Abstract
The aim of the present study was to evaluate the protective effect of aqueous extract from
Introduction
Biliary obstruction causes acute hepatocellular injury and leads to progressive fibrogenesis. It is also characterized by portal tract expansion, leukocyte infiltration, bile duct and septal proliferation, liver fibrosis and eventually cirrhosis. Although the mechanisms for the development of cholestatic liver disease are not well elucidated, oxidative stress may be an important causative factor. Cholestasis has been shown to stimulate the expression of collagen gene transcripts. 1 –3 Antioxidants have been shown to block stellate cell activation via type I collagen in hepatic fibrogenesis. 3 Endogenous antioxidant defense mechanisms could play a central role in preventing extensive injury in cholestatic livers. 4
The key pathological feature of hepatic fibrosis is the accumulation of extracellular matrix protein. It is well known that the fibrogenic cytokine transforming growth factor-beta (TGF-β) plays a pivotal role in the development of hepatic fibrosis and cirrhosis through its stimulatory effect on matrix protein generation and its inhibitory effect on matrix protein removal. 5,6 Therefore, an approach involving the inhibition of TGF-β1, a key member of the TGF-β superfamily, has been used in several therapeutic approaches to prevent hepatic fibrosis. However, there is no clinically effective treatment for liver fibrosis, and an effective therapeutic approach against the development of hepatic fibrosis is needed. 5 –7
Recently, a report described that Sho-saiko-to, the most popular herbal medicine for the treatment of chronic liver disease in China and Japan, and silymarin, a hepatoprotectant with anti-hepatitis C virus (HCV) activity, significantly reduced the expression of TGF-β1, and platelet-derived growth factor inhibited hematopoietic stem cell (HSC) proliferation and activation in a bile duct ligation (BDL) model of cirrhosis. 8,9 Herbal therapies and products derived from natural compounds such as silymarin and Sho-saiko-to may well prove to be of use as adjunctive measures in the care of patients with HCV, but there have not yet been any adequately designed clinical trials to support this assumption. 10,11
Herbal medicines that have been used in China for thousands of years are now being manufactured in Korea as drugs with standardized qualities and quantities of ingredients. The roots of
The aim of the current study was to investigate the beneficial effects of the standardized
Materials and methods
Chemicals and reagents
Assay kits for thiobarbituric acid reactive substances (TBARS), glutathione (GSH) and nitric oxide (NO) were purchased from BioAssay Systems (Hayward, California, USA). The assay kit for superoxide dismutase (SOD) was obtained from Cayman Chemical (Ann Arbor, Michigan, USA). Test kits for serum alanine aminotransferase (ALT), aspartate aminotransferase (AST), blood urea nitrogen (BUN) and total bilirubin (TBIL) were obtained from IDEXX (Westbrook, Maine, USA). TGF-β1 enzyme-linked immunosorbent assay (ELISA) kit was purchased from R&D systems (Minneapolis, Minnesota, USA). Other chemicals were obtained from Sigma chemicals (St Louis, Missouri, USA). High-performance liquid chromatography (HPLC)-grade acetonitrile and methanol were obtained from Mallinckrodt Baker (Phillipsburg, New Jersey, USA).
Preparation of standardized P. grandiflorum aqueous extract
The standardized
Animals and treatments
Male Sprague-Dawley rats weighing 250–300 g (8 weeks old) were obtained from Orient BioKorea (Seongnam, Korea). The rats were housed in the animal facilities of Chungnam National University Animal Research Resources Center on a 12-h light/dark cycle and fed with food and water ad libitum for 1 week before beginning the experiments.
The rats were anesthetized with an intraperitoneal injection of tiletamine (90 mg/kg) and zolazepam (10 mg/kg) and then their common bile duct were exposed through a midline abdominal incision. The common bile duct was ligated using double ligatures with 4-0 silk. The first ligature was made below the junction of the hepatic ducts and the second ligature was made above the entrance of the pancreatic ducts. Immediately after surgery, BDL rats were divided into three groups (
Twenty eight days after the BDL operation, the rats that survived were killed by cardiac puncture after being anesthetized lightly with carbon dioxide. Collected blood samples were separated by centrifugation at 800
Serum biochemical examination
The serum levels of ALT, AST, BUN and TBIL were determined using a dry chemistry system, VetTest 8008 blood chemistry analyzer (IDEXX, Westbrook, Maine, USA).
Hepatic lipid peroxidation, NO and GSH content
The content of malondialdehyde, a terminal product of lipid peroxidation, was measured using the thiobarbituric acid reduction method using a commercially available kit (QuantiChrom TBARS Assay Kit, BioAssay systems, Hayward, California, USA). Hepatic GSH levels were determined using the improved 5,5′-dithiobis-(2-nitrobenzoic acid) method (QuantiChrom GSH Assay Kit, BioAssay Systems, Hayward, California, USA). NO was determined using a colorimetric assay based on the Griess reaction (QuantiChrom NO assay Kit, BioAssay Systems, Hayward, California, USA). Total SOD activity in the hepatic homogenates was assessed on the basis of the superoxide disappearance detected using a tetrazolium salt (Cayman SOD Assay kit, Cayman Chemical, Ann Arbor, Michigan, USA).
Measurement of plasma TGF-β1 levels
Plasma TGF-β1 levels were measured using an ELISA kit (R&D systems, Minneapolis, Minnesota, USA) according to the manufacturer’s guidelines.
Histopathological examination
Liver slices were obtained from a part of the left lobe and fixed immediately in a 10% buffered formalin phosphate solution, embedded in paraffin and cut into 5 μm sections. Four random samples of each liver sample were stained with hematoxylin and eosin (H&E). Additionally, Masson’s trichrome staining was performed to facilitate the evaluation of periportal fibrotic bands. The degree of fibrosis was scored according to a modified histological activity index (HAI), 21,22 which included portal inflammation, focal necrosis, confluent necrosis, piecemeal necrosis, apoptosis, focal inflammation and fibrosis. The number of biliary canals in five portal sites for each section was also noted. The samples were examined without prior knowledge of the clinical information and biochemical results.
Statistical analysis
Results were expressed as mean ± SEM. The significance of the differences among the experimental groups was determined using one-way analysis of variance or the corresponding nonparametric (Kruskal–Wallis) test, as required. Where significant effects were found, post hoc analysis was performed using Tukey’s multiple comparison test or Mann–Whitney
Results
During the period of 4 weeks, there was no mortality in any of the experimental groups. However, all BDL rats showed progressive jaundice, ascites, hepatomegaly and slight splenomegaly except for sham-operated rats. Liver injury was assessed by determining the serum levels of liver enzymes including ALT, AST, CRE and TBIL (Table 1). As shown in Table 1, the serum levels of AST, ALT, CRE and TBIL were significantly higher in BDL rats than in sham-operated rats (
Effect of BC703 on serum biochemical parameters in BDL-induced cholestasis in rats.

ALT: alanine aminotransferase; BDL: bile duct ligation; AST: aspartate aminotransferase; BUN: blood urea nitrogen; TBIL: total bilirubin.
Values are expressed as means ± SEM (in survival animals). After BDL operation, the rats in BC703-treated groups were orally given BC703 (0, 10 and 50 mg/kg) once a day for 4 weeks. The sham-operated groups were orally given the same volume of saline as the BDL-treated animals that received BC703.
a
b
To evaluate the possible effects of BC703 on oxidative stress status, lipid peroxidation products, GSH and SOD, were measured in liver homogenates. These analyses showed significantly reduced activities of GSH and SOD, together with increased levels of NO and TBARS in the group treated with BDL alone (Figure 1). The hepatic TBARS level in the positive control group was significantly increased by 1.9-fold than that in the sham-operated group (

Effect of BC703 on TBARS (a), NO (b), GSH (c) and SOD (d) content in the BDL-induced cholestasis. After BDL operation, the rats in BC703-treated groups were orally given BC703 at 0, 10 and 50 mg/kg body weight/day for 4 weeks. The sham-operated groups were orally given with the same volume of saline as the BDL-treated animals that received BC703. Values are expressed as mean ± SEM. a
The HAI scores of the different experimental groups are summarized in Table 2. The livers of the animals in the sham-operated group had normal hepatic cells with well-preserved cytoplasm, a prominent nucleus, a nucleolus and visible central veins. In contrast, the livers collected from BDL-operated rats showed typical histological changes, which were characterized by bridge fibrosis formation in the portal area prominent ductular proliferation, edema and mild-to-moderate polymorphonuclear leukocyte and lymphocyte infiltration in the periportal region. The BDL rats that were treated with BC703 (50 mg/kg) had markedly reduced histological collagen accumulation, ductular proliferation, edema and inflammation than did the group treated with BDL alone (Figure 2).
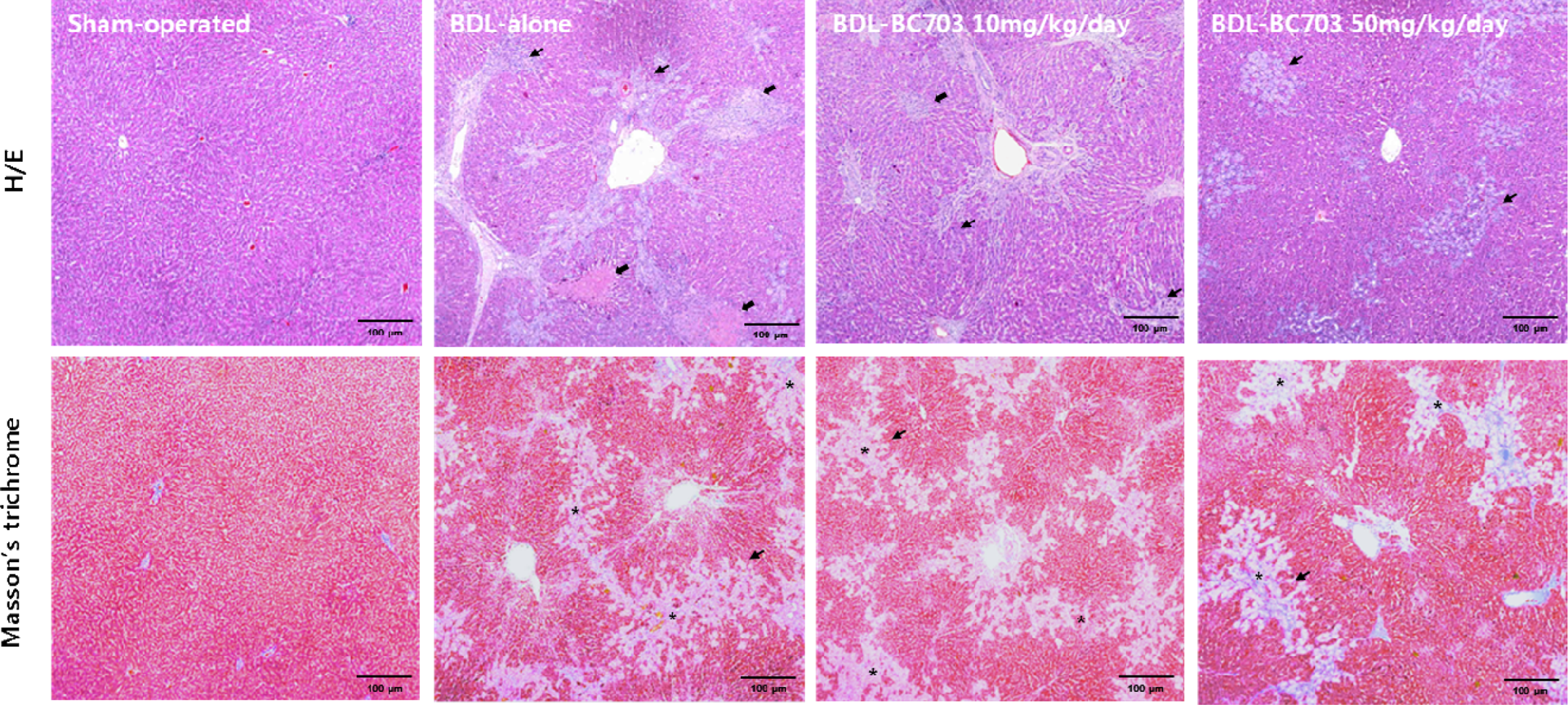
The histopathological changes in the liver in BDL-induced cholestasis stained with H&E and Masson’s trichrome stain (×40). After BDL operation, the rats in BC703-treated groups were orally given BC703 at 0, 10 and 50 mg/kg body weight/day for 4 weeks. The sham-operated groups were orally given with the same volume of saline as the BDL-treated animals that received BC703. The livers of the sham-operated rats had normal histological features of liver, but the livers collected from BDL-operated rats showed typical histological changes, which were characterized by bridge fibrosis formation in the portal area prominent ductular proliferation (thin arrows), mild-to-moderate PNL and lymphocyte infiltration (thin arrows) and piecemeal necrosis (thick arrows) in the periportal region. Asterisk indicates bridge fibrosis by ductular proliferation and collagen accumulation in portal area. BDL: bile duct ligation; H&E: hematoxylin and eosin; PNL: polymorphonuclear leukocyte.
Scores for necor inflammation (focal necrosis, confluent necrosis, piecemeal necrosis, focal and portal inflammation and apoptosis) and fibrosis using modified HAI grading system.
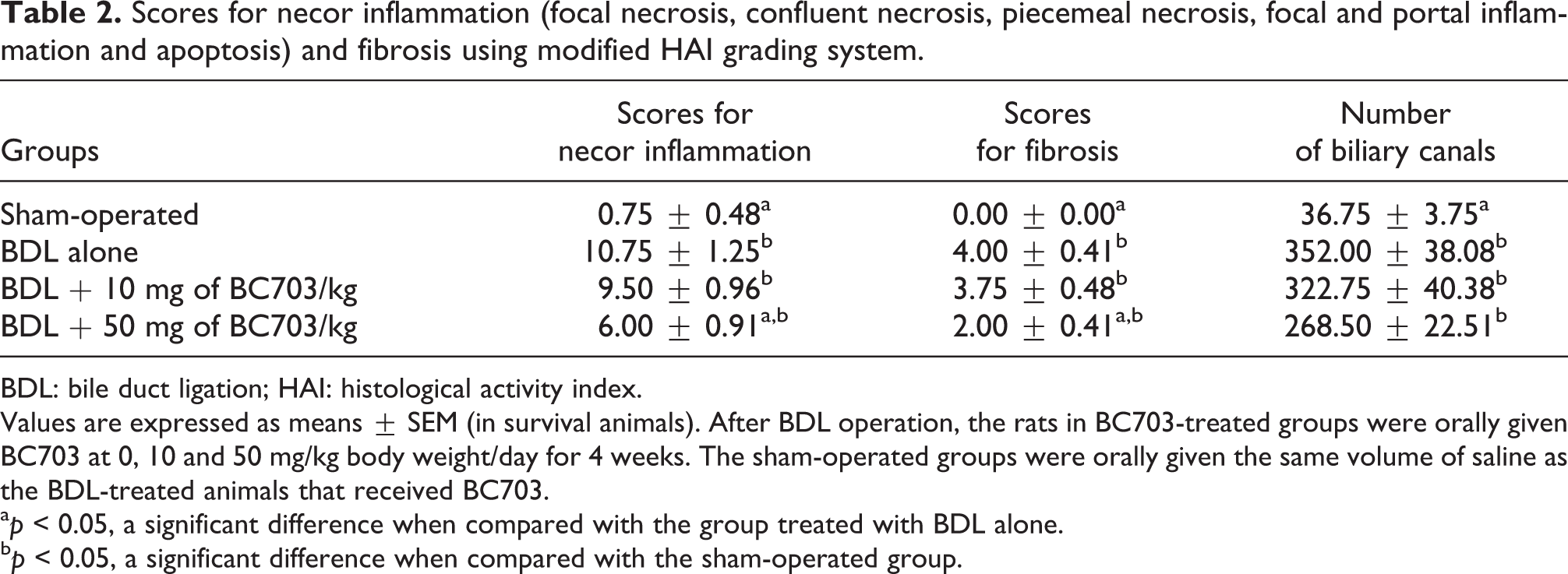
BDL: bile duct ligation; HAI: histological activity index.
Values are expressed as means ± SEM (in survival animals). After BDL operation, the rats in BC703-treated groups were orally given BC703 at 0, 10 and 50 mg/kg body weight/day for 4 weeks. The sham-operated groups were orally given the same volume of saline as the BDL-treated animals that received BC703.
a
b
The plasma fibrogenic cytokines, TGF-β, which play important roles in the activation of hepatic stellate cells, were significantly increased by 2.2-fold in the group treated with BDL alone (Figure 3). However, TGF-β1 production was significantly reduced in BC703-treated BDL rats than in the rats treated with BDL alone.

Serum level of TGF-β1 in the BDL-induced cholestasis. After BDL operation, the rats in BC703-treated groups were orally given BC703 at 0, 10 and 50 mg/kg body weight/day for 4 weeks. The sham-operated groups were orally given the same volume of saline as the BDL-treated animals that received BC703. Values are expressed as means ± SEM. a
Discussion
One of the standard animal models for research on cholestasis is the total ligation of the common BDL model. 23 During bile duct obstruction and the subsequent cholestasis, increased concentrations of bile acids and toxins in the liver result in the activation of Kupffer and hepatic stellate cells. 24,25
Serum levels of ALT, AST and TBIL are classical markers of obstructive cholestasis in the clinical setting. Clinically, the AST to ALT ratio is significantly elevated in patients with advanced fibrosis. 26 In this study, elevated serum levels of ALT, AST and TBIL, together with the AST/ALT ratio were observed in rats treated with BDL alone, but these elevations were ameliorated in the BC703-treated BDL groups.
BDL induces a type of liver fibrosis that etiologically and pathogenically resembles the biliary fibrosis in human.
27
The bile stasis and backpressure that occur because of the obstruction induce proliferation of the duct epithelial cells and looping and reduplication of the ducts, which is termed “bile duct proliferation”. The hepatocellular degeneration and death observed in cholestasis have been reported to be related to the retention of toxic bile salts, which leads to oxidative stress via the entry of nicotinamide adenine dinucleotide phosphate oxidase isoforms into the immune activation pathway.
3
,28
It has been suggested that hepatocyte apoptosis and/or necrosis may be associated with the activation of Kupffer cells, which release TGF-β and tumor necrosis factor-α.
3,5,6
Furthermore, TGF-β is upregulated in liver fibrosis and known to cause hepatic satellite cell proliferation and the production of collagen.
6
Increased TGF-β expression has been reported in bile duct-obstructed liver tissue and it leads to the pathological accumulation of extracellular matrix protein.
25,29
Intracellular oxidative stress is a major contributor to fibrogenesis, and recent studies have shown the induction of profibrogenic TGF-β1 by peroxide radicals, thereby providing a rationale for the use of intracellular antioxidants as adjunctive antifibrotic agents.
7,10
Several promising drugs derived from plants may be useful in antifibrotic combination therapy. Silibinin from milk thistle (
BC703 ameliorated hepatotoxic chemical-induced hepatic injury, which inhibited the production of excessive ROS and strongly inhibited HCV genotype 1b replicon replication in Huh7 cells.
19,20
In addition, triterpenoid saponins from
Recent findings suggest that the Wnt/β-catenin pathway is strongly involved in the normal activation and proliferation of adult hepatic progenitor cells in both acute and chronic human liver diseases.
30
Canonical Wnt/β-catenin signaling also suppresses the expression and promoter activation of peroxisome proliferator-activated receptor γ (PPARγ) in HSC transdifferentiation. Moreover, PPARγ agonists inhibit HSC activation and counteract liver fibrosis in models of cholestasis.
31
–33
In addition, some studies have shown that PPARγ agonist, such as rosiglitazone, improves steatosis and transaminase levels, which is an effect related to an improvement in insulin sensitivity.
31
It was recently reported that
In conclusion, the protective effect of BC703 against BLD-induced hepatic fibrosis may be mainly associated with the ability of this extract to attenuate oxidative stress and to inhibit TGF-β1. The capacity of BC703 to attenuate oxidative stress and suppress the release of TGF-β1, and the advantage of it being a nontoxic natural product are important factors that make this extract an interesting candidate for preventing and treating human hepatic fibrosis and cirrhosis.
Footnotes
Funding
This research was supported by iPET (Korea Institute of Planning and Evaluation for Technology in Food, Agriculture, Forestry and Fisheries), Ministry for Food, Agriculture, Forestry and Fisheries, Republic of Korea.
