Abstract
Effective communication is an essential part of building and maintaining good physician-patient and physician-colleague relationships. It has been shown to significantly impact patients’ satisfaction, care, and further, to improve healthcare outcomes. The aim of the present study was to evaluate the attitude of medical practitioners in the Raichur district toward effective communication in practice. It was a cross-sectional study undertaken at the urban field practice area of Navodaya Medical College, Raichur. The study included a total of 60 medical practitioners from private and government hospitals. All participants were invited to participate in the study during December 2020. The majority of the participants have a positive opinion toward greeting the patient (86.7%), informed consent (86.7%), confidentiality (90%), and explaining the medication doses (93.4%). The age of the medical practitioners was significantly associated with effective communication skills (P < .005). Other factors like gender and years of practice were not significant. Physician communication skills are critical in gaining patients’ happiness and confidence in their doctors. Initiatives and training to generate a trained workforce might strengthen doctor-patient relationships, reducing future healthcare system disagreements and institutional mistakes.
Introduction
Communication skills are verbal and non-verbal words, phrases, voice tones, facial expressions, gestures, and body language that you use in the interaction between persons. Effective communication is an essential part of building and maintaining good physician-patient and physician-colleague relationships. It is a central clinical function in building a therapeutic relationship. A large part of a medical career involves both verbal and non-verbal transmission of information to the patient and to the nursing team and vice versa. 1
It has long been recognized that difficulties in the effective delivery of health care can arise from problems in communication between patient and provider, rather than from any failure in the technical aspects of medical care. Improvements in provider-patient communication can have beneficial effects on health outcomes. 2
Communication skills are essential for medical practice. 3 Interpersonal communication skills of physicians have been shown to significantly impact patients’ satisfaction, care and further, to improve healthcare outcomes. Even the WHO (World Health Organization) in its Global Competency Model has advised to include interpersonal skills in a credible and effective way as a core competency of a practicing physician. 4
Violence against doctors or other medical fraternities hardly made any news, and there is no discussion about this in India in medical journals. About a decade back they were probably infrequent though such violence in Western countries was known.5, 6 Traditional teaching methodologies in medical colleges give the students adequate knowledge about treatment and diagnosis but very few address communication skills and how to deal with patients. Better communication between doctor and patient builds confidence, improves compliance, and reduces mistakes and mishaps, thereby reducing malpractice suits.7–9
Association of American Medical Colleges Cincinnati, the expert panel identified seven components considered to be fundamental to all encounters between clinician and patient: build the relationship, open the discussion, gather information, understand the patient’s perspective, share information, reach agreement on problems and plans, and provide closure.4–6
The aim of the present study was to evaluate the attitude of medical practitioners of the Raichur district toward effective communication in practice and to compare the extent of communication skills with various demographic factors. There are very limited studies available on this context in Raichur district, Karnataka and the findings of this study could serve as baseline information for future studies.
Materials and Methods
Study Setting
It was a cross-sectional study undertaken at the urban field practice area of Navodaya Medical College, Raichur. Study participants were interviewed at their clinics/nursing homes. The study was conducted in December 2020. The study included all the clinical practitioners who were willing to participate in the study by giving their valid consent.
Sample Size
The study included a total of 60 medical practitioners from private and government hospitals in Raichur and their 60 corresponding patients. All doctors and patients were invited to participate in the study during December 2020.
Data Collection
The participants were requested to provide written consent and they were informed about their right to participate or withdraw from the study, and that their responses will be subjected to analysis and could be published with anonymity.
The Communication Skill Attitude Scale (CSAS) is a widely used instrument to measure the attitude of medical students toward learning communication skills and has been extensively validated. Each item in the questionnaire is accompanied by a 5-point Likert scale: 1 = “strongly disagree,” 2 = “disagree,” 3 = “neither agree nor disagree,” 4 = “agree,” and 5 = “strongly agree.”
The first part of the standardized (by asking the same questions to everyone) questionnaire for doctors included questions of socio-demographics (age, year of completion of, years of experience of medical practice, working in the government or private healthcare sector) the second part included items on communication skills (Greeting the patient on arrival, Enquiring about the name and background of, Language, patient listening and attention) and the last part included—implementation of effective communication skills (“Do you think communication skills are important for a physician?” “Do you think you should be taught communication skills as a part of your curriculum?” and “Do you think you can actually learn communication skills?”
Results
In the present study, a total of 60 doctors who were private practitioner and their 60 corresponding patients were subjects for the interview for the purpose of meeting the required objective.
Discussion
In our present study (Table 1), the majority of the participants believed that greeting the patients, enquiring to know the background history, making a patient comfortable, obtaining valid informed consent, confidentiality, and educating the patient on disease outcomes and prognosis are part of good and effective communication skills.10, 11
The capacity of a physician to speak with his patient in a nice manner is regarded as the most significant aspect of medical art, and it is essential for a physician to develop this skill. If the physician had adequate communication skills, he could get vital information regarding the patient’s physical and mental condition. The medical field in developing nations is transitioning from a physician-centered to a patient-centered approach to care. Rezaei et al. found a link between physicians’ interest in listening to their patients and patient satisfaction in their research. 10 A similar study done by Khatri R et al. in Nepal, poor communication has often been cited as one of the reasons for increased violence against both healthcare professionals and health facilities. 11
More than half of the participants in our study feel that the language barrier, being accessible to patients always, lack of time to understand the mental health of patients, and the cost of treatment underlines the effective communication between treating doctor and patient (Table 1). These findings were supported by Kumari A et al. 12
Distribution of Participants’ Responses for Improving Effective Communicative Skills Between Patient and Doctor.

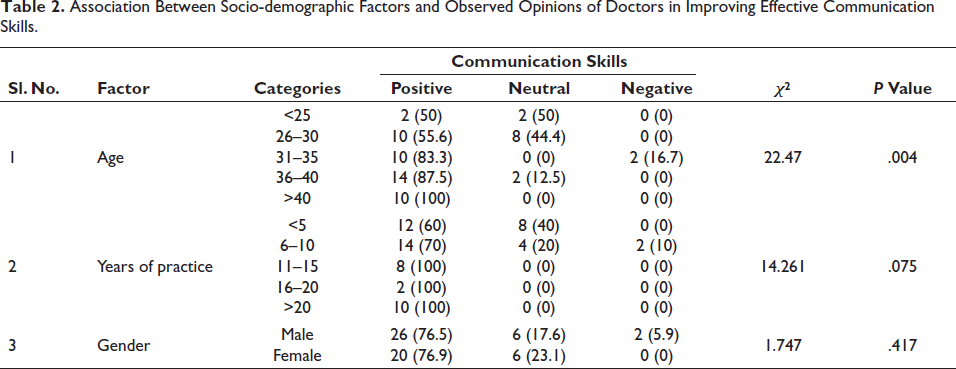
In this study, the age of the treating doctor was found to play a significant role in achieving a good and effective communication skill with patients (Table 2) (P < .05). Other factors, like years of practice or experience, gender, and place of work, were not found to be statistically associated (P > .05). A similar study done by Marambe et al. and Varna J et al. reported better communication skills among female doctors when compared to male. 13 Outside the medical context, females tend to have warmer and more engaging conversations, encourage others to open up, and express more empathy. The patient’s happiness is influenced by the explanation of the diagnostic and treatment procedure. This is consistent with the study done by Suh et al. from his research. There was also a strong link between doctors’ friendliness and patient satisfaction. 14
Association Between Socio-demographic Factors and Observed Opinions of Doctors in Improving Effective Communication Skills.
This is understandable since everyone enjoys being treated with respect. According to the findings of research done by Korsch et al., there is a substantial link between patient satisfaction and doctors’ courteous behavior. 15 Effective communication is a necessary skill for providing high-quality patient care and developing compassionate and mutually respectful patient-doctor partnerships.
According to studies, student’s communication abilities deteriorate as they become older. Medical students are more interested in medical situations and information, even though this may accidentally lead to a lack of communication skills. 16 Other studies, on the other hand, have shown no change in students’ attitudes about developing communication skills over time. 17 it is a good idea to start teaching communication skills early in the undergraduate medical curriculum. Because attitude is a learned response that can be changed, intervening early is more likely to result in quicker positive adjustments. In fact, the early years may be crucial in developing skilled and successful future doctors.18, 19
Conclusions
Physician communication skills are critical in gaining patients’ happiness and confidence in their doctors. Initiatives and training to generate a trained workforce might strengthen doctor-patient relationships, reducing future healthcare system disagreements and institutional mistakes. Because of this, favorable attitude toward developing communication skills, progressive integration of communication skills curriculum into undergraduate medical education may help to strengthen doctor-patient relationships and reduce institutional violence. Faculty development initiatives and training to generate a trained workforce in the nation might also strengthen doctor-patient relationships.
Footnotes
Acknowledgement
We acknowledge all the participating doctors of urban area of Raichur.
Data Analysis
Data were analyzed using SPSS version 21. Cronbach’s alpha was used to measure the consistency of items within the scale. Chi-squared test was done to find the association between different demographic variables and study questions with the Communication Skills Attitude Scale. The numerical values were expressed as mean ± SD and categorical variables as percentages.
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Ethical Approval
Ethical approval for the study was obtained from the Institutional Ethics Committee—Navodaya Medical College (IEC/NMC/2020/12-10).
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Informed Consent
Informed consent from the participants were taken.
