Abstract
Background
This case study investigated the effects of an progressive overload eccentric-tempo resistance training intervention (3sECC/1sCON) on muscle function in adults with mild and type I osteogenesis imperfecta (OI).
Methods
Eight adults with mild or type I Osteogenesis Imperfecta completed a mixed supervised and unsupervised six-week resistance training program with overloading protocols. Isometric squat (ISOS), countermovement jump (CMJ) and a 5 s sit to stand (5STS) test were undertaken pre- and post-intervention and evaluated by paired sample t-tests (p ≤ 0.05) and effect sizes. A numerical rating scale (NRS) questionnaire monitored muscle soreness and general musculoskeletal pain assessments and evaluated via a Wilcoxon signed rank test (p ≤ 0.05).
Results
Post intervention there was a significant increase in bodyweight normalised ISOS peak force (p = <.001; g = −2.205) as well as CMJ height (p = .017; g = −0.98), concentric impulse (p = .019, g = −0.953) and peak power (p = .035, g = −0.82). 5STS time was significantly reduced (p = .004; g = 1.343). Training muscle soreness (p = .027) and general musculoskeletal pain (p = .028) significantly decreased following the training intervention. No other significant changes between pre- and post-testing were observed.
Conclusion
An eccentric-tempo resistance training program improved muscle function and reduced muscle soreness and general musculoskeletal pain. This feasibility study provides the first insights into the potential benefits of resistance training, and proposes a framework for future practical prescription and research for adults with mild and type I OI
Introduction
Osteogenesis Imperfecta (OI) is a condition characterised by bone fragility giving it the name the ‘brittle bone disease’; with an incidence at birth of between 1: 10–20,000. 1 The majority of cases are highlighted by autosomal dominant mutational variants in the COL1A1 and COL1A2 genes; which are responsible for encoding the a1 and a2 polypeptide chains of type 1 collagen.1,2
Type 1 collagen makes up a significant amount of the total organic component of bone matrix profoundly affecting bone quality. 3 Individuals with OI suffer from wide-ranging skeletal pathologies such as various forms of dysplasia, low bone mass, high fracture frequency and stunted bone growth.4,5 However, type 1 collagen is not restricted to bone, as it also found in musculoskeletal tissues such as tendon, muscle and ligament. OI has been reported to result in musculoskeletal manifestations such as joint hypermobility and laxity as well as muscle weakness in both humans and mice.6–10 As a result, muscle weakness represents an important symptom toward OI diagnosis, 11 as strength deficiencies are commonly reported in individuals with OI when compared to healthy controls.12–15 Thus, it is no surprise that exercise and physiotherapy are widely recommended,3,16,17 underscoring the need for wide-ranging therapeutic modalities for condition management. However, a template for an exercise intervention to address such musculoskeletal symptoms for OI adults currently does not exist.
As an exercise (resistance training) modality, eccentric focused resistance training has been observed over a range of clinical conditions. 18 The use of submaximal intensities (60–70%1RM) during eccentric tempo-based training can elicite similar adaptations in muscle, tendon and strength19,20 as concentric focused maximal- and supramaximal intensity training. At present, neither fast or slow tempo are deemed superior with regards to hypertrophy and strength adaptations. 21 However, the consensus recommendation is a combination of slower eccentric and faster concentric phases. 21 Thus, the slower and varied eccentric-tempo exercise movement may be ideal for clinical and untrained populations due to lower loading strategies in a non-ballistic context that more replicate everyday movements such as descending stairs. 18 Therefore, submaximal eccentric tempo-based training that consists of faster concentric phases has the potential to benefit the muscle performance of OI sufferers.
To date, a lack of research has investigated the effects of resistance training as a form of physical therapy treatment on adults diagnosed with OI. To the authors knowledge, only a single study by Van Brussel et al. (2008) 22 has explored the use of exercise as a therapy on children with a mild to moderate OI phenotype, though this was restricted to basic exercises and light weights (∼1 kg). Therefore, the aim of the feasibility study is to investigate the viability of a supervised/unsupervised eccentric-tempo strength training intervention and whether this improves muscular performance via maximal and dynamic strength in mild and type I OI adults.
Materials and methods
Subjects
The current feasibility investigation recruited 8 participants (age = 35.9 ± 10.5 yr; height = 1.75 ± 0.46 m; body mass = 71.5 ± 16.3 kg; resistance training experience = 2.3 ± 2.9 yr; female = 6, male = 2). Inclusion criteria required individuals to be aged between 18 and 55 years old, be physically active, and have a self-reported OI diagnosis given by a medical practitioner, as per the expanded Sillence et al., (1979), 23 of type I or ‘mild’ OI either by a COL1A1, COL1A2 mutation or by the National Health Service in the United Kingdom and Ireland. Physical activity engaged by participants in the year prior to the study included erg-rowing, walking, swimming, running and pilates. Two participants reported to engage in strength training at least once per week. Exclusion criteria included long bone deformities, major scoliosis, fractures within the past 6 months and surgery within the past 12 months.12,15,24,25 Further, participants were excluded if they had no prior physical activity experience. All participants were informed of the outlined risks and benefits of the study. Written informed consent was obtained from each participant. Ethical approval was granted by the institutional awarding body (SMU_ETHICS_2022-23_089).
Procedures
The study examined the effects of a tempo-eccentric strength training intervention on muscle performance via a longitudinal analysis of adults with mild and type I osteogenesis imperfecta. Participants undertook pre- and post-testing separated by a 6-week training intervention. Prior to the commencement of data collection (week 0), each participant was assessed for their movement competency. Depending on their movement competency, participants completed a minimum of 1 and a maximum of 4 testing and exercise familiarisation sessions that were separated by at least 48 h over the week and a half preceding the intervention testing to ensure acceptable reliability. 26 Following initial familiarisation, and prior to the commencement of pre-intervention testing, the participant's chronological age, resistance training age, standing height and body mass were recorded. Standing height was measured barefoot using a stadiometer (Ecomed Trading, Seven Hills, Australia). Body mass was recorded using digital scales (Tanita Corporation, Tokyo, Japan). The pre-intervention testing required participants to complete the following physical capacity assessments in order, with a 3-min rest between tests: isometric squat (ISOS), countermovement jump (CMJ), and 5 s sit to stand (5STS). Both the isometric squat and CMJ were performed on a calibrated portable force plate (PASCO Scientific, Roseville, USA) measuring vertical force at 1000 Hz and analysed in custom software (ForceDecks version 2.0.8245,Vald, Newstead, Australia). A standardised warm-up, consisting of dynamic stretches followed by 2 sets of 5 repetitions of each exercise used in the training program was undertaken.
Brief descriptions of countermovement jump force key phrases and metrics.
Brief descriptions of countermovement jump force key phrases and metrics.
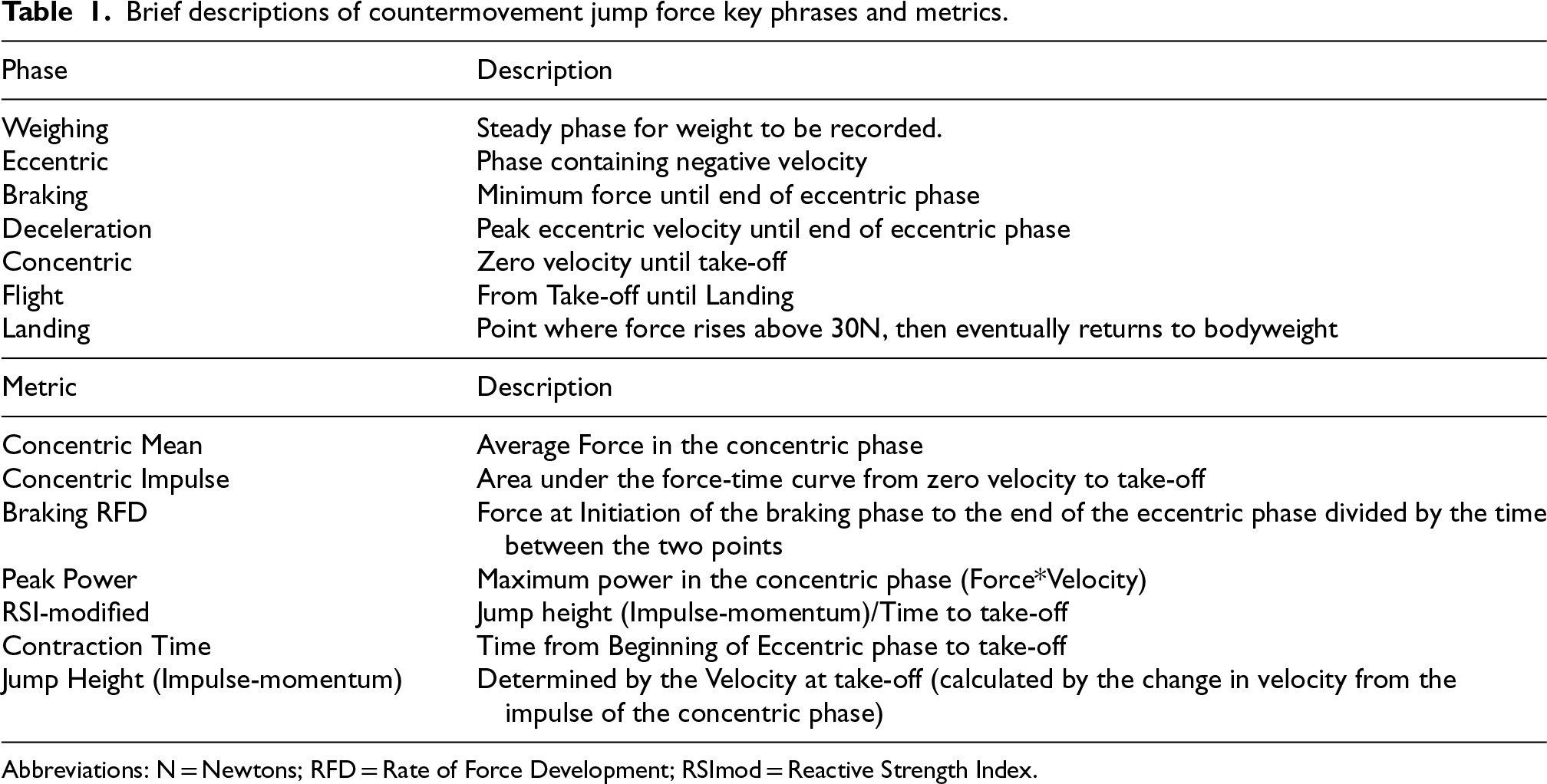
Abbreviations: N = Newtons; RFD = Rate of Force Development; RSImod = Reactive Strength Index.
Lower-limb maximal strength was assessed using a 120° isometric back squat on the aforementioned force plate within a customised power rack as previously described. 27 A universal goniometer was employed to standardise knee angle. 28 The subjects performed two warm-up attempts of the isometric back squat at 50 and 75% of perceived maximal effort. Individuals completed three maximal efforts that were separated by three minutes. 27 Strong verbal encouragement was given to each participant to push maximally into the floor for each effort. The best of three attempts were used for analysis. Peak force (PF) was determined as the primary outcome measure as it is a valid and reliable metric,29,30 and it correlates strongly with 1 repetition max (1RM) isoinertial squat performance. 27
Countermovement jump
Lower-limb dynamic muscle function was assessed via a CMJ on the aforementioned force plates as previously described. 31 Prior to CMJ testing, each participant performed 5 practice trials that increased in intensity. 32 Each CMJ was performed with arms akimbo, with legs extended during flight and self-selected countermovement depth. Trials that were performed with the addition of arms or tucking of the legs during flight were excluded and additional trials performed. 33 Participants performed three CMJ efforts that were separated by 1 min of passive rest. Participants were instructed to achieve a maximum jump height (JH) which is the standard protocol across clinical OI testing whilst also being the most reproducible when measuring peak power (PP). 15 Definition of phase and investigated force-time variables can be viewed in Table 1.
5-Second sit to stand
Relative pre- and post-testing ((mean ± standard deviation) and difference (mean difference ± 95% confidence limits [CL]) of isometric squat peak force measurements, sit to stand times, concentric mean force, concentric impulse, eccentric RFD, peak power, reactive strength Index, contraction time and jump heights (n = 8).
Relative pre- and post-testing ((mean ± standard deviation) and difference (mean difference ± 95% confidence limits [CL]) of isometric squat peak force measurements, sit to stand times, concentric mean force, concentric impulse, eccentric RFD, peak power, reactive strength Index, contraction time and jump heights (n = 8).
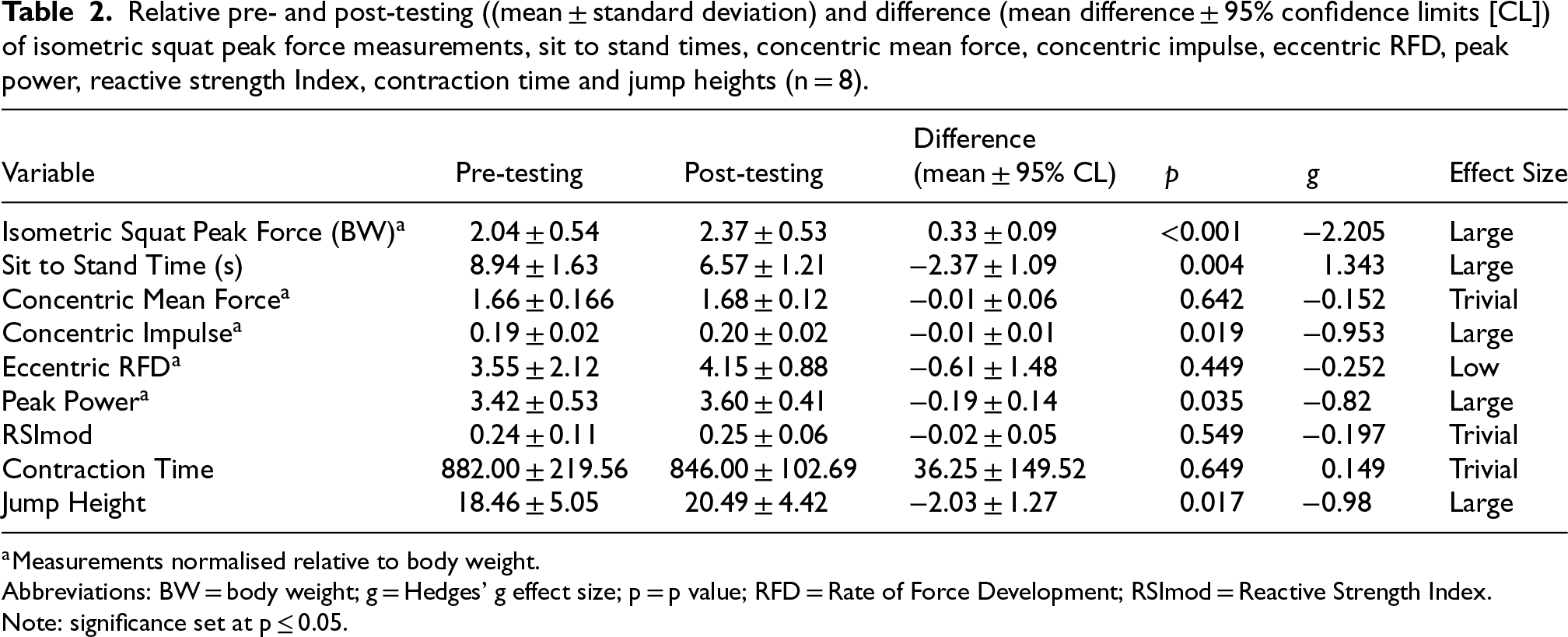
Measurements normalised relative to body weight.
Abbreviations: BW = body weight; g = Hedges’ g effect size; p = p value; RFD = Rate of Force Development; RSImod = Reactive Strength Index.
Note: significance set at p ≤ 0.05.
An outline of the 6-week eccentric-tempo training plan for participants is presented in Appendix 1 and 2. The training plan involved two exercises per session, twice a week on non-consecutive days (a minimum of 48 h rest between sessions). Periodization of the intervention plan follows block training and eccentric-tempo training guidelines.39–41 The two separate 3-week blocks are highlighted by differences in repetition and load (inverse), with the repetition in reserve (RIR) scale proposed by Zourdos et al. (2016) 42 adding the reference point for participant load self-prescription. A rating of perceived exertion (RPE) via the CR-10 scale was additionally employed to monitor intensity and the participants acute, somatic response to training. 43 Participants recorded their self-prescribed load and RPE during each training day, replacing the corresponding letter (Appendix 1). Given some participants had minimal resistance training experience, participants were familiarised with the RIR scale prior to the intervention during week 0.
Participants were instructed to play a metronome at the start of each set, allowing them to more accurately regulate tempo during each exercise. 44 Participant box-squat height for the intervention was controlled at the same height utilised for their 5STS test. Participants were instructed to cease all other resistance training during the study.
Statistical analyses
Descriptive statistics are presented as means and standard deviations. The Shapiro-Wilk test was employed to test the normality of data. 45 A two-tailed paired t-test assessed differences in isometric squat, CMJ, and 5STS test means between pre- and post-testing. Criterion alpha level was set at p ≤ 0.05 significance, with 95% confidence interval. Additionally, a Hedge's G effect size measure was employed to investigate the magnitude of group performance in the isometric squat, CMJ, and 5STS. The magnitude of Hedge's g follows the Cohen convention of small (0.2), medium (0.5), and large (0.8). 46 Finally, a Wilcoxon Signed Ranks Test was employed to analyse the change in participants pain and soreness scores between weeks 1 and 6. All statistics were computed using the Statistics Package for Social Sciences Version 29.0 (IBM, Armonk, USA).
Results
All data was normally distributed across all assessed variables. Results for the isometric squat are presented in Table 2. There was a significant difference of 15.95% between pre- and post-test body weight normalised PF means (p = <.001; g = −2.205). Regarding 5STS performance, there was a significant reduction of 26.5% between pre- and post 5STS performance (p = .004; g = 1.34).
Of the bodyweight normalised CMJ variables, concentric impulse (CI), PP and JH significantly increased by 6.8%, 5.3% and 11%, respectively. All improvements exhibited large effect sizes [CI (g = −0.953), PP (g = −0.820) and JH (g = −0.980)]. Concentric mean force (p = 0.642), eccentric rate of force development (RFD) (p = 0.449), reactive strength index (RSI) mod (p = 0.549) and contraction time (p = 0.649) did not significantly change as a result of the intervention. Muscle soreness (p = 0.027) and general musculoskeletal pain (p = 0.028) both significantly reduced across the exercise training intervention (Table 3).
Descriptive statstics for post-training muscle soreness and general musculoskeletal pain at baseline and week 6 of the resistance training intervention (n = 8).
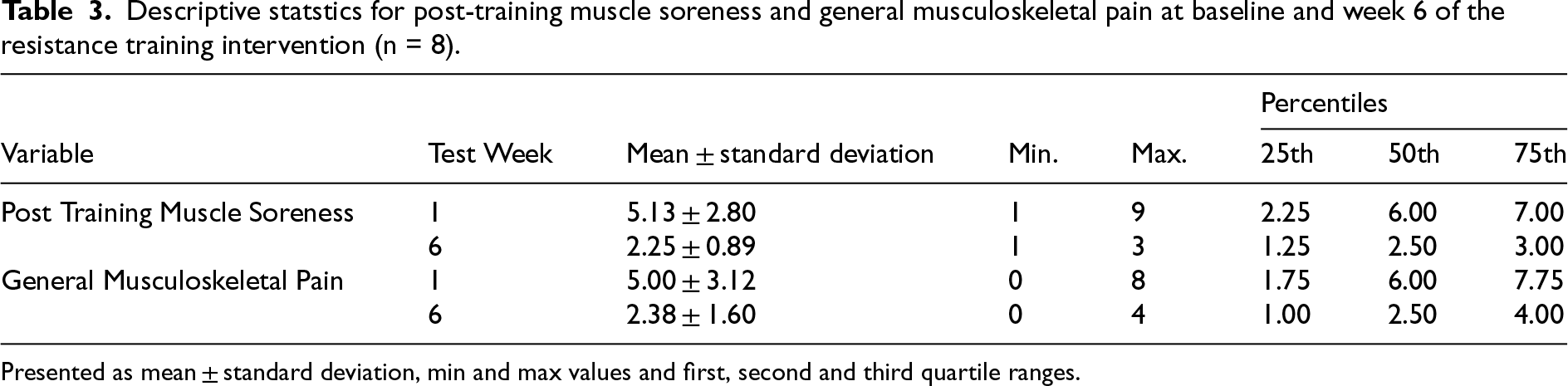
Descriptive statstics for post-training muscle soreness and general musculoskeletal pain at baseline and week 6 of the resistance training intervention (n = 8).

Presented as mean ± standard deviation, min and max values and first, second and third quartile ranges.
This is the first study to evaluate the effects of a six-week eccentric-tempo resistance training program on lower-limb muscle function in adults diagnosed with mild and type I OI. The main findings were that the resistance training program was successfully completed by 87.5% of participants remotely without complication and was able to demonstrate significant improvements in maximal and dynamic strength and power, as well as significant reductions in pain and soreness in a small sample of adults diagnosed with mild and type I OI. Seven out of eight participants completed all 12 sessions over the six weeks, with one participant missing 2 sessions due to being away. Such findings support the use of exercise therapy in improving independence and quality of life (QOL) outcomes in OI sufferers that likely possess reduced muscle strength and exercise tolerance capacities. 47 Finally, the results support the present methodology as a basis for larger resistance training-based studies in this population and provides an initial reference point for medical practitioners regarding resistance training exercise.
Importantly, as a feasibility study, the flexible exercise program employed appears applicable for mild and type I OI adults with little-to-no resistance training experience. The hybrid nature of intervention delivery, comprising both in-person and remote supervised training in addition to unsupervised training, aimed to instil confidence and self-efficacy amongst individuals with OI. Despite potential differences in the efficacy of unsupervised physiotherapy compared to supervised physiotherapy, 48 variables such as exercise selection and imparting movement knowledge can impact an individuals’ ability to successfully and regularly conduct unsupervised exercise.49,50 Amongst healthcare professionals, it been reported that there is a tendency to limit treatment options for OI due to fear of fracturing bones. 51 Thus, the present results may be foundational in changing the discourse around management for mild and type I OI. The flexibility of remote therapy may be more suitable for OI adults as using the home to conduct individual exercise training is a popular choice among this population. 52
The significant improvement in lower limb strength, assessed via the isometric squat, is a novel finding in OI populations. The substantial training effects may reflect the greater strength adaptations typically seen in less-trained individuals compared to those with prior resistance training experience. 53 Initial strength gains are often attributed to neuromuscular adaptations, which may explain the present results.54,55 Although not assessed here, such adaptations could enhance motor unit coactivation, improving joint stability and stiffness 56 —potentially beneficial for individuals with OI, given their predisposition to joint hypermobility and ligamentous laxity.8,57 Encouragingly, these findings also address muscle weakness, which may contribute to reduced bone strength in type I OI. 10 Previous research suggests that force magnitude, rather than its rate of development, influences bone mass remodelling. 24 However, as skeletal adaptations occur over months, further research is needed to explore long-term resistance training effects on skeletal mass quality in OI populations.
This is the first study to investigate changes in muscular power and dynamic strength through a CMJ as a result of resistance training in individuals with OI. While all CMJ variables tended to increase as a result of the resistance training program, only CI, PP and JH significantly improved (Table 2); possibly owing to the small sample size. The significant increase in JH contrasts past results from OI type I studies, where JH was employed as an instructional protocol and not as a true outcome measure. Rather, these studies reported PP as the only quantitative measure of muscular performance for the CMJ.15,58 One of these cross-sectional studies contained a similar demographic to the current study (mean age = 45.5) reported a lower mean PP of 2.5 Kw per body weight. 58 In contrast, the other cross-sectional study which involved youth participants (mean age = 12.6), reported a similar mean PP of 3.79 Kw per body weight. 15 However, it must be noted that jump height with regards to vertical jumping may not be a good indicator of maximal lower-limb power.59,60 It is well established that jumping ability depends on the velocity at take-off and preceding vertical net impulse. 60 In the current study, PP was shown to increase as a result of the eccentric-tempo training program, suggesting that such training prescription results in positive neuromuscular adaptations. Conversely, the lack of meaningful change in RSImod and contraction time may stem from the slow-velocity, eccentrically focused training, which is less effective in activating the stretch-shortening cycle (SSC).41,61 Moreover, vertical force-time data from a CMJ may not fully reflect muscle-tendon unit behaviour, 31 highlighting a need for future research in OI populations, particularly given the Achilles tendon's high type I collagen composition. 62 Nonetheless, the results of the present study provide additional evidence for an eccentric-tempo intervention in improving dynamic strength and power, but not SSC ability. Such results may increase independence; and give confidence for mild and type I individuals to participate in more exercise and non-contact sporting activities, although this depends on professional guidance. However, there are numerous examples of individuals with OI reaching high levels of sporting activity. 3 Lastly, this calls for the standardization of future OI research regarding CMJ measures in the assessment of dynamic strength; as assessing a wider range of variables as has been employed in the present study may better inform of changes to dynamic strength and jumping performance.
Finally, the large improvement observed in 5STS performance infers meaningful change in functional muscle strength and participant ability to repeatedly sit and stand. The 5 repetition 5STS test has previously been employed in research on OI type I participants. 25 Although no data currently exists for cut-off times amongst individuals with a mild or type I OI phenotype, the improvement in 5STS performance reported in the current study (8.9 ± 1.6 vs 6.6 ± 1.2 s) infers a meaningful shift away from times associated with physical impairment in other populations, and towards cut-off times representative of healthy individuals (6.2 ± 1.9 s). 63 The significant improvement in the 5STS test suggests that an eccentric-tempo resistance training program may help adult patients with mild and type I OI to achieve key treatment outcomes such as improved mobility and functional independence. 64 The importance of this improvement in 5STS performance in OI adults is evident as past research has reported a meaningful relationship between physical function and the ability to undertake fundamental tasks such as walking and climbing stairs. 65
Indeed, all participants completed the intervention injury-free. Participants were supervised via online consultation for the first 3 weeks and unsupervised for the last 3. Participants demonstrated that they were successfully able to self-manage their training loads throughout the six-week exercise training program, incorporating progressive overload, including the weeks where they were unsupervised. The observed reduction in participant musculoskeletal pain across the six-week program suggests that such an exercise therapy may help alleviate generalised pain typical of OI. Anecdotally, some participants reported improvements or elimination of lower-back pain, which may be noteworthy given it is a commonly reported symptom in among mild OI adults. 57 Past research has reported a trend in pain limiting levels of physical activity and influencing QOL in adults with mild and moderate OI. 65 However, the extent to which general musculoskeletal pain experienced by mild and type I OI adults limits lifestyle factors, and how exercise or sedentary behaviour affects the severity of OI symptoms remains to be determined.
Training related muscle soreness also significantly improved across the six-week exercise intervention, as is typical of apparently healthy cohorts. Two participants that reported no or trivial musculoskeletal pain and training related muscle soreness throughout the intervention, also possessed the most resistance training experience. As expected, there was high levels of training related muscle soreness initially reported for the rest of the cohort. Training-related muscle soreness is influenced by multiple factors, reflecting its complexity. A key contributor is the limited resistance training experience of most participants, which likely heightened their soreness and related indicators. 66 Additionally, the eccentric-tempo training program, emphasizing eccentric-focused exercises, is well-documented for inducing muscle soreness and extracellular matrix (ECM) damage. 67 This damage, particularly to the ECM, is theorized to underlie the soreness phenomenon. 68 Eccentric contractions are known to cause greater collagen breakdown and ECM remodelling than concentric contractions due to their propensity for microtrauma in connective tissue, 69 where type 1 collagen plays a crucial role. 72 ( 70 ) Furthermore, ECM reconstruction following eccentric contractions is delayed, potentially prolonging muscle recovery. 71 Notably, the relationship between OI-associated type I collagen mutations and muscle ECM remains unexplored. Given the ECM's critical role in skeletal muscle adaptation and function,69,72 further research is warranted to better understand OI pathology and its implications for exercise tolerance and adaptation.
The present study is not without limitations. Firstly, despite the positive results from the timed 5STS test, a shortfall of the present methodology was the absence of force-time data which would have provided more detail around changes in muscle performance and power. Secondly, the heterogeneity of supervision amongst participants may have altered individual results, as supervised exercise programs demonstrate greater training adaptations than unsupervised training. 48 However, this novel blended supervision approach employed in the current study is proposed to be more widely applicable than fully supervised exercise for OI populations. Further, the addition of a non-intervention control group would improve the temporal strength of the study. 73 As no comparison group exists, any causal relationship and interpretation of intervention effectiveness must be met with caution. For future and larger research on exercise interventions for OI, it seems beneficial to employ a repeated measures design where participants act as their own controls. Controlling for individual differences in a condition characterised by phenotype and genotype variability, even within OI classifications, can reduce confounding variables and help eliminate between participant noise when comparing treatment outcomes. 74 Lastly, having a larger sample size would increase the statistical power of the study, though the aim of this study was not solely to hypothesis test but to determine if study design and participant involvement was replicable for future research.
Conclusion
In conclusion, the present feasibility study demonstrates that an eccentric-tempo resistance intervention with overloading protocols could be employed at larger scale within mild and type I OI populations whilst inferring positive adaptations to strength capacities and pain outcomes. The current program appears safe and may be undertaken remotely with self-prescribed training loads under professional guidance. This study provides a framework for medical practitioners and greater research into strength training as a therapeutic option for adult individuals with OI, in the hope to improve QOL and reduce injury.
Footnotes
Acknowledgements
Many thanks to the Brittle Bone Society who sponsored this study with regards to participant recruitment. Thanks to the participants for their time and effort.
Ethical approval and informed consent statements
Written informed consent was obtained from each participant. Ethical approval was granted by the institutional awarding body (SMU_ETHICS_2022-23_089).
Authors contributions
CJNB participated and contributed to study design, data collection, data analysis, interpretation of results and manuscript writing and accepts responsibility for the integrity of the data analysis; SDP contributed to study design and manuscript writing; SJC contributed to study design and manuscript writing. All authors reviewed and edited the manuscript and approved the final version of the manuscript.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Declaration of interest
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Appendix 1: The six week periodized strength training program.

| Lower-limb training plan Day 1 | |||||||||||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| Week | 1 | 2 | 3 | 4 | 5 | 6 | |||||||||||||
| Sets | Reps + Load | Load (kg)a | Sets | Reps + Load | Load (kg)a | Sets | Reps + Load | Load (kg)a | Sets | Reps + Load | Load (kg)a | Sets | Reps + Load | Load (kg)a | Sets | Reps + Load | Load (kg)a | Tempo (s) | |
| Box Squat | 3 | 9 + 4RiR | X | 3 | 9 + 3RiR | X | 3 | 9 + 2RiR | X | 4 | 5 + 4RiR | X | 4 | 5 + 3RiR | X | 4 | 5 + 2RiR | X | 3Ecc/1Con |
| Y | Y | Y | Y | Y | Y | ||||||||||||||
| Z | Z | Z | Z | Z | Z | ||||||||||||||
| Hip Raises | 4 | 9 + 4RiR | W | 4 | 9 + 3RiR | W | 4 | 9 + 2RiR | W | 4 | 5 + 4RiR | W | 4 | 5 + 3RiR | W | 4 | 5 + 2RiR | W | 1Con/3Ecc |
| X | X | X | X | X | X | ||||||||||||||
| Y | Y | Y | Y | Y | Y | ||||||||||||||
| Z | Z | Z | Z | Z | Z | ||||||||||||||
| RPE (1–10: Fill out in set order from left to right) | Box Squat | X,Y,Z | Box Squat | X,Y,Z | Box Squat | X,Y,Z | Box Squat | W,X,Y,Z | Box Squat | W,X,Y,Z | Box Squat | W,X,Y,Z | |||||||
| Hip Raises | W,X,Y,Z | Hip Raises | W,X,Y,Z | Hip Raises | W,X,Y,Z | Hip Raises | W,X,Y,Z | Hip Raises | W,X,Y,Z | Hip Raises | W,X,Y,Z | ||||||||
| Inter-set rest (m) | 2 | 2 | 2 | 2–3 | 2–3 | 2–3 | |||||||||||||
| Frequency (per week)b | 1 | 1 | 1 | 1 | 1 | 1 | |||||||||||||
Abbreviations: RiR: repetitions in reserve; RPE: rating of perceived exertion.
Load (kg) = Self-prescribed load.
Frequency = number of times per week a day is trained.
Appendix 2: The six week periodized strength training program.
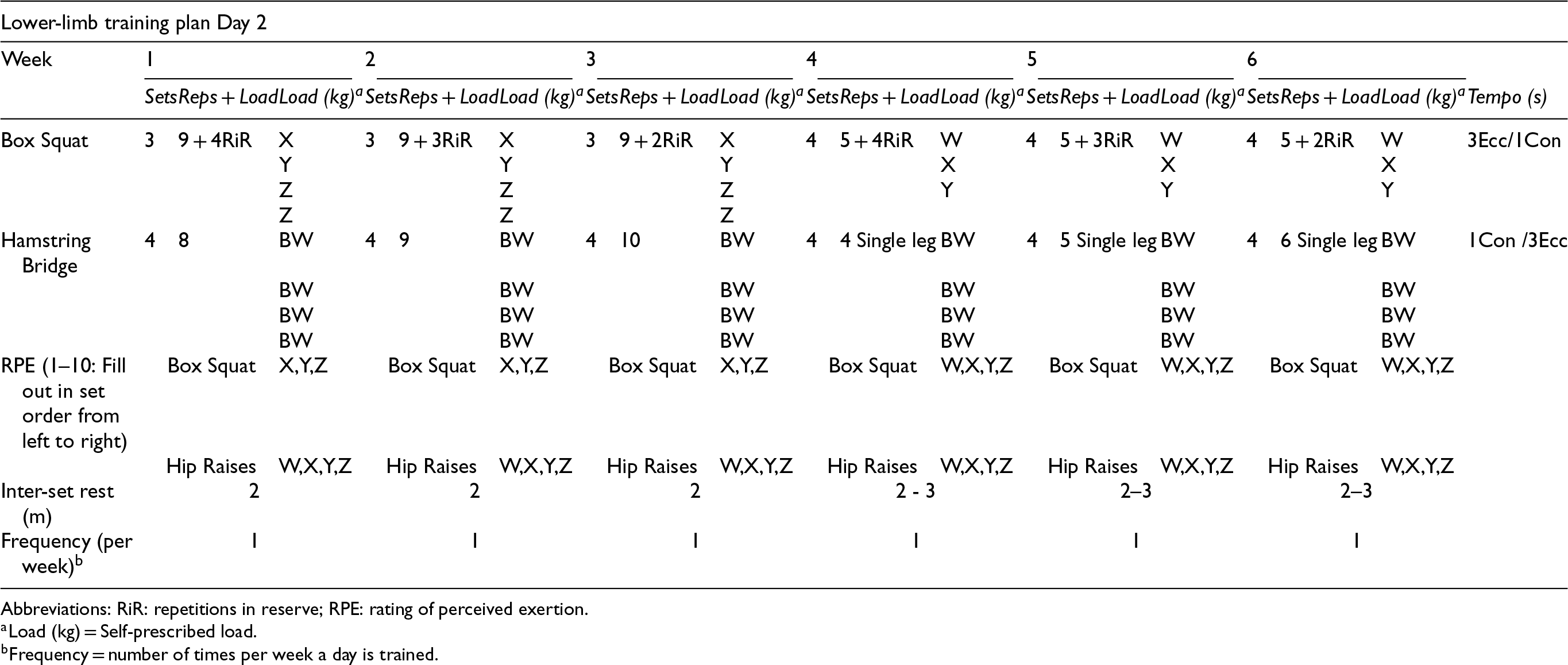
| Lower-limb training plan Day 2 | |||||||||||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| Week | 1 | 2 | 3 | 4 | 5 | 6 | |||||||||||||
| Sets | Reps + Load | Load (kg)a | Sets | Reps + Load | Load (kg)a | Sets | Reps + Load | Load (kg)a | Sets | Reps + Load | Load (kg)a | Sets | Reps + Load | Load (kg)a | Sets | Reps + Load | Load (kg)a | Tempo (s) | |
| Box Squat | 3 | 9 + 4RiR | X | 3 | 9 + 3RiR | X | 3 | 9 + 2RiR | X | 4 | 5 + 4RiR | W | 4 | 5 + 3RiR | W | 4 | 5 + 2RiR | W | 3Ecc/1Con |
| Y |
Y | Y | X | X | X | ||||||||||||||
| Z | Z | Z | Y | Y | Y | ||||||||||||||
| Z | Z | Z | |||||||||||||||||
| Hamstring Bridge | 4 | 8 | BW | 4 | 9 | BW | 4 | 10 | BW | 4 | 4 Single leg | BW | 4 | 5 Single leg | BW | 4 | 6 Single leg | BW | 1Con /3Ecc |
| BW | BW | BW | BW | BW | BW | ||||||||||||||
| BW | BW | BW | BW | BW | BW | ||||||||||||||
| BW | BW | BW | BW | BW | BW | ||||||||||||||
| RPE (1–10: Fill out in set order from left to right) | Box Squat | X,Y,Z | Box Squat | X,Y,Z | Box Squat | X,Y,Z | Box Squat | W,X,Y,Z | Box Squat | W,X,Y,Z | Box Squat | W,X,Y,Z | |||||||
| Hip Raises | W,X,Y,Z | Hip Raises | W,X,Y,Z | Hip Raises | W,X,Y,Z | Hip Raises | W,X,Y,Z | Hip Raises | W,X,Y,Z | Hip Raises | W,X,Y,Z | ||||||||
| Inter-set rest (m) | 2 | 2 | 2 | 2 - 3 | 2–3 | 2–3 | |||||||||||||
| Frequency (per week)b | 1 | 1 | 1 | 1 | 1 | 1 | |||||||||||||
Abbreviations: RiR: repetitions in reserve; RPE: rating of perceived exertion.
Load (kg) = Self-prescribed load.
Frequency = number of times per week a day is trained.
