Abstract
The rapid acquisition of larg volumes of thin-section CT images has created a considerable need and interest for 3D postprocessing during the interpretation of medical imaging. As a result of the increasing number of postprocessing applications, requiring diagnostic radiologists to perform postprocessing is no longer realistic. This article is a comprehensive review of medical resources regarding establishing a postprocessing radiology laboratory. Besides, leadership and managerial aspects have been covered through a professional business lens. In large-volume settings, a dedicated 3D postprocessing lab ensures the quality, reproducibility, and efficiency of images. Adequate staffing is necessary to fulfill the postprocessing requirements. Educational and experience requirements for 3D technologists may vary among different running laboratories. To evaluate the establishment and running of a 3D lab, it is beneficial to implement diagnostic radiology cost-effectiveness tools. Although establishing a 3D lab has many benefits, certain challenges should be considered. Outsourcing or offshoring may serve as alternatives for establishing a postprocessing laboratory. Building and operating a 3D lab is a significant change in healthcare facilities, and it is crucial for organizations to be aware of the strong resistance toward alternatives the status quo, known as the status quo trap. The change process has essential steps, and skipping the steps creates an illusion of speed but never produces satisfactory results. The organization should ensure the engagement of all interested parties in the whole process. Moreover, a clear vision and proper communication of the vision are vital, and it is crucial to value small wins and ensure expectation clarity in leading the lab during the process.
Background
The rapid acquisition of large volumes of thin-section CT images has generated a significant need and interest in the utilization of 3D postprocessing techniques during interpretation. 1 To enhance the accuracy of extremity bone and joint fracture assessments, several postprocessing technologies such as Multiplane Reconstruction (MPR), Surface Shadow Display (SSD), and Volume Rendering Three-Dimensional Imaging (VRT) have proven to be valuable. These noninvasive CT scan postprocessing techniques have demonstrated improved detection rates and reduced instances of missed or misdiagnosed extremity and joint injuries. 2
Cardiac 3D imaging, including 3D MR angiography, offers a radiation-free and contrast agent-free approach for the detailed evaluation of coronary arteries, minor myocardial scarring, and identification of regional or global myocardial abnormalities. 3 Moreover, Cone Beam Computed Tomography, Three-Dimensional Digital Subtraction Angiography (3D DSA), and 3D visualization of the vascular tree aid in the safe and accurate planning of epilepsy surgeries. 4
In virtual endoscopy, multidetector CT scan (MDCT) postprocessing techniques have created new possibilities by simulating more invasive endoscopy procedures in the gastrointestinal, respiratory, and urinary systems. Virtual endoscopy is crucial in guiding surgical procedures and diagnosing abnormalities in the head and neck region, facilitating practical assessment of tracheal tumours and foreign bodies in the thorax, and serving as an investigated area for early detection of precancerous polyps in virtual colonoscopy. Additionally, virtual gastroscopy and cystoscopy have proven invaluable in the early detection of gastric cancer and bladder neoplasms, respectively. Postprocessing techniques like CT segmentation and volumetry are also applied to pretransplant liver and kidney imaging for surgical planning purposes. 5
Volume rendering techniques contribute to 3D depiction for surgical planning and education, while Maximum Intensity Projection (MIP) and multiplanar reformatted images aid in evaluating vessel calibre and patency during CT angiography of different organs. MIP images also serve as a valuable tool for pulmonary nodule detection in CT scans. 1
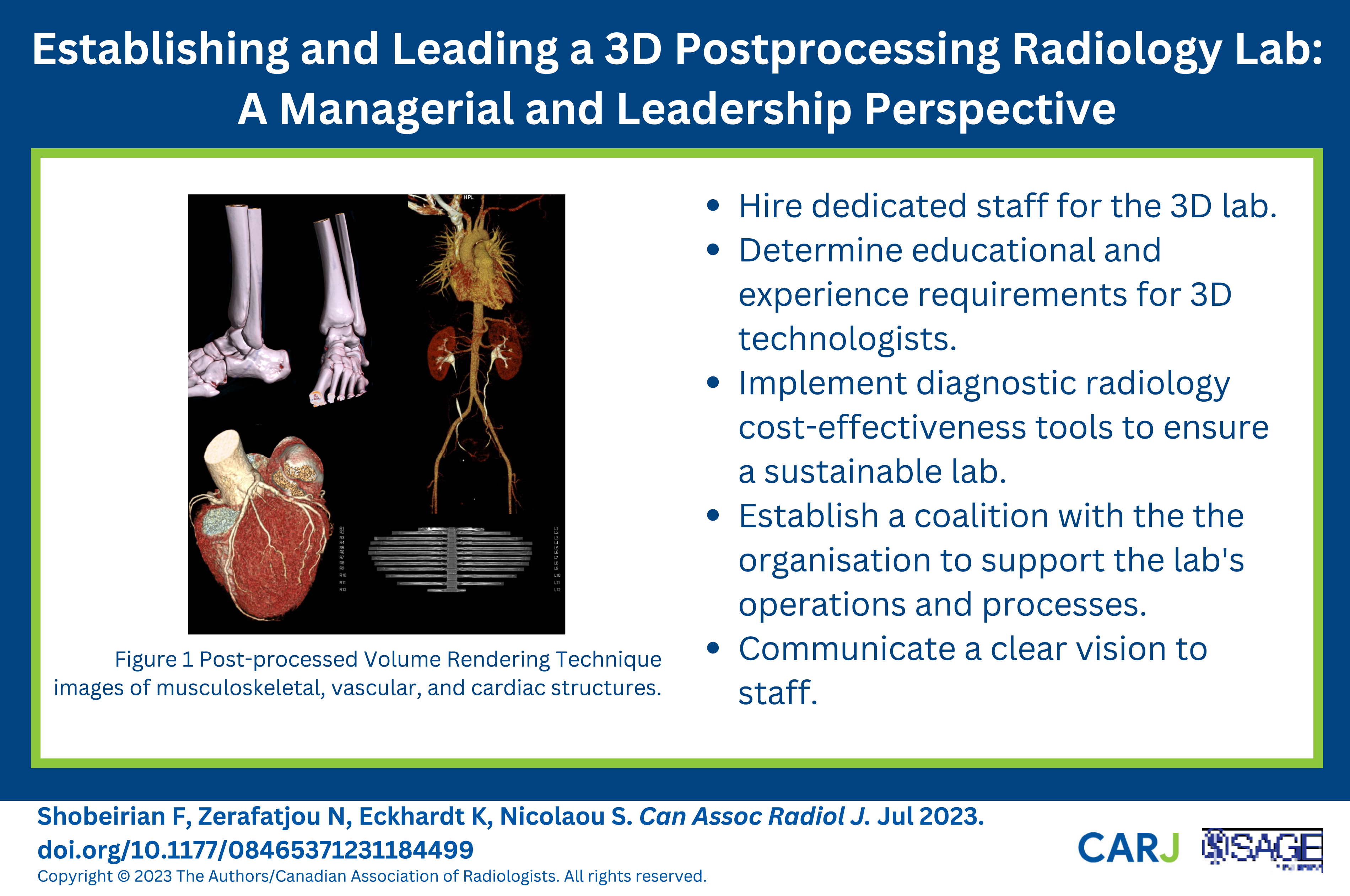
The applications and implications of 3D postprocessing techniques are expanding rapidly due to their ability to enhance the accuracy of diagnosis and treatment planning, reduce costs, and minimize the invasiveness of procedures (Figure 1). 3D images promote pre-surgical planning, leading to shorter operating room time and reduced healthcare costs by increasing diagnostic sensitivity. Besides, 3D postprocessing decreases care costs by mitigating or eliminating the need for some diagnostic procedures. For example, the vascular structure evaluations by combined catheter angiogram and intravenous pyelogram before renal transplant have been replaced by CT angiography plus a delayed phase CT urogram.
6
Post-processed VRT (Volume Rendering Technique) images of musculoskeletal, vascular, and cardiac structures.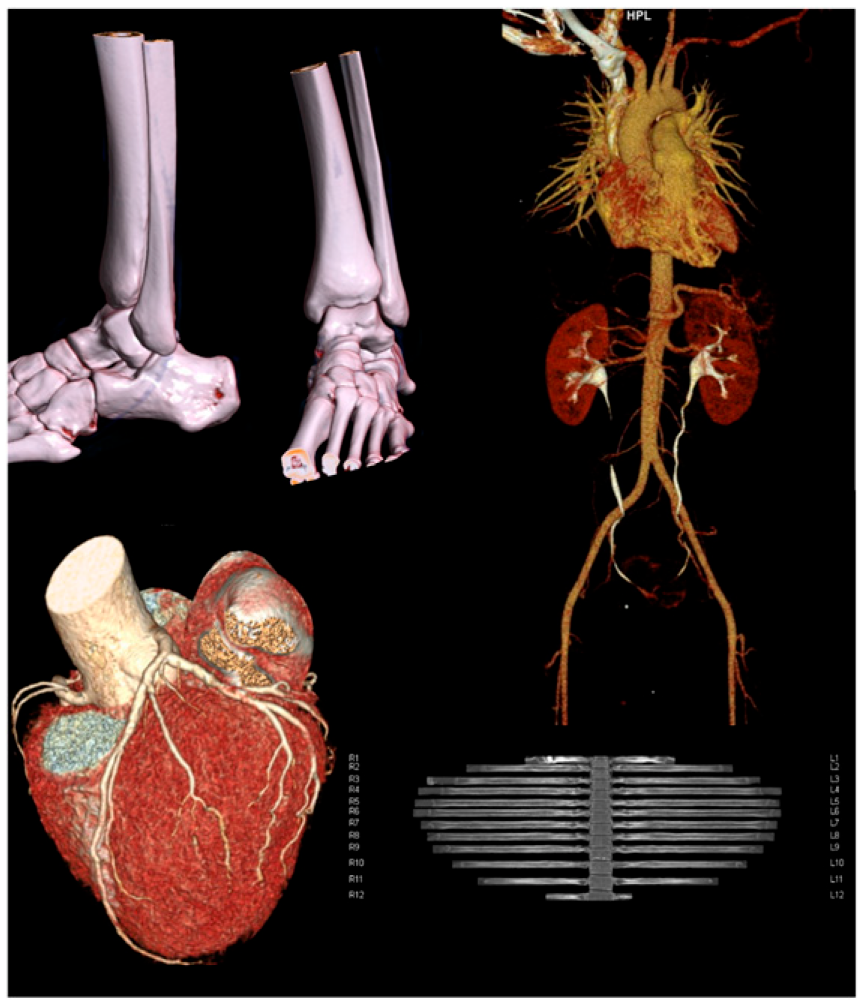
Some commercially available tools for 3D postprocessing are Siemens Syngo.via, Vitrea Advanced Visualization, Intuition Hybrid Suite, Mimics Innovation Suite, and OsiriX MD. Siemens Syngo.via is a multi-modality 3D imaging software developed by Siemens Healthineers. It offers tools for postprocessing, advanced visualization, and clinical applications in radiology. 7 Vitrea Advanced Visualization, presented by Canon Medical Systems, provides various tools for 3D rendering, vessel analysis, cardiac imaging, and more. 8 Intuition Hybrid Suite, developed by TeraRecon, is a versatile 3D postprocessing providing advanced visualization features like MPR, VRT, and cardiac analysis. 9 Mimics Innovation Suite, by Materialise, also offers a wide range of medical image processing, segmentation, and 3D modelling tools and is commonly used in various medical fields. 10 OsiriX MD, a widely used DICOM viewer, offers advanced visualization and postprocessing capabilities. It is specifically designed for medical professionals and includes features like 3D rendering, multiplanar reconstruction, and vessel analysis. 11
The Problem
The growing volume of CT and MRI images and increasing numbers of 3D postprocessing imaging applications have led to a vast number of performing 3D postprocessing. As a result, requiring diagnostic radiologists to complete all the medically indicated that 3D postprocessing is no longer realistic. 1 It is because postprocessing is a task apart from interpreting prepared images. For example, they should open the source images in the postprocessing application software, launched separately from a physically different workstation or through PACS in the most modern PACS, choose the proper processing application and perform the processing by completing the required steps. This process usually takes a few minutes to even 1 hour for each patient.
The Solution
Establishing a Dedicated 3D Postprocessing Lab
As a result of the high clinical demand for postprocessing, several successful dedicated labs have been established worldwide. 12 In a dedicated 3D lab, the time that imaging technologists spend on postprocessing in the traditional model could be utilized for imaging another patient, or radiologists allocate the postprocessing time to interpreting another examination. 1 In busy imaging practices, a 3D advanced postprocessing lab can transfer postprocessing responsibilities from radiologists to 3D lab technologists with specialized training to complete 3D postprocessing. 1 In this model, trained 3D technologists generate 3D postprocessing outputs parallel to the radiologists, and radiologists can make some adjustments if needed. 1
Many , including neurologists, cardiovascular surgeons, plastic surgeons, and dentists, refer their patients to receive postprocessing services that significantly help them diagnose and treat their patients. To build referring physicians’ trust, medical imaging facilities must provide a consistent quality presentation of postprocessing services which is much easier to control with a dedicated postprocessing lab instead of individual radiologists. 12 In dedicated postprocessing labs, the processed products are delivered by 3D lab technologists with high quality, reliability, and efficiency, enabling radiologists to find time to perform interpretive tasks.6,12 In addition, it is more likely for a dedicated postprocessing lab to keep up with the increasing volume of postprocessing requests compared to individual radiologists. 12
Requirements for Establishing a 3D Post-Processing Laboratory
Staff
A dedicated staff is needed to provide 3D postprocessing adequately. 12 The number of full-time 3D technologist staff required depends on the anticipated volume of 3D postprocessing. The salary of an expert 3D technologist is expected to be slightly higher than a modality technologist. 1 However, the pool of experienced 3D technologists is small in the US and is even smaller in Canada. Therefore, recruiting 3D technologists takes much work. Experienced registered CT or MR technologists are the best workforce members to work in the 3D lab. 6 However, biomedical engineers might be potential options, particularly if the lab expands and includes 3D printing, virtual reality (VR), and artificial intelligence (AI). 3D lab technologists should comprehensively understand anatomy, pathology, and scan artifacts. They should work closely with radiologists and referring physicians to generate the most valuable views. 6 Neuroradiology and cardiovascular postprocessing are the priorities for recruiting postprocessing-trained technologists. Radiology fellows and residents can incorporate a rotation in the 3D postprocessing lab as part of their curriculum along with Radiology Technology program students. 13 Some qualifications advertised for the 3D Imaging Technologist job position in 3D labs on the Indeed Website are completion of an accredited Radiology Technology program, a minimum of 2 to 3 years of scanning experience as a CT or MRI technologist, experience with 3D or multiplanar reformatting preferred, knowledge in cross-sectional anatomy and gross pathology. Some labs accept accredited Radiologic Technology programs and bachelor’s degrees in health science or hospital-based programs with preferred CT and MR licenses. The ability to perform tasks accurately, work cooperatively in multidisciplinary teams, and work under time pressure are valuable skills in this role. A similar job description was posted on the Indeed Website under the Image Analyst job title with required qualifications of bachelor’s or master’s degrees in bioengineering, biology, pre-med, or related fields. ARRT (American Registry of Radiologic Technologists)-Certified Radiologic Technologists, especially those with CT or MR specialization, were announced as of interest in this job post. Hired people in such positions would complete PIA (Precision Image Analysis) Analyst Certification processes after hiring. 14
By advertising the 3D technologist jobs to university students in aimed programs, technologists can be attracted to the 3D lab just after graduation. Holding sessions to introduce 3D labs to university students and participating in job fairs are effective measures. Marketing the lab in the communities, such as radiology conferences, can also attract technologists. When a technologist is hired, measurable goals should be defined to set expectations for both the technologist and the manager. To reach full competency, a new 3D technologist takes 6 to 12 months. 1 Generally, it takes 2 to 4 months for a technologist to get familiar with the software, 4 to 6 months to get comfortable with it, and up to 12 months to fully understand radiologists’ and referral physicians’ needs. The more interaction the 3D technologists have with the radiologists, the shorter these periods will be, as the technologists can comprehend what radiologists need for the reliable interpretation of postprocessing results. Besides, technologists’ participation in the meetings, consisting of different specialities, held to decide for patients helps technologists find a clinical sense and understand what referral physicians are looking for in postprocessing images. Then, they can generate what physicians need to make the best decisions. The 3D technologists should regularly receive constructive feedback on areas of development, and insufficiencies should be identified early. Recruiting skilled 3D technologists is not an end goal. The picture archiving and communication system (PACS) and postprocessing techniques are evolving. Therefore, the postprocessing lab should consider these ongoing advancements in staff training and requirements for hiring new technologists. 1
Physical Space
3D technologists may eventually start dedicated postprocessing with a workstation in reading rooms to find a dedicated physical space. Existing thick-client workstations can be used aligned with new full-featured workstations until they gradually get replaced by new ones. New full-featured workstations run thin-client postprocessing with access to PACS and electronic medical records. Tablets and pens, wall-mounted displays, and ergonomic furniture (adjustable monitors, keyboards, and chairs) are also needed in a 3D lab. 1
Costs
In order to create a financial plan for the 3D lab, we need to take into account various factors. These include expenses related to constructing or renovating the physical space, acquiring necessary hardware and software, and covering the salaries of technologists. 1 Additionally, there are other expenses to consider, such as staff training and development, equipment and furniture maintenance and renewal, software updates, commercially available post-processing tools, marketing activities, and innovation initiatives. It is important to note that apart from the initial setup costs for the dedicated post-processing lab, ongoing expenses will be associated with its operation.
Cost-Effectiveness of Establishing a Postprocessing Lab
Radiology imaging is the fastest-growing medical expenditure and is central to medical decision-making. As a result, there is an increasing demand for cost-effectiveness analysis of imaging technology assessment. When it comes to limited healthcare resources, cost-effectiveness analysis helps with proof of value for medical expenditures and maximizing health effects. Performing cost-effectiveness analysis is challenging in diagnostic imaging as the effects on costs and health outcomes highly depend on the treatment strategy decisions based on the imaging result. Standardized methodologies for diagnostic imaging cost-effectiveness analysis still need to be included. However, some tools are available to perform and interpret cost-effectiveness analysis for radiology technologies expenditures. 15 The return on investment for establishing and running a dedicated lab takes work to measure. However, it immediately pays off to the referring physician and patient care. 12 Moreover, in a dedicated 3D postprocessing lab, the processing is done by 3D technologists, who are a less expensive workforce at about a third of the salary of radiologists leading to an immediate cost reduction. Without a dedicated 3D lab, radiologists spend a few hours daily performing 3D postprocessing. With a 3D lab, dedicated 3D technologists, with lower costs/per hour, do the postprocessing and radiologists interpret additional radiology images. This work assignment decreases the need for additional radiologists, a costly workforce, to read medical imaging. 6 To maximize the cost reduction, it is helpful to take the postprocessing responsibilities from radiologists and give them to 3D technologists as much as possible. Some potential sources of revenue for postprocessing are the provision of service to research projects or accepting contracts of doing the postprocessing for other healthcare or imaging centres.
Challenges of Establishing a Postprocessing Laboratory
One of the challenges is the billing and coding of the services provided by the 3D imaging laboratory, which should be planned precisely in advance, considering various aspects. Another challenge is balancing demands for postprocessing and providing the services. Regarding the volume of postprocessing services, balancing what is needed for an accurate diagnosis/planning and what is more than necessary is challenging. The existence of a dedicated 3D lab may lead to an unnecessarily high volume of postprocessing requests, and the 3D lab might produce some 3D images with higher quality than diagnostically necessary. Creating clear guidelines and imaging postprocessing protocols based on local needs and effectively communicating postprocessing indications with referral physicians and radiologists mitigate this challenge. The organization should not underestimate the importance of ongoing evaluation in running the 3D lab. Quality control is essential to ensure that postprocessing follows the protocols. Running a dedicated 3D lab requires regular input from interested parties, including radiologists and referral physicians. 1 The quality of postprocessing services can be measured by responsiveness to the customers, referring physicians or radiologists.1,12
Alternatives for Establishing a Postprocessing Lab
Outsourcing/Offshoring
Outsourcing or offshoring are alternatives for establishing a 3D postprocessing radiology laboratory. A local dedicated 3D postprocessing lab can provide more customized services based on local needs and local referral physicians’ practice and is faster. However, establishing and running a 3D postprocessing lab might be expensive in the beginning. Outsourcing occurs when a firm contracts with another firm to provide service, while offshoring occurs when a domestic firm outsources service to a firm in another country. 16 The ‘Laboratoire de reconstruction anatomique 3D’ in Québec is the only 3D postprocessing lab available in Canada. 17 Meanwhile, multiple 3D postprocessing labs in the USA accept contracts for providing postprocessing services to other healthcare centres. A precise analysis is needed to evaluate these alternatives.
The Next Step
3D Printing Lab
3D printing labs are the extension of 3D postprocessing labs. The applications of 3D printing include anatomical models, modified anatomic models, and virtual surgical planning with templates. In practice, complex cases require detailed discussion that can be supported by 3D visualization to clarify complex anatomy. Many university environments provide 3D printing labs. 3D printing lab can start within a medical staff office. The leader of the 3D printing lap can be physicians or engineers/physicists with anatomy background knowledge. Radiology technologists have a prominent role as 3D printing is based on CT or MRI DICOM images. The partnership of referring physicians with technical experts is fundamental in a 3D printing lab. The early strategy for developing a 3D printing lab is growing a partnership between radiologists and one group of specialists, like cardiology surgeons. 18
Leadership Recommendations
Change Management
Establishing a 3D lab is a significant change in an organization and requires the healthcare team to adapt to this change. The establishment and running of a 3D lab change the practice in the organization to a great extent and disrupt the status quo. The organization should be aware that there is a strong resistance toward alternatives that perpetuate the status quo, known as the status quo trap. To prevent the status quo trap, decision-makers should be aware of it and ask themselves whether they would choose the status quo (no 3D laboratory) as an alternative if it were not the status quo. Besides, they should not exaggerate efforts or costs in switching from the status quo and remember that the desirability of the status quo will change in the future due to ongoing developments. 19 Building and running a 3D lab is a significant change in a healthcare facility. The change process has essential steps, and skipping the steps creates an illusion of speed and never produces satisfactory results. A successful change starts with a sense of urgency in the organization. The information about potential crises and great opportunities should be communicated dramatically to motivate individuals to acquire aggressive cooperation. 20
Engagement
After capturing the interested parties’ attention to the problem, the organization should ensure the engagement of interested parties. All interested parties should be involved in the decision-making process of establishing and running a successful 3D lab. Interested parties, particularly radiologists and radiology technologists, should be involved in decision-making and encouraged to share their ideas to build collective wisdom. It is essential that people feel the decision is based on fair processes to increase the organization’s collective strength and everyone’s chance of winning. To achieve this, leaders should be active moderators and insist on the team playing an active role in meetings. 21 Engagement results in better decisions and more significant commitment from involved individuals. 22 Moreover, A powerful coalition within the organization, in terms of titles, expertise, reputation, and relationships, is needed to support the establishment of a 3D lab. 20
Vision
A clear vision for establishing and running a 3D lab is needed for a successful process. This vision comes from analytical thinking and a little dreaming. 20 The vision should centre on patients or patient safety. Without a clear vision, this project might take the organization in the wrong direction. 20 Suppose the establishment of a 3D lab is to become a successful movement. In that case, the organization’s employees must not only recognize the need for this change and what needs to be done but also want to do it. 21 Therefore, the proper communication of the vision is vital.
Communication
People should be willing to help or even make short-term sacrifices to make the 3D lab succeed; without much communication, this will not happen. Hence, leaders should use all the available communication channels to share the vision. 20 Good communication keeps employees accountable for moving the 3D lab forward. 23 Everyone involved in and affected by the decision should understand the reasons behind the decision. Explanation and comprehensive communication allow employees to trust that decisions are in the overall interest of the organization. Winning employees’ trust is crucial; otherwise, they will withhold their full cooperation. 22 The more meaningful the rationale is, the more likely the employees will live up to their performance potential. 24 Moreover, it is imperative to keep the whole organization updated about the 3D postprocessing imaging laboratory establishment and running in different phases, including planning, execution, opening, running, and expanding.
Short-Term Wins
The establishment and running of a 3D lab do not happen overnight, and the team starts from almost zero to achieve acceptable performance and service delivery after a while. Then, it is crucial to value small wins. 24 The organization should set short-term goals because most people cannot go far without short-term wins and celebrations. 20 To make the successful 3D lab manageable, a series of achievable goals at different levels should be defined. 21 Specifying milestones and performance goals as symbols of accomplishment can motivate and energize the team and challenge them to commit themselves to making a difference. 24 Regular meetings help introduce the culture of performance by producing results and responsibilities clear to everyone. 21
Expectation Clarity
Expectation clarity is essential in leading the 3D imaging lab. Clear performance goals help the team to keep track of their progress and hold them accountable. 24 In addition, new roles and policies should be adequately communicated to employees, and they should know expectations from them. 22
Feedback
3D technologists must receive feedback regularly. 3D lab leaders should keep feedback positive and constructive, and team performance should be recognized and rewarded. However, the organization should ensure that 3D team members do not take feedback personally because sometimes it is challenging to distinguish self from the role and not respond to what feels like a personal attack. 23
Footnotes
Acknowledgements
We extend our sincere acknowledgment to Shannon Walters, the Executive Director of the Stanford 3D Lab, for graciously sharing his invaluable vision and expertise, which greatly contributed to the creation of this article.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
