Abstract
Boldenone is an anabolic steroid developed for veterinary use. Recently, it is used by bodybuilders in both off-season and precontest, where it is well known for increasing vascularity while preparing for a bodybuilding contest. However, the side effect of this steroid on the human health is still unclear. Therefore, the present study was designed to investigate the possible effect of the growth promoter, boldenone undecylenate, on the function and structure of the rabbit’s kidneys. A total of 36 adult New Zealand rabbits were divided into 4 groups. Control group includes animals that were injected intramuscularly with olive oil and dissected after 3 weeks. Three experimental groups include animals that receive one, two and three intramuscular injections of 5 mg/kg body weight boldenone, and dissected after 3, 6, and 9 weeks, respectively, and the interval of each dose of boldenone was 3 weeks. The biochemical analysis of the blood serum of treated rabbit showed a significant increase in the total protein, urea and creatinine concentrations, with a significant decrease in albumin/globulin (A/G) ratio. At the same time, a significant glomerulus mass reduction that accompanied with the expression of CD34, a marker for endothelial cells deterioration, was also determined. The incidence of the glomerulosclerosis was significantly increased compared with the control group (0.46 ± 0.05, p < 0.05). The glomerulosclerosis scores were 1.32 ± 0.10, 2.14 ± 0.11 and 3.02 ± 0.09 in groups 2, 3 and 4, respectively. These findings suggest that misuse of the boldenone undecylenate may contribute to the occurrence of a chronic renal injury that may lead to a progressive renal failure.
Introduction
Anabolic and androgenic steroids are synthetic substances related to the primary male sex hormone, testosterone. Their biological actions include anabolic effect promoting muscle growth, behavioral effect causing aggressiveness among others and haematopoietic effect which make the bodybuilders attractive candidates for enhancement of athletic performance. 1 –4 Certain veterinary products have the same mechanism of action and have been reclassified as schedule III drugs. These include boldenone, mibolerone, stanozolol, trenbolone and their esters and isomers. 5,6 Boldenone (BOL; 1,4-androstadiene-17β-ol-3-one) is obtained from dehydrogenation of testosterone. 7 –9 BOL is well known under the trade names Equipoise, Ganabol, Equigan and Ultragan. It improves growth and feed conversion in veal calves and therefore might be used illegally to achieve more efficient meat production. 10 Its role in increasing the muscle size is due to the promotion of positive nitrogen balance by stimulating protein production and reducing protein destruction. Moreover, it produces retention of body water, nitrogen, sodium, potassium and calcium ions. 11 BOL has a very long half-life and can show up on a steroid test for up to 1.5 years. This is because of the long undecylenate ester attached to the parent steroid. So, trace amounts of the drug can be easily detected for months after discontinued use. 12 –14 Its use is forbidden by European directives 96/22/EC and 03/74/EC to protect consumer’s health; and in the United States, it is not indicated for use in human and is only available through veterinary clinics. 12,14
Primary function of the kidney in plasma filtration is controlled by the integrity of the glomerular capillary tuft. Progressive capillary damage, with the destruction of the microvasculature, frequently accompanies fibrosis as a characteristic feature of the chronic renal disease. 15 Bohle et al. 16 and Kelly et al. 17 reported that the capillary damage closely correlates with declining function in a range of kidney diseases and may represent the endothelial component of a common adverse response to renal insult. At the same time, Haraldsson et al. 18 found that microalbuminuria is due to the increased passage of albumin through the glomerular filtration barrier. This barrier is composed of glomerular endothelial cells (GEnCs), a glomerular basement membrane and glomerular epithelial cells. GEnCs are covered by an endothelial surface layer. 19
CD34 is a transmembrane glycoprotein constitutively expressed as a surface membrane molecule of the immature normal human haematopoietic progenitors and leukemic cells. 20 It is also described as a marker in a variety of endothelial beds. 21 CD34 has potentially important roles in blood vessel formation as it is involved in cell adhesion process. 22 , 23 CD34 as other endothelial cell markers are modulated under pathological conditions. 21 In addition, being an adhesion molecule, CD34 plays a significant role in the maintenance of glomerulus function and in its alterations occurring by different pathological conditions. Generally, the increase in CD34 expression reflects its involvement in the pathogenesis of glomerular alterations. 24
Generally, misuse of the anabolic androgenic steroids caused some pathogenic effects such as disturbance of the endocrine and immune function, alterations of sebaceous system and skin, changes in haemostatic system and urogenital tract. 8,25,26 However, the effect of these steroids on the renal function and structure is still unclear. Therefore, the aim of the present study was to investigate the possible effect on the renal function and the integrity of the glomerular endothelial surface layer after BOL injection in rabbits.
Materials and methods
The experiment adhered to the guidelines of the ethical committee of the national research center, Egypt. The present study was conducted at Zoology Department, Faculty of Science, Tanta University, Egypt, during summer 2010.
Animals
The experiment was performed on 36 adult male New Zealand rabbits weighing 2.25 ± 0.1 kg and of 3–4 months age. The animals were fed ad libitum pellets of standard rabbit ration and free access to water ad libitum. Animals were divided into four groups (9 animals each). Control group (G1) includes animals that were injected with olive oil intramuscularly. The animals of the control group are subdivided into 3 subgroups and dissected after 3, 6 and 9 weeks, respectively. Animals of groups 2, 3 and 4 received 1, 2 and 3 intramuscular injections of 5 mg/kg body weight boldenone undecylenate and dissected after 3, 6 and 9 weeks, respectively, and the interval of each dose was 3 weeks. Boldenone undecylenate was dissolved in the olive oil. 14 At the end of the experiment, the rabbits were euthanized with intravenous injection with sodium pentobarbital and subjected to a complete necropsy.
Biochemical investigations
Blood samples were individually collected from the inferior vena cava of each rabbit in nonheparinized glass tubes to estimate the biochemical parameters. Blood serum was separated by centrifugation at 3000 rpm for 15 min. The collected serum was stored at −18°C. Blood serum was analysed to determine the concentration of the total protein, albumin, globulin, creatinine and urea spectrophotometrically using commercial diagnostic kits (AMS, Italy) and according to Gabr et al. 14
Histological preparation
The kidney was then immediately removed, sliced sagitally and fixed in 10% neutral-buffered formalin for 24 hours. The specimens were then dehydrated, cleared and embedded in paraffin. Serial sections of 5 μm thickness were cut by means of rotary microtome. Some sections were processed for haematoxylin and eosin. 27 Others were processed for immunohistochemical staining.
Immunohistochemical preparation
Avidin–biotin complex (ABC) method was used to localize CD34, a marker for endothelial cell deterioration. 28 Dewaxed and rehydrated sections were washed in distilled water for 5 min, rinsed in phosphate-buffered saline containing 0.3% Triton X-100 (PBST) for 10 min and incubated with 10% normal goat serum (Nichirei, Tokyo, Japan) for 15 min to reduce nonspecific background staining. Then, the sections were incubated with CD34 rabbit-human antiserum (N. Yanaihara, Shizuka, Japan, 1:1000) for 1–2 hours at room temperature.
The sections rinsed in PBST were then incubated for an hour with biotinylated goat antirabbit immunoglobulin (Nichirei, Tokyo, Japan). Then further incubated with ABC (Nichirei, Tokyo, Japan) for 1 hour at room temperature (RT). Negative control was attained by substituting CD34 primary antibody with normal serum of the goat.
The sections were analysed in a blind fashion. The severity of glomerular injury was evaluated by glomerulosclerosis score from 0 to 4 as described previously. 29 Grade 0, normal; grade 1, sclerotic area up to 25% (minimal); grade 2, sclerotic area 25–50% (moderate); grade 3, sclerotic area 50–75% (moderate to severe); and grade 4, sclerotic area 75–100% (severe). The glomerulus was considered the area internal to and including Bowman’s capsule. At least 50 glomeruli were randomly selected in 4 rabbits from different groups and the mean score was calculated. Then, the accurate sizes of their diameter were estimated by measuring their majors and minors perpendicularly.
Statistical analysis
Data were expressed as mean values ± standard error (SE) and statistical analysis was performed using one way analysis of variance (ANOVA) to assess significant differences among treatment groups. The criterion for statistical significance was set at p < 0.001 for the biochemical data and p < 0.05 for the histological data. All statistical analyses were performed using SPSS statistical version 16 software package (SPSS® Inc., USA).
Results
Analysis of blood parameters
Table 1 shows that serum total protein, globulin, urea and creatinine concentrations were significantly increased, while albumin and A/G ratio were significantly decreased (p < 0.05) after one, two and three intramuscular injections of BOL as compared with their values in the control groups.
Levels of total protein, albumin, globulin, urea and creatinine levels in serum of different groups under study a

a Data are expressed as mean ± SE of five observations. Superscripts of different letters differ significantly (p < 0.05) from each other.
Histological examination
Examination of haematoxylin and eosin–stained sections of control kidney cortex revealed a normal structure of the renal glomeruli. The glomerulus is enclosed by two layers of epithelium, surrounded by Bowman’s capsule (mesangial area). Cells of the outer or parietal layer of Bowman’s capsule form a simple squamous epithelium. Cells of the inner layer are extremely complex in shape and do not appear by routine histological staining. The glomeruli are round to oval in shape. The mean value of the glomerular diameter is 183.2 ± 2.07 μm. Group 2 which includes rabbits that received one intramuscular injection of blodenone showed a histopathological alterations in the renal glomeruli. The glomeruli lose their regular round to oval shape and appear irregular. A significant decrease in the size of the renal glomeruli was observed compared with the controls. The mean value of the glomerular diameter is 165.3 ± 1.87 μm (p < 0.05). Slight expansion of the mesangial area was also determined. Congestion and dilatation of the blood vessels were the most prominent feature in this group. Group 3 which includes rabbits that received two intramuscular injections of boldenone showed a multifocal glomerular injury. The glomeruli of group 3 rabbits appeared smaller in size compared with the control and group 2. The mean value of the glomerular diameter is 136.5 ± 1.88 μm (p < 0.05). Mesangial area appeared wider. In addition, markedly congested sinusoidal and dilated blood vessels were detected. Group 4 which includes rabbits that received three intramuscular injections of BOL exhibited severe histopathological lesions. Renal glomeruli completely lost their typical shape with the appearance of some vacuoles of different shapes and sizes. Marked decrease in their size was observed compared with the other groups. The mean value of the glomerular diameter is 127.9 ± 2.77 μm (p < 0.05). Mesangial area appeared wider compared with the other groups. Moreover, they had severe blood vessels congestion and dilatation (Figure 1 and Table 2).

Representative photomicrographs of rabbit’s glomeruli stained with haematoxylin and eosin. (A and B) Control rabbits group showing a normal structure of the glomeruli and a normal appearance of mesangial area (arrows). (C and D) Groups treated with one injection of boldenone. (E and F) Groups treated with two injections of boldenone. (G and H) Groups treated with three injections of boldenone showing irregular glomeruli with expanded mesangial areas (arrows), congested and dilated blood vessels (asterisks) and some glomerular vacuoles (arrowheads).
The renal glomerular diameter (RGD) and glomerulosclerosis scores in different groups under study a

a Data are expressed as mean ± SE. Different superscript letters differ significantly (p < 0.001) from each other.
Immunohistochemical examination
Immunohistochemical observation of the sections of control group kidney revealed a normal glomerular capillary pattern with CD34, a marker for endothelial cells, as it gave a negative expression with this antibody. Glomerular injury was evaluated by glomerulosclerosis score in all groups. The incidence of the glomerulosclerosis was very low in the sections of control group kidney. Glomerulosclerosis score was 0.46 ± 0.05. Alternatively, abnormal expression of CD34 was determined around the glomerulus in BOL-treated rabbits in groups 2, 3 and 4. The incidence of the glomerulosclerosis increased significantly in a severe manner when compared with the control sections and with other groups (p < 0.05). The glomerulosclerosis scores were 1.32 ± 0.10, 2.14 ± 0.11 and 3.02 ± 0.09 in groups 2, 3 and 4, respectively (Figure 2 and Table 2).
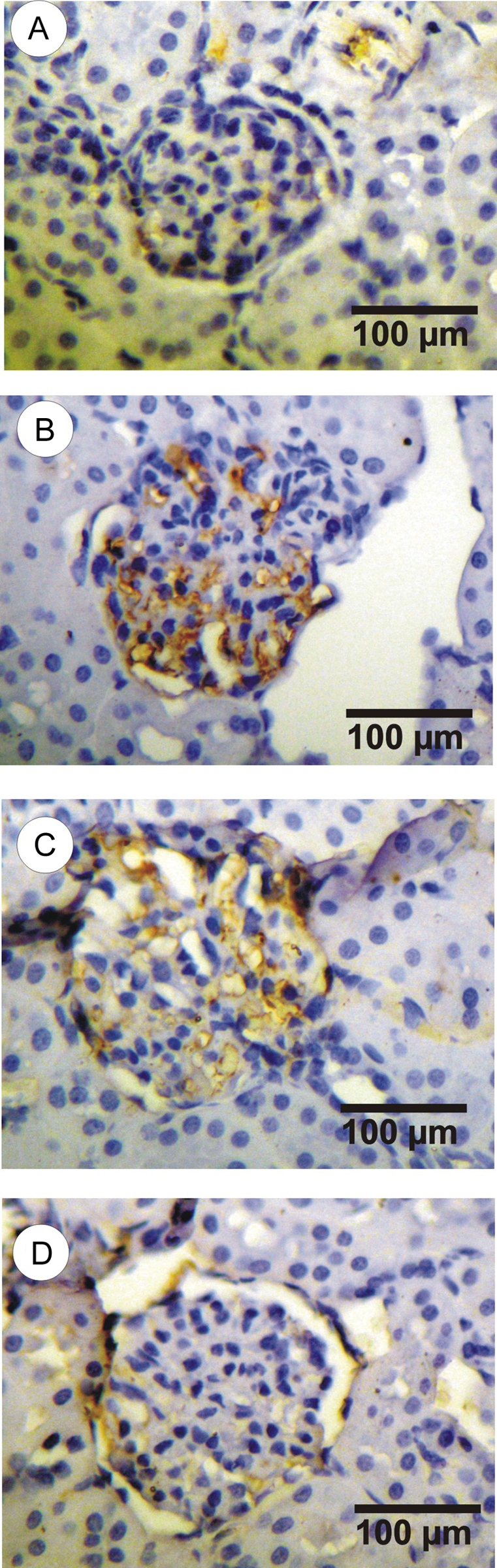
Representative photomicrographs of glomeruli labeled with CD34 antibody, a marker for endothelial cell deterioration. (A) Control rabbits group. (B, C and D) Groups treated with one, two and three injections of boldenone, respectively, showing CD34 expressions.
Discussion
Anabolic and androgenic steroids are synthetic substances related to the primary male sex hormone, testosterone. Their biological actions include anabolic effect promoting muscle growth, behavioral effect causing aggressiveness among others and haematopoietic effect making them attractive candidates for enhancement of athletic performance. 1,3,4 Here, we tested the effect of BOL injection on the function and structure of kidneys. The results showed a marked alteration in the biochemical parameters and the histological structure of the kidney after different doses of BOL injection. Biochemical analysis of the rabbit’s blood serum showed a significant increase in the total protein, urea and creatinine concentrations but showed a significant decrease in A/G ratio. Histopathological examination elucidated a significant glomerulus mass reduction that accompanied with the widening of the mesangial areas. These changes were adjunct to the severe congestion of the blood vessels and the expression of CD34, a marker for the endothelial cell deterioration. Incidence of glomerulosclerosis also appeared significantly high after BOL injection. Recently, Kuwabara et al. 19 reported that glomerular endothelial surface layer perturbation coincides with increased glomerular vascular permeability and albuminuria in a rat model of metabolic syndrome. Endothelial surface layer covers the systemic vascular endothelium and coats the luminal surface of the glomerular capillaries. They proved that the main function of these endothelial cells is to regulate the vascular permeability. A decrease in the thickness of the endothelial surface layer is associated with an increase in vascular permeability and the onset of albuminuria. 30 Furthermore, decreased thickness of endothelial surface layer was found to increase the GEnCs permeability in an in vitro study. 31
Other clinical studies have indicated that a decreased glomerular filtration rate and albuminuria are not only strong risk factors for end-stage renal disease but also cardiovascular events including coronary heart disease, heart failure, stroke and peripheral arterial disease. 32,33 Go et al. 33 recorded that an elevated urinary albumin excretion rate is associated with a two- to fourfold increase in cardiovascular and all-cause mortality rates. The risk of cardiovascular events increases with an increase in urine albumin–creatinine ratio, starting well below the microalbuminuria cutoff. 34
The structure of the endothelial surface layer and its mechanism indicated that it contains glycocalyx. This component regulates the vascular permeability, senses shear stress as a mechanotransduction sensor, attaches to blood cells, regulates enzyme activity and anchors enzymes to the cell surface. 30,35 –38 Jeansson et al. 39 demonstrated that reduction of the glomerular endothelial glycocalyx is involved in deterioration of permselectivity in an adriamycin-induced rat model of nephritic syndrome.
Our results are in agreement with a number of recent studies which provided evidence that anabolic steroid causes an adverse effect on the human health. Dickerman et al. 40 reported that using such steroids may cause hepatotoxicity. Welder et al. 41 recorded that anabolic androgenic steroids have toxic effects in the primary rat hepatic cultures. Gabr et al. 14 and Tousson et al. 42 reported that in spite of the growth-promoting effects, anabolic steroids have shown adverse effects in cardiovascular, hepatic and endocrine systems. Hartgens and Kuipers 43 reported that administration of anabolic androgenic steroids may cause some problems in the genital systems. Many other adverse effects such as the disturbance of the endocrine and immune function, alterations of the sebaceous system and skin, changes of the haemostatic system and urogenital tract associated with the misuse of anabolic androgenic steroids were recorded. 8,25,26
In conclusion, using BOL while preparing for a bodybuilding contest may cause an alteration in the biochemical parameters and the histological structure of the kidneys. These findings suggest that misuse of the growth promoter, boldenone undecylenate, may contribute to the occurrence of a chronic renal injury that may lead to a progressive renal failure.
Footnotes
This research received no specific grant from any funding agency in the public, commercial, or not-for-profit sectors.
