Abstract
Introduction
Delusions are common in Lewy body disease (LBD), significantly impacting quality of life. This study examined clinical factors, characteristics and themes associated with delusions in LBD.
Methods
Clinical and demographic factors were compared between 91 individuals attending St. James’s Hospital in Ireland with LBD both with and without delusions. Clinical scales include the Clinical Dementia Rating Scale (CDR), Epworth sleepiness scale (ESS), Addenbrooke’s Cognitive Evaluation (ACE-III), and Neuropsychiatric Inventory-12 (NPI-12). Themes of delusions extracted from clinical descriptions were mapped onto a typology from primary psychiatric populations.
Results
Individuals with delusions were older, had higher CDR and ESS scores, lower ACE-III performance, higher scores on the NPI-12, and demonstrated cognitive impairment at the MCI or dementia level. Misidentification delusions were most common, followed by delusions of “being harmed, attacked, or killed” and “residence is not their home”.
Conclusion
These findings suggest delusions are related to disease stage, sleep, distinct cognitive and neuropsychiatric patterns, and follow a unique thematic typology.
Introduction
Lewy body disease (LBD) refers to a group of neurodegenerative disorders comprising idiopathic Parkinson’s disease (PD), inclusive of Parkinson’s disease with mild cognitive impairment (PD-MCI) and Parkinson’s disease dementia (PDD), and dementia with Lewy Bodies (DLB). 1 General population estimates of DLB range from 0% to 5%. 2 Together, DLB and PDD, collectively known as Lewy body dementia, are estimated to account for 4%–30% of all dementia cases.3-6 LBD is thought to exist on a spectrum based on symptomatology, with motor symptoms falling on 1 end (PD and PD-MCI), and dementia at the opposite end (PDD and DLB). The “1 year rule” is recommended to distinguish between PDD and DLB due to their overlap in clinical presentation, endorsing a diagnosis of DLB when cognitive decline precedes or occurs within 1 year following motor symptom onset. PDD, then, is indicated when motor symptoms occur more than 1 year prior to cognitive decline. 7
Prevalence and Impact of Delusions in LBD
Delusions are estimated to occur in 3%–14% of individuals with PD, with higher prevalence in PDD, ranging from 19% to 51%. 8 In DLB, approximately 55% of individuals experience delusions over a 12-year period, and the frequency of delusions increases with disease progression.9,10 Delusions and other psychotic phenomena in LBD can have a significant impact on quality of life and caregiver burden. 11 Higher frequency and severity of neuropsychiatric symptoms has also been correlated with functional decline in Lewy body dementia. 12 Psychotic symptoms in LBD have also been associated with increased mortality, higher rate of hospitalisation, and increased nursing home placement.13-15
Associated Factors
Research that has investigated psychosis in LBD has mainly focused on hallucinations or comorbid hallucinations and delusions, and has primarily been conducted in the context of PD.16-19 A review of delusions in PD conducted by Warren et al 20 reported cognitive impairments present in 17.9% of cases, with higher frequency in cases with comorbid hallucinations. A 2014 study in a PD sample further demonstrates this pattern, finding that only hallucinations had significant correlations with cognitive functioning. 21 Neuropsychiatric and behavioural symptoms such as anxiety, agitation, and impulse control disorders were also associated with delusions in PD, as was age of onset, with 49.5% meeting criteria for early onset PD. 20 However, the study did not distinguish between cognitive impairment levels in PD, overlooking potential differences across diagnoses, and assumed any unmentioned symptoms were definitely absent. Additionally, dichotomising continuous variables further limited nuanced analysis. Nocturnal sleep disturbances, including RBD, have also been associated with psychosis in both PD and DLB.22,23
A 2018 study by Tzeng et al 9 provides preliminary evidence for associations with delusions in DLB. Anxiety and agitation were found to be associated with delusions, as were disinhibition, hallucinations, irritation, increased disease severity, and aberrant motor behaviour. Comorbid diabetes was associated with less frequent delusions. Higher frequency of delusions was also associated with poorer cognitive performance, contrasting the results found in PD studies. However, in this study 67% of the delusional group had comorbid hallucinations, limiting the ability to draw associations exclusively between delusions and cognitive functioning. The generalisability of this study is also limited as all individuals were sourced from 3 hospitals in Taiwan. Additionally, the cross-sectional design limits the ability to identify patterns of associations over time. These limitations warrant further investigation to clarify the associated clinical and demographic factors linked to delusions in LBD.
With respect to pharmacotherapy, a 2020 study by Oliveira et al 24 found that the length of time since an LBD patient’s first systematized delusion was associated with higher rates of polypharmacy. Additionally, dopaminergic medication has been associated with delusional jealousy in PD. 25 While these studies are limited in their generalisability due to small sample sizes and cross-sectional design, they offer preliminary findings which impel further investigation into the relationship of pharmacotherapy and delusions in LBD.
Thematic Typology
There exists no universal thematic typology for delusions in LBD. Person-centered care models emphasise the importance of the lived experience of complex health conditions, and necessitate a better understanding of the personal relevance and thematic content of delusions in LBD. 26 Using the Neuropsychiatric Inventory (NPI) 8-item typology, a 2018 study found the most common delusion in DLB was of other people stealing, occurring in 35.3% of the delusional cohort. 9 However, the use of a pre-existing typology of only 8 themes inherently hinders the accurate assessment of thematic prevalence. A 2020 study included a neurodegenerative group consisting of PDD, DLB, and Alzheimer’s disease (AD), using the typology from the Questionnaire for Psychotic Experiences (QPE), comprising 9 delusional themes of which the most common was paranoia. 19 While these studies provide valuable insight, the inclusion of AD and absence of PD without dementia prohibits a full understanding of delusional themes in LBD. The use of deductive analysis with such limited typologies also lends itself to confirmation bias, and precludes the possibility of considering more suitable themes, elucidating the need for further investigation to develop a typology best suited for LBD.
Delusional misidentification syndromes (DMS) can also occur in LBD. The highest prevalence is reported among the DLB population, with estimates ranging from 38% to 57.1%.27,28 In DLB, the most common DMS is Capgras syndrome, reported in up to 33.3% of individuals.28,29 DMS are less frequently reported in PD and PDD, with 1 study finding that 16.7% of participants experienced DMS, though no individuals in this study reported Capgras or Fregoli syndrome. 30 These syndromes have not been frequently reported among PD samples, with a 2017 review 31 finding a total of 30 cases of Capgras syndrome in PD or PDD samples, and only one reported case of Fregoli syndrome in PD which was associated with Levodopa therapy.
A thematic analysis conducted by Jones et al 30 found significant variation in delusional themes reported by individuals referred to Early Intervention for Psychosis Services, producing a typology of 15 themes and 50 sub-themes. Though this typology was based on a primary psychiatric population, limiting its generalisability to the LBD population, the significant breadth of themes presented provides an ample basis for which delusional themes may be compared in order to create a thematic typology specific to LBD.
Aims and Hypotheses
Despite the prevalence and impact of delusions in LBD, research on the lived experiences and associated factors of delusions in LBD remains limited. Better understanding, in conjunction with insight into associated factors, would better inform intervention strategies and support for delusions in LBD. This study aimed to describe the clinical and demographic factors, as well as cognitive and neuropsychiatric profiles associated with delusions in LBD. Additionally, this study sought to describe the thematic typology of delusions in LBD, providing a baseline for future studies into this topic. This study hypothesised that delusions would be associated with specific cognitive and neuropsychiatric profiles.
Methodology
Study Design and Participants
A cross-sectional study design was employed based on data collected from the first 100 referrals to a specialised neuropsychiatric clinic for individuals with suspected or established LBD. These individuals were referred to the Mind and Movement clinic at St. James’s Hospital in Dublin, Ireland between the years 2020 and 2022. Of the 100 referrals, five individuals were excluded from the study, having received non-LBD diagnoses. An additional 4 individuals were excluded from analyses due to incomplete records. The remaining 91 individuals were recorded as having Lewy body disease and were included in the analyses. PD diagnosis was made in accordance with the criteria set forth by the Movement Disorder Society for probable PD. PD-MCI was diagnosed according to Level I certainty criteria set forth by Litvan et al (2012), 33 and diagnosis of PDD was made according to the criteria set forth by Emre et al for probable PDD (2007). 34 Diagnosis of DLB was made in line with the recommendations and criteria for probable DLB published in the 2017 consensus report of the DLB consortium. 35 No individuals were recorded as having prodromal DLB.
Procedure
Demographic and Clinical Data
Demographic and clinical data were obtained from paper and electronic medical records, including medical history, medication profile, neuroimaging results, and collateral information provided by informants (primarily family members).
Measures
Table S1 presents an overview of the assessment tools utilised as well as their scoring guidelines. Individuals were administered the Epworth Sleepiness Scale (ESS) to assess level of daytime sleepiness. 36 Cognition was assessed using the third version of the Addenbrooke’s Cognitive Examination (ACE-III). Individuals were also administered the CDR to evaluate cognition and functional ability. 37
Two measures were utilised to evaluate neuropsychiatric symptoms: the 15-item Geriatric Depression Scale (GDS) and the 12-item Neuropsychiatric Inventory (NPI-12).38,39 In order to assess distinctions in neuropsychiatric profiles between individuals with and without delusions, NPI domains were grouped into 4 superordinate categories: psychosis, affect, hyperactivity, and apathy/neurovegetative, in line with the model produced by Kang et al
40
using factor analysis (Figure 1). Elation/euphoria and motor disturbances were not included in these categories due to incompatible factor loading. Category totals reflect the number of individuals who had clinically significant (≥4) scores in at least one of the category’s respective NPI domains. Superordinate categorisation of NPI domains.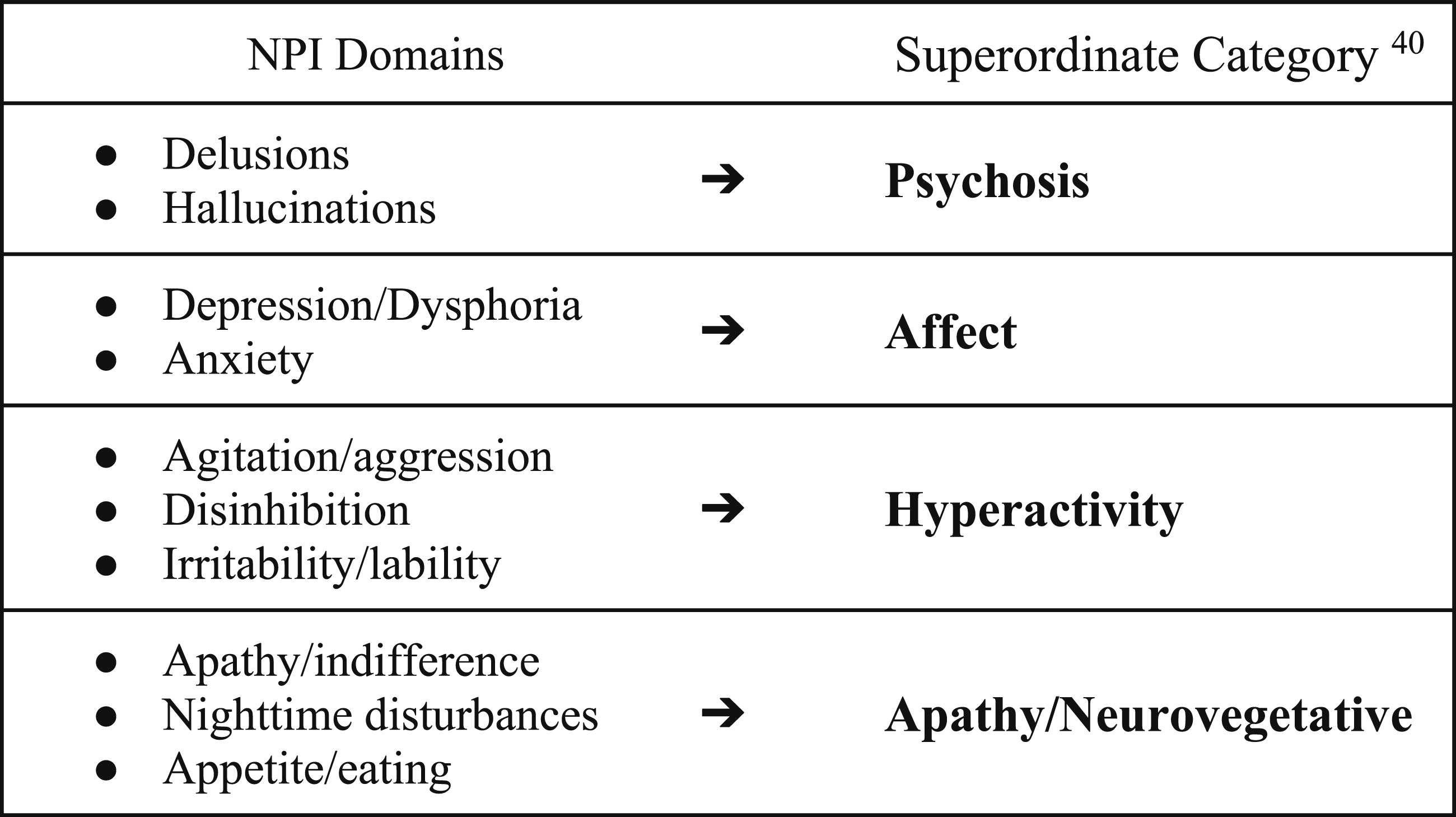
Statistical Analyses
Statistical analyses were carried out using R (Version 4.3.2). Univariate comparisons of proportional data between individuals with and without delusions was conducted via chi square testing. Yates’s continuity correction was applied when using 2 × 2 contingency tables to account for the overestimation of the chi square statistic which occurs when using such tables. In 2 × 2 contingency tables where the assumption of minimum expected cell counts of 5 was not met, Fisher’s exact test was utilised instead of chi square. A phi coefficient was obtained as the effect size for comparisons using 2 × 2 contingency tables, while Cramer’s V was obtained for those using larger tables.
For continuous variables that were compared between individuals with and without delusions, assumptions of normality and homoscedasticity were evaluated using the Shapiro-Wilk and F-tests, respectively. Mann-Whitney-Wilcox tests were utilised as a non-parametric alternative to t-tests when the assumptions of normality and/or homoscedasticity were violated. Rank-biserial correlation coefficients were obtained as the effect size for two-group comparisons using Mann-Whitney-Wilcox tests.
For comparisons of continuous variables across more than two groups, the assumption of normality was assessed using the Shaprio-Wilk test. Normally distributed variables were assessed for homoscedasticity using the Bartlett Test of Homogeneity of Variances. If variables were not normally distributed, the Fligner-Killeen Test of Homogeneity of Variances was used. Normally distributed data was analysed using one-way analysis of variance (ANOVA) when the assumption of homoscedasticity was maintained; if heteroscedasticity was present, Welch’s F test was used. If data violated normality and homoscedasticity assumptions, the Kruskal-Wallis test was utilised. Epsilon squared was obtained as the effect size for Kruskal-Wallis tests, and partial eta-squared was utilised for ANOVA and Welch’s F test. Post-hoc testing was conducted via pairwise independent t-tests or pairwise Mann-Whitney-Wilcox tests, dependent on the distribution of the data. Post-hoc pairwise comparisons were executed using Bonferroni correction to mitigate the risk of type I errors. All results were evaluated at the .05 significance level.
Predictors of delusions as a dichotomous variable (where 0 = does not have delusions and 1 = has delusions) were evaluated using multivariable binary logistic regression. Predictors considered in the regression included ACE total score, NPI domain scores for Hallucinations and Agitation/Aggression, and ESS score, while controlling for age, sex, and CDR score. A reduced model where ACE total score was the only predictor was compared to a full model employing all predictors using a chi squared test. Multicollinearity and linearity of the logit were assessed using variance inflation factor (VIF) and by evaluating the interaction of each variable with its log. McFadden’s pseudo R2 was calculated as a measure of goodness of fit.
Missing Data
Due to the pragmatic nature in which data was obtained, symptoms were recorded based on patient reports rather than using a structured interview or checklist of symptoms. For univariate analysis of categorical variables, symptoms which were not recorded were considered absent for the purposes of statistical analysis. For univariate analysis of continuous variables, missing values were removed from analyses, rather than being considered zeros, and statistics were calculated based on the number of responses available for each test/domain, rather than the total number of individuals in that group. For logistic regression, in order to effectively compare models, missing data was imputed with the median respective to which group the individual was in (with or without delusions). Median imputation was utilised given the non-normal distribution of variables; median imputation has demonstrated comparable validity and robustness to more complex methods of imputation 41 (Berkelmans et al, 2022).
Qualitative Data
Descriptions of patients’ lived experience with delusions were obtained through clinical interviews with patients and informants and supplemented with patient history/notes. Qualitative content analysis was employed, using deductive coding to map themes from the clinical descriptions onto both the NPI 8-theme typology as well as the 15-theme typology from Jones et al 30 Delusions which were unable to be classified into a theme from the original Jones et al typology, or those which were determined could better be described using a different theme/sub-theme, were re-classified via inductive coding to provide a more accurate and comprehensive list of the themes present in the clinical descriptions. These themes were then used to create an adapted version of the Jones et al typology to better represent the themes identified, with the results from our sample presented alongside the findings from the Jones et al primary psychiatric population. Initial coding was conducted by one author, reviewed by a second author. The clinical descriptions were presented alongside each typology for verification by the second author. Any discrepancies in the categorisation of a delusion was discussed between authors before agreeing on the final thematic classification.
Results
Demographic and Clinical Characteristics
Demographic and Clinical Characteristics.
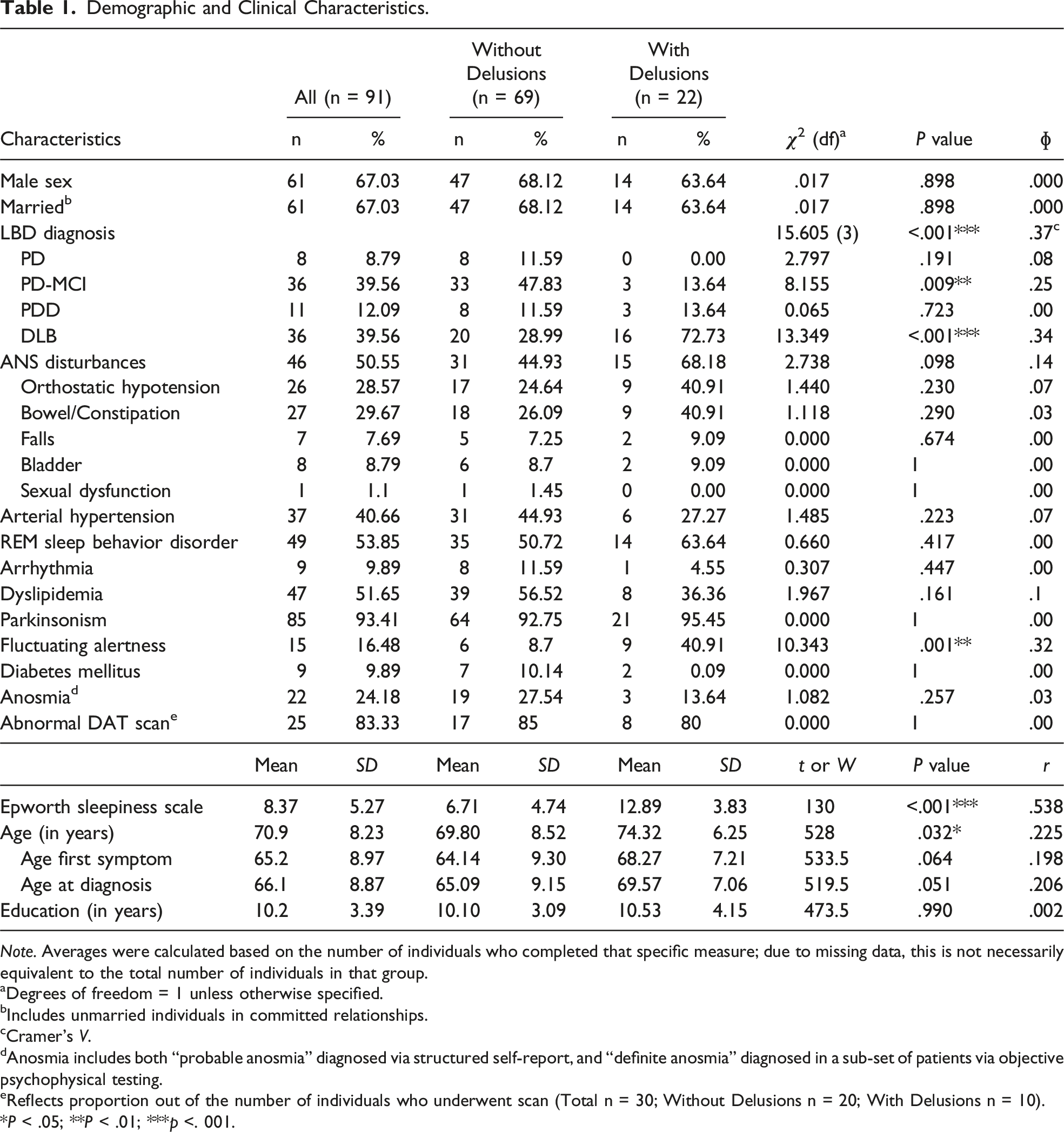
Note. Averages were calculated based on the number of individuals who completed that specific measure; due to missing data, this is not necessarily equivalent to the total number of individuals in that group.
aDegrees of freedom = 1 unless otherwise specified.
bIncludes unmarried individuals in committed relationships.
cCramer’s V.
dAnosmia includes both “probable anosmia” diagnosed via structured self-report, and “definite anosmia” diagnosed in a sub-set of patients via objective psychophysical testing.
eReflects proportion out of the number of individuals who underwent scan (Total n = 30; Without Delusions n = 20; With Delusions n = 10).
*P < .05; **P < .01; ***p <. 001.
Autonomic nervous system (ANS) disturbances including orthostatic hypotension, constipation/bowel issues, falls, bladder issues, and sexual dysfunction were reported by 50.55% of individuals. Parkinsonism was present in 85 individuals (93.41%), and RBD was present in 40 individuals (53.85%). Arterial hypertension and arrhythmia were reported by 40.66% and 9.89% of the sample, respectively. Nine individuals had diabetes mellitus, 47 had dyslipidaemia, and 22 had anosmia. Fluctuating alertness was reported by 15 individuals, with a significantly higher proportion among those with delusions,
Antiparkinsonian medications, including dopamine therapies, amantadine, and COM-T and MAO-B inhibitors, were prescribed to 74.73% of individuals. Antipsychotic medications were prescribed to 17.58% of individuals. There was a significantly higher rate of antipsychotic prescriptions among individuals with delusions (36.36%) compared to individuals without delusions (11.59%),
Cognitive Profile
LBD dementias comprised the majority of diagnoses among individuals with delusions, accounting for 86.37% of the group. DLB was the most common diagnosis among individuals with delusions (72.73%), and occurred at a significantly higher rate than in those without delusions,
Performance on the Addenbrooke’s Cognitive Examination III (ACE-III)
Mean Scores of Addenbrooke’s Cognitive Examination III (ACE - III) and Clinical Dementia Rating Scale (CDR).
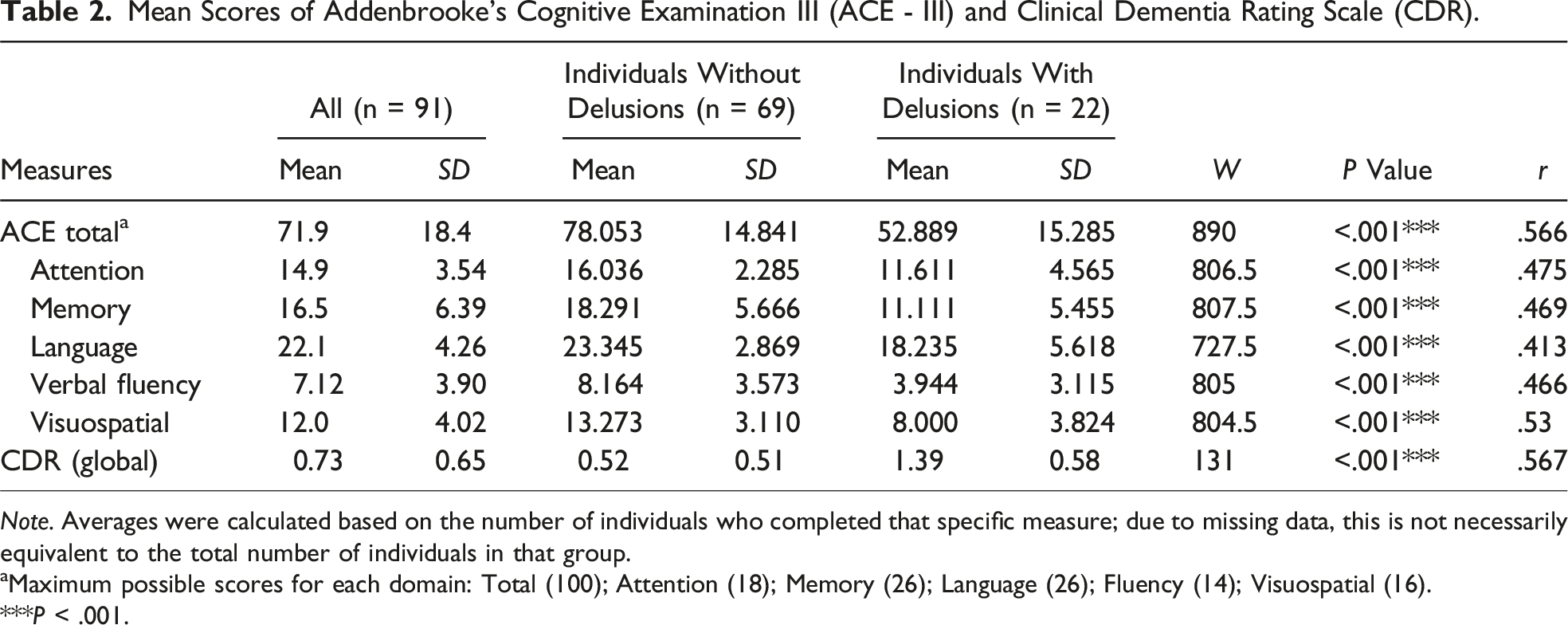
Note. Averages were calculated based on the number of individuals who completed that specific measure; due to missing data, this is not necessarily equivalent to the total number of individuals in that group.
aMaximum possible scores for each domain: Total (100); Attention (18); Memory (26); Language (26); Fluency (14); Visuospatial (16).
***P < .001.
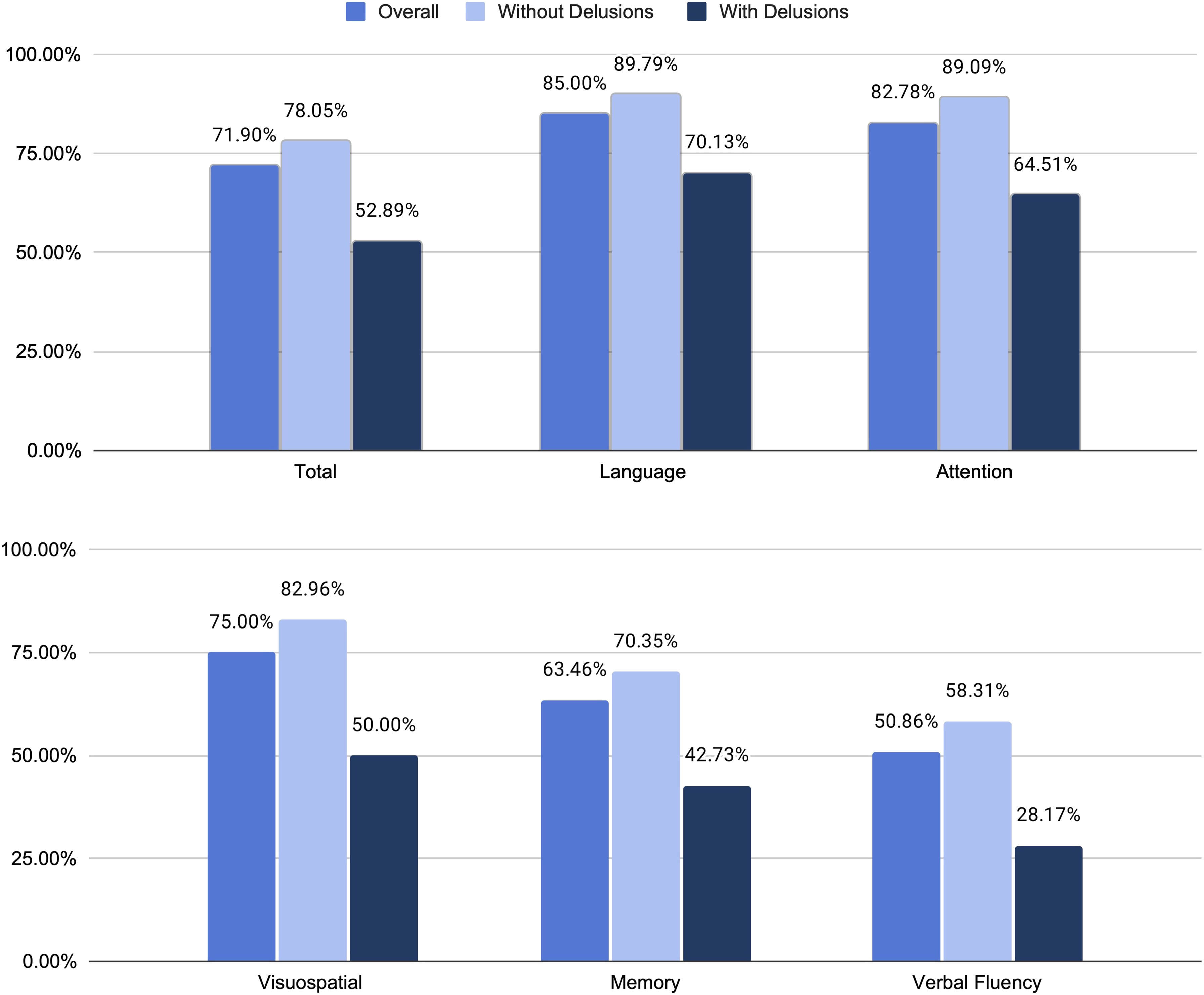
Performance on the Addenbrooke’s Cognitive Examination.
Clinical Dementia Rating Scale (CDR) Scores
CDR global scores were available from 63 participants (Table 2). Questionable dementia was the most common CDR stage (n = 25), followed by mild dementia (n = 19), no dementia (n = 18), and moderate dementia (n = 11). None of the 63 participants had scores matching the severe dementia stage (CDR = 3). The average global score on the CDR was .73 (SD = .65), falling between the questionable and mild dementia stages.
NPI Delusions Domain Score Across Clinical Dementia Rating Scale (CDR) Stages.
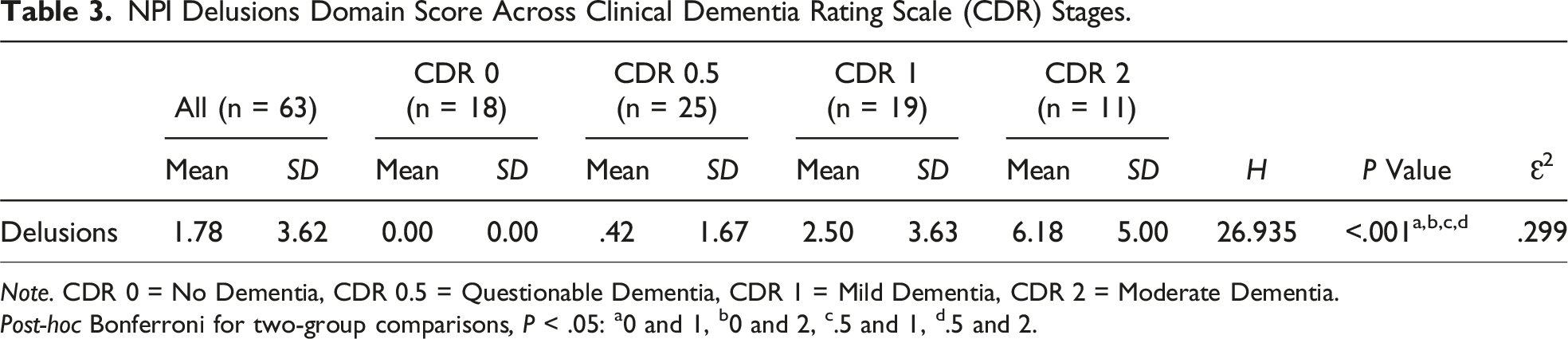
Note. CDR 0 = No Dementia, CDR 0.5 = Questionable Dementia, CDR 1 = Mild Dementia, CDR 2 = Moderate Dementia.
Post-hoc Bonferroni for two-group comparisons, P < .05: a0 and 1, b0 and 2, c.5 and 1, d.5 and 2.
Neuropsychiatric Characteristics
Frequency of Hallucinations and Average Geriatric Depression Scale (GDS) Scores.
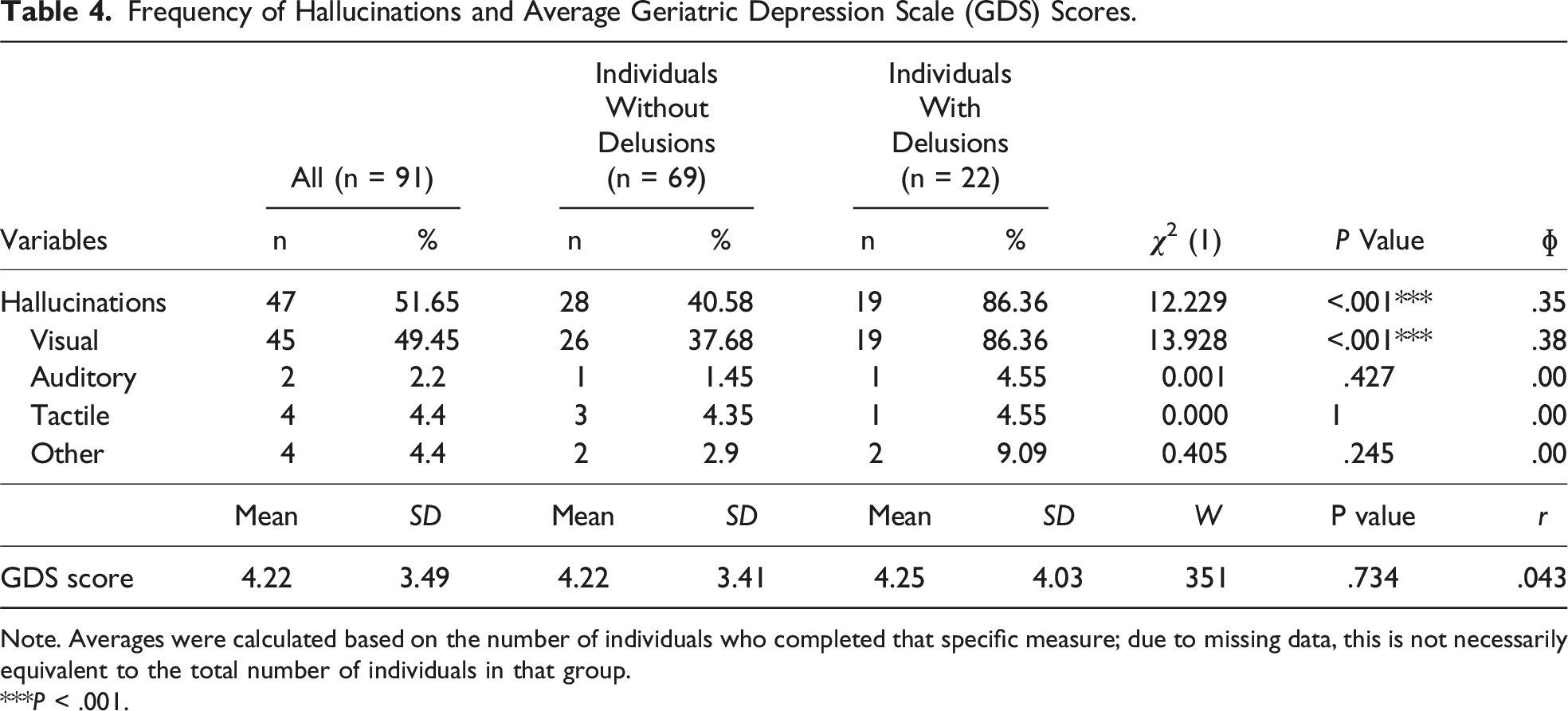
Note. Averages were calculated based on the number of individuals who completed that specific measure; due to missing data, this is not necessarily equivalent to the total number of individuals in that group.
***P < .001.
Mean Scores of the Neuropsychiatric Inventory (NPI).
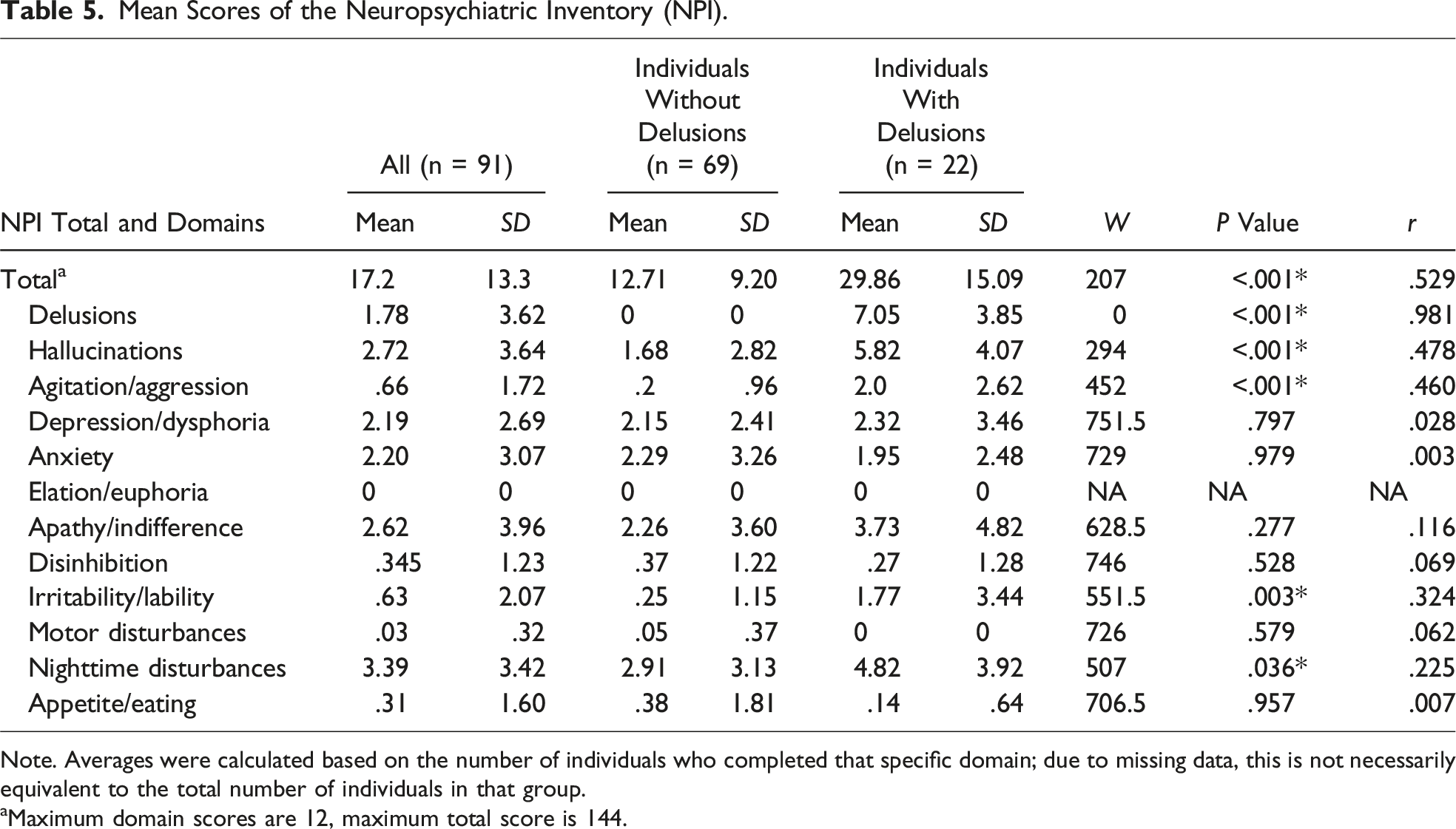
Note. Averages were calculated based on the number of individuals who completed that specific domain; due to missing data, this is not necessarily equivalent to the total number of individuals in that group.
aMaximum domain scores are 12, maximum total score is 144.
Proportion of Endorsed Neuropsychiatric Inventory (NPI) Domains.
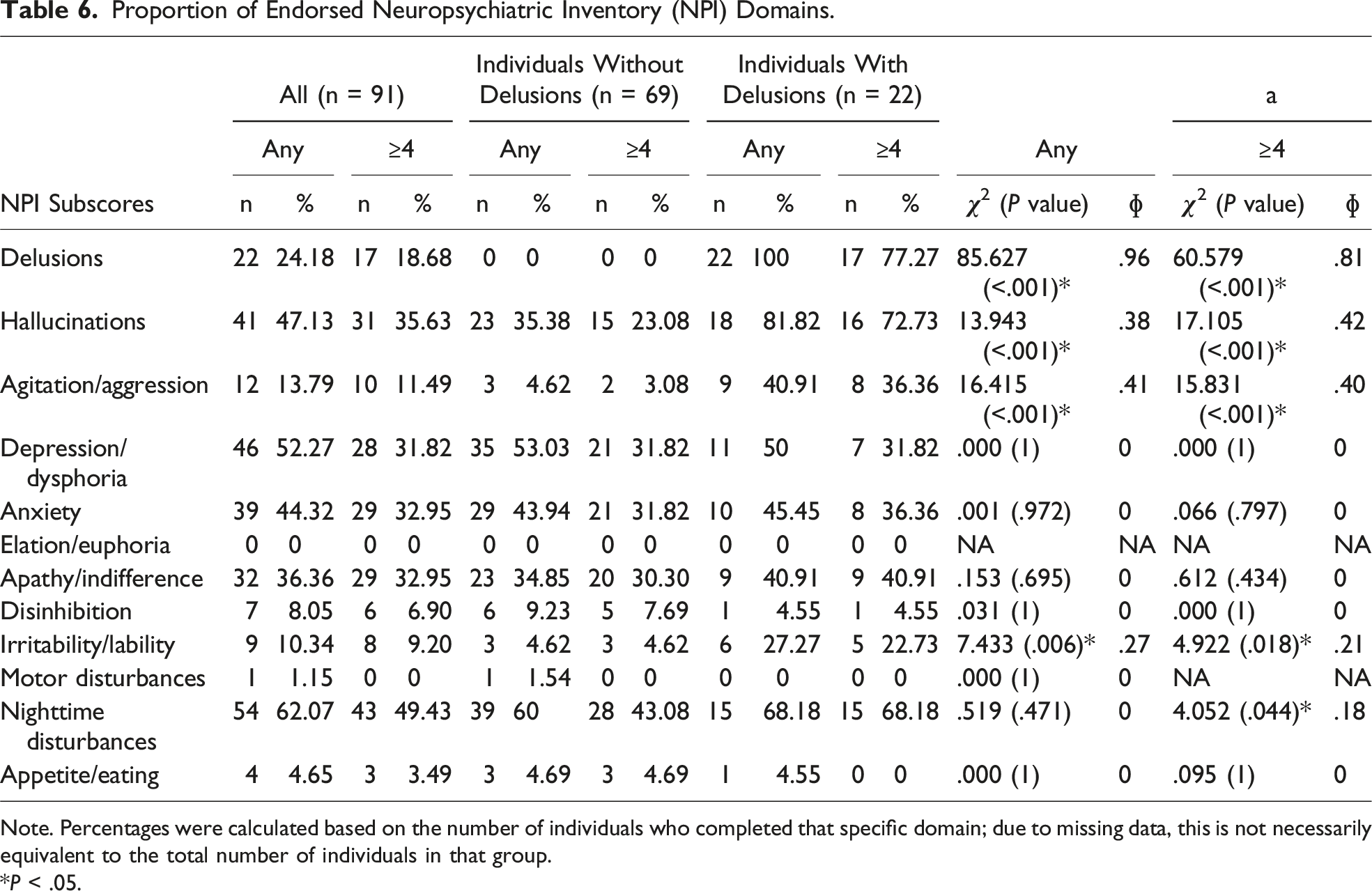
Note. Percentages were calculated based on the number of individuals who completed that specific domain; due to missing data, this is not necessarily equivalent to the total number of individuals in that group.
*P < .05.
Neuropsychiatric Characteristics Across 4 Superordinate Categories
To evaluate the neuropsychiatric profiles of individuals with and without delusions, the proportion of individuals with clinically significant scores in the 4 superordinate NPI categories were compared. Among the entire sample, apathetic/neurovegetative symptoms were the most commonly endorsed, with 63.64% of individuals scoring ≥4 in at least one of the relevant NPI domains. Affective symptoms were the second most frequently endorsed (43.18%), followed by psychosis, and hyperactivity (see Figure 3). Distribution of clinically significant scores across 4 superordinate NPI categories.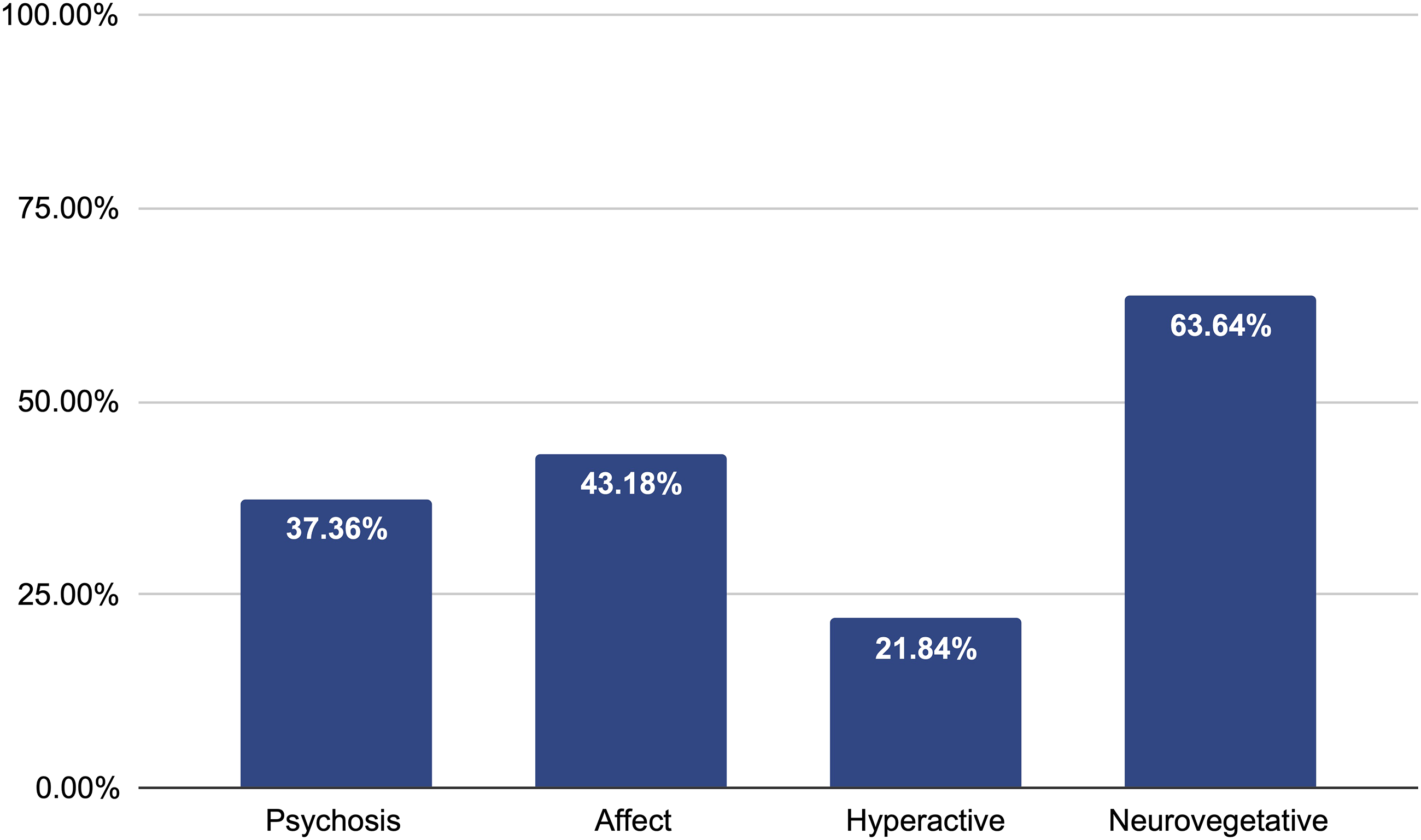
Clinically Significant Symptoms Across 4 Superordinate Categories.
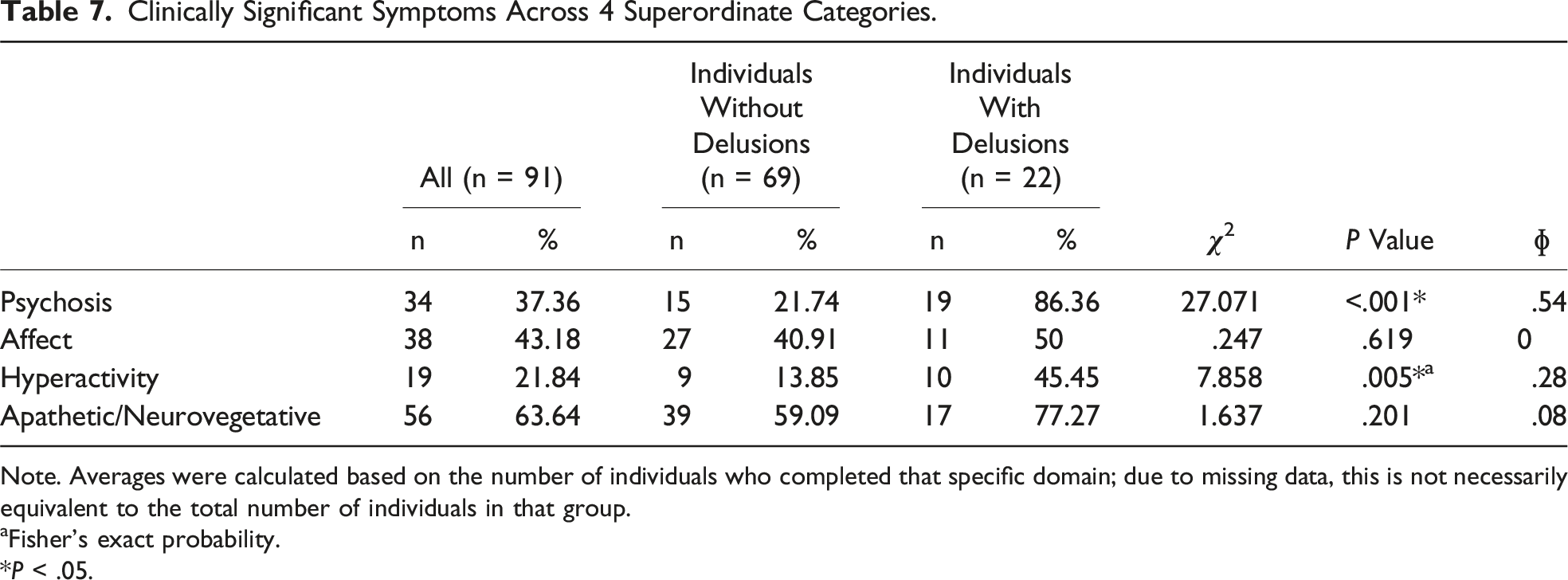
Note. Averages were calculated based on the number of individuals who completed that specific domain; due to missing data, this is not necessarily equivalent to the total number of individuals in that group.
aFisher’s exact probability.
*P < .05.
Figure 4 describes the neuropsychiatric profiles of individuals with and without delusions with respect to clinically significant scores in the 4 superordinate NPI categories. The most common clinically significant symptoms in individuals with delusions were psychosis, followed by neurovegetative, affective, and hyperactive symptoms. In individuals without delusions, the most frequent symptoms were neurovegetative, followed by affective, psychotic, and hyperactive. Neuropsychiatric profiles of individuals with and without delusions.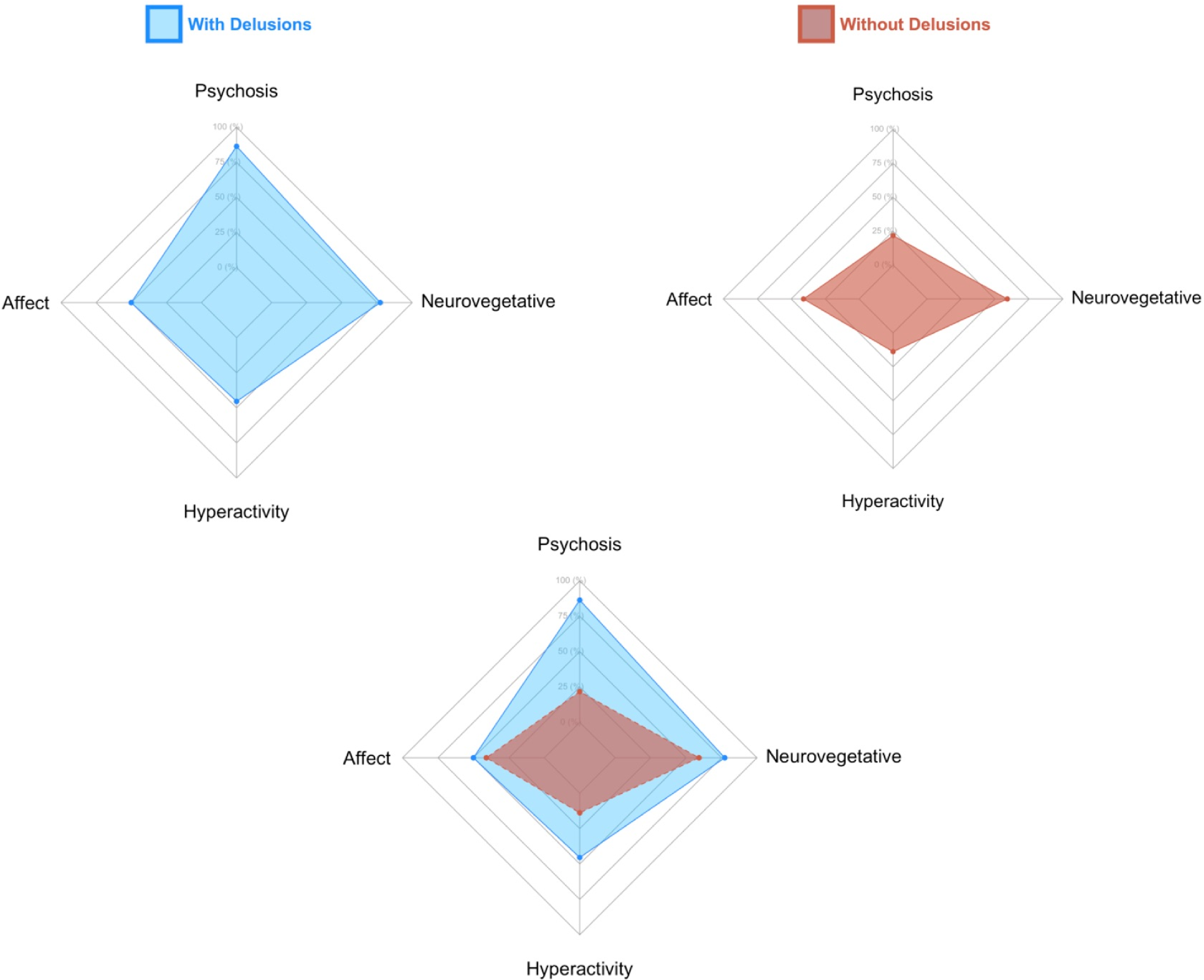
Logistic Regression
Predictors of delusions were evaluated using multivariable binary logistic regression, wherein a full model including ACE total score, NPI domain scores for hallucinations and agitation/aggression, and ESS score as predictors was compared to a reduced model which included only ACE total score as a predictor (both models controlled for age, sex, and CDR). The hallucinations and agitation/aggression domains were chosen for the regression as they were the most significantly different domains between groups (excluding NPI Delusions), with P-values of < .001 (Table 5). The Akaike Information Criterion (AIC) and McFadden’s pseudo R2 indicated the full model (AIC = 60.749; R2 = .555) was more accurate in predicting delusions than the reduced model (AIC = 64.74; R2 = .456). Chi squared testing confirmed the full model was significantly better at predicting the presence of delusions than the reduced model, X2 (7) = 9.991, P = .019.
Evaluating Predictors of Delusions Using Logistic Regression.
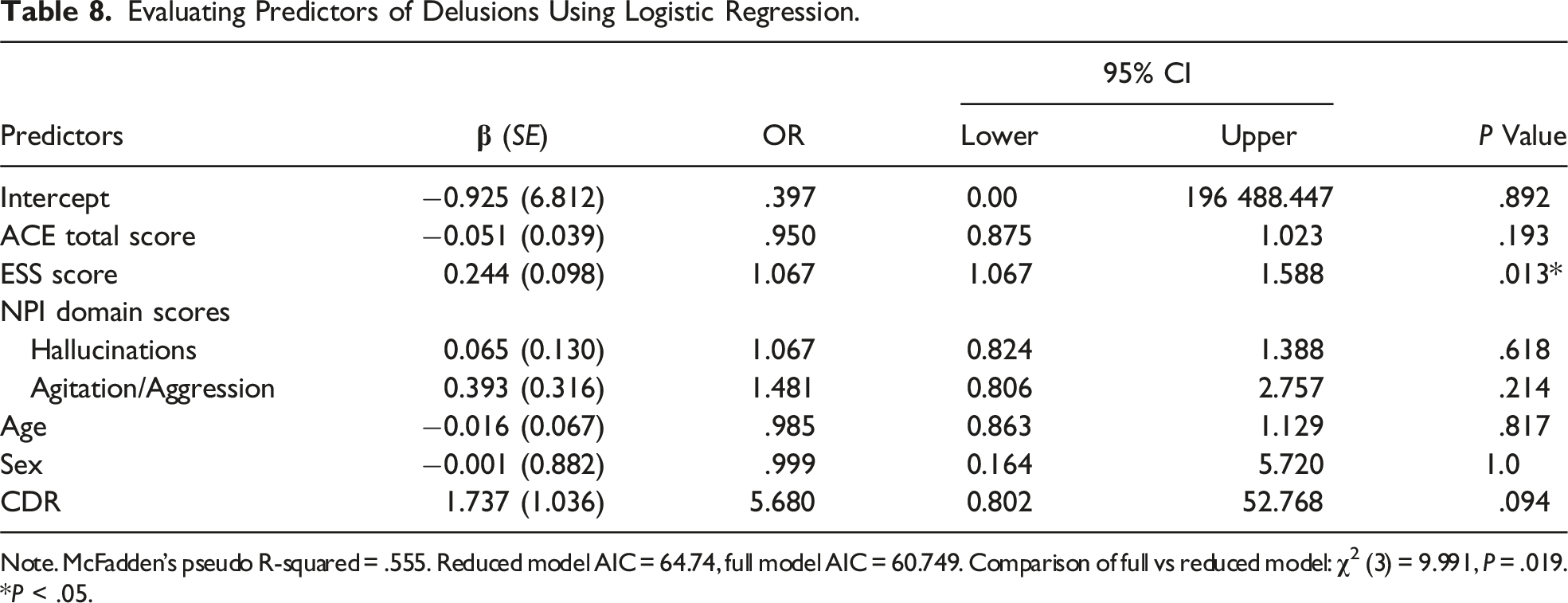
Note. McFadden’s pseudo R-squared = .555. Reduced model AIC = 64.74, full model AIC = 60.749. Comparison of full vs reduced model:
*P < .05.
Thematic Typology
Frequency of Delusions Across Individuals Using NPI 8-Theme Typology.

Note. “Other” category includes 22 delusions across 14 individuals. From “The Neuropsychiatric Inventory: Comprehensive assessment of psychopathology in dementia,” by Cummings JL et al, 1994, Neurology, 44(12), p. 2308-14. (https://doi.org/10.1212/wnl.44.12.2308). Copyright © 1994, Wolters Kluwer Health.
Frequency of Delusional Themes.
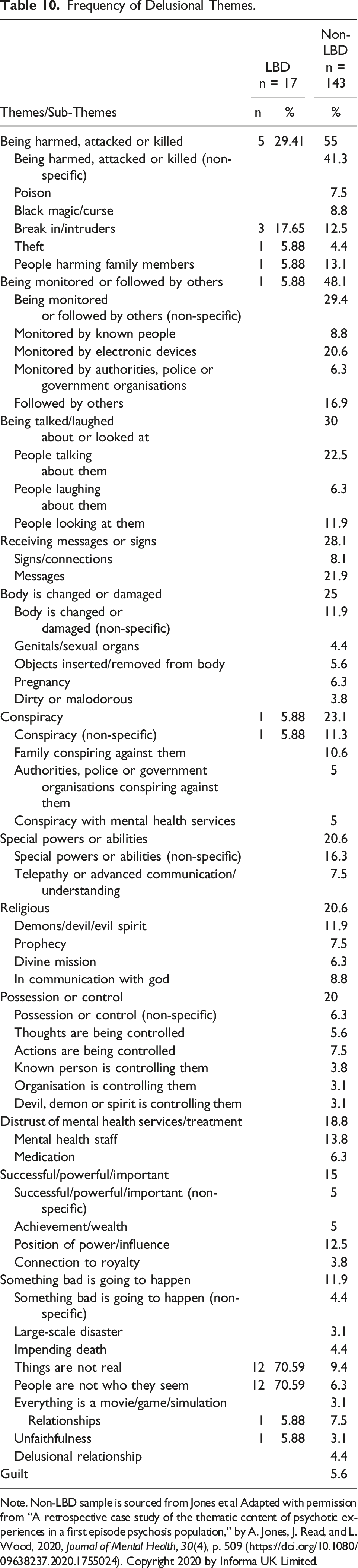
Note. Non-LBD sample is sourced from Jones et al Adapted with permission from “A retrospective case study of the thematic content of psychotic experiences in a first episode psychosis population,” by A. Jones, J. Read, and L. Wood, 2020, Journal of Mental Health, 30(4), p. 509 (https://doi.org/10.1080/09638237.2020.1755024). Copyright 2020 by Informa UK Limited.
Adapted Typology of Delusional Themes.

Note. Adapted with permission from “A retrospective case study of the thematic content of psychotic experiences in a first episode psychosis population,” by A. Jones, J. Read, and L. Wood, 2020, Journal of Mental Health, 30(4), p. 509 (https://doi.org/10.1080/09638237.2020.1755024). Copyright 2020 by Informa UK Limited. Non-LBD sample sourced from Jones et al.
aNew themes and sub-themes not present in original typology.
In the adapted typology, the most common theme was Misidentification (n = 16), renamed from the original “People are not who they seem” to reflect variability among misidentification delusions. Misidentification contained the most common delusion of “misidentification (non-specific)” (n = 6). Additionally, Capgras delusion was observed 4 times, television sign was observed once, and clonal pluralisation was observed twice. Examples of misidentification delusions observed include a delusion that one’s daughter had been replaced with a different person pretending to be her, another individual’s delusion that her husband had been cloned, and one individual’s belief that television characters were real.
The sub-theme “other individuals/groups conspiring against them” was added to account for a delusion in which local labourers were throwing rats on the individual’s roof. The individual also believed that these rats had now infested his home, impelling the addition of “infestation” as a sub-theme of “being harmed, attacked, or killed”, which remained the second most common theme, tied with “residence is not their home”.
The de novo theme “responsibilities” was created to account for 3 delusions in which the individual believed they needed to be fulfilling certain duties. In 2 cases, this was the belief that they needed to care for a child, and in the third case the individual believed he needed to be at work. Two individuals held delusions that deceased family members were still alive, prompting the addition of the theme “deceased person is still alive”. Additionally, 3 individuals experienced delusions wherein they believed someone else was living in their home, and 4 individuals did not believe their residence to be their home. These delusions were classified into “phantom boarders” and “residence is not their home”, respectively.
Discussion
Demographic and Clinical Factors
There were clear demographic and clinical factors associated with delusions in LBD. Individuals with delusions were significantly older than those without, though age at diagnosis and age at first symptom did not differ significantly between the 2 groups. This observation may suggest that delusions are associated with later disease stages, in line with previous research.9,10 Significantly higher CDR scores among individuals with delusions further supports this association, and higher NPI delusion domain scores among those with moderate dementia (compared to questionable or no dementia) may suggest that delusion severity and/or frequency are also associated with later disease stages. No significant difference was found regarding sex, with males constituting the majority of each group, in line with previous research demonstrating a higher ratio of males to females in PDD and DLB. 42 These results are also in line with a recent meta-analysis which reported no significant sex difference in the prevalence of delusions and hallucinations in alpha-synucleinopathies when controlled for clinical diagnosis. 43
Rates of sexual dysfunction and bladder issues were lower than what would be expected of an LBD sample.44-46 Additionally, the rate of hypertension was lower than what would be expected of a sample of older people. 47 However, information regarding preexisting conditions (including diabetes mellitus, arterial hypertension, dyslipidaemia, and arrhythmia) was extracted from medical records or obtained via family members, which should be considered a limitation of this study given conditions were not confirmed diagnostically. Similarly, anosmia was assessed using a structured self-report anchored to past smell ability, and, if positive, considered “probable anosmia”, though a subset of patients were referred for objective psychophysical testing to verify a diagnosis of “definite anosmia”. Further, arrhythmia was recorded as an overarching condition group so we are unable to specify which types of arrhythmia were present in our sample.
Cholinesterase inhibitors were prescribed to significantly more individuals with delusions, and overall were prescribed at a higher rate than antipsychotics. This is consistent with research which supports using cholinesterase inhibitors as first-line treatments for psychotic symptoms in LBD.7,48,49 The unequal rates of parkinsonism and dopaminergic antiparkinsonian prescriptions are in line with practices that suggest lowering or eliminating dopaminergic medications to reduce the risk of psychotic symptoms in LBD. 49 There was no significant difference in antiparkinsonian prescriptions between those with and without delusions, though this category includes several different types of antiparkinsonian medication (dopaminergic therapies, COM-T and MAO-B inhibitors, and amantadine), so we are unable to draw conclusions about dopaminergic medications specifically. The decision to include multiple types of medication under the antiparkinsonian category should be considered a limitation to our study, and future research could be improved by analysing medications more closely, including by individual medication or specific class. While our study did not include analyses specific to delusional jealousy, Perugi et al (2013) identified a potential relationship between dopaminergic medication and delusional jealousy in PD. 25 Future research may seek to clarify this relationship to enable clinicians to make more informed decisions when determining which antiparkinsonian agents to prescribe to LBD patients. Higher rates of fluctuating alertness and higher ESS scores were demonstrated by the delusions group; however, neither NPI nighttime disturbance scores nor rates of RBD were found to be significantly different among groups. This is not in line with previous research which has suggested an association between nocturnal sleep disturbances, including RBD, and psychosis in LBD. 22 Studies in PD have demonstrated that sleep disorders and EDS can negatively impact cognitive functioning, which in turn may lead to source monitoring errors that allow for the maintenance of delusional beliefs.43,51,55 A link between RBD and delusions in PD was also demonstrated by Pacchetti et al (2005). 23 The exact underlying mechanisms and relationship between nocturnal sleep disturbances and delusions in LBD remain unclear, though there exist hypotheses that brainstem degeneration in parkinsonian-like conditions eventually may lead to dysregulation of normal sleep patterns. 22 In non-LBD populations, similar links between sleep and psychosis have been made.51,52 Irregular melatonin secretion has been observed in schizophrenia, and is hypothesised to play a role in dopamine dysregulation, ultimately contributing to the creation and/or maintenance of psychotic symptoms.53,54
It is possible that our results indicate a relationship between excessive daytime sleepiness (EDS) and delusions irrespective of RBD/other sleep disturbances. A link between EDS and delusions is further supported by the results of our regression analysis in which ESS score was the only variable found to be a statistically significant predictor of delusions, demonstrating better predictive ability than total ACE scores and NPI hallucination and agitation/aggression domain scores. However, a limitation of these findings is that the diagnosis of RBD was based on clinical expert assessment only as polysomnography was not available for most patients. We note that while sensitivity is often high in non-PD populations, it may drop significantly in PD cohorts, with a high rate of false positives, unless bed partner history is taken into account, 50 as was the case in our series. Given that our results are not in line with prior research, future studies should seek to clarify the relationship between RBD/other sleep disturbances and delusions in LBD. We note that the use of polysomnography to confirm RBD in participants would be beneficial and allow for more robust conclusions to be drawn.
The Association Between Delusions and Distinct Cognitive Profiles
Overall, delusions were associated with significantly poorer cognitive functioning. All individuals with delusions were diagnosed with MCI or dementia, with DLB being the most common diagnosis occurring at a significantly higher rate than in those without delusions. Scores on the NPI Delusions domain were also significantly higher among those in the mild or moderate dementia stages. These results are in line with previous findings that psychotic symptoms occur more often in PDD and DLB, and provide further support for an association between delusions and later disease stage.8-10,56
Both groups demonstrated the same pattern of ACE-III domain performance, with highest scores in the language domain and lowest scores in the verbal fluency domain. However, individuals with delusions performed significantly worse in all domains, reflecting a considerably more impaired cognitive profile, supporting the hypothesis that delusions are associated with a distinct cognitive profile. This is in line with previous findings reflecting an association between psychosis and poorer cognition in LBD.9,20 A potential explanation for this relationship is that impaired cognition may allow for the maintenance of delusional beliefs through source monitoring errors.51,55 The finding that cognition is considerably more impaired in those with delusions indicates that preserving cognition may indeed help to alleviate or prevent delusions in LBD. Future research may seek to evaluate whether methods to help reduce the decline of cognition in LBD, such as cognitive training or medications aimed at slowing decline, also results in less frequent/severe delusions. It should be noted, however, that the regression analysis did not indicate total ACE-III score to be a significant predictor of delusions. One explanation for this finding is that there may exist conceptual overlap with other predictors included in the regression model, such as the CDR and NPI, which may more directly capture the cognitive and functional features associated with delusions. The inclusion of these variables may have reduced the unique predictive value of total ACE-III score, despite no statistical indication of multicollinearity among the predictors. It is also possible that total ACE-III score was not a significant predictor of delusions in our model due to a lack of power resulting from a relatively small sample size. The discordant nature of these results highlights the need for further investigation into the exact relationship of cognition and delusions.
The Association Between Delusions and Distinct Neuropsychiatric Profiles
Results of the NPI revealed that overall, individuals with delusions reported more neuropsychiatric symptoms, and had significantly higher total NPI scores. The domain scores and the frequency of clinically significant symptoms were significantly higher among individuals with delusions in the non-delusion domains of hallucinations, agitation/aggression, irritability/lability, and nighttime disturbances. These results largely mirror the findings of Warren et al’s 2018 systematic review of delusions in PD, as well as the preliminary findings from the 2018 study by Tzeng et al investigating delusions in DLB.9,20
When evaluating the proportion of clinically significant symptoms in 4 superordinate categories of NPI domains, psychosis and hyperactive symptoms were significantly higher in those with delusions, while rates of affective and apathetic/neurovegetative symptoms did not differ significantly. For individuals with delusions, the most common category was psychosis followed by apathetic/neurovegetative symptoms. For individuals without delusions, apathetic/neurovegetative symptoms were most common, followed by affective symptoms. Additionally, despite being the least common category for both groups, hyperactive symptoms were significantly more common in those with delusions, endorsed by almost half of the group compared to 13.85% in those without delusions. In conjunction with significantly higher rates of psychotic symptoms, these results point to a distinction in the pattern of neuropsychiatric symptoms experienced by those with and without delusions. Individuals with delusions present with primarily psychotic-apathetic/neurovegetative profiles, while those without delusions present with primarily apathetic/neurovegetative-affective profiles. Those with delusions also present with a more hyperactive profile, which includes symptoms of agitation/aggression, disinhibition, and irritability/lability. These results are in line with previous findings.9,20 This difference in symptomatology supports the hypothesis that delusions are associated with distinct neuropsychiatric profiles.
It is possible that delusions and hyperactive symptoms share common underlying mechanisms, helping to explain the distinction in neuropsychiatric profile. Neurotransmitter systems associated with psychosis, such as dopamine, glutamate, and serotonin, and consequently the brain structures involved in their transmission, have been implicated in hyperactive symptoms including aggression, agitation, and disinhibition in non-LBD populations.57,58 However, it is also possible that hyperactive symptoms and delusions arise from distinct yet co-occurring mechanisms. While overlapping neurotransmitter systems contribute to both symptom domains, the regional neuroanatomical substrates may differ causing the distinctive symptomology. This idea is supported by Kanemoto et al’s 2025 59 recent study, finding that psychosis in DLB was associated mainly with hypoperfusion of the left posterior cortex, insula and frontal gyrus; whereas agitation was linked to hyperperfusion within frontal, striatal, and thalamic tracts. Should a link between delusions and hyperactive symptoms be confirmed, interventions which target hyperactive symptoms may prove effective in alleviating delusions as well.
Despite significant differences between the groups, regression analyses did not identify NPI domain scores for agitation/aggression or hallucinations as significant predictors of delusions. However, given that agitation/aggression was the only hyperactive symptom included in the regression, this does not necessarily indicate that hyperactive symptoms as a whole lack predictive ability; future research may seek to investigate whether domain scores for disinhibition and irritability/lability are significant predictors. The failure to identify hallucinations as a significant predictor was unexpected, given their significantly higher severity and frequency in the delusions group. These results indicate that while hallucinations and agitation/aggression scores may be related to delusions, when controlling for other predictors this association is much weaker. Further research is needed to re-examine these relationships in order to provide clarity regarding associated neuropsychiatric symptoms.
The Thematic Typology of LBD
There were many delusions from the LBD sample which could not sufficiently be categorised using the NPI typology, nor the original Jones et al typology. This reflects substantial inadequacy in their ability to be utilised among an LBD population. It is particularly concerning that the NPI typology was unable to align thematically the majority of delusions identified in our sample, given that the NPI is used specifically with neuropsychiatric populations. Additionally, aligning themes from the LBD sample to the Jones et al typology revealed several differences in thematic frequency. Namely, the most common delusions among the LBD sample were delusions of misidentification, reported by nearly all individuals in the sample. This contrasts the pattern identified in the non-LBD sample from Jones et al, wherein “people are not who they seem ” was one of the least commonly observed themes. 32 In the LBD sample, “being harmed, attacked, or killed” was the second most common theme, though it was only recorded in roughly one-third of individuals, compared to over half of individuals in the non-LBD sample. The differences in thematic frequency highlight the unique spread of themes found in LBD delusions, further supporting the need for a distinct LBD typology.
To address the insufficiency of the NPI and Jones et al typologies, an adapted typology based on Jones et al was created including additional themes and sub-themes. The changes made in our adapted typology, including both the addition and modification of existing themes, again underscore the distinct spread of themes identified in our LBD sample, emphasizing the need for an LBD-specific typology. However, while the results of the adapted typology do reflect the common nature of delusions of misidentification in LBD, only Capgras delusion, TV sign, and clonal pluralisation were observed; this is not in line with previous research which has observed other kinds of delusions of misidentification, such as Fregoli syndrome or reduplicative paramnesia, in LBD samples.30,59 Additionally, theft was only observed in one description, despite prior research reporting the theme in over one-third of a DLB sample. 9
There remained several descriptions which lacked sufficient detail to discern a specific theme and/or sub-theme. Because of this, 2 descriptions referencing paranoid delusions could not be classified, and 9 descriptions of misidentification could only be classified as “misidentification (non-specific)”. The inability to extract specific themes for these delusions, in addition to only analysing 17 descriptions total, limited the ability to adequately assess the fit of the NPI and Jones et al typologies to the LBD sample and to construct a comprehensive LBD-specific typology. 32 It is also possible that the use of retrospective chart descriptions, particularly from such a small sample, may introduce bias as more characteristic symptoms are likely to be documented compared to common ones. Our adapted typology provides a starting point from which we hope future studies may expand upon using larger sample sizes to more accurately capture the thematic typology of delusions in LBD.
Conclusions and Future Directions
This is the first study to investigate the clinical and demographic factors, as well as the cognitive and neuropsychiatric profiles, associated with delusions across 4 LBD diagnoses. This study has provided valuable insights which may be used by clinicians to guide future clinical practices and ultimately improve intervention strategies for patients with LBD. The findings suggest that clinicians should closely monitor for delusions in patients with LBD, particularly as the disease progresses. Furthermore, increased vigilance is warranted when symptoms such as excessive daytime sleepiness or agitation emerge, as this study found that delusions may be associated with more advanced disease stages and increased levels of daytime sleepiness The strong association between delusions and distinct cognitive and neuropsychiatric profiles indicates that routine screening for delusions should be integrated into cognitive and behavioural assessments. Additionally, this study revealed that delusions in LBD demonstrate a distinct thematic typology. The results also support the use of cholinesterase inhibitors as a preferred first line treatment over antipsychotics in managing psychotic symptoms.
Future research should seek to re-evaluate clinical/demographic factors utilising a larger sample size, more diverse patient cohorts and more standardised assessment protocols, in order to better characterise delusional themes and identify predictors. Further, researchers should conduct structured interviews with patients in order to ascertain sufficient details regarding the thematic content of delusions to construct a comprehensive thematic typology.
Supplemental Material
Supplemental Material - Delusions in Lewy Body Disease: A Cross-Sectional Study on Associated Factors and Lived Experiences
Supplemental Material for Delusions in Lewy Body Disease: A Cross-Sectional Study on Associated Factors and Lived Experiences by Caroline Sirna, Ashay Panse, Panos Alexopoulos, Ella Carol, Orla Keane, Iracema Leroi in Journal of Geriatric Psychiatry and Neurology
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This was an unfunded project, but supported in kind by the Global Brain Health Institute, Trinity College Dublin, for the time and resources of Iracema Leroi as well as the Erasmus + mobility program to support the time of Panos Alexopoulos.
Ethical Considerations
This study received full ethics approval from the St. James’s Hospital/Tallaght University Hospital Join Research Ethics Committee (Submission number: 4020; Project ID: 4325). Full ethics approval was granted March 11th, 2025. This is an IRB-approved retrospective study, all patient information was de-identified and patient consent was not required. Patient data will not be shared with third parties.
Consent to Participate
The participant information sheet and consent checklist specifically refers to ‘consent to publish'
Consent for Publication
All authors have signed up to a publication code for the study. The participant information sheet and consent checklist specifically refers to ‘consent to publish’.
Data Availability Statement
All data, once fully anonymised, may be made available following specific request to the corresponding author, in concordance with ethical considerations, legal frameworks (GDPR), and institutional policies.
Supplemental Material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
