Abstract
Health worker burnout is not a new phenomenon; it existed before the COVID-19 pandemic but has worsened since. Organizations have implemented various interventions to help staff recover from burnout, but few have focused on preventing or addressing sources of burnout. This article addresses this gap by focusing on promising practices and interventions that can be utilized to prevent and address burnout. By using a mixed-method approach, we learned that listening to frontline staff is essential for creating a short list of interventions that can be tailored to meet the unique needs of different organizations. Time, money, and other resources are required to implement sustainable change, along with balancing a top-down and bottom-up approach. Finally, building on an inherent desire for more connection both within individual sites and across organizations is key. Health leaders are encouraged to engage staff members regarding their concerns and dedicate sufficient resources to support necessary changes.
Introduction
Healthcare workers have been experiencing higher rates of burnout since the COVID-19 pandemic. 1 According to the International Classification of Diseases, burnout is a syndrome resulting from chronic workplace stress that has not been successfully managed. 2 Its three dimensions include feelings of energy depletion, increased mental distance from one’s job, and reduced professional efficacy.
Meaningful interventions are needed, and many have been developed that address different issues that work best in tandem. 3 Individual level interventions include stress management techniques; self-care promotion such as yoga, mindfulness, and relaxation practices, communication skills training, coping strategies, and access to mental health support. 4 Team level interventions tend to focus on peer support, mentorship, and leadership within a group setting. Organizational level interventions include policies within an organization, such as leadership development and training opportunities, which tend to target aspects of the work environment that an individual has very little ability to change. 5 Finally, system-level interventions target policies at an association/union level, including collective agreements, government action and advocacy efforts aimed at promoting sustainable workforce well-being. 6
The IGLOO framework emphasizes that successful interventions must be multi-level to be sustainable, targeting five specific levels: individual, group, leader, organization, and overarching/social context. 7 This framework enhances how health leaders can support staff experiencing burnout. There are several interventions designed to prevent, address, reduce, and support recovery from burnout. One example includes a Web-based Implementation Science of Enhancing Resilience (WISER) that shows promise in reducing the emotional exhaustion component of burnout. 8 Different aspects of burnout can also be examined. For instance, the Copenhagen Burnout Inventory (CBI) assesses personal, work-related, and client-related burnout. 9 The Maslach Burnout Inventory (MBI) focuses on emotional exhaustion, depersonalization, and reduced personal accomplishment. 10 Given the gendered nature of the health workforce, it is important to consider the gender and intersectional dimensions, such as household and childcare demands, workplace discrimination based on ethnicity/race are typically shown to be higher for women 11 compared to men, 12 along with greater dissatisfaction surrounding work-life balance. 13
In our ongoing work, we described the development of a bilingual on-line toolkit to prevent, address, and recover from burnout among health workers. 14 In this article, we report qualitative data on promising practices among organizations that yielded positive changes in health worker burnout.
Methods
A mixed-method approach, including 463 surveys and 43 interviews, was undertaken at two different time points (pre- and post-intervention) across three clinical sites representing acute, primary, and mental health/housing support sectors in an urban centre in the province of Ontario. Although the quantitative data informed our participating sites, this article presents findings from an analysis of qualitative interview data which are presented under four key themes.
Data Collection
The Number and Type of Interview Participants Across the Three Sites
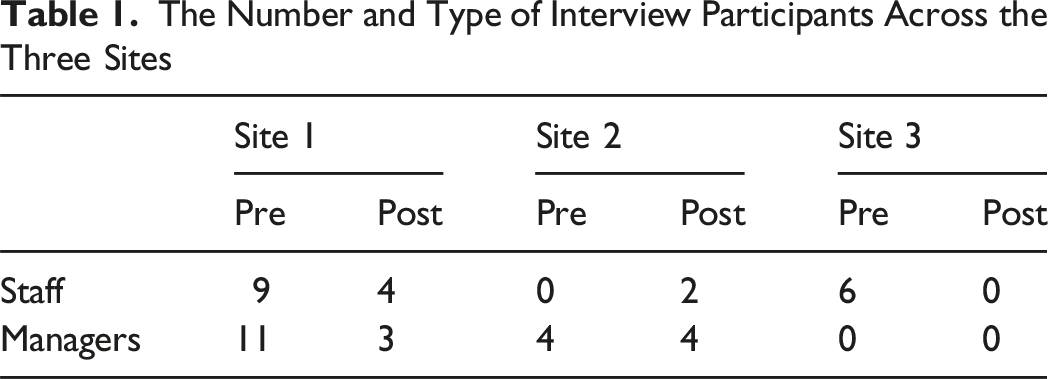
Data Analysis
The research team utilized a structured analytic approach involving transcription, organization, and thematic coding using a constant comparison approach 15 to categorize the qualitative interview data across all three sites into categories. 16 Members of the research team independently read each transcript and applied an open-ended coding approach to classify the data. 17 Team members met monthly to compare findings and discuss trends across the data. This collaborative nature of data analysis enhances the reliability of the findings through analytical triangulation. 18
Findings
Four key themes were uncovered from the qualitative interviews as promising practices across the sites (Figure 1). The findings hold implications for health leaders in terms of addressing burnout within their organizations. The first theme focuses on tailoring interventions to meet the needs of each unique site. The second theme highlights the need to find resources to make the required change(s). The third theme focuses on a balance between top-down and bottom-up approaches. The final theme centres on building an inherent desire for more connection within and across organizations. Themes Uncovered Across All Three Sites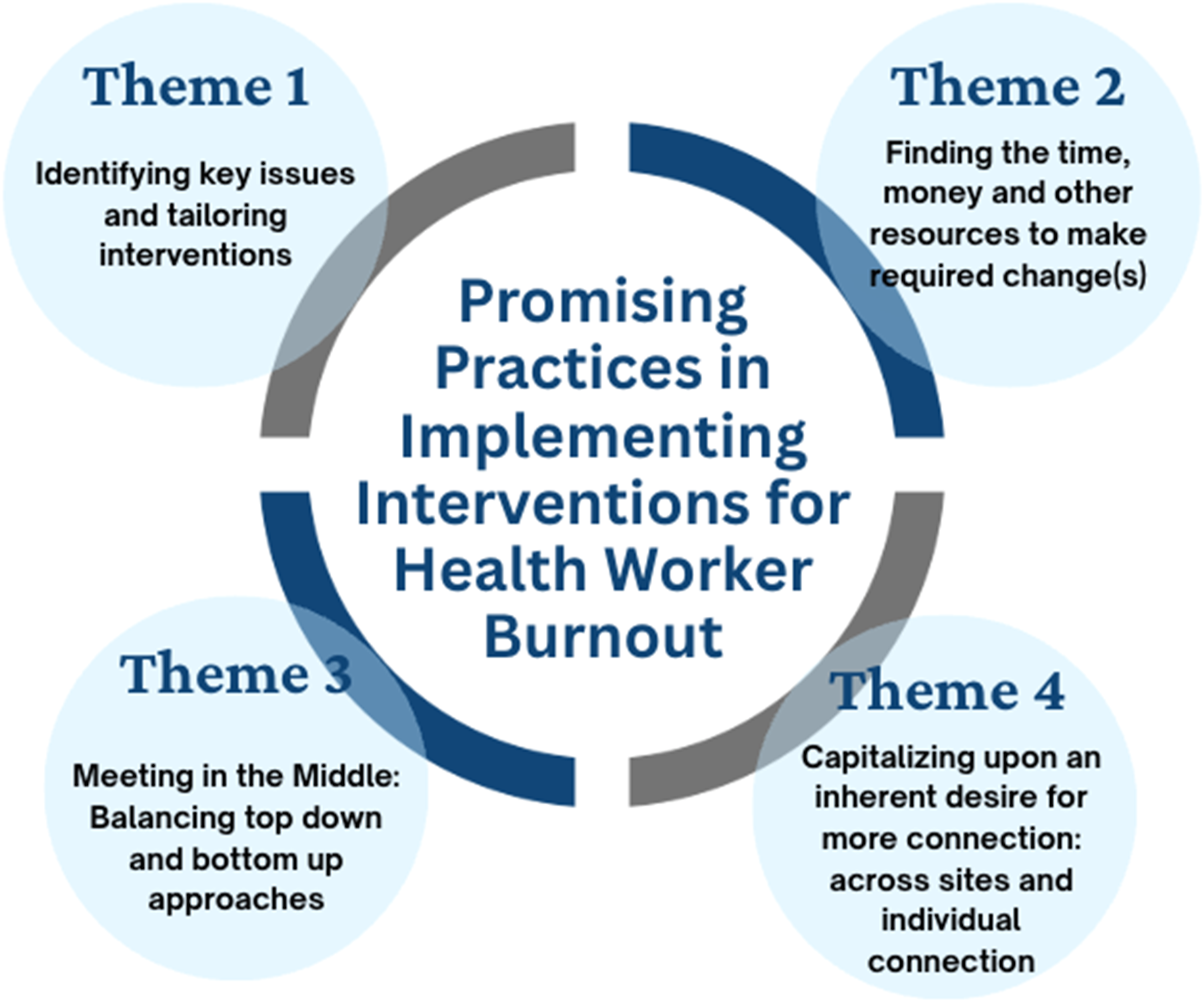
Identifying Key Issues and Tailoring Interventions
An initial analysis of the surveys was undertaken and integrated with the interview data and presented to leadership, management, and staff for discussion of the key issues arising from the data. Each site was also provided with a shortlist of interventions from our toolkit to address these concerns. The staff at all three sites articulated the importance of prioritizing worker well-being; however, each site was at a different stage with respect to what had been done in the past and the current initiatives being offered at the time. Common concerns across sites included ensuring the interventions aligned with organizational strategic goals and not duplicating efforts or inundating staff with yet another initiative. Site 1, for example, hired a company to conduct a survey in the past, but no action was subsequently taken. This led staff to question the purpose of this research, which required trust to be rebuilt. Site 2 understood their burnout challenges but lacked clarity on what actionable steps to take moving forward. Site 3 already had a long list of interventions being implemented and was reluctant to implement any further interventions.
Process for Shortlisting Interventions to Be Adopted or Adapted
The first promising practice included listening to what frontline staff had to say to create a short list of meaningful interventions. A short list of interventions was shared with staff, including ideas at a leadership, team, organizational, and systems levels. The research team emphasized the intervention could be one contained idea or it could be a combined set of interventions and it could involve one team, the whole organization or anything in between. To move from ideas to implementation a variety of intervention examples were shared with the idea of a “living” intervention.
Having a wellness team or group of champions narrow down an intervention, given the resources and capacity available was helpful. Receiving input from a variety of staff (i.e., part-time, full-time, casual, and different departments) ensured the adoption or adaptation of specific interventions was also successful. Figure 2 provides an overview of the promising practices for shortlisting interventions at site 1. A roadmap for shortlisting interventions at site 1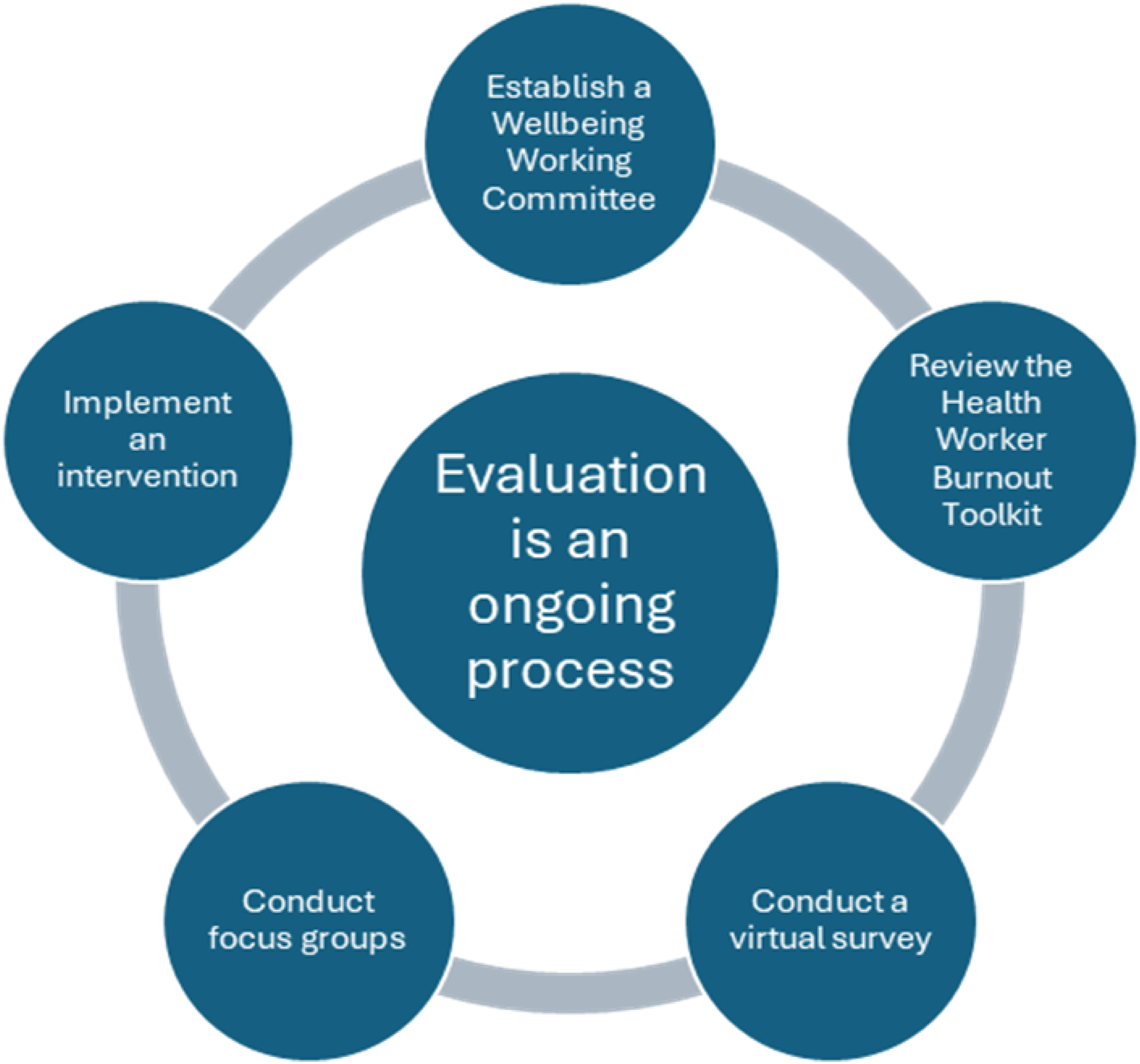
Tailoring
At site 1, the Wellness Working Committee met on a regular basis and took the time to create a summary document of the interventions we had shortlisted for them, how they worked, why they were valuable, the cost, and what coordination for roll out would look like. Site 1 decided to pilot an intervention called Commensality Groups, which aims to increase the sense of connection and collegiality among staff and build comradery and meaning in work, but they were not drawn to the name. They decided to change the name to Connection Circles to better represent their shared purpose.
Finding the Time, Money, and Other Resources to Make Required Change(s)
Funding interventions is an important consideration that aligns closely with time and other supportive resources. Site 1 did not have any competing initiatives when our research team engaged with their organization. They also created time and space for their staff to step away from their work to support the interventions by developing a Wellness Working Committee. Finding the time to identify and commit to an intervention was a challenge for sites 2 and 3 because they had competing priorities and demands from other related activities. Site 2 was utilizing a program called Guarding Minds at Work, which they used to address psychological health and safety at work. Some participants were sceptical: I'm hoping some concrete steps, actions will be taken, coming out of the Guarding Minds, and not just like, ‘we’re working on mental health through blah, blah, blah,’ Like, yeah, that’s not helpful. You know?
Site 3 was engaged in a survey through Accreditation Canada to assess the culture of their organization and the organizational partners were aware of the fatigue amongst personnel about being surveyed for issues that are not improving, which increased scepticism regarding fully engaging in a research project. Site 3 was also undergoing a financial freeze, which prevented any new initiatives from occurring.
Meeting in the Middle—Balancing Top-Down and Bottom-Up Approaches
The third theme we uncovered as a promising practice included meeting staff in the middle which involved participation from frontline staff with leadership support. At site 1, front-facing staff chose the interventions which were in turn supported by their leadership team. An ongoing dialogue between different levels of management kept everyone engaged and motivated to continue even when other organizational demands emerged. Staff told us they felt involved, listened to and that their concerns mattered and were being heard by those with the means to make a change.
When initiatives are implemented from the top down, with less input from the staff who will be most affected, disengagement can result. A participant at site 2 talked about a staff appreciation event where the staff was not consulted during the planning phase.
They shared Leadership should do a better job by asking us ‘what do you want’ instead of ‘this is what you want’ I think they have a hard time understanding what is of value to people.
Site 3 experienced a similar situation where the interventions came directly from the leadership team, resulting in minimal participant engagement. The top-down approach can leave front-facing staff feeling as though the initiatives are more onerous than helpful: The whole process is just another thing that ends up being part of my workload and something I’m expected to participate in on top of all my other usual things I’m expected to manage and take care of.
Interventions that feel burdensome to staff can be challenging, especially for individuals experiencing burnout symptoms.
Capitalizing Upon an Inherent Desire for More Connection
A promising practice of creating a “community of practice”
19
across all three sites builds upon an inherent desire across sites. All three sites were curious and often asked what other sites were doing. Sites did not want to be isolated in their challenges and hearing common struggles across organizations can offer much needed reassurance that they are not alone. The desire for connection within sites includes peer support and peer supervision. The importance of informal connections was also mentioned across sites, with another participant saying: Creating those opportunities for connecting and building more relationships with colleagues, it’s probably made some of the biggest differences in the workplace.
Feeling disconnected was a theme that emerged initially from sites 1 and 2, with staff mentioning they felt like they were working in silos. After the follow-up focus groups, the discussion shifted to talk about sustainability and communication. Staff emphasized the importance of building connections and trust amongst departments, setting up dedicated forums for staff to provide input and fostering a more positive work environment through open communication and empathy.
Discussion
Health worker burnout is a complex problem necessitating a multifaceted approach to address it.20-22 Toolkits offer a practical means of consolidating diverse strategies into an accessible format; however, their effectiveness ultimately depends on their implementation and sustained use. 23 Our findings indicate that implementing interventions is most effective when grounded in empirical evidence from organizations and designed to accommodate the needs of different groups within those organizations. Once the sites included in our project identified their primary site-specific challenges, they were better positioned to make informed decisions regarding which resources or interventions would be most responsive to their needs. Successful application and implementation are further supported when interventions are tailored to the specific contexts and priorities of organizations, and when trusted, collaborative relationships are established between staff and leadership teams within organizations.
Contextual factors within each workplace must be carefully considered before initiating any mental health initiative. 24 Expecting employees to find the time to undertake additional responsibilities without appropriate compensation is both impractical and inequitable. This expectation is also deeply gendered, as women—who are overrepresented in caring and service professions—are disproportionately asked to perform such invisible labour. 25 An additional consideration concerns the scope, scale, and timing of interventions. Providing an overabundance of resources may inadvertently heighten stress, particularly among individuals experiencing significant burnout, especially if organizational, team, and system-level factors are not adequately considered. It is also essential that organizations prioritize and sequence interventions in alignment with employees’ capacity to engage. 26
Although the research team facilitated the development of a short list of potential interventions, leadership and staff were ultimately given the autonomy to determine which interventions to implement. Decision-making power is best when it rests with those who will both enact and be affected by these interventions. 27 Meeting in the middle and finding an intervention that fits the context of the organization, along with identifying champions, leads to the most buy-in from staff.
When there is a disconnect between leadership and frontline staff—particularly regarding the prioritization and pacing of change—implementation efforts can falter and exacerbate employee burnout. 28 Leaders can introduce and champion new ideas, but frontline staff must be actively engaged as partners in the change process. Our findings emphasize how critical it is for health leaders to engage frontline staff in understanding the distinct issues specific to that organization and co-design next steps together.
Organizations are curious about what other sites are implementing and want to be involved in a larger community of practice. Participants emphasized the importance of creating forums dedicated to sharing experiences and connecting across sites to foster a more positive work environment.
Limitations
Caution is warranted when extrapolating these findings to broader contexts, as each clinical site operated within a distinct organizational culture and population demographic. Drawing on insights from the implementation of the interventions described in this study, future research should assess both organizational and individual readiness among workers and leaders prior to initiating mental health interventions. Additional time and resources would likely have benefited sites that were slower to progress during the implementation phase. Organizational support was confined to the duration of the funding period, emphasizing the importance of building internal capacity and empowering staff to sustain initiatives beyond project timelines.
Conclusions
Health leaders are encouraged to engage staff members about their workplace concerns, dedicate sufficient resources to support necessary changes, while continuously soliciting and integrating staff feedback. To achieve a balance between a top-down and bottom-up approach, leaders can introduce and champion new ideas, but frontline staff must be actively engaged as valued partners in the change process. Establishing and maintaining meaningful relationships with staff will be critical to collaboratively developing, implementing, and evaluating interventions that promote psychological well-being and foster positive workplace culture. Health leaders can promote sustainable change in their organizations to address burnout when interventions are co-developed with staff and tailored to meet their unique needs.
Footnotes
Acknowledgements
We would like to thank all the clinical sites for their participation in our research study and we appreciate the time and relationships that were fostered throughout our time together.
Ethical Considerations
Ethical approval was obtained from CHEO: 22/93X, University of Ottawa REB #: S-11-22-8668, Montfort: #23-24-06-015, and the University of Waterloo: #44992.
Consent to Participate
All participants provided verbal consent to participate.
Funding
The authors disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: The Health Worker Burnout Research Project was funded by the Canadian Institutes of Health Research, as part of the Operating Grant Studying the Global Impact of COVID-19 on health, Grant # 478269.
Declaration of Conflicting Interests
The author declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
