Abstract
Objectives
To monitor the early effect of a national population screening programme for abdominal aortic aneurysm in 65-year-old men.
Setting
The study used national statistics for death rates from abdominal aortic aneurysm (Office of National Statistics) and hospital admission data in England (Hospital Episode Statistics).
Methods
Information concerning deaths from abdominal aortic aneurysm (ruptured and non-ruptured) (1999–2014) and hospital admissions for ruptured abdominal aortic aneurysm (2000–2015) was examined.
Results
The absolute number of deaths from abdominal aortic aneurysm in men and women aged 65 and over has decreased by around 30% from 2001 to 2014, but as the population has increased, the relative reduction was 45.6% and 40.0%, respectively. Some 65% of all abdominal aortic aneurysm deaths are in men aged over 65; women aged 65 and over account for around 31%. Deaths from ruptured abdominal aortic aneurysm in men aged 60–74 (the screened group) appear to be declining at the same rate as in men aged 75 and over. The relative decline in admissions to hospital with ruptured abdominal aortic aneurysm may be greater in men and women aged 60–74 (which contains the screened group of men), than those older, giving the first possible evidence that abdominal aortic aneurysm screening is having an effect.
Conclusion
The death rate from abdominal aortic aneurysm is declining rapidly in England. There is the first evidence that screening may be contributing to this reduction.
The NHS Abdominal Aortic Aneurysm Screening Programme (NAAASP) aims to reduce premature deaths from ruptured abdominal aortic aneurysm (rAAA) among men aged 65 and over by up to 50% through early detection, appropriate follow-on tests, and referral for potential treatment. Men are invited for an ultrasound scan of the abdomen during the year they turn 65, while men over 65 who have not previously been tested can self-refer for screening. The UK National Screening Committee recommended the Programme in March 2009, and NAAASP completed roll out in England in 2013. 1
NAAASP has already screened over a million 65-year-old men. The prevalence of AAA detected in the first 700,000 men was 1.34%, lower than the around 5% recorded in the randomized trials of two decades ago. 2 The death rate from rAAA was known already to be falling in the UK and elsewhere before population screening started.3,4 The NAAASP remains cost effective at current prevalence rates. 5 We here aim to update national statistics concerning rAAA in England.
Available national statistics were collected in January 2016. Office of National Statistics (ONS) data on mortality rates were examined using the codes I171.3 (death from rAAA) and I171.4 (death from AAA without mention of rupture). Data were for full calendar years up until the end of 2014 and included men and women. Hospital Episode Statistics (HES) from English hospitals with the admission code for rAAA were also collected. These are presented by financial year up to the end of 2014/2015.
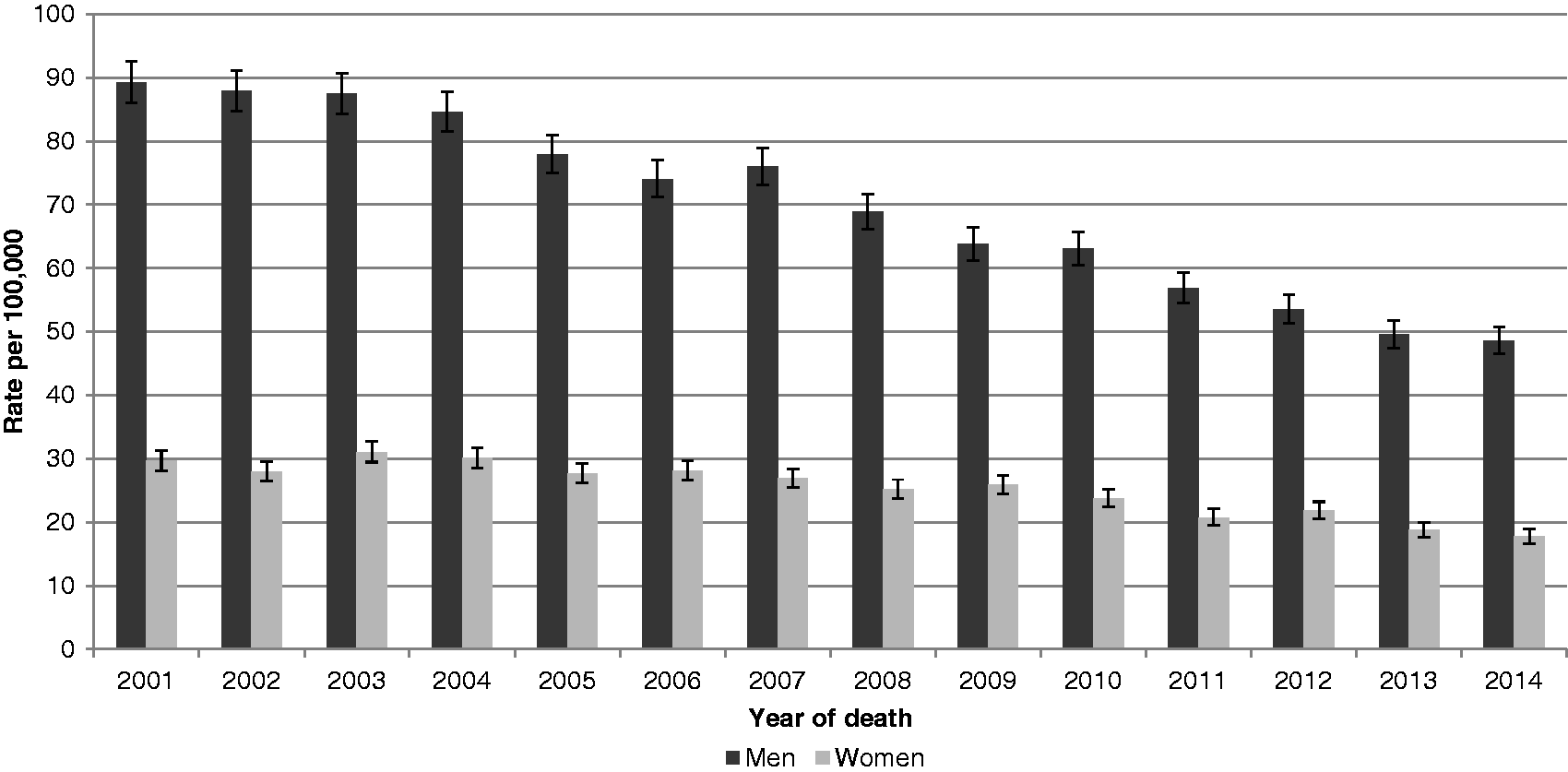
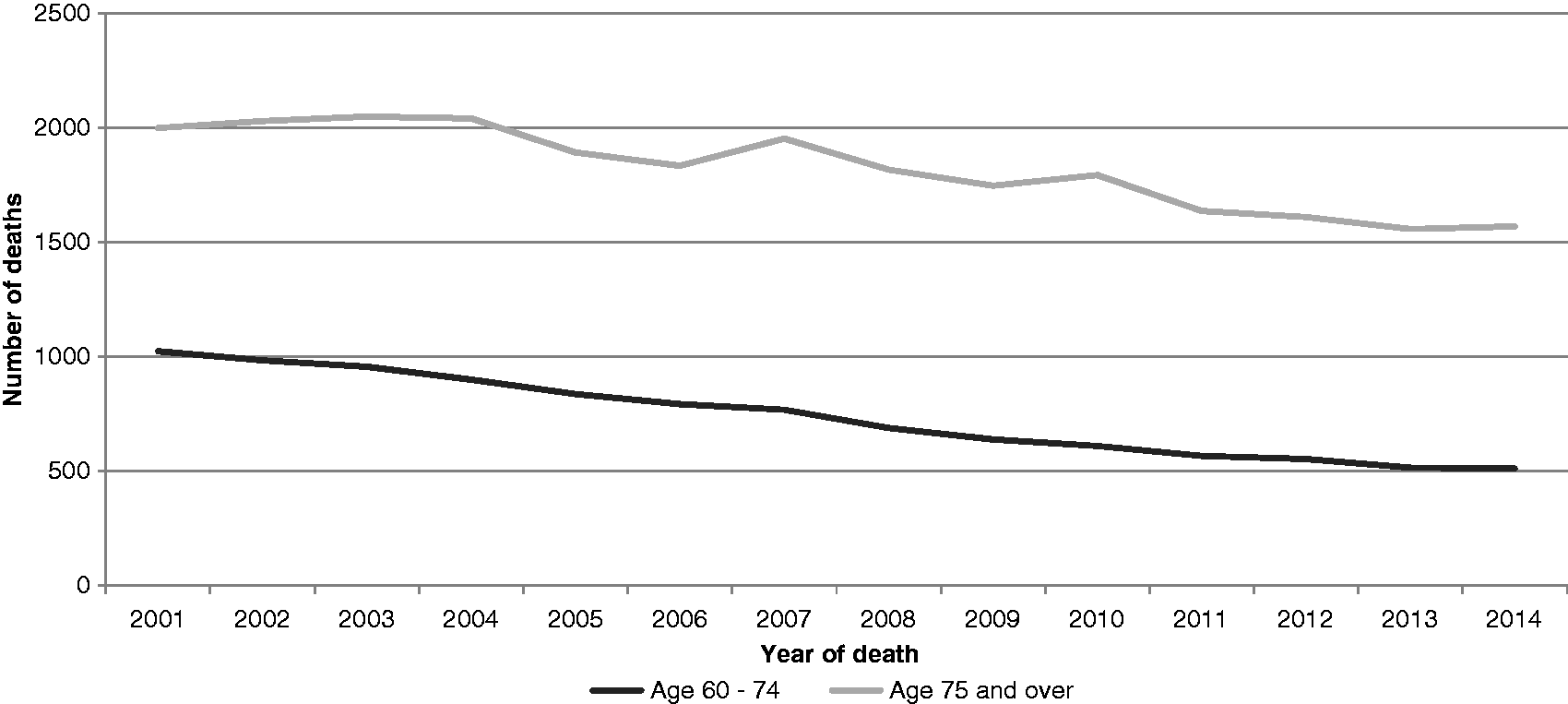
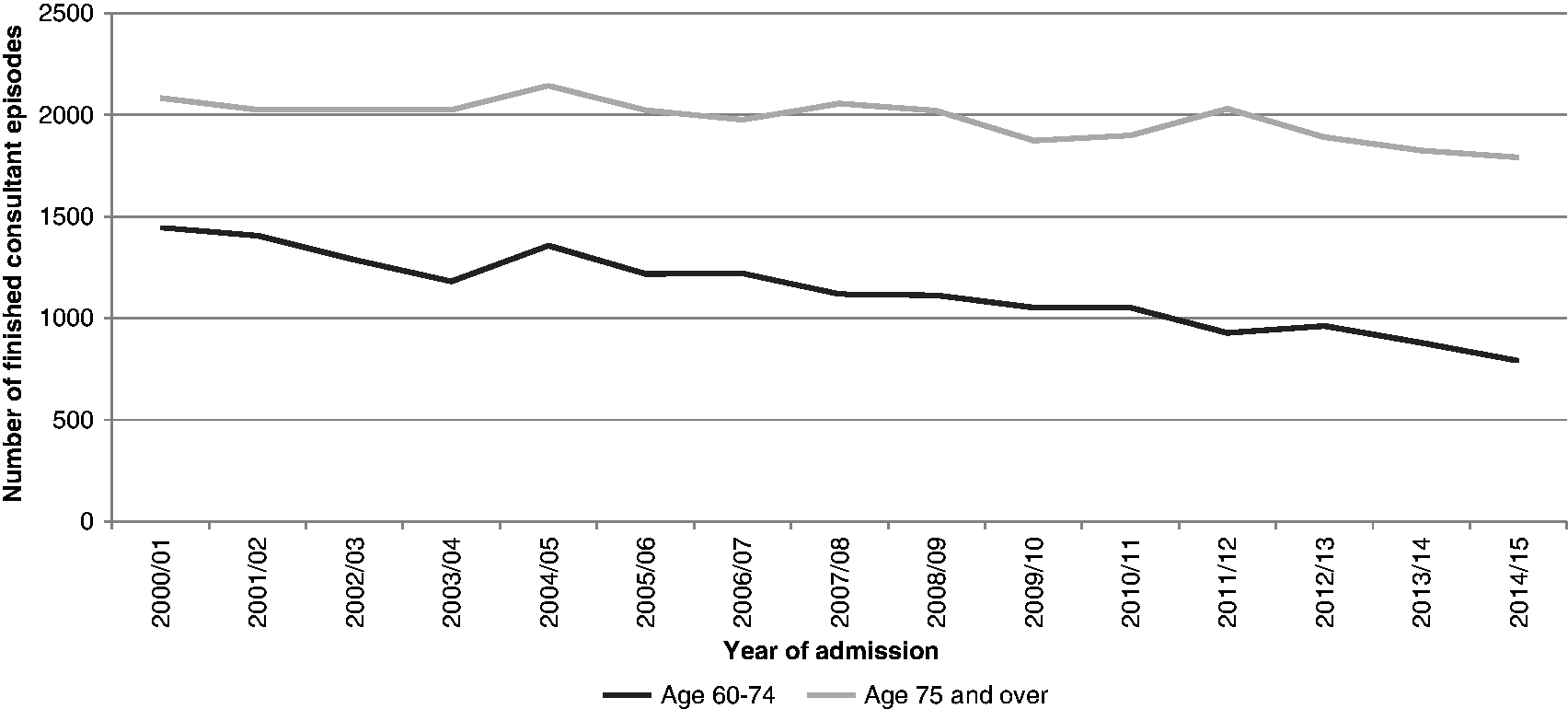
In 1999, from ONS data, 3286 men and 1290 women had rAAA mentioned as cause on their death certificate. By 2014, this had fallen to 2113 and 942, respectively (Figure 1). Using ONS data, from 1999 to 2014, men aged 65 and over have accounted for around 65% of all AAA deaths; women aged 65 and over account for around 31%. The absolute number of deaths in men and women aged 65 and over has decreased by around 30% from 2001 to 2014 (see online supplementary file ONS). However, there has been a 29.3% increase in the number of men, and a 15.3% increase in the number of women in the population over the same time interval, so the relative reduction in the rate of deaths in men and women aged 65 and over was 45.6% and 40.0%, respectively (Figure 2). Although the rate of deaths from AAA rupture is declining in men aged 65 and over, men still account for approximately two out of every three deaths from rAAA. Deaths from rAAA in men aged 60–74 appear to be declining at the same rate as those in men aged 75 and over (Figure 3). Using HES data for emergency admission with rAAA: in 2009, 2809 men and women were admitted, which fell to 2010 by 2014/2015, a reduction of almost 800 people (30%) (see online supplementary file HES). The relative rate of reduction may be faster in men and women aged 65–74 (which includes the screened group of men), than in those aged 75 and above (Figure 4).
Deaths with mention of AAA in men and women in England from ONS statistics. Deaths from ruptured AAA in men and women per 100,000 population from ONS data. Deaths from ruptured AAA in men in England from ONS statistics according to age. Hospital admission with code for ruptured AAA in men and women in England according to age.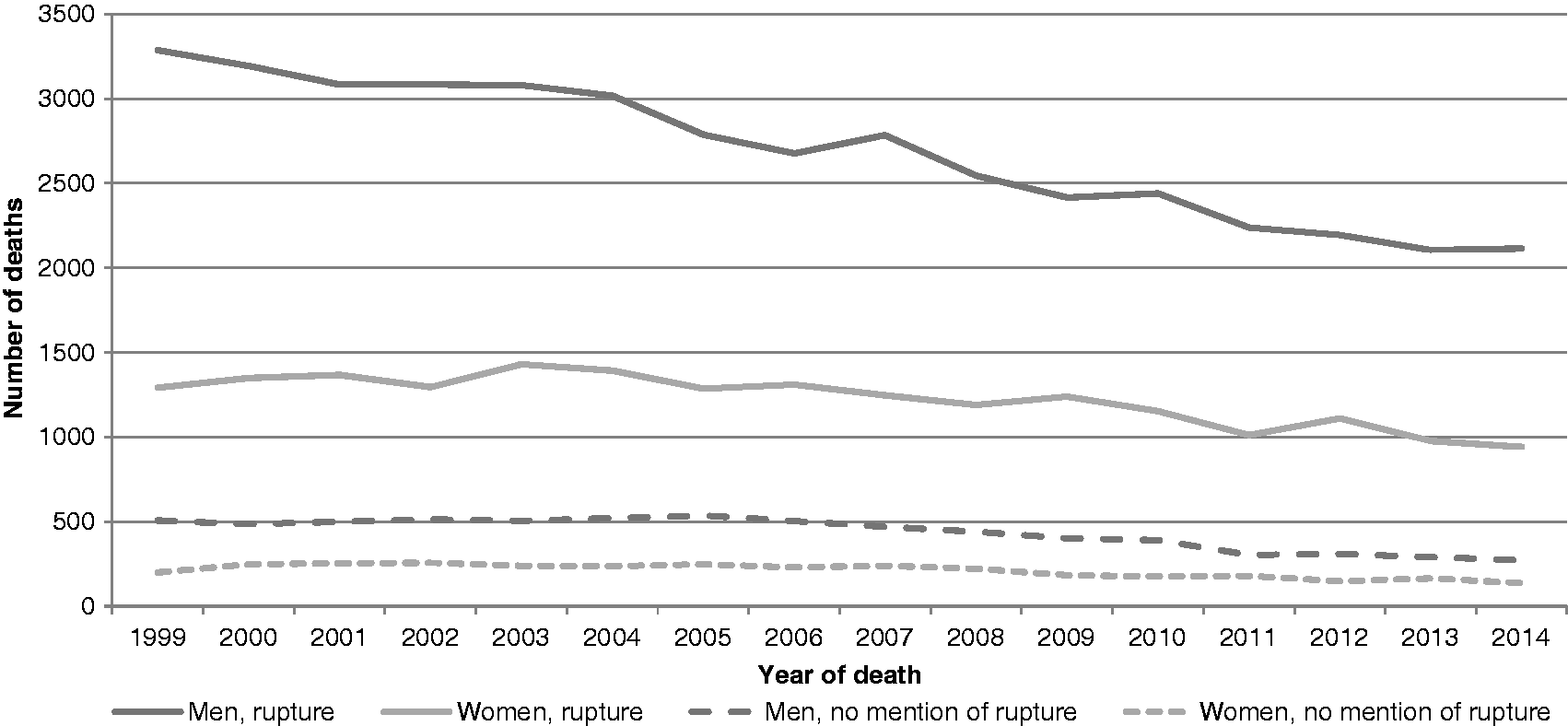
Since it peaked in the 1990s, there has been an ongoing reduction in the number of deaths from AAA in men and women, which is probably the result of better health and fitness in the elderly and reduced smoking rates. It is too early to be certain whether screening for AAA in men is contributing to this reduction, as the effects of screening are diluted by the ongoing reduction in prevalence of AAA. Death rates will also be affected by better medical treatment of men with small AAA; men in surveillance in NAAASP receive advice from specialist nurses about best medical care. There is, however, a suggestion from HES data that the rate of decline in rAAA in England may be accelerating in the screened age group, although this includes women. Final conclusions will not be available until at least 10 years of screening have elapsed. In the meanwhile, it is clear that ultrasound screening is only one part of ongoing interventions to reduce the death rate from rAAA. Screening for women may need to be reconsidered as the prevalence rates become more equal between the sexes with time.
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The NHS AAA Screening Programme is funded by the Department of Health and provided through Public Health England. The authors are grateful for the continued support of the 41 local screening programme teams in England.
