Abstract
South African law recognises the evolving capacity of minors to consent to medical treatment. This is manifested in the Children’s Act 2005 which governs minors’ rights and determines that children aged 12 years and above are presumed to have the capacity to consent to medical treatment provided they are of sufficient maturity to understand its nature and consequences. Although the word ‘maturity’ appears repeatedly in the Children’s Act, it does not provide a definition or guidance on how maturity should be determined. This article therefore, first, discusses the meaning of ‘maturity’, ‘sufficient maturity’, and related terminology and, second, elucidates on the role of brain development in the determination thereof in order to propose foundational elements regarding evidence-based guidelines for establishing whether the legally requisite ‘maturity’ to consent to medical treatment is present. The discussion is informed by South African and foreign case law, relevant regulatory instruments, human rights considerations, and literature on child brain development and consent.
Introduction
Children, persons below the age of 18, 1 are regarded as having an evolving capacity to consent to medical treatment. This may be in reaction to the 1989 adoption of the Convention on the Rights of the Child (CRC) 2 and its recognition of a child as autonomous, 3 regional instruments providing for children’s rights such as the African Charter on the Rights and Welfare of the Child (ACRWC), 4 and global trends in the reorganising of the parent–child relationship. 5 In addition, the children’s rights movement has affected how children are perceived and has led to special protections such as those provided for in various international, regional, and domestic regulatory instruments. South African law recognises this evolving capacity as illustrated by the diverse ages associated with consent to various medical interventions. 6 For example, a child of any age may consent to termination of pregnancy, 7 and a child aged 12 may consent to HIV testing. 8 Further recognition of this evolving capacity is manifested in the Children’s Act 2005, which governs the rights and duties of minors and states that children aged 12 years and above are presumed to have the capacity to consent to medical treatment provided that the child is of sufficient maturity and has the mental capacity to understand the benefits, risks, social, and other implications of the treatment. 9 The Act does not define medical treatment. Treatment may, as such, be understood in its most general sense as a non-invasive and innocuous medical intervention. 10 It may include vaccinations and psychological treatment and receiving blood or blood products. 11 Children may also consent to surgical operations on similar conditions as those required for medical treatment. 12
Although the word ‘maturity’ appears continually throughout the Children’s Act, it does not define or guide on how maturity and sufficient maturity are determined or how these terms should be understood. The Act further omits to stipulate how healthcare professionals ought to assess a child’s decision-making abilities. 13 This article thus asks the following questions: what is meant by ‘maturity’ and ‘sufficient maturity’ (how this might be understood or interpreted), how ‘sufficient maturity’ might be determined, and what role brain development plays in this determination. To answer these questions, this article therefore explores ‘maturity’, ‘sufficient maturity’, and related terminology in the context of a child’s consent to medical treatment by considering scholarly work on this issue, relevant regulatory instruments, which includes mention of the terminological discrepancies between the different domestic, regional, and international instruments, case law from South Africa and other jurisdictions, as well as pertinent human rights considerations. Although the selected foreign case law may provide some valuable insights, the aim of this article is not to provide a comprehensive comparative analysis of foreign law and foreign legal sources are only discussed where relevant to the South African context and the aim of this article. Literature on child brain development and maturity is also discussed to facilitate an understanding of a child’s decision-making capacity to consent as it may inform how clinicians and courts interpret the statutory requirement of ‘sufficient maturity’. In addition to answering the above questions, the aim of the article is therefore to recommend foundational elements regarding evidence-based guidelines for determining whether the legally requisite ‘maturity’ to consent to medical treatment is present.
Maturity and the Children’s Act – some clarification
Consent to medical treatment is provided for in the South African Constitution, 14 which will be discussed in further detail below, as well as several other Acts. The National Health Act 2003 (NHA) provides for consent to medical treatment in general and states that a health service may not be provided without the informed consent of the healthcare user. 15 A ‘user’ is a person who receives treatment in a health establishment and if such a person is below the age ‘contemplated in section 39(4) of the Child Care Act 1983’, includes the person’s parent or guardian or another person authorised to act on their behalf. 16 In terms of the old Child Care Act 1983, this contemplated age was 18 years of age.
In general, the requirements for informed consent are competence, the disclosure of information, understanding and appreciation of the disclosed information, voluntariness, and the ability to exercise or express a choice. 17 In other words, valid informed consent has occurred where a competent person has received proper disclosure of information and understands and appreciates this information and then voluntarily consents to an intervention. 18 In addition, Castell v. De Greef, 19 which solidified the principle of informed consent in South African law in 1994, which has since been reaffirmed by the 2014 case of Sibisi NO v. Maitin, 20 held that a consenting person must have knowledge of the nature or extent of the risks or harm, appreciate, and understand the nature thereof and consent to the harm or assume the risks. The required information to be disclosed has also been elaborated on by the NHA which, according to section 6, includes the consenting person’s health status, the range of diagnostic procedures and treatment options generally available, and the benefits, risks, costs, and consequences generally associated with each treatment or diagnostic option. Disclosure should also, where possible, be done in a language that the person understands and in a manner which takes into account their level of literacy. 21 Furthermore, the Children’s Act requires that a child be given information on the cause of their illness or disease. 22 Finally, it should be noted that consent may be expressed verbally, in writing, or may be implied. 23
Being capable of giving consent means that a person has reached a legally prescribed age of consent and has decisional capacity.
24
The Children’s Act, the primary piece of legislation in regard to children, amended the law as it relates to the age of consent in the medical context and section 129(2) of the Act now provides that
A child may consent to his or her own medical treatment or to the medical treatment of his or her child if—(a) the child is over the age of 12 years; and (b) the child is of sufficient maturity and has the mental capacity to understand the benefits, risks, social and other implications of the treatment.
In terms of section 129(3) of the Children’s Act, a child may also consent to their own surgical operation on similar conditions but with the additional requirement that the child be duly assisted by a parent or guardian. 25 The legally required assistance of a parent or guardian may be interpreted as indicating that this provision deems a child as not fully autonomous in the decision-making process. 26 It is argued, however, that the use of the word ‘duly’ rather than negating the child’s autonomy requires parental support thereof and places a responsibility on the parent or guardian to assist a child in an appropriate and meaningful manner. This means that they cannot simply ‘rubber stamp’ the child’s decision but must apply their mind to the matter and advise the child accordingly so that the child is able to make a decision. Where the child and the parent have differing opinions, the best interests of the child, which will be discussed below, must be determined as the tiebreaker. 27
Section 129 of the Children’s Act sets two requirements for valid self-consent to medical treatment by a child. First, the child must be 12 years of age or above and, second, they must possess sufficient maturity and mental capacity to understand the risks, benefits, and implications of the treatment. Although a determination of the requisite age is simple enough, the meaning of ‘sufficient maturity’ is unclear. The Act itself is also silent on this issue and provides no definition of or guidance on what this means, in other words – how it may be understood, or how it may be determined.
To establish what constitutes ‘sufficient maturity’, how it may be understood, and how it may be determined, however, it is first necessary to elaborate on and distinguish between ‘competence’, ‘capacity’, and ‘maturity’ as literature on the matter of ‘sufficient maturity’ is rife with mention of these concepts which may lead to confusion. 28 These concepts all relate to an individual’s ability to make decisions, particularly in the context of giving consent to medical procedures and while these concepts may seem to overlap, they also have distinct differences. Although terms such as ‘competence’ and ‘capacity’ are often used interchangeably in international literature, South African law and scholarship treat them as distinct concepts. 29 This article adopts these distinctions to reflect the statutory language and to clarify the developmental and functional dimensions of decision-making in children. As these distinctions may be confusing, a summary of differences and relationships between these terms is provided in Table 1. 30
Key differences and relationships between competence, capacity, maturity, and sufficient maturity. 31
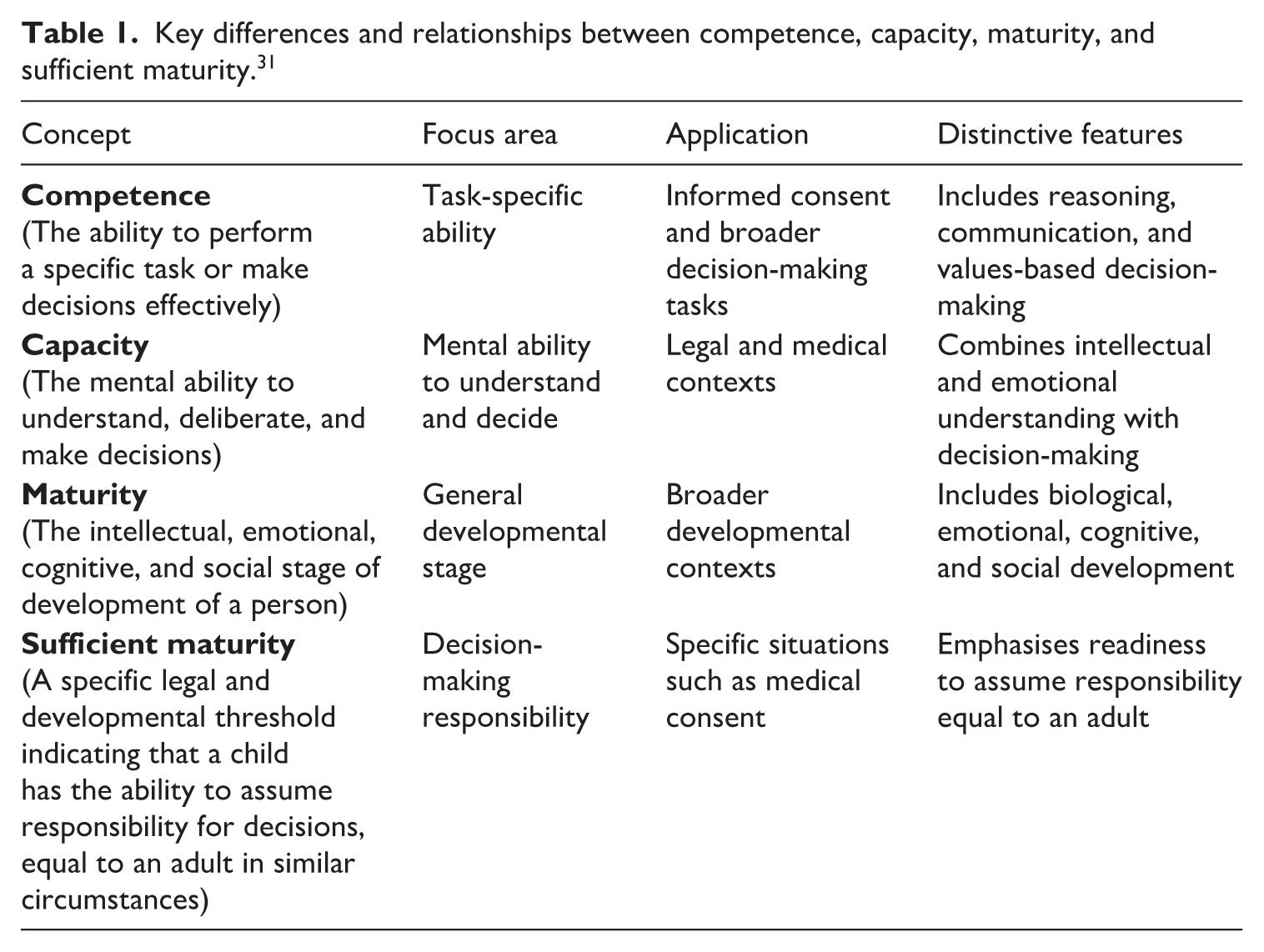
On the one hand, capacity and competence focus on the ability to understand and make decisions, while on the other hand, maturity incorporates a broader range of developmental factors. Sufficient maturity specifically relates to the level of maturity required for a child to consent to medical treatment. The nexus between these concepts lies in their relevance to assessing a person’s ability to make informed decisions and give informed consent to medical treatment and will be elaborated on in the course of this article.
‘Competence’ and ‘capacity’
Competence, plainly stated, means the ability to perform a task. 32 In the context of this article, it is the legal and cognitive ability to understand and make informed decisions regarding matters that affect a person, such as medical treatment. Competence is the first requirement for valid informed consent as discussed previously. It is also linked to capacity, but capacity refers more to the mental ability to understand, comprehend, deliberate, and make decisions. When a person has the ability to understand and make decisions, they are regarded as having decisional competence. However, decision-making competence relies on having capacity. As such, there are three general capacities that have been identified for decision-making competence 33 :
Understanding and communication. This entails the various capacities that enable a person to be informed of a particular treatment and to express their choice in this regard. It includes linguistic, conceptual, and cognitive abilities needed to receive and understand the given information. Understanding also requires the ability to appreciate the nature and meaning of alternatives and to integrate this into the decision-making process. Young children may lack this level of understanding due to a lack of relevant life experience.
Reasoning and deliberation. Competence requires the ability to reason and deliberate, which necessitates adequate short-term memory to retain information during the time it takes to make the decision. This also requires the ability to draw inferences regarding the consequences of a particular decision and to compare alternative outcomes.
A set of values or a concept of what is good. A competent decision-maker should be able to rely on a consistent and stable set of values or some conception of what is good. This allows the decision-maker to evaluate certain outcomes and to decide whether they are beneficial or harmful and assign importance to them.
In addition, Kruger suggests that an investigation into social science theory may be of value when giving meaning to the concept of ‘competence’ and establishing the standards for assessing a child’s maturity and reiterates that competence should be understood as decision-making capacity. 34 This necessarily also requires that the nature of the choice and the specific conditions under which it is made to be specified. As a result, competence is seen as relative, so a person may be competent to make a decision in some circumstances, but not others. This ultimately means that competence is a specified person’s capacity to make a specified decision at a specified time and under specified conditions. 35 This is indicative of the need to individualise the determination of capacity and maturity to the child involved. Although no standard objective tools to assess a child’s competence to consent to medical treatment exists, several tests have been developed to assist in this regard, such as the Hopkin’s Competency Test, Competency Questionnaire–Child Psychiatric, and the Competency Questionnaire–Paediatric Outpatient Modified Version. 36
Capacity, like competence, also takes two forms: legal and mental. 37 While the Children’s Act is clear as to what constitutes legal capacity in certain contexts, such as consent to treatment or surgery, it offers less clarity on what is meant by mental capacity. 38 Drawing from other sources of law, 39 however, the meaning of ‘mental capacity’ may be clarified. In this regard, South African courts have held that ‘mental capacity’ has two elements 40 : first, the ability to intellectually and emotionally understand the nature and consequences of an action and, second, the ability to exercise judgement and make decisions. 41 Derish and Vanden Heuvel, as discussed by Pillay and Singh, have also stated that mental capacity comprises two elements, with the first being the capacity to assimilate relevant facts and the second being an understanding or appreciation of the situation as it relates to the facts by the relevant person. 42 When examining the mental capacity of a child, a further element has been suggested, namely, the child’s ability to communicate their choice. 43 This means that to legally consent to a medical procedure, a person must have the requisite capacity to understand the benefits and risks involved as well as to weigh their options, exercise a choice, and provide reasons for their decision.
Although South African law does not define a child’s mental capacity concerning healthcare decision-making, capacity in this context generally relates to a clinical evaluation of a person’s functional ability to make autonomous and authentic decisions. 44 Healthcare practitioners are therefore required to rely on their clinical skills and knowledge when judging the decision-making capability of a child. Although no hard-and-fast legal guidelines in this regard currently exist in South Africa, legal scholars such as Van Heerden have suggested that an individual capacity assessment must be made in each case. 45 Havenga and Temane have also argued that the following should be considered when assessing mental capacity 46 :
Age;
Personal experiences which may include a history of illness or even abuse;
The healthcare professional’s attitude towards competence, such as whether they are of the opinion that minors in general can in fact have competence or not;
Parental involvement, attitude, and support;
The complexity, magnitude, and circumstances surrounding the diagnostic test, treatment, or procedure; and
Influences on the child such as whether they are in pain, scared, tired, or medicated at the time of decision-making.
To summarise, this means that the concept of competence refers to the ability of a person to perform a specific task or make an effective decision. In the context of medical consent, this includes the cognitive, communicative, and evaluative abilities necessary to understand treatment information, consider alternatives, and arrive at a decision that reflects a person’s own values. Competence is thus task-specific and is commonly assessed in relation to informed consent procedures and other decision-making processes. It does not require a person to function at the level of a fully autonomous adult, but rather to demonstrate the necessary reasoning and communicative capacities to engage meaningfully with the decision at hand.
Dissimilarly, capacity is defined as the mental ability to understand, deliberate, and make decisions. It is a broader and more stable concept than competence, although still context-dependent. In legal and medical contexts, capacity incorporates both intellectual and emotional dimensions which require a person to not only understand factual information but to appreciate its implications and act accordingly. A person with legal capacity, for example, has been deemed able to exercise rights and responsibilities in accordance with the law. Mental capacity is assessed clinically, typically focusing on abilities such as understanding, memory, reasoning, and communication.
‘Maturity’ and ‘sufficient maturity’
In general, the concept of maturity reflects a child’s intellectual and emotional stage of development. Once a child reaches the age of 18, they are regarded as mature adults. 47 The law, however, has both a rigid and flexible view on maturity: rigid in the sense that maturity is linked to a set age, that is, at the age of 18 a person is presumed to be mature, but also flexible as a child below the age of 18 may be considered mature enough to consent to medical treatment if they have ‘sufficient maturity’. 48 The flexibility of maturity has also been confirmed in South African case law such as Christian Lawyers Association v. Minister of Health (Reproductive Health Alliance as Amicus Curiae) where the court held that it is flexible in recognising and accommodating the individual position of a person based on their intellectual, psychological, and emotional makeup. The court further held that it could not be in the interest of the child to adopt a rigid age-based approach that takes no or inadequate account of their individual peculiarities. 49 Ganya et al. agree with this flexible approach and are of the opinion that ‘sufficient maturity’ means a degree of cognitive development comparable with that of a fully developed adult which affords a child the necessary engagement to make decisions. 50 This implies that ‘sufficient maturity’ means mature enough to make a decision.
Some have, however, argued that in determining sufficient maturity, the notion of capacity for responsibility may be of assistance.
51
In terms of this school of thought, a person should not only consider the given choices when making a decision, but must also accept the related responsibilities. This, according to Van Niekerk and Nortjé, means, ‘to be able to be held accountable for whatever decisions are taken, on the basis of the assumption that reasons can be provided, that they have been thought through, and even though they might be fallible.’
52
This would indicate that a consenting person must not only be able to make a decision but also of dealing with the consequences thereof to be considered mature or sufficiently mature.
53
Based on this notion of capacity for responsibility, Ganya et al. have suggested the following definition of ‘sufficient maturity’:
A child has sufficient maturity to consent to medical treatment insofar as he or she can independently demonstrate (or be facilitated either by aids or a helper as far as it is practically possible in that given setting to possess) the commensurate wherewithal required to assume responsibility for that specific decision.
54
Although the Children’s Act, as has been stated, does not define ‘maturity’ or ‘sufficient maturity’, South African policymakers have incorporated this inclusive idea of how to be mature and sufficiently mature may be understood into guiding policy documents. The Department of Health’s HIV counselling and testing policy, for example, describes ‘sufficient maturity’ as instances in which a child is able to demonstrate that they understand information on HIV testing and can act in accordance with that appreciation. 55 Maturity, however, has various dimensions including biological, emotional, cognitive, and social 56 and, as such, the policy further states that in deciding whether a child is sufficiently mature, the age, knowledge of HIV and its implications, the views of the child and whether the child is able to articulate these as well as the personal circumstances of the child, should be taken into account.
From the discussion above, Pillay and Singh recommend that to determine ‘sufficient maturity’, the following must be evaluated, ideally by a multidisciplinary team 57 :
The child’s intellectual functioning to be able to fully comprehend the nature of the circumstances as to have appropriate insight and to respond accordingly;
The presence of any abnormal behavioural psychopathology which may interfere with the child’s ability to properly understand or to administer treatment;
The cognitive functioning of the child which includes memory and retention, attention and concentration, reasoning, information processing, and verbal comprehension;
Social and emotional functioning to establish whether the child has stage-appropriate social, emotional, and moral development to understand, and make a decision;
The personality development of the child which should include assessing impulse control, expressive acts, interpersonal conduct, cognitive style, self-image, object representations, and the regulatory mechanisms of the child;
Any disability and vulnerability although this should not automatically exclude maturity; and
Cultural practices and concerns of the child which may include the evaluation method and norms being used.
In summary, maturity therefore encompasses the intellectual, emotional, cognitive, and social stage of a person’s development. It reflects a general developmental state rather than a specific decision-making ability and is shaped over time through biological, psychological, and social experiences. Maturity is therefore more diffuse than competence or capacity, and is rarely assessed in a single moment or by reference to a specific decision. Rather, it is an evolving trait that informs a person’s ability to respond to life’s demands in a manner that is reasoned and responsible. In law, maturity is often related to age and presumed stages of development, but these assumptions can be misleading when applied to individual children whose personal circumstances may significantly differ.
The legal construct of sufficient maturity, as found in the Children’s Act 2005, blends elements of maturity and capacity to create a threshold tailored for specific legal decisions – consent to medical treatment. It refers to a developmental and legal threshold at which a child is considered capable of assuming responsibility for a decision in a manner similar to an adult. This includes not only understanding the information relevant to the decision but also being able to anticipate and bear the consequences of that decision. Sufficient maturity therefore emphasises both cognitive engagement and psychosocial responsibility. It is a functional measure grounded in context, such as the complexity of the treatment or the child’s past experiences, and signals the need for nuanced, case-specific evaluations rather than rigid age-based criteria.
Understanding the distinctions between competence, capacity, maturity, and sufficient maturity is essential for evaluating a child’s ability to consent to medical treatment. Competence refers to a task-specific ability to reason, understand, and decide, while capacity encompasses broader cognitive and emotional faculties required for meaningful deliberation and informed choice. Maturity, by contrast, reflects a child’s general developmental stage, including cognitive, emotional, and social growth. The legal concept of sufficient maturity, as found in the Children’s Act, incorporates these elements and requires that a child not only understand the implications of a decision but also be developmentally prepared to take responsibility for its consequences. Unlike capacity, which may be assessed clinically, sufficient maturity must often be inferred through contextual judgement and cannot be determined by age alone. The child’s intellectual functioning, behavioural and emotional regulation, cognitive abilities, social maturity, and personality development are all shaped by brain development, a matter which will be discussed in greater detail in the course of this article. 58
Human rights considerations
The South African Constitution is the supreme law of the country and, as such, all law must be interpreted in a manner which is aligned with the Constitution and its provisions. 59 The Constitution provides for a multitude of human rights, many of which may be relevant in the medical context such as equality, 60 dignity, 61 life, 62 bodily and psychological integrity, 63 privacy, 64 and the right to access to healthcare services. 65 The Constitution also expressly lists rights that apply specifically to children. 66 In considering the human rights aspects relevant to this article, the Constitution’s provisions regarding equality, autonomy, access to healthcare, and children’s rights are of primary concern. In order to better align South African law with global standards, section 39 of the Constitution provides for the interpretation of the Bill of Rights and states that international law must, while foreign law may, be considered in the interpretation of the rights in the Bill of Rights. 67 As such, mention will be made of international and regional instruments where relevant. It should be noted that all rights discussed below are subject to the limitation clause and are not absolute. 68
Equality
In terms of section 9(3) of the Constitution, no person may be unfairly discriminated against based on, inter alia, age or disability. In terms of this section, the mere young age of a person should therefore not automatically disqualify them from being seen as able to participate in issues which affect them and they cannot be denied the consideration of their capacity due to their age. Although the use of age as a proxy for the determination of capacity is useful in the absence of a general guide to assess maturity, and especially since no gold-standard test exists to determine a child’s decision-making capacity, it has long been criticised as being arbitrary. 69 This was evident in the Christian Lawyers Association case in which it was held that rather than using age as a measure of control or regulation, capacity to give consent be applied as a yardstick and where such capacity is found to exist, it must be recognised in spite of the relevant person’s age or youthfulness. 70 In this case, the essence of the plaintiff’s argument before the court was that females below the age of 18 years are not capable, without parental consent or control, of making an informed decision regarding the termination of a pregnancy. The court, with reference to the Choice on Termination of Pregnancy Act 1996 (CTPA), held that the capacity to give informed consent is determined on a case-by-case basis, founded on the emotional and intellectual maturity of the concerned individual and not on an arbitrarily predetermined and inflexible age requirement. 71
Age may also at times be regarded as a disability when considering that having a disability generally indicates a condition, be it physical, mental, cognitive, or developmental which impairs, interferes with, or limits the ability to participate in certain tasks, actions, or typical daily activities and interactions. It should be noted that disability may also, in and of itself, not preclude a person’s views from being taken into account in deciding whether they have the capacity to make certain decisions. The nature and extent of the disability and the specific circumstances of the decision being made will have to be considered on an individual basis.
Integrity and autonomy
Healthcare decision-making requires the exercise of autonomy 72 and section 12 of the Constitution provides for bodily and psychological integrity and states that everyone has the right to such integrity, which includes the right to make decisions concerning reproduction 73 and to not be subjected to medical or scientific experiments without their informed consent. In its provision for the right to consent, this section is seen as protecting and including autonomy.
Autonomy is the right to make decisions for oneself and, as such, it is the right to self-determination. Although self-determination is not expressly protected in the Constitution, it may be derived from several fundamental rights in the Bill of Rights. 74 This was confirmed in Christian Lawyers Association 75 in which the court had to decide on the validity of provisions of the CTPA, and as was mentioned previously, South African law does not set a minimum age for a female to consent to termination of her pregnancy. In this case, the plaintiff argued that it is impossible for a person below the age of 18 to make such a decision without any parental control over her decision. In casu, the court made important findings in regard to what it termed ‘the right to self-determination’ and held that it is a constitutional imperative when considering the rights to dignity, bodily and psychological integrity, privacy, and access to healthcare which includes reproductive healthcare. Furthermore, the court stressed that ‘everyone’ is entitled to these rights and that includes a person below the age of 18. In addition to this emphasis by the court, it was also reiterated that section 9(3) of the Constitution prohibits discrimination based on age. It may be noted that the right to self-determination may also be derived from the right to dignity, privacy, freedom of religion, freedom of expression and perhaps even the freedom of association, depending on the nature of the decision to be made. 76
Although some arguments have been made that a child has only limited autonomy, if any, 77 this point of view cannot be compatible with the South African approach to children’s rights. The Constitution affords children the same rights as conferred on ‘everyone’ apart from the right to vote and to hold office. 78 As with adults, the right to self-determination and autonomy may be derived from other fundamental rights. 79 Where a child does not have sufficient maturity, parental control over the child will constitute a justified limitation of the exercise of these rights. 80 However, where a child does have such maturity, it may be an unjustifiable limitation of a child’s autonomy as a child is not a mere extension of their parent, who is ‘umbilically destined to sink or swim with them’ as was stated by Sachs J in S v. M. 81 The use of the word ‘their’ in section 12(2)(c) also indicates that the requisite consent is that of the person, or then child, who will be undergoing a specified intervention. 82
In addition, the notion of autonomy as self-regulation or self-determination is a constitutional value and has been described by the courts as the ability to regulate one’s own affairs, even if to one’s detriment. 83 It has been argued that recognition of autonomy as a developmental phenomenon is implicit in this definition. 84 This is inferred from the use of the word ‘ability’ which denotes that autonomy is an evolving capacity which may be acquired during the process of development. 85 If the evolving capacity of a child is recognised, so too must their autonomy be recognised, meaning that the child has a right to freely express their views in matters which affect them and for this expression to be respected. 86 The recognition of a child’s autonomy is also aligned with the ACRWC as well as the CRC. 87 Article 12 of the CRC provides for a child’s right to be heard and for their expression of a decision to be given due weight. To give due weight to the views of the child means to do more than merely listen to the child and rather requires that these views be considered in all seriousness. 88 The ACRWC also provides for a child’s participation in matters affecting them as article 4(2) provides that such participation is protected where the child is capable of communicating their views. This sentiment is also found in section 10 of the Children’s Act which provides that children who are at an age, maturity, and stage of development where they are able to participate in decisions regarding their future, have the right to do so, in an appropriate way and to have due consideration given to their views.
Access to healthcare
The Constitution also provides for healthcare-related rights and states that ‘everyone has the right to have access to healthcare services, including reproductive health care’ 89 and as has been pointed out previously, ‘everyone’ includes children. It is noteworthy that children’s right to healthcare is provided for in two sections of the Constitution, and that in addition to the general provision found in section 27, section 28(1)(c), which is found in the portion of the Bill of Rights dealing specifically with children’s rights, states that children have the right to basic healthcare services. These healthcare rights must be respected, promoted and fulfilled 90 as well as progressively realised. 91 Arguments have been made that this twofold provision of a child’s right to healthcare services indicates that the Constitution intended to stress the need for child-specific measures to be taken regarding healthcare. 92 In the context of this article, this might also be taken to mean that matters such as a determination of capacity, competence, maturity and sufficient maturity require better clarification, which is what this article attempts to provide.
Children’s rights and their best interests
Section 28 of the South African Constitution provides for the rights of a child and states in subsection (2) that ‘a child’s best interests are of paramount importance in every matter concerning the child’. This is echoed in the Children’s Act which in section 9 states that in all matters concerning the care, protection, and well-being of a child, the standard that the child’s best interests are of paramount importance must be observed. Although the Constitution itself does not elaborate on what is meant by the ‘best interests’ of the child, section 7 of the Children’s Act contains a list of factors to be taken into account when deciding what these best interests are. For the purpose of this article, the most relevant factors are age, maturity and stage of development; gender; background and any other relevant characteristics of the child; physical and emotional security and intellectual, emotional, social, and cultural development; any disability; any chronic illness; and the need to protect the child from any physical or psychological harm. 93 The South African Constitutional Court has also developed a rich jurisprudential body in determining what the ‘best interests of the child’ mean such as that it must not be seen as an overbearing and unrealistic trump card which automatically overrides other rights or that these interests are absolute. 94 The case of S v. M also held that to apply a predetermined formula in a determination of the best interest for certainty’s sake, regardless of the circumstances, would be contrary to the best interests of the child concerned. 95
In this regard, Kruger opines that the strength of the best interest standard may be found in its contextual nature and intrinsic flexibility 96 and supports this with reference to the words of Sachs J in S v. M where it was held that ‘[a] truly principled, child centred approach requires a close and individualised examination of the precise real-life situation of the particular child involved’. 97 This allows for an individualised, contextualised determination of the child in question’s circumstances and the taking into consideration of the impact of all relevant factors on the child. 98 This inherent flexibility of the best interests of the child standard is significant in the context of both protecting the child and in recognising their autonomy. It also allows for the protection of very young children and for the protection of children who have the sufficient maturity to make their own decisions. 99 Unfortunately, no definition of sufficient maturity was offered either in the S v. M case or by Kruger.
It may be noted that the best interest of a child standard is also found in international and regional instruments such as in articles 4(1) of the ACRWC and 3(1) of the CRC. The CRC states that ‘in all actions concerning children, whether undertaken by public or private social welfare institutions, courts of law, administrative authorities or legislative bodies, the best interests of the child shall be a primary consideration.’ It is interesting to note that the CRC refers to ‘a primary consideration’ and not ‘the primary consideration’ which indicates that although the child’s best interests are an important factor to be taken into account, it is not the only factor at play in matters related to a child. 100 It would seem that the South African Constitution in its use of ‘of paramount importance’ is in agreement with the CRC as to the various factors, of which the child’s best interest is an important, but not the lone factor to be considered.
In summary, considering the discussion above on the human rights aspects related to children’s consent to medical treatment, it has been established that a child has the right to access to healthcare as well as the autonomy to consent to their own medical treatment when accessing healthcare. Furthermore, the mere youthfulness of a child may not disqualify them from making their own decisions and in determining whether a child has the sufficient maturity and capacity to consent to their treatment, their best interests are of paramount importance, but should be considered along with various other individualised factors. It is suggested that the brain development of the child is such an individual factor.
Foreign case law
Much attention has been given to the South African legal framework surrounding a child’s self-consent to medical treatment. As mentioned above, however, foreign law may be used when interpreting South African law and, as such, the approach of foreign courts may illustrate conceptual parallels and provide some valuable insight in establishing how ‘sufficient maturity’ may be understood and determined. For this article, two pertinent cases, one from the United States and the other from the United Kingdom, are discussed.
The mature minor – United States
In the United States, there are three situations where a minor (a person younger than 18 years) can legally make decisions about their health care: (1) emancipated minors, (2) condition-specific exceptions for public health reasons as opposed to the belief that minors possess full decision-making capacity (e.g. the diagnosis and treatment of sexually transmitted diseases, pregnancy-related care, and the treatment of substance abuse), and (3) the granting of ‘mature minor’ status. 101
A ‘mature minor’ is a child below the age of 16 who may consent to their own medical treatment if it is determined that the child is sufficiently mature to understand, discern, and appreciate the benefits and risks of the proposed treatment. The mature minor exception, as it is an exception to the common law rule that a parent gives consent to a child’s medical treatment, was dealt with in the case of Cardwell v. Bechtol 102 in which it was held that for a minor child to be considered as mature, and as such to have the capacity to self-consent to medical treatment, there must be clear and convincing evidence that the child fully understands the consequences of his actions. In making this determination, the court may consider various factors such as the ‘age, ability, experience, education, training and degree of maturity or judgment of the minor’, as well as their conduct and demeanour at the time of the relevant intervention. The court, however, also warned that the mature minor exception should not be used as a ‘general license to treat minors without parental consent’, and that the application of this exception should be determined on a case-by-case basis.
This case is interesting in its inclusion of education and training as factors to be considered when a child gives self-consent to treatment. It is also important to note that this case recognises that maturity manifests in degrees. However, it is in this recognition that the helpfulness of this case may be criticised in the South African context. In this case, for the mature minor exception to apply, a person must be above the age of 16, while the South African Children’s Act provides that a child of 12 is able to self-consent. According to a 2020 study conducted by Van Heerden et al., children aged 12 and above had the capacity to give self-consent to medical treatment since they are able to make a treatment choice, understand information, weigh their options, and give reasons for their decision. 103 This same study, however, found that only children aged 14 and over understood more abstract concepts. The conclusion drawn was that children below 14 do not have the same reasoning ability as adults. If an age difference of two years is substantial enough to cast doubt on the decision-making abilities of a child, a difference of four years does so all the more.
Gillick competence – United Kingdom
The United Kingdom’s Gillick competence, as framed in the 1986 Gillick case, 104 may be of assistance in overcoming the age-difference criticism discussed above. Although there has been some judicial back-and-forth on the Gillick case, it is still regarded as having tremendous value. 105 The Gillick competence test is used to help a court establish whether a child below the age of 16 has sufficient understanding and intelligence to be able to fully understand what a proposed medical intervention entails and the capacity to consent to that intervention. It considers whether the child understands the nature and implications of the proposed treatment as well as the risks and benefits involved. If the child demonstrates sufficient understanding and intelligence to comprehend these factors, they may be deemed ‘Gillick competent’ and able to self-consent to medical treatment. In many countries, especially in Western Europe, this competence is usually assessed by the health practitioner. 106
Of importance is the test’s recognition that the understanding required of the child for different medical interventions will vary considerably. This means that a child below the age of 16 may have the capacity to consent to some interventions, but not others. For the purposes of this article, this is significant as this reiterates that the nature of the intervention must be kept in consideration when a child self-consents and it again suggests degrees of maturity.
An in-depth discussion of the United Kingdom’s Mental Capacity Act 2005 (MCA) falls outside the scope of this article and the Act is not binding in South Africa. It is, however, interesting to note that while Gillick competence remains the operative standard in cases involving persons below 16, the MCA provides for a distinct framework regarding consent, establishing a statutory scheme for assessing the capacity of persons aged 16 and above. Under the MCA, a person is presumed to have capacity unless it is shown that they are unable to make a specific decision due to an impairment of, or disturbance in, the functioning of the mind or brain. The Act provides a structured test: the individual must be able to
(a) understand the information relevant to the decision,
(b) retain that information,
(c) use or weigh that information as part of the decision-making process, and
(d) communicate their decision.
This decision-specific and functional approach applies to healthcare and other areas of life, and it highlights the difference from Gillick, which is framed in terms of sufficient intelligence and understanding in those below16. Although the MCA is aimed at those above 16, section 2(5) confirms that it can also apply to persons below 16 if the courts or statutory schemes expressly provide for it. In practice, this has meant that the MCA may govern certain situations involving 15-year-olds, particularly where long-term incapacity is at issue (in cases of serious disability for example). However, for most persons below 16, Gillick remains the standard, with the MCA functioning as a complementary, not substitutive, framework.
An evaluation of the multidisciplinary literature on the brain development of children, as will be discussed below, is of great assistance in establishing to what degree a child may be regarded as mature enough, or then sufficiently mature, to consent to treatment.
Decision-making capacity in children: child brain development and maturity
Research on brain development provides measurable, functional indicators that can be operationalised in clinical assessments to evaluate the cognitive and emotional capacities underlying the maturity of the child. An understanding of the science on brain development, maturity, and decision-making capacity in children allows clinicians to move beyond simple age-based assumptions and assess the actual decision-making capacity of individual children.
It is thus essential to consider the scientific literature on brain development and maturity in the context of decision-making capacity in order to recommend foundational elements regarding evidence-based guidelines for determining whether the legally requisite ‘maturity’ to consent to medical treatment is present. Law and policy should adapt as our understanding of science adapts to ensure it remains legitimate. Ensuring the legitimacy of legal concepts and guidelines requires an understanding of the scientific literature regarding a particular topic. We agree with Grootens-Wiegers et al. that in reviewing the science regarding child decision-making capacity, maturity, and brain development, a multidisciplinary approach is beneficial because of the multifaceted nature of the issue, as many factors may influence a child’s decision-making capacity and maturity. 107 The discussion thus includes high-level insights from neuroscience, psychology, decision-making science, and medical practice. As neuroscience is a rapidly evolving field, new insights into how brain structure may influence decision-making capacity and maturity may develop over time.
Considering empirical research and clinical practice in addition to normative considerations also offers an opportunity to give direction to the discussion. 108 Furthermore, accurate assessment of children’s decision-making capacity through evidence-informed guidelines can help avoid either denying children their rights by excluding capable children from decision-making, or imposing complex medical decisions on children who are unable to make such decisions. 109
Development and maturity
While, as mentioned, health professionals have no common definition of ‘maturity’, they generally follow a developmental approach which views the child as progressing from one stage to the following sequentially in their development from infancy through early and later childhood, to adolescence, early adulthood, late adulthood, and old age. 110 Each stage is marked by particular developmental milestones and abilities, which can be age-linked but may be achieved earlier or later than expected. Several factors influence development, including culture, gender, available resources, and the environment. Stressors, traumatic events, or illnesses may also lead to regressions in developmental stages. 111 Furthermore, in neuroscience, it has been accepted that epigenetic changes (changes in developmental outcomes like regulation of gene expression, that is, which aspects of DNA are activated in development or not) can be affected by specific experiences, leading to changes in the nervous system. 112 A better understanding of neurodevelopmental changes during early development has contributed to the international shift in conceptualising decisional capacity where each child’s unique circumstances are considered rather than their chronological age. 113
Brain development starts in utero, around three weeks after conception and continues roughly through a series of stages (beginning with neurogenesis, progressing to neural migration, maturation, synaptogenesis, pruning, and myelin formation) until an adult reaches 30 years of age. 114 Studies have shown that decision-making relies on dual systems within the brain, of which both systems are important for good decision-making: first, a socioemotional system composed largely of limbic and paralimbic structures and, second, a cognitive-control system composed of prefrontal and parietal cortical structures. 115 Brain regions mature at different rates, with the prefrontal cortex (the part of the brain associated with high-level reasoning, executive function, weighing of consequences, planning, organisation, emotional regulation, and rational decision-making) reaching maturity last at about age 30. 116 The amygdala (responsible for emotion processing and input in the reward system) stabilises during mid- to late adolescence. 117 The socioemotional system (involving rapid, automatic processing that is often reactive, intuitive, and unconscious) matures around the time of puberty, while the cognitive-control system (consciously controlled, volitional, deliberate, reasoned, analytic, reflective and requires more time and a conscious effort) matures in the mid- to late 20s, along with integration between the systems. 118 This temporal imbalance between the two systems can lead to risky behaviour in adolescents and a focus on short-term gain rather than long-term consequences. 119
Decision-making capacity and the neurological skills required
According to Appelbaum and Grisso, decision-making capacity can be defined by four standards 120 :
Understanding the disclosed information about the nature and procedures of the research.
This requires sufficient intelligence and language proficiency to process the information, memory and recall skills (children aged 10–12 have recall abilities comparable with adults), and the ability to orient and direct attention towards the information (maturity develops ages 7–10). 121
2. Reasoning in the process of deciding about participation.
This involves reasoning about risks and consequences. Children aged 6 to 8 already demonstrate the ability of logic reasoning, which improves significantly between ages 8 and 11 due to use and experience, becoming more accurate in adolescence (though adolescents deal differently with risk than adults, as will be discussed below). 122
3. Appreciation of the nature of the situation.
This includes appreciating the various options and their relevance to one’s personal situation, which requires the skill of abstract thinking, including the awareness that others have a mind of their own (theory of mind). 123
4. Expressing a choice about participation.
This implies that a preference can be communicated, either verbally or written. Verbal language development initiates in early childhood, with reasonable understanding at age 5. 124
Empirical studies suggest that there is no significant difference in the ability of adolescents to make rational and reasonable health care decisions by the age of 14. 125 One widely cited such study by Weithorn and Campbell employed a rigorous methodology and used hypothetical treatment dilemmas and a scoring system designed to rate subject responses in terms of each of the four tests of competency. 126 They concluded that adolescents older than 13 years possessed the capacity to make decisions about their health care, a sentiment echoed by many other scholars, apart from where such adolescents demonstrate that they lack capacity. 127 These findings seem to be congruent with those of Van Heerden mentioned above.
A study by Hein et al. demonstrated in a sample of 161 paediatric patients aged 6 to 18 years that children’s decision-making capacities regarding clinical research could be assessed in a valid and reliable way by utilising the modified MacArthur Competence Assessment Tool for Clinical Research (MacCAT-CR). The MacCAT-CR is a semistructured interview format developed by Appelbaum and Grisso in 2001, which measures the abovementioned four aspects of decision-making capacities. 128 Hein et al. found that children of 11.2 years and older generally appeared to be competent, while children of 9.6 years and younger were not. The age of 11.2 years serves as an indication at what age competence might be expected given favourable environmental factors. 129 Children between 9.6 and 11.2 years were in a transition period where their maturity was not pervasive, with the cross-over point estimated at 10.4 years. 130
In the literature on developmental psychology, some scholars attribute maturity to either cognitive (relating to thought processes) or psychosocial (related to emotional and social capability) differences between adults and children. 131 In truth, judgement (or decision-making) is influenced by both cognitive and psychosocial influences. 132 Diekema opines that psychosocial factors appear to interact in important ways with the cognitive elements of decision-making, which suggests that a model of capacity assessment that rests solely on the adolescent’s ability to understand and reason is incomplete. 133
Diekema highlights one problem with assuming that adolescents have decision-making capacity is that assumption is based on an assessment of the adolescent’s rational faculties, namely, assessments of understanding and reasoning. 134 This does not account for the fact that although adolescents have the capacity to make decisions approximate to that of adults, an emphasis on intellectual and rational capacity ignores other elements of decision-making, like emotional and social maturity. 135 Adolescents are more prone to the influence of peers, less future oriented, more impulsive, and differ in their assessment of risks and rewards compared with adults. 136 Adolescents are more likely than adults to underutilise their cognitive skills and make decisions differently than adults. 137 In emotional (or ‘hot’) situations versus analytical (or ‘cold’) situations, decision-making can be severely influenced, with increased risk-taking and a focus on short-term rewards. 138 This may be connected to the capacity for responsibility mentioned above. Reasoning capacity may be hampered by emotions linked with conflicts that may exist between the child and their parents as well. 139 This has implications for adolescent decision-making in emotionally charged or pressured situations, especially where significant threats to their future well-being are involved. 140 Adolescents may have the maturity and decision-making capacity to make some decisions in some contexts, but not others. 141
Diekema recommends that adolescent decisions about their healthcare should be respected, but that limits should be placed on the types of decision they are allowed to make in conditions of high stress and emotion, or under pressure from family or influential community members.
142
This includes that children should not be allowed to refuse lifesaving interventions with a reasonable probability of success. He offers a useful guideline for consideration:
if a parental decision to refuse a medical intervention on the adolescent’s behalf would be challenged (because it places the adolescent at significant risk of serious harm compared with rejected alternatives), we should be reluctant to allow the adolescent to make it.
143
Grootens-Wiegers et al. state that although children from the age of 12 can have decision-making competence, this coincides with the onset of adolescence and thus early development of the brain’s reward system combined with late development of the control system diminishes decision-making competence in adolescents in specific contexts. 144 Thus, adolescents may need support to facilitate environmental factors and create a context within which they can make decisions competently.
Recommendations of assessing ‘maturity’ and decision-making capacity in children
Michaud et al., a multidisciplinary team of professionals working in the field of adolescent medicine, neurosciences, developmental and clinical psychology, sociology, ethics, and law, developed policy guidelines on how to assess the decision-capacity of minor adolescents and found that the evaluation must be guided by a well-established procedure, and health professionals should be trained accordingly. 145
One model on children’s decision-making capacity proposed by Miller identifies initial predisposing factors (cognitive development and experience), followed by four groups of factors that influence decision-making competence 146 :
Child (including personality, emotional state, and disease severity which can affect understanding, as well as retention of information and reasons to consent);
Parent (attitude towards the child and the attention and support provided in decision-making process);
Clinician (attitude towards the child and the attention and support provided in decision-making process); and
Situational factors (type and complexity of the decision, the setting and time constraints).
Healthcare professionals’ personal beliefs and attitudes about children’s rights and involving children in treatment-related decision-making can impact their assessment of a child’s decision-making capacity. 147 When children are viewed as incapable of understanding or forming opinions by healthcare professionals, it leads to children not being provided with adequate information to allow them to make an informed decision. 148 Information must be adapted to the child’s level of communication and understanding, for example, by providing separate sheets for the child and offering oral explanations, as decision-making competence is “only as good as the provided information”. 149
Hein et al. recommend a selective implementation of individual assessment of children’s competence in medical decision-making using a standardised tool, like MacCAT-CR, while also considering generally appropriate age limits. 150 Tools like the MacCAT-CR operationalise neuroscientific insights by translating them into clinical practice. This provides a structured, evidence-based method for determining competence in legal and medical contexts. Michaud et al. contend that no universally accepted approach to assess the autonomous decision-making capacity of children is yet available. 151 Although there is some consensus in the literature that the four areas assessed by the MacCAT-T tool, as discussed above, should be evaluated, Michaud et al. recommend that this assessment be done in a step-by-step procedure 152 :
Assess the adolescent’s understanding of the different facets of the situation,
Evaluate the adolescent’s reasoning about his or her present situation, health condition, and the therapeutic options,
Assess the adolescent’s thinking on various options, and
Make sure that the adolescent is able to express a choice.
Michaud et al. further recommend that the designated person or (preferably) team that should carry out the assessment should be the primary health care team, as opposed to a delegated process to specialists. The reasons for this include that the primary health care team knows the patient better than a delegated specialist, the patient is more likely to trust their regular provider, and in low- or middle-income countries specialists are simply unavailable. 153 The opinions of the parents or guardians, other relatives or educators, mental health providers or social workers can also provide valuable information about the understanding of the adolescent patient. Deliberation in a team regarding the assessment would assist with making a fair decision, and where a team is not available, practitioners should be encouraged to involve at least one colleague who is removed from the case. 154 The setting and the relationship between the health care team and the adolescent patient are important to facilitate the environment within which adolescents can make decisions. 155
Strode et al. 156 recommend the following in determining decisional capacity of a child:
Healthcare practitioners must focus on the choice to be made by establishing what understanding would be required considering the information provided to a child and keeping in mind that children between the ages of 12 and 14 may struggle with abstract concepts.
Contextualise the child by considering their age, life circumstances, and their ability to weigh and balance differing factors that will guide them to an appropriate decision.
Identify and develop decisional supports for younger children such as simple language, and age-appropriate materials explaining the potential benefits and risks of a medical intervention.
Include parents and guardians in instances where children do not have capacity or where the child wants to include them in decision-making.
Based on the above discussion of applicable law in South Africa, children’s rights considerations, and the evidence on brain development and its connection to maturity and decision-making ability, we recommend the following:
● That standardised and universally applicable guidelines should be implemented regarding assessments of sufficient maturity and decision-making capacity in children. The assessment should be guided by a step-by-step procedure, which might involve a standardised tool such as the MacCAT-CR if such a tool becomes widely accepted.
● The step-by-step assessment procedure should involve the four standards of decision-making capacity, which are widely accepted by scholars as valid 157 :
1. Assess the child’s understanding of the different facets of the situation,
2. Evaluate the child’s reasoning about their present situation, health condition, and the therapeutic options,
3. Assess the child’s thinking on various options, and
4. Make sure that the child is able to express a choice.
● The step-by-step procedure should be completed by the child’s primary healthcare team, or in consultation with an objective healthcare provider if there is no team.
● The assessment should include consultation with caregivers and other relevant parties who know the child well.
● Healthcare professionals should provide decisional supports like simple language, and age-appropriate materials to facilitate an environment within which the child can make an informed decision.
● The assessment should consider emotional state and disease severity, as these factors may affect understanding and decision-making capacity.
● The assessing clinician should create a supported and trusting environment.
● The complexity of the decision should be considered when deciding whether a child can understand and appreciate the situation, consequences, and options available (as an example, simple diagnostic tests like blood draws require less complex decision-making than life-altering or life-threatening medical decisions like in the case of limb amputations or critical illness).
● In situations where time constraints and urgency are involved, the assessing professional should be cognisant of how this may negatively affect a child’s ability to assess the risks and long-term consequences involved in a decision. In such cases, the assessment should be repeated at a different time, if possible, to ensure that the child patient has understood and appreciated the situation.
● Healthcare professionals should be trained on the step-by-step assessment procedure, which should be clear, simple, and easy to implement.
It must be mentioned here that any assessments of sufficient maturity will rely on professional judgement. Legal rules and developmental science provide important parameters, but in practice, healthcare professionals must weigh the child’s demonstrated maturity in the specific treatment context. Professional judgement should not be understood as subjective intuition, but the structured application of clinical expertise within the legal framework. As such, guidelines and tools, such as MacCAT-CR, for example, should be seen as aids to professional judgement rather than substitutes for it.
While these recommendations propose foundational elements for guidelines regarding evidence-based assessment of ‘sufficient maturity’, further empirical validation may be needed. Future research should refine these indicators in clinical settings and test their applicability across diverse contexts.
Conclusion
The aim of the article was to propose foundational elements for evidence-based guidelines for determining the legally requisite ‘maturity’ for a child to self-consent to medical treatment and to elucidate on the role of brain development in this determination. To do this, a clarification of how ‘maturity’ and ‘sufficient maturity’ may be understood was undertaken and it was found that maturity relates to the intellectual, emotional, cognitive, and social stage of development of a person. It is normally used to determine readiness for certain responsibilities or actions and in the context of medical consent, maturity plays a role in assessing the ability to understand and make decisions regarding healthcare. It was further found that ‘sufficient maturity’ of a child may be understood as the level of maturity to independently demonstrate the ability to assume responsibility for a decision equal to that of an adult. In other words, ‘sufficient maturity’ means being mature enough to make decisions in the same manner as an adult would and, as such, it is a term used to describe a level of cognitive, emotional, and social development in a child that enables them to understand information relevant to a decision and to act in accordance with that understanding. It includes factors such as age, knowledge, ability to articulate their views as well as their personal circumstances and experiences.
This article also observed that competence is closely related to capacity and refers to a person’s ability to perform a task or make decisions. For medical consent, competence is an essential requirement for valid informed consent and capacity was found to mean a person’s ability to understand the nature and consequences of an action as well as the ability to exercise judgement and make a decision.
Once terminological clarity was provided, attention was given to how such maturity and sufficient maturity may be determined. The article demonstrated that literature on child brain development and maturity provides a lens through which ‘sufficient maturity’ can be understood and assessed. By identifying specific neurodevelopmental milestones, such as the development of abstract reasoning, emotional regulation, and executive functioning, healthcare professionals can make more accurate, evidence-based judgements about a child’s ability to consent to medical treatment and whether they possess the legally requisite sufficient maturity.
It was found that in determining a child’s maturity and mental capacity, a rigid, one-size-fits-all approach is not suitable and numerous contextual factors must be considered.
Various factors to be taken into consideration were identified throughout the course of this article. For ease of reference, these factors are listed here:
Competence. This includes understanding and communication, reasoning and deliberation as well as a set of values. Competence may be established by making use of certain tests such as the Hopkin’s Competency Test, Competency Questionnaire–Child Psychiatric, and/or the Competency Questionnaire–Paediatric Outpatient Modified Version.
Capacity. This includes legal and mental capacity; the ability to intellectually and emotionally understand the nature and consequences of an action, to exercise judgement and make decisions as well as to communicate a choice. Mental capacity may be determined by taking age; personal experiences; a healthcare professional’s attitude; parental involvement, attitude, and support; the complexity, magnitude, and circumstances of a diagnostic test, treatment, or procedure and any influences on the child into consideration.
Maturity in general. This includes more than mere age and extends to the intellectual, cognitive, social, and emotional functioning of the child; any abnormal behavioural psychopathology; personality development; disability and vulnerability; and cultural practices and concerns. In addition, the child’s capacity for responsibility, understanding of the decision-making process and ability to assume responsibility for specific decisions may be considered. Additional factors to be considered also include education and training as well as the need to recognise that there are degrees of maturity.
Children’s rights aspects may also be taken into consideration. This article has found that children have the right to access to healthcare and have the autonomy to self-consent to medical treatment when accessing healthcare. The mere young age of a child may not disqualify them from making their own medical decisions. The best interests of the child are of paramount importance but are not overriding.
Child brain development. This includes the stage of brain development; cognitive-control systems; socioemotional systems; temporal imbalances; the child’s understanding of information, reasoning skill, abstract thinking, and expression of their choice. These may also be influenced by the personality and emotional state of the child, the severity of their disease, parental support, and situational factors.
Recommendations have also been provided as to how these various factors may be practically considered in determining whether a child has the legally requisite maturity to self-consent to medical treatment. This comprehensive approach to determining sufficient maturity in children involves a multidisciplinary assessment considering various cognitive, emotional, social, and contextual factors, aiming to ensure children’s rights are respected while safeguarding their well-being in medical decision-making.
It must be noted, however, that while the introduction of the concept of ‘sufficient maturity’ into South African law has advanced children’s autonomy rights, its undefined and contextually fluid nature also creates uncertainty in clinical and legal practice. While the term offers flexibility and adds value if embedded in structured, evidence-based assessments that include neurodevelopmental and psychosocial indicators, it risks confusion without clearer operational criteria.
In closing, it is important to note that if standardised and universally applicable guidelines for assessing maturity are not implemented, there is a risk for wide margins of application of clinical judgement. If guidelines are implemented, it will ensure more uniform decision-making regarding child maturity and capacity to consent to medical treatment instead of relying on individual healthcare professionals’ knowledge and outlook. This is especially pertinent from the above discussion about how healthcare practitioners’ knowledge and attitudes towards children can affect the determination of whether the child is sufficiently mature to make decisions about their own medical care. Any resulting deprivation of autonomy may violate children’s rights, who are an especially vulnerable population considering they would rarely be in a position (financially or otherwise) to enforce their rights on their own behalf, either because they are without support from their caregivers or similar interested parties or because they are self-reliant. Implementing a set of standardised guidelines may also lay the groundwork for adolescents to appeal decisions that are contrary to their wishes.
Cases cited
South Africa
Barkhuizen v. Napier (CCT72/05) [2007] ZACC 5 (4 April 2007).
Castell v. De Greef 1994 (4) SA 408 (C).
Christian Lawyers Association v. Minister of Health (Reproductive Health Alliance as amicus curiae) 2005 (1) SA 509 (T).
S v. M (Centre for Child Law as Amicus Curiae) 2008 (3) SA 232 (CC).
Sibisi NO v. Maitin 2014 (6) SA 533 (SCA).
USA
Cardwell v. Bechtol 724S.W.2d 739 (1987).
UK
Gillick v. West Norfolk and Wisbech Area Health Authority [1986] AC 112.
Re E (A Minor) (Wardship: Medical Treatment) [1993] 1 FLR 386.
Re W (A Minor) (Medical Treatment: Court’s Jurisdiction) [1993] Fam 64.
Footnotes
Declaration of conflicting interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Preprint
None.
1.
Section 28(3) Constitution of the Republic of South Africa, 1996.
2.
See articles 3, 5, and 12 of the United Nations Convention on the Rights of the Child, 1989.
3.
A. Strode, Z. Essack, and C. Slack, ‘Adolescent Self-Consent to Medical Interventions in South Africa’, South African Journal of Child Health 17 (2023), pp. 136–139.
4.
See articles 4 and 9 of the African Charter on the Rights and Welfare of the Child, 1990.
5.
H. Kruger, ‘The Protection of Children’s Right to Self-Determination in South African Law with Specific Reference to Medical Treatment and Operations’, Potchefstroom Electronic Law Journal 21 (2018), pp. 1–34.
6.
See, in general, A. Strode, C. Slack, and Z. Essack, ‘Child Consent in South African Law: Implications for Researchers, Service Providers and Policy-Makers’, South African Medical Journal 100 (2010), pp. 247–249.
7.
Section 5 Choice on Termination of Pregnancy Act 1996.
8.
Section 130 Children’s Act 2005.
9.
Section 129(2) Children’s Act 2005.
10.
W. Ganya, S. Kling, and K. Moodley, ‘Autonomy of the Child in the South African Context: Is a 12 Year Old of Sufficient Maturity to Consent to Medical Treatment?’, BMC Medical Ethics 17 (2016), p. 66.
11.
Kruger, ‘Protection’, p. 1.
12.
Section 129(3) Children’s Act 2005.
13.
Ganya et al., ‘Autonomy of the Child’, p. 1.
14.
Constitution of the Republic of South Africa, 1996.
15.
Section 7(1) National Health Act 2003.
16.
Section 1 National Health Act 2003.
17.
Ganya et al., ‘Autonomy of the Child’, p. 4.
18.
Op. cit.
19.
Castell v De Greef 1994 (4) SA 408 (C).
20.
Sibisi NO v Maitin 2014 (6) SA 533 (SCA).
21.
Section 6 National Health Act 2003.
22.
Section 13(1)(c) Children’s Act 2005.
23.
Ganya et al., ‘Autonomy of the Child’, p. 5.
24.
Y. Havenga and M. Temane, ‘Consent by Children: Considerations when Assessing Maturity and Mental Capacity’, South African Family Practice 58(Suppl. 1) (2016), pp. S43–S46.
25.
‘Duly assisted’ has been interpreted by some as meaning assistance in the consent process and that this is part of parental rights and responsibilities and specifically the duty to care for the child. Caring for the child means to guide, advise and assist the child in decision-making, in a manner appropriate to the age of the child, their maturity and stage of development. See, in general, Kruger, ‘Protection’.
26.
B. Pillay and J. Singh, ‘“Mental Capacity”, “Sufficient Maturity”, and “Capable of Understanding” in Relation to Children: How Should Health Professionals Interpret these Terms?’, South African Journal of Psychology 18 (2018), pp. 538–552.
27.
Op. cit., p. 540.
28.
The term ‘judgement’ is also relevant here. It is a related, but distinct concept that refers to the ability to make considered choices after weighing options and anticipating consequences. In healthcare practice, judgement is usually assessed as part of evaluating mental capacity, especially in adolescents. It is closely tied to executive functioning and impulse control, both of which continue to develop during adolescence. A lack of sound judgement can lead to impulsive or poorly reasoned decisions, even where the adolescent shows intact intellectual understanding. In this article, ‘judgement’ refers both to the child’s cognitive ability to weigh options and anticipate consequences, and to the professional judgement exercised by clinicians in assessing whether the child demonstrates sufficient maturity and capacity, depending on the context. Professional judgement should be understood not as subjective intuition, but as the structured application of clinical expertise within the legal framework. See, in general, B. Luna, ‘The Maturation of Cognitive Control and the Adolescent Brain’, in Francisco Aboitiz and Diego Cosmelli, eds., From Attention to Goal-Directed Behavior (Berlin: Springer, 2009), pp. 249–274.
29.
For example, in international literature such as Ganya, Kling and Moodley expressly state, ‘in this article we use the terms competence and capacity interchangeably.’ Another example may be found in Applebaum who states, ‘the terms “competence” and “capacity” are used interchangeably in this article, since the oft-cited distinctions between them — competence is said to refer to legal judgments, and capacity to clinical ones — are not consistently reflected in either legal or medical usage.’ South African scholars such as McQuoid Mason, on the contrary, track the Children’s Act’s maturity and mental capacity test as may be seen from this quote: ‘. . .children may consent. . . if they are 12 years of age or more and of sufficient maturity and with the mental capacity to understand the benefits, risks. . .’. In other words, competence encompasses more than capacity in South African scholarship. See Ganya et al., ‘Autonomy of the Child’, p. 7; P. Applebaum, ‘Assessment of Patients’ Competence to Consent to Treatment’, The New England Journal of Medicine 357 (2007), pp. 1834–1840 at p. 1834; and D. McQuoid Mason, ‘Provisions for Consent by Children to Medical Treatment and Surgical Operations, and Duties to Report Child and Aged Persons Abuse: 1 April 2010’, South African Medical Journal 100 (2010), pp. 646–648 at p. 646.
30.
To avoid any doubt and to align with the Children’s Act’s own wording, this article uses ‘capacity’ to denote the child’s functional, decision-specific ability (to understand, weigh and communicate), ‘maturity’ to denote the broader developmental context (cognitive, social, and emotional development), and ‘sufficient maturity’ as the link between them in the Act’s dual threshold. It is for this reason that this article distinguishes terms that are sometimes used interchangeably in other jurisdictions. The aim here is to track South Africa’s statutory language accurately.
31.
Ganya et al., ‘Autonomy of the Child’, p. 4; Kruger, ‘Protection’, p. 8; Pillay and Singh, ‘Mental Capacity’, p. 540; J. Van Heerden, R. Delport, and M. Kruger, ‘Children’s Ability to Consent to Medical Management in South Africa’, South African Journal of Child Health 14 (2020), p. 26; and Havenga and Temane, ‘Consent by Children’, p. 44.
32.
Ganya et al., ‘Autonomy of the Child’, p. 4.
33.
A. Buchanan, and D. Brock, Deciding for Others: The Ethics of Surrogate Decision Making (Cambridge: Cambridge University Press, 1989), pp. 18–20 as discussed in Kruger, ‘Protection’, p. 8.
34.
Op. cit., p. 7.
35.
Op. cit.
36.
Ganya et al., ‘Autonomy of the Child’, p. 4.
37.
While the Children’s Act refers specifically to mental capacity, this article distinguishes it from legal capacity to highlight that legal recognition of a child’s decisional ability is often contingent upon both mental competence and legal entitlement under the law. See in general B. McSherry, ‘Legal Capacity and Neuroscience: Implications for Mental Health Laws’, Laws 4 (2015), pp. 125–138.
38.
Pillay and Singh, ‘Mental Capacity’, p. 540.
39.
Pillay and Singh are referring to legal tests for mental capacity drawn from criminal responsibility in terms of the Criminal Procedure Act 1977, as well as contractual capacity and testamentary competence. Although these provide useful conceptual insights, they function in different legal and developmental contexts and cannot be directly transposed onto the medical consent framework for children as governed by the Children’s Act.
40.
Christian Lawyers Association v Minister of Health (Reproductive Health Alliance as amicus curiae) 2005 (1) SA 509 (T).
41.
Strode et al., ‘Adolescent Self-Consent’, p. 136.
42.
Pillay and Singh, ‘Mental Capacity’, p. 540.
43.
Op. cit., p. 541.
44.
Op. cit.
45.
Van Heerden et al., pp. 25–29.
46.
Havenga and Temane, ‘Consent by Children’, pp. 44–45.
47.
J. Heaton, The South African Law of Persons (Sandton, South Africa: LexisNexis South Africa, 2017), p. 35.
48.
Strode et al., ‘Adolescent Self-Consent’, p. 137.
49.
Christian Lawyers Association v Minister of Health (Reproductive Health Alliance as amicus curiae) 2005 (1) SA 509 (T) para 56.
50.
Ganya et al., ‘Autonomy of the Child’, p. 2.
51.
Op. cit., p. 3.
52.
A. van Niekerk and N. Nortjé, ‘Phronesis and an Ethics of Responsibility’, South African Journal of Bioethics and Law 6 (2013), pp. 28–31.
53.
Ganya et al., ‘Autonomy of the Child’, p. 5.
54.
Op. cit.
55.
It appears as though the HIV policy therefore recognises cognitive capacity and the ability to act according to knowing or understanding as is found in the Criminal Procedure Act 1977 as well as the Child Justice Act 2008. South African National Department of Health, ‘Policy Guideline for HIV Counselling and Testing (HCT)’, 2009, p. 53, available at ![]() (accessed 9 July 2024).
(accessed 9 July 2024).
56.
Ganya et al., ‘Autonomy of the Child’, p. 2.
57.
Pillay and Singh, ‘Mental Capacity’, p. 541.
58.
Although ![]() provides an overview, it is necessary to clarify how these concepts operate together under South African law. In the Children’s Act, ‘mental capacity’ supplies the functional test (understanding, weighing, and communicating a decision in the particular context), while ‘sufficient maturity’ supplies the developmental threshold (the psychosocial readiness to assume responsibility for that decision). Read together, they form a dual requirement: capacity ensures that the adolescent can make the decision; sufficient maturity ensures that the decision is made from within a developmental stage where responsibility for consequences can realistically be borne. This interpretation explains why the Act retains both concepts and emphasises why this article’s inclusion of varying terminology clarify, rather than complicate, the assessment of minor or adolescent consent in practice.
provides an overview, it is necessary to clarify how these concepts operate together under South African law. In the Children’s Act, ‘mental capacity’ supplies the functional test (understanding, weighing, and communicating a decision in the particular context), while ‘sufficient maturity’ supplies the developmental threshold (the psychosocial readiness to assume responsibility for that decision). Read together, they form a dual requirement: capacity ensures that the adolescent can make the decision; sufficient maturity ensures that the decision is made from within a developmental stage where responsibility for consequences can realistically be borne. This interpretation explains why the Act retains both concepts and emphasises why this article’s inclusion of varying terminology clarify, rather than complicate, the assessment of minor or adolescent consent in practice.
59.
Section 2 Constitution of the Republic of South Africa, 1996.
60.
Op. cit., section 9.
61.
Op. cit., section 10.
62.
Op. cit., section 11.
63.
Op. cit., section 12.
64.
Op. cit., section 14.
65.
Op. cit., section 27(1)(a).
66.
Op. cit., section 28.
67.
Op. cit., section 39(1).
68.
See in general section 36 of the Constitution of the Republic of South Africa, 1996.
69.
Strode et al., ‘Adolescent Self-Consent’, p. 137.
70.
Christian Lawyers Association v Minister of Health (Reproductive Health Alliance as amicus curiae) 2005 (1) SA 509 (T) para 23.
71.
Op. cit.
72.
Pillay and Singh, ‘Mental Capacity’, p. 539.
73.
Section 12(2)(a) Constitution of the Republic of South Africa, 1996.
74.
H. Kruger, ‘Allowing Competent Children in South Africa to Refuse Medical Treatment: Lessons from England’, Stellenbosch Law Review 32 (2021), pp. 410–434.
75.
S v M (Centre for Child Law as Amicus Curiae) 2008 (3) SA 232 (CC).
76.
Kruger, ‘Allowing Competent Children’, p. 426.
77.
See in general Ganya et al., ‘Autonomy of the Child’, p. 6.
78.
M. Labuschagne, S. Mahomed, and A. Dhai, ‘Evolving Capacity of Children and Their Best Interests in the Context of Health Research in South Africa: An Ethico-Legal Position’, Developing World Bioethics 23 (2023), pp. 358–366.
79.
Section 12 Constitution of the Republic of South Africa, 1996.
80.
See in general section 36 of the Constitution of the Republic of South Africa, 1996.
81.
S v M (Centre for Child Law as Amicus Curiae) 2008 (3) SA 232 (CC) para 18.
82.
Section 12 reads as follows: ‘(2) Everyone has the right to bodily and psychological integrity, which includes the right— (a) to make decisions concerning reproduction; (b) to security in and control over their body; and (c) not to be subjected to medical or scientific experiments without their [emphasis added] informed consent.’
83.
Barkhuizen v Napier (CCT72/05) [2007] ZACC 5 (4 April 2007) para 57.
84.
Ganya et al., ‘Autonomy of the Child’, p. 5.
85.
Op. cit.
86.
Op. cit., p. 2.
87.
Op. cit.
88.
Kruger, ‘Allowing Competent Children’, p. 420.
89.
Section 27(1)(a) Constitution of the Republic of South Africa, 1996.
90.
Op. cit., section 7(2).
91.
Op. cit., section 27(2).
92.
M. Buchner-Eveleigh, ‘Children’s Rights of Access to Health Care Services and to Basic Health Care Services: A Critical Analysis of Case Law, Legislation and Policy’, De Jure 49 (2016), pp. 307–325.
93.
Section 7(g)-(j) and (l) Children’s Act 2005.
94.
S v M (Centre for Child Law as Amicus Curiae) 2008 (3) SA 232 (CC) para 26.
95.
Op. cit., para 18.
96.
Kruger, ‘Allowing Competent Children’, p. 426.
97.
S v M (Centre for Child Law as Amicus Curiae) 2008 (3) SA 232 (CC) para 24.
98.
Kruger, ‘Allowing Competent Children’, p. 426.
99.
Op. cit., p. 427.
100.
Op. cit., p. 420.
101.
D. S. Diekema, ‘Adolescent Brain Development and Medical Decision-making’, Pediatrics 146 (2020), pp. S18–S24, at p. S19; A. L. Katz and S. A. Webb, ‘Informed Consent in Decision-Making in Pediatric Practice’, Pediatrics 138 (2016), pp. 1–7.
102.
Cardwell v. Bechtol 724 S.W.2d 739 (1987).
103.
Van Heerden et al., ‘Children’s Ability to Consent’, p. 26.
104.
Gillick v West Norfolk and Wisbech Area Health Authority [1986] AC 112.
105.
See, for example, Re W (A Minor) (Medical Treatment: Court’s Jurisdiction) [1993] Fam 64 and Re E (A Minor) (Wardship: Medical Treatment) [1993] 1 FLR 386.
106.
P. A. Michaud, R. W. Blum, L. Benaroyo, J. Zermatten, and V. Baltag, ‘Assessing an Adolescent’s Capacity for Autonomous Decision-Making in Clinical Care’, Journal of Adolescent Health 57 (2015), pp. 361–366 at p. 362.
107.
P. Grootens-Wiegers, I. M. Hein, J. M. van den Broek, and M. C. de Vries, ‘Medical Decision-making in Children and Adolescents: Developmental and Neuroscientific Aspects’, BMC Pediatrics 17 (2017), pp. 1–10, at p. 3.
108.
I. M. Hein, P. W. Troost, A. Broersma, M. C. de Vries, J. G. Daams, and R. J. L. Lindauer, ‘Why Is It Hard to Make Progress in Assessing Children’s Decision-making Competence?’, BMC Medical Ethics 16 (2015), pp. 1–6, at p. 2.
109.
I. M. Hein, M. C. De Vries, P. W. Troost, G. Meynen, J. B. Van Goudoever, and R. J. L. Lindauer, ‘Informed Consent Instead of Assent Is Appropriate in Children from the Age of Twelve: Policy Implications of New Findings on Children’s Competence to Consent to Clinical Research’, BMC Medical Ethics 16 (2015), pp. 76–82, at p. 76.
110.
Pillay and Singh, ‘Mental Capacity’, p. 541.
111.
Op. cit., p. 545.
112.
B. Kolb, R. Mychasiuk, and R. Gibb, ‘Brain Development, Experience, and Behavior’, Pediatric Blood & Cancer 61 (2014), pp. 1720–1723, at p. 1720.
113.
Pillay and Singh, ‘Mental Capacity’, p. 541.
114.
Kolb et al., ‘Brain Development’, p. 1721.
115.
Diekema, ‘Adolescent Brain Development’, p. S21
116.
Kolb et al., ‘Brain Development’, p. 1721; B. J. Casey, J. N. Giedd, and K. M. Thomas, ‘Structural and Functional Brain Development and Its Relation to Cognitive Development’, Biological Psychology 54 (2000), pp. 241–257; Diekema, ‘Adolescent Brain Development’, p. S21; Grootens-Wiegers et al., ‘Medical Decision-making’, p. 5.
117.
Grootens-Wiegers et al., ‘Medical Decision-making’, p. 5.
118.
Diekema, ‘Adolescent Brain Development’, p. S21; Grootens-Wiegers et al., ‘Medical Decision-making’, p. 5.
119.
Katz and Webb, ‘Informed Consent’; Michaud et al., ‘Assessing an Adolescent’s Capacity’, p. 363.
120.
P.S. Appelbaum and T. Grisso, The MacArthur Competence Assessment Tool for Clinical Research (MacCAT-CR) (Sarasota, FL: Professional Resource Press, 2001).
121.
Grootens-Wiegers et al., ‘Medical Decision-making’, pp. 3–4.
122.
Op. cit., p. 4.
123.
Op. cit., p. 4.
124.
Op. cit., p. 3.
125.
Grootens-Wiegers et al., ‘Medical Decision-making’, p. 2; Diekema, ‘Adolescent Brain Development’, p. S20.
126.
L. A. Weithorn and S. B. Campbell, ‘The Competency of Children and Adolescents to Make Informed Treatment Decisions’, Child Development 53 (1982), pp. 1589–1598; Diekema, ‘Adolescent Brain Development’, p. S20.
127.
R. F. Weir and C. Peters, ‘Affirming the Decisions Adolescents Make about Life and Death’, Hastings Center Report 27 (1997), pp. 29–40, as cited in Diekema, ‘Adolescent Brain Development’, p. S20.
128.
Hein et al., ‘Informed Consent’, p. 3.
129.
Grootens-Wiegers et al., ‘Medical Decision-making’, p. 4.
130.
Hein et al., ‘Informed Consent’ p. 3.
131.
Kruger, ‘Protection’, p. 10.
132.
E. Cauffman and L. Steinberg, ‘(Im)maturity of Judgment in Adolescence: Why Adolescents May Be Less Culpable than Adults’, Behavioural Sciences & the Law 18 (2000), pp. 741–760, as cited in Kruger, ‘Protection’, p. 10.
133.
Diekema, ‘Adolescent Brain Development’, p. S20.
134.
Diekema, ‘Adolescent Brain Development’, p. S20.
135.
Grootens-Wiegers et al., ‘Medical Decision-making’, p. 5.
136.
Diekema, ‘Adolescent Brain Development’, p. S20; Grootens-Wiegers et al., ‘Medical Decision-making’, p. 5.
137.
Katz and Webb, ‘Informed Consent’, p. 5.
138.
Grootens-Wiegers et al., ‘Medical Decision-making’, p. 6; Michaud et al., ‘Assessing an Adolescent’s Capacity’, p. 363.
139.
Michaud et al., ‘Assessing an Adolescent’s Capacity’, p. 363.
140.
Katz and Webb, ‘Informed Consent’, p. 5.
141.
Michaud et al., ‘Assessing an Adolescent’s Capacity’, p. 363.
142.
Diekema, ‘Adolescent Brain Development’, p. S22; Grootens-Wiegers et al., ‘Medical Decision-making’, p. 6.
143.
Diekema, ‘Adolescent Brain Development’, p. S22.
144.
Grootens-Wiegers et al., ‘Medical Decision-making’, p. 6.
145.
Michaud et al., ‘Assessing an Adolescent’s Capacity’, p. 361.
146.
V. A. Miller, D. Drotar, and E. Kodish, ‘Children’s Competence for Assent and Consent: A Review of Empirical Findings’, Ethics & Behavior 14 (2004), pp. 255–295, as cited in Grootens-Wiegers et al., ‘Medical Decision-making’, p. 3.
147.
Pillay and Singh, ‘Mental Capacity’, p. 550.
148.
Grootens-Wiegers et al., ‘Medical Decision-making’, p. 7.
149.
Op. cit., p. 7.
150.
Hein et al., ‘Informed Consent’, p. 76.
151.
Michaud et al., ‘Assessing an Adolescent’s Capacity’, p. 364.
152.
Op. cit., p. 364.
153.
Op. cit., p. 364.
154.
Op. cit., p. 364.
155.
Op. cit., p. 365.
156.
Strode et al., ‘Adolescent Self-Consent’, p. 138.
157.
Appelbaum and Grisso, The MacArthur Competence Assessment Tool; Michaud et al., ‘Assessing an Adolescent’s Capacity’, p. 362; Hein et al., ‘Informed Consent’, p. 76.
