, affecting the well vascularized structures like the brainstem and causing changes in Brainstem Auditory Evoked Potentials (BAEPs).
Purpose
To find out the usefulness of BAEPs as a screening tool in apparently healthy individuals with a family history of HTN.
Methods
One hundred and ten volunteers, aged 17 to 23 years, were enrolled in the study as participants with proper consent. After excluding the subjects with existing diseases or co-morbidities (e.g. diabetes, HTN, schizophrenia, neuropathy, etc.), those on ototoxic or neurotoxic drugs, a preliminary physical examination was performed, following which BAEPs were recorded with a proper device. Statistical analysis is done with SPSS 2016 software using the chi-square test.
Results
A consistent distortion in the inter-peak latency of III-V waves is noted when a family history of HTN is present in either parent or maternal grandparents. Other statistically significant findings are present in V/I% (HTN in mother), wave I (HTN in paternal grandfather), wave III (HTN in maternal grandfather), and inter-peak latency I-V (HTN in maternal grandmother).
Conclusion
BAEP may be used as a screening tool in individuals with a family history of HTN with supportive evidence from further studies in the near future.
Introduction
The impairment of cochlear microcirculation is the most frequently cited pathophysiology for sudden sensorineural hearing loss (SSNHL). 1 Cochlea, supplied by the labyrinthine artery, is highly susceptible to ischemic or hypoxic damage as it has high metabolic activity. Hence, the etiology of SSNHL must focus on cardiovascular risk factors like hypertension (HTN), 2 and metabolic syndrome is an independent risk factor for SSNHL, vertigo, and total hearing loss being poor outcomes of it. 3 According to the NCEP ATP III definition, metabolic syndrome is present if three or more of the following five criteria are met: waist circumference over 40 inches (men) or 35 inches (women), blood pressure over 130/85 mmHg, fasting triglyceride (TG) level over 150 mg/dl, fasting high-density lipoprotein (HDL) cholesterol level less than 40 mg/dl (men) or 50 mg/dl (women) and fasting blood sugar over 100 mg/dl. The blood supply through the labyrinthine artery may be compromised, thus, reducing the oxygen tension in cochlear fluids and lymph which may result in SSNHL. 4
Family history of HTN influences end organ damage even after blood adjustment, the notable ones being stroke and intracerebral hemorrhage. 5 Complex modeling of blood pressure in families suggests the inheritance of genes that leads to a steeper rise in blood pressure with age.6, 7 The prevalence of HTN progresses from 7.2% in those aged 18 to 39 years up to 30.1% in the age group of 40 to 59 years and then to 65.4% in 60 years old people and above. 8
Keeping the inheritance pattern and deadly long-term complications of HTN in mind, we aim to establish Brainstem Auditory Evoked Potential (BAEP) as a screening test for young individuals with a family history of HTN considering the fact that HTN can result in sudden hearing loss.
Methods
The cross-sectional case-control study, which was conducted between January 2019 and July 2019 was approved by the Institute Ethics Committee. As for the subjects for this study, apparently healthy MBBS students from IMS BHU, about 110 of them, were taken, and their BAEP waves and inter-peak latencies were analyzed. It was based on the statistical data available that the sample size was chosen. Family history of HTN was confirmed verbally and relevant history with respect to their lifestyle was also recorded.
Inclusion criteria of subjects: Non-diabetic medical students of age group 17 to 23 years
Exclusion criteria of subjects:
Presence of Diabetes, HTN, or other co-morbid conditions leading to neuropathies. Subjects with neurodegenerative diseases. For example, Parkinson’s disease and Alzheimer’s disease. Subjects with hearing disorders or a family history of the same. Use of ototoxic and sedative drugs. For example, Antipsychotics, Antidepressants, Methyldopa, Reserpine, Phenytoin, and so on. Subjects with psychiatric disorders. Strokes, severe head injuries. Subjects with peripheral neuropathy.
Peripheral neuropathy was ruled out by performing various tests. Besides a pressure test with the back of a pencil, proprioception (sense of the position of joints), both proximal and distal, were tested by asking the subject to keep his eyes closed, followed by rotating a limb in various directions, allowing it to stay in that particular direction and then finally asking the subject to place the other limb in the same position without actually seeing the position of the former limb. Several other tests, including a pain test using a pinprick and tendon pinch, tactile localization and discrimination, and temperature tests using warm and cold objects, were also performed.
Measurement of the body height of the subjects was taken by asking the subjects to stand firmly on the ground against the wall and the height was noted by a measuring scale fixed to the same wall, after sliding a flat object down up to the head.
A digital device was used to take the weight. By dividing the weight in kilograms by the square of height in meters, the BMI of the subjects was calculated. The respiratory rate was counted. Using the radial arteries, the pulse was counted bilaterally and all parameters were noted. Blood pressure was noted using a sphygmomanometer. BAEP was carried out with a proper BAEP device called BERAGRAPH (Medical Systems, 389, Industrial area, Phase-II, Chandigarh) under standard conditions. After directing the subjects to be comfortable, the skin of the forehead and both the mastoid were made grease free. The subject was asked to give up any jewelry, cell phones, or other devices that could hinder the process. While the active electrode was placed on the vertex, the placement of the reference electrode was made on the mastoid and that of the ground electrode was made over the forehead. The headphone was in position, the low filter was 100 Hz and the high filter was 10 kHz. Brief click monoaural stimuli were used at 55 dB 2,000 times (11 per second) and the wave pattern was noted.
The normal range of sound perception of an apparently healthy individual is approximately from 20 to 80 dB with slight individual variations, provided the perception is not that of noise. Fifty-five decibel lies within this favorable range, thus, 55 dB has been used to avoid subjective bias. We recorded all waves in the rarefaction setting. The room was soundproof. At least two readings from each ear were taken to confirm the reproducibility of the waveform; the absolute latencies of waves I-V and inter-peak latencies I-III, I-V, III-V were recorded along with V/I ratio percentage (V/I %). The entire process is conducted after taking proper consent from the subject. The following parameters are recorded during the BAEPs study:
Wave I: Acoustic nerve (1.4–1.8 ms)
Wave II: Cochlear nucleus (2.8 ms)
Wave III: Superior olivary nucleus (3.6–4.1 ms)
Wave IV: Nucleus of the lateral lemniscus (5.1 ms)
Wave V: Inferior colliculus (5.5–6.0 ms)
Wave VI: Medial geniculate body
Wave VII: Originates between medial geniculate body to auditory complex 8
Inter-peak latency I-III: 1.6–2.6 ms
Inter-peak latency I-V: 3.5–4.5 ms
Inter-peak latency III-V: 1.4–2.4 ms
Normal V/I %: 50%–300%
Statistical analysis was done using SPSS 2016 software trial version by chi-square test.
Results
History of HTN in Father
No significant association was found in subjects with a family history of HTN in the father with the BERA waves I, III, V; inter-peak latencies I-III, I-V, and III-V (left ear) and also with V/I ratio.
A total of 94 subjects (85.5%) have a positive history of HTN in fathers while the rest 16 (14.5%) do not.
According to Table 1, the proportion of individuals showing normal latency is much higher in those without a family history of HTN in the father (93.6%) in comparison to those with a family history (75%). Out of the total subjects in the group with family history, 6.2% showed decreased inter-peak latency while 18.8% showed increased interval. The results are statistically significant (p = 0.011).
Inter Peak Latency Between Wave III and Wave V of Right Ear (III-VR).

History of HTN in Mother
No significant association was found in subjects with a family history of HTN in mothers with the BERA waves I, III, V; inter peak latencies I-III and III-V and also with V/I ratio (right ear).
One hundred and three (93.6%) subjects lacked a history of HTN in their mother while the other seven possessed it (6.4%).
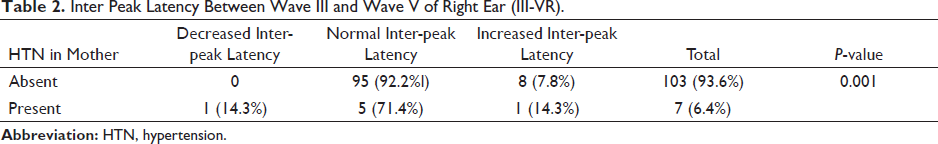
According to Table 2, a significantly higher proportion of individuals show normal inter-peak latency between the I and V waves of the right ear (92.2%) if they do not have a history of HTN in the mother, having which the percentage drops to 71.4%. Equal proportions of subjects show increased and decreased latencies (14.3% each) in those with the stated family history.
Inter Peak Latency Between Wave III and Wave V of Right Ear (III-VR).
According to Table 3, a significantly higher proportion of individuals show a normal time interval between the III and V waves of the left ear (96.1%) if they do not have a history of HTN in the mother, having which the percentage drops to 85.7%. A 14.3% of individuals show decreased latency among those with HTN in mothers.
Interval Between Wave III and Wave V of Right Ear (III-VL).

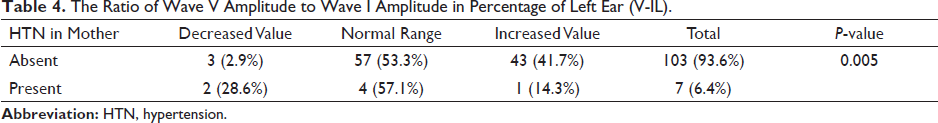
According to Table 4, the proportion of individuals with normal values is almost equal. Those without a history of HTN in mothers show an increased value of V/I%L in a greater proportion (41.7%) when compared to the other group (14.3%). A 28.6% of subjects among those with a history of HTN in mothers show a low value and a lower proportion (14.3%) show an increased value. The results are statistically significant.
The Ratio of Wave V Amplitude to Wave I Amplitude in Percentage of Left Ear (V-IL).
Family History of HTN in Paternal Grandfather
No significant association was found in subjects with a family history of HTN in the paternal grandfather with BERA except wave I of the right ear.
One hundred and nine (99.1%) subjects do not have any history of HTN in paternal grandfather while only one subject (0.9%) has a positive history.
According to Table 5, the only subject with a positive family history showed increased latency of wave I in the right ear. Among the other subjects without a family history, 56 (51.4%) had increased latency, 40 (36.7%) had normal latency and 13 (11.9%) had increased latency.
Wave I of Right Ear (IR).

Family History of HTN in Paternal Grandmother
No significant association was found in subjects with a family history of HTN in the paternal grandmother with BERA.
Family History of HTN in Maternal Grandfather
No significant association was found in subjects with a family history of HTN in maternal grandfather with BERA waves I, III (left ear), V; inter-peak latencies I-III, I-V, III-V (left ear), and V/I% ratio.
One hundred and six (96.4%) don’t have a history of HTN in their maternal grandfather, and four (3.6%) have it.
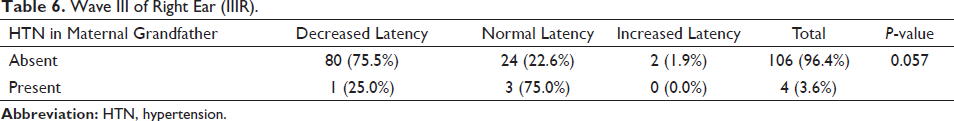
According to Table 6, the proportion of subjects in the decreased latency range of the III wave of the right ear is almost triple in the case of subjects without a positive family history of HTN in the Maternal grandfather (75.5% as compared to 25.0%). Normal latency was almost three times more in the subjects with a positive family history of the same (75% as compared to 22.6%). No subject with a positive family history showed increased latency while only two subjects showed increased latency in the other group. The findings are nearly statistically significant.
Wave III of Right Ear (IIIR).

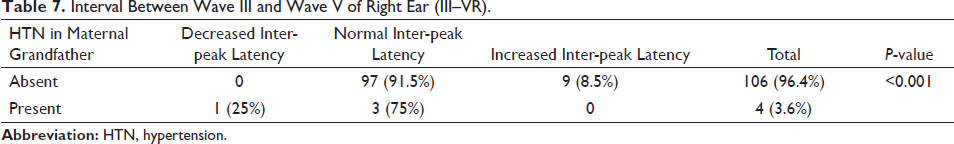
According to Table 7, a significantly high proportion of subjects have normal inter-peak latency when they don’t have the history (91.5%) as compared to those with the history (75%). Only one subject shows decreased latency who belongs to the group with positive family history. Nine (8.5%) subjects have increased latency and they belong to those without a family history. The results are statistically significant.
Interval Between Wave III and Wave V of Right Ear (III–VR).

Family History of HTN in Maternal Grandmother
No significant association was found in subjects with a family history of HTN in maternal grandmother with BERA waves; inter-peak latencies I-III, I-V (left ear), III-V (left ear), and V/I% ratio.
One hundred and two subjects (92.7%) don’t have this family history while eight (7.3%) have the history.
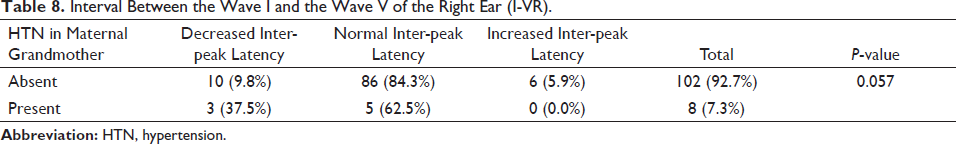
According to Table 8, the proportion of subjects within the normal range of inter-peak latency between Wave I and Wave V in the right ear is significantly more in the case of subjects without a positive family history of HTN (84.3%) as compared to those with a positive family history of HTN (62.5%). Among those with a positive family history, three (37.5%) showed decreased time intervals between the I and V waves of the right ear which is a significantly higher proportion as compared to those without the similar history, 10 (9.8%). No subject with a positive family history of HTN showed increased latency while six subjects showed increased latency in the other group. The data is nearly statistically significant.
Interval Between the Wave I and the Wave V of the Right Ear (I-VR).
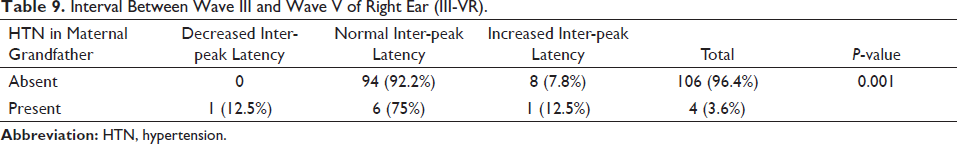
According to Table 9, a significantly high proportion of subjects have normal latency when they don’t have a history (92.2%) as compared to those with a history (75%). One subject shows increased latency (3.6%) among those who have a positive family history. Eight other subjects with increased latency belong to the group without any positive history for the same (7.8%). Only one subject shows decreased latency who belongs to the group with positive family history (12.5%). The results are statistically significant.
Interval Between Wave III and Wave V of Right Ear (III-VR).
Discussion
From the results above, we can see a consistent distortion in the inter-peak latency of III-V waves when a family history of HTN is present in either parent or maternal grandparents. This finding is accompanied by a few other findings in this study that have been mentioned.
The hypothesis which might explain the above can be stated by the authors as follows. The ascending auditory pathway through the brainstem is the one concerned with waves III, IV, and V in BAEP and this is the most consistently affected in our study. The brainstem which houses many of the critical centers in our body has a rich vascular supply. HTN, being a vascular entity, will affect those areas with rich blood supply early as compared to those with low vascularity. However, the study participants are healthy, with some having a family history of the disease. HTN has a genetic component6, 7 as well which might cause early microvascular organ damage to the highly perfused structures like the brainstem 5 that have not become clinically apparent in healthy individuals with a family history of HTN and the brainstem houses the auditory pathway. So, the auditory pathway may incur some damage without being manifested clinically and this might explain the findings in our study.
Arterial HTN causes dysfunction of the entire auditory system, more in the central auditory pathway, as per Przewoźny et al. and there is impaired sound localization, which might go unnoticed even in the eyes of the patient himself and the attending physician. 9 Some authors have even shown HTN only to be a weak risk factor for hearing loss.10, 11
Hence, we can observe that there are discrepancies in the studies performed to date and this might be attributed to confounding factors such as age and ethnicity. With further study in the near future, the evidence of the usefulness of BAEP in screening healthy individuals with a family history of HTN might be clearer.
Strengths of the study: (a) Kept the confounding factors like age and ethnicity to a bare minimum. (b) No conflict of interest. (c) Inclusion and exclusion criteria have been followed strictly to avoid any discrepancy with bias and confounding. (d) The study has been able to give an insight into the use of BAEP as a screening tool in individuals with a family history of HTN.
Limitations of the study: (a) Small sample size. (b) Subjects have been gathered from a pool of medical students only, hence a small aspect of selection bias may exist
Conclusion
BAEP may be used as a screening tool in individuals with a family history of HTN with supportive evidence from further studies in the near future since the results support that BAEP shows changes in the early life of asymptomatic individuals with a family history of HTN.
Footnotes
Acknowledgments
A token of gratitude shall be reserved for the Institute of Medical Sciences, Banaras Hindu University, and its ethics committee for its support and approval. The cooperation of all the participants was extremely crucial and the authors are indebted to each of them.
Statement of Ethics
The study was conducted after obtaining clearance from the Institute Ethical Committee of the Institute of Medical Sciences, Banaras Hindu University, dated 18th January 2019, numbered Dean/2019/EC/1028. Written informed consent was taken and confidentiality of data was maintained.
Declaration of Conflicting Interests
The authors hereby certify that the work shown here is genuine, original, and not submitted anywhere, either in part or full. All necessary permission from the participants and institution has been taken.
Funding
The authors received no financial support for the research, authorship and/or publication of this article.
Participant’s Consent
Detailed written consent from the participant was taken. The participant’s identity has been adequately anonymized. If anything related to the participant’s identity is shown, adequate consent has been taken from the participant. The journal will not be responsible for any medico-legal issues arising out of the issues of the patient’s identity or any other issues arising from the public display of information.
