Abstract
Fixed drug eruption (FDE) is an unusual drug-related side effect that results in recurrent lesions whenever the causative drugs are used. FDEs usually occur as a single, sharply demarcated, round erythematous patch or plaque, occasionally with localized bullae. The most common offending agents include antimicrobials, nonsteroidal anti-inflammatory drugs, and antiepileptics. There are some reports where contact dermatitis and cutaneous vasculitis have been associated with the use of flurbiprofen. We present the case of a 50-year-old man with flurbiprofen-induced generalized bullous FDE. To the best of our knowledge, the most serious form of FDE, the generalized bullous FDE, to be caused by flurbiprofen has not been reported previously.
Introduction
A fixed drug eruption (FDE) is a cutaneous reaction to an ingested drug that recurs at the same site each time the offending drug is taken. FDEs usually occur as a single, sharply demarcated, round erythematous patch or plaque, occasionally with localized bullae. However, generalized bullous FDEs are relatively rare and can be clinically confused with Stevens–Johnson syndrome (SJS). 1,2 We present the case of a 50-year-old man with flurbiprofen-induced generalized bullous FDE.
Case report
A 50-year-old man presented to our dermatology clinic with pruritic lesions on the trunk and limbs that started 6 h after taking flurbiprofen 100 mg. Family history was unremarkable. Patient’s medical records revealed that he had had similar symptoms without eroded areas 1 year earlier after having taken a single dose of flurbiprofen with 100 mg strength. Dermatological examination revealed multiple well-circumscribed, purplish-livid patches on the trunk and limbs (Figure 1(a) and (b)). Although intact bullae were not observed, eroded areas were noted on the trunk and limbs. The mucous membranes, the palms and soles, and the face were not involved. There was not any pathological finding in the physical examination. His temperature was 37°C, and his other vital signs were within the normal range. Laboratory findings showed the following values: white blood cell count of 14.5 × 109 L−1 (normal range, 4.5–11 × 109 L−1) and C-reactive protein of 11 mg L−1 (normal range 0–5 mg L−1). The rest of the tests were unremarkable. A biopsy specimen from one of the hyperpigmented lesions in the trunk was taken under local anesthesia. The histopathological examination showed hydrophic degenerations of the basal membrane, necrotic keratinocytes in the epidermis, pigment incontinence, and superficial perivascular lymphocytic infiltrate in the dermis (Figure 2). Biopsy findings were in line with the clinical diagnosis of FDE. Although we recommended a patch test with flurbiprofen for an accurate diagnosis, the patient refused the test. Based on clinical and histological findings, he was diagnosed with generalized bullous FDE. The patient was successfully treated with oral antihistamine and application of topical steroid. The patient’s lesions recovered after 4 weeks with residual hyperpigmentation.
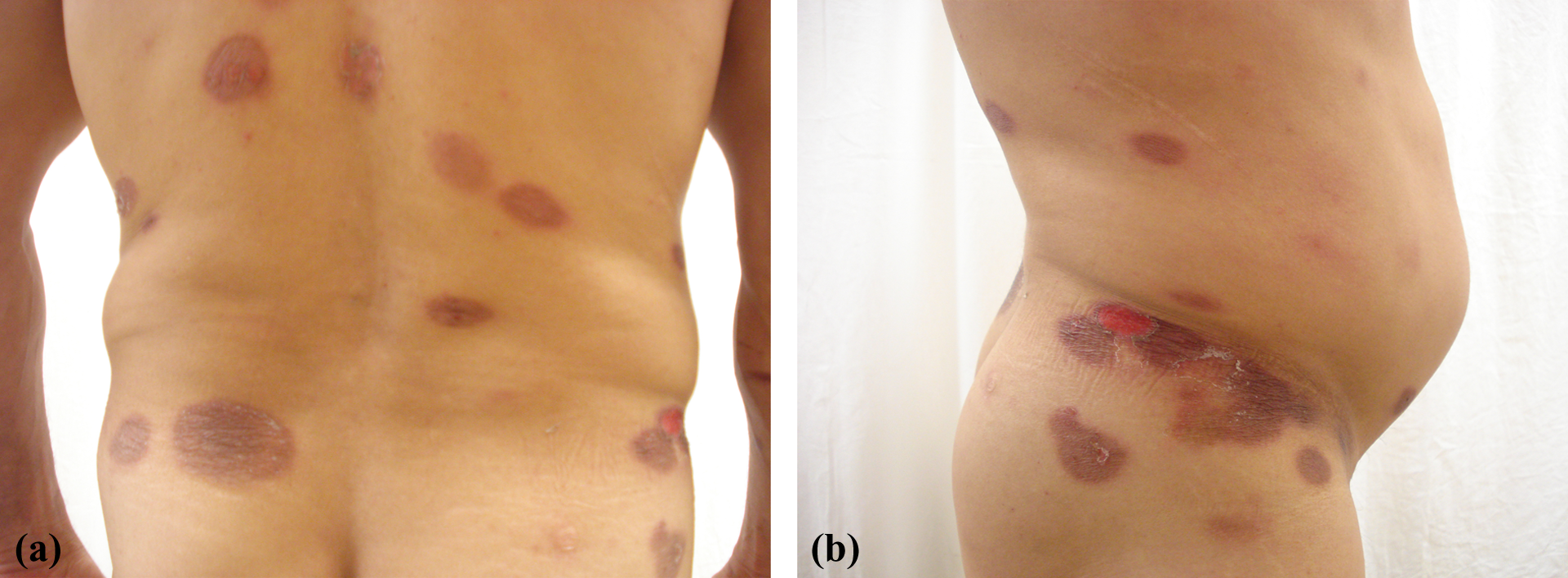
(a, b) Multiple well-circumscribed, purplish-livid patches, and eroded areas on the trunk and limbs.

Hydrophic degenerations of the basal membrane (dotted arrows), necrotic keratinocytes in the epidermis (straight arrows), and pigment incontinence (asterisk) (hema-toxylin and eosin, ×40).
Discussion
FDE is an unusual drug-related side effect that results in recurrent lesions whenever the causative drugs are used. 2 The pathogenesis is not clear, but cytotoxic memory CD8+ cells in the epidermis may play a major role in the pathogenesis. Severe epidermal damage in FDE lesions may be related to intraepidermal CD8+ T cells, which rapidly produce a large amount of interferon γ. 2,3
The most common offending agents include antimicrobials, nonsteroidal anti-inflammatory drugs (NSAIDs), and antiepileptics. 2,3 However, in the study by Andrade et al., they reported that FDEs have been associated in up to 40% of cases with NSAIDs. 4 Notable drugs among NSAIDs are phenylbutazone, ibuprofen, naproxen, piroxicam, and celecoxib. 2,3,5,6
In a previous study, the authors evaluated 450 patients with FDE to determine the causative drugs. According to the oral provocation test results, in 73% of the cases, co-trimoxazole was the most common causative drug. NSAIDs including metamizole (28%), phenylbutazone (24%) ibuprofen (4%), and diclofenac sodium (1.5%) were also reported in association with FDE. However, in none of the patients were found flurbiprofen as the causative drug. 7 Although there are some reports of the drug eruptions with flurbiprofen such as contact dermatitis and cutaneous vasculitis, but generalized bullous FDE has not been reported previously. 8,9
The severity of reactions in FDE may increase after repeated exposures to the drug and very rarely progress to a so-called clinical state of generalized bullous FDE. Generalized bullous FDE with its characteristic multiple large, purplish-livid patches, at times with flaccid blisters, may be clinically misdiagnosed as SJS or toxic epidermal necrolysis (TEN). The lesions heal rapidly without complication, leaving residual hyperpigmentation 10
Histopathological differentiation of generalized bullous FDE from SJS and TEN may be challenging. Epidermal changes varying from a few scattered necrotic keratinocytes to full-thickness epidermal necrosis cannot be distinguished in all the three conditions. In FDE, a mixed inflammatory infiltrate containing not only lymphocytes but also neutrophils and eosinophils is present around both the superficial and deep plexus. In SJS and TEN, the infiltrate is mainly lymphohistiocytic and tends to be located around the superficial plexus. 10
Systemic and topical provocation or challenge test may be used to confirm the causative drug in the case of FDE. Our patient had two episodes of FDE caused by oral intake of flurbiprofen. Based on the characteristic clinical and histological findings, it is not difficult to make a diagnosis of FDE. Generally, patch testing with the presumed drug will give positive results when it is applied to the lesional skin. There is usually no reaction in the topical provocation test on unaffected skin, although rarely there can be.
Based on clinical and histological findings, our patient was diagnosed with generalized bullous FDE. Differential diagnosis from SJS was applied with previous history of a milder drug eruption, but the lack of mucosal involvement and the rapid and uneventful recovery led to residual hyperpigmentation. Therefore, a detailed history, a careful physical examination, and a histopathological examination are essential in the differential diagnosis.
Footnotes
Funding
This research received no specific grant from any funding agency in the public, commercial, or not-for-profit sectors.
