Abstract
Moral distress among nurses is well researched and well documented, but there is limited research on the moral distress experienced by care leaders, who serve as intermediaries between patient care nurses and higher levels of administration. Healthcare professionals experience moral distress daily in the context of older adult care. The aim of this scoping review was to evaluate recent literature on moral distress in older adult care with the goal of revealing how care leaders’ experiences of moral distress in older adult care have been conceptualized in earlier studies. The research questions were: How is the concept of moral distress as experienced by care leaders in older adult care defined in the existing literature? How is the concept of moral distress conceptualized in the literature? The research has been conducted in accordance with the guidelines set forth by the Finnish National Advisory Board on Research Ethics TENK. We saw that consensus on how moral distress is defined is lacking. Care leaders in older adult care experience substantial moral distress, which could be linked to the duality of their leadership role. Moral distress can be caused by a complex interplay of individual and structural factors and the challenging complex moral issues inherent to older adult care. Moral distress could impact care leaders’ emotional health, job performance, overall job satisfaction and result in higher turnover rates, absenteeism, decreased quality of patient care, and increased organizational costs. Addressing moral distress on the individual, team, and organizational levels is crucial for enhancing care leaders’ well-being and improving the overall quality of care for older adults. A focus on the identification of strategies whereby care leaders can be supported, exploration of the long-term effects of moral distress on healthcare professionals in general, and the organizational outcomes associated with moral distress should be included in future research.
Introduction
Moral distress among nurses is a well-researched and well-documented phenomenon, but there is limited research on the moral distress experienced by care leaders. Care leaders act as intermediaries between the nurses who provide direct patient care and those on higher administrative levels. Healthcare professionals experience moral distress daily in the context of older adult care, 1 and researchers have previously identified moral distress as a reason underlying why many healthcare professionals in recent years have chosen to leave their professions.2–4 In this study, a scoping review was undertaken to evaluate recent literature on moral distress in older adult care with the goal of revealing how care leaders’ experiences of moral distress in older adult care have been conceptualized in earlier studies.
Background
Moral distress can be defined as something that occurs when a person understands what the right thing to do is but is unable to act accordingly due to external obstacles. 5 Moral distress can also be defined as a psychological imbalance that occurs when healthcare professionals are aware of the ethically appropriate action required but cannot perform this action due to an external obstacle,6,7 such as power structures, legal constraints, or lack of time.6,8,9
A subjective experience, moral distress affects each individual differently. 10 While it can be considered an ethical phenomenon where ethical and moral obligations come into conflict, one can also experience moral distress without experiencing any internal conflict.11–13 Moral distress can lead to work-related stress, reduced self-esteem, or negative emotions, such as frustration, anxiety, sadness, or fear2,6–9,14,15 and also physical responses, such as loss of appetite, headaches, or fatigue. 16 Yet moral distress can even lead to positive outcomes such as professional growth, a stronger sense of responsibility for patients, or positive emotions, and improved self-reflection.11,14
Healthcare professionals often find themselves in a state of moral distress or experience a sense of unease and tension because of ethical conflicts such as an inability to act in accordance with their own ethical values.2,6,12,13,17 Ethical conflicts have become increasingly common in older adult care owing to rapidly changing healthcare environments and an increased emphasis on efficiency.9,17,18 Researchers have also found that healthcare professionals working in older adult care can experience more moral distress than those working in other healthcare settings. 19
Care leaders can experience moral distress when torn between following directives that could compromise patient care or advocating for what they believe is the right course of action. 11 The moral distress inherent to being unable to ethically respond to such challenging situations can negatively impact care leaders’ psychological and physical well-being.11,16 The moral distress that care leaders experience can be related to a lack of time, patient-related issues, relative-related issues, or other ethically difficult situations. 11 It can also arise from an imbalance between care leaders’ personal values and organizational values or other healthcare professionals’, patients’, or relatives’ values.11,15,20
Moral distress, as a result of ethical conflicts can arise when the top management introduces changes or issues directives that conflict with care leaders’ ethical values,11,18,20 and care leaders perceive that organizational responsibilities should be prioritized over their human and ethical responsibilities.6,21 Especially if there are limited resources or a limited budget, care leaders might be required to prioritize, which may conflict with meeting patients’ basic needs.16,22 The pitting of economic values against humanistic values can also lead to conflicts with care leaders’ own values.11,18
Value imbalances between care leaders and their staff can lead to care leaders’ moral distress.11,20 For example, due to staffing shortages care leaders may hire staff who lack interest in caring for older adults, thus creating a mismatch in values between those staff and the organization. 11 Even the inability to complete administrative work can increase care leaders’ moral distress, for example, if care leaders must provide direct patient care instead of focusing on own tasks due to staffing shortages. 11
However, while situations characterized by moral distress can be burdensome they can also promote professional growth and positive outcomes such as enhanced self-reflection. 14 Reflection and discussion can help care leaders learn valuable lessons and enable them to develop strategies whereby future ethical challenges can be navigated.11,23 Moral distress reduces work performance, and while the number of older adults in need of care is rapidly increasing, the number of healthcare professionals is decreasing. 2 There is an urgent need to find solutions to mitigate moral distress in older adult care. Although challenging, efforts on individual, team, and institutional levels are needed to reduce moral distress among healthcare professionals in general. 24 As shown above, new and better strategies are urgently needed to address moral distress in healthcare. 25 Knowledge about care leaders’ moral distress is necessary as this could help organizations to identify, prevent, and make it easier to manage. Doing so can improve the quality of patient care, increase care leaders’ well-being and make healthcare organizations more efficient.22,26
The aim of this scoping review was to evaluate recent literature on moral distress in older adult care with the goal of revealing how care leaders’ experiences of moral distress in older adult care have been conceptualized in earlier studies. The research questions were as follows: How is the concept of moral distress as experienced by care leaders in older adult care defined in the existing literature, and how is the concept of moral distress conceptualized in the literature.
Research design
It was determined that a scoping review was the most relevant study design. A scoping review is an overview study through which the aim is to provide a picture of the research available in a field.27,28 Scoping reviews are considered appropriate if a systematic review design does not satisfy the study purpose.27,29 A scoping review also facilitates focus on a broader question and can thus be considered preferable to a systematic review if many different study designs might be applicable.27–30 Furthermore, a scoping review can be considered appropriate when the purpose of the study is to identify knowledge gaps, examine research conduct, or clarify concepts.27–30
For the purposes of this study, the scoping review framework first described by Arksey and O’Malley 29 and further advanced by Levac, Colquhoun, and O’Brien 30 and Peters, Godfrey, Mclnerney, Munn, Tricco, and Khalil 31 was used. To effectively guide this scoping review, the Population, Concept, Context (PCC) framework recommended by the Joanna Briggs Institute (JBI) 31 was used. The PCC framework facilitates the setting of clear and meaningful objectives and eligibility criteria appropriate for a scoping review. The PCC framework can be used to identify main concepts, “break down” research questions, inform search strategies, and ensure relevant and important inclusion and exclusion criteria appropriate for the study protocol. Use of the PCC framework allows for the organization of the research around the population of interest, the main concepts, and the specific context, thus improving the clarity and focus of the study and yielding a more thorough and reliable review process. 31 The research questions were as follows: How is the concept of moral distress experienced by care leaders in older adult care as defined in the existing literature, and how is the concept of moral distress conceptualized in the literature? Seen in terms of this scoping review, the PCC framework was extrapolated as care leaders (P) experiencing moral distress (C) in older adult care (C).
The following steps were undertaken: definition of the topic; definition of the research question through use of the PCC framework; development of inclusion criteria; description of planned evidence search; identification of relevant studies; screening, organizing, and charting of the data; risk of bias appraisal; and summarization and description of the evidence so as to answer the research question. 31
Study selection
Development of inclusion criteria
To gain a current and timely overview of the research topic, studies conducted and published between 2010 and 2024 were included. The start date of 2010 was chosen because since then more perspectives and research have started to emerge on this challenging topic. Peer-reviewed and gray literature (theses, white papers, policy statements, and conference reports) were included, as well as studies in all languages to get a more reliable result.28,31 Also included were studies in which moral distress was defined, and studies in which moral distress was experienced by care leaders in older adult care.
Description of planned evidence search
The search for evidence was planned to encompass the identification of relevant studies via searches of selected databases, with the goal of retrieving all that matched the search criteria, that is, the inclusion and exclusion of studies in accordance with stated inclusion and exclusion criteria. The search included an initial review of all titles and abstracts followed by the obtaining and assessment of the full text, in line with the inclusion and exclusion criteria. Each article was then thoroughly read to determine its relevance to the stated aim of the study.
Identification of relevant studies
A literature search was conducted in accordance with Preferred Reporting Items for Systematic Reviews and Meta-Analyses Extension for Scoping Reviews (PRISMA-ScR) guidelines.
32
The databases and registers searched included Cinahl, Medline, PsycInfo, Academic Search Complete, and Web of Science. For an overview of this process, see Figure 1. Preferred Reporting Items for Systematic Reviews and Meta-Analyses Extension for Scoping Reviews (PRISMA-ScR) flow chart of the study selection.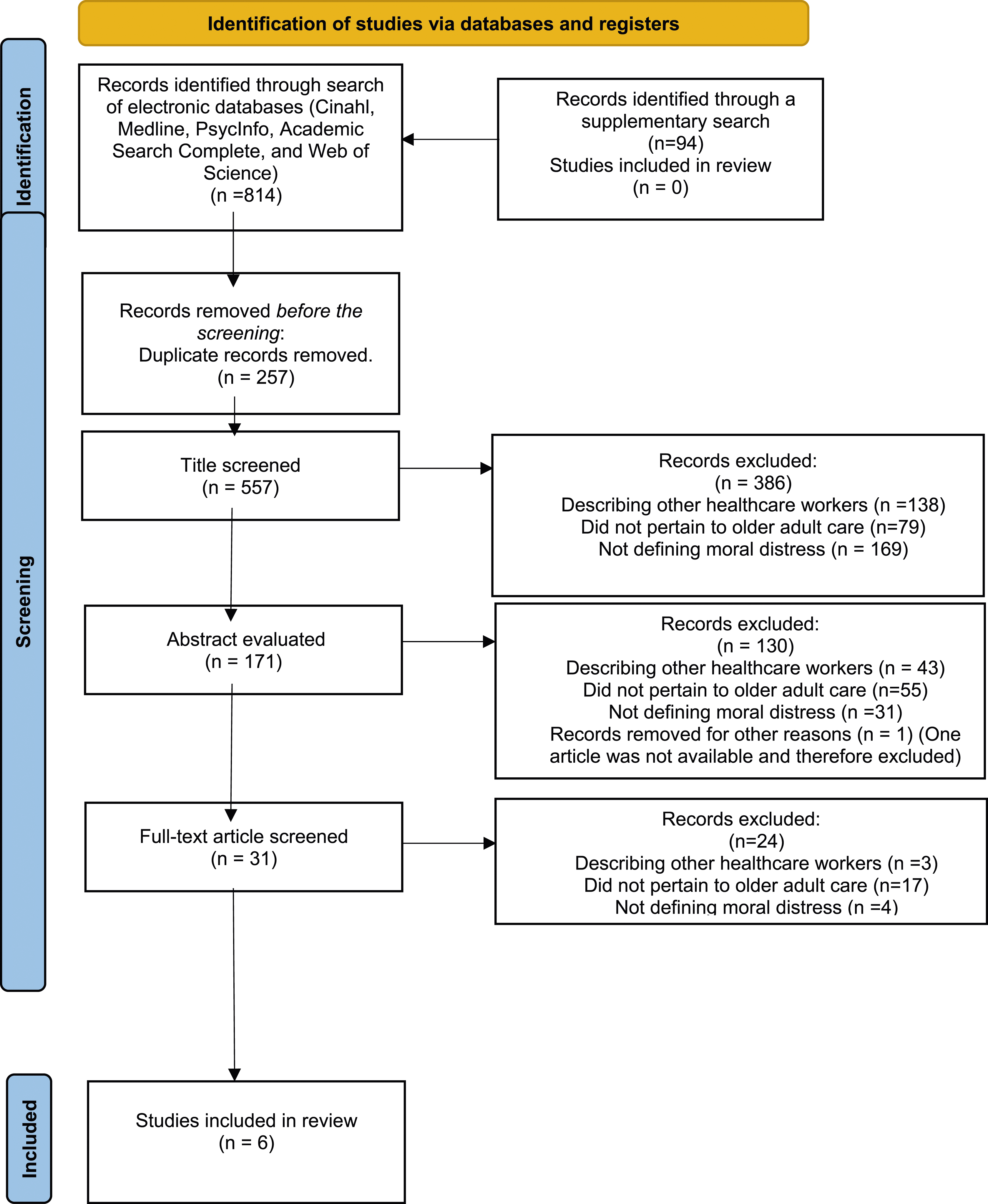
Inclusion and exclusion criteria.

Overview of the database search process.

Charting of the data
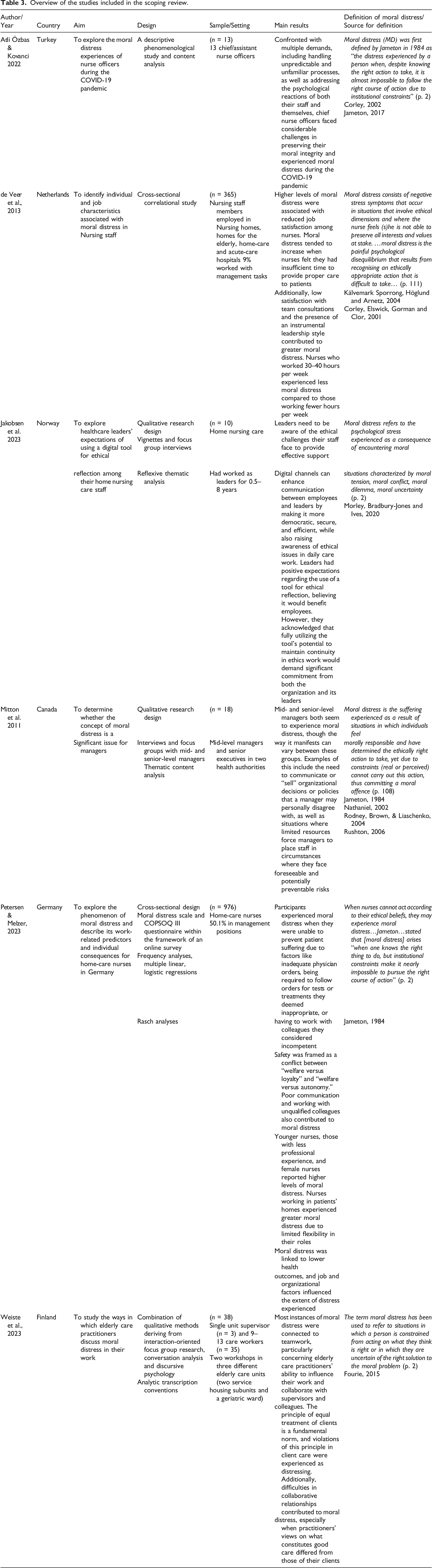
Overview of the studies included in the scoping review.
Ethical considerations
The research has been conducted in accordance with the guidelines set forth by the Finnish National Advisory Board on Research Ethics TENK 36 . This scoping review is the second sub-study in a PhD research project, with the purpose to examine the experiences of care leaders and nurses regarding moral distress in older adult care, in order to gain an understanding of the phenomenon and explore ways to reduce moral distress. Ethical approval was granted for the PhD research project by an ethical committee at a setting where the researchers are domiciled. Ethical approval was not required for this scoping review.
Findings
The aim of this scoping review was to evaluate recent literature on moral distress in older adult care with the goal of revealing how care leaders’ experiences of moral distress in older adult care have been conceptualized in earlier studies. The research questions were as follows: How is the concept of moral distress as experienced by care leaders in older adult care defined in the existing literature, and how is the concept of moral distress conceptualized in the literature.
Definition and conceptualization of moral distress
How moral distress was defined and conceptualized varied widely between the various included studies. Of the studies, Atli Özbas and Kovanci 37 defined moral distress in accordance with definitions set forth by Corley 38 and Jameton. 39 De Veer et al. 33 defined moral distress in accordance with Kälvemark Sporrong, Höglund and Arnetz 40 and Corley et al. 38 Jakobsen et al. 41 defined moral distress in accordance with Morley, Bradbury-Jones, and Ives. 42 Mitton et al. 43 defined moral distress in accordance with Jameton, 5 Nathaniel, 44 Rodney, Brown, and Liaschenko, 45 and Rushton. 46 Petersen and Melzer 34 defined moral distress in accordance with Jameton. 5 Weiste et al. 35 defined moral distress in accordance with Fourie. 12 Although definitions vary, they still have the same meaning and are rooted in Jametons’ definition: distress is experienced by a person when it is almost impossible to follow the right course of action due to institutional constraints, despite knowing the right action to take. The variations of the definitions are displayed in Table 3.
In all of the studies, moral distress was found to be characterized as negative stress symptoms that can arise when an individual recognizes the ethically appropriate action to take but feels unable to act upon said action due to different constraints.31,33,35,37,41,43,47 Negative stress was seen to be rooted in moral tension, conflict, dilemma, limitation, and uncertainty, while constraints could be institutional, organizational, or situational. Both negative stress and constraints were found to create a moral conflict that resulted in psychological stress.
In one study, moral distress was seen to arise from situations where an individual is not able to preserve all of the values and interests at stake. 33 In another study, moral distress was found to result from that care leaders must both reflect on own moral and ethical values and others’ values and choices. 35 In one study, older adult care practitioners were found to experience more moral distress than those in other sectors, which was linked to the simultaneous decrease in the number of nursing professionals and increase in the elderly population and need for care. 35
Moral distress among care leaders in older adult care
In one study, care leaders in older adult care were seen to face unique challenges concerning moral distress due to that they must navigate own ethical values while also supporting their staff 35 and aligning with organizational directives. 43 In another study, care leaders were found to often experience higher levels of moral distress compared to frontline nurses, which was attributed to care leaders’ dual responsibilities. 33 In one study, care leaders were found to not only need to manage and be aware of own moral difficulties and distress but also that of the institution and their workers. 37 In another study, care leaders were found to experience pressure to be role models in ethical situations and when undertaking ethical decisions. 41
In one study, older adult care practitioners were found to experience more moral distress than those working in other sectors, which was linked to factors specific to their work environment and patient demographics. These factors were seen to include the unique ethical challenges inherent to older adult care, organizational and resource constraints, interpersonal dynamics, and the high emotional toll of the work. Alongside observations that the care of older adult patients is charged with complex ethical issues, such as the use of coercive methods, lack of informed consent, and the need to manage differing opinions between patients and their families, care leaders were seen in this study to often encounter situations where their ethical and professional responsibilities clash, which in turn was seen to create a significant source of moral distress. 35
Causes of moral distress in older adult care
In one study, care leaders’ moral distress was found to be caused by a complicated interaction between individual and structural factors. 33 The individual factors comprised personal values, moral sensitivity, and ethical awareness, while the structural factors comprised organizational constraints, inadequate staffing, high job pressure, and conflicting interests between patient care and administrative directives.
Conflicts between organizational factors and patient needs were seen to be linked to care leaders’ moral distress in five studies.33,35,37,43 Ethical dilemmas relevant to patient autonomy and end-of-life care were found to be linked to moral distress in two studies.33,37 In four studies, care leaders’ moral distress was associated with discrepancies between patient, doctor or family wishes or when doctors/physicians act in a manner not aligned with care leaders’ own ethical values.33–35,47 In one study, moral distress was linked to the performance of managerial functions, for example, when care leaders must communicate organizational information that they do not support. 43 In four studies, the observation of colleagues’ unethical behavior or mistakes were seen to be linked to care leaders’ moral distress,33,34,37,41 while having inadequate resources or the time to provide proper care were found to be linked to care leaders’ moral distress in five studies.33–35,37,43 In one study, part-time workers were found to have a higher moral distress level than full-time workers, which might be linked to full-time workers having more knowledge and experience in ethics and being more capable of dealing with situations that can lead to moral distress. 33 In one study, the lack of opportunity and space to express ethical concerns and reflection was seen to negatively impact workers, care, and the environment. 41 In two studies, a lack of support from upper leadership, including the need to perform actions that care leaders do not support, was found to be linked to care leaders’ moral distress.35,48 In two studies, care leaders’ primary source of moral distress was found to be linked to challenges associated with the care leader (leadership) role and organizational constraints.33,37
In one study, moral distress was seen to be associated with care leaders’ perceiving a lack of understanding from higher managers and that care leaders, as middle managers, experience first-hand the issues and consequences of organizational decisions, such as budgetary decisions. 43 In one study, care leaders’ moral distress was seen to be associated with a lack of empowerment, for example, when management rendered care leaders’ decisions invalid. 37
Effects of moral distress in older adult care
The individual level
Care leaders’ moral distress was found to be linked to various negative emotions, such as anger, frustration, guilt, sadness, or powerlessness.34,35,41,43 It was also seen to be associated with significant impacts on psychological and physical well-being,34,35,37 such as burnout, depression, anxiety, headaches, or sleep disturbances.34,35,37 Severe cases of moral distress might result in hospitalization, 48 and moral distress can lead care leaders to quit their jobs.34,35
The organizational level
Care leaders’ moral distress was seen to be associated with lower job satisfaction, increased turnover rates,33,34 and higher absences due to sick leave,33,34,43 which can impact the quality of patient care 41 and increase organizational costs. Care leaders’ moral distress was even found to be linked to lower team morale, 43 a negative work environment, 41 and becoming more sensitive to future moral issues. 35 Care leaders’ moral distress was furthermore seen to be associated with the intent to leave a management position, which was linked to long work hours, heavy workload, and inadequacies. 37
Reducing care leaders’ moral distress in older adult care
The fostering of an open and supportive culture where ethical concerns can be freely discussed was seen to possibly mitigate care leaders’ moral distress, 41 likewise the promotion of teamwork and effective communication,33,35,37 and having more and broader discussions about moral dilemmas within a unit. 35 Ensuring adequate staffing to reduce time pressure, 33 the provision of ethics consultations and support programs, 48 and support in the form of guidelines and scientific information 37 were also seen to be important in the reduction of care leaders’ moral distress. The implementation of leadership styles through which support and relationship-building are emphasized over task-focused management, that is, a supportive culture, was also found to be important.33,35 Furthermore, the equal treatment of all parties, staff, patients, and family, was seen to be key to the reduction of care leaders’ moral distress. 35
Care leaders’ role in addressing and reducing moral distress in older adult care
In three studies, care leaders were seen to play an important role in addressing and reducing moral distress in older adult care, and a supportive leadership style in which care work errors are emphasized in such a manner so as to facilitate learning rather than criticism was found to lead to better communication and reduced moral distress.33,35,41 Care leaders’ encouragement of ethical reflection and discussions between staff, seen as the emotional and professional support of one’s team, was even found to help address and reduce moral distress.33,35 Also, care leaders empowering staff to act in accordance with their ethical beliefs33,35 and assisting in developing competence in moral and ethical situations 41 were seen to help mitigate moral distress in older adult care. In one study, care leaders as role models for ethical decision-making and resilience in moral and ethical dilemmas was seen to be linked to reduced moral distress, 41 while in another study seeking support and discussing moral dilemmas within the unit were found to be associated with reduced moral distress. 35
Discussion
The aim of the study was to evaluate recent literature on moral distress in older adult care with the goal of revealing how care leaders’ experiences of moral distress in older adult care have been conceptualized in earlier studies. We discerned that moral distress is a significant and universal issue in older adult care, driven by the conflict between ethical obligations and external constraints. We found that care leaders in older adult care face significant challenges when navigating ethical dilemmas, including the balancing of organizational directives with patient care needs and the management of moral tensions arising from such conflicts.
We saw that consensus on how moral distress is defined within the parameters specific to this review is lacking. Of the seven included studies, definitions of moral distress emanating from Jameton were most frequently used; Jameton’s 1984 definition was used in two studies and Jameton’s 2017 definition was used in one study. Improved clarity on the issue, including consensus on a standardized definition of moral distress and the use of theoretical frameworks, should be investigated in future research.
We found that care leaders in older adult care experience substantial moral distress, often more than their counterparts in other healthcare sectors. We discerned that care leaders’ moral distress could be linked to the duality of their leadership role; they must balance adhering to organizational policies that may conflict with own ethical values while also supporting their staff. We saw that moral distress among care leaders in older adult care can be caused by a complex interplay of individual and structural factors and the challenging complex moral issues inherent to older adult care. We also found that the effects of moral distress in the context of older adult care can lead to negative consequences on both the individual and organizational levels. We discerned that moral distress could impact care leaders’ emotional health, job performance, and overall job satisfaction and that moral distress can result in higher turnover rates, absenteeism, decreased quality of patient care, and increased organizational costs.
Moral distress is a pervasive problem in the care of older people. Although its effects are well documented among frontline nurses, the unique challenges faced by care leaders deserve greater attention. By addressing moral distress at the individual, team and organizational levels, and by addressing the root causes of moral distress, organizations can increase the well-being of both leaders and their teams as well as improve the overall quality of care for older people.
Strengths and limitations
The trustworthiness of the present study was ensured by a complementary search of all databases prior to the submission of the study. One of its strengths is the inclusion of both qualitative and quantitative studies, leading to a detailed and broader picture of moral distress. Another is that no gray literature was used, owing to a lack of such and that all languages were included in the search. One limitation may be the small number of studies included in the analysis because of the dearth of studies on care leaders and moral distress in older adult care which is why the findings and comparisons can be considered somewhat limited.
Conclusions
Moral distress is an important and common issue in older adult care, driven by the conflict between ethical obligations and external constraints. This review highlights the significant challenges care leaders face in navigating ethical dilemmas, balancing organizational directives with patients’ care needs, and managing the moral tensions that arise from these conflicts. The literature shows that there is no consensus on the definition of moral distress. Care leaders in older adult care experience significant moral distress, often more than their colleagues in the same positions in other health sectors. There is a need to develop standardized definitions and effective interventions. Future research should focus on identifying strategies to support care leaders and exploring the long-term effects of moral distress on healthcare professionals in general and the organizational outcomes associated with moral distress. To identify methods to alleviate moral distress and improve ethical competence in older adult care, an extended investigation of care leaders’ experiences of moral distress should be part of further research.
Footnotes
Author contributions
All authors (FA, MS, ATH, JH) meet the criteria for authorship. FA contributed to the study conception, background, design, data collection, realized the selection of studies, data analysis, discussion, and conclusions and drafted the manuscript at all stages. MS and JH contributed to the study conception, design, the final review of the study and provided critical comments. ATH contributed to the study conception, and the final review of the study and provided critical comments. All authors have read and approved the final manuscript.
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The authors disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This work was supported by Åbo Akademi University, Svenska Kulturfonden [grant number 206188], and Villa Ensi.
