Abstract
Objectives
Cervical cancer screening programs reduce cervical cancer mortality; however, screening engagement is not equally distributed across populations, and evidence on factors contributing to variation remains limited.
Methods
Using data from the Canadian Partnership for Tomorrow's Health (CanPath) across five regional cohorts (BC Generations Project, Alberta's Tomorrow Project, Ontario Health Study, CARTaGENE, and Atlantic Partnership for Tomorrow's Health Study (Atlantic PATH), we assessed self-reported engagement in Pap test cervical cancer screening among participants recruited between 2008 and 2016. Self-reported Pap (Papanicolaou) screening status was categorized as “never” or “ever.” Ever screening was further classified as “recent” (≤3 years) or “past” (>3 years). Multivariable logistic regression models assessed associations with screening status while adjusting for potential confounders.
Results
A total of 166,804 individuals met the inclusion criteria. Across cohorts, 162,592 (97.5%) and 4212 (2.5%) reported ever and never undergoing cervical cancer screening, respectively. Among those with a screening history, 135,823 (83.5%) were recently screened, ranging from 78% in CARTaGENE to 85% in Atlantic PATH. Nonwhite ethnicity, lower household income, single or never-married status, low physical activity, poorer self-perceived health, and ≥24 months since the last medical checkup were associated with never or past screening. Current smoking, younger age, and reproductive and hormonal factors showed differential associations between never versus ever screened individuals and past versus recent screening.
Conclusion
The national target of 80% cervical cancer screening adherence was exceeded in most regions. Persistent socioeconomic and health-related disparities highlight the need for targeted interventions. Differences between factors associated with screening initiation and maintenance warrant further investigation.
Introduction
In Canada, about 1.3% of all new female cancers and 1.1% of female cancer-related deaths are attributed to cervical cancer. 1 Standard screening programs using the Papanicolaou (Pap) test have been proven to reduce cervical cancer mortality rates. 2 Since cervical cancer is a preventable and curable disease, recently the World Health Organization (WHO) announced a global cervical cancer elimination strategy including a combination of primary prevention through human papilloma virus (HPV) vaccination coverage of 90%, cervix screening coverage of 70%, and access to treatment for 90% of precancerous and cancer diagnosed women in all countries, worldwide. 3 While provinces are transitioning to HPV-based primary screening, currently (2025) the Pap test, a cervical swab used to collect a sample of cells, is the primary recommended screening test to identify early-stage cervical cancer in Canada.1,4,5
Participation in cervical screening is not equally distributed across different populations in Canada.6–8 Studies have shown that 12–43% of Canadian women have never been screened for cervical cancer. 8 Disparities in screening uptake are multifactorial and related to personal, clinical, and sociocultural factors as well as access to healthcare services and guidelines.8–10 In two recent studies conducted by our team, using data from the Canadian Partnership for Tomorrow's Health (CanPath), we observed considerable variation in breast and colorectal cancer screening across Canadian provinces, with low household income and poor self-perceived health significantly reducing the likelihood of adherence to screening recommendations.9,10
Although the transition to HPV testing for cervical cancer screening is occurring across Canada,11,12 HPV-based screening is still too recent at a population level to understand the screening patterns to the same extent as those observed using historical Pap test data. Moreover, many barriers and facilitators to Pap test screening adherence are likely to persist in the new cervical screening program. Identifying these factors can therefore support policymakers in identifying priority populations and targeting health promotion activities. Considering the recommended five-year screening interval, it will not yet be possible to assess sustained engagement with HPV testing until approximately 2029, as the HPV-based screening program was introduced in British Columbia in 2024. Finally, although HPV testing is available, some women may still choose to undergo Pap testing collected by their healthcare provider. To address these gaps, the objective of the current study was to assess factors associated with self-reported Pap test cervical cancer screening participation across five regional cohorts contributing to CanPath.
Methods
Study population
CanPath and its regional cohorts have been previously described. 13 Using questionnaires, data on social and medical determinants of health, including age, sex, education, country of birth, race, marital status, income, self-perceived health, family history of cancer and chronic diseases, physical activity, smoking status, number of pregnancies, and history of breastfeeding, among individuals aged 30 to 74 were collected from 2008 to 2016. In this study, women aged 30 to 69 with no prior self-reported diagnosis of cervical cancer were included. Individuals with missing information on age, cancer status and/or type, and with an unknown history of cervical cancer screening were excluded.
Screening status and risk factors
To examine engagement in cervical screening, the baseline questionnaire included questions on lifetime history of cervical cancer screening, as well as the timing of the last Pap test relative to study enrollment. Cervical cancer screening status was categorized as “never screened” if participants reported no previous history of a Pap test and “ever screened” if participants reported any history of cervical cancer screening at study enrollment. Based on the screening recommendation of every three years among women aged 25 to 69 at the time of data collection, we further categorized ever screening status as “recent” with history of screening “≤3 years” if participants reported history of Pap test less than six months to less than three years ago, and “past” with history of screening “> 3 years” if participants reported history of Pap test more than three years ago.
Variable creation
As described previously,9,10 variables explored in this study were age (i.e. 30–39, 40–49, 50–59, 60–69), total annual household income (i.e. <$50,000, $50,000–99,999, ≥$100,000), education (i.e. high school or less; trade, technical school or diploma from a community college; university certificate below bachelor's level; bachelor's degree; graduate degree), marital status (i.e. married or living with a partner, divorced, widowed, separated, single/never married), ethnic background (i.e. white, black, Arab, East Asian, Latin American/Hispanic, Southeast Asian, South Asian, East Asian, Jewish, Other/Unknown), first language (i.e. English, French, other), perception of health (i.e. poor, fair, good, very good, excellent), country of birth (i.e. Canada, other), smoking status (i.e. never smoked at least 100 cigarettes, past smoker [ever smoked at least 100 cigarettes], current occasional smoker, current daily smoker), level of physical activity (i.e. low, moderate, high), presence of comorbidities, time since last routine medical checkup by a doctor or a nurse (<12 months, ≤12 to <24 months, ≥24 months), number of pregnancies (0, 1, 2, ≥3), total lifetime duration of breastfeeding (0, ≤12 months, >12 months), ever use of hormone replacement therapy (HRT) (no/yes), ever use of hormone fertility treatment (no/yes), ever use of contraceptives (no/yes), and premenopausal versus postmenopausal status.
Statistical analysis
Sociodemographic characteristics of participants stratified by study cohort at enrollment were presented as counts and percentages. Multivariable logistic regression models were used to assess factors associated with cervical cancer screening status by comparing participants who had never been screened with those who had ever been screened. Among individuals with a history of screening, additional models compared recent versus past cervical cancer screening.
In the models, only variables selected through backward elimination using a p-value cutoff of ≤0.05 were included to evaluate the association between cervical cancer screening and potential predictors. Associations were estimated as odds ratios (ORs) with 95% confidence intervals [95% CI] and corresponding p-values. All analyses were performed using SAS version 9.4 (Cary, NC, USA). Ethical approval was provided by the Health Research Ethics Board, University of British Columbia. This study is reported in accordance with the STrengthening the Reporting of OBservational studies in Epidemiology guidelines. 14
Results
Characteristics of the study participants are summarized in Table 1. From a total of 261,760 respondents at enrollment in CanPath, 166,804 individuals aged 30–69, including 18,977 (11.4%) from the BC Generations Project (BCGP), 24,291 (14.6%) from Alberta's Tomorrow Project (ATP), 84,221 (51.7%) from the Ontario Health Study (OHS), 22,193 (13.3%) from CARTaGENE, and 15,122 (9.1%) from the Atlantic Partnership for Tomorrow's Health Study (Atlantic PATH), met the inclusion criteria (Figure 1, Table 1). In total across all cohorts, 97.5% (N = 162,592) of individuals reported ever history of cervical cancer screening. Overall, among individuals with history of cervical cancer, 83.5% reported recent history of screening. The recent history of cervical cancer screening ranged from 78.9% in CARTaGENE to 85.1% in Atlantic PATH (Table 1).
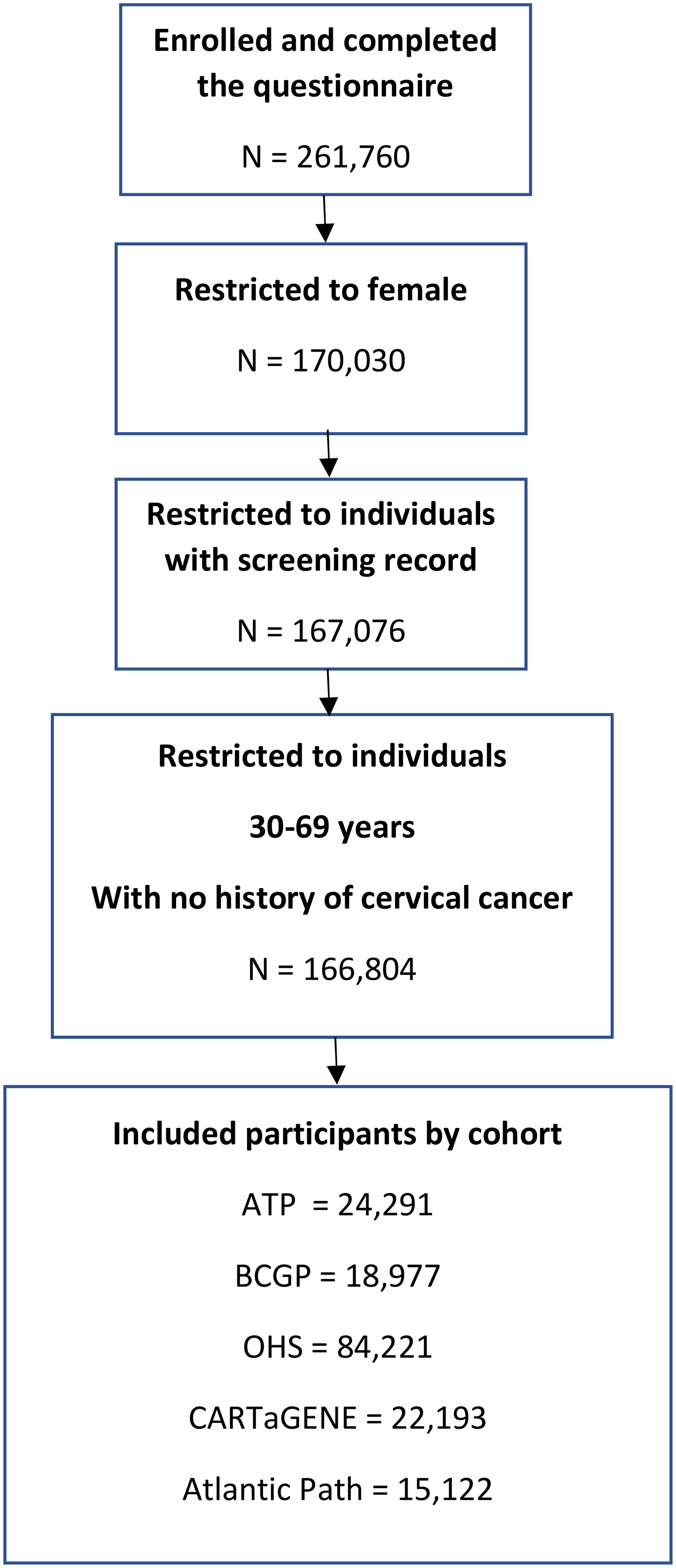
Study flow diagram.
Summary characteristics of Canadian Partnership for Tomorrow's Health (CanPath) by regional cohort.
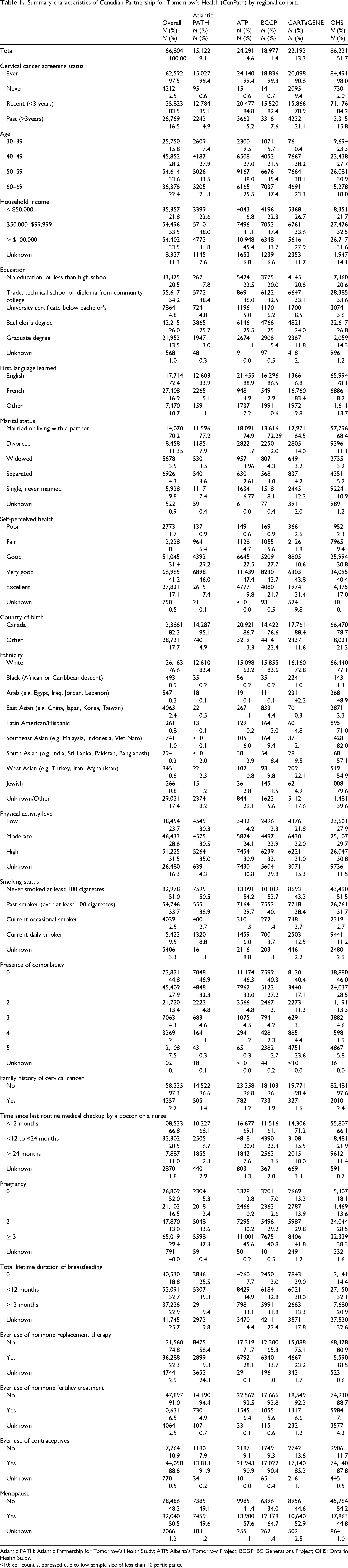
Atlantic PATH: Atlantic Partnership for Tomorrow's Health Study; ATP: Alberta's Tomorrow Project; BCGP: BC Generations Project; OHS: Ontario Health Study.
<10: cell count suppressed due to low sample size of less than 10 participants.
Across all cohorts, most participants were married or living with a partner (70.2%), were white (76.6%), and were never smokers (51.0%). Furthermore, greater proportions of participants reported household incomes ranging from $50,000 to 99,999 (33.5%), an education at the level of trade, technical school, or diploma from community college (34.2%), very good self-perceived health (41.2%), a high level of physical activity (31.5%), with no history of comorbid condition (44.8%), and less than 12 months since last routine medical checkup (66.8%). No history of pregnancy (52.0%), never use of HRT (74.8%), ≤ 12 months lifetime duration of breastfeeding (32.7%), ever use of contraceptives (88.6%), and postmenopausal status (50.5%) were most frequently reported. Across all cohorts, 2.7% of individuals reported a family history of cervical cancer (Table 1).
Table 2 presents characteristics of study participants by screening status. Overall, among never, past and recent screened individuals, 60.4%, 57.3% and 62.6% of participants were aged 40–59, respectively. A higher proportion of individuals with recent screening history reported a household income of ≥$100,000 (33.5%), an education status of Bachelor's degree or higher (27.4%), being married or living with a partner (71.3%), never smoking (52.4%), a higher level of physical activity (31.9%), good or very good self-perceived health (30.4% and 42.5%), no presence of a comorbid condition (46.6%), and <12 months since last routine medical checkup (69.9%). On the other hand, a higher proportion of women with past screening history reported postmenopausal status (70%), family history of cervical cancer (3.3%), and ever use of HRT (33.8%). Among individuals with no screening history, a higher proportion were aged 30–49 (55.6%), had a household income <$50,000 (41.0%), reported ethnic backgrounds other than white, spoke a first language other than English (70.2%), never smoked (62.7%), reported low level of physical activity (31.3%), had no comorbidities (54.3%), and had their last routine medical checkup <12 months (55.1%).
Summary characteristics of Canadian Partnership for Tomorrow's Health (CanPath) by screening status.

<10: cell count suppressed due to low sample size of less than 10 participants.
Table 3 presents predictors of cervical cancer screening engagement among ever versus never screened individuals. Overall, compared to OHS (the CanPath region with the largest number of participants), the likelihood of being never screened compared to being ever screened was lower across three regions, ranging from 30% in ATP to 50% in BCGP. In contrast, participants from CARTaGENE had substantially higher odds of being never screened compared with those from OHS (OR: 5.50; 95% CI [4.87–6.21]). Several ethnic backgrounds (Arab, East Asian, Southeast Asian, South Asian, West Asian), lower household income ($50,000–99,999), education status (less than high school), first language other than English, marital status of single or never married, reduced physical activity, poor self-perceived health status, country of birth other than Canada, no history of pregnancy or breastfeeding, never use of contraceptives and more than 12 months since last routine medical checkup were significantly associated with higher odds of never being screened for cervical cancer.
Predictors of cervical cancer screening comparing ever (reference category N = 162,592) versus never screening (N = 4212) status.
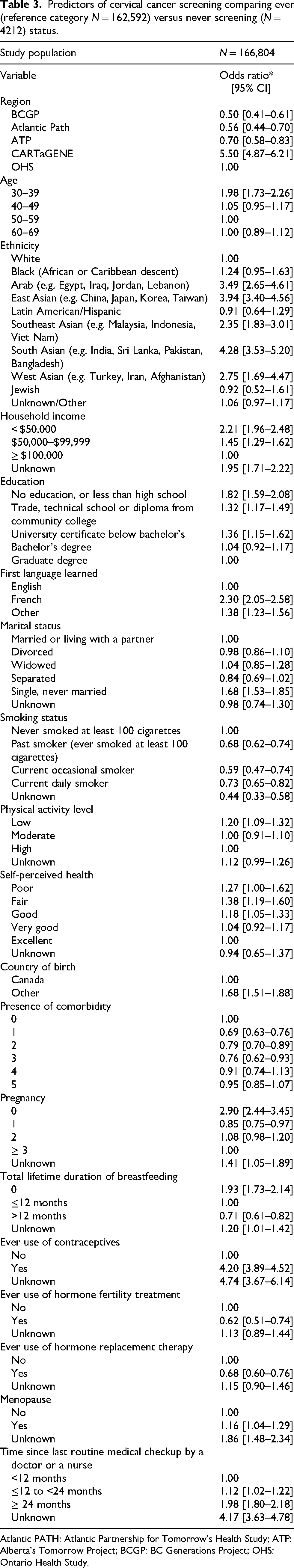

Atlantic PATH: Atlantic Partnership for Tomorrow's Health Study; ATP: Alberta's Tomorrow Project; BCGP: BC Generations Project; OHS: Ontario Health Study.
Table 4 presents predictors of cervical cancer screening engagement among individuals with past compared to recent screening status. Overall, compared to OHS, the likelihood of past compared to recent engagement in cervical screening was significantly lower across three regions, ranging from 8% in ATP to 17% in Atlantic PATH, except CARTaGENE with significantly higher odds of past screening status (OR: 1.07; 95% CI [1.00–1.14]) (Table 4). Lower household income, education status less than high school, French compared to English language, Southeast Asian and South Asian ethnic backgrounds, widowed marital status or single/never married, poor self-perceived health status, more than 12 months since last routine medical checkup, no history of breastfeeding and never use of contraceptives were significant factors associated with past cervical cancer screening.
Predictors of cervical cancer screening comparing individuals screened ≤3 years (reference category) versus individuals screened more than three years ago.
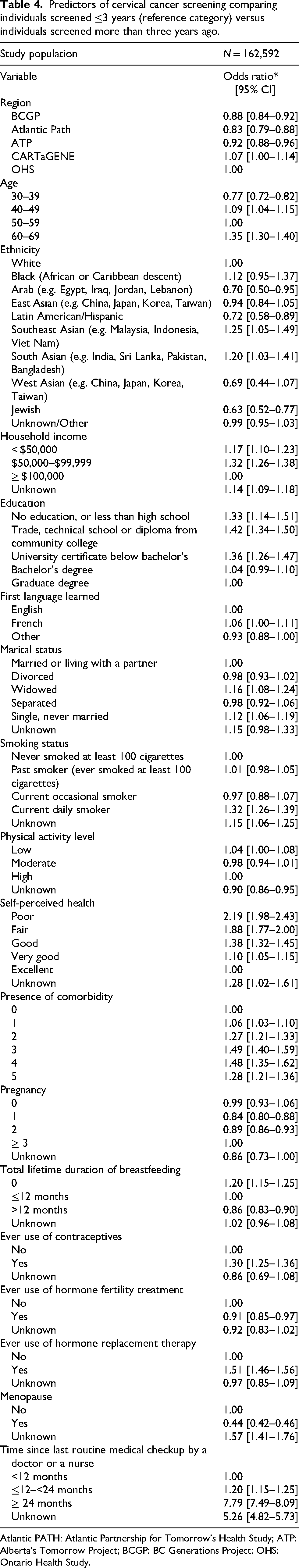

Atlantic PATH: Atlantic Partnership for Tomorrow's Health Study; ATP: Alberta's Tomorrow Project; BCGP: BC Generations Project; OHS: Ontario Health Study.
Several variables demonstrated differential associations across the two screening comparisons. In the analysis comparing individuals who had never been screened with those who had ever been screened, younger age (OR 1.98; 95% CI [1.73–2.26]) and premenopausal status (OR 1.16; 95% CI [1.04–1.29]) were associated with higher odds of never having been screened. In contrast, current daily smoking (OR 0.73; 95% CI [0.65–0.82]), having one comorbidity (OR 0.69; 95% CI [0.63–0.76]), and never use of HRT (OR 0.68; 95% CI [0.60–0.76]) were associated with lower odds of never screening (i.e. greater likelihood of ever being screened).
When restricting the analysis to individuals who had ever been screened and comparing past versus recent screening, older age (60–69 years: OR 1.35; 95% CI [1.30–1.40]), current daily smoking (OR 1.32; 95% CI [1.26–1.39]), having one comorbidity (OR 1.06; 95% CI [1.03–1.10]), and never use of HRT (OR 1.51; 95% CI [1.46–1.56]) were associated with higher odds of past screening (i.e. lower likelihood of recent screening). In contrast, postmenopausal women were more likely to report recent screening (OR 0.44; 95% CI [0.42–0.46]) compared with premenopausal women. The direction and magnitude of associations for several variables differed between the two screening comparisons (Tables 3 and 4).
Discussion
Guidelines in Canada indicate that, besides the overall screening coverage of 90%, at least 80% of eligible individuals in any identifiable group should be up to date with cervical screening. 4 In our study, we found that, with the exception of CARTaGENE (78.9%), all CanPath cohorts exceeded this target. We also found that among individuals with past screening status, social factors (namely lower household income and education status, marital status of widowed or single/never married), personal characteristics and behaviors (such as older age, current daily smoking), as well as clinical factors (including self-perceived health besides excellent, presence of comorbidity condition, more than 12 months since last routine medical checkup by a doctor or nurse, never use of HRT) were identified factors associated with cervical cancer screening recommendations. Furthermore, our findings suggest that factors associated with screening initiation may differ from those associated with adherence to recommended screening intervals among individuals already engaged in screening. While younger and premenopausal women were more likely to report never being screened, older age and smoking were associated with a greater likelihood of past rather than recent screening among those previously screened. This pattern suggests that determinants of screening uptake may differ from those affecting continued adherence to recommended screening intervals.
Our findings were similar to those reported by Datta et al. based on a study conducted among women residing in the Montreal metropolitan area in 2018. 15 In that study, about 26% of women had not been screened for cervical cancer in the past three years. 15 Not having a family physician, older age, and lower education were among the strongest predictors of not having up-to-date screening status. 15 In a recently published study assessing concurrent cancer screening participation among Canadian women, having a regular healthcare provider was also strongly associated with full participation in all screening programs (OR: 1.87, 95% CI [1.14–3.07]). 16 In a study conducted by Ince-Cushman et al. in Montreal, male primary physician sex was associated with lower cervical cancer screening. 17 On the other hand, in a study conducted by Bouck et al. in Ontario, having a male physician was associated with an increased odds of overuse and frequent order of low-value Pap tests (defined as Pap tests within seven days among low-risk primary care outpatients undergoing an annual health examination) for women younger than 21 years or older than 69 years. 18 These findings highlight the significant impact of the primary physician on an individual's cancer screening behavior. In prior research on adherence to screening programs, lack of time within medical appointments has also been found to be an important barrier to screening participation.19,20 Primary care physician encouragement has been identified as a factor that positively affects women's decision to screen.19,21 Using physician-linked notifications such as reminder letters to encourage women to screen could increase participation or retention rates within organized cancer screening programs.22–24 Hence, future studies assessing screening participation and retention rates should take into account physician-related factors, namely the number of visits, reminder mechanisms to encourage women to attend regular screening programs, as well as clear communication on screening recommendations for different age groups.
Our findings are consistent with those of other studies demonstrating that age, income, marital status, and education are associated with engagement with cervical cancer screening. In a previously published study assessing Pap test screening and its timing among immigrant women aged 21 to 69 in Ontario, using Canadian Community Health Survey data, not having a timely test was significantly associated with older age, being single, the presence of comorbidity, and low-income status. 25 Furthermore, in this study, 29% of immigrant women did not have regular access to a Pap test, and this rate increased to almost 48% among recent immigrants. In our study, adherence to screening was significantly lower among individuals with Southeast Asian or Filipino descent. In addition to ethnicity, religiosity, and women's beliefs and attitudes toward sex and cervical cancer could contribute to low adherence to the cervical cancer screening program. 26 In a mixed-method design study conducted among Muslim immigrant women in Ontario, religious affiliation and difficulty in having open dialogue about sexual activity were related to low frequency of regular physician visits and limited access to screening services, especially among patients with a male primary care provider. 26 These findings highlight the importance of clear sexual health communication between physician and patient, the availability of educational workshops about the benefits of regular screening, and addressing language barriers in screening uptake.26–28
Consistent with our findings, previous studies showed that low socioeconomic status was significantly associated with underscreening, irrespective of immigration status.6,9,10,16 In the study conducted by Adefemi et al., women with middle or high incomes were more likely to participate in screening programs compared to individuals with low incomes. 16 In general, the coexistence of factors such as low income and education status and their potential impact on women's beliefs and attitudes toward healthcare-seeking behavior could hinder adherence to the screening programs and should be considered while implementing new screening programs in Canada. 16
Our results provide further evidence of the strong association between screening engagement and age. Our findings demonstrated that the odds of being recently screened decreased with increasing age, with the lowest rate of 22.4% among individuals aged 60–69. Previous studies have reported that patients without a timely Pap test were more likely to be older.6,29 In a qualitative study conducted in the United Kingdom exploring barriers to cervical screening in women over the age of 50, considering the age-specific characteristics and needs of older participants, including their lifestyle choices, availability of easy and fast appointment systems, physical and emotional supports, as well as physician knowledge of menopause were among contributing factors for adherence to cervical cancer screening. 29
Our findings provide additional insight into differential associations for certain factors that determine screening initiation versus those influencing screening maintenance. Consistent with previous studies, sociodemographic determinants associated with never having undergone cervical cancer screening (e.g. age, low income, low education) differ from predictors of being up-to-date or adherence to recommended screening intervals. 30 In contrast, factors related to regular health system contact (e.g. having at least one comorbidity condition, history of pregnancy, and breastfeeding) play a role in maintaining adherence over time. 31 Future studies should further investigate factors that influence screening initiation and support ongoing adherence among populations with diverse sociodemographic characteristics.
To our knowledge, this is the first Pan-Canadian study to assess factors associated with cervical cancer screening. The harmonized questionnaires in CanPath support the internal validity of the study and comparability of datasets across the different regions. 31 In addition, the large study sample and availability of data on different personal, social and clinical factors (e.g. race/ethnicity, self-perceived health, cigarette smoking, presence of comorbidity conditions) strengthen the study findings. However, the self-reported nature of responses could potentially affect the observed associations and the voluntary enrollment of the participants in CanPath might limit the generalizability of our findings, although due to the harmonized nature of the data the observed associations across study cohorts are unlikely to be differential.9,10
In conclusion, almost all CanPath cohorts exceeded the national target of 80% adherence to cervical cancer screening, with slight variations among specific groups between regions. Observed associations of social, personal and clinical factors with past screening status provide a deeper insight toward implementing targeted interventions to enhance communications about screening recommendations and access to primary care provider services, and to mitigate inequalities, especially among individuals with nonwhite ethnic backgrounds, of older age and with low socioeconomic status, both at the provincial and national levels. The differential associations observed for certain factors suggest that determinants of screening initiation may differ from those influencing screening maintenance, warranting further investigation in future studies.
Footnotes
Acknowledgments
The data used in this research were made available by CanPath (formerly CPTP) (Regional Cohorts: BCGP, ATP, the OHS, Quebec's CARTaGENE, and the Atlantic PATH.
Funding
The authors disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: CanPath was created with financial support from the Canadian Partnership Against Cancer and by Health Canada. The views expressed herein represent the views of the authors and do not necessarily represent the views of Health Canada. CanPath regional cohorts were also supported by the Ontario Institute for Cancer Research, Alberta Health Services, Alberta Health, Alberta Cancer Foundation, Alberta Health Services, Genome Quebec and the BC Cancer Foundation. Trevor JB Dummer holds the Canadian Cancer Society Chair in Cancer Primary Prevention.
Declaration of conflicting interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
