Abstract
Introduction
South Asians represent one of the largest ethnic minorities in the UK 1 comprising of 9.3% of the population of England and Wales. 2 Globally, research indicates that the burden of life-threatening and chronic diseases among South Asian migrants is significantly higher than other ethnic groups. 3 Despite this, ethnic minority communities often encounter obstacles in accessing palliative care services.4,5 These obstacles include cultural or religious practices being poorly or misunderstood or language barriers 6 making it harder for South Asians to access timely and appropriate care. Therefore, understanding how these minority groups experience healthcare systems and whether their needs are met appropriately is crucial for enhancing healthcare outcomes. 7
Palliative care services aim to provide holistic care and improve the quality of life for individuals with advanced illness or nearing the end of life, while also supporting their families. This encompasses managing pain and distressing symptoms, as well as offering psychological, social, and spiritual support. 8 In this review, we use the term “palliative care” to refer to holistic care that addresses the physical, emotional, social, and spiritual needs of individuals with life-limiting illness. The term “end-of-life care” is used specifically to denote care provided during the final phase of life, typically the last weeks or days. Inequality in palliative care provision persists in the UK.9,10 The Care Quality Commission’s 2016 report highlighted enduring inequalities in end-of-life care for minority ethnic groups, particularly those with diagnoses other than cancer and older individuals. Challenges included difficulties in timely access to appropriate care, inadequate identification of patients, poor communication, and lack of individualized care, affecting various equality groups and vulnerable populations. 10
Some evidence indicates that there are higher hospital deaths among individuals from ethnic minority backgrounds compared to other groups. 10 However, recent analyses based on the National Survey of Bereaved People in England 2015 11 showed varied results, with no significant difference in hospital deaths between ethnic minority and white groups. Despite this, individuals from ethnic minority backgrounds were less likely to rate overall care in the last three months of life as “outstanding” or “excellent.” Thus indicating a need for further investigation into underlying reasons. 9 Challenges for ethnic minority groups accessing appropriate palliative and end of life care include, lack of culturally sensensitive information, lack of awareness of palliative care services, mistrust in healthcare systems, language barriers, and experiences of racism.12,13
As the population of South Asian older adults in the UK grows the need to understand their end of life and palliative care requirements becomes increasingly important. Therefore, the aim of the current review was to understand the experiences of South Asian adults, their carers and the health care professionals involved in their care of receiving or delivering palliative or end-of-life care. While the focus of this review is specifically on South Asians living in the UK, this research aim has implications beyond the UK, since South Asian communities constitute large minorities in other western countries such as Canada 14 and Australia 15 where they also experience inequities in palliative care provision.16,17
Methods
This review was registered in advance on PROSPERO (https://www.crd.york.ac.uk/prospero/ ref: CRD42023442603) and the findings are reported in accordance with Preferred Reporting Items for Systematic Reviews and Meta-Analyses (PRISMA) guidelines. 18
Search Strategy
The searches took place in the Ovid database across MEDLINE, PsycINFO, and SCOPUS (see Supplementary Table 1 for search terms). All studies meeting inclusion criteria were subject to forward and backward citation searching. Studies were included if they: explored the experiences of South Asians (defined as people originating from Afghanistan, Bangladesh, India, Pakistan, Nepal, Bhutan, Maldives, and Sri Lanka) patients and or carers or health care professionals; aged 18+; receiving end-of-life care (i.e., palliative care, advanced care planning, end-of-life, and end-of-life decisions); conducted in a UK setting; reported qualitative findings; and was peer reviewed. The search was limited to between August 2003 and August 2023 to ensure results reflected recent and current policies, experiences, and service provision. The search results were de-duplicated and then a title and abstract screen was conducted. Full texts were examined for inclusion into the current study. A second reviewer double rated 10% of the hits at each screening stage. Consensus agreement was 100%.
Data Extraction, Analysis, and Synthesis
One reviewer (JP) extracted the data reported in Table 1. To maintain a clear distinction between direct quotations from patients and the authors’ analysis, direct participant quotations are presented in italicized quotation marks, while the study authors’ interpretations are presented within regular quotation marks. Following guidelines 19 all sections labelled “results,” “findings,” or “discussion” in the papers were coded. The primary aim was to code first-order data, specifically direct quotations from participants, wherever feasible. Subsequently, second-order data, encompassing the words and interpretations provided by the authors of the studies, was coded. Participant quotations and relevant text from the “results”, “findings” or “discussion” sections were coded. Text was imported into NVIVO for analysis.
Summary of Included Studies.
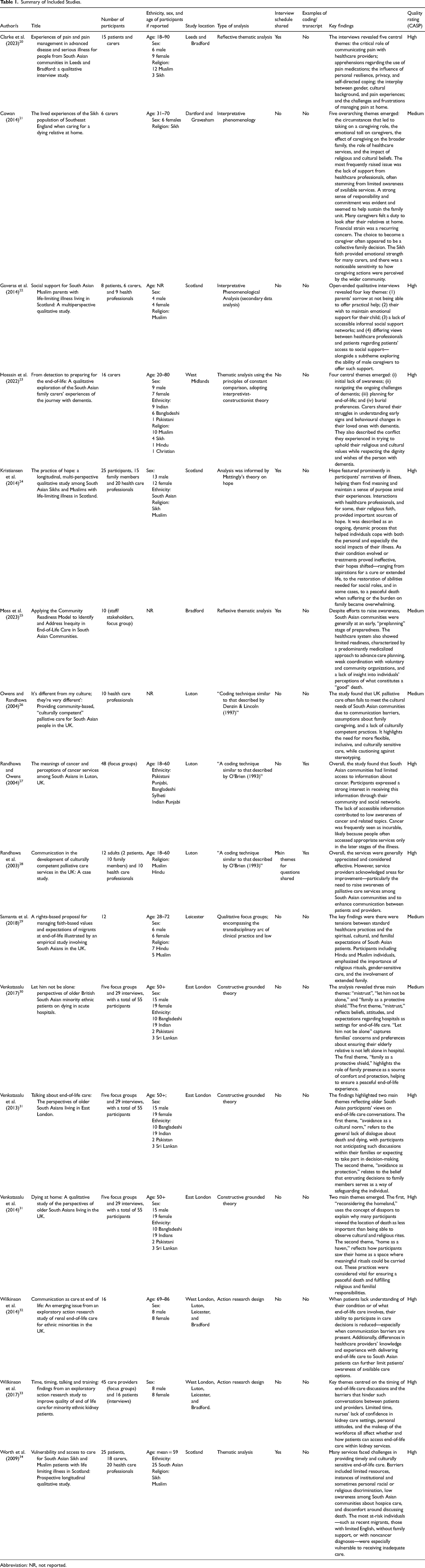
Abbreviation: NR, not reported.
A thematic synthesis framework was used.35,36 The first step involved becoming familiar with the data and generating initial codes which were synthesized into comprehensive themes. Line-by-line coding of the findings of the primary studies was conducted, conceptualizing the data, and identifying concepts inductively. Similar concepts were grouped into themes and subthemes. Conceptual links among themes were identified using a mind-mapping approach to extend the findings offered by the primary studies and to develop a preliminary thematic schema. An inductive approach was employed for data analysis, deriving insights directly from the data rather than imposing preexisting codes or attempting to address predetermined research inquiries. 19
Higher quality studies were coded initially, allowing them to form the foundation of the coding framework and to influence the study's overall findings more heavily. 37 Initially, all 16 papers were reviewed to establish familiarity with the data and initiate the identification of potential codes. Following this, an inductive line-by-line coding process was employed on the data extracted from the papers recognized as high quality. The primary aim was to code first-order data, and subsequently, second-order data was coded. Next, the studies of medium quality were reviewed, utilizing the existing codes from the higher-order papers and introducing new ones where appropriate. These codes were then applied to the papers that had been previously coded. The initial set of codes was scrutinized, and the codes were formulated into descriptive themes. Subsequently, analytical themes were developed to formulate new interpretive constructs, explanations, or hypotheses. 19
Quality Appraisal
Quality evaluation was carried out using the Critical Appraisal Skills Programme Checklist 38 (CASP) for assessing qualitative research. This tool consists of 10 questions addressing various methodological aspects of qualitative research and is endorsed by the Cochrane Qualitative and Implementation Methods Group. 39 To establish quality ratings for each paper, assessments were based on the proportion of criteria met by each study. In cases where studies employed mixed methods, only the qualitative components of each study were subject to appraisal. Although the CASP Checklist does not prescribe a specific scoring system, a score was calculated for each paper based on the percentage of items rated as “yes.” In line with the recommendations 37 the studies were categorized as high quality (scores: 8–10), medium quality (scores: 5–7), or low quality (scores: 0–4).
Results
The search yielded 366 articles. Of these, 296 were screened out at the title and abstract screening stage. Thirty-nine articles were screened fully and 16 met inclusion criteria for the current study (see Figure 1). See Supplementary Table 2 for the list of the excluded studies with reasons.
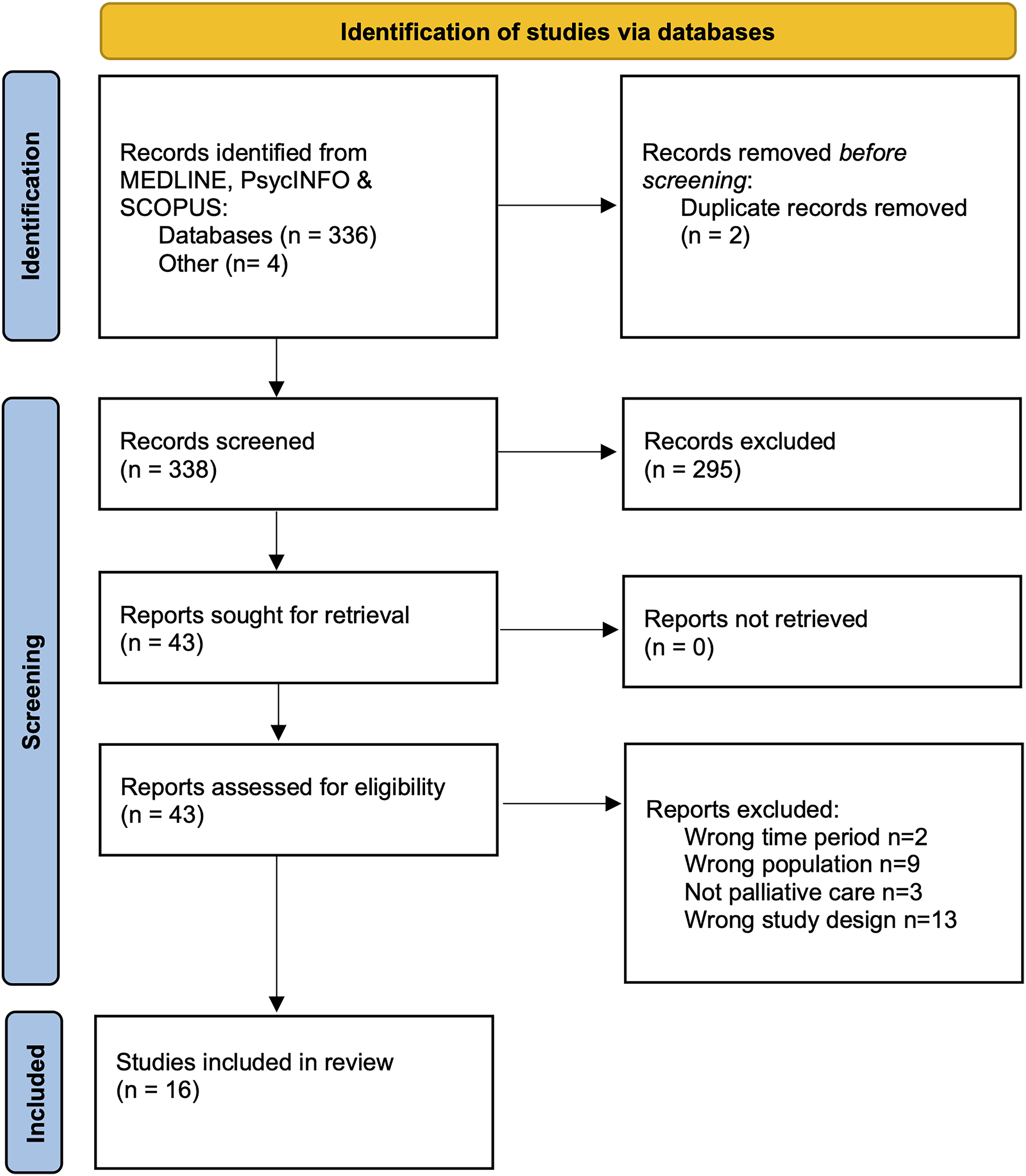
PRISMA flow diagram of included studies. 18
Study Characteristics
See Table 1 for the full details of study characteristics. Four of the sixteen studies (25%) used a participatory approach to inform topic guides. Interview schedules were shared in five (31%) studies, and examples of the coding process was shared in two studies (12.5%). Three studies30, 31, 40 included in this review reported analyses from concurrently collected data, resulting in participant overlap. During data integration, themes and study characteristics were cross-examined to ensure balanced representation of findings, avoiding undue influence from duplicated participant data. Participant counts were adjusted to reflect this overlap, resulting in a total of 407 unique patients, caregivers, and professionals included in the qualitative synthesis. As a result, there was sample overlap in these studies. Accounting for this, a total of 407 patients, carers, and professionals participated in the qualitative components of these studies.
Four studies used thematic analysis, three constructive grounded theory, two action research design, two Interpretative Phenomenological Analysis (“IPA”), two described analysing data in a “similar manner to the technique of O’Brien (1993),” one described a “coding technique similar to that described by Denzin & Lincoln (1997),” one was informed by “Mattingly's theory on hope,” and one used a qualitative “hybrid methodology” encompassing clinical practice and law.
Thematic Synthesis
A summary of the themes and subthemes is shown in Table 2.
Themes and Subthemes from the Included Studies.

Theme One: Barriers and Facilitators to Discussing and Preparing for End of Life
Discussing Death: Patient and Family Perspectives
One barrier described by some participants when it came to accessing palliative care services was stigma around discussing death. The reasons for avoiding discussions about death among patients and families encompassed cultural norms, a belief that conversing about death might accelerate its arrival, and a sense among patients that their families would take charge of necessary arrangements or plans for their passing.
In one study, five participants explained how they typically sidestepped discussing death or completing a will due to stigma-related concerns. 23 Some Muslim participants, expressed a belief existed that contemplating death might bring it closer and alarm others: “I’m frightened, but who do I tell? If I let her know that I’m suffering so much, she (wife) may panic. So no one I can talk to but I can deal with that at the moment….” 32 Participants highlighted how talking about death or services which support people at end of life was not commonplace: “As a society we don’t talk about death, generally, in the same way that we will dedicate our time to preparing for the arrival of a new birth in the family or in the community….” 25
Moreover, some participants discussed their resistance to discussing wills and advanced planning due to cultural stigmas linked to financial matters: “They don't like to talk about the will, if the children say have you made, we need to make a will, they think that they want to take everything away from them (laughs)….” 23 Reticence to engage in discussions about death and dying was evident in instances where family members withheld information about terminal illness: “We never told our father he had cancer. He was very ill first, few days how long he survived… He didn’t know it. This is the last because there is no cure.” 27 This attitude reflected a cultural norm where conversations regarding death and dying were considered taboo within many families. 30
Discussing Death: Health Care Professional Perspectives
Healthcare professionals felt apprehensive initiating conversations about death due to insufficient training and fear of causing distress, “There's just collusion… nobody actually wants to bring it into the air and have that discussion and upset people….” 32 This discomfort suggests a mutual discomfort between healthcare providers and patients to discuss death. Moreover, providers struggled with understanding what constituted a “good death” for South Asian patients, “What does a good death look like from a South Asian patient point of view? We don’t know. All we know is a good death from a middle-class, white Caucasian… point of view.” 25
Language Barriers, Use of Interpreters, and Impact on Care
Patients with limited English faced significant challenges in communication, often relying on family members or nonverbal signals, “…they just pointed to machines and chairs and I understood….” 26 In emergency situations, this language barrier complicated articulating needs and understanding medical information, adding a layer of stress for both patients and their families, “My husband cannot speak English… if he was in somewhere where people cannot communicate with him, that would be difficult.” 26
Using family members as interpreters involved ethical and practical challenges. For example, family members could unintentionally filter the patient's voice, “I sometimes felt I got the opinion of the relative rather than the patient.” 32 This dual role can blur the line between advocacy and interpretation, leading to potential miscommunication. However, many patients preferred family interpreters due to distrust of professional interpreters and privacy concerns within their community. However, the reliance on family interpreters could be an burden, “It's a big responsibility… fairly upsetting… it's so unfair on the child.” 28 Nonetheless, some saw benefits in using family interpreters for conveying bad news sensitively, “By using a family member, you have an understanding of their personality… and they have a relationship with them.” 32 Despite the complexities, family interpreters were often seen as the most practical option.
Theme Two: The Impact of Identity and Culture on End-of-Life Practices and Rituals
The Role of Faith in End-of-Life Discussions and Care
Patients and carers highlighted how religion provided hope and emotional support, as well as the challenges of practicing faith in a hospital setting. Faith often sustained hope amidst terminal illness. A Sikh woman emphasized this, “We believe that taking medication and praying to God to help towards cure.” 24 However, maintaining hope can be a burden, “The expectations on participants to remain hopeful despite their poor prognosis and immense suffering put a tremendous burden on them.” 24
Participants stressed the importance of religious rituals at the end of life. One reflected, “I would prefer to have my children with me, and if that's not possible, then I at least want to be with someone that I can trust… and pray to God when I die.” 31 Despite the importance of faith, integrating religious practices into healthcare posed challenges. Tensions often arose between healthcare providers’ understanding of care and patients’ cultural and religious expectations. For example, issues around personal care and nudity reflected this discord, “In my religion [Islam] administering simple hygiene at the time of death should be left to the family and [my religious] community rather than nonMuslim doctors or nurses.” 29 Some participants were wary of treatments that impair consciousness, “We as Muslims, want to be alert for as long as possible in order to read our final prayers.” 29 Positive experiences occurred when healthcare staff supported religious practices, “The nurse would phone me… I’ll clean him now and you go to the temple.” 26 These accounts highlight the complex interplay between faith, cultural practices, and the need for healthcare systems to integrate these beliefs.
Gendered Perspectives on End-of-Life Dynamics
In the realm of end-of-life care among South Asian communities in the UK, gender disparities and cultural intricacies significantly shaped responses. Women, burdened with societal expectations, stoically shoulder familial responsibilities despite personal distress, as highlighted by the quote, “In Asian families, the women are expected to just get on with it, carry on with it no matter what.” 20 Conversely, men grapple with the erosion of their provider role due to illness, echoing sentiments of feeling stuck and inadequate. 23 Cultural norms dictate gender roles, influencing how pain and emotional distress are communicated. Men often refrain from disclosure, hindered by societal expectations of masculinity. Acknowledging and addressing these disparities is crucial for equitable end-of-life care, requiring culturally sensitive approaches.
Theme Three: Family Roles and Expectations Regarding Palliative Care
Family as Carers
Respect for elders is a core belief in many South Asian communities, meaning that carers have strong respect for their elders as well as a desire to fulfill their wishes around care, My mother-in-law did not want to be looked after anywhere else. I was very close to her so I did not feel that I was doing any [extra] work. I explained that I would look after her as much as I can. I wanted what my mother-in-law wanted…..
21
Many carers expressed a deep willingness and responsibility to care and there was a reluctance to opt for care homes or hospices, reflecting a desire to preserve dignity and familial pride, “Our personal thing is that he deserved to be looked after with respect. We can talk about him in a way with pride.”
21
Some participants reported stigma associated with seeking help outside of the family, Because culturally we have to look after our parents … We don't want extra support, whatever it is, you see … I think that's sort of negative. By asking somebody else, it could sort of like a negative on them.
23
Mirroring this, staff had strong perceptions that South Asian families would look after each other and have large family networks, “I think it's a very big culture thing, you know, the Asian families have a lot of family around them for a support network.” 26 The dedication of family members to remain by the side of their dying relatives without seeking external support showcased a clear sense of duty and an avoidance of potential guilt. 40
Roles and Expectations of the New Generation in End-of-Life Care
Many participants expressed a strong connection to their cultural roots and expressed concerns about the potential loss of their heritage across subsequent generations living in the UK. One patient spoke about how in the past it was common for children to take their parents’ ashes to India, but now, “most of the children start putting the ashes in the river here.”
23
Some participants expressed a concern that the core tenets of their culture could be lost unless they set a strong example for their children. Despite this, participants spoke of their children adopting a different approach, If we don’t follow our culture, our son or daughters will not do the same for us. They won’t care for you when you are dying. But some people will die here and send their ashes to India. [But] my daughter said to me, look mum. If you die, I am going to spread your ashes here. I don’t want to fly to India for that.
31
Some professionals also felt that receptiveness to services varied with age, with younger people being more likely to explore what was available. 27
Owens & Randhawa 26 paid heed to the dangers of stereotyping when it comes to South Asian families, explaining that, “there was a ready acknowledgement that South Asian families may not have the desire or ability to ‘look after their own,’ especially within a context of rapid social and demographic change.” While care at home appeared to be readily adopted by many interviewees, some reflected on how in the past sending a relative to a care home or hospice might have led to stigma but thought things were changing: “So people would have talked, very much, very much so. It's not something you do [sending relatives to a care home] but it's getting more and more common.” 21
Theme Four: Navigating Challenges Across Care Settings and Healthcare Interactions
Lack of Awareness
There was a notable lack of awareness about available services among many participants, with health professionals also noting this, particularly among older adults. In one study lack of awareness of palliative care services was voiced by several carers and patients and may have accounted for periods where carers and patients were left unsupported.
21
Many participants did not know that palliative care services could be provided in one's own home “So your hospice, you actually go into people's homes. We don’t even know about that, we don’t even know about hospice at home service!.”
21
In some South Asian communities there was only a “vague awareness” of palliative care services. This was despite efforts made to increase awareness within these communities, such as relocating a hospice to a more ethnically diverse inner city and employing a South Asian liaison worker.
25
In another study a staff member noted: There don’t seem to be many (South Asian Patients) attending there and I’ve just spoken to one and she's got no idea what it's about that's why she wouldn’t go. But when we actually got her to go, she started attending and she really likes it… highlighting how some patients may be missing out on services which could benefit from.
27
Similarly, another study 28 found most patients and their families had a limited understanding of their, or their relative's health condition and had limited awareness of the services available.
Experiences with Hospital and Homecare Services at the End of Life
A prominent thread running through all participants’ narratives was the significance of cultural considerations in end-of-life care. This was particularly evident in the difficulties faced when homecare staff did not adhere to cultural norms. The home was seen for many as a locus of cultural identity and intimacy, and most participants expressed a preference to die at home. One carer recounted a situation where a homecare worker declined to remove their shoes indoors, which was culturally important, leading to a conflict: “I asked her to take her shoes off…she went back and complained.” 32 Carers highlighted their struggle in securing culturally appropriate care, often encountering limited availability of staff who could cater to their cultural needs: “When the carer requested another homecare attendant, he was told there were a limited number of attendants available.” 32
Some carers and patients had negative experiences of hospital care, which lead to guilt and frustration on the carer's part: He suffered a lot because of their lack of attention. Next morning, when I went early, I felt very bad. I saw one cup of cold coffee and his capsules … everything is there… (in front of him), but nobody bothered about how the man can take of himself.
40
Another participant explained that their loved one was left in an unhygienic state, leaving them reluctant to put their faith in healthcare staff: “So, how can we trust such people for our problems?” 40
One individual recounted their friend’s husband receiving excellent care at the hospital, expressing satisfaction with the attentive treatment provided by nurses which encompassed culturally appropriate language, kindness and appropriate medical care. “He was taken care by nurses very well. Everyone liked him and they called him uncle … so we also have that kind of experience. They gave him his food, medication and talked nicely with him.” 40
Participants faced multifaceted challenges when accessing and utilizing formal support services. Negative experiences with these services included perceptions of long delays, inadequate care packages, and language barriers. 23 Cultural and religious obligations sometimes clashed with scheduled support services, leading to restricted access or nonparticipation. Conflicts between children’s religious activities and scheduled therapy sessions hindered one participant's involvement in emotional support services, impacting the ability of the family to access these resources. 22
In certain instances, healthcare providers encountered challenges when determining the involvement of family members in caring for the patient. For example, one healthcare provider observed that a patient's daughter played a significant caregiving role, aligning with family's preference to be the main providers of support: “I think (daughter) had helped her mum so much in the earlier stages—helping her managing her menstruation, showering, and everything was so…it's such a lot.” However, interviews with the patient showed that she did not think her daughter should take on such responsibilities: My daughter was only 12 and I was told you’ve got family. I said for God's sake, my daughter is only 12. What you want me to do tell her to drop out of school and stay with me all the time?.
22
Discussion
The aim of this review was to explore the experiences and needs of South Asian patients and their carers regarding end-of-life and palliative care services in the UK, while also incorporating the perspectives of healthcare staff working in these services. The review identified four primary themes: barriers and facilitators to end-of-life discussions, the impact of identity and culture on practices and rituals, family roles and expectations, and navigating challenges across care settings. While the review focused on literature from the UK, the findings have implications for many Western countries in which South Asians have immigrated and settled.
The reluctance to engage in end-of-life discussions, as observed in theme one, aligns closely with Terror Management Theory. 41 This theory suggests that individuals construct and maintain cultural worldviews to manage the existential anxiety associated with the awareness of mortality. For South Asian communities, these worldviews often include religious and cultural beliefs that discourage open discussions about death, seen as potentially inviting bad luck or hastening death. This cultural stigma around discussing death reflects a broader societal discomfort with mortality, which can impede the uptake of palliative care services. This highlights the need for cultural humility among healthcare providers, which is essential in addressing these beliefs. 7 The discomfort healthcare providers expressed when discussing end-of-life care with South Asian patients indicates a gap in cultural competency that could be addressed through targeted training and education. The review's findings on the impact of language barriers and the use of interpreters is mirrored in the existing literature on healthcare communication. 42 The ethical and practical challenges of relying on family members as interpreters have been well documented, with concerns about the accuracy of information conveyed and the potential emotional burden placed on family members, particularly children. This issue is compounded by the fact that many South Asian patients may prefer family members over professional interpreters due to concerns about privacy and trust. 20 These dynamics highlight the need for healthcare providers to be aware of the potential pitfalls of using family interpreters and to seek alternatives, such as professional interpreters or bilingual support workers, where possible.
Theme two's exploration of the role of faith in end-of-life care is well supported by existing theoretical frameworks that emphasize the importance of spirituality in coping with terminal illness. 43 Faith often provides a source of hope and comfort, as seen in the narratives of the participants in this review. However, tensions can arise when healthcare practices conflict with religious beliefs. The review highlights the need for a more nuanced understanding of these beliefs among healthcare providers, suggesting that guidelines on spiritual care in palliative settings should be more widely implemented. Gender norms and expectations also have significant implications for caregiving in South Asian communities. The current review found that women often bear the primary responsibility for caregiving, reflecting broader societal expectations about gender roles. In contrast, men's narratives frequently centred on their distress at being unable to contribute financially, with some struggling to voice emotional distress due to perceived norms of masculinity. 20 This finding is consistent with previous research 44 which found that Bangladeshi men traditionally rely on female family members for support. Given these findings healthcare providers should be aware of these dynamics and offer additional support to female caregivers who may experience carer related stress or burnout. In parallel, several participants noted a generational shift in attitudes. Younger South Asians appeared more open to discussing and accessing palliative care, potentially due to greater exposure to British healthcare systems and more flexible interpretations of cultural norms 26 . These shifts present opportunities to engage younger family members as advocates for early planning and to co-design culturally sensitive care strategies that bridge traditional values with contemporary perspectives.
Theme three focuses on the role of the family and cultural expectations of this in South Asian communities. However, this responsibility often comes with challenges, including reluctance to seek external support due to stigma and cultural expectations. Younger South Asians are increasingly open to using palliative care services, reflecting broader social changes. The findings suggest the need for culturally sensitive palliative care models that respect traditional values while accommodating evolving attitudes among younger generations. Integrating cultural competence into care practices is crucial for effectively supporting these families.
Finally, theme four highlights the lack of awareness about available palliative care services among South Asian communities, particularly older adults. This finding is consistent with studies that have shown that ethnic minorities in the UK often have limited knowledge about healthcare services, which can lead to delays in seeking care. 45 The review suggests that increasing awareness and understanding of palliative care among South Asian communities should be a priority for healthcare providers and policymakers.
While this review highlights overarching barriers and facilitators to palliative care among South Asians in the UK, it is also important to recognize the diversity that exists within this population. Although commonly grouped under the term “South Asian,” individuals from Indian, Pakistani, Bangladeshi, and Sri Lankan backgrounds, as well as those identifying as Sikh, Hindu, Muslim, or Christian, may have differing beliefs, language needs, and care preferences. Several studies in this review included participants from diverse ethnic and religious groups, yet many did not disaggregate findings by subgroup. Nevertheless, qualitative insights pointed to important variations in how illness, death, and palliative care were approached. For example, Muslim participants often referenced the significance of prayer and modesty, 29 while Sikh families emphasized community support and collective decision-making. 21 In addition, there are other important differences such as language barriers which were more commonly noted among older generations and those with limited English proficiency, affecting access to services and trust in providers. Socioeconomic status further shaped experiences, with working-class participants citing financial constraints as limiting their engagement with formal care services. 22 These findings highlight the need to move beyond generic categorizations and instead adopt a more nuanced, intersectional approach when designing and delivering palliative care services for South Asian communities in the UK.
Practice and Research Recommendations
The findings of this review suggest several practical recommendations for improving palliative care services for South Asians. First, there is a clear need for enhanced cultural competence training for healthcare professionals. This training should not only address the specific cultural and religious beliefs of South Asian patients but also provide healthcare workers with the skills to navigate difficult end-of-life conversations. This could include training on how to approach discussions about death in a culturally sensitive manner, recognising the importance of religious practices, and understanding the role of family dynamics in decision-making processes. In addition, healthcare providers should be encouraged to involve South Asian patients and their families in the co-design of palliative care services. This could help ensure that the services provided are relevant and culturally appropriate, thereby improving patient satisfaction and outcomes.
Research should focus on developing and testing culturally tailored interventions that address the specific needs of South Asian patients. These interventions could include community-based education programs aimed at increasing awareness of palliative care services, as well as initiatives to improve language services within healthcare settings. Additionally, future studies should explore the role of clinical psychologists in palliative care, particularly in providing emotional support to both patients and healthcare staff. This review noted a significant gap in the literature regarding the role of psychology in palliative care, suggesting an area ripe for further exploration. Finally, the role of family members as caregivers should be further investigated, with a focus on how healthcare providers can better support these individuals, particularly in light of changing gender roles and expectations.
Internationally, culturally sensitive models of palliative care have been implemented with success. In Canada, community engagement efforts involving South Asian temples and gurdwaras have enhanced awareness and acceptance of palliative care services among immigrant populations. 16 Similarly, in Australia, tailored models for Indian migrants have incorporated spiritual care, family-centred planning, and language support to improve care experiences. 17 These examples illustrate how meaningful collaboration with community organizations can extend outreach, reduce stigma, and improve service delivery. In the UK, similar partnerships with trusted community and faith leaders may help co-design services, promote health literacy, and create culturally congruent care environments.
Strengths and Limitations
One of the strengths of this review lies in its focus on a specific minority group within the UK, providing valuable insights into the unique experiences of South Asian patients and their families in palliative care settings. The thematic synthesis approach allowed for a rich, in-depth understanding of the data, highlighting the multifaceted challenges faced by this population. However, the review also has several limitations. The review was limited by the scope of the included studies, many of which did not disaggregate data by specific South Asian subgroups. This lack of specificity may obscure important differences in experiences and needs between different South Asian communities, such as between Indian, Pakistani, and Bangladeshi patients. Furthermore, the review highlighted a gap in the literature regarding the role of psychology in palliative care for South Asian patients, with few studies addressing this aspect of care. The subjective nature of qualitative research, along with potential biases in data interpretation and the reliance on family members as interpreters, also poses challenges to the reliability and validity of the findings. Another limitation is that the review did not fully explore the potential impact of socioeconomic status, education level, or acculturation on the experiences of South Asian patients in palliative care. These factors could play a significant role in shaping patients’ access to and experiences of care, and future research should aim to address these gaps.
Conclusions
In conclusion, this review highlights the critical importance of culturally sensitive approaches to palliative care for South Asian communities in the UK. The findings suggest that addressing cultural and language barriers, involving patients and caregivers in the planning and delivery of care, and enhancing the cultural competence of healthcare providers are essential steps towards improving the quality of end-of-life care for this population. The findings from this review could inform policy and practice, contributing to the development of more inclusive and equitable palliative care services across the UK and other Western countries in which South Asian populations have settled.
Supplemental Material
sj-docx-1-pal-10.1177_08258597251343932 - Supplemental material for South Asian Experiences of Palliative and End-of-Life Care Provision in the UK: A Systematic Literature Review and Thematic Synthesis
Supplemental material, sj-docx-1-pal-10.1177_08258597251343932 for South Asian Experiences of Palliative and End-of-Life Care Provision in the UK: A Systematic Literature Review and Thematic Synthesis by Jane Pardi, Eleanor Nuzum, Ugne Judickaite, Joshua Stott, Georgina Charlesworth and Roopal Desai in Journal of Palliative Care
Footnotes
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Supplemental Material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
