Abstract
This scoping review sought to identify the barriers and enablers to implementing environmentally sustainable practices in healthcare, as well as propose a multi-phased approach to enable such implementation. The three concepts guiding the search were (1) environmental sustainability; (2) healthcare; and (3) barriers or enablers. The PRISMA checklist for scoping reviews was used to guide this search. A total of 16 articles were included and reviewed for data extraction. While most articles focused on healthcare in general, dentistry and surgery were the most recurring clinical areas of focus. Barriers and enablers were related to the individual (e.g. knowledge, skills, and attitude), institutional (e.g. budget, strategy, and readiness), geographical/infrastructural (e.g. infrastructure and public awareness), political (e.g. regulations and incentives), and other (e.g. patient awareness and knowledge). A key enabler identified was having transformational leadership with a clear vision and collaborative approach.
Introduction
Growing global challenges served as a key impetus for the increased importance placed on integrating environmentally sustainable practices across many sectors, including healthcare.1,2 The latest estimates suggest that healthcare accounts for ∼4-6% of global greenhouse gas emissions with most stemming from scope 3 emissions (e.g. supply chains). 3 The United Kingdom’s national health service is the largest public sector greenhouse emitter 3 and in the United States, 4 approximately 8.5% of all greenhouse gas emissions are due to healthcare system activities. While climate change has been widely positioned as a detriment to the planet, humans are evidently not immune with non-optimal temperatures being associated with substantial mortality burden. 5
While the United Nations’ Sustainable Development Goals have set a clear direction for countries, 6 it has become evident that achieving these goals will only be possible through concerted efforts by all key stakeholders, including the private sector. 6 An increasing number of companies are disclosing their sustainability or ESG (environment, social, and governance) practices with various initiatives and organizations aiming to standardize different areas of reporting (e.g. taskforce on climate-related financial disclosures, carbon disclosure project, science-based targets initiative, and the global reporting initiative).7-10 Overall, sustainability is gaining momentum in the business world for various reasons such as physical (e.g. floods and droughts) and transitional risks (e.g. regulations) related to inaction on climate change issues. 7 Moreover, while results are mixed, some studies suggest that companies that score higher on ESG experience lower risks, higher financial returns, and lower return volatilities.11-15
From an ESG perspective, the healthcare sector is perceived as more adept on social aspects (e.g. reducing inequality in healthcare access by implementing innovative technology), but still lacking on the “E” and the “G” principles.1,2 Nonetheless, given the mounting evidence for the impact of climate change on individual and population health, the healthcare sector (both public and private providers) is increasingly placing an emphasis on integrating environmentally sustainable practices in their delivery of care.1,16-19
To successfully enable the healthcare sector in adopting and achieving its environmental goals, it is important to map the complexities that these facilities encounter. This is particularly important in the wake of the challenges that health systems around the world had to overcome due to the recent COVID-19 pandemic. Identifying the factors associated with the success or failure of environmentally sustainable practices in healthcare could prevent wasted investments. As such, this scoping review sought to identify the barriers and enablers for adopting or achieving environmentally sustainable practices in healthcare settings. This study leverages the factors identified through the review to propose a roadmap to implementing environmentally sustainable practices in healthcare.
Materials and methods
Eligibility criteria
The three main overarching concepts that guided this search were (1) environmental sustainability; (2) healthcare; and (3) barriers or enablers. Articles that were included in the review were those that (1) considered the adoption or achievement of environmentally sustainable practices in healthcare, (2) focused on healthcare organizations (irrespective of their size and type, such as a clinic or hospital), (3) provided insights on the barriers and enablers for integrating environmentally sustainable practices, and (4) were written in English or French. Exclusion criteria were articles that (1) focused on the social or governance aspects and (2) focused on an industry other than healthcare services (e.g. pharmaceuticals). To allow for a wide array of results to be included, quantitative, qualitative, and mixed-methods studies or reports were eligible for inclusion.
Although this scoping review does not entail quality assessment of included studies, it follows a sound methodological approach to map out the results in a concise manner for knowledge users. This scoping review follows the 2018 checklist developed by Tricco et al. for reporting scoping reviews. 20 Due to the nature of this article, ethics approval was not required.
Information sources and search
This scoping review systematically searched citation databases (i.e. Medline (Ovid), Scopus, CINAHL (EBSCO), ProQuest One Business, and Web of Science) and the grey literature (i.e. Google Scholar). The citation databases were selected based on their scope and relevant aspects covered. The final search strategy for each data source was defined and refined with the assistance of a librarian and was finalized on October 12, 2022. For replication, an example of the search strategy for Medline (Ovid) can be found in the Supplementary material. The results were exported into Zotero for screening.
Selection of sources of evidence
Once duplicates were removed in RefWorks, the screening process involved three researchers. The decision tree in Figure 1 was used as a guide to screen titles and abstracts. Articles that were extracted from the title and abstract screening stage were read in their entirety. Uncertainties and discrepancies were discussed by the three researchers and disagreements were resolved through consensus. Following the full-text review, the references of included articles were screened for additional relevant articles. Decision tree for article inclusion.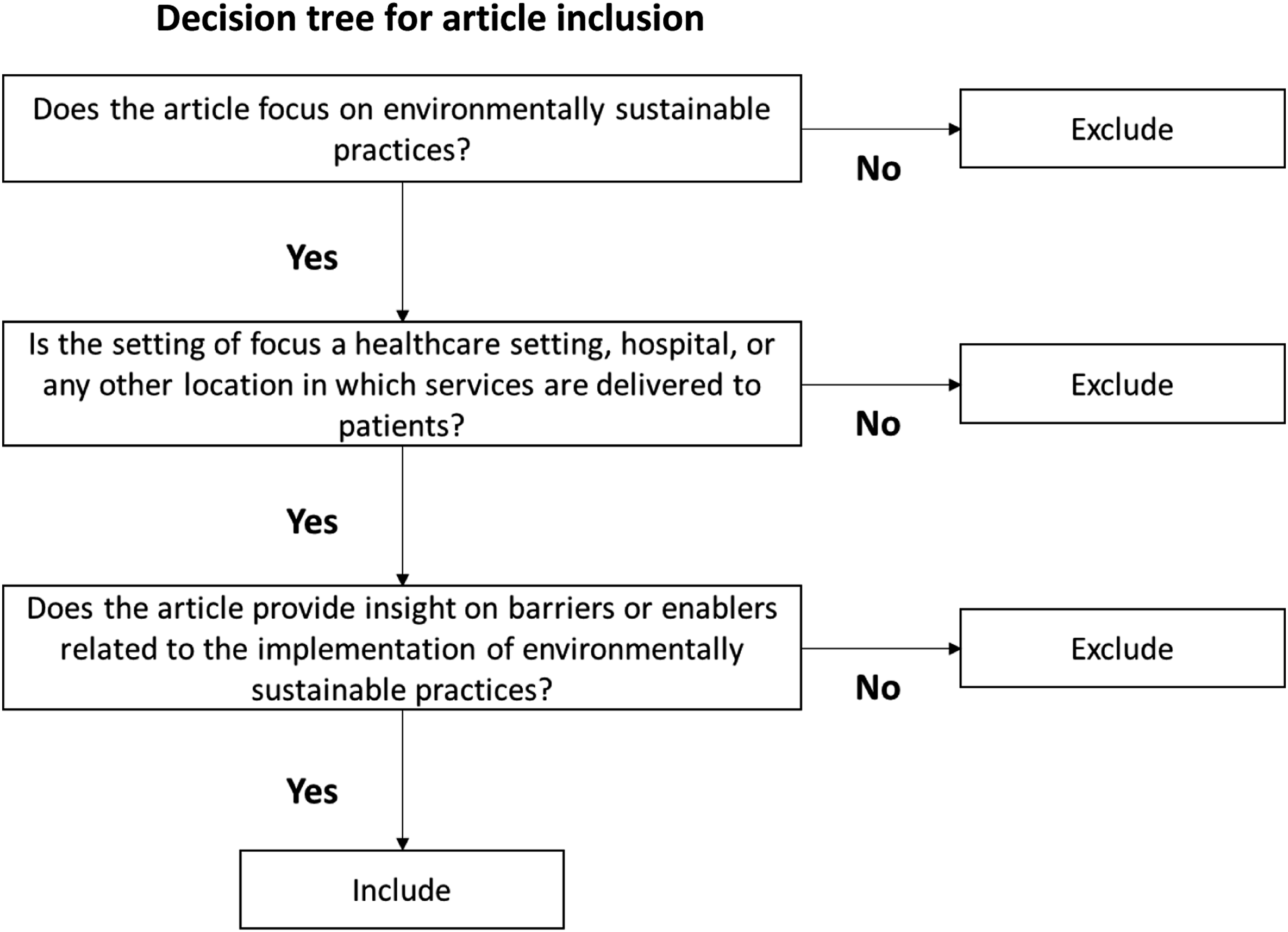
Data charting process
Once the final number of articles was determined, a scan through the articles allowed the research team to gain a high-level understanding of the topics of interest in which environmental sustainability factors were being integrated in healthcare. A key focus on barriers and enablers was outlined in the data charting form which was pre-tested with the same five articles across two researchers to assess consistency in data extraction.
Data extraction
The variables collected through the data charting form included the following where applicable: country, year of publication, study design and summary, and key results.
Synthesis of results
Scoping reviews provide knowledge users with a concise overview on the literature available on a given topic of interest. Given the heterogeneity of the studies included in this review, data were groups based on the key objective of this review which focused on barriers and enablers. Tables were used to provide an overview on the types of articles found in the literature and the data extracted from each article. A thematic synthesis focused on barriers and enablers was used to outline key factors in the literature and other considerations.
Results
Selection of sources of evidence
Figure 2 depicts the flow chart, which illustrates the selection process at each screening step. Our search identified a total of 3,465 from which 530 were duplicates. A total of 2,935 titles and abstracts were screened from which 2,801 were excluded based on relevance and eligibility criteria. A total of 134 full-text articles were retrieved and assessed for eligibility. Of these, 113 articles were excluded for the following reasons: considered sustainability in terms of longevity and not related to the environment, did not focus on healthcare services, provided an overview of opportunities rather than enablers or barriers, or did not cover enablers and barriers. Five additional articles were excluded because it was not possible to retrieve them. This resulted in a total of 16 articles for inclusion.20-35 Inter-rater reliability was assessed at the full-text stage which resulted in a score of 82% between the three reviewers. Discrepancies in article selection were mostly related to differencing perspectives on what constitutes a barrier or enabler. These discrepancies were discussed as a research team and resolved through consensus. Flow chart of the screening process.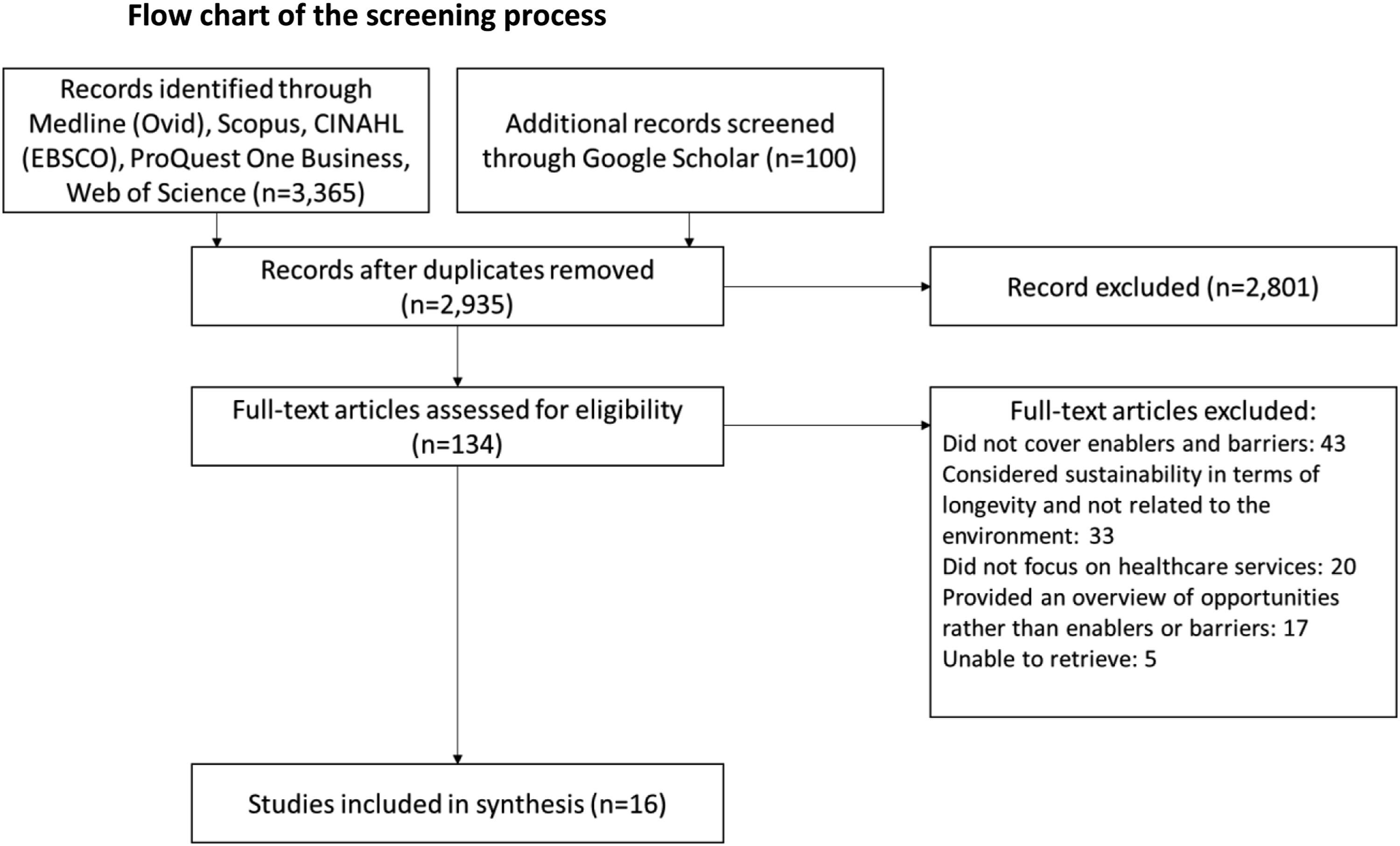
Article characteristics
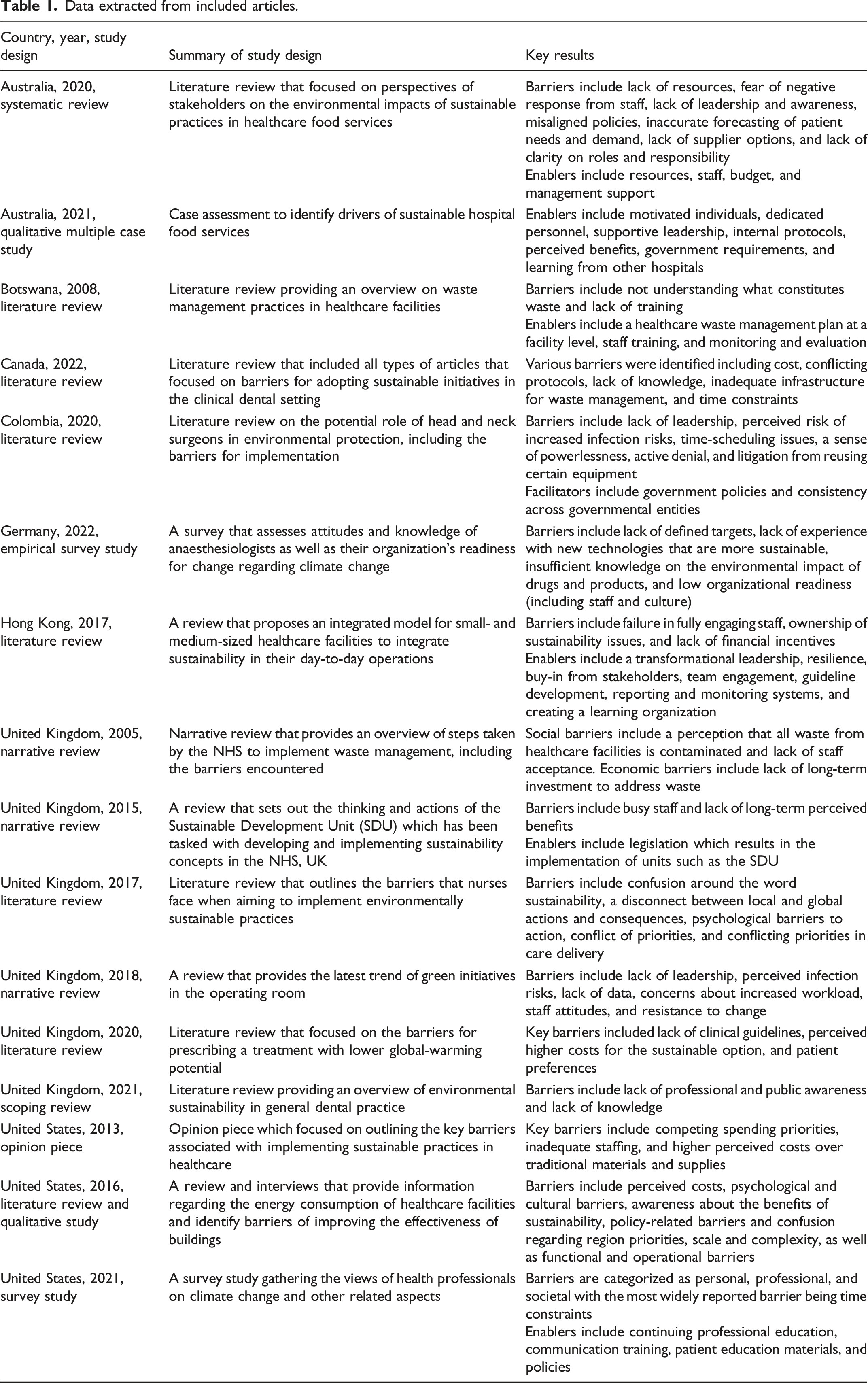
Data extracted from included articles.
Barriers and enablers
Many more barriers were identified as compared to enablers. In some cases, the barriers were naturally the opposite of the enablers to implementing environmentally sustainable practices in healthcare. Identified factors could be categorized at the individual, institutional, geographical/infrastructural, and political levels. It is noteworthy that a common theme across articles is the key importance of a top-down approach in successfully implementing sustainable practices in healthcare. While health professionals are ultimately the ones implementing such practices, the institution in which they work needs to enable these practices through structural and operational changes or levers.
Barriers and enablers to implementing environmentally sustainable practices in healthcare.

It seems that most barriers are at the institutional level as institutions play a critical role in the success or failure of sustainable practices. Healthcare organizations set the vision, strategy, and key objectives; as such, if environmental sustainability is not part of the vision or is not part of a clear strategy, successful implementation of these practices will not be possible. A recurring theme across articles is that the onus should not be on health professionals to make a practice a success; rather, the institution in which they work should allow for environmentally sustainable practices to be second nature. This would address, for example, a barrier found in a study in which junior staff were following non-environmentally sustainable practices to avoid disturbing existing group culture. 21
It is important to note, however, that without addressing barriers encountered at the individual level, well-intentioned institutions will not be successful. 35 It seems that health professionals regard their primary role to be, naturally, patient care rather than environmental sustainability. When considering all potential barriers encountered at the individual level, it seems that a successful practice would be one that would not require much time from the health professional, is easy to implement, is in line with clinical practice guidelines, and has clear benefits for the environment; all while allowing the provision of quality care to patients and respecting patient preferences. Having a well-structured incentive framework in place would also support in promoting desirable practices. 29
In addition, the geographical location in which the health organization operates will have an impact with those in developing countries that lack certain infrastructure being the most vulnerable to unsuccessful environmental practices. 35 For example, waste management requires an infrastructure that stems beyond the health organization to ensure that segregated or recycled waste are treated appropriately at the municipal level. While organizations can be involved in building the required infrastructure, buy-in from municipalities is required.
At the government level, there are many levers that could be implemented to support organizations in their transformations. Developing and implementing a performance framework for environmental sustainability would encourage healthcare facilities to transform their operations. For example, rather than only monitoring the number of patients serviced, the amount of greenhouse gas emissions emitted per patient could be another outcome on which hospitals are assessed and rewarded. These policies would incentivize organizations to invest the required resources, time, and budget to implement environmentally sustainable practices.24,33
Other factors that could impede environmentally sustainable practices are clinical practice guidelines that do not consider or prioritize sustainable products as compared to alternative options. For example, Starup-Hansen et al. found that dry powder inhalers which have lower global-warming potential are not as widely prescribed as compared to pressurized metred dose inhalers. 23 This is mainly due to lack of guidance in prescription guidelines for inhalers, perceived associated costs, and patient preferences. 23 This highlights the importance of considering the role of researchers and organizations that develop clinical practice guidelines. An environmental lens should be considered by these stakeholders to support healthcare settings and health professionals in their vision for environmentally sustainable practices. This, evidently, must be balanced with patient preferences which could be influenced by patient education. While the individual factors mentioned in this article were mostly related to health professionals, patients also play a critical role and should be included in education efforts. 35
Proposed roadmap
Proposed roadmap for implementing environmentally sustainable practices in healthcare.
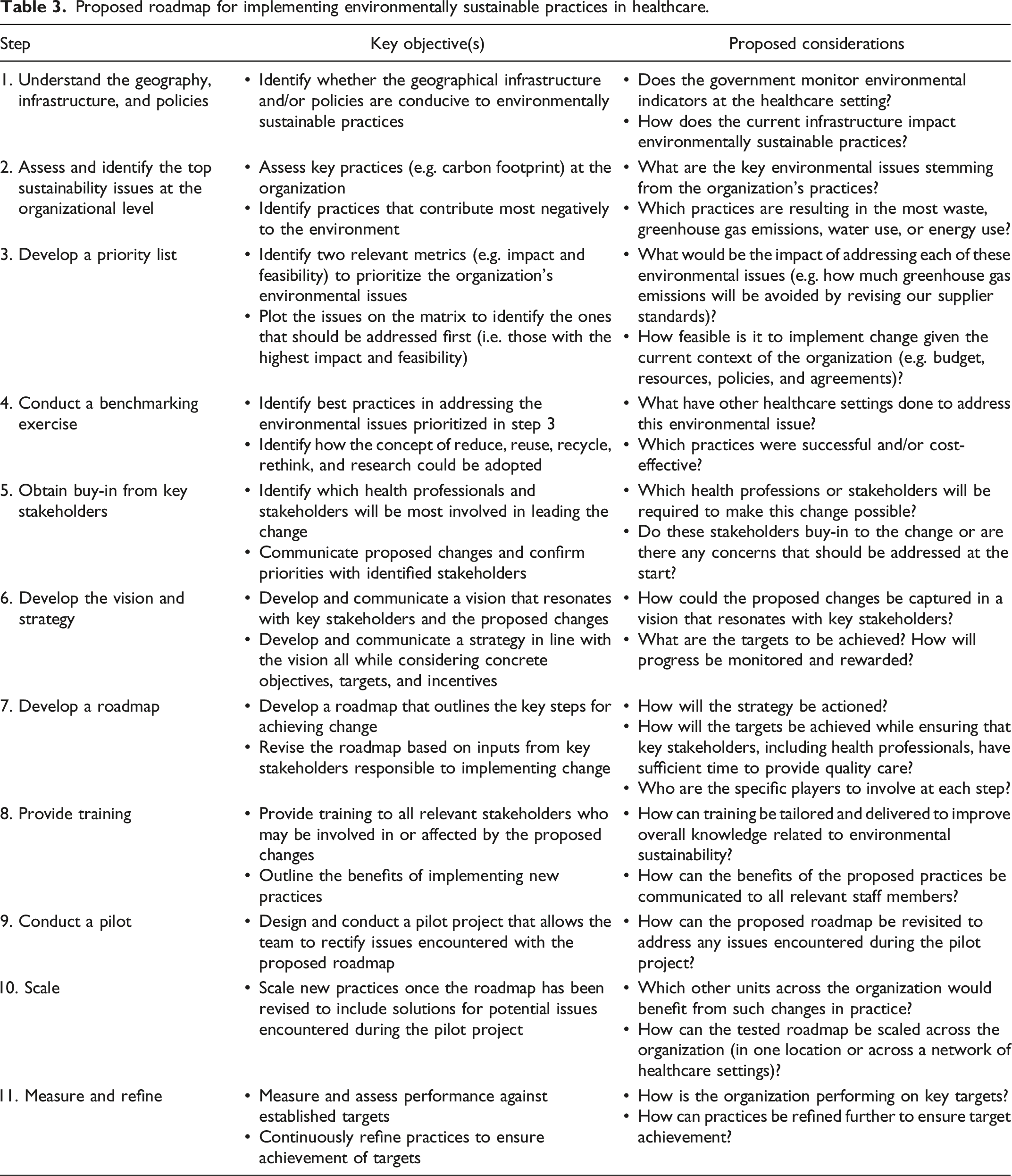

It is important to note that practices which were not prioritized as part of this roadmap should not be disregarded. This is especially the case for practices deemed having high impact but low feasibility. It would be beneficial to identify the factors making the proposed practice unfeasible and work in parallel to help mitigate these barriers.
Additionally, not part of the roadmap is the key role that organizations can play in shaping the infrastructure and policies in their geographical area. Knowledge acquired through implementing new practices could support organizations in championing efforts at the municipality level. For example, if an organization implemented practices related to waste management but the current infrastructure has proven to be obstructive of such practices, concrete examples could be provided to local decision-makers to support wider change.
Additionally, other key aspects to consider are clinical guidelines that shape the practice of health professionals. There should be a bigger emphasis on assessing the environmental impact in addition to clinical effectiveness. This will enable practitioners to prescribe equally effective treatments, but that also have a lower impact on the environment. While this is out of the healthcare settings’ purview, it is possible for organizations to work closely with relevant stakeholders to support this approach.
Discussion
It is evident that there is an increasing interest from and need for organizations to implement environmentally sustainable practices.17,36,37 Scaling healthcare services to improve access without considering environmental impacts may have unintended consequences for populations at large. 38 This scoping review identified some of the barriers and enablers encountered by healthcare settings when implementing environmentally sustainable practices. While most studies focused on practices in healthcare, some clinical areas namely dentistry and surgery were the most recurring focus areas. Overall, it was found that various barriers exist and are related to various levels of the organization and beyond (i.e. individual, institutional, geographical/infrastructural, political, or other).
Individual-level barriers were mostly related to competing interests, lack of time and knowledge, and attitudes towards climate change. At an institutional level, lack of leadership and strategy, incentives framework, and buy-in from key stakeholders hindered successful implementation. At a broader level, lack of policies and infrastructure supporting transformational change impede a healthcare setting’s willingness to implement environmental sustainability practices. Patients and organizations developing clinical practice guidelines also play a role in implementation success. Conversely, enablers identified in this review were primarily related to having a transformational leadership style that fostered a collaborative approach and prioritized engagement from all key stakeholders. Unlike other leadership styles, transformational leadership allows for consensus between the leader and followers intending to work collaboratively in the realization of a goal. 39 Factors found to influence transformational leadership are idealized influence, inspirational motivation, intellectual stimulation, and individual consideration. 40 Specifically, environmentally specific transformational leadership is gaining traction due to its focus on an organization’s performance on environmental aspects. 41 More empirical studies and case studies are needed to further understand the role of this leadership style on environmental outcomes.
Currently, the success of healthcare initiatives is being studied individually for each healthcare setting which could be cumbersome to replicate.17,36,38 This scoping review suggests synthesizing the literature is continuously needed to reduce redundancy, identify best practices, and translate findings into practice. To our knowledge, this is the first review to focus on the barriers and enablers across all medical specialities. Similar reviews are available, but they focus on specific medical specialities (e.g. dentistry). Nonetheless, the overarching takeaway from this review resonates with other reviews; that is, implementing environmentally sustainable practices is impacted by multiple factors that extend beyond healthcare systems. Importantly the role of leadership in addressing environmental issues cannot be overstated. 19
The practical implication of this review includes the proposed multi-phased approach which was informed by the factors identified. While this roadmap targets healthcare settings, policy-makers and researchers should consider it when developing policies and researching relevant topics of scientific inquiry. Policy-makers should specifically assess approaches to address the barriers outlined in this review while considering the potential unintended consequences. Researchers should collaborate at national and international levels to ensure that learnings are shared. Importantly, leaders in healthcare settings should consider the uniqueness of each healthcare setting when aiming to implement the proposed roadmap.
There are some limitations that warrant mention. First, this review focused on healthcare settings thus omitting other greenhouse gas emitters in the healthcare sector such as pharmaceutical companies. Future empirical studies are needed to explore other clinical areas within healthcare that significantly emit greenhouse gases. Moreover, most studies included in this review explored barriers and enablers as a secondary objective; as such, future studies are needed to explore this topic as a primary objective.
Conclusions
Various barriers to implementing environmentally sustainable practices were identified and should be considered by healthcare settings when developing strategies and action plans. A focus on leadership should be prioritized for implementation success. More research across clinical areas is needed to identify practice-specific barriers and enablers of relevant environmentally sustainable practices. In the meantime, healthcare organizations may benefit from adopting and adapting a multi-phased approach that considers the barriers and enablers identified in this review. In the longer-term, policies (at all governmental levels and organization level) and regulations (at national or provincial levels) will be key in creating an environment that is conducive to successful healthcare transformation.
Supplemental Material
Supplemental Material - Barriers and enablers to implementing environmentally sustainable practices in healthcare: A scoping review and proposed roadmap
Supplemental Material for Barriers and enablers to implementing environmentally sustainable practices in healthcare: A scoping review and proposed roadmap by Stephanie Aboueid, Menilek Beyene and Teeyaa Nur in Healthcare Management Forum
Footnotes
Acknowledgements
The authors want to acknowledge the contribution of the librarian, Marie-Cécile Domecq (University of Ottawa, Faculty of Medicine), for their assistance in developing the search strategy for this review.
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Ethical approval
Institutional Review Board approval was not required.
Disclaimer
At the time of publication, Dr. Aboueid is employed by Institutional Shareholder Services Canada Inc., a wholly-owned subsidiary of Institutional Shareholder Services Inc. (“ISS”). This paper presents the authors’ opinions and not necessarily those of ISS, its clients, affiliates, or employees.
Supplemental material
Supplemental material for this article is available on-line.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
