Abstract
Integrating research into health service delivery is essential for building an equitable learning health system that values continuous improvement, innovation, and patient-centred care. At the organizational level, evidence shows that research-active hospitals achieve better patient outcomes and experiences, increased staff satisfaction and retention, enhanced operational efficiency, and greater opportunities for innovation and revenue generation. Yet, most Canadian hospitals are community hospitals which lack the infrastructure and organizational supports to conduct research. This article presents a case study of a research institute within a community hospital in Southern Ontario, describing its development, early outcomes, and strategic impact in establishing research as an organizational priority. We also introduce a novel adaptation of the balanced scorecard to guide the implementation and evaluation of research programs in community hospital settings. Reflections from this case highlight patient and organizational benefits, offering practical insights for community hospitals leaders seeking to build research capacity in their organizations.
Introduction
Integrating research into health service delivery is essential to building an equitable Learning Health System (LHS) that values evidence-based practice and continuous improvement. 1 Hospitals play a key role in developing a LHS by facilitating the intersection between research and acute health service delivery. 1 However, 90% of the 602 hospitals in Canada are community hospitals, 2 many of which lack the infrastructure and strategic focus to engage in research. The concentration of research within a small proportion of Canadian hospitals limits our health system’s ability to efficiently generate evidence, limiting the fulsome development of an equitable LHS.3-5
Engaging in health research offers several organizational benefits that warrant the attention of hospital leaders. Research-active hospitals have demonstrated improved patient outcomes and experiences,6-8 enhanced clinical staff satisfaction and retention,9,10 increased operational efficiency, 10 and greater opportunities for innovation and revenue generation. 9 Moreover, research-active hospitals are positioned to rapidly adopt evidence-based standards of care, 10 reinforcing their commitment to quality improvement. Expanding research in community hospitals not only benefits individual organizations but also enhances health system equity. It ensures that patients in suburban, rural, and remote areas have access to clinical studies and that research findings are both relevant to local communities and generalizable to wider Canadian populations.3,11-13 In response, scholars and health system leaders have increasingly called for strategic investment in community hospital research infrastructure.3,5,9,12,14-16 Recent shifts in the health research landscape, such as the growth of regional medical campuses 17 and the impact of the COVID-19 pandemic, 4 have accelerated community hospitals’ interest 11 and participation in health research.18,19
Despite this momentum, the literature offers limited guidance on building community hospital research capacity at the organizational level. Previous work, including that by our own group, has largely focused on building research capacity at the program or unit level,4,18-24 where research is typically driven by individual champions within single clinical departments. 24 Others have examined regional approaches,25,26 such as those employed in British Columbia, where health authorities coordinate research across multiple institutions. 26 In contrast, Ontario’s health system comprises independently governed hospitals, 27 which presents both unique challenges and opportunities for integrating research into the organizational structures. Understanding how to build sustainable, organization-wide research capacity in these settings remains an underexplored but critical question that must be addressed if we are to move toward becoming a true and equitable LHS.
This article contributes to the dialogue on building Canadian community hospital research capacity by presenting a case that describes the development, early outcomes, and strategic impact from establishing a research institute in a community hospital in Southern Ontario—illustrating the organizational and patient benefits achieved.
Developing the Niagara Health Knowledge Institute
Niagara Health is a publicly funded, community hospital system in Southern Ontario, serving over 500,000 residents across the Niagara region. It operates 5 sites with 900 inpatient beds 2 and a team of over 7,000 staff and 600 physicians. In 2022, building on the NH Physician Research Lead’s ongoing national research capacity building work in community hospitals, a proposal to establish a research institute at NH was put forward to the McCall MacBain Foundation. In May 2023, the Niagara Health Knowledge Institute (NHKI) was established with the support of a $4 million donation from the McCall MacBain Foundation. The decision to establish a research institute was primarily driven by the desire to formalize research within the organizational structure, enhance research capacity, and align it with the hospital’s strategic priorities. As supported by previous literature, the creation of an institute was also seen as a strategy to increase patient access to research, improve quality of care, attract external funding and talent, unify and coordinate existing research efforts, and enhance visibility within the broader health research landscape.3,5,9,10,12,14-16,28
Prior to establishing the NHKI, there were several foundational elements for research in place at NH (Figure 1A). These included collaborations with nearby academic institutions and hospitals, access to a Research Ethics Board (REB), and several clinical research programs led by physician investigators on their own time. However, these efforts were largely decentralized and operated without a formal strategic framework or governance structure. In early 2024, a 4-year strategic plan for the NHKI was developed to guide its initial direction and implementation. Co-developed by the NHKI team and NH’s senior leadership, the plan intentionally aligned the research institute’s purpose, vision, values, and guiding principles with the hospital’s broader strategic goals, reflecting an organizational commitment to becoming a LHS by embedding research across organizational priorities. Recognizing that research capacity building strategies are well-established in the literature,29-31 we retrospectively mapped the NHKI’s development process onto Cooke’s Research Capacity Building (RCB) framework
29
to summarize our approach (Figure 1B). Cooke’s RCB principles were also used to inform the NHKI’s short- and medium-term priorities and establish performance targets during its initial years. (A) Timeline of Foundational Activities and Milestones Leading to the Establishment of the Niagara Health Knowledge Institute. (B) Alignment of Niagara Health Knowledge Institute Activities With Research Capacity Building Principles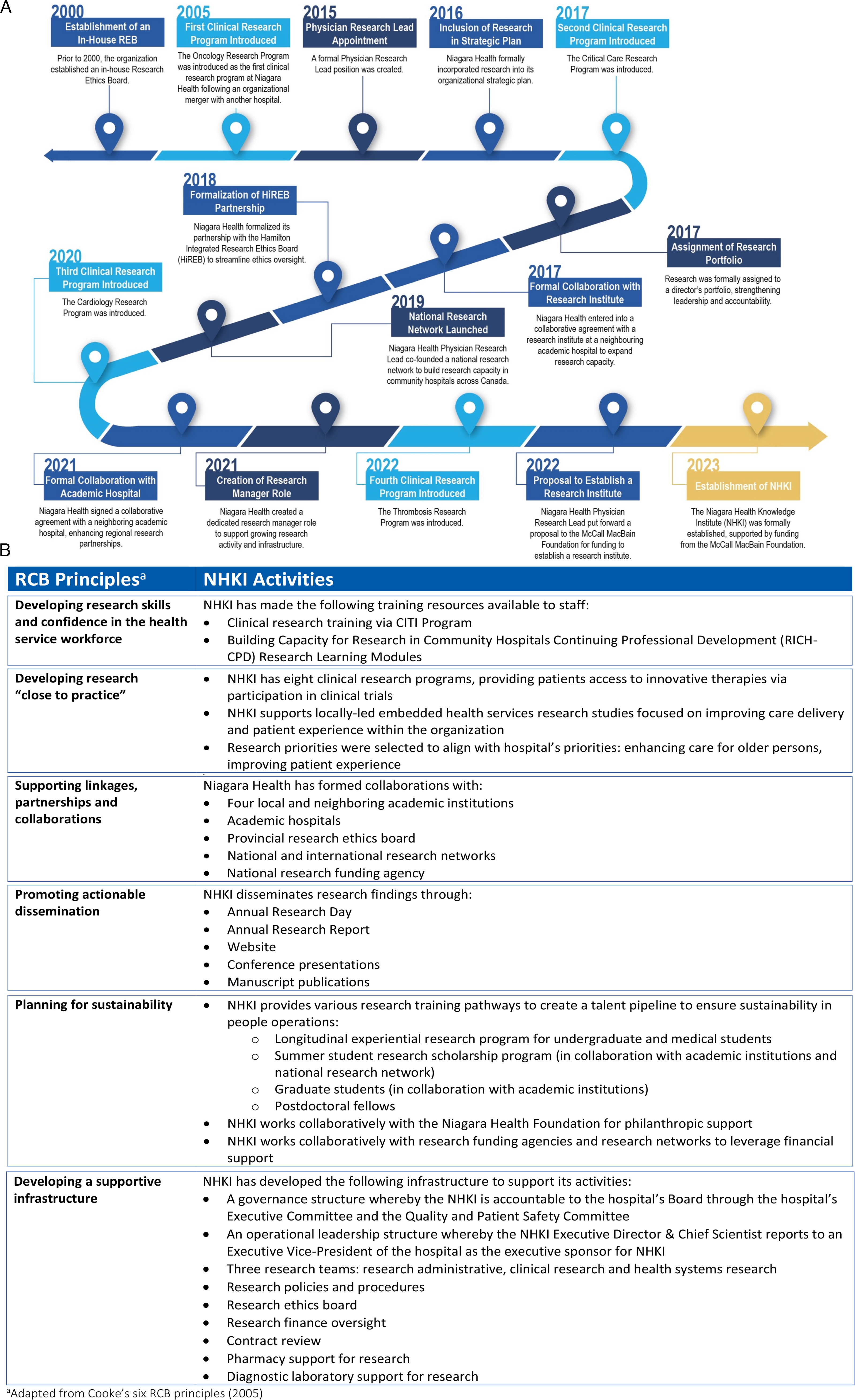
Evaluating the Niagara Health Knowledge Institute
Developing the NHKI’s Balanced Scorecard (BSC)
Two years after its establishment, the NHKI administrative team developed a framework to assess its initial performance using the Balanced Scorecard (BSC) approach. The BSC is a performance management tool that translates the organization’s strategic goals into a holistic set of measurable performance objectives.32,33 The BSC consists of 4 interrelated ‘perspectives’: (1) financial, (2) customer, (3) internal business, and (4) learning and growth.
32
When applied to the context of Canadian hospitals, Baker and Pink
33
explain that these perspectives are focused on addressing the following questions: (1) How do we look to funders? (2) How do our customers (i.e., patients and families) view us? (3) What must we excel at? (4) Can we continue to improve? Previous studies have found value in adapting the BSC framework to reflect the unique characteristics, mission, and objectives of individual organizations.18,34 Guided by this approach, we mapped the NHKI’s guiding principles onto the four perspectives in Kaplan and Norton’s BSC to develop a custom scorecard for the NHKI (Figure 2). We identified relevant goals and associated performance indicators for each perspective using data from the NHKI’s strategic plan, as well as insights from previous literature on applying the BSC in similar contexts.18,33 Output measures were retrieved from the NHKI’s 2023 and 2024 annual reports.35,36 It’s important to note that the scorecard is not intended to measure annual improvements but rather, to ensure that performance is assessed holistically. Niagara Health Knowledge Institute Balanced Scorecard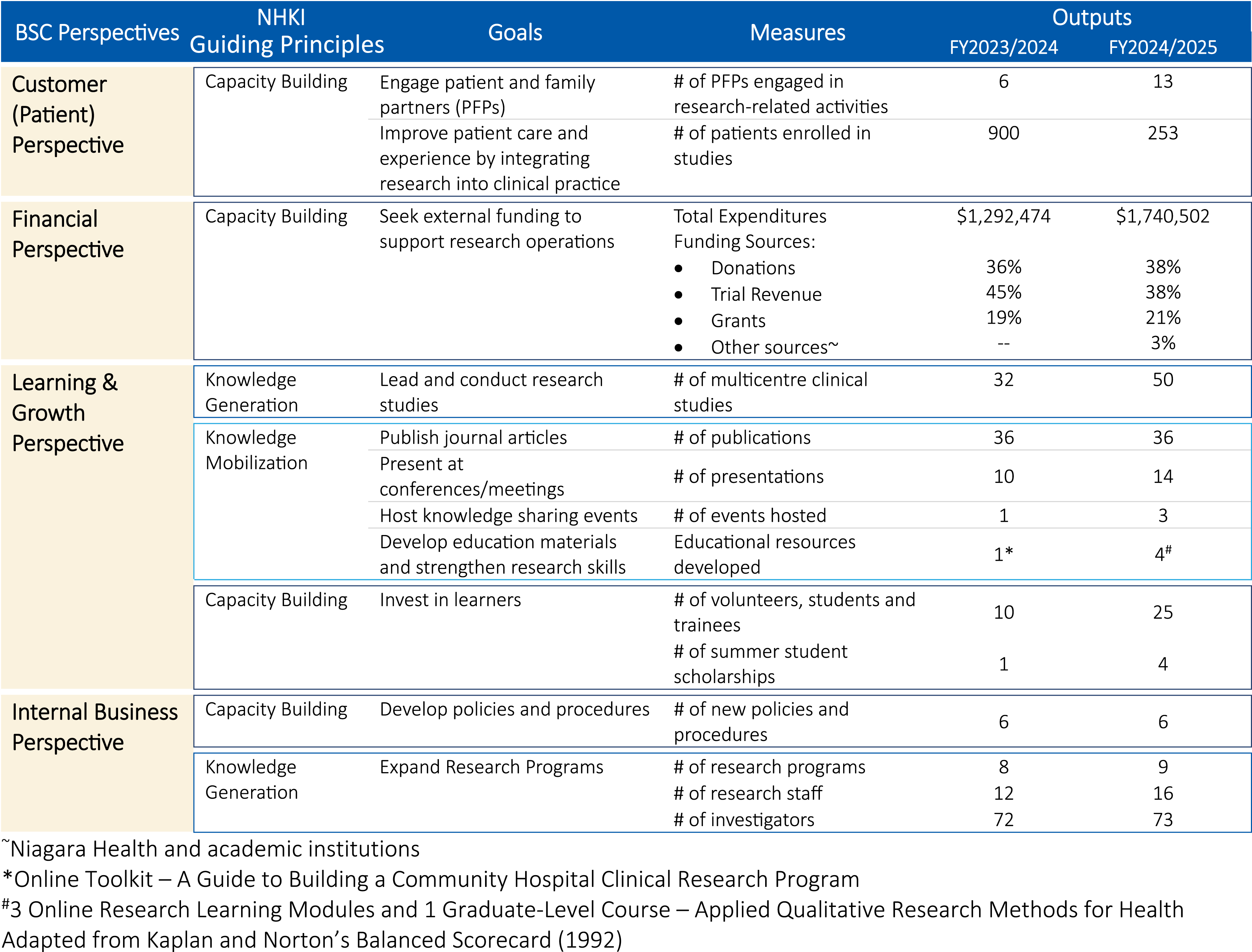
Early Outcomes and Alignment With Organizational Goals
The NHKI has demonstrated early success across the four perspectives of the BSC. Early outputs have also supported several of the hospital’s strategic goals including: delivering safe and quality care, fostering a patient-centred culture, equipping staff with the tools for success, and transforming the workforce. 37 Supporting the first goal, active studies increased from 32 in 2023 to 50 in 2024, enrolling a cumulative total of 1,153 patients over the first 2 years (Figure 2). These outputs reflect improved integration of research into clinical care and expanded patient access to research, reinforcing the hospital’s commitment to evidence-informed care. 37
To strengthen the hospital’s commitment to fostering a patient-centred culture, 37 the NHKI prioritized Patient Experience as an area of research focus and sought to actively engage Patient and Family Partners (PFPs) in research co-design. A dedicated postdoctoral fellow role was created to coordinate a pathway for PFP engagement in research by tapping into the hospital’s established infrastructure for patient partnership through its Niagara Health Engagement Network. The number of PFPs involved in research increased from 6 in 2023 to 13 in 2024. While current engagement levels are encouraging, future plans include the development of a comprehensive organizational framework and the establishment of an NHKI Patient and Family Engagement Committee to guide and expand PFP involvement in research, informed by best practices from other organizations. 38
The NHKI has also helped to support the hospital’s workforce strategy by investing in staff and trainee development, and developing initiatives to attract and retain new graduates. Trainee participation increased from 10 in 2023 to 25 in 2024, including postdoctoral fellows, undergraduate, medical, graduate students, and surgical resident pursuing formal research training (Figure 2). Four undergraduate research scholarships were established in partnership with its local and neighbouring academic institutions, and external funding opportunities (such as the Canadian Critical Care Trials Group Network of Networks 39 scholarships) were obtained to support summer student salaries in 2023 and 2024. Beyond the hospital, the NHKI also created 3 research learning modules to support the development of community hospital clinicians’ research skills, and developed and deliver an annual graduate-level research methods course at a nearby academic institution. Anecdotal feedback has indicated that these efforts have enhanced the hospital’s reputation as a leader in health research and positioned it as an attractive employer for emerging clinicians and researchers.
Beyond advancing the hospital’s strategic objectives, the NHKI has demonstrated strong performance across other key dimensions of organizational value. Financially, the institute has demonstrated early self-sufficiency, with the majority of its revenue coming from external sources while less than 3% was derived from the hospital’s operating budget in fiscal year 2024/2025 (Figure 2). This is largely due to a strong relationship between the NHKI and the hospital foundation internally, and research networks externally. From an internal business perspective, efforts have focused on standardizing research processes and developing policies, which have set the stage for the continued growth and will remain a focus for the coming years. Additionally, infrastructure expansion has supported the addition of three new clinical research programs in neurology, hematology/transfusion medicine and infectious diseases, increasing the total number of clinical research programs to 8 (Figure 2).
The NHKI has also achieved success in academic dissemination, contributing to 72 publications from 2023 to 2024 and hosting 4 knowledge dissemination events (2 internal, 1 regional, and 1 national), strengthening its growing national and international presence and collaborative potential. However, limitations in tracking outputs persist. Some clinician-investigators may not list Niagara Health as their primary affiliation, and no centralized system exists to capture all conference presentations. Moreover, challenges remain in centralizing siloed research programs that predated the NHKI’s establishment.
Discussion
This paper describes the development and early evaluation of a nascent research institute embedded in a community hospital in Southern Ontario. Previous literature highlights core principles for strengthening organizational research capacity, including collaboration development, research prioritization, academic dissemination, embedding research within organizational structures, and securing sustained organizational and financial support.29,31 While not specific to community hospital settings, many of these strategies parallel those implemented in establishing the NHKI and align with our group’s earlier work focused on strategies to strengthen research capacity in Canadian community critical care units.4,24 Using the BSC framework adapted to this unique setting, we offer insights for other community hospitals seeking to embed research as a strategic priority. Early successes such as securing external funding through developing strong relationships with the hospital foundation and external research networks, expanding clinical research infrastructure, supporting teaching and learning, and establishing national and international presence through knowledge dissemination, reflect the untapped potential for research to thrive within community hospital settings and contribute more broadly to the organization’s strategic goals.
Formalizing research through the establishment of a research institute has increased patient access to research, fostered new opportunities for PFP engagement, provided training opportunities, and attracted talent and new sources of revenue, advancing broader organizational goals and strategic impact. Existing literature supports the value of integrating research within hospital operations, linking it to improved patient outcomes,6-8 greater staff satisfaction,9,10 and a stronger culture of continuous improvement. 10 Further evidence suggests that embedding research in clinical roles can also improve workforce retention and recruitment, especially in underserved areas.28,40 Collectively, these insights highlight the strategic value of research integration in advancing innovation and capacity within community hospitals. Furthermore, when examining the aforementioned outcomes of research engagement, it is apparent that there is alignment with the quadrants of the original BSC (i.e., financial, customer, internal business, learning, and growth), suggesting that most hospitals would find alignment between the positive outcomes of a research-active organization and their broader strategic plan.
The NHKI’s success in securing external funding from grants, donations, and industry/academic partners, demonstrates that short-term financial support is achievable, even in resource-constrained settings.4,24 However, long-term financial sustainability has not yet been achieved and remains a priority. Grassroots clinician-led efforts to build research capacity through independent clinical programs laid critical groundwork, underscoring the effectiveness of bottom-up approaches to building research capacity in community hospitals. 24 Consistent with existing literature, dedicated operational and systems-level funding remains crucial to ensuring continued growth and sustainability.4,24,41
Internationally, the United Kingdom’s National Health Service demonstrates a successful system-wide integration of research into healthcare delivery, making research a strategic focus across all trusts. 28 Within the Canadian context, community hospital participation in research is growing.42,43 While many of these initiatives are in the early stages of development, a notable example is Trillium Health Partners’ Institute for Better Health (IBH), now in its 11th year. 44 IBH’s success is reflected in its recognition as one of Research Canada’s Top 40 Research Hospitals 45 ; an impressive achievement for a community hospital competing among primarily academic and research-focused organizations. A key factor in scaling their capacity is their partnership with their hospital foundation, which secures philanthropic funding to provide salary support for embedded researchers. While IBH is just one example, its success illustrates the potential for community hospital-based research institutes with sustained investment and organizational commitment.
The BSC framework has proven valuable in evaluating NHKI’s progress holistically, capturing both tangible outcomes and essential early-stage activities. However, there is a need for standardized metrics for evaluating research performance tailored to community hospital settings. Traditional indicators such as publications, grant funding, research spending, and recruitment rates are useful for cross-organizational comparisons and board-level reporting. 31 Yet, in early-stage resource-limited environments like community hospitals, foundational milestones such as infrastructure development, staffing, policy creation, and other key RCB activities 29 are equally important and were therefore incorporated into our BSC. Future metrics should capture the impact of research on patient experience, collaboration across departments, and integration into practice. 28 Consensus on these indicators would improve benchmarking and inform system-wide learning and targeted investment.
Conclusions
Our reflection on the development and early evaluation of the NHKI demonstrates the organizational benefits of integrating research into the operations and strategic priorities of a community hospital. Using the case of the NHKI, this article introduces a novel application of the BSC tailored to this unique context, providing a practical framework to guide the implementation and evaluation of research programs in similar settings. While this work offers a useful starting point for other community hospitals aiming to establish or strengthen research as a core function, future research should refine this framework, test it in diverse community hospital settings, and identify additional indicators to evaluate performance and sustainability. Another consideration is to apply the LEADS framework when approaching community hospital research capacity building by incorporating the 5 domains (lead self, engage others, achieve results, develop coalitions, and systems transformation). As we strive towards building more equitable LHSs across Canadian hospitals, the integration of research into community hospitals is a critical step forward.
Footnotes
Acknowledgements
The authors would like to acknowledge Jessica Thompson for assisting with data visualization and graphic design.
Ethics Considerations
Institutional Review Board approval was not required.
Funding
The authors disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: The establishment of the Niagara Health Knowledge Institute was supported by a donation from the McCall MacBain Foundation.
Declaration of Conflicting Interests
The authors declared the following potential conflicts of interest with respect to the research, authorship, and/or publication of this article: Kian Rego is a Research Coordinator at the Niagara Health Knowledge Institute. Elaina Orlando is the Research Manager of the Niagara Health Knowledge Institute. Gail Riihimaki is a Patient Partner and a Member of the Quality and Patient Experience Committee of Niagara Health. Harpreet Bassi is the Executive Vice-President, Strategy and Communications and the Executive Lead Research and the Niagara Health Knowledge Institute at Niagara Health. Jennifer Tsang is the Executive Director and Chief Scientist of the Niagara Health Knowledge Institute. She has received research grants from Canadian Institutes of Health Research and Physicians’ Services Incorporated Foundation, not related to this work.
