Abstract
Emergency Departments (EDs) have faced mounting pressures in recent years as greater volumes of patients seek care, many with increasingly complex clinical and social needs. However, the potential contributions of rehabilitation professionals to help alleviate these pressures in the ED are not well understood or leveraged. To address this knowledge gap, the authors conducted a literature review of rehabilitation models of care and the impact of rehabilitation professionals in the ED, as well as an environmental scan to understand rehabilitation models of care across two large regions in Ontario. This article outlines these findings, as well as future opportunities related to leading care and patient flow practices based on rehabilitation models in the ED.
Introduction
Emergency Departments (EDs) across Ontario are facing unprecedented pressures. 1 Multiple factors have contributed to the current ED crisis; prior to the COVID-19 pandemic, Ontario EDs were already under pressure due to an increase in older patients seeking care, many of whom have increasingly complex medical needs. 2 Reduced health human resources in the hospital and community sectors have also contributed to an exacerbation of patient flow challenges out of hospitals and intensified pressures in the ED. Although unique diversion practices have been implemented in some EDs, the evaluation and spread of these diversion strategies are in the early stages. 1 From a patient care perspective, ED overcrowding leads to delayed treatment,3,4 poor patient outcomes, 3 increased mortality, 3 increased inpatient Length of Stay (LOS), 3 and increased exposure to error. 3
Physiotherapists (PTs) working in the ED primarily assess the mobility and function of patients with musculoskeletal injuries and older adults with frailty. Intervention includes determining the most effective plan to facilitate safe discharge home and recommending and/or educating the patient on the use of mobility aids, if needed. 5 Occupational Therapists (OTs) in the ED assess patients’ cognitive abilities, functional mobility, and transfers and then recommend ideal discharge locations based on how patients are able to engage safely with activities they need to do at home. 6
A recent Ontario Health operational guidance document recommended that acute care hospitals consider staffing EDs with rehabilitation professionals to avoid acute care admissions or mitigate functional decline in patients who are admitted, but for whom no bed is available on an inpatient unit. 7 However, models of care that include rehabilitation professionals as staff who are dedicated to working in the ED have not been widely implemented. To identify potential opportunities that enhanced rehabilitation staffing in EDs could offer, the authors undertook a comprehensive literature review on this topic and conducted an environmental scan in the fall of 2023 to better understand current rehabilitation models of care across nineteen EDs.
Literature review on physiotherapy and occupational therapy in the emergency department
A comprehensive literature review focused on OT or PT in the ED was conducted with the assistance of a librarian based on review articles from 2012 and primary source articles from 2018. Due to a dearth of high-level evidence in the OT literature, the search for literature on OT in the ED was extended back to the year 2000. In addition, to establish a timeline of when research in this area of practice started and grew, the authors also captured the volume of OT or PT ED articles by decade.
The literature worldwide reflecting rehabilitative care in the ED started in the 1960s for PTs and in the 1990s for OTs. Based on a Medline search, PT literature specific to the ED setting worldwide since 1990 was almost ten times greater than OT literature for the same time period. In Canada, the peak growth in the volume of literature for both professions in the ED occurred over the last decade (2010-2019).
The body of literature focusing on the impact of OT or PT in the ED falls into three main categories: 1. Physiotherapists taking on an enhanced role in the ED for musculoskeletal conditions. 2. Occupational therapists and/or physiotherapists providing comprehensive geriatric assessments as part of an interprofessional team. 3. Occupational therapists and physiotherapists, evaluated as discrete professions, working within their scope of practice.
Enhanced physiotherapist role in the emergency department
Different terminologies were observed in the literature describing the roles of physiotherapists in the ED, including “advanced practice,” “extended scope,” “primary contact,” “first contact,” and “direct access.” In these models, PTs do not require a referral from a physician to assess patients; they have a higher level of responsibility and engage in activities for which training comes from outside of traditional PT practice (e.g., diagnostic imaging and pharmacology).8,9 The use of these various models and terminologies is based on jurisdictional differences in the scope of practice for PTs. For the purposes of this article, these models will be described as enhanced PT roles. These enhanced models of care for PTs in the ED were not found in the OT literature. However, it should be noted that in Alberta, OTs may perform restricted activities such as setting or resetting a fracture for the purpose of splinting, applying fracture braces and performing cranioplasty, reducing dislocation of a joint, and administering diagnostic imaging contrast agents. 10
The body of literature focused on the enhanced PT role in the ED has flourished in the United Kingdom and Australia. In these countries, the enhanced role is specific to the assessment and treatment of patients with low urgency musculoskeletal conditions with no fractures, such as low back pain and neck pain. In Canada, a consistent team of researchers in the province of Quebec has also been conducting research in this area.8,11–15 This body of literature has produced strong levels of evidence supporting the positive contribution of the enhanced PT role to the healthcare system. A few recent high-level evidence publications on the impact of the enhanced PT role are listed in Table 1. Here are some highlights: - The literature indicates that enhanced PT roles in the ED have had a positive impact on: • Patient flow: shorter wait times in ED,16-20 shorter LOS in ED,17-20 and fewer hospital admissions.
19
• Patient care: improved access to care,16,21 improved quality of care,
21
no adverse events or patient complaints,
17
returned less often to ED,
13
received more timely analgesia,
18
lower levels of pain,
13
and used fewer prescription medications.
13
• Provider experience: reduced workload of other clinicians.
16
- Matifat and colleagues
15
established that there was very good diagnostic agreement between a team of advanced practice PTs and a group of emergency physicians. In addition, moderate agreement was found in advanced practice PT discharge planning practices as compared to ED physicians.
15
- Based on three review studies, the cost analysis outcomes of advanced practice PT roles are currently inconclusive due to methodological heterogeneity.14,16,22 However, there are two studies currently underway in Canada focused on this topic: one in Quebec and a multi-centre study across three provinces: Quebec, Ontario, and Alberta.11,12 Literature review summary.
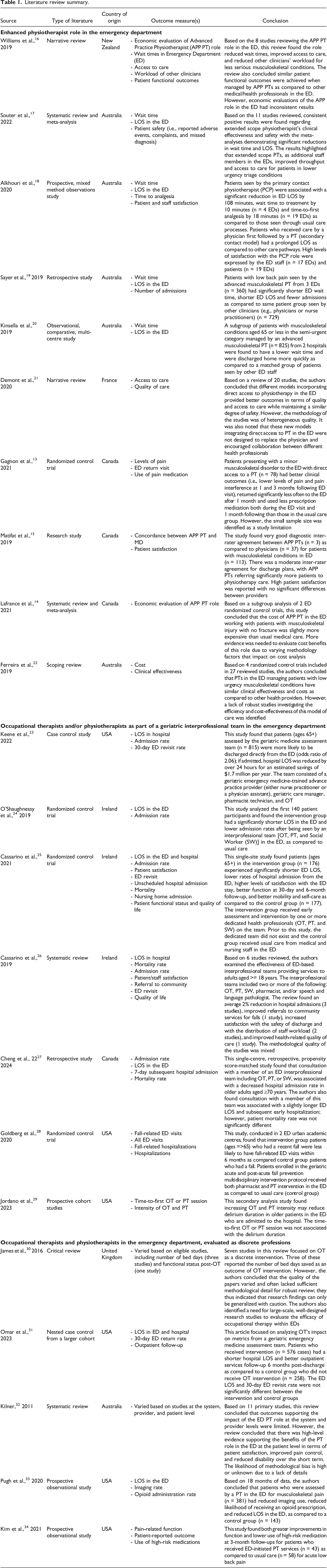
Occupational therapists and/or physiotherapists as part of a geriatric interprofessional team in the emergency department
This area of research, mostly from Ireland and the United States, also presents strong levels of evidence supporting the benefits of either OT, PT, or both professions as part of a team working with older adults in the ED.
Evidence indicates that including rehabilitation professionals as part of the interprofessional team contributed to cost savings through a reduction in length of hospital stay
23
and had a positive impact on: - Patient flow indicators: decrease in ED LOS,24,25 decreased rate of hospital admission,23,25-27 decrease in hospital LOS,
23
and lower likelihood of ED revisit due to a fall.
28
- Patient and provider experience: high patient satisfaction for the ED visit,
25
high patient and staff satisfaction with safety of discharge,
26
and high staff satisfaction on workload distribution.
26
- Patient care: improved referrals to community services for patients post-fall,
26
better function at follow-up,
25
better quality of life at follow-up,25,26 and reduction in delirium duration for admitted patients.
29
Details of the publications are summarized in Table 1.
A recent randomized control trial design evaluating the role of PT and OT in the ED and patients’ transition to home is noteworthy. This study compares three models of care: usual care with no dedicated interprofessional team in the ED, a comprehensive geriatric assessment in the ED involving an interprofessional team with OT and PT, and a comprehensive geriatric assessment model with an interprofessional team in the ED, in addition to 6 weeks of follow-up including PT and OT visits or phone calls (i.e., ED Plus). 35 Although the full study results have not yet been published, the transition to home from the ED model of care, including a self-management program at home involving interprofessional rehabilitation professionals, has demonstrated promising preliminary outcomes on patients’ mobility and quality of life, with decreased ED revisits and rehospitalization. 36
Occupational therapists and physiotherapists in the emergency department evaluated as discrete professions
Most of the recent outcome studies on OT or PT roles in the ED were from lower level evidence, primary studies. The quality and focus of publications for OT roles in the ED were varied and often lacked sufficient methodological details for a robust review; therefore, findings reported should be taken with caution. 30 These included: bed days saved, 30 shorter hospital LOS, and better outpatient follow-up at 6 months post-discharge. 31
A systematic review study on PTs in the EDs that were not enhanced roles concluded positive patient-level outcomes related to high patient satisfaction, improved pain control, and reduced disability. 32 The PT role in the ED was also associated with shorter LOS in the ED, 33 lower use of high-risk medication for low back pain, 34 fewer opioid prescriptions for musculoskeletal pain, 33 and less imaging. 33
Details of the studies are summarized in Table 1.
Regional rehabilitation models of care in the emergency department
Participating hospitals by Ontario health region.
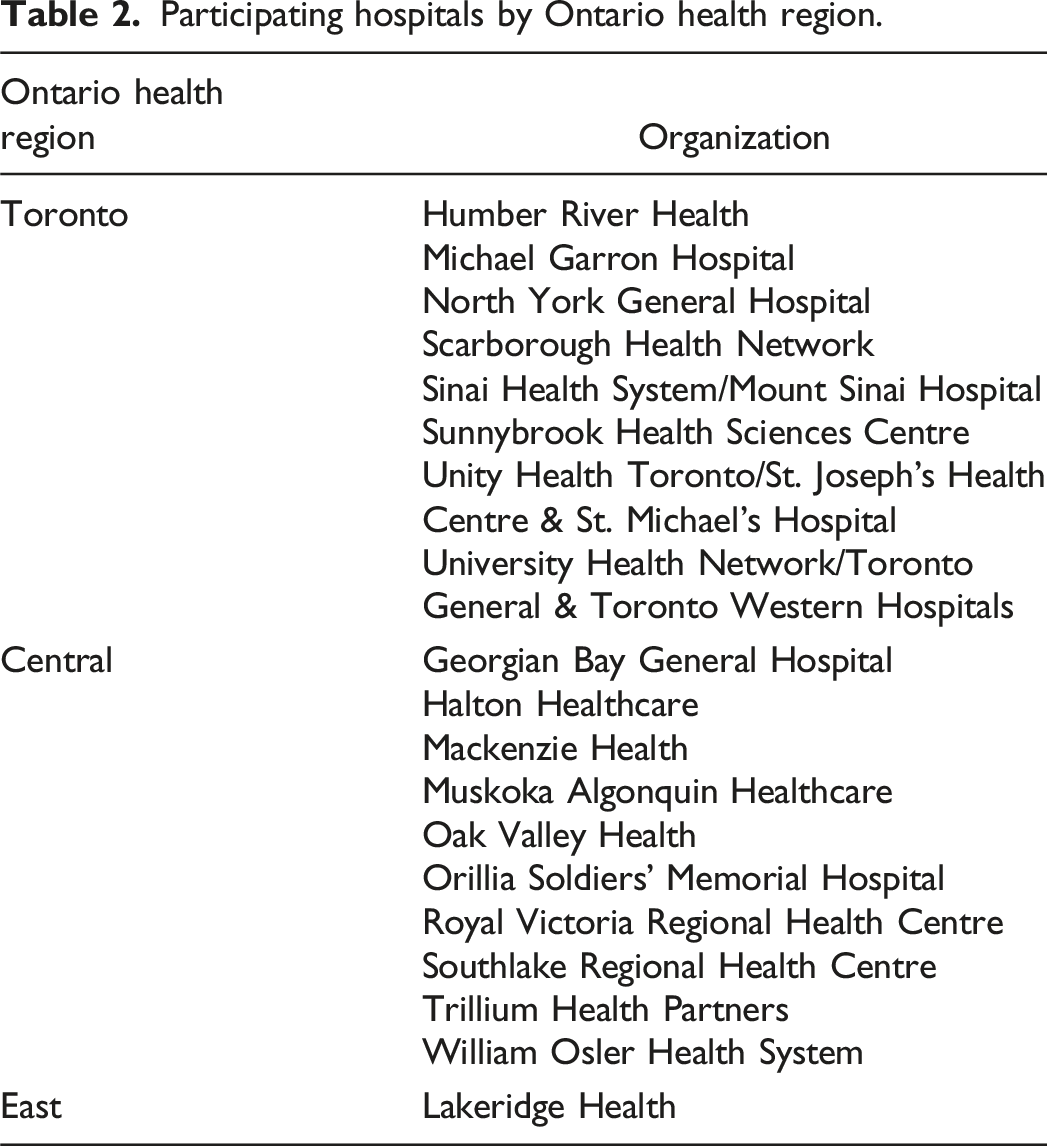
Program goals
Staffing the ED with rehabilitation professionals was for (1) admission diversion only and/or (2) initiating assessment and/or treatment of admitted patients waiting in the ED for an inpatient unit bed. The focus of rehabilitation professionals in the ED for the purpose of admission diversion was to identify patients who could functionally manage in the community with supports (e.g., at home) or be directly admitted to inpatient rehabilitative care if there were no acute medical issues to be addressed. For those patients who were admitted and awaiting an inpatient bed in the ED, rehabilitation professionals not only focused on initiating a functional status assessment but also on preventing functional decline and hospital-acquired conditions such as pressure ulcers or delirium. Anecdotal comments from those interviewed indicated that early assessment and intervention in the ED resulted in shortened lengths of stay on inpatient units, and/or being able to discharge patients directly from the ED.
Rehabilitation staff and operations
Variability was observed in which professions provide services in the ED, how integrated the rehabilitation role is with other staff in the ED, and the hours the ED is staffed with rehabilitation professionals. For multi-site organizations, the rehabilitation staff model may also differ within the same organization. In the majority of the organizations interviewed, physiotherapy tended to be the rehabilitation profession dedicated either full-time or part-time in the ED, particularly if the organization’s primary program goal was admission avoidance. Speech-language pathologists in the ED were identified by only a few organizations and their role was primarily to provide consultation for admitted patients who had experienced a stroke.
Organizations with rehabilitation staff covering the ED on either a consultative basis (i.e., without a dedicated full-time equivalent [FTE]) or dedicated part-time with less than 0.5 FTE consistently identified more challenges in keeping up with the referrals, especially with the current ED pressures. The amount of time rehabilitation staff could see patients in the ED was correlated with the development of their role in this setting and their ability to develop relationships with other ED team members and leaders, which were reported to enhance the interprofessional approach to patient care.
Observed models of care based on categories.
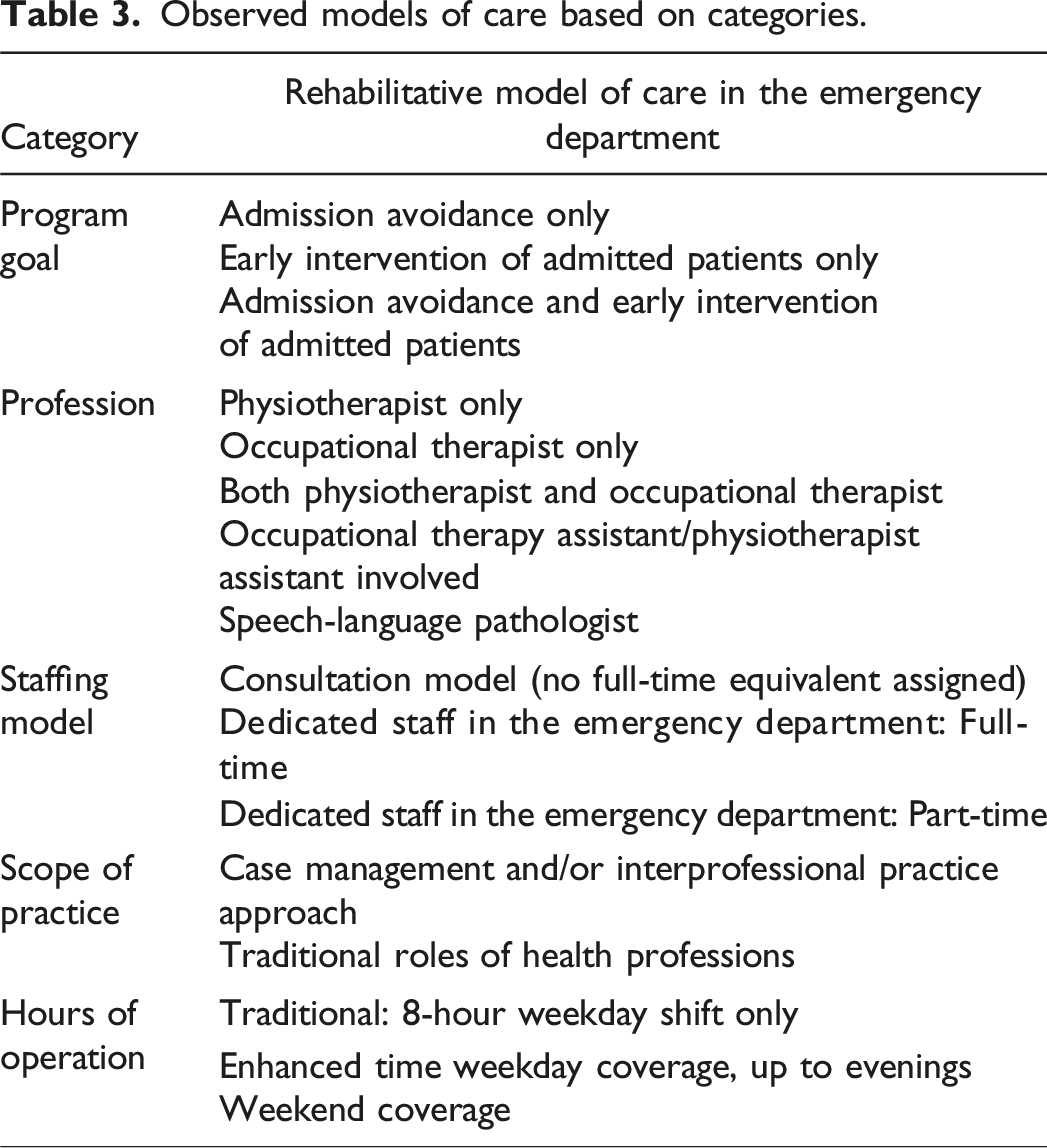
Lessons learned in emergency department rehabilitation role implementation
Key lessons learned related to the implementation of rehabilitation roles in the ED included: - Clarity in roles of OT, PT, or occupational therapy assistant/physiotherapist assistant: This process may involve ongoing iterative education of all team members and a sustainability plan in addressing role clarity. - Importance of relationship building with ED team members and external partners: This is also an intentional, ongoing process. Appreciation of the value each rehabilitation profession can contribute in the ED requires that their roles be integrated within the ED team and care processes. - Physical environment in the ED: Existing EDs are generally not designed for older adult mobility intervention. A lack of equipment storage and the loss or misplacement of mobility aids were also identified as challenges.
Evaluation and measuring impact
The majority of organizations interviewed that had recently implemented a rehabilitation role in the ED measure the impact of this change by monitoring referral volumes, attendances of rehabilitation professionals and the number of patients admitted or redirected from the ED. Since the interviews were conducted, some organizations monitoring metrics have reported further investments in OT and/or PT coverage in the ED, which reflects the organization’s appreciation of the rehabilitation role’s contribution. For those organizations with longstanding rehabilitation staffing in the ED, quantitative metrics are no longer collected as there is recognition of the value of having dedicated rehabilitation staff in the ED. There is currently no regional strategy to evaluate the impact of OT or PT roles in the ED.
Opportunities
As mentioned, Ontario EDs face significant pressures due to higher numbers of older adults with more complex needs seeking care and waiting for inpatient beds. 37 The risks, and even dangers, for older adults within acute care hospitals are clear. Among them are deconditioning, one of the most common reasons for delayed discharge from acute hospitals, 38 and prolonged immobility associated with a decline in muscle strength and muscle mass, as well as in physical and cognitive function.39,40 This highlights the importance of early, targeted rehabilitation intervention, which can reverse functional decline in older adults associated with acute hospitalization 41 and can expedite their discharge, as higher levels of mobility are associated with shorter lengths of stay. 42
Given these system pressures and risks for older adults seeking care, there is an opportunity for government to develop policies and funding incentives such as the Pay-for-Results program in the ED 43 that will encourage health service provider organizations to develop alternate models of rehabilitative care in EDs that can help alleviate capacity pressures and assist older adults and others in continuing to live well in the community. Based on findings from the environmental scan and literature review, promising models that should be further explored include enhanced roles for rehabilitation professionals, in which they do not require a physician’s referral to assess patients, have a higher level of responsibility, and engage in activities beyond traditional PT and OT scope of practice; and the “transition to home” model in which OTs and PTs are part of a geriatric interprofessional team in the ED and support time-limited follow-up after ED discharge with a self-management program at home.
Rehabilitative professionals in the ED, as additional members of the interprofessional team, have evolved as ED programs are designed to better manage patient flow. These professionals, with promising impacts on patient flow, patient care, and provider experience, complement the skill mix of other professions in the ED. Dedicated rehabilitation staff should be considered as part of a broader strategy to address patient needs efficiently and effectively while helping to alleviate pressures on EDs.
Footnotes
Acknowledgements
We would like to thank Emilia Main, librarian at the University Health Network, for assisting with the literature review search, and Laura Glynn, for proofreading this article.
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Ethical approval
Institutional review board approval was not required.
