Abstract
The quest to improve patient safety has become a global movement. In order to improve a culture of patient safety, it is important for medical students who will start the profession, as well as health professionals, to know patient safety before graduation. The study aims to assess the attitudes of medical students to patient safety culture and the notification of medical error. The study has been conducted with a total of 1,278 volunteer students from the Faculties of Medicine in Turkey. A web-based survey was administered to medical students. It was found that the attitudes of medical students to the culture of patient safety are generally moderate (64.06 ± 18.55 and 69.0 [IQR: 59.8–75.9]), and few of the students (32.3%) who witnessed a medical error shared the malpractice with someone. There was almost no education on patient safety during medical school. The students in the fourth grade got higher scores in disclosure responsibility compared to those in the other grades. In the study, age was significantly linearly and negatively correlated with the scores of error reporting confidence, team functioning, patient’s role in error subscales and total score. We concluded that the attitudes of medical students to patient safety culture and the notification of medical errors should be developed and supported by the faculty management. Furthermore, this study creates an awareness in terms of the application of about patient safety at training programme in medicine faculties in Turkey.
Introduction
Seeking to raise patient safety has become a worldwide movement (World Health Organization, 2011). It is important for medical students, who will begin their careers as health professionals, to know about patient safety before graduation (Rubin & Franchi-Christopher, 2002). Medical students should identify medical errors and should be educated to report them in case of encountering a medical error (Seiden et al., 2006).
The Association of American Medical Colleges emphasised that students should have the ability to describe the principles of patient safety development prior to graduating from medical faculty (Batalden et al., 2001). Based on the above justifications, significant international institutions have reached a consensus on including subjects on patient safety in medical curricula as early as possible and have issued various reports regarding this in recent years (Batalden et al., 2001; Institute for Healthcare Improvement, 2010). However, the World Health Organization (WHO) published a report for the preparation of a curriculum about patient safety in medical faculties in 2009 (World Health Organization, 2009). In line with these reports, the subject of patient safety was included in curricula of medical faculties in several countries (Bechtold et al., 2007; Patey et al., 2007). In Turkey, only a medical faculty of a university incorporated a lecture called ‘patient safety and interprofessional cooperation’ into its curriculum. As it is seen, the studies regarding this subject were limited to an elective course only at one university in Turkey.
Providing education on patient safety before starting work is important for the health systems of countries to develop a culture of patient safety accordingly and to minimise medical errors. When physicians and other health personnel have a perception towards patient and employee safety before graduation, they can protect themselves, patients/relatives and colleagues from the first time they start working against the risks of illness and occupational accidents. Today, many healthcare personnel are needed during the fight against the COVID-19 outbreak. Most countries have called on newly graduated health workers to meet the staffing needs. These newly recruited healthcare professionals found themselves in this struggle before they even gained a corporate culture. For this reason, it has become an important issue to have healthcare personnel with a patient safety culture before graduation.
Material and Methods
The study was designed as descriptive and cross-sectional using self-report questionnaires on the web.
Study Population and Sample
The study population consisted of 81 units in Turkey that have a medical school with fourth-grade, fifth-grade and sixth-grade classes. The total number of students in the specified classes of these universities was 37,964. A permission letter was sent to the medical faculties of the universities to carry out the study. Thirty-eight universities (
Data Collection Tools
In the study, ‘questionnaire on attitudes to patient safety among medical students’ developed by Carruthers et al. (2009) was used. It was determined by another study conducted between 2000 and 2013 that this questionnaire ideally measures the culture of patient safety among medical students (Chanelière et al., 2016).
The original questionnaire consists of 9 factors and 26 questions: patient safety training received to date (Factor 1), 3 questions; error reporting confidence (Factor 2), 3 questions; working hours as an error cause (Factor 3), 3 questions; error inevitability (Factor 4), 3 questions; professional incompetence as an error cause (Factor 5), 4 questions; disclosure responsibility (Factor 6), 3 questions; team functioning (Factor 7), 2 questions; patient’s role in error (Factor 8), 2 questions; and importance of patient safety in the curriculum (Factor 9), 3 questions. Eight questions in the questionnaire contain negative statements. Cronbach’s alpha value of the original questionnaire is 0.73, whereas the factor loading of each scale item varies between 0.55 and 0.82. Translation of the questionnaire into Turkish and its validity and reliability study were carried out. It was detected in the validity and reliability analyses that the measurement material generally accorded with the factor structure of the genuine scale. It was decided to exclude two questions from the 26 questions due to very low factor loadings (0.129) and the presence of a negative relationship. As a consequence of DFA conducted with 24 questions, it was identified that the factor loadings obtained were above 0.40 and the RMSEA value was at an acceptable level (between 0.05 and 0.08). Considering the sub-factors which consisted of the questions determined, and internal consistency coefficients obtained for the sum (0.650–0.845), scale result was determined to be quite reliable.
Data Collection
A web-based survey was conducted, consisting of demographic characteristics and the questionnaire via Google Forms, and the survey link was shared with the collaborators working at each medical school. All students were informed before the survey link was sent to their e-mail addresses by the collaborators. The study was conducted between May 2019 and September 2020. During the study, a total of four reminders were set for the students to participate in the study. After waiting two more months following the fourth reminder, the study was terminated, considering that there would be no more volunteers for the study.
Ethical Principles of the Research
Ethics committee approval for the research was obtained from the university (dated February 13, 2019 and No 07). Verbal consent was obtained from the participants. All procedures were applied in accordance with the principles of the Declaration of Helsinki.
Statistical Analysis
The distributions of age, duration of clinical training at the hospital in a week, duration of patient safety (PS) education during medical school, and scores of the Patient Safety Culture Attitude Scale (PSCAS) were examined using normality plots. Age and PSCAS scores were summarised by mean ± standard deviation (SD) and median (interquartile range, IQR 1st–3rd quartile); durations were summarised as median (IQR), and categorical variables were assessed by frequency (%).
The Cronbach’s
All statistical analyses were performed via IBM SPSS Statistics 22.0 (IBM Corp. Released 2013. IBM SPSS Statistics for Windows, Version 22.0. Armonk, NY: IBM Corp.). Graphs were drawn by Microsoft Office Excel 2016.
Results
In total, 44.8% (
Considering the university where students have attended, 24.57% (
The Distribution of University and the Witnessing Malpractice.
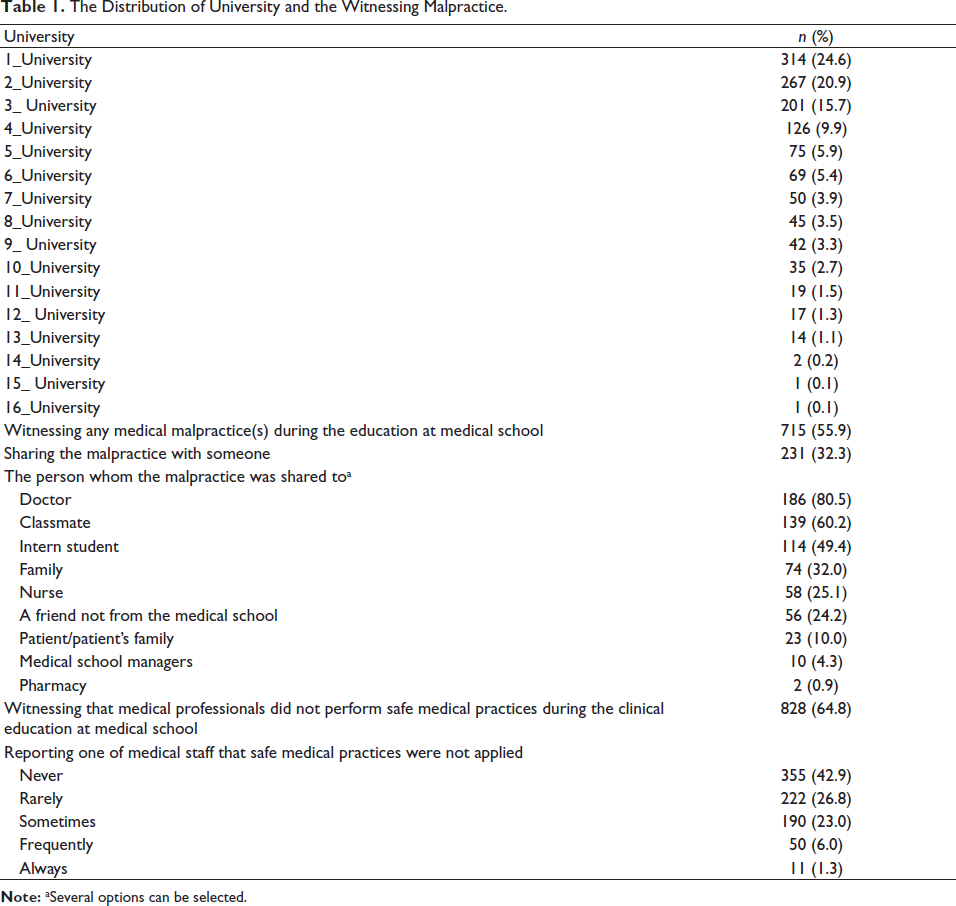
Of the participants, 54.6% (
Seven hundred and fifteen students (55.9%) have witnessed any medical malpractice(s) during their education at medical school, while 32.3% (
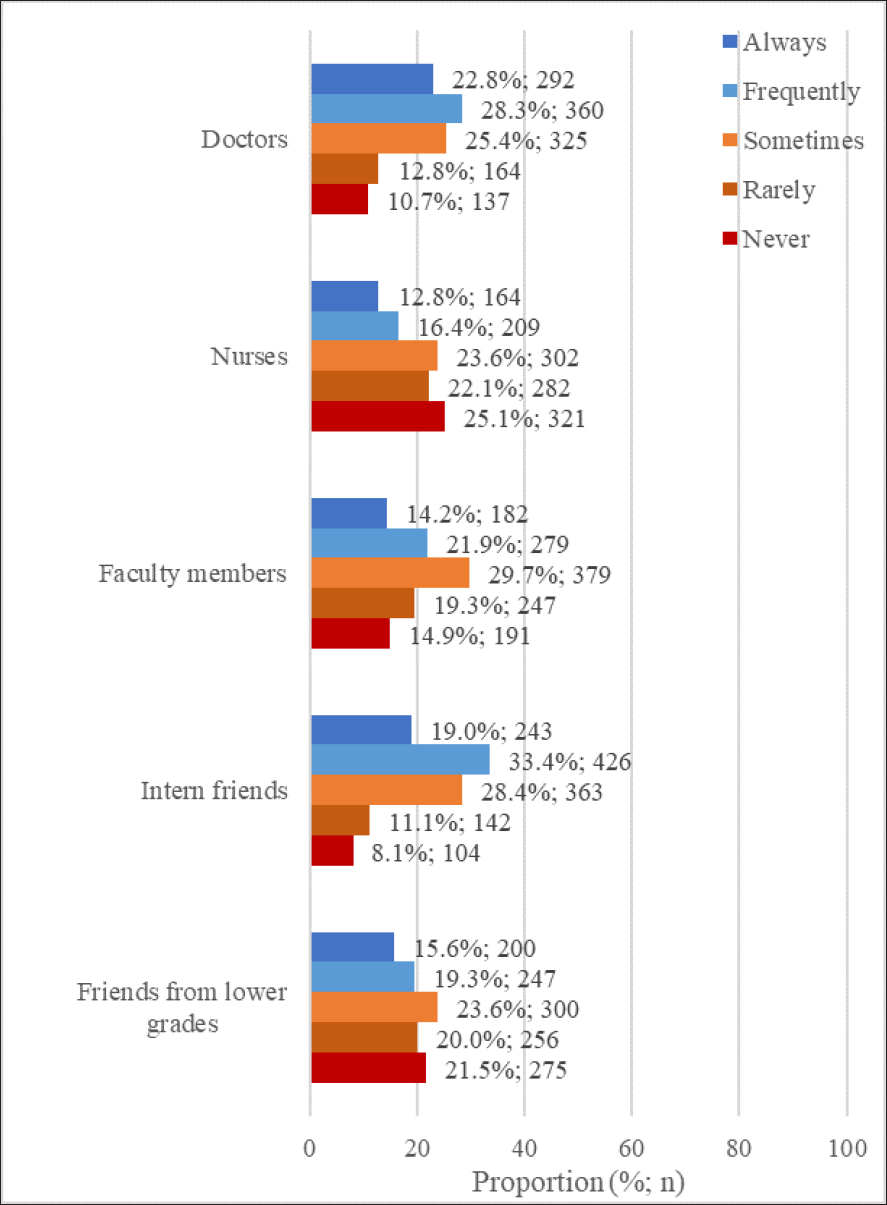
When the desire of the students’ to report the specified persons that the safe medical practices were not applied was asked, 28.3% (
The Cronbach
Comparisons of PSCAS Scores of Students Regarding the Gender.
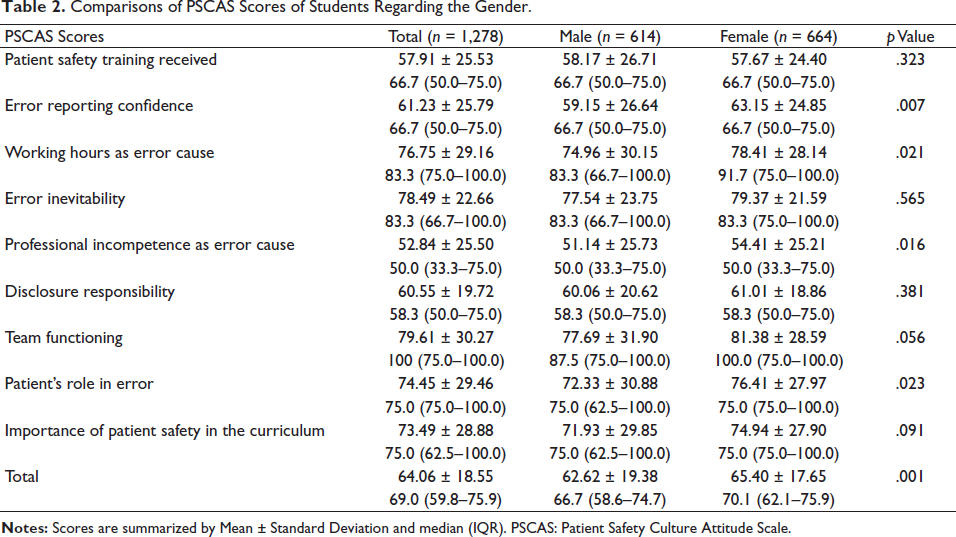
When the PSCAS scores were compared regarding the gender of the students, female students were found to have higher scores than male students for the subscales of error reporting confidence, professional incompetence as an error cause, patient’s role in error, and the whole scale (
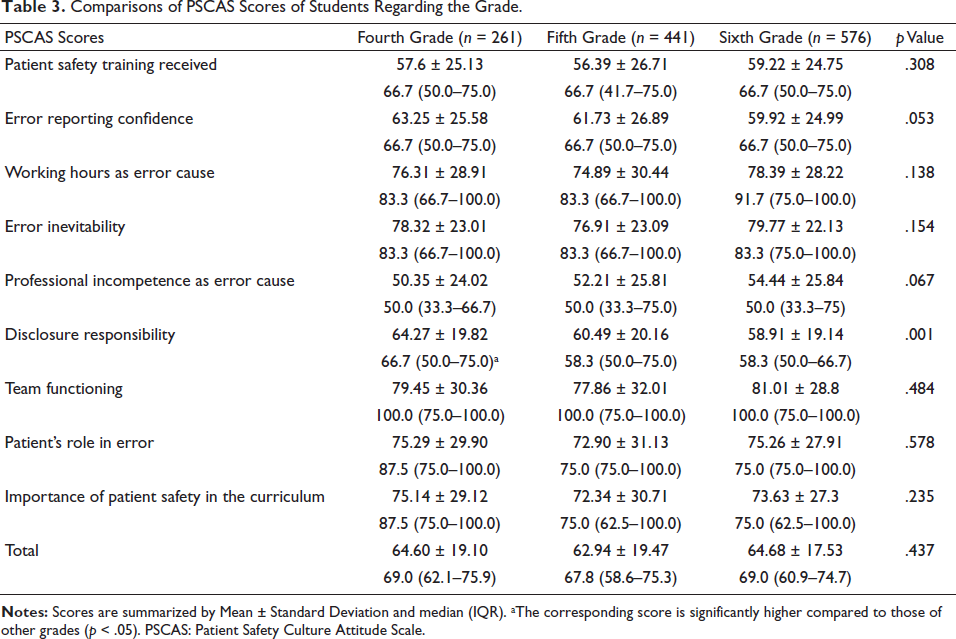
The students in the fourth grade got higher scores in disclosure responsibility subscale compared to those in the other grades (
Comparisons of PSCAS Scores of Students Regarding the Grade.
The students who received PS training during education at medical school had higher scores in the patient safety training received subscale and the total scale, compared with those who had not received any PS training (
Comparisons of PSCAS Scores of Students Regarding the Recipience of PS Training and the Witnessing Any Malpractice(s) During the Education at Medical School.
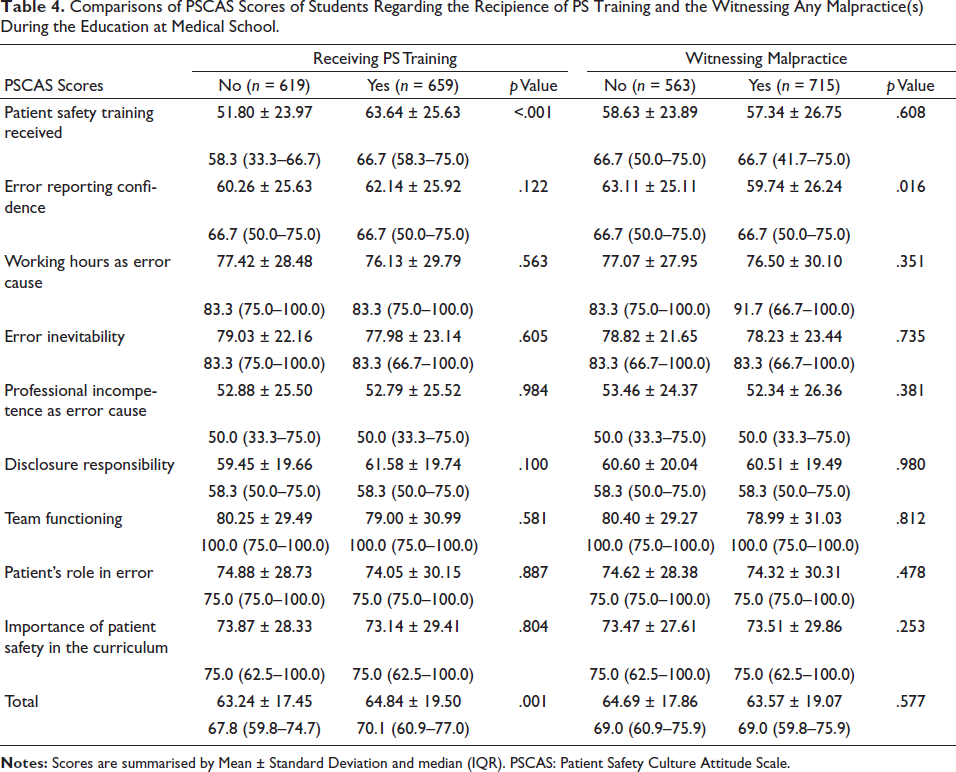
The students who had witnessed any malpractice(s) during education at medical school had significantly lower scores in the error reporting confidence subscale than those who had not witnessed any malpractice(s) (
Age was significantly linearly and negatively correlated with the scores of error reporting confidence (rS = −0.079,
Discussion
In line with the results of the study, it was found that 55.9% of the students had witnessed any medical malpractice(s) during their education at medical school, while 32.3% of them had shared the malpractice with someone. It was seen that the majority (60.2%) of the students who reported medical error(s) notified physicians. However, most (33.4%) of the students who wanted to report those who did not follow safe medical applications had the will to notify their intern friends. Among the students who witnessed that safe medical applications were not performed, the frequency of willing to report to interns was determined to be significantly lower than the frequency of willing to report to other people. Even though several students reported the medical errors they witnessed and those who did not follow safe medical applications to unauthorised people, their act of reporting the errors is important for creating a culture of patient safety (Intepeler & Dursun, 2012). Pursuant to The Joint Commission’s accreditation standards, health organisations are required to ensure the reporting of unexpected results related to the treatment of patients (The Joint Commission, 2015). Evidence collected shows that physicians and students report errors inadequately because of the possible adverse effects on relationships, as well as social habits and rituals (Kaldjian et al., 2008; Madigosky et al., 2006; O’Connor et al., 2010; Seiden et al., 2006; Wetzel et al., 2012). Therefore, the infrastructure required to encourage healthcare professionals and candidates to report medical error(s) should be established and the necessary relevant education should be provided, and communication channels should be kept open (Bell et al., 2010; Gallagher et al., 2006; Karsh et al., 2006).
In this study, it was found that the mean and median total score of PSCAS of students were 64.06 ± 18.55 and 69.0 (IQR: 59.8–75.9), respectively. Patey et al. (2007) revealed in their study that medical students have very little knowledge about patient safety. Levels of the students’ attitudes to culture of patient safety with respect to ‘team functioning’, ‘working hours as error cause’ and ‘error inevitability’ are highest whereas levels of the students’ attitudes to ‘professional incompetence as error cause’ and ‘disclosure responsibility’ were lowest.
The present study showed that female students had higher scores than male students for the subscales of error reporting confidence, professional incompetence as an error cause, patient’s role in error and the whole scale. According to this result, it can be said that female students’ perception of patient safety culture is better.
In the literature, it is stated that education is influential in raising knowledge and awareness about patient safety (Coyle et al., 2005; Gaupp et al., 2016). The students who received PS training during education at medical school had higher scores in the patient safety training received subscale and the total scale, compared with those who had not received any PS training, as determined in this study. Based on this finding, it can be concluded that providing education about the culture of patient safety to medical students is important.
In the study, it was seen that only the students in the fourth grade got higher scores in disclosure responsibility subscale compared to those in the other grades. It was seen that age was significantly linearly and negatively correlated with the scores of error reporting confidence, team functioning, patient’s role in error subscales and total score, as well. Hence, it will be more influential if education on the culture of patient safety is included in the curriculum as early as possible (Bell et al., 2010; Gunderson et al., 2009).
The students who had witnessed any malpractice(s) during education at medical school had significantly lower scores in the error reporting confidence subscale than those who had not witnessed any malpractice(s). On the other hand, it was seen that the duration of clinical training at the hospital per week was significantly, linearly, and positively correlated with the scores of the working hours as an error cause, error inevitability, and team functioning subscales, as well as the total score. The Accreditation Council for Graduate Medical Education has undertaken several reforms related to working hours of health workers to improve patient safety. There are some studies analysing the effect of these reforms on patient safety. It has been concluded, following the studies, that working hours do not have any effect on patient safety, while they have both positive and negative effects (Lee, 2015). The ‘error inevitability’ score of the students who had work experience in the health sector prior to going to medical faculty was observed to be lower. This finding makes us think that errors of the students who had work experience previously can be prevented. A comprehensive event learning system can define many fields that should be improved, and it can be related to the significant and continuous improvements in the culture of patient safety (Kusano et al., 2015). Furthermore, it has been observed in another study that the older healthcare professionals with more working experience and those with a higher education level have more patient safety knowledge (El-Jardali et al., 2014).
Conclusion
It was seen as a result of the study that the attitudes of medical students towards the culture of patient safety are generally at a moderate level, and few of the students who witnessed medical errors shared the malpractice with someone. In order to further develop students’ perception of patient safety culture, management units of the faculties should encourage students to report medical errors that they face and show exemplary attitudes towards them.
Also, it was seen that the students in the fourth grade got higher scores in disclosure responsibility compared to those in the other grades. In the study, age was significantly linearly and negatively correlated with the scores of error reporting confidence, team functioning, patient’s role in error subscales and total score. For this reason, the sooner education is started, the better it will be to create a perception of patient safety culture.
As a result of the study, it was seen that there was almost no education (they had a very short time (median 5 h) or none) on patient safety during medical school. If students who will start their careers soon after medical education receive sufficient education about the culture of patient safety before graduation, they will contribute to health facilities and the health economy by reducing the costs related to medical errors.
In addition, the causes of medical errors must be carefully analysed, and comprehensive preventive programmes should be implemented due to the financial burden of medical errors on hospitals (David et al., 2013). Health leaders and professionals focus on quality and patient safety as they have never done before, since the economics of quality have changed significantly (Andel et al., 2012).
In a study, learning and continuous improvement, hospital management support, supervisor/manager expectations, error feedback and communication, teamwork and leaving the hospital were found to be important culture determinants of patient safety (Ammouri et al., 2015). Thus, it is important that patient safety and the factors affecting patient safety are taught before graduation from the medical faculty to improve patient safety.
In the study conducted by Kirkman et al. (2015), it has been argued that, although there is an increasing tendency for the development of patient safety training given to medical students, methodological deficiencies continue, and their effect on patient outcomes should be investigated (Kirkman et al., 2015). There is a need for more research to determine whether patient safety training improves patient outcomes (DiCuccio, 2015).
Furthermore, this study is important for evaluating the attitudes of medical students towards the culture of patient safety and developing the curricula of medical faculties with respect to the culture of patient safety.
Similar to envisagement of the WHO, the conclusion of this study supports that an education programme regarding patient safety should be applied at medical faculties. It will be better to utilise the results of other research to determine whether the programme on patient safety that will be included in the curricula of medical faculties should be at a theoretical level or a clinical level.
Footnotes
Acknowledgement
The authors would like to thank the collaborators: Yeliz Kaşko Arici, Gökhan Oturak, Didem Derici, Sara Salcan, İnci Arikan, Meltem Akdemir, Cihan Fidan, Dursun Çadirci, Zerrin Gamsizkan, Ali Ceylan, Adem Doğaner, Pembe Keskinoğlu, Elif Şafak, Melih Gaffar Gözükara, Mustafa N. İlhan and Hüseyin Ali Küçük. They helped conduct surveys for students at the medical school where they worked.
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship and/or publication of this article.
Funding
The authors received no financial support for the research, authorship and/or publication of this article.
