Abstract
Objective
CAPACITI (Community Access to PAlliative Care via Interprofessional Teams Improvement) is a virtual training program that teaches primary care providers how to incorporate an early palliative approach to care in practice. Building this capacity can help primary care providers better meet the needs of their seriously ill patients; however, there has been limited in-depth study as to the added benefits of active facilitation in on-line education. We completed a qualitative inquiry with CAPACITI participants to explore perceived differences in self-directed and facilitated e-learning to understand how these modalities contribute to change in practice.
Methods
We completed a qualitative analysis of semi-structured focus groups with primary care teams that participated in CAPACITI. This study was part of a cluster randomized controlled trial where teams were randomized to self-directed or facilitated modalities for each of the three CAPACITI modules. We followed a qualitative descriptive design, using a constant comparative approach to determine emergent themes to understand participant experience and preference in learning modality.
Results
We conducted 63 focus groups throughout the trial, representing 42 unique teams, about a quarter of which had experienced both learning modalities at the time of the focus group. Qualitative analysis revealed three main themes: changes in thinking (ie identifying patients early in the illness trajectory), change in behavior (ie increased collaboration), and preference in learning modality and perceived benefits. Interestingly, we found no overwhelming preference in learning modality.
Conclusions
Self-directed and facilitated learning modalities were both perceived as effective in promoting changes in thinking and behavior among primary care providers across diverse care settings. Future studies should further explore the use of tailored facilitation such as simulated patient encounters and innovative coaching strategies to optimally promote behavior change in virtual palliative care education.
Keywords
Introduction
Early palliative care has been demonstrated to improve quality of life, satisfaction, symptom control, and illness understanding, and also reduce aggressive care treatments and hospitalizations.1–4 A 2025 scoping review reported that many studies define early palliative care for both cancer from noncancer illnesses as prognosis-based, using the onset of advanced disease at the time of initialization. 5 Research shows that primary care providers working in community-based interprofessional teams play an important role in providing palliative care, particularly in these earlier stages.6,7 Primary care providers are willing to provide palliative care,8,9 but often lack the knowledge, confidence, tools, and practical support to do so.10–12 As such, palliative care education programs are needed to help develop provider competency and confidence in providing an early palliative approach to care in their unique context of care delivery.
In recent years, particularly after the COVID-19 pandemic, there has been a shift towards using virtual learning platforms to deliver professional development courses due to accessibility, cost-efficiency, and effectiveness.13,14 Virtual learning encompasses a variety of learning modalities. On one hand, there is facilitated learning where a trained facilitator leads group education synchronously and guides discussions to enhance learning. On the other hand, there is self-directed learning where a participant completes the education independently. Online education for providers has increased across all sectors, including palliative care training, and can efficiently reach professionals across multiple different care settings with some demonstration of effectiveness.15,16 General challenges to this virtual approach have been identified such as substantial participant drop-out, preferences for face-to-face interaction, and poor integration of content in an online format.16–18 However, research specifically on optimal learning modalities to improve e-learning outcomes and the potential benefits of expert facilitation in palliative care education is limited. 19
CAPACITI (Community Access to PAlliative Care via Interprofessional Teams Improvement) is a virtual training program for primary care providers that teaches how to incorporate an early palliative approach to care in practice. We conducted a national cluster randomized controlled trial of CAPACITI where interprofessional teams were randomized to facilitated or self-directed learning for each of three learning modules. 20 We previously published quantitative analyses that found that CAPACITI improved palliative care identification and provider competency: but there was no significant difference between the facilitated and self-directed groups.21,22 The objective of this qualitative study was to explore perceived differences in self-directed and facilitated learning experienced by participants and changes in their thinking, behavior, and practice as a result of taking CAPACITI.
Methods
Study Design
We conducted a qualitative study using data collected from focus groups, purposively selected from teams that completed a CAPACITI module within our randomized controlled trial (RCT). We used a qualitative descriptive design for this study, embedded in the larger RCT, often used to expand upon quantitative findings in health environment evaluations. 23 The primary goal of a descriptive design approach is to describe the phenomenon in detail, using participants’ own words and experiences. 24 The qualitative data complement the interpretation of the prior reported quantitative data by adding depth and context to our understanding of the impact of CAPACITI and differences between the education modalities. Importantly, for participants who experience both self-directed and facilitated modes (explained in Sampling Strategy and Data Collection), they can directly articulate the comparative effectiveness of each approach. This research was approved by the Hamilton Integrated Research Ethics Board (#13867) (see https://clinicaltrials.gov/ct2/show/NCT05120154 for approved and registered operating protocol).
CAPACITI Intervention
CAPACITI consists of three distinct modules: (1) identify and assess like an expert; (2) enhancing communication skills; (3) enhancing skills for ongoing care (including involvement of family physicians and specialists). Each module is comprised of 4 1-hour sessions, which include expert advice and tips, evidence-based tools, and case studies to serve as practical examples (see Supplemental Figure 1 for detailed content). The development, structure, and content of CAPACITI have been described previously in detail in the published protocol for this study, outlining the research process and intervention.20,25
CAPACITI session content was hosted on an online Learning Management System (Moodle, https://moodle.org/) which allowed for secured control of the study materials and access to facilitated sessions. Teams were randomized to either facilitated (intervention group) or self-directed (control group) learning at the start of each module, meaning that teams may have been allocated to one arm for a module and the other arm for the next module. Both groups received full access to the CAPACITI online session materials (eg, slide decks, evidence-based tools, cheat sheets, resources, assignments). The cluster randomization of teams prevented contamination between study arms among members of a team.
Individuals in the facilitated group were also invited to participate in facilitated virtual webinars (1 webinar per session, 4 per module) via the Zoom application. The webinars were each 1 hour and included a synchronous presentation of the respective session slide deck and case study, and a discussion to adapt the content to local context, facilitated by a palliative care expert. CAPACITI was run in 2 cohorts, from November 2021 to April 2022.
Participants
Primary healthcare teams and solo prescribing clinicians (eg, primary care physician, nurse practitioner) from across Canada were invited to enroll and participate in CAPACITI through notifications forwarded from provincial primary care and palliative care associations/organizations. CAPACITI was offered free of charge to all participants and there was no compensation or financial incentives for completing the course.
Sampling Strategy and Data Collection
We conducted independent focus groups with teams (equally divided between study arms), immediately after each module. A strategy that employed convenience sampling, with purposive selection, was used to determine participating teams. Team members indicating willingness to participate in postintervention focus groups were contacted, sampling from diverse team sizes, locations, and study allocations. Focus groups were conducted by 2 experienced interviewers (VB and SK) and hosted using Zoom. Participants provided informed consent prior to focus group initiation. The focus groups were semistructured and probed perceptions of the most recent module, and if applicable, any prior modules. 20 Teams that had completed a module in both study arms were also asked to compare these experiences.
The focus groups followed a discussion guide about the impact of the modules on the teams’ thinking and behavior, previously tested in the pilot study 26 (see supplemental Figure 2). This guide was informed by the Consolidated Framework for Implementation Research (CFIR 2) which lists multilevel contextual factors integral to assessing program implementation and impact.26–28 The focus group facilitators were flexible in questioning to pursue unexpected areas of interest and probe for additional details. The focus groups were recorded, transcribed verbatim using Otter.ai software, and checked for accuracy by the analysts by reading the transcripts of the focus groups they each facilitated for concordance and rectifying unclear statements with the audio recordings. Focus groups were conducted with additional teams until data saturation of themes was achieved.
Data Analysis
Focus group transcripts were analyzed using NVivo (Version 14). Two primary analysts (VB and SK) were involved in the thematic analysis of the data. The analysts were from nonclinical backgrounds (public health and genetics) with extensive experience in qualitative research. Analysts independently and repeatedly reviewed the transcripts for emergent themes and coded them in NVivo using the constant comparative method. 29 Through this iterative process, the analysts continuously compared new data with existing data, emerging concepts, and refining codes throughout the analysis. Initial codes were directly derived from the transcript text, ensuring the fidelity of the coding process. The analysts compared their individual coding after each module, consolidating coding approaches through discussion to reach a consensus. A shared codebook was developed and revised as required, to ensure common definitions of themes. Twelve transcripts were coded in duplicate. With consistency in coding and thematic development established, the analysts divided and coded the remaining transcripts. Upon completion of the thematic analysis, the analysts and the research team (that includes clinical backgrounds in palliative medicine and social work) independently reviewed and then discussed all coding, finalized the themes, and synthesized the overarching themes. We used the Consolidated Criteria for Reporting Qualitative Research (COREQ) to report this study to help ensure methodological rigor and transparency in the thematic analysis and synthesis. 30
Results
Participant Characteristics
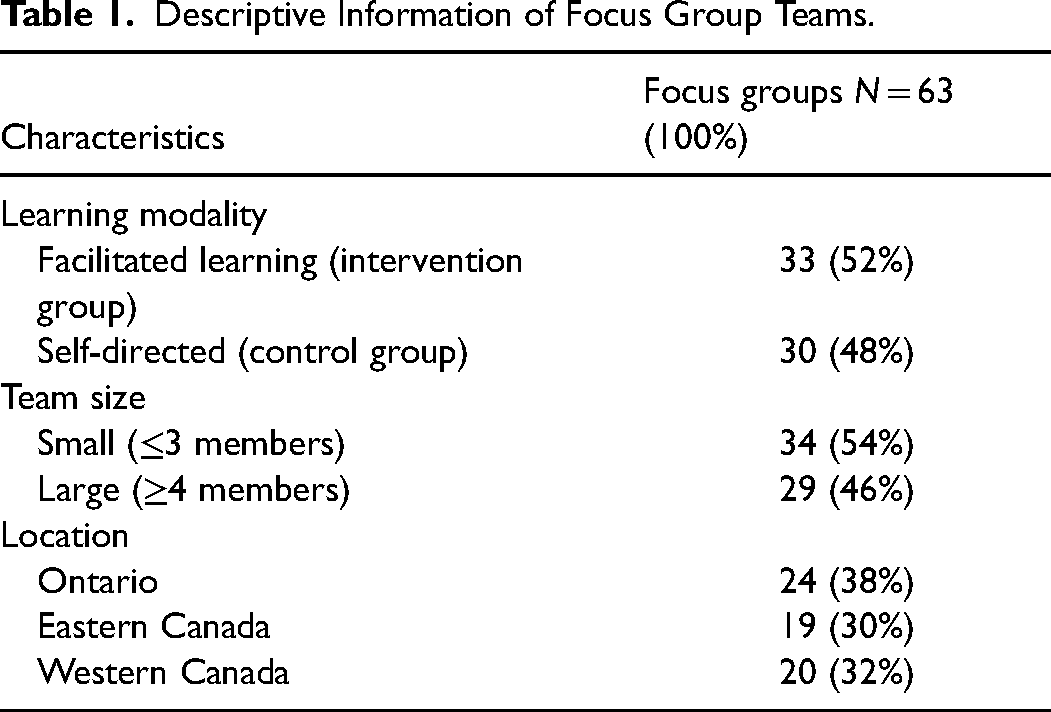
We conducted a total of 63 focus groups with 30 self-directed teams and 33 facilitated teams (allocated at the time of the focus group) that completed each module of the CAPACITI education program. Teams were classified by size and location (Table 1). Overall, the 63 focus groups represented 42 unique teams, with some participating in 2 focus groups over the study. The 42 unique teams represented 249 providers, of which 208 (83%) were female, 39 (60%) were male, and 2 (1%) were gender diverse. Among these providers, 88 (35%) had no prior palliative care education, 117 (47%) had taken LEAP, and 70 (28%) had other related training. Of the 42 unique teams, 10 (24%) teams had the opportunity to experience both modes of learning at different points in the program, 14 (33%) experienced only self-directed learning, and 18 (43%) experienced only facilitated learning. This subgroup of 10 teams was demographically similar (size, professions, location) to the broader sample. Participants in the focus groups were from a wide range of roles, including nurses (n = 34 (43%)), allied health professionals (n = 14 (16%)), and physicians (n = 10 (11%)). Focus groups ranged from 20 to 30 minutes and consisted of 1 to 15 participants.
Descriptive Information of Focus Group Teams.
Thematic Analysis of the Focus Groups
We identified 3 main themes: (1) preference in learning modality and perceived benefits, (2) change in thinking, and (3) change in behavior, all of which in total, encompassed 8 subthemes (Table 2).
Summary of Themes.

Theme 1. Preference in Learning Modality and Perceived Benefits
Ten teams had the opportunity to experience both the self-directed and facilitated learning modalities for different modules during the program. These participants compared their experiences, shared their preferences, and explained how each approach benefited their learning.
Subtheme 1. Experiences in Self-Directed Learning
Most participants reported working independently, regardless of whether they were taking the CAPACITI training with their team members. Participants appreciated the flexibility of self-directed learning as many reported lack of time during the workday as a barrier to completing the modules: “I enjoy the self guided learning because I get to focus, put it in my agenda. And if I'm having a busier day, I'll move it to another day and focus on the actual training” (Team U, Ontario, Large Team). Participants also noted that self-directed learning allowed them to participate regardless of where they were in Canada and their time zone.
Participants with less palliative care experience thought that the opportunity for peer interactions and to hear diverse perspectives could have enhanced their learning: In this circumstance, where my experience isn't as vast as it would be in some other areas, it would have been really nice to hear some of the perspectives of the other participants and see what other people are doing and some of the questions they asked. (Team Y, Eastern Canada, Small Team)
Many participants also described challenges associated with the self-directed approach such as no scheduled time to complete the modules and lack of motivation. To address this, some self-directed teams implemented group meetings or check-ins while others relied on their team lead or email reminders from the CAPACITI administrators to stay on track.
Subtheme 2. Experiences in Facilitated Learning
Participants enjoyed the interactive aspects of facilitated learning such as the breakout rooms and group discussions. These components allowed participants to learn from health care providers in different professions from across Canada: “I'd rather attend the breakout rooms and actually meet the people that are doing the course … I think it was just a really great way to kind of get to know what all the different programs and provinces are doing” (Team V, Eastern Canada, Small Team).
However, some participants noted little engagement during the group discussions, “There wasn't a whole lot of participation, not really having cameras on, and just kind of quiet. And it's hard because it's people from all different backgrounds and walks of life” (Team S, Western Canada, Large Team).
Participants shared that having a facilitator guide group conversations was valuable to their learning and created a sense of “camaraderie.” Many noted that being part of the facilitated group gave them a sense of accountability to participate in the live sessions. Despite this, some encountered scheduling challenges and could not attend. These participants reported watching the recorded sessions and completing the modules independently.
We asked teams representing the facilitated or self-directed arms about how their thinking and behavior changed due to the education. The themes that emerged during thematic analyses were very similar between both arms, so we grouped them together into the 2 themes below.
Theme 2. Change in Thinking
Subtheme 3. Early Identification
Participants expressed identifying patients earlier in the illness trajectory and recognizing the importance of early intervention. Others noted they were being proactive by initiating conversations about palliative care at the time of diagnosis or shortly thereafter by using exercises introduced in the CAPACITI program: “The exercise for early identification was a good one and it sort of helped us to realize that we are not identifying palliative care plans as early as we can, so that we can be more proactive as opposed to being reactive” (Team A, Ontario, Large Team). Some took the opportunity to be proactive in general appointments or consultations by discussing palliative care or advance care planning. Finally, many participants reported recognizing the importance of identifying patients early in the illness trajectory rather than at end of life.
Subtheme 4. Using Evidence-Based Tools
Participants appreciated the evidence-based tools and cheat sheets they received during the CAPACITI program. Many shared they were thinking about how they could implement them in their daily interactions with clients, and some reflected on previous clients they had that could have benefitted from specific tools: I did find it really interesting and it's something I'll try to keep in mind just as a tool for helping myself kind of flag patients who might benefit from a palliative approach where I wouldn't necessarily have thought of it otherwise. (Team E, Ontario, Large Team)
Participants also discussed how certain tools, such as illness trajectories, could be used in practice to help patients understand their diagnosis.
Subtheme 5. Reflection on Practice and Patients
Many participants engaged in self-reflection throughout the CAPACITI program to think about how they provide care, learn from prior experiences, and gain confidence in their approach. While all participants were familiar with palliative care, many expressed that CAPACITI changed the way they think about providing care and how they interact with their patients: “It was a great opportunity to sit back and sort of check myself and remind myself of why I do this work and how I can continue to improve” (Team J, Ontario, Large Team). Some also reflected on past patients and how they could have handled complex situations differently with the information they received from CAPACITI, such as advocating on a client's behalf or including the caregiver in advance care planning.
Theme 3. Change in Behavior
Subtheme 6. Sharing Information With Others
Many participants shared information from CAPACITI with others. Some created new materials using the information provided and gave presentations to their team members: “I've been able to share this message and this hope about moving palliative care upstream with talking about it earlier. And about encouraging capacity building throughout other fields of social work to create capacity for palliative conversations” (Team L, Eastern Canada, Small Team).
Others distributed hard copies of the CAPACITI cheat sheets and resources within their team, “Those cheat sheets, I think are fantastic… I have shared some of those with some of our nurses in long term care” (Team H, Western Canada, Large Team). Some participants also used the CAPACITI resources to guide their conversations with patients and their caregivers.
Subtheme 7. Interacting With Clients
Participants expressed a change in client interactions after taking the training, such as pausing to allow for emotion or including the family caregiver in conversations. One participant described feeling more prepared going into appointments because of how they had started to identify and track those who may benefit from a palliative approach to care: Now I have a bit of a coding system that helps me be able to not only articulate the number of palliative people that I have, but also I can find things a lot more efficiently and I can monitor people a lot more efficiently so I will reach out to my palliative people a lot more frequently. (Team N, Eastern Canada, Small Team)
Subtheme 8. Increased Collaboration
Participants frequently described increased collaboration within their internal team and with the broader care team and external providers. Many participants reported having more team meetings to discuss clients who may benefit from a palliative approach to care: “As a group, I feel that it's much easier to talk about palliative patients and dying patients in a group setting when we have interdisciplinary rounds” (Team O, Western Canada, Large Team).
Others shared that they felt more comfortable reaching out to external care providers. Notably, some described how they realized the importance of including caregivers and family members as a result of taking CAPACITI, I find that a lot of my patients have caregivers, and I've found that the modules did help me with some of them. Before I might not have given as much attention to, but I really … tried to get [caregivers] involved more than I had before. (Team Q, Eastern Canada, Small Team)
Discussion
Given that our prior quantitative research about the virtual CAPACITI palliative care education showed no significant differences between facilitated or self-directed study arms, we conducted focus groups after each module of CAPACITI to understand in-depth the potential differential impact of this education based on learning modality. Healthcare providers in both facilitated and self-directed study arms reported that the CAPACITI program helped in their early identification of patients who could benefit from a palliative approach to care, their use of evidence-based tools, and being generally more proactive in this care. Participants also reported experiencing a change in behavior in how they shared information with others, approached interactions with patients, and collaborated with the broader care team, regardless of whether the CAPACITI sessions were facilitated. Even among the teams that experienced both learning modalities, there was no overwhelming preference for one modality over the other as both were seen as effective agents to build competency in providing an early palliative approach to care. To our knowledge, this is the first qualitative study within a randomized controlled trial of an interprofessional palliative care education program to explore the experiences of multidisciplinary primary care providers in self-directed and facilitated learning cohorts.
Our qualitative analysis further elucidates the reasons underlying our previously reported findings of no detectable differences between facilitated and self-directed learning modalities in CAPACITI. The absence of a strong preference for learning modality suggests that each modality offers distinct advantages depending on individual learner needs and contexts. Some participants, particularly those with less palliative care experience, appreciated the valuable opportunities for a stronger sense of accountability, expert-guided discussions, and learning from a variety of primary care providers that the facilitated learning modality provided. Other studies have reported a similar preference for expert facilitation when learning about palliative care collaboration and having serious illness conversations, emphasizing the value of social learning and guided discussion in building clinical confidence and competence.14,31,32 However, challenges such as inconsistent group engagement in discussions and scheduling conflicts impacted the effectiveness of the facilitated learning modality for some, similar to recently reported challenges of virtual learning. 33 In contrast, a key perceived benefit of self-directed learning was its flexibility, particularly accommodating time constraints of clinical work and varying time zones across the study setting (Canada), aligning with previous findings in healthcare education. 34 These findings may suggest that if resources allow, offering multiple learning modalities can support diverse learner needs and professional contexts. Our results also suggest that some palliative care competencies and skills can be acquired by interprofessional care teams without added facilitation. This is important since self-directed learning can be efficiently scaled, reaching rural/remote communities across the country where limited resources, staff, and scheduling conflicts are barriers, as recognized in other studies.14,35
There are limitations inherent to the nature of voluntary focus groups. Although we included a large number of participants, the perspectives of individuals who declined to participate and may have had less favorable experiences, were not captured. Participants in the focus groups may have been biased towards expressing positive change or might not have been comfortable disclosing their true feelings among their co-workers. In large focus groups, not all participants may have an equal chance to fully share their perspectives. Focus group facilitators were mindful in attempting to elicit responses from each and every team member, and all participants seemed forthcoming in expressing their opinions. A limitation of our sample is that only about a quarter (10) of the teams experienced both learning modalities, allowing them to directly compare these education experiences. As indicated earlier, teams that only experienced one modality throughout CAPACITI expressed similar views regardless of learning allocation. Finally, while we asked about perceived changes to thinking and behavior, we did not confirm these changes through objective measures nor assess the sustainability of any changes that were stated. Future studies should examine longer-term outcomes to determine the sustainability of changes to knowledge and practice reported immediately following the education intervention.
Conclusion
In conclusion, our qualitative analysis of the CAPACITI trial found that delivering education using self-directed and facilitated learning modalities were both perceived as effective by primary care providers in changing their thinking and behavior towards integrating an early palliative approach to care. The multicomponent education approach we used in CAPACITI and our evidence of the efficacy of this program across diverse care settings can be used to help inform the design of future virtual training programs for interdisciplinary care providers. Given our findings that the facilitated sessions had minimal impact on the learning experience, but some degree of interaction had value, future iterations of CAPACITI could be self-directed with a final interactive discussion session to reinforce program content. Additional research is also needed on the optimal use of enhanced facilitation in building complex palliative care competencies, such as one-on-one coaching, artificial intelligence-assisted tutoring, hands-on virtual practice (eg, simulated patient encounters), and personalized feedback.
Supplemental Material
sj-docx-1-pal-10.1177_08258597251351432 - Supplemental material for Primary Care Providers’ Perceptions of the CAPACITI Palliative Care Education Trial: A Qualitative Study of Experiences With Self-Directed and Facilitated Modalities
Supplemental material, sj-docx-1-pal-10.1177_08258597251351432 for Primary Care Providers’ Perceptions of the CAPACITI Palliative Care Education Trial: A Qualitative Study of Experiences With Self-Directed and Facilitated Modalities by Shilpa Jyothi Kumar, Valerie Bishop, Daryl Bainbridge, Frances Kilbertus, Kathy Kortes-Miller, Samantha Winemaker and Hsien Seow in Journal of Palliative Care
Supplemental Material
sj-docx-2-pal-10.1177_08258597251351432 - Supplemental material for Primary Care Providers’ Perceptions of the CAPACITI Palliative Care Education Trial: A Qualitative Study of Experiences With Self-Directed and Facilitated Modalities
Supplemental material, sj-docx-2-pal-10.1177_08258597251351432 for Primary Care Providers’ Perceptions of the CAPACITI Palliative Care Education Trial: A Qualitative Study of Experiences With Self-Directed and Facilitated Modalities by Shilpa Jyothi Kumar, Valerie Bishop, Daryl Bainbridge, Frances Kilbertus, Kathy Kortes-Miller, Samantha Winemaker and Hsien Seow in Journal of Palliative Care
Footnotes
Authors’ Contributions
All authors contributed to the conception and design of the study. SJK and VB completed data collection and analysis. VB, SJK, DB, and HS drafted the manuscript. All authors read, edited, and approved the final manuscript.
Consent for Publication
This manuscript contains no personally identifiable information on study participants.
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Ethics Approval and Consent to Participate
Ethical approval for this study was obtained from the Hamilton Integrated Research Ethics Board (#13867). Informed consent to participate was obtained from all subjects involved in the study.
Funding
This work was supported by the Canadian Institutes of Health Research (grant number 408099).
ORCID iDs
Patient and Public Involvement
Patients or the public were not involved in the design of this research.
Trial Registration
Supplemental Material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
