Abstract
Naproxen is a non-steroidal anti-inflammatory drug (NSAID) widely used for symptomatic relief of arthritis and other painful disorders, such as dysmenorrheal. Pruritus is the most common side effect of naproxen. Fixed drug eruption (FDE) due to naproxen is a rarely reported side-effect. No previous report has declared cross-reactivity between naproxen and other propionic acid derivatives. A 28-year-old man, presented with edematous and erythematous patchy lesion along with pruritus and inflammation on lip, have been suffering since 3 hours. It started after taking naproxen 550 mg for headache. On detailed inquiry, he defined similar symptom which recurred after whenever he took naproxen. Based on clinical and histopathological findings, it is evaluated as naproxen-induced FDE. We have tested cross-reactivity between naproxen and other propionic acid derivatives, and then we obtained negative result for oral provocation test with flurbiprofen. Here, we present a case of naproxen-induced FDE of 28-year-old man, by overviewing literatures.
Introduction
Naproxen is a propionic acid derivative with analgesic, antipyretic and anti-inflammatory properties. It is widely used in clinical practice for painful and inflammatory disorders, such as arthritis. 1 Pruritus is the most common symptom with naproxen use. Fixed drug eruption (FDE) to naproxen is an uncommonly reported side-effect. 2
FDE is a skin reaction to some drugs even used within normal doses. It is a distinctive variant of drug-induced dermatosis with characteristic recurrence at the same site of the skin or mucous membrane. It is characterized with appearance of skin lesions in the instant of same drug ingestion. A number of case with fixed drug eruptions gradually increases in clinical practice due to increase in diversity of drugs.
Gold standard in diagnosis of FDE caused by drugs is the recurrence of skin lesions in same site of previous lesions involved whenever offending drug is taken. 3 First-line treatment for FDE is discontinuation of causative drug. Treatment otherwise is symptomatic. Systemic anti-histamines and topical corticosteroids may all be required. The patients should be informed about causative agent. 4
Case
A 28-year-old male patient admitted to our clinic, presenting with erythematous, inflammatory lesion on lip spreading to left shoulder and posterior region of neck. He suffered from an itchy and painful skin lesion approximately 3 hours after taking a single dose of naproxen 550 mg for a headache. On patient's symptom inquiry, he described that he had experienced similar symptom whenever taking analgesic containing naproxen after sport activity, and it disappeared after he discontinuing it. The lesion on his left shoulder healed with scar formation. Family and previous medical history of patient was normal.
On physical examination, there was erythematous and hyperpigmented plaque lesion of 5 × 5 cm in size on left shoulder (Figure 1 ). In addition to this finding, we detected well-defined, circular, edematous and erythematous multiple plaque lesions ranging 0.5–5 cm in size on per oral, neck and left palmar region (Figure 2 ). Other systemic examination was normal. Erythrocyte sedimentation rate, urinalysis, biochemical and complete blood count tests were normal.
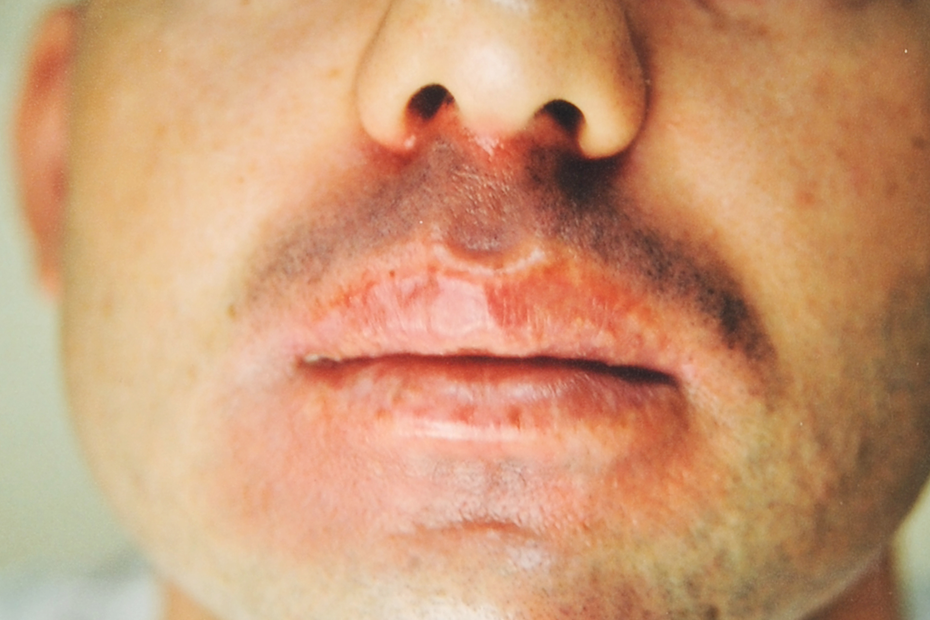
Multiple plaque lesions ranging 0.5–5 cm in size on per-oral 299 × 199 mm.

Hyperpigmented plaque lesion of 5 × 5 cm in size on left shoulder 299 × 199 mm.
Histopathological examination of sample lesion from left shoulders of patient, hydropic degeneration in basal lamina, pigment incontinence along with chronic inflammatory cell infiltration of lymphocytes and leucocytes around vascular structures were observed (Figure 3 ).

Hydropic degeneration in basal lamina, pigment incontinence along with chronic inflammatory cells infiltration of lymphocytes and leucocytes around vascular structures, there are amounts of melanin within macrophages in the upper dermis. (H&E ×100).
We diagnosed our case as FDE according to clinical signs, typical history of our patient and histopathological findings. Short-term systemic corticosteroid and oral anti-histaminic therapy was administered to patient. On second day of treatment, eruption was regressed.
We planned to perform provocation test for cross-reactivity with other propionic acid derivatives such as flurbiprofen before treatment administration. The patient was informed, informed consent was obtained. Flurbiprofene 100 mg in therapeutic doses, divided into three doses, was given to patient in 2-hours interval. No reaction to provocation test was observed. The patient was informed about naproxen use.
Discussion
Naproxen is propionic acid derivative which has anti-pyretic, anti-inflammatory and analgesic effect. It is mainly used in conditions resulting from inflammatory diseases and sport activities. Naproxen causes many side effects such as pruritus, eruptions and dyspepsia. Pruritus is the most common. 1,2 FDE was rarely reported in literatures. Other drug eruptions caused by naproxen are bullous photodermatitis, cutaneous vasculitis, purpura, urtikaria, hyperhidrosis, erythema multiforme and linear IgA dermatosis.1,3 Although cross-reactivity between naproxen and other propionic acid derivatives are expected, it is not proven and not reported in studies. 4,5
FDE is characterized by single or multiple erythematous, edematous, circular commonly seen cutaneous disorder. 1 Although it is reported in all age group, it is mainly seen between 21 and 40 years of age. FDE frequently involve lips, hand, trunk and genital regions. Of these areas, oral and genital involvement compromises more half the lesions. 6 Recurrence whenever causative agent is taken and occurrences in the same region within hours is gold standard for FDE diagnosis. 2
Etiology for FDE is not well known; nonetheless, it is considered to be late-type hypersensitivity reaction. Among drugs known to cause FDE are tetracycline, phenylbutazones, metronidazole and paracetamol. 1
Topical and oral provocation tests are helpful to find out agents that cause FDE. Topical provocation test (patch test) is safe to perform with suspicious agent in order to confirm diagnosis. Patch test has some limitations due to technical reasons in diagnosis: adjusting drug concentrations, selecting suitable tools, determining reaction time and modifying methods. Oral provocation tests are safe and effective to confirm diagnosis. 7 This test also has some disadvantages. These are anaphylactic reaction, old lesion reactivity and new lesion formation may be seen. Therefore, it should be performed in hospital conditions, and is performed before treatment administration, and patient should not have used anti-histaminic and corticosteroid agents within last 2 weeks. 8,9
Discontinuation of causative agent is main therapy for FDE. In severe cases, short-term systemic corticosteroid therapy can administered for rapid relief. For pruritus, oral anti-histaminic agents can be used. However, oral antihistaminic agent-induced FDE was also reported. 10
In our case, cross-reactivity with flurbiprofen was not observed. In previous studies, cross-reactivity with ibuprofen and ketoprofen was also obtained. 11 To our knowledge, it seemed to be first study in which cross-reactivity with flurbiprofene was studied. Consequently, no cross-reactivity between naproxen and other propionic acid derivatives was occurred as in previous studies. 12
Footnotes
This research received no specific grant from any funding agency in the public, commercial, or not for-profit sectors.
