Abstract
Purpose
Bowel cancer screening (BCS) is a critical preventive health measure. However, participation in BCS remains suboptimal in some populations. We aimed to examine the association between psychosocial factors and participation in bowel cancer screening among adults aged 45 years and above in Australia.
Design
Prospective cohort study.
Setting and sample
Our study utilised longitudinal data from four waves of the Household, Income, and Labour Dynamics in Australia (HILDA) Survey, comprising 29 334 person-year observations from 11 315 individuals.
Measures
We employed social connection, social isolation, and community membership as proxies for psychosocial factors and explored their relationship with bowel cancer screening participation.
Analysis
We performed descriptive statistics and random-effects logistic regression. The relationships were also stratified by age groups and gender to highlight heterogeneous effects.
Results
After adjusting for various confounding factors, our findings demonstrated that high social connection (adjusted Odds Ratio [aOR]): 1.14, 95% CI: 1.06-1.22) and community membership (aOR: 1.23, 95% CI: 1.15-1.32) were significantly and positively associated with participation in bowel cancer screening. Further stratified analysis revealed that this association was heterogeneous; the link between high social connection was significant for men (aOR: 1.17, 95% CI: 1.06-1.30) but not for women. Additionally, while community membership served as a significant predictor across all age groups, the positive association with social connection was evident in adults aged 45 to 59 (aOR: 1.13, 95% CI: 1.01-1.27) and those aged 60 to 74 years (aOR: 1.13, 95% CI: 1.09-1.36).
Conclusion
Our study highlighted the role of psychosocial factors in influencing participation in bowel cancer screening. Our results suggest that public health policies should prioritise initiatives that promote social engagement and strengthen community ties.
Keywords
Introduction
Bowel cancer (BC) remains a major global health crisis and is currently ranked as the third most commonly diagnosed cancer and the second leading cause of cancer-related deaths worldwide. 1 Interventions to increase awareness of population-wide bowel cancer screening programs have demonstrated substantial benefits in reducing mortality and disease burden. Initiatives such as the Australian National Bowel Cancer Screening Program (NBCSP) invite citizens aged 45-74 years to complete a faecal occult blood test kit (FOBT) every 2 years through direct mail to the homes of the invited participants. 2 Evidence has shown that NBCSP has led to earlier diagnoses, fewer cancer-related complications, and improved survival rates. 3 Despite the success rate of these initiatives, the participation rates for screening programs have been suboptimal, often failing to maximise the marginal benefits of large interventions. Between 2021 and 2022, only approximately 40% of invited kit recipients to the Australian NBCSP participated in the screening.4,5 This low participation rate could result from a range of psychosocial determinants of health behaviours, including social connection, social isolation, and community membership.
In the expanding body of literature, psychosocial factors, such as social connection, social capital, and social isolation, have gained recognition as critical determinants of preventive healthcare use, including cancer screening. High social connections and high levels of social capital have been consistently linked to greater engagement in preventive healthcare services.6-9 In this context, social connections refer to the relationships and networks that individuals maintain, which have the potential to influence their health behaviours and access to healthcare resources significantly. These connections facilitate emotional support, the sharing of health-related information, and heightened awareness, all of which encourage participation in preventive health measures.10,11 For example, individuals embedded in robust social networks often benefit from increased motivation and practical guidance, making them more likely to engage in screening programs. A growing number of studies have highlighted the positive association between high social networks and participation in colorectal cancer screening.6,9,12 Individuals with high social connectivity have been shown to exhibit higher rates of engagement with screening programs, underscoring the vital role of social structures in promoting preventive healthcare behaviours.6,9,12
Social capital refers to the resources accessible through social networks, including trustworthiness, social norms, and mutual assistance.13,14 Community membership serves as a direct, measurable indicator of an individual’s engagement in the activities that generate and sustain these vital social resources. In this study, we used community membership as a proxy to assess an individual’s active investment in building the social networks that influence health behaviours. Community membership significantly impacts social capital by providing vital opportunities for social interaction, shared purpose, and network building, all of which are crucial elements of robust social capital resources. Higher levels of social capital are linked to greater utilisation of preventive healthcare services. Existing studies have demonstrated that communities with high social cohesion and trust experience higher rates of participation in bowel cancer screening.7,8,15-17 Social capital fosters a sense of collective responsibility and facilitates the dissemination of health-related information, thereby encouraging engagement in health-promoting behaviours.
Conversely, social isolation, defined as a lack of social contacts, connections, and support, has been identified as a significant barrier to participation in health-related behaviours. Socially isolated individuals often encounter obstacles in accessing healthcare information and may lack the social encouragement required to engage in preventive services. 11 Unlike the positive associations of social connection and social capital, social isolation has been widely documented in the literature as a deterrent to preventive healthcare utilisation. 10 Evidence indicates that social isolation is correlated with lower participation rates in preventive health services, including bowel cancer screening.11,12,18,19 These findings highlight the dual role of social factors in either facilitating or hindering engagement with health-promoting behaviours.
While demographic and socioeconomic factors remain critical determinants of healthcare utilisation, the COVID-19 pandemic has further highlighted the pivotal role of psychosocial factors in shaping health behaviours and influencing preventive healthcare engagement. Behavioural and health economic models, including the widely recognised Andersen 20 model of healthcare utilisation, have traditionally emphasised the demographic and socioeconomic determinants of healthcare access and usage. However, the pandemic’s impact, particularly the widespread social isolation measures, 21 has highlighted the essential influence of psychosocial factors, such as social connections, social isolation, and social capital, on access to and utilisation of healthcare services. 22 Using panel data from a longitudinal population-based survey, we aim to explore the relationship between psychosocial factors and bowel cancer screening among Australian adults aged 45 years and over. While the overall benefits of screening are clear, participation is not uniform across all demographic groups. The uptake of screening often varies by age and gender. Furthermore, the influence of psychosocial factors on health behaviours may not be consistent across these groups; for instance, social connection might be more significant for men than for women, or for younger adults compared to older adults. Understanding this potential variation is vital for designing and targeting effective public health interventions. Therefore, a key secondary objective of our study was to explore these potential heterogeneous effects to identify specific populations that may benefit most from initiatives aimed at strengthening social ties.
Methodology
Data Source and Sample Selection
We utilised restricted release data from the Household, Income, and Labour Dynamics in Australia (HILDA) Survey. The HILDA Survey is a longitudinal study that tracks a nationally representative sample of Australians, involving over 17 000 residents from 7000 households annually, since its inception in 2001. Households were selected using a multi-stage area-based probability sampling design in the HILDA Survey. Using distinct survey questionnaires (e.g., household questionnaires, continuing person questionnaires, self-completion questionnaires, and interview showcards), the HILDA Survey collects a wide range of data on individuals and households, including wealth, material deprivation, health, fertility, employment, income, and lifestyle factors. A detailed description of the survey design, data collection procedures, and participant recruitment can be found elsewhere. 23
We analysed data from four waves (9, 13, 17, and 21) of the HILDA Survey spanning 2009 to 2021. The key reason for using these four waves is that the HILDA Survey collects data on the health module every 4 years. Therefore, data on bowel cancer screening are available only for these four waves. The NBCSP in Australia invites individuals aged 45-74 years to participate in screening every 2 years for the early detection of bowel cancer. To align with the NBCSP, we included individuals aged ≥45 who were eligible for screening. To minimise bias and enhance the statistical power of our analysis, we retained all the samples, including those with missing data. We filled in the missing data points using established imputation techniques. This enabled us to work with a complete dataset without losing valuable information from the partially incomplete records. Our final analytic sample comprised 29 334 person-years of observations from 11 315 unique respondents.
Outcome Variable
The primary outcome variable of our study was participation in bowel cancer screening (BCS). This variable was derived from participants’ responses to the question: “Had check-up or test in the last 12 months - Screening for bowel cancer?”. Responses were recorded as a binary indicator with affirmation taken as 1 and 0 otherwise. We acknowledge that the NBCSP operates on a biennial cycle, while our outcome measure captures screening within the last 12 months.
Exposure Variables
Three psychosocial measures were extracted from the Self-Completion Questionnaire (SCQ): (1) social connection, (2) social isolation, and (3) community membership. These measures collectively assess social networks, which encompass the extent of social connections, levels of social isolation, and community membership.
Social Connection
The social connection metric was derived from five items, each rated on a 7-point Likert scale ranging from 1 (strongly agree) to 7 (strongly disagree). The items are as follows: (1) “I seem to have lots of friends”, (2) “When something’s on my mind, just talking with the people I know can make me feel better”, (3) “I enjoy the time I spend with the people who are important to me”, (4) “When I need someone to help me out, I can usually find someone”, and (5) “There is someone who can always cheer me up when I’m down.”
Responses to these items were summed to create a composite social connection score ranging from 5 to 35, with higher scores denoting stronger social connections. Concerning its psychometric properties, the five-item social connection scale demonstrated good construct validity and Cronbach’s alpha reliability. 24 To aid the analysis, social connection scores were classified into two groups: low connection (scores below the median value of 28) and high connection (scores of 28 or above).
Social Isolation
Social isolation scores were derived from five items rated on a 7-point Likert scale (1 = strongly agree, 7 = strongly disagree). The items were (1) “I often need help from other people but can’t get it”, (2) “I have no one to lean on in times of trouble”, (3) “I don’t have anyone that I can confide in”, (4) “I often feel very lonely”, (5) “People don’t come to visit me as often as I would like.” The total scores range from 5 to 35, with higher scores indicating greater social isolation. The construct validity and internal reliability of these five-item social isolation scales have been established. 25 Participants were classified as experiencing low social isolation (scores below the median of 12) or high social isolation (scores of 12 or above).
Community Membership
Community membership was evaluated using the self-reported question: “Are you currently an active member of a sporting, hobby, or community-based club or association?” Responses were recorded as binary indicators, with affirmation counted as 1, and 0 otherwise.
Potential Confounder
Potential confounding factors were identified based on the availability of variables in the HILDA study and their relevance, as indicated in the related literature.6,8,10,19,20,22,26-28 These factors encompass age groups (45-59, 60-74, and ≥75 years), gender (male vs female), relationship status (partnered vs unpartnered), completed years of education (Year 12 and below, certificate course completed, and university degree achieved), household yearly disposable income quintiles (quintile 1 [poorest] and quintile 5 [richest]), labour market status (employed, unemployed, and not in the labour force), race (Indigenous vs non-Indigenous), region of residence (major city, regional city, and remote area), body mass index categories (underweight, healthy weight, overweight, and obese), chronic conditions (no chronic condition, single chronic condition, and multimorbidity), smoking status (never smoked, former smoker, and current smoker), alcohol consumption status (never drunk, ex-drinker, and current drinker), physical activity status (none to <1 time a week, 1 to 3 days a week, and 4 to 7 days a week), healthcare card status (yes/no), and private health insurance ownership status (yes/no).
Statistical Analysis
The statistical analysis included descriptive statistics to provide an overview of the sample and longitudinal regression models to identify correlations. Descriptive statistics summarised the analytical sample, presenting categorical variables as frequencies and percentages, whereas continuous variables were reported as means and standard deviations. Random-effects logistic models were fitted to investigate the association between psychosocial factors and bowel cancer screening among middle-aged and older Australians. By addressing potential confounders, random-effects logistic regression models were used to examine between-person differences to identify linkages between psychosocial factors and bowel cancer screening. To explore the potential heterogeneity in the key findings, we conducted further analyses stratified by age groups and gender. We also conducted a robustness check to assess whether the main findings are consistent across different periods, specifically before and during the COVID-19 pandemic. The analysis was divided into two models: one for the pre-COVID-19 period (Waves 9, 13, and 17) and one for the period during the pandemic (Wave 21). The model provided an adjusted odds ratio (aOR) with 95% confidence intervals (CIs) and was considered statistically significant at P < .05. All analyses were conducted using STATA 17 software version (Stata SE 17, College Station, TX: Stata Corp LLC, USA).
Results
Sample Characteristics
Distribution of the Analytic Sample: Baseline, Final, and Pooled Across all Waves
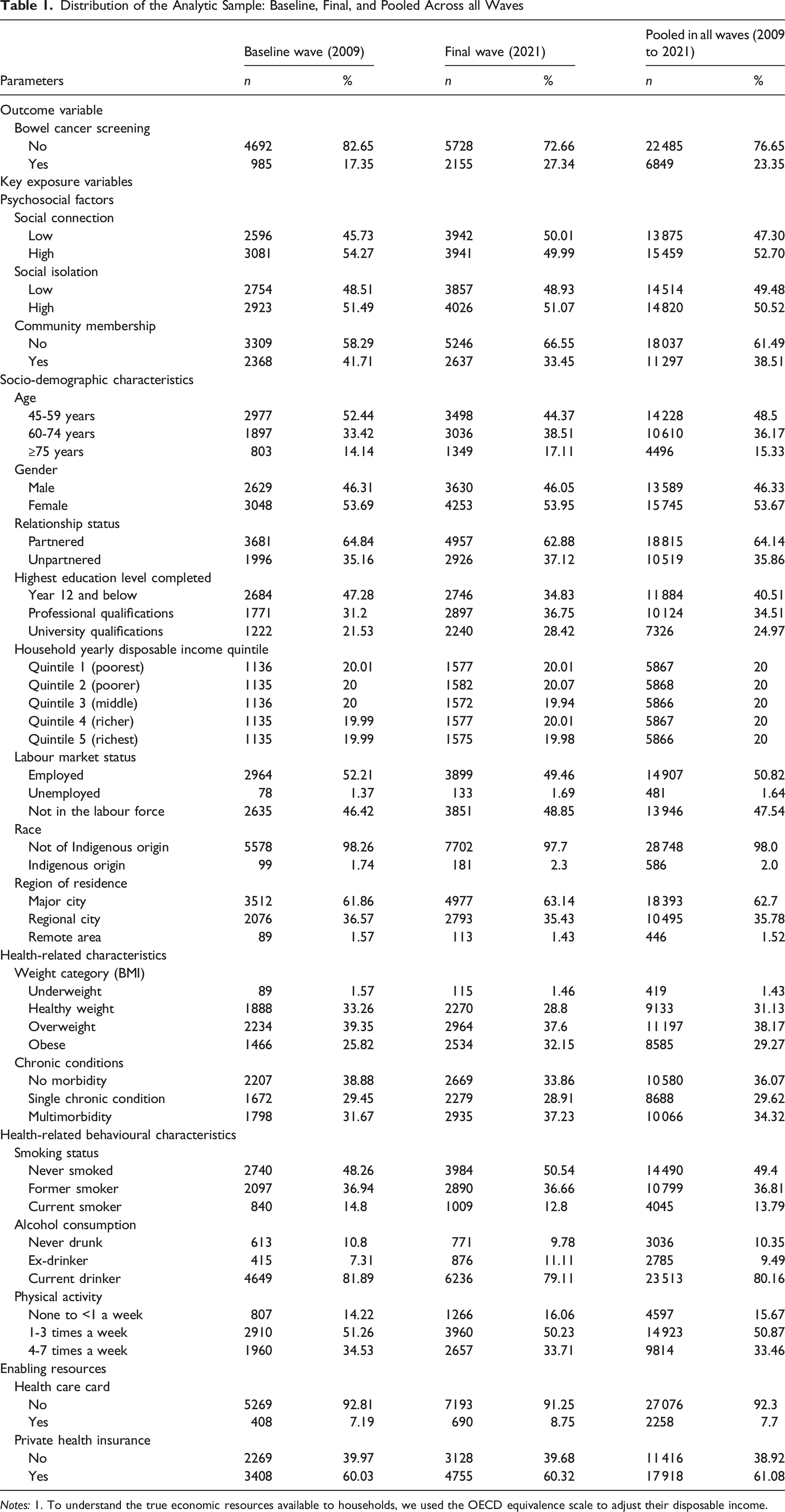
Notes: 1. To understand the true economic resources available to households, we used the OECD equivalence scale to adjust their disposable income.
Based on the pooled data across all waves, the results indicated that nearly half of the participants were aged 45 to 59 years (48.5%), predominantly female (53.67%), partnered (64.14%), of non-Indigenous origin (98.0%), and primarily resided in major cities (62.7%). The most common level of educational attainment was Year 12 and below (40.51%). Regarding economic factors, about half of the participants were employed (50.82%), while 47.54% were not in the labour force. In terms of health status, a significant portion of the sample was overweight (38.17%) or obese (29.27%), with over a third experiencing multimorbidity (34.32%). Common health-related behaviours included being a current alcohol drinker (80.16%), a never-smoker (49.4%), and engaging in physical activity 1 to 3 times per week (50.87%). Regarding enabling resources, the majority of participants held private health insurance (61.08%), while a minority held a healthcare card (7.7%).
Figure 1 illustrates the proportions of bowel cancer screening, high social connection, high social isolation, and community membership across the survey waves. The results indicate a significant increase in bowel cancer screening rates, rising from 17.4% in 2009 to 27.3% in 2021. The proportion of individuals reporting high levels of social connections has decreased, particularly during the COVID-19 pandemic in 2021. Specifically, the proportion of people reporting high levels of social connection fell from 53.1% in 2017 to 50.0% in 2021. While social connections declined during the COVID-19 pandemic, there was a slight increase in the proportion of individuals experiencing social isolation, from 49.4% in 2017 to 51.1% in 2021. A significant decline in community membership was noted, with the proportion decreasing from 41.7% in 2009 to 33.5% in 2021. Proportion of Bowel Cancer Screening, Social Connection, Social Isolation, and Community Membership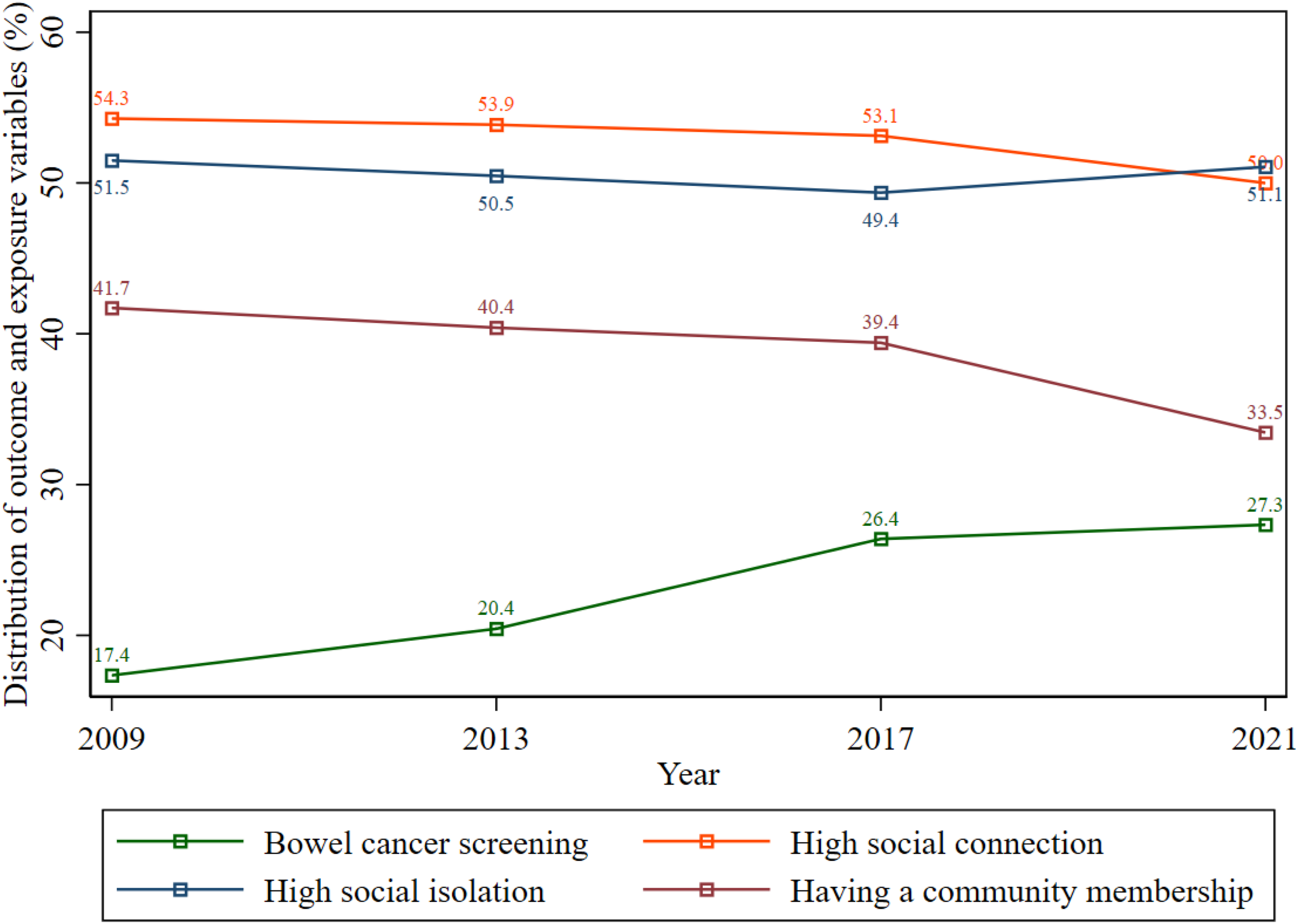
Figure 2 (Panels 2A, 2B, and 2C) illustrates the proportions of bowel cancer screening based on key exposure variables, such as social connection, social isolation, and community membership, across different waves. This figure indicates that individuals with high levels of social connection were more likely to undergo bowel cancer screening than those with low levels of social connection (Figure 2A). Individuals with high social connections showed a higher bowel cancer screening rate (29.03%) than those with low social connections (25.65%) in 2021. Additionally, Panel 2B illustrates that participants with low social isolation had higher rates of bowel cancer screening than those with high social isolation across all waves. In 2021, individuals with low levels of social isolation were more likely to undergo bowel cancer screening, recording a screening rate of 28.23%, in contrast to 26.43% for those with high social isolation. Panel 2 C also indicates that individuals with community membership were more likely to undergo bowel cancer screening. In 2021, those with community membership had a higher bowel cancer screening rate (31.32%) compared to those without (25.33%). The Rate of Bowel Screening by Social Connection, Social Isolation, and Community Membership Over the Study Period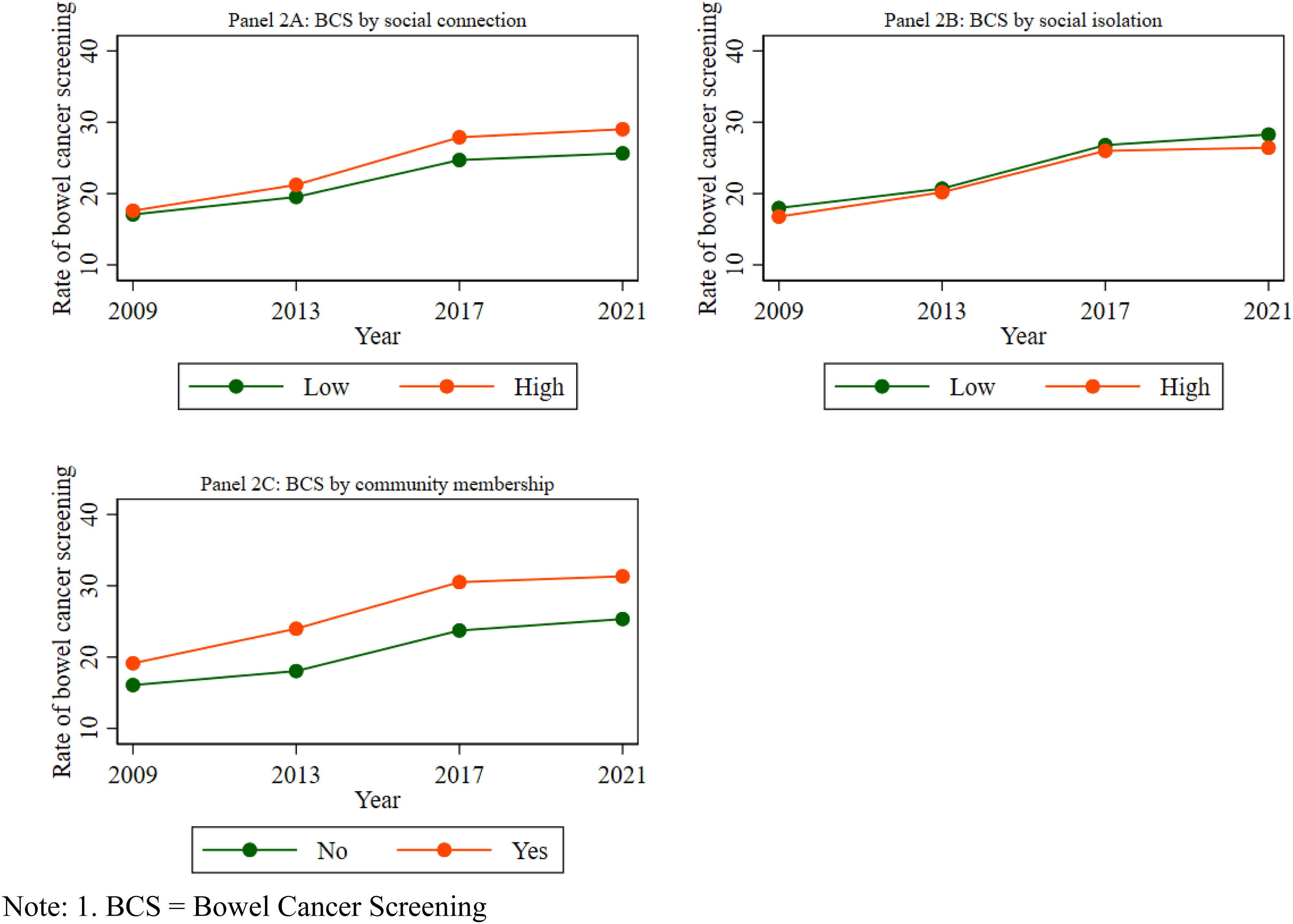
Main Regression Results
The Relationship Between Psychosocial Factors and Bowel Cancer Screening, Random-Effects Logistic Regression Model
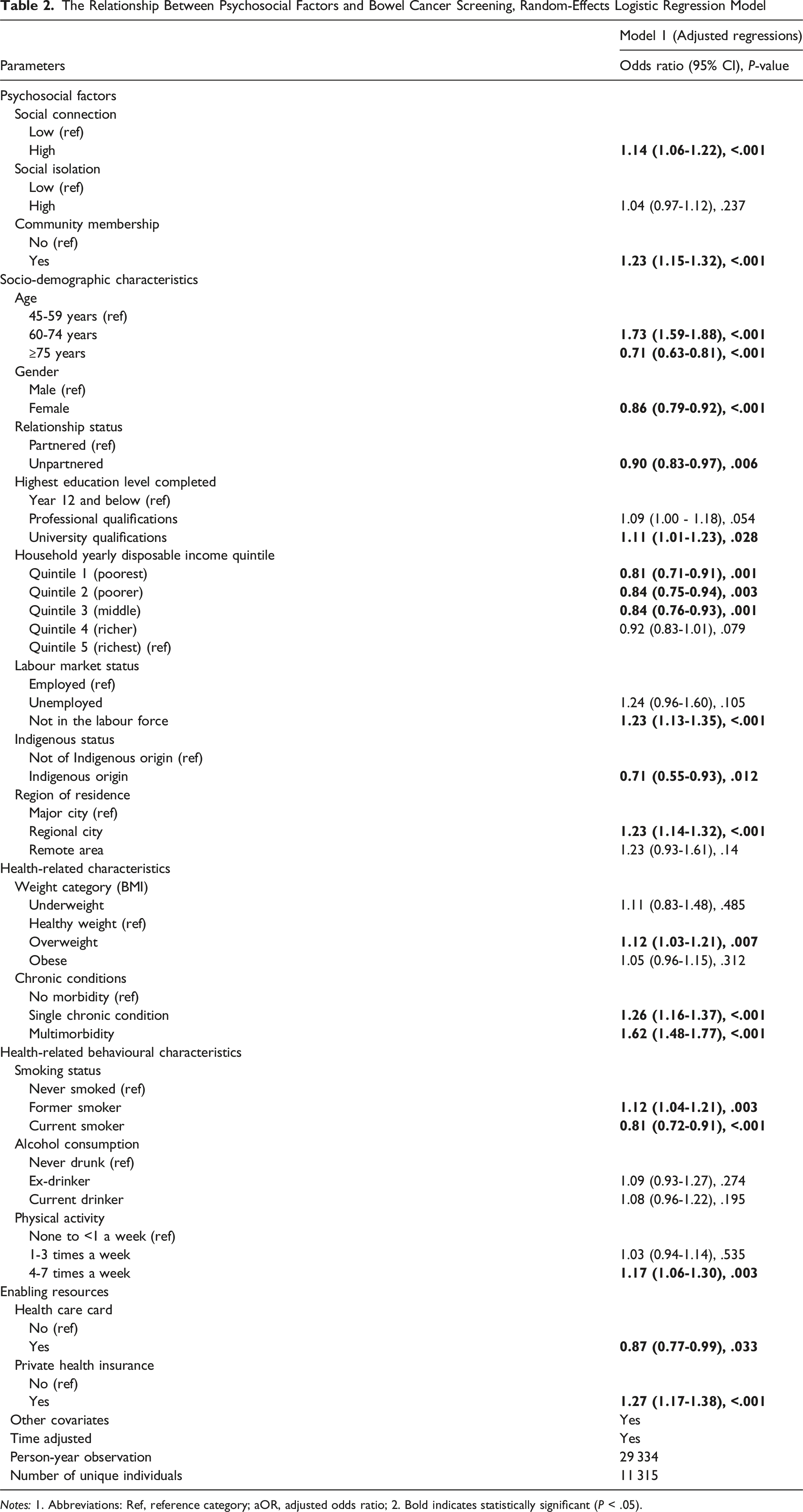
Notes: 1. Abbreviations: Ref, reference category; aOR, adjusted odds ratio; 2. Bold indicates statistically significant (P < .05).
Robustness Check
Random-Effects Logistic Regression Model of the Association Between Psychosocial Factors and Bowel Cancer Screening, Stratified by the COVID-19 Period
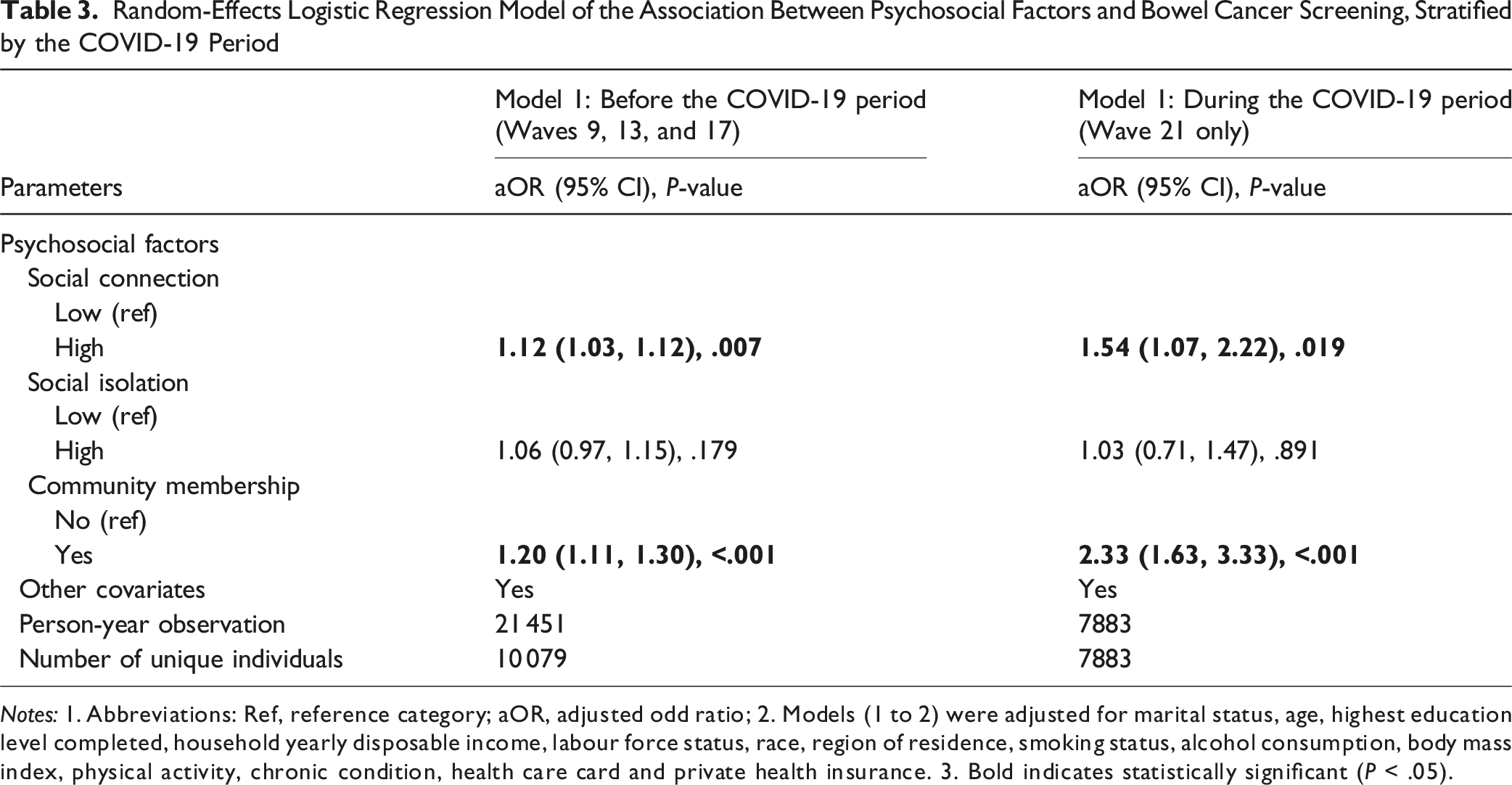

Notes: 1. Abbreviations: Ref, reference category; aOR, adjusted odd ratio; 2. Models (1 to 2) were adjusted for marital status, age, highest education level completed, household yearly disposable income, labour force status, race, region of residence, smoking status, alcohol consumption, body mass index, physical activity, chronic condition, health care card and private health insurance. 3. Bold indicates statistically significant (P < .05).
Heterogeneous Effects
Random-Effects Logistic Regression Model of the Association Between Psychosocial Factors and Bowel Cancer Screening, Stratified by Age
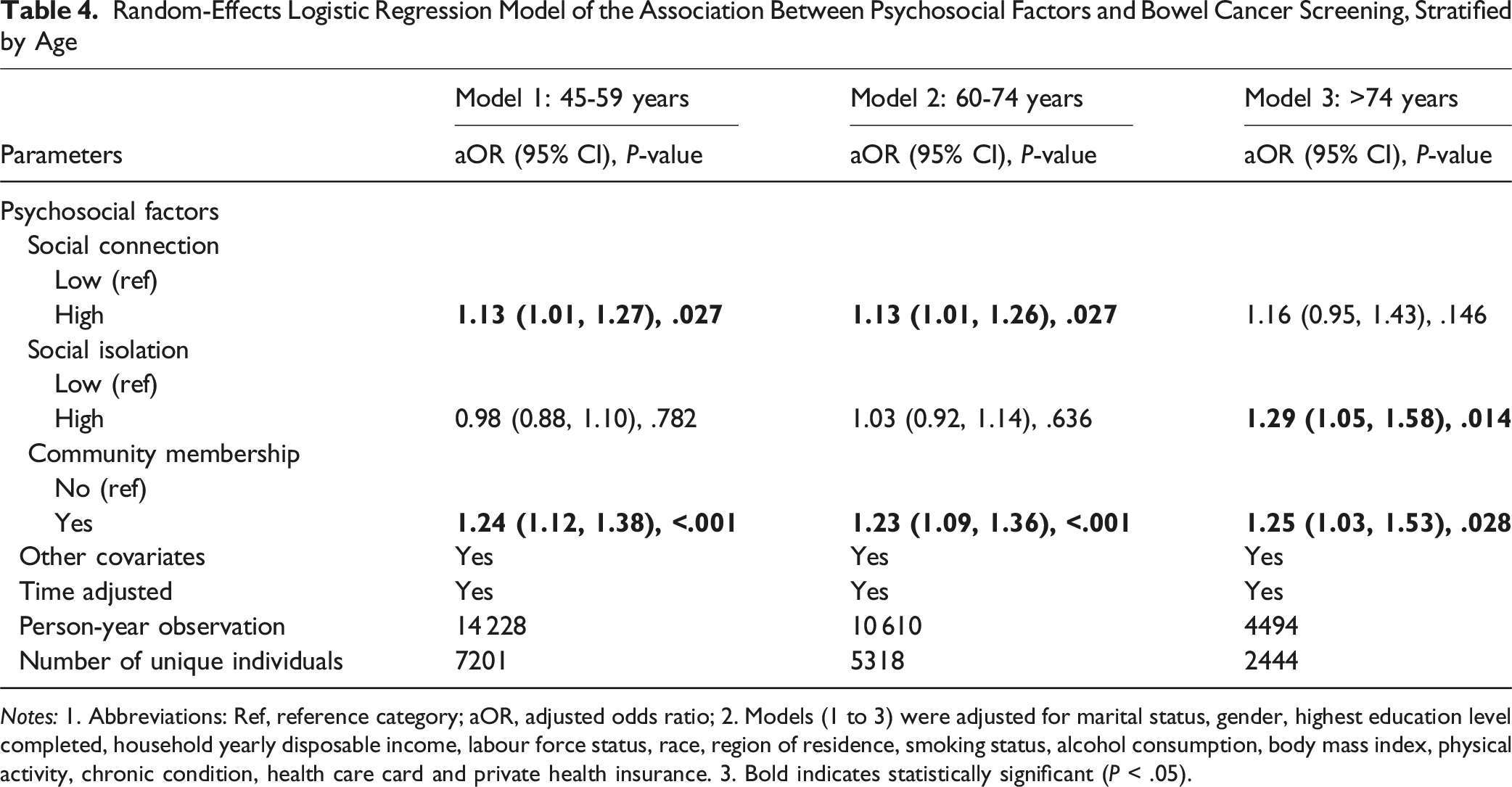
Notes: 1. Abbreviations: Ref, reference category; aOR, adjusted odds ratio; 2. Models (1 to 3) were adjusted for marital status, gender, highest education level completed, household yearly disposable income, labour force status, race, region of residence, smoking status, alcohol consumption, body mass index, physical activity, chronic condition, health care card and private health insurance. 3. Bold indicates statistically significant (P < .05).
Random-Effects Logistic Regression Model of the Association Between Psychosocial Factors and Bowel Cancer Screening, Stratified by Gender

Notes: 1. Abbreviations: Ref, reference category; aOR, adjusted odd ratio; 2. Models (1 to 2) were adjusted for marital status, age, highest education level completed, household yearly disposable income, labour force status, race, region of residence, smoking status, alcohol consumption, body mass index, physical activity, chronic condition, health care card and private health insurance. 3. Bold indicates statistically significant (P < .05).
Discussion
Key Findings
This study aimed to investigate the relationship between psychosocial factors and bowel cancer screening among Australian middle-aged and older adults. We found a statistically significant association between social connections, community membership, and a greater uptake of bowel cancer screening. To examine the potential differences in the relationship between psychosocial factors and bowel cancer screening across various demographic groups, we conducted subgroup analyses by age and gender. Our findings suggest that social connection is a significant predictor of bowel cancer screening uptake among men, while community membership is linked to increased screening rates for both men and women. Furthermore, social connection is statistically significant in its association with bowel cancer screening among Australian adults aged 45 to 59 and those aged 60 to 74 years.
These findings corroborate prior studies demonstrating the relationships between psychosocial factors and participation in bowel cancer screening. Specifically, previous research has shown that high community membership and social connections are positively associated with increased participation in screening programs.7-9,12,15,16,28 Building on the established research, along with the findings of our study, we recommend that strategies to enhance participation in bowel cancer screening programs should include efforts to improve social connections and community membership, ensuring that patients receive optimal care and treatment.7,8
Additionally, our study observed that high social connection and community membership were statistically significant factors positively associated with bowel cancer screening among men across various age groups. 28 Furthermore, these findings align with the existing literature, indicating that gender and age are significant factors in colorectal cancer screening participation. 29 These findings highlight the need for targeted interventions aimed at facilitating social engagement, as having adequate support from friends and family is crucial for fostering confidence and good self-esteem throughout life. 30
Policy Implications of the Study’s Findings
This study provides a clear and actionable message for public health policymakers and clinicians: strategies to increase bowel cancer screening rates should move beyond traditional demographic and socioeconomic factors and actively incorporate psychosocial considerations. Our findings highlight a compelling “so what” for the Australian public health landscape. The findings of our study have substantial implications for public health policies and the implementation of preventive healthcare services. To increase the effectiveness of these initiatives, recommendations are outlined in two key domains: addressing the demand side of public health initiatives for policymakers and the supply side of healthcare providers.
On the demand side, public health interventions should prioritise comprehensive community-based initiatives to increase awareness of and engagement with bowel cancer screening programs. Local health outreach efforts, in conjunction with strategic utilisation of social media platforms, can capitalise on existing social networks and community structures to effectively disseminate information and encourage participation. 31 These initiatives can foster greater community involvement and reduce the stigma or misconceptions surrounding bowel cancer screening, ultimately leading to higher participation rates.
On the supply side, healthcare providers should integrate psychosocial considerations into clinical practice to address the barriers that hinder individuals from participating in screening programs. This integration could involve the routine assessment of social health factors, such as social connections and community membership, to identify individuals at risk of non-participation. Additionally, providers should establish pathways to connect patients with community resources to strengthen social ties and support networks. This approach not only aligns with holistic healthcare models but also addresses the critical determinants of health, thereby improving overall program effectiveness.31,32 These dual approaches highlight the necessity for a synergistic strategy that merges policy-driven community engagement with provider-led individual support to maximise the reach and impact of bowel cancer screening programs.
Strengths and Limitations
Our study has several strengths. Firstly, a key strength of this study is the use of a large, nationally representative sample, which increases the generalisability of the findings and reduces the potential for selection bias. Secondly, to account for individual-level heterogeneity, we employed longitudinal data and random-effects logistic regression models to examine the relationship between psychosocial factors and bowel cancer screening. Random effects models recognise that individuals may differ in their baseline risk or responses to interventions. This allows for more accurate estimates of the average effects of exposure variables and psychosocial factors. Thirdly, to ensure that other factors did not confound the observed association between psychosocial factors and bowel cancer screening, we controlled for a wide range of variables under predisposing characteristics (e.g., age, gender, education), need factors (e.g., BMI, chronic conditions), health-related behavioural characteristics (smoking, alcohol consumption, physical activity), and enabling resources (e.g., income and health insurance). Fourthly, to explore potential heterogeneity in the relationship between psychosocial factors and bowel cancer screening, we conducted subgroup analyses by age and gender.
Our study also has several limitations that need to be mentioned. A potential limitation of this study is the reliance on self-reported data, which may be subject to recall and social desirability biases. Due to the observational nature of the study, it was not possible to definitively establish a causal relationship between psychosocial factors and bowel cancer screening. Further research is needed to confirm causality between psychosocial factors and bowel cancer screening. Another key limitation is the potential underestimation of the true screening participation rate. The NBCSP invites participants biennially, yet our study relied on a 12-month self-report period. Consequently, as many as half of the eligible population may not have received an invitation to screen in the survey year, which could dilute the observed associations.
Conclusion
Although the link between psychosocial factors and cancer screening has been studied in countries such as the US and Mexico, a significant gap remains in understanding these relationships within the Australian context and its unique healthcare system, particularly regarding the National Bowel Cancer Screening Program. Our study aims to fill this critical gap by providing the first longitudinal evidence on this topic based on a nationally representative Australian sample. Our study offers new, longitudinal evidence that high social connections and community membership were significantly linked to higher participation in bowel cancer screening among middle-aged and older adults in Australia. This finding emphasises the crucial role of psychosocial factors in influencing engagement with preventive healthcare programs, especially during the COVID-19 pandemic, which has increased social isolation and related health issues. Social connections and community membership may facilitate health-promoting behaviours, such as bowel cancer screening, by providing emotional support, encouragement, and access to vital health-related information. These elements help individuals overcome screening barriers, including fear, misinformation, and logistical challenges. In light of the disruptions caused by pandemic-related isolation, incorporating social connections and community membership into public health strategies is crucial for increasing screening rates, particularly among populations at risk of underutilising these services.
A strong link between psychosocial factors and bowel cancer screening has significant implications for public health policies and clinical practice. Our study findings emphasise a clear need for public health policies in Australia to go beyond traditional risk factor models and include psychosocial factors, such as strengthening community bonds, to increase participation in the NBCSP. Our results provide solid, contextually relevant evidence for a specific national program and should guide the development of targeted, community-based initiatives. Previous research has demonstrated a correlation between psychosocial factors, including social connections, and increased participation in cancer screening. However, there is still a significant gap in understanding these relationships within the Australian context and its unique healthcare system. This article provides new longitudinal evidence on the association between psychosocial factors and bowel cancer screening within the Australian context. It emphasises that the influence of social connection and community membership was even more pronounced during the COVID-19 pandemic. It also reveals heterogeneous effects, indicating that social connection is a significant predictor for men but not for women. The findings suggest that health promotion should expand to include psychosocial factors, such as social connections and community involvement. In practice, this involves developing community-based initiatives that strengthen social bonds to encourage higher participation in bowel cancer screening. Regarding research, the observational nature of the study indicates that further investigation is necessary to establish the causal link between these factors and screening uptake.So What?
What is Already Known on This Topic?
What Does This Article Add?
What are the Implications for Health Promotion Practice or Research?
Footnotes
Acknowledgements
The authors would like to thank the Melbourne Institute of Applied Economic and Social Research for providing the HILDA dataset. This study uses unit record data from the Household, Income, and Labour Dynamics in Australia Survey (HILDA) conducted by the Australian Government Department of Social Services (DSS). The findings and views reported in this paper, however, are those of the authors and should not be attributed to the Australian Government, DSS, or any of DSS contractors or partners. DOI: 10.26193/OFRKRH, ADA Dataverse, V2.
Ethical Consideration
The HILDA Survey commenced in 2001 and has been conducted annually following the University of Melbourne’s ethical guidelines. The Human Research Ethics Committee of the University of Melbourne has approved this research project. The ethics ID number of the research project (HILDA Survey) is 1647030. The HILDA Survey is conducted under a new human research ethics approval (Project ID 31363, approved February 2025) received from The University of Melbourne. This paper uses unit record data from the HILDA conducted by the Australian Government Department of Social Services (DSS). This study did not require ethical approval as the analysis used only de-identified existing unit record data from the HILDA Survey.
Consent to Participate
Informed consent to participate in the HILDA Survey was gained through the use of an information letter to all potential respondents. This letter described the voluntary nature of participation in The Survey and outlined that informed consent would be implied when participants agreed to be interviewed. Further, more detailed information about the purposes of the HILDA was sent after the interview to Wave 1 respondents (and any new sample members at later waves), along with further information about the way the data are being held, what is being done with the data, and how individuals can, on request (but after undergoing a range of security checks), access that information.
Author Contributors
SAK, NFS, ASB initiated the study, and conducted the data analysis. SAK, NFS, NB, CO, and ASB drafted the manuscript. NFS, NB, and CO offered advice, critical comments and edited the draft manuscript. All the authors read and approved the final manuscript.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Declaration of conflicting interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Data Availability Statement
There are two versions of the HILDA data: the General Release and the Restricted Release. This study utilised restricted release data from the Household, Income and Labour Dynamics in Australia (HILDA) Survey. Funded by the Australian Government Department of Social Services (DSS), the Survey is managed by the Melbourne Institute of Applied Economic and Social Research at the University of Melbourne. Access to the complete HILDA dataset is limited and requires specific approval as it contains sensitive personal information. To apply for access to any of the DSS Longitudinal Studies datasets, first, all applicants and collaborators who need to view unit record data must complete and sign a once only Confidentiality Deed Poll and email the scanned, signed copy to DSS (![]() .
.
Declaration of AI assistance
The authors acknowledge the use of Gemini 2.5 Pro (![]() ) and Grammarly to enhance the academic language and readability of this manuscript. On 4 June 2025, the corresponding author used the prompt, “Improve the academic tone and accuracy of language, including grammatical structures, punctuation and vocabulary,” with Gemini 2.5 Pro. The output was subsequently revised by the authors to align with our intended meaning and style. Grammarly was used for a final proofreading check. The authors retained full responsibility for the final content of this paper.
) and Grammarly to enhance the academic language and readability of this manuscript. On 4 June 2025, the corresponding author used the prompt, “Improve the academic tone and accuracy of language, including grammatical structures, punctuation and vocabulary,” with Gemini 2.5 Pro. The output was subsequently revised by the authors to align with our intended meaning and style. Grammarly was used for a final proofreading check. The authors retained full responsibility for the final content of this paper.
