Abstract
Enhancing the use of technology in long-term care has been identified as a key part of broader efforts to strengthen the sector in the wake of the COVID-19 pandemic. To inform such efforts, we convened a series of citizen panels, followed by a national stakeholder dialogue with system leaders focused on reimagining the long-term care sector using technology. Key actions prioritized through the deliberations convened included: developing an innovation roadmap/agenda (including national standards and guidelines); using co-design approaches for the strengthening the long-term care sector and for technological innovation; identifying and coordinating existing innovation projects to support scale and spread; enabling rapid-learning and improvement cycles to support the development, evaluation, and implementation of new technologies; and using funding models that enable the flexibility needed for such rapid-learning cycles.
Introduction
The COVID-19 pandemic has significantly affected the long-term care sector for many reasons, including residents being at higher risk for serious and life-threating health concerns from COVID-19, exposure to staff with COVID-19, residents living close to each other yet also experiencing significant social isolation, and challenges with providing needed care and support during long periods of lockdown. 1 The challenges faced during the pandemic were made worse by many long-standing and significant concerns in the sector. These include (but are not limited to) lack of coordination with the sector and between other sectors (eg, primary care, specialty care, rehabilitation, and public health) in health systems, limited collection and use of data to make improvements, limited staff training, satisfaction, and retention, and restrictions in the design and capacity of long-term homes.2,3
This has led to many recommendations4-8 and initiatives (including the development of standards for long-term care)9-13 to strengthen the long-term care sector across the country. Enhancing the use of technology has been identified as a key part of these efforts given its potential to help address some of the biggest challenges in the sector and to improve the health and well-being of residents and caregivers.3,5,7,14,15 For example, technology can and has been used to facilitate and enhance communication between facilities, care providers and caregivers, family, and friends (eg, through electronic health records), enhance safety of residents (eg, through location tracking, remote-monitoring technologies, and monitoring use of appliances), and make rooms more accessible (eg, using “Google” or “Alexa” to activate or adjust basic room features such as lights, blinds, temperature, and entertainment).16,17 However, many long-term care homes lack adequate internet bandwidth and cyber security and support to enable many of these technologies. 13
While important, technology needs to be carefully deployed in a way that puts residents, caregivers, and their families at the centre of care. Adopting such approaches can ensure that technology is used to move the needle on achieving the quadruple aim outcomes of enhanced client experiences, improved health outcomes, keeping costs manageable, and enhancing provider experiences. However, focusing the use of technology only as a way to keep costs manageable and ensure efficiency runs the risk of further de-personalizing care and exacerbating many of the existing challenges in the system. For example, technology could be deployed in a way that eliminates tasks for some staff. However, while such a change could free up staff and care providers for more time for interactions and support for residents and caregivers, it could also further reduce opportunities for human interaction if overall staff time is cut.
Addressing complex and pressing system-level policy issues such as these requires the creative interplay of, on the one hand, the best-available data and research evidence and, on the other hand, the tacit knowledge and views and experiences of those who will be involved in or affected by the issue. 18 Given this, we undertook a multi-component project that involved convening a series of citizen panels, followed by a national stakeholder dialogue with system leaders to identify key actions and priorities from citizens and system leaders to enhance the use of technology in the long-term care sector.
Approach to convening citizen panels and a national stakeholder dialogue
Our project was conducted in three phases (development of briefing materials, convening citizen panels, and convening the stakeholder dialogue) and guided by an interdisciplinary steering committee that met regularly throughout the project to collaboratively review and revise all project materials and plans for the citizen panels and stakeholder dialogue.
In the first phase, we iteratively developed an evidence brief that synthesized the best-available evidence about key challenges related to enhancing the use of technology in long-term care settings in Canada, three elements of a potentially comprehensive approach to address the problem, and key implementation considerations for the elements. An outline for the evidence brief was developed in collaboration with the steering committee, which was then refined through interviews with 13 key informants that included government policy-makers, organizational leaders, professional leaders, leaders of citizen groups, and researchers from across the country. We used the insights and feedback from the interviews to frame the evidence brief in a policy relevant way and to identify key resources to include. We then refined the evidence brief based on the local data and evidence and relevant systematic reviews (details about the methods are included in the publicly available evidence brief). 2 We worked collaboratively with our steering committee to turn the evidence brief into a plain-language citizen brief that was used to inform the citizen panels. 19
In phase two, we convened four virtual citizen panels on January 8, 2021 (with panellists from British Columbia, Alberta, Saskatchewan, and Manitoba), January 11, 2021 (with panellists from Ontario and Quebec), January 14, 2021 (with panellists from New Brunswick, Nova Scotia, Prince Edward Island, and Newfoundland), and on January 15, 2021 in French (with panellists from Ontario, Quebec, and New Brunswick). We recruited panellists in collaboration with AskingCanadians™ panels, which include more than 600,000 Canadians that are affiliated with loyalty programs in Canada and are representative of all the Statistics Canada demographic categories. We sought to engage 14-16 panellists who were diverse in terms of gender, age, sexual orientation, socioeconomic status, ethnocultural background, and geographic residence. We conducted a thematic analysis based primarily on notes taken by the facilitator and secretariat, but recordings of the panels were selectively revisited.
Last, we convened a virtual stakeholder dialogue over two days that was informed by the evidence brief that we pre-circulated and that included a summary of key messages from the citizen panels. Dialogue participants included government policy-makers, organizational leaders, professional leaders, leaders of citizen groups, and researchers that were identified from steering committee members and from suggestions provided by key informants. We aimed to engage system leaders from each province and territory and prioritized those who brought unique views, experiences, and tacit knowledge about the topic and who could champion change within their respective constituencies. The dialogue was facilitated by one of us with detailed notes taken by secretariat. Deliberations were thematically analyzed and a summary of key themes was shared with participants and refined at the end of the dialogue. The stakeholder dialogue was convened “off the record” according to the Chatham House Rule and therefore was not recorded.
Key insights from citizens and system leaders
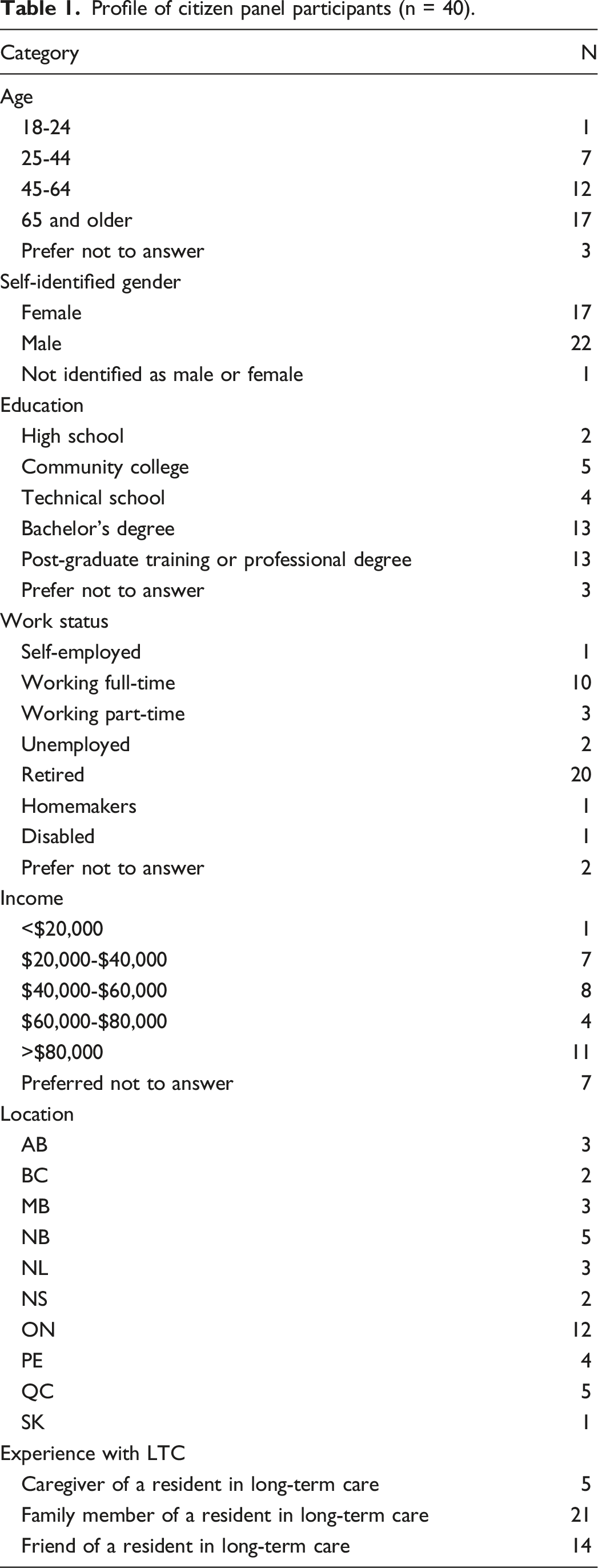
Profile of citizen panel participants (n = 40).
Insights about challenges related to the problem
Summary of citizens’ views about challenges related to enhancing the use of technology in long-term care settings in Canada.

In addition to the challenges identified by citizens, dialogue participants highlighted four additional challenges: 1) lack of a comprehensive innovation agenda for long-term care; 2) residents, families, and caregivers are rarely and inconsistently prioritized and meaningfully engaged in technology development and in efforts to strengthen long-term care more generally; 3) technologies are often not attuned to the individual needs of residents and local realities; and 4) the long-term care sector is not an innovative space and the value of technology is often questioned.
Insights about elements of a potentially comprehensive approach to address the problem
Insights from citizens and dialogue participants about three elements of a potential approach to enhancing the use of technology in long-term care settings in Canada.

Overall, citizens highlighted a need for establishing national standards and guidelines for improving long-term care in provinces. Citizens also emphasized the need for co-design approaches to be used in planning the renovation of existing long-term care homes and for building of new ones, and the context of long-term care homes should encompass the broader social, cultural, and policy environments that can support the adoption of suitable technologies. Innovation was identified as a recurrent theme, but some panellists emphasized the need for incremental innovations, while others advocated for radical innovations, which was also deliberated by system leaders in the stakeholder dialogue.
Building on this, the deliberations among system leaders culminated in a consensus about the need for an innovation agenda that could be advanced by focusing on the elements related to engaging long-term care home operators, staff, residents, and their caregivers in developing and adopting technologies, and to enabling rapid-learning and improvement cycles to support the development, evaluation, and implementation of new technologies. However, views on the form and scope of an innovation agenda that should be implemented differed, which we describe below in the section about implementation considerations.
For the element focused on engagement, participants underscored the need to focus an innovation agenda with solutions for what the long-term care sector should be. Overall, the participants highlighted this would first require a re-imagining of the sector and a co-design approach. The importance of a co-design approach (which was also emphasized by panel participants) was seen as critical given that insights from those engaged at the frontline (ie, staff, residents, caregivers, and families) in designing technology are important for it to be used more consistently and effectively. Moreover, co-design was viewed as essential for broader efforts to re-imagine long-term care.
Building on this, deliberations about rapid-learning and improvement cycles centred on how to use this type of approach to begin a re-imagining process and build an innovation agenda to address the many large and long-standing issues in the long-term care sector. The key issues emphasized included implementing country-wide standards, enhancing coordination for technology innovation within and between governments, addressing the challenges posed from having varied long-term care ownership models, and ensuring ongoing engagement as described above. Co-design was again seen as fundamental in this type of process to ensure that a rapid-learning approach to enhance technology use in long-term care (and re-imagining of the sector) is grounded on the values, needs and preferences of older adults and the best-available evidence.
Implementation considerations
While system leaders agreed on the need for an innovation agenda for enhancing the use of technology in long-term care and strengthening the sector, they highlighted three different implementation approaches: incremental, disruptive, and radical innovation. Incremental innovation focuses on setting and implementing short- to medium-term goals for enhancing quality of care and care processes. This was viewed as being achievable within the existing structure of long-term care in Canada. Examples included efforts to establish better communication and data sharing between sectors (eg, with the primary, specialty, rehabilitation, and public-health sectors), using technology for routine care and for leisure (eg, to address isolation among residents). Doing so would require addressing barriers to technology adoption, including those with procurement processes, lack of financial incentives and/or flexibility to do things differently and continuing to work through long-standing issues with data confidentiality, privacy and ownership. In contrast, disruptive innovation was seen as an opportunity for technology to be used as part of efforts to significantly change the long-term care sector. For example, some suggested moving from a more institutionalized setting to one that is more home like and therefore person centred. Last, adopting a radical innovation agenda was viewed as an opportunity to re-think long-term care for the digital age. Many system leaders who participated in the dialogue supported this option as they viewed the combination of rapidly emerging digital solutions with increasingly tech-focused residents, families and caregivers as an opportunity to re-engineer the sector. Moreover, it was noted that this approach might be needed to support an ageing baby boomer generation that seems to have little interest in entering long-term care in its current form.
Next steps
System leaders highlighted that the sustained interest in the need to reform the long-term care sector during the COVID-19 pandemic and in recovery stages can be capitalized on to pursue fundamental changes to the sector. With this window of opportunity, system leaders identified several inter-connected next steps to advance an innovation agenda for long-term care, including: 1) using a co-design approach in all efforts to reform the long-term care sector; 2) identifying and coordinating existing innovation projects to support scale and spread, and develop an innovation roadmap/agenda; 3) using technologies in a way that enables person-centred care and support in long-term care; 4) modifying policy and organizational processes in the sector to use decision-making processes that foster and implement innovation over time by prioritizing making small yet rapid changes that are centred on residents, caregivers, and families; and 5) using funding models that enable the flexibility needed for such rapid-learning cycles. Collectively, these actions were viewed as the foundation upon which a re-imagined long-term care sector could be built. Indeed, in the time since the citizen panels and the stakeholder dialogue were convened in early 2021, there have been national efforts to create standards in long-term care12,13 and to establish priorities for reforms in some provinces.20-22 Our findings will be important for operationalizing such standards and priorities.
Footnotes
Funding
This project was funded by AGE-WELL NCE Inc (AW-PP2020-PP6). The citizen panel convened in Ontario was also co-funded by the Government of Ontario through a grant provided to Rapid-improvement Support and Exchange (RISE).
Ethics approval
The Hamilton Integrated Research Ethics Board (HiREB) provided approval for the citizen panels (HiREB project # 13-369). All participants in the citizen panels provided informed consent. No ethics was obtained for the stakeholder dialogue as the HiREB has indicated that ethics approval is not required for the meeting as it is not recorded. Ethics approval has been acquired for our ongoing evaluation of stakeholder dialogues (HiREB project # 09-336), but those results are not presented here.
