Abstract
Problem-based learning (PBL), introduced in the 1960s, is a vital and often debated aspect of medical education. PBL is a highly effective educational method, often expressing a preference for it over traditional lecture formats. We aim to implement modified PBL in Forensic Medicine and compare the performance of II MBBS students using both traditional and modified approaches to enhance learning outcomes. A survey was conducted among 2nd MBBS students in their 5th semester to assess the effectiveness of a modified PBL approach. Utilizing a five-point Likert scale for data analysis, the findings revealed that a significant majority of students in batches C1 (45%), C2 (50%), and C3 (55.56%) believe that modified PBL is more effective than traditional learning methods. Furthermore, 60% of C1 students, 66.67% of C2 students, and 61.11% of C3 students reported improved communication skills resulting from this approach. Additionally, a notable percentage of students acknowledged an enhanced understanding of course material, with 52.50% from C1, 61.11% from C2, and 66.67% from C3 expressing this viewpoint. Modified PBL is an effective approach to enhancing student engagement and enriching education in preclinical and paraclinical sciences. It promotes interactive learning and develops essential problem-solving skills. Implementing modified PBL requires a spacious demonstration hall and a round table to foster discussions and interactions among students.
Introduction
Learning is the unique journey through which each person perceives, processes, and retains new information, shaping their understanding of the world. 1 Problem-based learning (PBL), introduced in the 1960s, is a vital and often debated aspect of medical education. 1 While discussions about its effectiveness continue, what is undeniable is the need for adaptability; no system can be perfect without modifications tailored to the unique dynamics of each student cohort and their learning environment. Challenges often stem from various constraints, such as limited resources, inadequate infrastructure, and a shortage of qualified teaching staff, particularly in specialized areas like Forensic Medicine. An article published by the World Health Organization regarding the reorientation of medical education underscores the value of PBL as a dynamic educational approach. This method involves presenting learners with real patient cases, fostering active engagement and critical thinking. It is imperative to thoughtfully select relevant issues for learning, as this selection process plays a significant role in enhancing the educational experience and effectively preparing students for future healthcare challenges. 2 Various studies have demonstrated that students perceive PBL as a highly effective educational method, often expressing a preference for it over traditional lecture formats. 3 This preference underscores the value of engaging and interactive learning experiences that promote deeper understanding and retention of knowledge. Addressing these issues is essential for maximizing the potential benefits of PBL and ensuring its success in preparing future healthcare professionals. Students engaged in PBL demonstrate a stronger emphasis on comprehension rather than rote memorization. They effectively utilize journals and online databases for information and select their own reading materials. This approach fosters greater confidence in their information-seeking skills and encourages a more thorough and analytical learning process. Furthermore, these students apply a “backward-directed” hypothetico-deductive method of reasoning. 4 They also show enhanced interpersonal skills, a deeper understanding of psychosocial concepts, and a positive attitude toward patient care.
Aims and Objective
The primary objectives of our study are established within three distinct timeframes: short term, intermediate term, and long term. The outlined goals are as follows:
Short term: We aim to implement modified PBL as an effective teaching tool in Forensic Medicine. By comparing the performance of II MBBS students using both conventional and modified PBL, we can demonstrate the benefits and improvements in learning outcomes that this innovative approach can provide.
Intermediate term: To utilize modified PBL as an effective evaluation tool for second-year MBBS students, enhancing their analytical and problem-solving skills.
Long term: To incorporate modified PBL as a foundational evaluation method in Forensic Medicine and Toxicology (FMT) as well as other paraclinical disciplines at DMIMS (DU), thereby contributing to the advancement of educational quality and patient care.
Material and Methods
Study site and population: This research was conducted at Jawaharlal Nehru Medical College, Wardha. Participants were second-year MBBS 5th-semester students. Three batches of a total number of 76 students were formed: batch C1, n = 40, C2, n = 18, C3, n = 18. All three batches were considered for our study. In the practical class, the modified PBL exercise case scenario of injury examination was given to all three groups. One faculty member as a facilitator, one professor as observer, was appointed. The participants were observed while solving the exercise in small groups and in a large group in three different practical classes. Each batch was given 40 minutes, and then participants were given a feedback form questionnaire containing 15 questions in the form of 5 Likert scale. Twenty minutes were given to the students to fill out the feedback form, and feedback was collected and data analyzed.
Data Collection Method
At the conclusion of the session, we requested that students complete a survey to assess their satisfaction with the modified PBL approach. This valuable feedback will aid us in evaluating the effectiveness of the method and identifying areas for enhancement.
Date Recording
Participants, who had firsthand experience with PBL and modified PBL, were briefed on the study’s objectives to understand their perceptions of both approaches. They were assured of voluntary participation, anonymity, and confidentiality. To encourage student responses, participants were instructed to answer freely, without hesitation. The survey questionnaire consists of 15 questions, consensus agreed upon by peers, covering key aspects of modified PBL. Participants selected one of four response options for each question: Strongly agree, Agree, Disagree, Neutral. This questionnaire aimed to elicit participants’ genuine feedback on their experiences.
Data Analysis
The data collected from students were thoughtfully analyzed using a five-point Likert scale, providing valuable insights for enhancing our programs and strategies.
Observations and Results
Our research shows that many students appreciate the seating arrangement for large groups. In fact, 55% of students in the C1 batch, 72.22% in the C2 batch, and 61.11% in the C3 batch find it to be a pleasant experience. An impressive majority of students from batches C1 (60%), C2 (72.22%), and C3 (66.67%) expressed their satisfaction with the level of interaction among group members, highlighting its adequacy as shown in Figure 1. This positive feedback underscores the value of collaborative engagement in enhancing the learning experience. Research showcases that larger group interactions significantly enhance the likelihood of achieving desired outcomes, as noted by half of the C2 and C3 batches. The undeniable advantages of modified PBL are evident, with C1 (45%), C2 (50%), and C3 (55.56%) asserting its superiority over traditional learning methods. The data further emphasizes that every group member can effectively communicate with the facilitator, highlighted by C1 (60%), C2 (61.11%), and C3 (66.67%) as shown in Figure 2. Additionally, a substantial majority—C1 (60%), C2 (66.67%), and C3 (72.22%) agreed that large group discussions lead to well-rounded conclusions. Importantly, participants also noted that modified PBL significantly enhances their communication skills, as supported by C1 (60%), C2 (66.67%), and C3 (61.11%), as shown in Figure 3. Adopting this approach can transform educational experiences for all.C1 (52.50%), C2 (61.11%), and C3 (66.67%) all affirmed that modified PBL significantly enhanced their understanding of the course material. Furthermore, the majority of students felt that this approach increased their comfort level in group work, with responses indicating C1 at 62.50%, C2 at 72.22%, and C3 at 77.78% as shown in Figure 4. This clearly demonstrates the positive impact of modified PBL on both learning and collaboration. C1 (75%), C2 (83.33%), and C3 (88.89%) all enthusiastically agree that modified PBL cultivates a meaningful, constructive thinking process. Furthermore, a notable majority of students—C1 (52.50%), C2 (66.67%), and C3 (55.56%)—clearly believe that PBL teaching surpasses traditional classroom instruction, highlighting its effectiveness in enhancing learning outcomes. C1 (60%), C2 (66.67%), and C3 (72.27%), as shown in Figure 5, found inspiration in the belief that additional trigger materials—such as photographs, video clips, and articles from scientific journals—can transform PBL into a more impactful experience.
Showing the Response to Questions 1, 2, and 3.
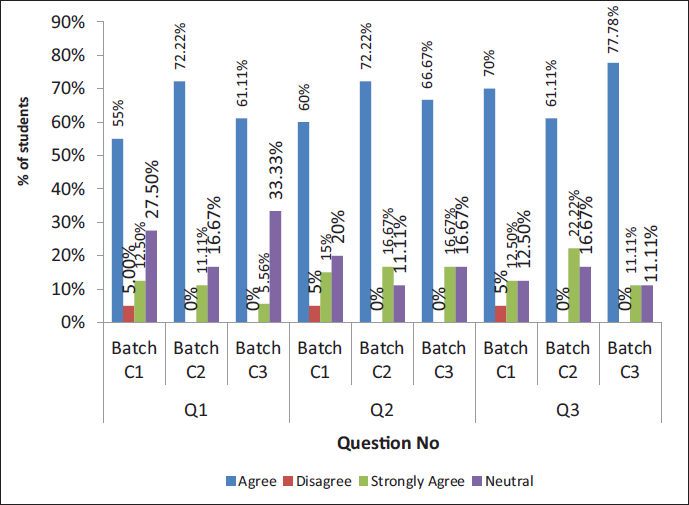
Showing the Response to Questions 4, 5, and 6.
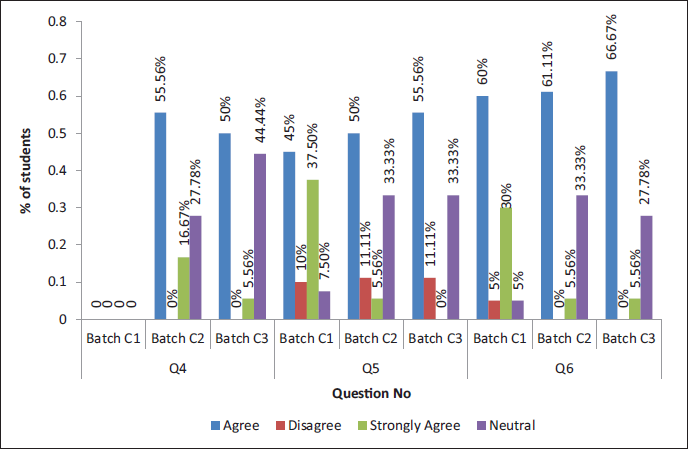
Showing the Response to Questions 7, 8, and 9.
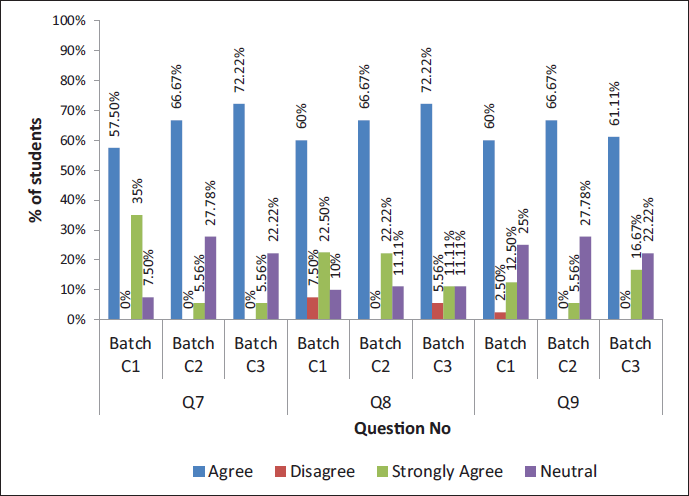
Showing the Response to Questions 10, 11, and 12.
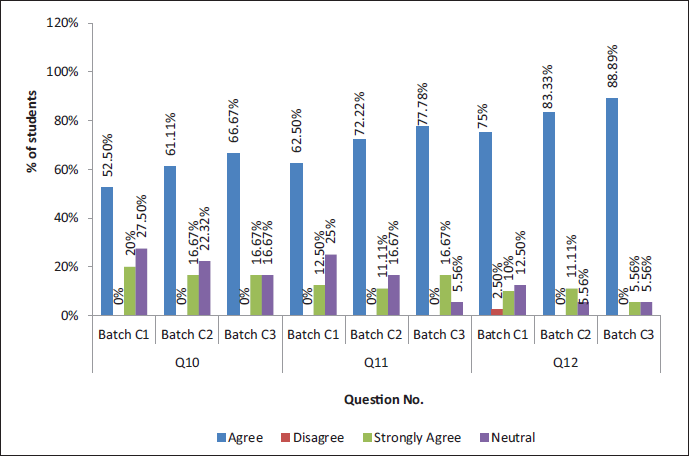
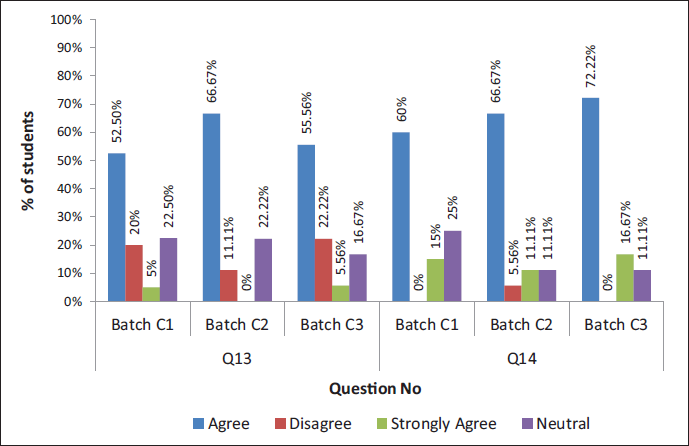
Showing the Response to Questions 13 and 14.
Discussion
A study conducted by E. Arruzza found that PBL yields statistically significant enhancements in preparedness and attitudes among medical students. 5 Globally, medical radiation students exhibit a positive reception toward PBL. However, we observed that a few areas need to be improved, such as insufficient resources, limited simulation realism, and challenges arising from group dynamics. A study by R. Hudec suggests that adopting a modified PBL approach could potentially enhance outcomes compared to traditional PBL, offering valuable insights for educational improvement. 6 These findings underscore the efficacy of PBL while highlighting opportunities for refinement. 7 The research conducted by K. A. J. Al Khaja emphasizes notable limitations in the PBL approach. Specifically, it indicates that during the pre-clerkship phase, students acquire prescribing skills to only a limited extent. 8 This finding underscores the need for further evaluation of the PBL curriculum to enhance student competencies in essential clinical skills. A study conducted by Virendar Pal Singh emphasizes the importance of incorporating PBL into the medical curriculum, particularly within the context of practical training in autopsy. 9 This method is proposed to enhance the students’ analytical skills and better prepare them for the complexities of their future medical practices. Our study indicates that PBL has the potential to strengthen students’ cognitive abilities, improve knowledge acquisition, and enhance satisfaction. Nevertheless, conducting additional research will help us better understand its full impact and effectiveness.
Conclusion
Modified PBL offers a promising approach to enhance student interaction and enrich the learning experience in preclinical and paraclinical sciences. Implementing modified PBL has the potential to greatly benefit undergraduate students, providing them with valuable skills and insights for their future studies and careers.
Challenges Faced
The implementation of modified PBL necessitates a spacious demonstration hall, complemented by a round table to facilitate discussions and promote interaction among students. This arrangement is vital for creating an inclusive and engaging learning environment.
Suggestion for Participants
To enhance the comparison of the PBL classes, it would be beneficial to schedule them on different days, focusing on the same topic. This arrangement will allow for a more thorough analysis and understanding of the differences in approach and outcomes.
Footnotes
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Ethical Approval and Informed Consent
The study commenced following the approval of the Institutional Ethics Committee (ethical approval letter no. DMIMS(DU)/IEC/2013-14/302). Participants who met the eligibility criteria were thoroughly informed about the study and included after granting verbally informed consent. We prioritized their privacy by assuring them that their data would remain confidential.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
