Abstract
The present study was designed to investigate the effect of embelin in metabolic endotoxemia (ME) mediated inflammation and associated obesity in high fat diet (HFD)-fed C57BL/6 mice. The molecular docking of embelin confirms its binding with the toll-like receptor-4 (TLR-4). In vivo study, mice were treated with HFD for 8 weeks to induce ME mediated inflammation and associated obesity. Further, mice were treated with embelin (50 and 100 mg/kg/day, p.o.) and orlistat (10 mg/kg/day, p.o.) from 5th to 8th week along with HFD to improve associated changes. After 8 weeks, mice were euthanized and assessed for body weight, body mass index (BMI), fat pad weights (mesenteric, retroperitoneal, and epididymal), intestinal permeability, TLR-4, tumor necrosis factor-α, interleukin-6, lipopolysaccharide, and serum lipid levels followed by histopathological analysis of liver and adipose tissues. Embelin significantly decreased the body weight, BMI, serum lipid levels, ME, and inflammation manifested by above parameters. Further, results of histopathological study showed that embelin restored the vacuolization, inflammation, one side shifting of nucleus in liver tissue, and decreased adipocyte cells size in adipose tissue in HFD-fed mice. Thus, our findings provide the strong evidence first time that embelin could modulate ME, mediate inflammation, and consequently reduce body weight gain, BMI, and serum lipid levels in HFD-fed mice.
Introduction
Metabolic endotoxemia (ME) generating from dysbiotic gut microbiota has been manifested as the important mediator in the pathogenesis of chronic low grade inflammation (CLGI) which plays a key role in development of obesity. 1 ME is characterized by increased plasma bacterial lipopolysaccharide (LPS) levels. LPS is a component of the cell wall of Gram-negative bacteria present in gut microbiome transit into systemic circulation due to the failure of gut barrier functioning or damage of intestinal epithelium. 2,3 Guo et al. described that LPS alters the intestinal permeability via increased expression of toll-like receptor-4 (TLR-4). 4 Further, LPS in systemic circulation binds with TLR-4 and leads to the increase in the expression of pro-inflammatory cytokines like tumor necrosis factor-α (TNF-α) and interleukin-6 (IL-6) that later contribute in the development of obesity. 5,6 Previous literature provides the strong evidence that high fat diet (HFD) plays a crucial role to facilitate the ME as results in gut barrier dysfunctioning which further involves in the development of the obesity. 1,7
An economic, effective, and safe alternative for conventional anti-obesity drugs is the need of the time. In the recent years, research on natural products/dietary phytochemicals has shown considerable interest as potential therapeutic agents to counteract obesity. Therefore, we hypothesized that the modification of ME, systemic inflammation, and decrease in intestinal permeability may provide a novel therapy to treat obesity.
Embelin (2,5-dihydroxy-3-undecyl-1,4-benzoquinone) is the major bioactive constituent of Embelia ribes (Family: Myrsinaceae) and has a wide spectrum of pharmacological activities including antitumor, antioxidant, analgesic, antifertility, wound healing, anticonvulsant, antidiabetic, antibacterial, anti-inflammatory, and anti-obesity potential. 8 –11 E. ribes commonly known as vidanga, widely distributed throughout India. One Ayurvedic formulation, vidangadya ĉurna (powder of vidanga), containing vidanga as a main ingredient is taken with honey to alleviate the obesity. 12 In a preliminary study, Bhandari et al. reported the anti-obesity potential of ethanolic extract of E. ribes in HFD-induced obesity in Wistar rats. 13 Further, Chaudhary et al. reported the protective effect of embelin in lipid metabolism and oxidative stress in HFD-induced obesity in Wistar rats. 14 Recently, Gao et al. reported that embelin inhibited the adipogenesis and lipogenesis in vitro via activation of canonical Wnt signaling pathway. 15 However, the effect of embelin in ME remains unexplored. Therefore, present study was designed to explore the effect of embelin on body weight gain via ME and inflammation in HFD-fed C57BL/6 mice. Here, we are providing a novel mechanism into the beneficial use of embelin in the management of obesity via modulation in ME and mediated inflammation.
Material and methods
Chemicals
Standard embelin (≥98% HPLC) and fluorescein isothiocyanate (FITC)–Dextran 4000 (DX-4000-FITC) were purchased from Chembio Lifesciences, Ghaziabad, Uttar Pradesh (UP), India. HFD (45% kcal fat, 20% kcal protein and, 35% kcal carbohydrates) was procured as a gift sample from Ashirwad Industries, Chandigarh, India. 16,17 Kits for measurements of lipids profile were purchased from Span Diagnostics, Ghaziabad, Uttar Pradesh (UP), India, and Elisa Kits for measurements of TLR-4, TNF-α, IL-6, and LPS were purchased from Genxbio Health Sciences Pvt. Ltd, Delhi, India.
Molecular docking analysis
The molecular docking was performed against TLR-4 protein receptor (organism: human) and carried out on Maestro, version 9.6 (Schrodinger Inc. USA). The protein for docking study was taken from protein data bank (PDBID: 5NAO). The ligand was sketched in 3D format using build panel and was prepared for docking using LigPrep application and prepared by removing solvent, adding hydrogen, and further energy minimization using protein preparation wizard. Grids for molecular docking were generated with standard ligand (orlistat). Embelin was docked using Glide extra precision (XP) mode, with up to three poses saved per molecule.
In vivo study
Animals
C57BL/6 mice of 6–8 weeks were procured from Central Animal House Facility of Jamia Hamdard, New Delhi, India, after the approval of Institutional Animal Ethics Committee (IAEC) as per Committee for the purpose of Control and Supervision of Experiments on Animals (CPCSEA) guidelines (Protocol No. 1391, Approval date—18/09/2017). Animals were maintained in a controlled room temperature (22 ± 2°C) and humidity (55 ± 5%) with a regularly followed 12-h day/12-h night cycle with food and water ad libitum. Animals had free access to a standard chow diet (normal control and per se group) or HFD (toxic control and treatment groups) for a period of 8 weeks.
Study design
Animals were divided into six groups, each group consisting of six mice and their treatment schedule was as follows: (1) Group I: mice fed with standard chow diet for 8 weeks + 1% gum acacia in 0.9% normal saline from 5th week to 8th week (normal control); (2) group II: mice received HFD for 8 weeks + 1% gum acacia in 0.9% normal saline from 5th week to 8th week (toxic control); (3) group III: HFD for 8 weeks + embelin (50 mg/kg/day, p.o.) from 5th week to 8th week (treatment I); (4) group IV: HFD for 8 weeks + embelin (100 mg/kg/day, p.o.) from 5th week to 8th week (treatment II); (5) group V: HFD for 8 weeks + orlistat 10 mg/kg/day, p.o.) from 5th week to 8th week (standard drug); (6) group VI: group received standard chow diet for 8 weeks + embelin 100 mg/kg/day, p.o. from 5th to 8th week (per se group). The dose of embelin was based upon the previous effect of embelin on body weight gain by Bhandari et al. 13 and Chaudhary et al. 14 and toxicological study of embelin by Debebe et al. 18 Food intake and water intake were measured daily and body weight was measured weekly. Mice were fasted overnight before euthanizing. Blood was collected via tail vein and centrifuged to separate serum and plasma. After the collection of blood samples, animals were euthanized and liver, adipose tissue, and colon tissue were removed, washed, wrapped, and stored at −80°C for the estimation of biochemical and histopathological parameters.
Assessment of anthropometric parameters
Body weight of mice were measured weekly and further, body mass index (BMI) was calculated by the formula: ratio of body weight and square surface area (g/m2), surface area was calculated by the formula: body surface (m2) = 0.007184 × weight (kg0.425) × height (cm0.725). 19
Assessment of serum lipids profile
Levels of serum total cholesterol (TC), low density lipoproteins (LDL), high density lipoproteins (HDL), and triglycerides (TGs) were determined by Span Diagnostics Kits according to the manufacturer’s instructions.
Assessment of TLR-4, TNF-α, IL-6, and LPS levels
TLR-4 levels in colon tissue, 20 TNF-α 21 and IL-6 21 levels in serum, and LPS levels 22 in plasma were measured using ELISA Kit, as per the instructions given by manufacturer (Genxbio Health Sciences Pvt. Ltd. India).
Intestinal permeability
To measure the intestinal permeability, DX-4000-FITC (500 mg/kg body weight, 125 mg/ml) was administered orally 1 h prior to withdrawal of the blood from the animals of all the groups. After 1 h, 120 µl of blood was collected from the tail veins of the animals of the all groups. The blood was centrifuged at 4°C at 12,000 × g for 3 min and plasma was collected and diluted with equal volume of PBS (pH 7.4). Diluted plasma was analyzed for DX-4000-FITC concentration with the fluorescence spectrophotometer at an excitation wavelength of 485 nm and emission wavelength of 535 nm. 23
Histopathological analysis of liver and adipose tissue
Isolated tissues of liver and adipose were stored in 10% formalin solution. Haematoxylin (H) and eosin (E) solutions were used to stain sections and observations were examined under Meiji microscope. Adipocytes sizes were estimated using Adiposoft from the Image J software (1.52u) Maryland, USA. 24
Statistical analysis
Significant differences of the body weight and BMI were analyzed by two-way analysis of variance (ANOVA) followed by Bonferroni’s post hoc test and significant differences of other parameters (LPS, TNF-α, IL-6, TLR-4, TC, LDL, very low density lipoproteins (VLDL), HDL, intestinal permeability) among groups were analyzed by one-way ANOVA followed by Tukey’s multiple comparisons test using Graph Pad Prism (5.0) software. Statistical significances were set at p < 0.05.
Results
Docking analysis
We performed in silico study of embelin drug against TLR-4 protein receptor (organism: human) and the docking studies reveal a common binding orientation of embelin in the catalytic binding pocket of TLR-4 protein receptor (PDBID: 5NAO). Herein, we reported the binding pose of embelin and also compared it with the standard drug, orlistat which is bonded with TLR-4 protein. Embelin showed binding interaction with backbone of TLR-4 protein receptor with the binding residues, that is, Ile3, Ser5, and Gln6. Embelin showed superimposition with orlistat and also showed same interaction in catalytic domain of TLR-4 protein receptor. Embelin showed better docking score (−1.964) than standard ligand (orlistat −0.776) (Figure 1).

Results of molecular docking of embelin and orlistat. (a) The binding mode of embelin (brown) is shown in the TLR-4 active site and important residues are highlighted with grey stick. (b) The binding mode of orlistat
Effect of embelin on body weight, BMI, food intake, and fat pad weights
Figure 2 showing the effect of treatment of embelin on body weight gain, BMI, food intake, and fat pad weights in C57BL/6 mice in different groups, respectively. The mice fed with HFD alone, that is, group II gained a significant body weight and BMI as compared to the normal control mice, that is, group I ( p < 0.01 at the 2nd week and p < 0.001 at the end of 3rd week to 8th week). On the contrary, the groups treated with embelin (50 and 100 mg/kg/day, p.o.), that is, group III and IV had shown significant decrease in body weight gain and BMI in comparison to the HFD-treated group, that is, group II ( p < 0.001) and the results were comparable with orlistat (10 mg/kg/day, p.o.), that is, group V. In addition, treatment of embelin showed a significant decrease in fat pad weights in HFD-fed mice. However, there was no significant difference between embelin per se group, that is, group VI and normal control group. Furthermore, there was no significant difference in food intake and water intake between HFD and HFD + embelin and orlistat-treated groups, significant difference was observed in food intake.

Effect of embelin on body weight (a), BMI (b), body weight gain (c), fat pad weight weights (d), and daily food intake (e). a p < 0.001 Normal control vs. HFD; b p < 0.001 HFD vs. embelin 50 mg; b p < 0.01 HFD vs. embelin 50 mg. c p < 0.001 HFD vs. embelin 100 mg and d p < 0.001 HFD vs. orlistat 10 mg. BMI: body mass index.
Effect of embelin on serum lipid levels in HFD-treated mice
Treatment of mice with HFD showed a significant increase in serum TC, LDL, VLDL, and TGs levels ( p < 0.001) and a significant decrease in serum HDL levels when compared with normal control group, that is, group I ( p < 0.001). Administration of embelin (50 and 100 mg/kg/day, p.o.) produced a significant decrease in serum TC, TGs, and LDL levels when compared with HFD-treated mice and the results were comparable with orlistat (10 mg/kg/day, p.o.) ( p < 0.001). Further, there was a significant increase in serum HDL levels in embelin (50 and 100 mg/kg/day, p.o.) and orlistat (10 mg/kg/day, p.o.)-treated groups ( p < 0.001). However, there was no significant difference observed in serum lipid levels between normal control and embelin per se groups (Table 1). All differences are determined by Tukey’s multiple comparison test.
Effect of embelin on serum lipids in HFD-fed C57BL/6 mice.a

HFD: high fat diet; TC: levels of serum total cholesterol; LDL: low density lipoproteins; HDL: high density lipoproteins; TGs: triglycerides; ANOVA: analysis of variance.
a Data are expressed as mean ± SEM. Significant differences were determined by one-way ANOVA followed by Tukey’s multiple comparison test.
b p < 0.001 Normal control vs. HFD.
c p < 0.001 HFD vs. embelin 50 mg.
d p < 0.001 HFD vs. embelin 100 mg.
e p < 0.001 HFD vs. orlistat 10 mg.
Effect of embelin on TLR-4, TNF-α, and IL-6 expression in HFD-treated groups
TLR-4 expression in colon tissue of intestine was statistically higher in HFD-treated mice when compared with normal control group ( p < 0.001). Treatment with embelin (50 and 100 mg/kg/day, p.o.) substantially decreased the TLR-4 levels in colon tissue ( p < 0.001). Orlistat administration (10 mg/kg/day, p.o.) showed significant decrease in the levels of TLR-4 in colon tissue when compared with HFD-treated group but decrease was less as compared to embelin-treated groups, that is, groups III and IV ( p < 0.01). However, there was no significant difference between embelin per se group and normal control group (Figure 3(a)).
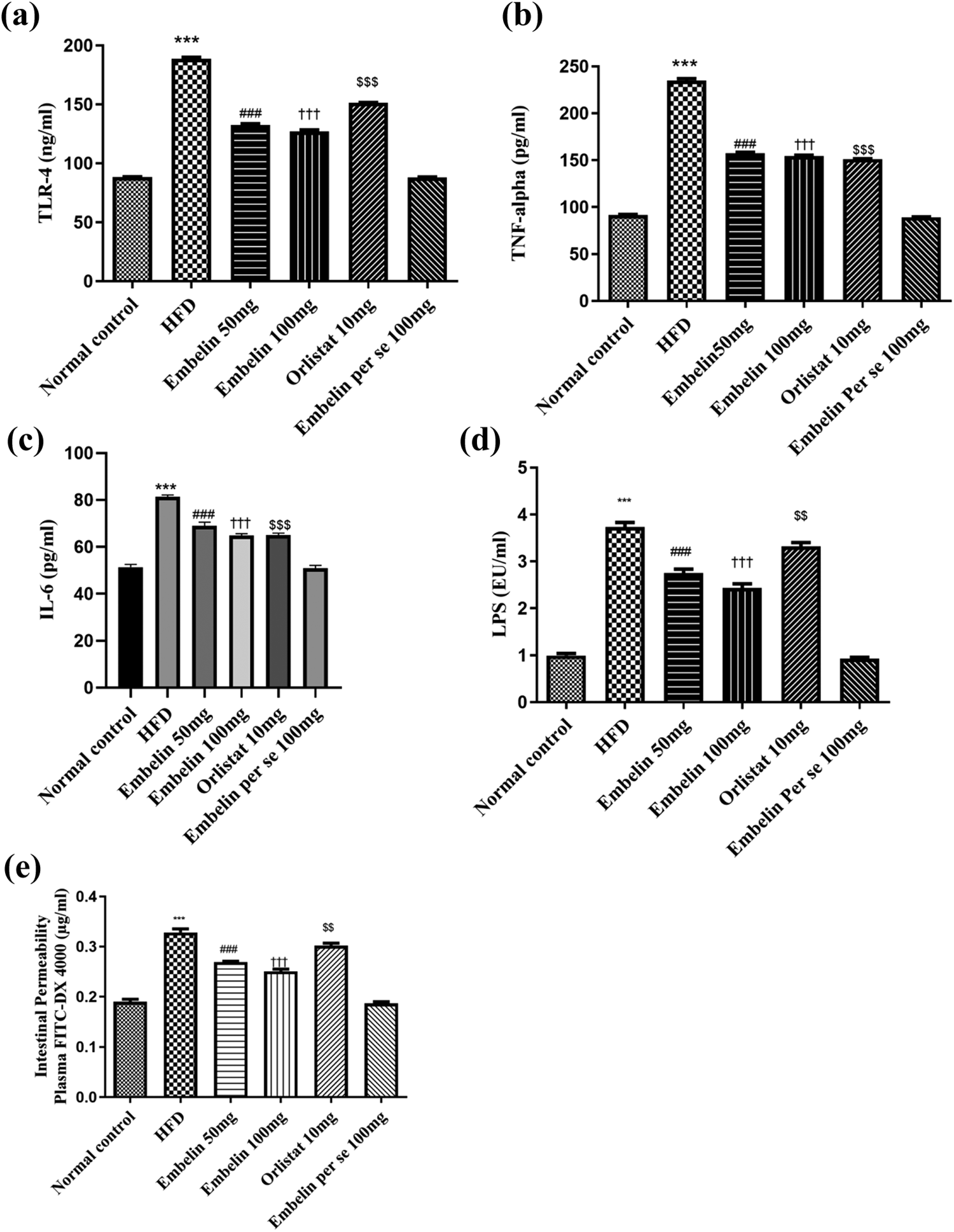
Effect of embelin on various parameters in HFD-fed C57BL/6 mice. (a) TLR-4, (b) TNF-α, (c) IL-6, (d) LPS, (e) intestinal permeability in normal control group, HFD, HFD + embelin 50 mg, HFD + embelin 100 mg, HFD + orlistat 10 mg and embelin per se 100 mg treated groups. Data are expressed as mean ± SEM. ***p < 0.001 Normal control vs. HFD; ### p < 0.001 HFD vs. embelin 50 mg; ††† p < 0.001 HFD vs. embelin 100 mg; $$$ p < 0.001 HFD vs. orlistat 10 mg, and $$ p < 0.01 HFD vs. orlistat 10 mg. HFD: high fat diet; TLR-4: toll-like receptor-4; TNF-α: tumor necrosis factor-α; IL-6: interleukin-6; LPS: lipopolysaccharide.
HFD diet treated mice showed significant increase in TNF-α level when compared with normal control mice ( p < 0.001). Treatment of embelin (50 and 100 mg/kg/day, p.o.) and orlistat (10 mg/kg/day, p.o.) significantly decreased the levels of TNF-α when compared to HFD-treated mice, that is, group II ( p < 0.001). However, the per se group showed nonsignificant difference when compared with the normal control group (Figure 3(b)).
Similarly, treatment of embelin (50 and 100 mg/kg/day, p.o.) and orlistat (10 mg/kg/day, p.o.) caused significant decrease ( p < 0.001) in the levels of IL-6 in HFD-fed mice as compared with only HFD-treated mice. There was no significant difference between the per se group and HFD group mice (Figure 3(c)).
Effect of embelin on plasma LPS concentration in HFD-treated mice
Treatment of mice with HFD (group II) showed significant increase ( p < 0.001) in the plasma LPS levels when compared with normal control group (group I). Embelin (50 and 100 mg/kg/day, p.o.) and orlistat (10 mg/kg/day, p.o.) showed a significant decrease ( p < 0.001 and p < 0.01, respectively) in the levels of LPS as compared to the HFD-treated animals (Figure 3(d)).
Effect of embelin on intestinal permeability in HFD-treated group
HFD treatment showed significant increase in the plasma concentration of DX-4000-FITC as compared to the normal control group ( p < 0.001). Treatment with embelin (50 and 100 mg/kg/day, p.o.) produced significant decrease in the plasma concentration of DX-4000-FITC ( p < 0.001). Administration of orlistat (10 mg/kg/day, p.o.) showed significant decrease ( p < 0.01) in the plasma concentration of DX-4000-FITC when compared with HFD-treated group. The embelin per se (100 mg) group showed nonsignificant changes when compared with the normal control group (Figure 3(e)).
Results of histopathological studies
Administration of HFD for a period of 8 weeks in C57BL/6 mice showed severe vacuolization and inflammation along with one side shifting of nucleus. Treatment of embelin (50 and 100 mg/kg/day, p.o.) and orlistat (10 mg/kg/day, p.o.) in HFD-treated mice showed restoration of vacuolization, inflammation, and shifting of nucleus but high dose of embelin (100 mg/kg/day, p.o.) showed more beneficial effect in reducing inflammation as compared with the low dose of embelin (50 mg/kg/day, p.o.) and orlistat (Figure 4; Table 2).
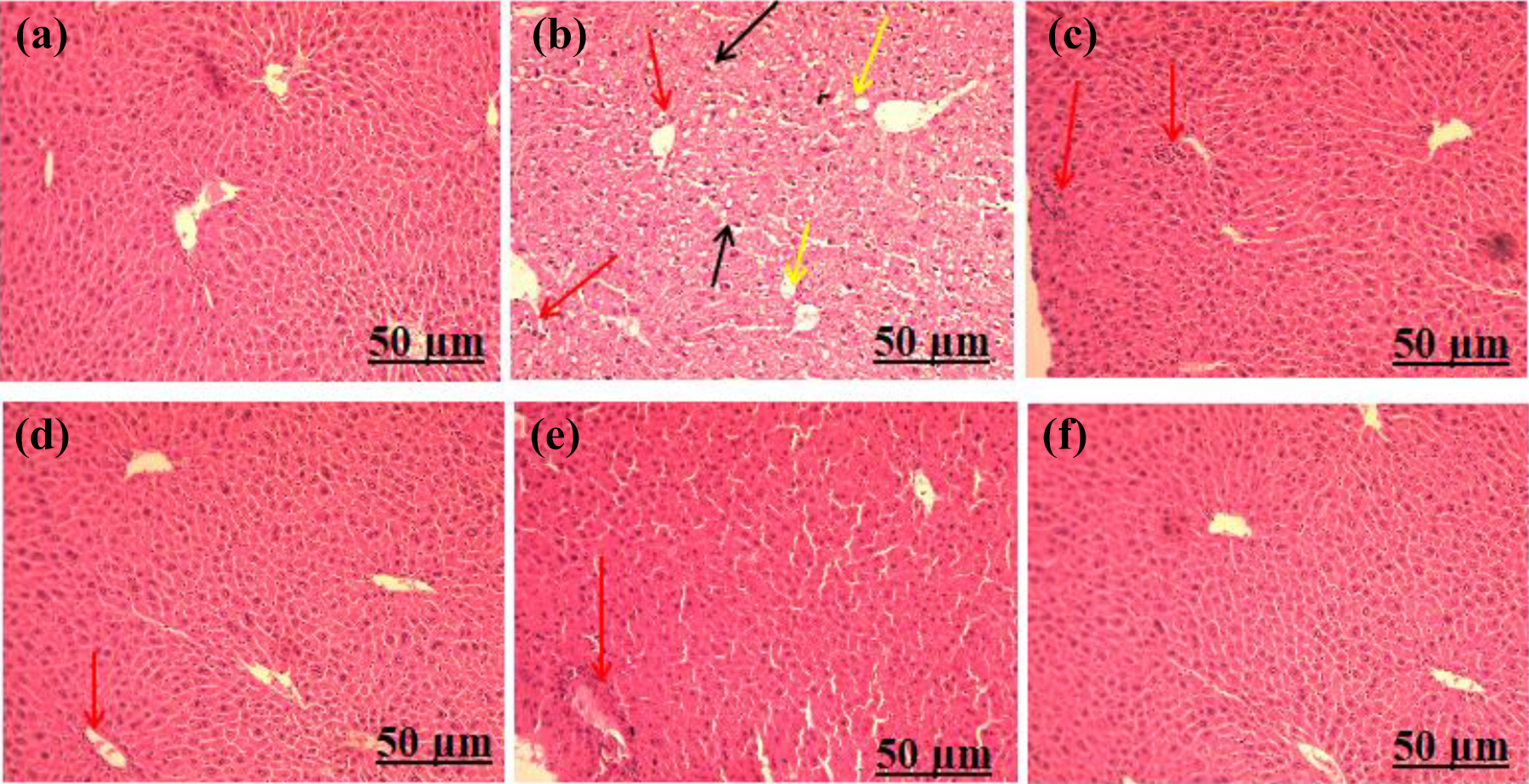
Photomicrograph showing histopathological changes in liver in different groups on 8th week (×10). (a) Normal control, (b) HFD treated, (c) HFD + embelin 50 mg, (d) HFD + embelin 100 mg, (e) HFD + orlistat 10 mg, and (f) embelin per se 100 mg. Yellow arrows: vacuolization, black arrows: one side shifting of nucleus, red arrows: inflammation. HFD: high fat diet.
Effect of embelin on degree of histopathological changes in liver tissue of HFD-fed C57BL/6 mice.a

HFD: high fat diet.
a The severity of changes are denoted as follows: 0 = no changes, + = mild changes, ++ = moderate changes, +++ = severe changes.
Figure 5 showing the effects of embelin treatment on adipocyte cell size in various groups. HFD administration for a period of 4 weeks caused significant increase in the number of large adipose cells when compared to the normal control groups. Embelin (50 and 100 mg/kg/day, p.o.) and orlistat (10 mg/kg/day, p.o.) treatments for a period of 4 weeks significantly reduced the adipocyte cells size in HFD-treated mice.

Photomicrograph showing histopathological changes in adipocyte cell size among several groups (×10). (a) Normal control, (b) HFD treated, (c) HFD + embelin 50 mg,
Discussion
ME and its associated CLGI play a crucial role in the pathogenesis of obesity and other health-related complications. 25 Modifying ME can be proposed as a safe and novel approach to prevent the development of obesity and its associated comorbid conditions. 17,25 Previous literature suggested that HFD administration in mice increases the synthesis of LPS in gut. Augmented LPS levels rise the TLR-4 expression in intestinal tissue and further altered the tight junction proteins that later increases the intestinal permeability. 4 Increased intestinal permeability allows the leak of LPS into systemic circulation (a condition called ME), circulatory LPS binds with TLR-4 receptors and increases the systemic inflammation; identifiable by increase in the levels of pro-inflammatory cytokines such as TNF-α and IL-6. 17,25 Pitocco et al. reported that gut microbiota has critical role in LPS translocation from intestinal barrier, modulating the lipids metabolism and increased fat deposition inside the body. 26 Hence, gut microbiota along with other inflammatory cascades plays a crucial role in developing insulin resistance that ultimately led to the development of obesity and other metabolic disorders. 17
Embelin, a major phytoconstituent of E. ribes, showed pleiotropic effects ranging from antioxidant to anticancer along with beneficial effects in metabolic disorders. 27,28 Additionally, Chaudhary et al. reported that embelin inhibits insulin resistance in HFD and low dose streptozotocin-induced diabetic nephrotoxicity in Wistar rats. 29 In the present study, we have screened the embelin and positive control, orlistat for their binding with TLR-4 receptor. We observed that among the two, embelin have higher affinity for the TLR-4 receptors (Docking score: −1.965). Previous literature also showed that TLR-4 might be a crucial key holder for the pharmacological activities of embelin. 30 Gao et al. reported that in an in vitro study embelin inhibited the adipogenesis and lipogenesis via activation of canonical Wnt signaling pathway. 15 Thus, considering the possible TLR-4 inhibitory activity of embelin along with other pleiotropic effects, we hypothesized that treatment with embelin might be an effective approach in reducing body weight gain and lipid levels via averting the ME and ME mediated inflammation. To the best of our knowledge, no previous study investigated the role of embelin via involvement of TLR-4 in the prevention of metabolic endotoxemia and its associated obesity.
In this study, HFD administration caused significant increase in the body weight gain and BMI with marginal changes in food intake. Thus, rise in body weight gain and BMI is occurred due to the high fat consumption rather than increase in food intake. Similarly, HFD consumption increases the serum TC, LDL, VLDL, and TGs level. Both conditions aggravate LPS and contribute to the chronic inflammation and obesity. 7 Treatment with embelin reverts this rise in body weight gain, BMI, and elevated serum lipid levels. Our findings are in the fine line with previously published literature. Chang et al. demonstrated that alleviating LPS levels reduces body weight gain, fat weight, and serum lipid levels in HFD-fed experimental animals. 21 Thus, the reversal of pathogenic changes by embelin is undeniably managed by controlling LPS levels and reliving ME. Our results (Figure 3) showed that HFD administration substantially increased the plasma LPS levels and intestinal TLR-4 levels in HFD-fed group. However, treatment with embelin (50 and 100 mg/kg/day, p.o.) for a period of 4 weeks in HFD-fed mice significantly reduced the plasma LPS levels, decreased the TLR-4 levels in the intestinal tissue as well as decreased the intestinal permeability; as manifested by decrease in the concentration of DX-4000-FITC ( p < 0.001). In the previous findings, Jiang et al. reported that administration of HFD for 8 weeks increased the intestinal TLR-4 expression and the gut permeability which further lead to the induction of ME and associated obesity which was reversed by the treatment of apple-derived pectin (5% wt/wt) for 6 weeks in HFD-fed Wistar rats. 31 Further, Kang et al. also reported that capsaicin 0.01% along with HFD was shown to modulate the intestinal TLR-4 expression and gut permeability, leading to the improvement in ME, mediated inflammation and associated obesity which were induced by administration of HFD in C57BL/6 mice. 17 Similarly, we have used the HFD for a period of 8 weeks for the induction of ME, its mediated inflammation and associated obesity which was reduced by the treatment of embelin (50 and 100 mg/kg/day, p.o.) as manifested by decrease in TLR-4 expression, and intestinal permeability, decrease in LPS levels as well as and biomarkers of obesity. Thus, our results have corroborated the findings of Jiang et al. 31 and Kang et al. 17
Additionally, earlier studies have demonstrated that TLR-4 activates the movement of pro-inflammatory cytokines such as TNF-α and IL-6 via NF-κB signaling. 32 In the present study, we also observed that HFD-fed mice showed abnormal upsurge in the levels of TNF-α and IL-6 which were substantially relieved with the embelin treatment as compared with HFD-fed C57BL/6 mice ( p < 0.001). Our results corroborates with the finding of Hogan et al. Authors reported the reduction in obesity by reliving the level of pro-inflammatory cytokines like TNF-α and IL-6. 33 Our data showed that embelin decreased the intestinal levels of TLR-4, suggesting that reduction in levels of pro-inflammatory cytokines may be mediated by dampening TLR-4.
Our histological studies reported the increase in size of adipose tissue in HFD-fed mice. Since adipose tissues are mainly involved in storage of excess nutrients but increase in size may cause lipid deregulation and mitochondrial dysfunction. 34 Increase in the size of adipocytes also upgrades the release of TNF-α in circulation. 35 Both of which contribute to the activation of inflammatory process. 34,35 However, the treatment of embelin (50 and 100 mg/kg) decreased the size of adipocyte cells as compared to HFD-treated group as shown in Figure 5. Gu et al. also reported that reduction in the size of adipocyte cells are correlational with the inflammation and ME in HFD-fed mice. Thus, our findings are in the fine line with the results of previous research work. 36
Our literature search suggested that liver is a key organ for the metabolism of lipids. Administration of HFD increases lipolysis in liver which uprise the free fatty acid flux and aggravates insulin resistance in muscle and liver through direct and indirect production of metabolites (triglyceride deposits). 37
In the present study, histopathological analysis of liver tissue showed that the administration of HFD caused vacuolization, one side shifting of nucleus and inflammation in liver which was later reversed by the embelin treatment. Embelin probably prevented the deregulation of free fatty acid metabolism and accumulation of TGs in liver cell, thus preventing hepatocyte damage.
The data from this study showed the prominence of embelin in avoiding pathogenic changes triggered by prolonged administration of HFD in mice. Our results were comparable to the standard drug, orlistat. Our findings from present study also strongly suggest the probable involvement of TLR-4 in the embelin mediated alleviation of ME and associated obesity.
Conclusion
Taken together, it is suggested that embelin can modulate ME, that is, increase in plasma LPS levels, by reducing the intestinal permeability as manifested by decreased concentration of DX4000-FITC. Further, the present study also revealed anti-inflammatory effect of embelin by suppressing the levels of TLR-4, TNF-α, and IL-6 in C57BL/6 mice. Furthermore, markers of obesity (body weight and BMI) and adipocyte size were decreased by embelin treatment. Decrease in serum lipid levels in embelin-treated mice further suggested the antihyperlipidemic effect of embelin.
Therefore, the conclusive results of our study provide strong evidences that embelin could modulate HFD-induced ME and CLGI, and consequently, reduces the weight gain, BMI, and serum lipid levels in HFD-fed C57BL/6 mice.
Footnotes
Acknowledgments
Authors acknowledge the support given by the Ashirwad Industries, Chandigarh, India, to give the high fat diet as a gift sample. Authors gratefully acknowledge the assistance of Dr AK Tiwari, Veterinary Pathologist, Incharge, Central Animal House Facility, Jamia Hamdard, India, for histopathological interpretation.
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
