Abstract
Sexual harassment and gendered discrimination in the workplace are global issues that can affect anyone regardless of their age, gender, job title, or field of employment. The medical field is also relevantly concerned, yet effective prevention measures are scarce. The purpose of this study was to explore preventive options for sexual harassment in an academic medical context from the employees’ perspective and to develop transferable strategies. We conducted semi-structured interviews with 15 female physicians and 15 female nurses working at a tertiary referral center in Berlin, Germany, in the months of April to November 2015. The one-on-one interviews addressed the perception of sexual harassment and available and desirable preventive measures. Data were analyzed by qualitative content analysis. The participants outlined preventive measures at two levels: individual and institutional. Individual options included personal safety measures and individual protection strategies against patients, peers, and superiors. Institutional strategies included guidelines and workplace policies, structured complaint and reporting procedures, formal training options, and organizational development and leadership strategies. The current study highlights how the prevention of sexual harassment hinges on a combination of individualized and system-wide measures to capture the personal as well as the organizational dimension of sexual harassment. Only a concerted effort addressing both aspects will sensitize the workforce, support the victims, and prevent sexual harassment in medical institutions.
Introduction
Sexual harassment and gender discrimination in the workplace are global societal issues that affect people regardless of their age, gender, job title, or field of employment (DeSouza & Solberg, 2003; Fundamental Rights Agency [FRA], 2014; Strub, 2008). Harassment can range from being subjected to unwanted and unrequested sexualized behavior to being a victim of threatening or aggressive actions (Antidiskriminierungsstelle des Bundes [ADB], 2015a; Fitzgerald et al., 1997; Gelfand et al., 1995; Latcheva, 2017; McDonald, 2012).
Studies of sexual harassment and violence around the world identified high rates of sexual harassment among health care professionals (Cheung et al., 2017; Fallahi Khoshknab et al., 2015; Wang et al., 2012; Wu et al., 2012). Forms of harassment range from verbal attacks to unwanted attention to physical attacks. Perpetrators in the medical workplace can be patients and their relatives, colleagues, and superiors, as well as administrative staff. According to the international literature, those most at risk are female doctors (Bruce et al., 2015; Carr et al., 2000; Crebbin et al., 2015; Jagsi et al., 2016) and female nursing staff (Cogin & Fish, 2009; Magnavita & Heponiemi, 2011; M. B. D. Nielsen et al., 2017; Spector et al., 2014). The latter appear to be the most significantly affected group by various forms of verbal aggression and violence (Mai et al., 2015; Schnapp et al., 2016; Shafran-Tikva et al., 2017; Vorderwülbecke et al., 2015).
Sexual harassment has several dimensions. It is a health issue (Chan et al., 2008; Fitzgerald et al., 1994; M. B. Nielsen & Einarsen, 2012; Rospenda et al., 2009) that can lead to a range of psychosomatic symptoms such as chronic back pain, neck pain and headache, chronic gastrointestinal pain, cardiovascular symptoms, as well as anxiety disorder and depression (Harned & Fitzgerald, 2002; Mamaru et al., 2015; Rospenda et al., 2009; Stock & Tissot, 2012; Thurston et al., 2019). Second, sexual harassment has a structural dimension. It can weaken the capacity to work as a team and negatively impact the general work environment (Magnavita & Heponiemi, 2011; Malik et al., 2014; Raver & Gelfand, 2005; Willness et al., 2007). Over time, the waning commitment and lack of trust in the organization can lead to a decline in productivity and innovation. Third, it has an economic dimension due to incurring medical costs and loss of productivity (Fitzgerald et al., 1997; Lapierre et al., 2005; Merkin, 2008; Sims et al., 2005). Last, it has a public dimension in the form of tainting an organization’s reputation with all the associated consequences.
Both international and domestic studies point toward a need for protective and preventive measures against sexual harassment in the workplace (ADB, 2015b; Fitzgerald et al., 1994; Joubert et al., 2011; McDonald et al., 2015). Although the European Union (EU) commission requested member states to prevent and proactively engage with sexual harassment in the workplace in the year 2002/2006 (EU Commission & Parliament, 2002; Latcheva, 2017; Zippel, 2009), these recommendations were enforced in the member states to varying degrees. In Germany, the equal opportunity law (AGG—“Allgemeines Gleichbehandlungsgesetz”) from the year 2006 enforces the employer’s and supervisor’s duty of protection toward employees and recommends a proactive approach (ADB, 2015a). The AGG, however, is not specifically targeted at sexual harassment, but at all forms of discrimination in the workplace. Organizations are encouraged to institute an official AGG complaints office; yet, the law does not specify how the structural management of complaints has to be enacted. Furthermore, even with a legal framework in place, actions in the workplace to reduce the taboo and stigma of sexual harassment and proactively engage in prevention remain rare. Preventive measures need to be adjusted to the specific work environment, as harassment might appear in different forms depending on the work culture of the organization. In the present study, we explored the array of different personal and institutional preventive measures known to hospital staff. We assume that preventive measures against sexual harassment will be more effective if they are adapted to the organizational context and that this needs to be taken into account during their development. Thus, while considering the specifics of our organization, we sought to identify options that could be successfully transferred to other settings.
Method
Aim
The purpose of this study was to explore the breadth of preventive options for sexual harassment in the academic medical context from the employees’ perspective.
Setting
Charité–Universitätsmedizin is one of the largest medical faculties in Europe. At the time of the project, it had around 11,000 employees, of whom around 1,600 were physicians and around 3,200 nurses. The faculty is composed of several hospitals throughout the city, and with its 17 centers, it covers all clinical and surgical specialties. The medical center has been home to a violence prevention clinic and a network of specialized practitioners for a decade. The subject of their work is, however, the identification and prevention of domestic violence, not sexual harassment. The target population for these activities are patients, not employees of the hospital. The current project was the first investigation of sexual harassment within the institution. The qualitative study presented in this manuscript was one of three subprojects within the larger WPP (watch–protect–prevent) study. WPP included one quantitative subproject aimed at identifying prevalence of sexual harassment (Jenner et al., 2019), one structural subproject directed at exploring legal options for prevention, that is, workplace policies (Oertelt-Prigione & Jenner, 2017), and the present subproject directed at the participatory exploration of preventive options. The aim of the subproject was twofold: the exploration of transferrable protective measures and the development of a catalog of tailored interventions for our institution. As the organizational setting has a significant impact on the development of preventive measures, qualitative interviews exploring the institutional knowledge of various stakeholders represented the best option to acquire the analytical depth needed.
Study Design
The study consisted of qualitative semi-structured interviews with physicians and nurses working at Charité–Universitätsmedizin. Ethics approval (EA1/350/14, December 15, 2014) and approval by the three employee representations/staff councils (clinical, academic, and general) was obtained.
Sampling and Recruitment
Initially, we planned to include women and men in equal numbers in the current study but throughout the recruiting process, it became clear that male colleagues were very reluctant to participate in interviews on the topic of sexual harassment. As participation was voluntary and quality of data depends on willingness to share, we decided to focus on female employees only. Moreover, as women are significantly more affected by severe forms of sexual harassment in general and in our institutions’ sample (Jenner et al., 2019), their perspectives on prevention appear worthy of in-depth exploration. We focused on individuals active in the field of care and proceeded with recruiting 15 nurses and 15 physicians of different ages and with different degrees of experience. To recruit participants, an extensive information campaign about the study was conducted which included the following strategies: (a) an official invitation signed by the medical director to all department heads to encourage participation of their employees, (b) a feature of the study and its objectives in internal media (intranet, newsletters, etc.), (c) a project website with study-specific and general information as well as support materials, (d) a direct email to all physicians working in the hospital, (e) a visual advertising campaign, and (f) direct presentations at department meetings and grand rounds. Employees were addressed by personal mail and invited to participate through contacting the study coordinator.
The initial intention to recruit participants in equal numbers from different fields of medicine proved difficult due to the general reluctance to participate in individual interviews; hence, next to spontaneous recruiting, snowballing was also used to identify potential participants. These were approached personally and informed about the study and its aims and given time for opting in. If the study team received no feedback, no further attempt at recruitment was made.
Data Collection
We conducted one-on-one semi-structured interviews on the perception of sexual harassment and possible preventive measures in the months of April to November 2015. The questions were developed to integrate the findings from our quantitative survey on incidences of sexual harassment. Questions were open-ended and designed for maximum inclusiveness of different disciplinary backgrounds. The interviews were conducted face-to-face and audio recorded. Notes were also taken by the interviewer. All interviews were conducted by the same interviewer (S.J.) to minimize inter-researcher variability. Interviews were anonymized, transcribed by an external provider bound to professional secrecy, and returned for analysis. All participants were female. We did not collect any personal identifying information beyond the recruitment process; hence, all information on age, seniority, and field of work cannot be reconnected to the interviewees. The only information registered was whether the participant was a physician or a nurse. To ease reading, all interview quotes were translated into English.
Data Analysis: Choice of Methodology
For the research methodology, we have applied content structuring qualitative analysis, a variant of the qualitative content analytical procedure developed by Philipp Mayring (2015, 2016). Content categories or the category system represent the central defining feature of the analytical methodology (Mayring, 2016). M. Schreier defines the category system as a systematic structuring of text material into primary and subcategories. Content structuring analysis is systematic and rule-based, which increases its validity and reliability (Mayring, 2016). Intercoder reliability is secured through independent coding by two or more researchers. Results are then compared, reflected, discussed, and consistent results secured.
Data Analysis: Process
We applied the content structuring qualitative analysis. Briefly, two members of the team (S.J. and P.D.) analyzed the text by applying the following steps: familiarizing with the material, derivation of upper categories from the interview guideline, and marking of passages that contain a statement about the primary categories. After the consensus was reached, the primary analyst (S.J.) proceeded with the analysis of all transcripts. The text was analyzed in iterating rounds of paraphrasing and generalizing. Specifically, relevant text passages were identified and paraphrased, that is, rewritten in such a way that only a brief, content-limited statement remains. At the end of this step, many paraphrases emerge as “generalizations.” These generalizations substantially overlap in their content. The redundant paraphrases are then deleted or summarized in the next step—the reduction (Appendix 1 in Supplementary Material 2). After revision and further reduction, the subcategory system was defined (Appendix 2 in Supplementary Material 3). Written memos and annotations were recorded for the development of the coding and subcoding system using MAXQDA software (VERBI Software GmbH, Berlin, Germany). This facilitated the identification of exemplary text passages (“anchor examples”) and structuring of the text (Appendix 3 in Supplementary Material 4). As a final step, the third analyst (S.O.-P.) reviewed all anchor examples, codes, paraphrases, and subcodes, to identify potential incongruences.
Results
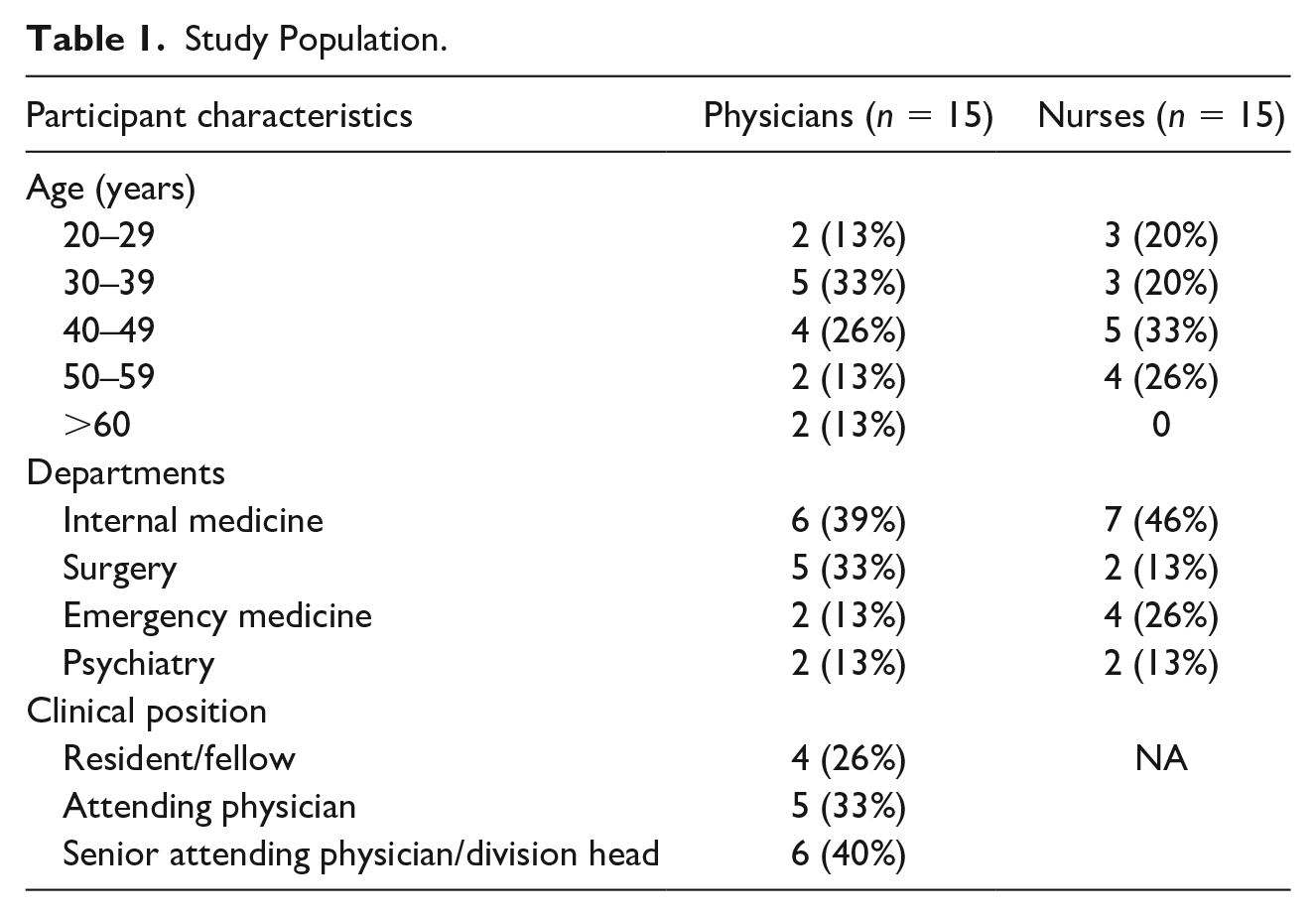
We interviewed 30 female employees, 15 physicians, and 15 nurses (Table 1). We aimed at the inclusion of different departments and disciplines to take different cultures into account. We included both emergency medicine and psychiatry as these are two high-risk fields given the nature of the patients’ illnesses. Seniority was also equally represented in the medical field as hierarchy and agency might be significantly correlated.
Study Population.
The participants described preventive measures at two levels: individual options and institutional interventions. Prevention can be executed at the individual level, in the form of behaviors, and actions that can be learned and implemented autonomously (Tables in Supplementary Material 2–4). Institutional interventions are powerful tools that can achieve cultural change; however, they depend on the participation and support of multiple stakeholders. Institutional interventions always require some form of compromise and sponsorship and usually take more time to be implemented. A combination of structural factors with individual options appears as the most effective way to combine immediate agency with long-term change. The development of the single categories is detailed in Supplementary Materials 2 to 4 of this manuscript. In the following description, we proceed from individual safety measures to measures that can be implemented at the team level, with peers and superiors. We then move to the institutional options, starting with the need of a guideline or workplace policy, and then moving down the hierarchy. We first address the need for leadership commitment at different levels and then proceed to discuss how information campaigns and trainings for all employees could be developed. Last, we address how sexual harassment and discrimination are phenomena embedded in a larger context of gender inequality and discrimination and how targeting these aspects could reduce incidences of harassment.
Individual Preventive Measures
Subjective safety protection
Doctors and nurses identify different individual strategies to protect themselves in threatening situations. Nonverbal communication and behavioral cues are commonly used, as well as simple and direct requests to stop a certain type of behavior. All participants clearly stated that certain behaviors are not tolerated and should not be normalized in the professional context.
I make it clear at an early stage using facial expressions and gestures that there is a shield here, nothing will penetrate it—I verbally clarify that you’d better not attack me. (Interview doctor, 12) In situations where someone is crossing a line I make my boundaries very clear: stop! Enough! That’s not how I want you to communicate with me! (Interview nurse, 4) Nurses are more likely to be targeted by patient abuse, white coats are protective. The more dominant and defensive she appears, the less likely a woman will become a victim. Clear, clear boundaries must be set immediately. (Interview doctor, 6) To protect myself I set clear limits, first of all with facial expressions and gestures, I distance myself and convey that I do not tolerate contact in this way. If necessary I verbalize this and say stop, I will not communicate with you. (Interview doctor, 7) This is not part of the job description, that you have to feel harassed, or that you are sexually attacked, but . . . you can deal with it self-confidently, you can set a clear stop signal and you should deal with it openly. This is what I think, this is something that needs to established. (Interview nurse, 4)
General de-escalation techniques developed in conflict management training are also addressed. Identifying oneself as a representative of the medical profession overall allows them to maintain emotional distance. The aggressive outbursts and verbal attacks are reframed as general feelings toward the institution or toward a particular medical situation and not as a personal matter.
I see myself purely . . . as a representative of the institution and the patient is acting out, but it’s not aimed at you personally. I shake off comments and deal with the situation quite well. (Interview nurse, 4) In the de-escalation training we were able to find a common language across all occupations, how to deal with attacks. (Interview doctor, 1)
Nursing staff, who are exposed to more direct physical contact with patients, emphasize how a clear definition of their role is helpful in establishing boundaries. This also includes verbalizing the fact that they are not to be perceived as an object of sexual attention.
What can work well is to clarify what your role actually is—you are not an object of lust, but are working in a professional, in a therapeutic capacity. (Interview nurse, 4) When it comes to patients I usually say something like “not like that” or “Stop! That’s going too far—that’s below the belt.” Sometimes people are really shocked, especially patients, by the reaction that I have [..] But you have to clearly say stop, so I do. (Interview nurse, 4)
If other strategies prove unsuccessful, ignoring patients, especially those that are cognitively impaired or under the influence is a common option. If the situation escalates, asking for help from a second, possibly male, colleague was advised.
Individual protection against harassment from peers and superiors
Physicians and nurses describe various methods of engaging with inappropriate behavior by colleagues and senior staff. Alliances between female colleagues who can trust each other are named as one form of self-protection, particularly in the case of sexual harassment.
Withdrawal or ignoring the attention is a first resort solution. This applies particularly when peers or personnel at different levels of the institutional hierarchy are involved, such as doctors in the case of nurses.
When it comes to my colleagues I don’t stoop to their level. Instead, I take a deep breath, step out of the situation for a moment, calm down and then talk about the situation privately so that I can retaliate when I have the opportunity. (Interview doctor, 4) Then I just distance myself from it. I don’t have a problem with that either, I mean he should say what he wants, after eight hours I’m out of here. [..] And if it’s really enough for me, then I make it verbally clear. I say: “So now stop it. We don’t know each other, we’re not friends and we don’t have to become friends but we’re in a professional working situation and everyone should treat each other respectfully.” (Interview nurse, 3)
When peers are involved the second step is direct confrontation of the person perpetrating the offensive or harassing behavior.
After the first incident I talk to the colleague as soon as possible and express my outrage, making it clear that behavior of that kind is completely out of order. (Interview doctor, 2)
In the case of superiors, a leadership figure is frequently involved to act as mediator on behalf of those affected. This was reported by both nurses and physicians. Leadership figures can have a protective role while also acting as role models. They can not only demonstrate how to engage directly with a toxic situation but also demonstrate protective and respectful leadership behavior. Trust is an essential component in this.
In one case, where one of our colleagues could no longer be tolerated, we went to the attending together and made it clear that it could not go on like this. And this led to, among other things, the contract of this man not being extended. (Interview doctor, 6) We’re very lucky with our head of department—she has a good overview of gender-specific issues. If things get really bad, we know we can go to her because we trust her. (Interview doctor, 1) That’s also a small additional protective measure for me to be able to go to my boss. This overly poisonous situation happened and I was worried about how to behave. (Interview nurse, 12)
One female doctor referred to the impact of private coaching that gave her professional tools with which to engage with gender-specific interaction on male dominated university panels.
I use skills from private coaching on power and communication to increase my presence in male dominated situations. Exercises around body language, how I present myself, self-awareness and awareness of others have helped me to identify and engage with gender specific behavior. (Interview doctor, 3)
The outlined strategies represent a wide range of potential actions, from the individual verbal and nonverbal protection, to the intercession of peers and mediators. Individual actions can be learned on the job or through professional coaching, thus, in a structured or unstructured manner. Significantly, nurses most frequently reported learning these strategies while on the job, emphasizing how coping strategies are an essential professional asset needed to perform their work. This applies to a lesser degree to the experiences of the interviewed physicians. Professional hierarchy might increase the risk for harassment in some context, but according to the interviewees, it also represents a powerful distancing tool against patients unwilling to respect professional boundaries. The inclusion of teammates or supervisors demonstrates the importance of bystanders as allies and their role in validating personal experiences and providing active support. The role of the team as protection from physical forms of harassment is particularly important for the nurses, who have more physical contact with patients and are exposed more frequently to physical harassment.
Institutional Preventive Measures
Guidelines against sexual harassment
A workplace policy for prevention is an opportunity for the hospital leadership to clarify and formalize expectations toward employees and contractors, patients, and relatives. All employees including external contractors should have access to the information about rights and obligations defined in the code of conduct. This should be formalized in the employment contract. Both occupational groups stress the need of guidelines for all employees and the need to make these universally known within the organization.
Guidelines surrounding procedures in the case of sexual harassment are important, to show that the business takes the issue seriously and that everyone knows which steps are taken after an incident. (Interview nurse, 11) Then I would publish a public statement in the first place on the intranet that tabooed topics like sexual harassment can be addressed and this is a way to establish a low-discrimination culture and a change in values. (Interview doctor, 13)
Clear guidelines for patients, like codes of conduct, are also mentioned. This is of particular importance to nursing staff, who feel more vulnerable and exposed to attacks from patients and relatives. Staff expect protection from management and clear guidelines for action in case of repeated unacceptable behavior. The difficulty of acting on patients’ abuse is also expressed.
Nursing care is at the front line and yet if a situation gets precarious we have hardly any protection. . . . I feel like we’re on our own and there’s no one supporting us. Everyone seems to avoid the topic of reprimanding patients and relatives or banning them altogether. (Interview nurse, 1) When patients or relatives are aggressive, threatening or sexually abusive, we can always call our head of department who will call for it to stop. In cases like this, people should actually be banned from the clinic, but no one is brave enough to do that. (Interview nurse, 2)
Leadership commitment
A public statement by the executive board is important in a hierarchical system and can contribute to engendering a shift in values and work culture. Interviewees from both professions believe that issuing a public statement regarding a “zero tolerance attitude” toward sexual harassment would be a significant step. A statement by the board has an impact on multiple levels; it shows openness to addressing taboo topics, raises awareness, and places the issue at the decision-making level.
A culture of political correctness is communicated from the top down, with the management committee and senior management acting as role models. Discrimination is not accepted. Politically correct behavior starts at the top, with the management and senior staff. (Interview doctor, 1) We have extensive specialist-case meetings, but there is no room for anything outside of this. Certain taboo and soft skills topics should be fundamentally integrated into the meetings as they play an important role in our socio-communicative qualifications for our profession and can help decrease conflicts within teams. (Interview doctor, 8)
The formal commitment can strengthen self-esteem among victims, encouraging them to defend themselves in these kinds of incidents and to report them. For the potential perpetrator, it also signals possible consequences. To translate such a commitment into practice, all employees need to be adequately informed. Information about policies and procedures should, thus, be accessible to all employees and known to everyone in the organization.
All (new) employees should be made aware of a transparent procedure in the case of an incident. . . . This is made possible if everyone has been adequately informed on the issue and its consequences. (Interview doctor, 7)
Senior positions
Both nursing staff and doctors emphasize the significant role that senior staff play as role models. Senior staff have a responsibility to promote a fair institutional culture. They should be able to recognize sexual harassment and discrimination, to actively intervene and to take the necessary steps to manage it. Some senior staff mentioned their awareness although they remain isolated examples.
It is senior staff that create a team culture that should be supportive and transparent, with clear boundaries. . . . As a boss, I have an open door and open eyes policy and try to initiate rituals that allow us to work together in the correct way, for example through supporting my colleague’s results and performance and of course by being a role-model myself when it comes to this topic. (Interview doctor, 12)
In a senior position, it also becomes clear that responsibility is held toward both victims and perpetrators. The latter should be held accountable and nudged into behavioral change. Teams should also appoint selected members as contact points in case of harassment. Many service responsibilities are delegated within teams and safety and counsel should be one of them.
I speak directly to the perpetrator and tell them very clearly that sexual harassment is completely unacceptable. I expect them to reflect on their behavior and change it. In our team meetings the case is talked about anonymously and evaluated. (Interview doctor, 13) Perhaps the head nurse should bring up the topic once a year in our meetings, to remind people of it—like “hey! If something happens, come to me!” Or name particular people in the team who are solely responsible for taboo topics. That would help make the issue more serious. We have people appointed for every other technical process but nobody when it comes to interpersonal matters. (Interview nurse, 12)
Information on complaint procedures and reporting
Clear indication of instances for reporting of incidents as well as clearly defined complaint procedures are of extreme relevance. This information should be readily available on the intranet. Employees should also be made aware that consultation does not necessarily lead to a formal complaint procedure.
All employees should know where they can turn in the case of sexual harassment. A notice could be placed in the showcase in the wards or on the first page on the intranet. (Interview nurse, 11) For me it would be important that for all groups of employees it is recognizable that when situations of abuse occur, and they do not have to be sexual, but they can also be abuse in the sense of superior misbehavior, they can be located in the area of bullying, that everyone is aware that the company offers a trustworthy place where one can make this a subject of discussion. (Interview doctor 12)
To facilitate support and advice, counseling offers should be easy to access. In addition to in-person options, anonymous options should also be considered. Suggestions include a centralized anonymous system (similar to the critical incident reporting systems [CIRS]), an informal hotline, or a whistleblower program to highlight taboo and discrimination issues. These options are considered especially relevant given the possible career-altering consequences of a formal complaint procedure.
Many people don’t really know what they should do, especially if their boss isn’t doing anything about it. We’re working in a hierarchical system in which complaints can have unforeseeable consequences. (Interview doctor, 8) I would actually create both anonymous, i.e. public information or advice or simply contact points where you can actually call anonymously and get informed. Maybe a bit like CIRS, there’s this system, that’s actually documenting things like that in order to get insights. (Interview doctor, 13)
Training
In the context of informing all employees, trainings have an important role. Mandatory trainings for superiors and voluntary training for junior staff are mentioned by both occupational groups. Nursing staff place emphasis on training in an interdisciplinary setting. Due to time constraints, female doctors suggest short and focused presentations on the topic within team meetings.
Short trainings on sexual harassment and soft skills should be integrated into the Journal Club, and clinic conferences. Senior staff responsible for personnel should be mandated to attend compulsory trainings around duty of care and how to deal with issues of sexual harassment. (Interview doctor, 10) I’d promote advanced trainings. Because you get shown a simple way, how can I behave and what may or must I allow, what can I allow? And what do I do to avoid having to put up with this at all! (Interview nurse, 5)
The trainings in methods of de-escalation that are mandatory for staff in high-risk environments, such as the ER or psychiatry wards, are mentioned as protective measures by both professions. Within the trainings, an example of a sexual harassment is employed and protective strategies are practiced. This format combined a self-protection training and the opportunity to honestly discuss personal experiences.
Sexual harassment was also mentioned in the de-escalation training. . . . The training allowed us, as an interdisciplinary team, to find a common language . . . For me it was also the first time that I had the chance to talk about my helplessness in those kinds of difficult patient situations. (Interview doctor, 1)
Organizational development
Sexual harassment can be facilitated or prevented by organizational factors. For example, staff shortage and unclear work schedules generate high pressure, stress, and uncertainty. Addressing these factors could decrease the general risk of discrimination, harassment, and inappropriate behavior.
Well one of the biggest problems we have is how we plan our work. It can be a really serious problem. . . . Our complaints regarding work schedules and organization are just not taken on board by the senior doctors and by management. (Interview nurse, 9)
Measures to strengthen gender equality, particularly in departments dominated by men are also mentioned as a long-term strategy to protect against sexual harassment.
Ensuring equal numbers of men and women within all commissions and boards in the faculty is an important step towards gender equality. In order to actively drive women towards senior positions, a reward-punishment system should be introduced by the top level management. (Interview doctor, 13) Promoting women as a management strategy! Introduce reward incentive schemes, or make contracts for women permanent until there is gender parity at this level. Senior level positions and qualifications towards consultancy positions should also be made possible at a part time level. This would all be a start in giving women with children or single parents the opportunity to advance their career. (Interview doctor, 14)
The most impactful measure at organizational level appears to be a guideline or workplace policy that lays out the legal framework for the management of incidents. Furthermore, the support by leadership, at the board, department, and team level, is essential to implement the interventions detailed in the guideline and provide support to victims. A lack of information about rights, policies, and counseling services is perceived as a major problem, which should be adequately addressed through information campaigns and formal inclusion of the guideline content in training. Doctors and nurses mentioned all these aspects in equal measure. Last, sexual harassment does not represent an isolated incident, but is rooted in an organizational culture, which provides impunity to perpetrators. One opportunity to disrupt this mechanism could be gender equity in leadership and formal interventions against gender discrimination, which is structurally connected to harassment.
Discussion
To the best of our knowledge, this is the first study addressing the development of preventive measures against sexual harassment in academic medicine from an employee perspective. The results clearly point toward two areas of prevention, personal and organizational (Table 2). The challenge lies in the need to combine highly tailored interventions for personal prevention with broad system-wide organizational measures.
Sexual Harassment Protection and Prevention Measures.
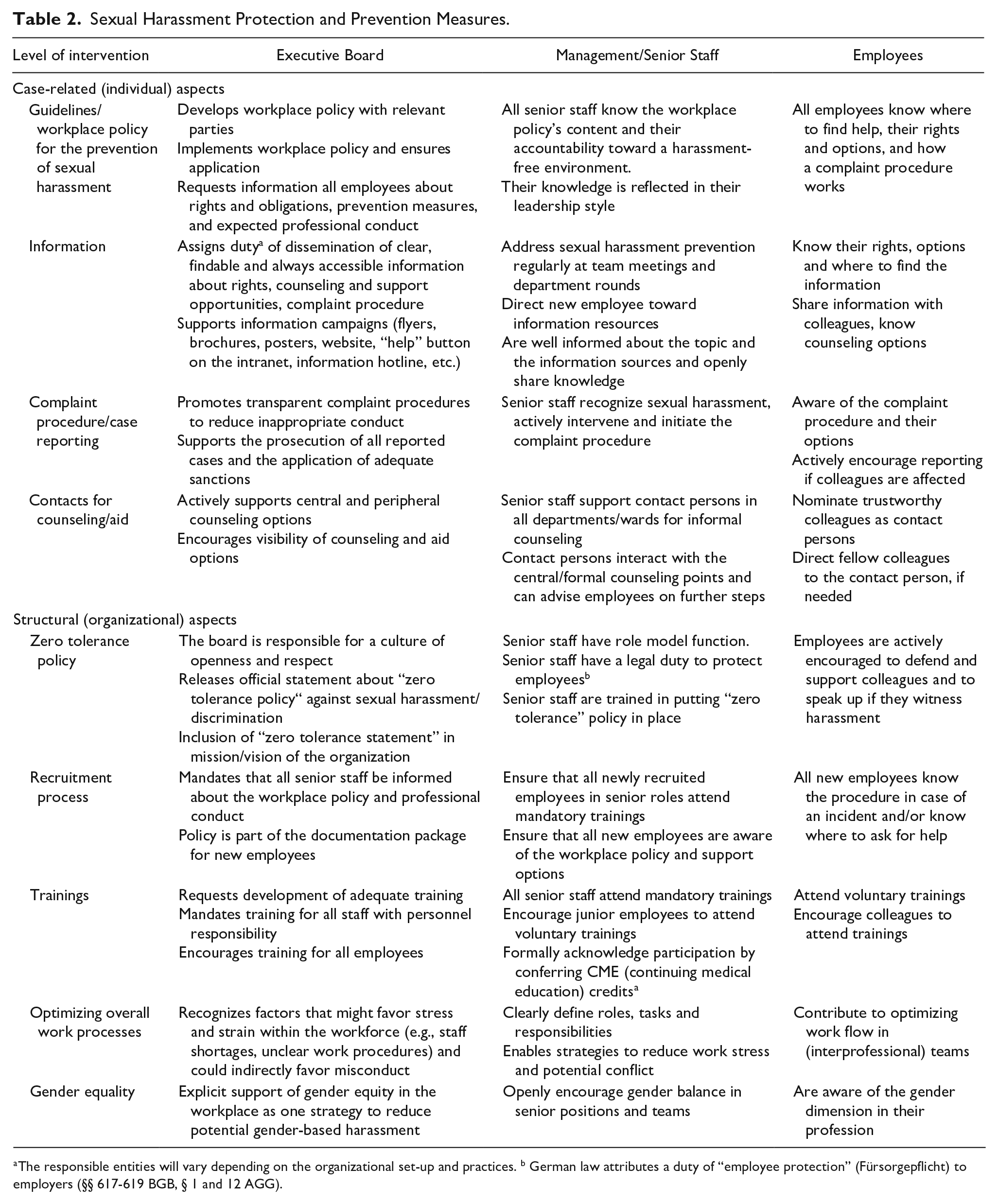
The responsible entities will vary depending on the organizational set-up and practices. b German law attributes a duty of “employee protection” (Fürsorgepflicht) to employers (§§ 617-619 BGB, § 1 and 12 AGG).
Sexual harassment is a phenomenon that is perceived at the personal level and several of the suggested prevention strategies emphasize this personal dimension. Perception and reaction to sexual harassment vary greatly (Hinze, 2004; McLaughlin et al., 2012; Stratton et al., 2005; Wear & Aultman, 2005), depending on agency, experience, and personality, yet the need for physical and emotional distancing represents a generalized first step. The ability to distance oneself, emotionally and physically, is, however, limited by the impact of power dynamics. Specifically, protection options toward a violent patient are much more immediate and actionable than distancing from a harassing colleague that one shares regular shifts with. Emotional distancing requires further steps, which frequently cannot be taken by the victim alone. Support from colleagues, bystanders, and superiors play an essential role. This is even more relevant if superiors themselves are the perpetrators. In this case, mediation by a third party becomes essential in supporting face-to-face communication, if this is an option. Overall, preventive measures at the personal level are highly individualized interventions that need to be tailored according to the characteristics of the victim, the perpetrator, and the power dynamics in their relationship. This represents a logistic challenge and emphasizes the need for expert counseling.
Organizational prevention, however, hinges on broad actions to reach the largest possible audience and on the establishment of general protective mechanisms. The initial step organizations should be taking is the removal of the taboo around sexual harassment itself. Sexual harassment is a ubiquitous phenomenon (FRA, 2014; McDonald, 2012; Quick & McFadyen, 2017; Rosenthal et al., 2016) and its incidence does not decrease if it is not explicitly addressed. On the contrary, the first step for system-wide preventive action is the acknowledgment of its existence (Feltes et al., 2012; Meloni & Austin, 2011; Stockdale et al., 2004; Walsh & Gates, 2018). Removing the taboo around sexual harassment will encourage an organization-wide discussion about the subject. Communication should be open and interdisciplinary to support proactive action. Next, the responsibility of supervisors, leaders, and board members to condemn harassment and protect employees needs to be emphasized to encourage a culture of trust (Dougherty & Smythe, 2004; Johnson et al., 2018; Mathews & Bismark, 2015; Vijayasiri, 2008). Individuals in a position of leadership are role models and have a legal and professional duty of care toward employees. Leaders need to be aware of their role and their responsibilities. Mandatory trainings for all staff and ad hoc offers for single departments or institutes should be implemented to guarantee adequate knowledge of the internal policies. Many employees refrain from seeking advice out of fear and lack of knowledge about the process. Barriers toward seeking help should be minimized and complaint procedures need to be transparent and consultation easily accessible. Overall, employees wish for an organization to display a clear and unmistakable commitment.
Our interviews highlighted the need for complex interventions that take into account the personal and systemic dimension of sexual harassment. Although the experience of the victim is always individualized, the conditions that lead to an incident are rooted in organizational culture. Thus, a comprehensive approach to the prevention of sexual harassment needs to offer individualized support, while promoting a safe, open, and accountable organizational culture at all levels.
Although our study highlighted a vast and transferrable range of preventive measures, the information was gathered at a single institution in an urban setting. Overall, the willingness to discuss the topic was limited among male participants, which did not allow us to gather their perspectives and which highlights the stigma associated with the phenomenon. Furthermore, the intersectional factors associated with working in a stereotypically “female” profession for male nurses and the potential consequences this might have on harassment experiences could not be gathered. A lack of male perspective is also a potential limit for the development of preventive measures that are universally accepted. Although the city of Berlin is relatively diverse for European standards, the majority of health care workers in our institution are Caucasian and mostly of German descent. We did include some participants with an immigrant (mostly Turkish) background, and although this is representative of the country’s reality, it does not represent the experiences of people of color. Participants in the study might have been particularly motivated to engage with the topic and, hence, reflect a specific subgroup. However, with this study, we were not trying to capture a representative picture of harassment experiences, but an array of generalized prevention measures. Hence, their higher engagement might have contributed to the richness of the data.
Conclusion
The current study highlights how the prevention of sexual harassment hinges on a combination of highly individualized and broad system-wide measures. This is needed to capture both the personal and the organizational dimension of the phenomenon (Table 2). Only a concerted effort addressing both aspects will sensitize the workforce, support the victims, and prevent sexual harassment in medical institutions.
Supplemental Material
sj-pdf-1-jiv-10.1177_0886260520903130 – Supplemental material for Prevention Strategies for Sexual Harassment in Academic Medicine: A Qualitative Study
Supplemental material, sj-pdf-1-jiv-10.1177_0886260520903130 for Prevention Strategies for Sexual Harassment in Academic Medicine: A Qualitative Study by Sabine C. Jenner, Pia Djermester and Sabine Oertelt-Prigione in Journal of Interpersonal Violence
Supplemental Material
sj-pdf-2-jiv-10.1177_0886260520903130 – Supplemental material for Prevention Strategies for Sexual Harassment in Academic Medicine: A Qualitative Study
Supplemental material, sj-pdf-2-jiv-10.1177_0886260520903130 for Prevention Strategies for Sexual Harassment in Academic Medicine: A Qualitative Study by Sabine C. Jenner, Pia Djermester and Sabine Oertelt-Prigione in Journal of Interpersonal Violence
Supplemental Material
sj-pdf-3-jiv-10.1177_0886260520903130 – Supplemental material for Prevention Strategies for Sexual Harassment in Academic Medicine: A Qualitative Study
Supplemental material, sj-pdf-3-jiv-10.1177_0886260520903130 for Prevention Strategies for Sexual Harassment in Academic Medicine: A Qualitative Study by Sabine C. Jenner, Pia Djermester and Sabine Oertelt-Prigione in Journal of Interpersonal Violence
Supplemental Material
sj-pdf-4-jiv-10.1177_0886260520903130 – Supplemental material for Prevention Strategies for Sexual Harassment in Academic Medicine: A Qualitative Study
Supplemental material, sj-pdf-4-jiv-10.1177_0886260520903130 for Prevention Strategies for Sexual Harassment in Academic Medicine: A Qualitative Study by Sabine C. Jenner, Pia Djermester and Sabine Oertelt-Prigione in Journal of Interpersonal Violence
Footnotes
Authors’ Contributions
S.J. and S.O.-P. designed the study; S.J. acquired the data; S.J. and S.O.-P coordinated the study; S.J., P.D., and S.O.-P analyzed the data; S.J. drafted the manuscript; P.D. and S.O.-P reviewed the manuscript for important intellectual content; and S.O.-P acquired funding.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: The study was funded by the Charité Foundation (Max Rubner Preis_2014_WPP) and the Equal Opportunity Program of the City of Berlin (BCP_SBel). The funding organizations had no role in design and conduct of the study; collection, management, analysis, and interpretation of the data; preparation, review, or approval of the manuscript; and decision to submit the manuscript for publication.
Ethics Approval and Consent to Participate
Ethics approval was sought and granted from the ethics committee of Charité–Universitätsmedizin (EA1/350/14, December 15, 2014). The study was furthermore approved by the three employee representations/staff councils (clinical, academic, and general).
Availability of Data and Material
Data are available upon reasonable request from the authors.
Supplemental Material
Supplemental material for this article is available online.
Author Biographies
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
