Abstract
Objective
This scoping review explores the past decade of research on interventions supporting informal caregivers of community-dwelling older adults.
Method
A systematic literature search was conducted in PubMed, Scopus, Web of Science, and PsycINFO. A total of 3408 studies were screened, of which 49 met the criteria for inclusion in this review.
Results
The majority of interventions targeted dementia caregivers, were individually delivered, and professionally guided. Psychoeducational and psychological support dominated, followed by practical support such as respite care or case management, and remote caregiving support. Most studies tested effectiveness/efficacy and predominantly included women. Interventions tailored to non-dementia caregivers and working caregivers, as well as studies addressing implementation strategies and cost-effectiveness, were largely underrepresented.
Conclusion
To move forward, future studies on interventions for informal caregivers of community-dwelling older adults should address diverse caregiving contexts, increase male participation, explore low-resource interventions, and identify strategies for sustainable, cost-effective implementation.
Introduction
Background
The number of people aged 65 years or older worldwide is projected to more than double, rising from 761 million in 2021 to 1.6 billion in 2050 (United Nations, 2023). This demographic shift is expected to pose profound challenges to healthcare systems worldwide. To mitigate its impacts, older adult long-term care systems increasingly rely on involving informal caregivers (Mickelson Weldingh & Kirkevold, 2022; Sattler et al., 2024). Further, most countries have standard policies supporting older adults to age at home, in line with the World Health Organization’s strategic direction on age-friendly cities and communities (WHO, 2023).
Central to this approach is the concept of “aging in place,” which reflects the preference of most people to remain in their own homes while receiving both medical and non-medical support adapted to their personal needs (Pani-Harreman et al., 2021). Informal caregivers often provide much of this support, making them essential to enabling aging in place.
Informal caregivers are individuals who provide unpaid care to older or dependent persons with whom they share a social relationship such as family, friends, and relatives (Broese van Groenou & De Boer, 2016). Worldwide, the economic contributions of informal caregivers are significant, accounting for approximately 2.5% of the European Union’s GDP (Eurocarers, 2024; European Commission, 2021), 2.6% of the United States’ GDP (Reinhard et al., 2023), and between 4.2% and 4.9% of Canada’s GDP (Fast et al., 2024). The reliance on informal care is expected to grow as formal care institutions have limited capacity (Broese van Groenou & De Boer, 2016). At the same time, the pressure on informal caregivers intensifies as a result of societal changes, including smaller and more geographically dispersed family networks and longer working lives (Broese van Groenou & De Boer, 2016; Fischer & Müller, 2020; Schmitz & Westphal, 2017). Informal caregivers often provide support across a broad spectrum of tasks, such as assistance with bathing, dressing, transportation, eating, medication intake, housekeeping, or financial management (Schulz et al., 2020). Due to these extensive responsibilities, informal caregivers often encounter significant challenges that impact their emotional, physical, financial, and social well-being (Zueras & Grundy, 2024).
In response to the diverse needs and health effects associated with caregiving, there is a clear need for targeted interventions to support informal caregivers of community-dwelling older adults (Bom et al., 2019; Gemito et al., 2024; Hall et al., 2022; Plöthner et al., 2019). Various supportive interventions have been studied in recent years, including those delivered individually or in groups, and in both digital and non-digital formats. Examples include psychosocial interventions (Dickinson et al., 2017), services to reduce caregiver workload (e.g., respite care and day care) (Zarit et al., 2017), interventions supporting caregivers during the palliative care phase (Akyar et al., 2019), remote monitoring solutions to facilitate caregiving from a distance (Sharma et al., 2021), and apps that support care planning and coordination (Kelley et al., 2024).
Efforts to synthesize the state of the art in research on interventions for informal caregivers of community-dwelling older adults have been undertaken. However, prior reviews have often limited their focus to the effects of specific types of interventions (Aksoydan et al., 2019; Dickinson et al., 2017; Kirvalidze et al., 2023) while a comprehensive and up-to-date overview focusing on a broader range of interventions is still lacking. To identify current research trends and gaps, there is a need for a more inclusive synthesis that examines both research characteristics (e.g., study designs, research foci, and characteristics of informal caregiver samples) and intervention characteristics (e.g., intervention types and goals, delivery modes, and implementation stages).
Study Aim
This scoping review provides an overview of research published over the past decade on interventions designed to support informal caregivers of older adults (aged 65 years and older) living at home. Specifically, the review addresses the following research questions: (1) What are the characteristics of studies on interventions for informal caregivers of community-dwelling older adults? (2) Which interventions have been studied and what characterizes these?
Based on the findings, this review seeks to identify current research trends and gaps to inform a future research agenda on supportive interventions for informal caregivers of community-dwelling older adults.
Method
Study Design
This study applied the scoping review framework in accordance with the guidelines of Arksey and O'malley (2005), Pollock et al. (2021), and Heyn et al. (2019). Scoping reviews are especially suitable for exploring broad and emerging fields of research, including a variety of study designs (Heyn et al., 2019). The scoping review was prepared and is reported according to the Preferred Reporting Items for Systematic reviews and Meta-Analyses extension for Scoping Reviews (PRISMA-ScR) Checklist (Tricco et al., 2018) (see Appendix 1). The study protocol was pre-registered through the Open Science Framework (OSF) registry (Wrede et al., 2025a).
Search Strategy
A systematic literature search in four databases (PubMed, Scopus, Web of Science, and PsycINFO) was performed in February 2025. The goal of the search was to find peer-reviewed publications describing the development, implementation, and evaluation of interventions which support informal caregivers of community-dwelling older adults. The scope of the search was defined according to the PCC (Population, Concept, Context) framework (Peters et al., 2020). Accordingly, the search string contained terms related to three categories: (1) Population: informal caregivers of community-dwelling older adults, (2) Concept: supportive interventions, and (3) Context: informal care provided in the home environment/in the community. The search string was developed by the review team (experts in the field of informal care, aging, and healthcare transformation) and two library information specialists from the University of Twente who provided critical feedback. Additionally, a preliminary screening (title and abstract) of the first 20 articles was performed. The relevance of those articles was discussed among the review team, and adjustments to the search terms were made accordingly. The final search string for each database can be found in Appendix 2.
Inclusion and Exclusion Criteria
Included studies needed to be peer-reviewed publications (qualitative, quantitative, or mixed-methods) describing the development, implementation, or evaluation of interventions which support informal caregivers of community-dwelling older adults (older adults were defined as 65+). Studies in English, German, and Dutch languages were searched. Studies were excluded, if one or more of the following criteria applied: No focus on informal care provided in the home setting. No focus on interventions. Age of care recipients < 65 or not mentioned or mixed with younger population. Not an original research article (e.g., literature review, viewpoint paper, and study protocol). Not a peer-reviewed journal article (e.g., pre-print and book chapter). Grey literature (this type of literature was excluded due to limited time resources, and because it often tends to be highly country-specific, which might hinder its applicability to an international context). Older than 10 years (we considered studies older than 10 years (before 2015) to be outdated, given the advancements and continuous progress in the field).
Screening and Data Extraction
The screening for this review was performed using the software Covidence. During title and abstract screening, each study was assessed for eligibility by two independent reviewers (CW, NS, JS, or AB), based on the inclusion and exclusion criteria. Conflicts between reviewers were signaled by Covidence and resolved through discussion. During the full-text screening, each study was assessed by one reviewer. To lower the risk of single-researcher bias, borderline cases (papers which a reviewer was unsure about) were discussed within the review team before a decision was taken.
Data from all included studies were extracted using a data extraction form in Excel. The form was used to extract information about study details (author, year, study location, aim, study design, study focus, main findings), sample characteristics (age, gender, informal caregiver type, cohabitation, work status, targeted sub-groups), and characteristics of interventions (description, type, main focus, delivery mode, providers, implementation stage). Each study was assigned to one of the four reviewers to perform the data extraction, and all extractions were checked by a second reviewer. Possible unclarities were discussed and resolved continuously within the review team. Prior to data extraction, the form was tested on two publications to check its clarity, and adjustments were made accordingly.
Synthesis
To provide an overview of study characteristics, the extracted data were organized into a summary table (Appendix 3), and frequency counts were applied to highlight key trends. Furthermore, to describe target group characteristics, informal caregiver demographics were aggregated across the included studies using descriptive analysis followed by frequency counting to map the distribution of targeted sub-groups.
In addition, to synthesize interventions for informal caregivers of older adults, an inductive categorization process was undertaken. Categories were derived from the extracted data based on the primary focus of the interventions and subsequently discussed and refined within the review team. Frequency counts (i.e., number of studies per category) were then used to identify key trends. Moreover, separate overviews were generated for intervention delivery modes and implementation stages, with frequency counts applied to highlight trends. The overview of implementation stages was obtained by deductively categorizing the studies according to the five stages of the NIH model for intervention development of the US National Institute on Ageing (NIH, 2025), namely, (0) basic research, (1) intervention generation/refinement, (2) efficacy testing in research setting, (3) efficacy testing in community setting, (4) effectiveness testing in community setting, and (5) implementation and dissemination.
Results
Included Studies
Figure 1 illustrates the study selection process. A total of 4522 studies were identified across four databases: Scopus, PsycINFO, Web of Science, and PubMed. After removing duplicates, 3408 studies remained. During the title and abstract screening, 3050 studies were excluded, leaving 358 studies for full-text screening. Of these, 49 studies met the inclusion criteria and were included in this scoping review. The remaining 309 studies were excluded based on the reasons provided in Figure 1. PRISMA flow diagram of the study selection process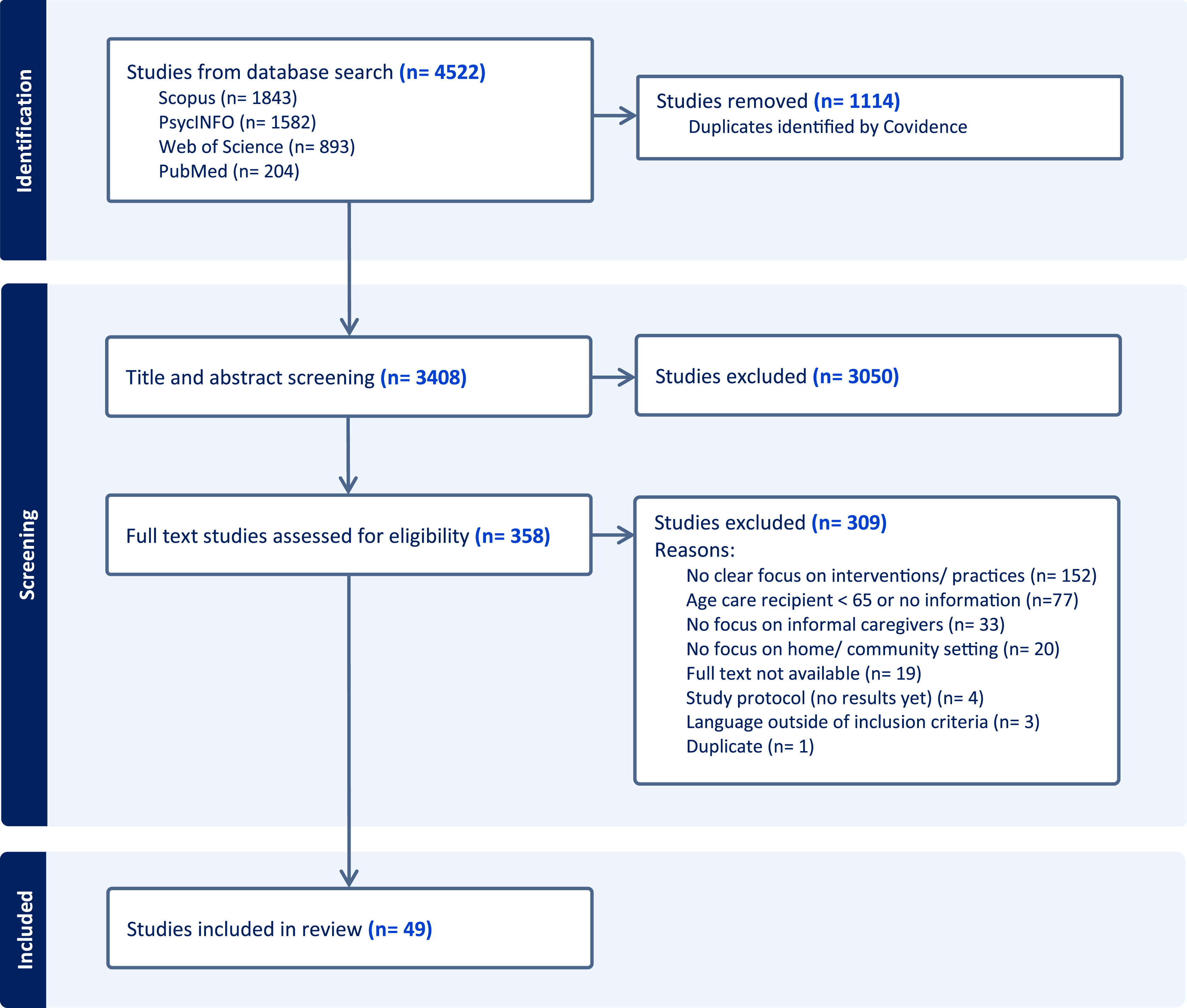
Characteristics of Included Studies
Overview
An overview of included studies is presented in Appendix 3. Most research on interventions to support informal caregivers of community-dwelling older adults was conducted in the first half of the last decade (55.1% of studies between 2015 and 2019; 44.9% of studies between 2020 and February 2025). In terms of location, the reviewed studies were distributed globally, with the highest contributions from Europe (49% of studies), North America (24.5% of studies), Asia (22.5% of studies), and Oceania (4.1% of studies). Countries with the highest number of studies included the USA (22.5% of studies), the Netherlands (18.4% of studies), Germany, and Taiwan (each 6.1% of studies). Among all included studies, 53% employed a quantitative study design (of which 26.5% were RCTs), 32.7% of studies used a mixed-methods design, and 14.3% used a qualitative approach. The most frequent research focus was effectiveness/efficacy (51% of studies), followed by user experiences (16.3% of studies), needs assessment (14.2% of studies), acceptability (10.2% of studies), and feasibility (6.1% of studies). Only 2% of the reviewed studies focused on cost-effectiveness.
Target Group Characteristics
Informal caregiver characteristics across studies
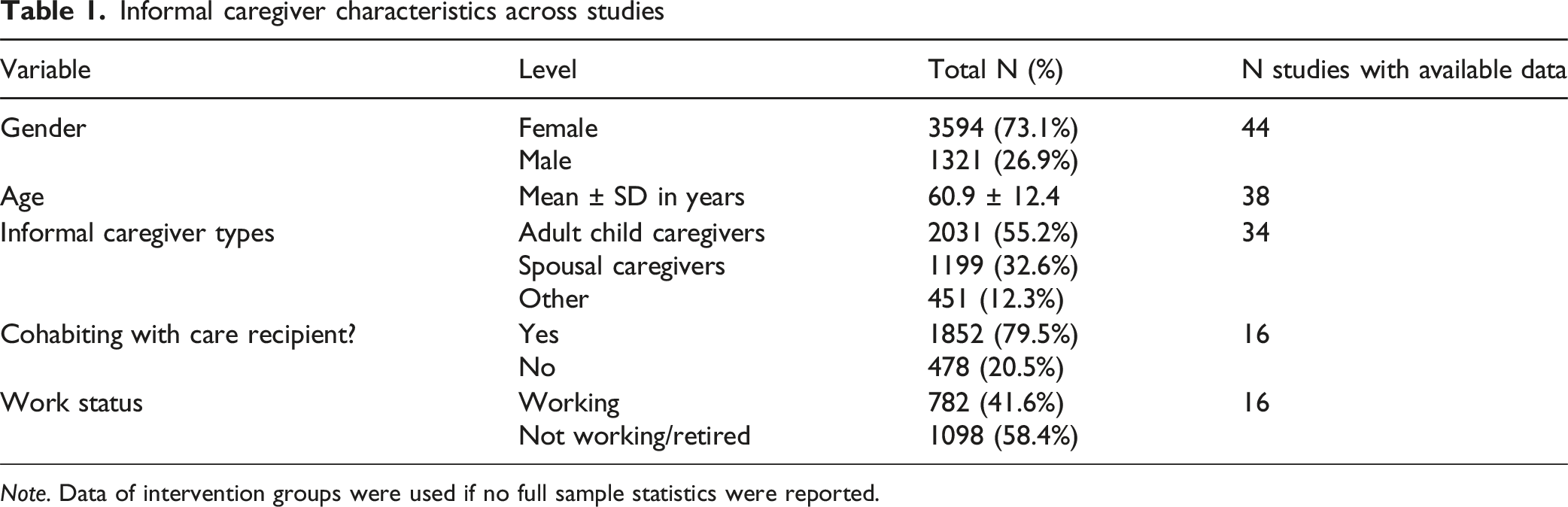
Note. Data of intervention groups were used if no full sample statistics were reported.
Targeted sub-groups

Characteristics of Interventions
Typology of Interventions for Informal Caregivers of Community-Dwelling Older Adults
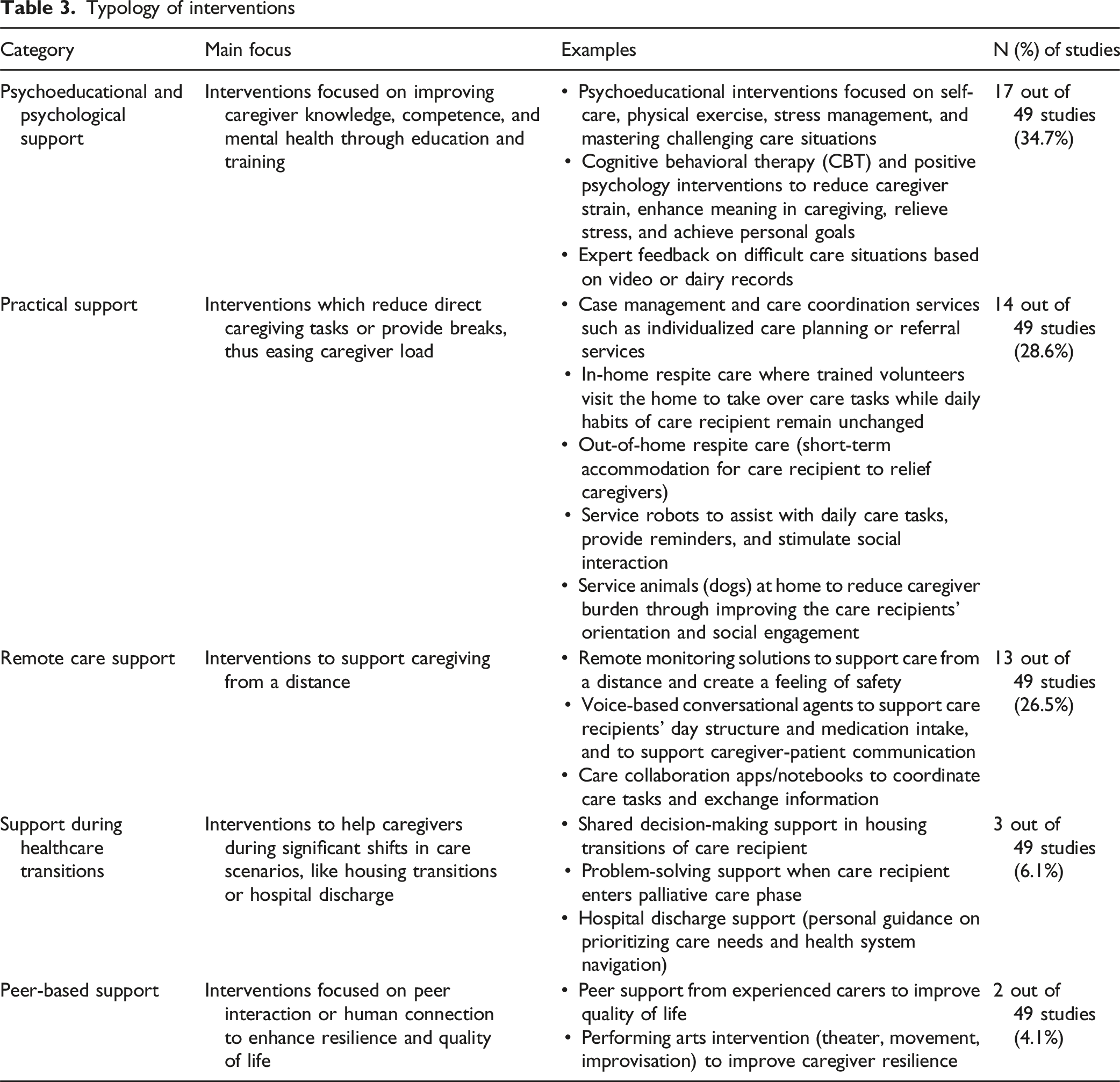
Table 3 presents an overview of supportive interventions for informal caregivers of community-dwelling older adults. In total, five categories were identified across the reviewed literature.
The largest category (34.7% of studies) addressed psychoeducational and psychological support focused on improving caregiver knowledge, competence, and mental health through education and training. This category included educational interventions focused on self-care and mastering challenging care situations, cognitive behavioral therapy (CBT) to reduce caregiver strain and achieve personal goals, and expert feedback on difficult care situations based on video or diary records.
The second largest category (28.6% of studies) centered on practical support, referring to interventions which reduce direct caregiving tasks or provide breaks, thus easing caregiver load. This category encompassed case management and care coordination services, in-home respite care (where volunteers visit the home to take over care tasks), out-of-home respite care (short-term accommodation for care recipients), service robots to assist with daily care tasks (e.g., reminders and stimulating interaction), and service animals (dogs) at home to reduce caregiver burden.
The third largest category (26.5% of studies) addressed remote care support focused on interventions to support caregiving from a distance. These included remote monitoring solutions to create a feeling of safety, voice-based conversational agents to support care recipients’ day structure and medication intake, and care collaboration apps/notebooks to coordinate care tasks and exchange information.
The fourth category (6.1% of studies) focused on support during healthcare transitions, related to interventions which help informal caregivers during significant shifts in care scenarios. These interventions included shared decision-making support in housing transitions of the care recipient, problem-solving support when entering the palliative care phase, and hospital discharge support (personal guidance).
The smallest category we identified (4.1% of studies) concerned peer-based support centered on peer-interaction or human connection to enhance caregivers’ quality of life. This category included peer support from experienced caregivers and a performing arts intervention (theater, movement, improvisation) to improve caregiver resilience.
Delivery Modes
As can be seen in Table 4, the majority of interventions were delivered in-person (55.1% of studies) to individual participants (83.7% of studies). Only 14.3% of interventions were delivered in a group-format. Most interventions were guided by a facilitator (59.2% of studies) instead of adopting a self-help approach (40.8% of studies). Facilitators included a broad range of professionals including nurses, psychologists, case managers, occupational therapists, palliative care specialists, social workers, respite caregivers, artists, and trained volunteers.
Implementation Stage
Typology of interventions
Delivery modes

Implementation stage

Discussion
Principal Results
This scoping review provides an overview of the last decade’s research on interventions to support informal caregivers of older adults living at home. Special attention was paid to study characteristics, characteristics of the involved target group, and the types and characteristics of interventions. The included studies generally varied in their design and focus. While the most common focus was effectiveness/efficacy testing, only one study particularly focused on cost-effectiveness, highlighting the need for more research which weighs service outcomes against costs, especially when health and social care resources are scarce.
Although informal caregivers of community-dwelling older adults are a diverse group, this diversity amongst the group was not fully reflected in the included literature for several reasons. First, most interventions in this review exclusively targeted dementia caregivers—possibly because burden and depression are highly prevalent within this group (Collins & Kishita, 2019)—and only a minority of interventions targeted any caregivers to older adults. Interventions tailored to specific care recipient conditions other than dementia were almost non-existent in this review. This limits our understanding of how to offer tailored support to informal caregivers of older adults with, for example, cancer, psychiatric problems, or other chronic conditions. Second, we found that research on interventions for informal caregivers from minority groups was relatively scarce. This gap highlights an underexplored, yet essential, area, as culturally appropriate interventions have been shown to enhance caregivers’ competence and quality of life (Xiao et al., 2016). Third, interventions tailored to working informal caregivers were underrepresented, although this relatively large group faces unique struggles related to balancing the demands of work and caregiving (Jiménez et al., 2019). Interventions tailored to the time constraints of this group, in particular, have shown positive potential (Jiménez et al., 2019).
This review found that the majority of study participants were female, which is not surprising, as women often bear the responsibility of providing informal care (Schulz et al., 2020). In that way, however, studies may lack inclusiveness and even reinforce the status quo. The gender care gap varies across geography (i.e., common in Southern Europe yet more balanced in Nordic countries) (Rodrigues et al., 2023), race and ethnicity (Cohen et al., 2019), and socio-economic status (Bertogg & Strauss, 2020). However, traditional role expectations are shifting, with more men considered to take on informal caregiving roles (Lindt et al., 2020). We therefore recommend striving for more gender-balance when co-designing and testing informal care support interventions.
Our study shows that during the last decade, a broad spectrum of interventions for informal caregivers of community-dwelling older adults has been studied. Psychoeducational and psychological support dominated, followed by practical support such as respite care or case management, and remote caregiving support. Many of the interventions identified in this review reflect the needs of informal caregivers of older adults found in earlier research. A recent review of Hall et al. (2022), for example, found that informal caregivers of older adults prioritize support such as learning caregiving skills and how to take care of one’s physical and mental well-being, respite care, psychoeducation, and help in navigating existing support options. However, certain needs of informal caregivers identified by Hall et al. (2022) were not or only indirectly addressed in our included interventions. These include the need for financial support and, more generally, the need for systemic changes in healthcare systems such as increased access to care, and more continuity and centralization of care.
Our review revealed a relatively strong emphasis on digital support for informal caregivers of community-dwelling older adults as 44.9% of the studies focused on digital interventions. Since a previous review from 2012 (Lopez-Hartmann et al., 2012), research interest has clearly shifted toward more advanced digital solutions, particularly those involving artificial intelligence such as remote monitoring systems, service robots, and voice-based virtual agents. While the future of informal care support looks increasingly digital or hybrid, a point of concern remains the digital divide between those who can and those who cannot use digital tools (Yang et al., 2024). The increasing focus on digital interventions may increase this divide, especially for older caregivers. This calls for inclusive design principles to ensure equitable access but also exploring older caregivers’ intention to use digital interventions (Wang et al., 2021).
A key finding of our review was that studies examining implementation strategies of interventions for informal caregivers of community-dwelling older adults were underrepresented. This aligns with the findings of Zhu et al. (2023), who reported a similar gap in the context of informal dementia care support. Also, it seems that implementation aspects (such as limited resources) have not always been considered in the design of the included interventions. A considerable number of interventions identified in this review appear to be quite labor-intensive, especially individually delivered, guided in-person multi-component interventions. One example is the study of Czaja et al. (2018) which presents outcomes of a six-month multicomponent psychosocial intervention which involved six individual face-to-face and six individual telephone sessions, and telephone support groups. The authors described that, due to changes within the organization and resource constraints, the entire intervention was not being implemented. This raises questions about how scalable and future-proof such labor-intensive interventions are. Even when shown to be effective, their successful implementation remains uncertain in the context of a shrinking workforce and increasingly constrained healthcare resources (OECD, 2020). Ultimately, considering implementation aspects in the early stages of intervention development reduces the risk of designing for a future which does not exist (Kip et al., 2024).
Lastly, it is worth noticing that the studies included in this review span multiple countries, where national and cultural contexts shape caregiving practices and caregiving burden (Clarke & Smith, 2011; Nayebi et al., 2025). Variations in health and social care systems and care funding influence the extent to which families are relied upon and the support that is being developed (Nayebi et al., 2025).
Limitations
There are a number of limitations to acknowledge in this review. First, this review included peer-reviewed journal articles only and excluded grey literature such as reports or books. These alternate sources could have provided additional insights into everyday support practices and policies for informal caregivers that were not scientifically studied but do exist. The literature search was also limited to publications in English, Dutch, and German which may have excluded relevant work published in other languages, potentially omitting region-specific interventions or culturally tailored practices. Additionally, many relevant studies (specifically studies with caregivers of persons with dementia) did not specify the age of care recipients and therefore did not meet the inclusion criterion of being 65 years or older; these studies were consequently excluded from the review. This criterion was applied to ensure that the review focused exclusively on interventions aimed at informal caregivers of older adults (65+). Furthermore, although multiple reviewers were involved in study selection and data charting, some degree of interpretative bias may remain. This is particularly relevant for the classification of implementation stages according to the NIH Stage Model, as these stages were not explicitly reported in the studies and were inferred by the authors based on their interpretation of the study data. Given the diversity of study designs and interventions studied in different implementation contexts, some classifications were less straightforward and required discussion within the review team. Finally, as this was a scoping review, the aim was to describe and map existing research rather than evaluate outcomes in depth. Evaluating outcomes such as effectiveness would require a systematic review and meta-analysis focused on specific intervention types, which was beyond the scope of this study.
Future Research Agenda
Based on the trends and gaps identified in this review, we propose five key directions for future research to ensure that interventions for informal caregivers are inclusive, scalable, and sustainable: (1) (2) (3) (4) (5)
Conclusions
With the increase in the older adult population, interventions that support their caregivers are critically important. This scoping review provides a recent and comprehensive overview of research on interventions supporting informal caregivers of community-dwelling older adults. The review highlighted a total of 49 interventions, with psychoeducational and psychological support being most common, followed by practical support such as respite care or case management, and remote caregiving support. The majority of identified interventions specifically targeted dementia caregivers, were individually delivered and guided by a professional. Most studies focused on testing service effectiveness or efficacy and predominantly included female caregivers in their samples. Moving forward, future research should prioritize the development of inclusive, scalable, and sustainable interventions that address diverse caregiving contexts, increase male caregiver participation, explore low-resource interventions, and establish strategies for cost-effective and long-term implementation.
Supplemental Material
Supplemental Material - Interventions for Informal Caregivers of Community-Dwelling Older Adults: A Scoping Review and Future Research Agenda
Supplemental Material for Interventions for Informal Caregivers of Community-Dwelling Older Adults: A Scoping Review and Future Research Agenda by Christian Wrede, Nikita Sharma, André Bieleman, Angelica Tinga, and Jodi Sturge in Journal of Aging and Health
Footnotes
Acknowledgments
We gratefully acknowledge Luuk van Ewijk and Dr Stella Kruit-van Rossum for their contributions to the development of the search strategy for this review. Furthermore, we thank Kerem Dogan for his feedback during the writing process.
Ethical Considerations
Ethics approval is not required as no participants were involved in this research.
Funding
The authors disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This work was executed as part of the project “Samenwerkingskracht Mantelzorg,” funded by Regio Deal Twente, the Netherlands.
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Data Availability Statement
The articles included in this scoping review are published and freely available.
Supplemental Material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
