Abstract
Objectives
Pediatric end-of-life (EOL) care at home is often provided by community palliative care (CPC) nurses who are not specialist pediatric service providers. This study explores the challenges, benefits, and future directions of home-based EOL care as perceived by CPC nurses in New South Wales (NSW), Australia.
Methods
Eleven CPC nurses participated in a semi-structured interview to elicit information about their attitudes and experiences regarding their work in providing community-based EOL care to children. Reflexive thematic analysis was used to explore themes regarding the benefits, challenges and their thoughts on future directions regarding home-based EOL care.
Results
Challenges identified by CPC nurses included resource access, complexity of pediatric, models of care, and family psychological factors. Benefits included patient and family autonomy, home comforts and the nurses’ sense of satisfaction. CPC nurses suggested the need for increased education, support and collaboration.
Conclusion
Areas of possible clinical and organizational improvements are discussed, including more pediatric training and experience for CPC nurses.
Introduction
Pediatric end-of-life (EOL) care is the provision of physical, psychosocial and spiritual care to a child living with a life-limiting condition and their family during the child's final stage of life. 1 Life-limiting conditions may include a broad range of conditions, with variable symptom profiles and illness trajectories. 2 The EOL care phase spans from a few hours to days and, in some cases, weeks.3, 4 Care during this period may be provided in a hospital, hospice, or home, with many patients and families preferring home-based EOL care.5–8
It is widely acknowledged internationally through key policy documents that collaboration with families about desired location for EOL care is an important component of quality pediatric palliative care. The American Academy of Pediatrics supports palliative care across a range of settings including the home, while acknowledging that preferences for location of death (LOD) are not always achievable. 4 The NICE guidelines in the UK promote choice in location of EOL care where possible. 9 Similarly, the Australian Commission on Safety and Quality in Health Care (ACSQHC) – National Consensus Statement 1 recommends that clinicians discuss alternatives to hospital-based EOL care and consider patient and family preferences.
Formal EOL care in the home setting is typically provided by community-based palliative care teams. The nature and availability of community-based palliative care services vary across countries and regions. These teams typically do not specialize in pediatrics,10–12 but care for children at the EOL when required. Notably, though, effective EOL care for children differs from that of adults. It requires knowledge of life-limiting conditions seen in childhood,13, 14 an understanding of pediatric medications and dosages, 15 and an ability to offer emotional support to caregivers and siblings. 16 Some documented challenges in the context of pediatric home-based EOL care relate to the coordination of care across facilities and between healthcare teams, 17 access to specialized training and resources,11, 12 availability of 24-hour services,13, 18 the emotional toll faced by the nurses,19–22 and staying within professional boundaries.13, 20
Documented benefits associated with effective pediatric EOL care in the home setting include familiarity and comfort for the patient and family,23, 24 parents being able to take an active role in their child's care,8, 25–27 greater scope for sibling involvement, 28 fewer hospitalizations, 29 and accommodation of religious and cultural practices. 30 Nevertheless, home-based pediatric EOL care may not be a preference or logistically possible for all families.4, 31
To date, most research exploring the potential challenges and benefits of home-based pediatric EOL care has been from the perspective of the family.17, 32 These studies highlighted the importance of families having opportunity to establish trusting relationships with care providers, receiving well-coordinated, family-centered care extending beyond the child's death, within the home environment.17, 32 However, there is a gap in our understanding of the challenges and benefits of pediatric home-based EOL care from the perspective of CPC nurses.
This qualitative study is part of a larger explanatory sequential mixed-methods 33 project, with the quantitative study component reported elsewhere. 34 The current qualitative study had two broad aims. The first aim was to identify challenges and benefits of home-based pediatric EOL care from the perspective of CPC nurses in NSW. The second aim was to document future directions, and possible strategies for improving home-based pediatric EOL care, as identified by CPC nurses.
Methods
This research is the second phase of a two-phase explanatory sequential mixed-methods design, 33 consisting of a predominantly quantitative survey reported elsewhere, 34 followed by a semi-structured interview. A reflexive thematic approach 35 , 36 was used to analyze the qualitative interview data. This study was approved by the Sydney Children's Hospital Network Human Research Ethics Committee (approval number 2022/ETH02393).
Participants
Participants were CPC nurses recruited from metropolitan, regional and rural locations of NSW, Australia. The inclusion criteria were: (1) employed as specialist CPC nurses, (2) worked for a service that accepts pediatric referrals, (3) had cared for at least one child at EOL in the last five years, and (4) had participated in an online survey asking about their experiences caring for pediatric patients at EOL and had expressed willingness to be contacted for an additional interview.
Of the 52 nurses who participated in the online survey, 26 were willing to be contacted to be invited for an interview. A total of 13 were invited to participate in an interview, with selection based on varied location of work, age and years working in CPC and invited to take part in an interview. Of those, two were unavailable at the time of contacting and 11 participated in an interview.
Procedure
Semi-structured interview questions were developed following an analysis of the quantitative phase of the research. 34 Broadly the interview covered the following areas: (i) questions about the challenges experienced when providing home-based EOL care to children, (ii) questions regarding any benefits associated with home-based EOL care for children, and (iii) questions regarding participant thoughts about potential changes that could help improve the EOL care experiences of patients, families, and CPC nurses. (See Supplemental Materials for the Interview Schedule.) Online semi-structured interviews were conducted by a student medical researcher (MH) who was unknown to all participants, with a second researcher present (ME). The second researcher was a pediatric palliative care nurse practitioner known to some participants. Interviews took approximately 45 minutes. Interviews were recorded using the Teams platform, transcribed from recordings and then deidentified for coding and analysis.
Analyses
Analysis of semi-structured interviews utilized a reflexive thematic approach. 35 , 36 This approach accounts for researcher reflexivity and awareness of their positionality during the analysis process. The following steps were taken: (1) Two coders familiarized themselves with the data (MH and SC). (2) One coder (MH) generated initial codes through analysis of the data, utilizing NVIVO software 37 to organize and code the data. (3) Codes were grouped into themes by both coders through an iterative process involving ongoing discussions and reflexivity, where coders critically examined their interpretations and any potential biases that might influence theme development. (4) Themes were reviewed and grouped into overarching themes. (5) Thematic groupings were further refined to ensure they accurately represented the nuances of the data. (6) Illustrative quotations were selected from the transcripts to support each subtheme.
Results
Sample Characteristics
Participant characteristics are outlined in Table 1. Ten of the interview participants were female and one was male. Gender information is not presented in Table 1 to preserve participant anonymity.
CPC nurse demographics.
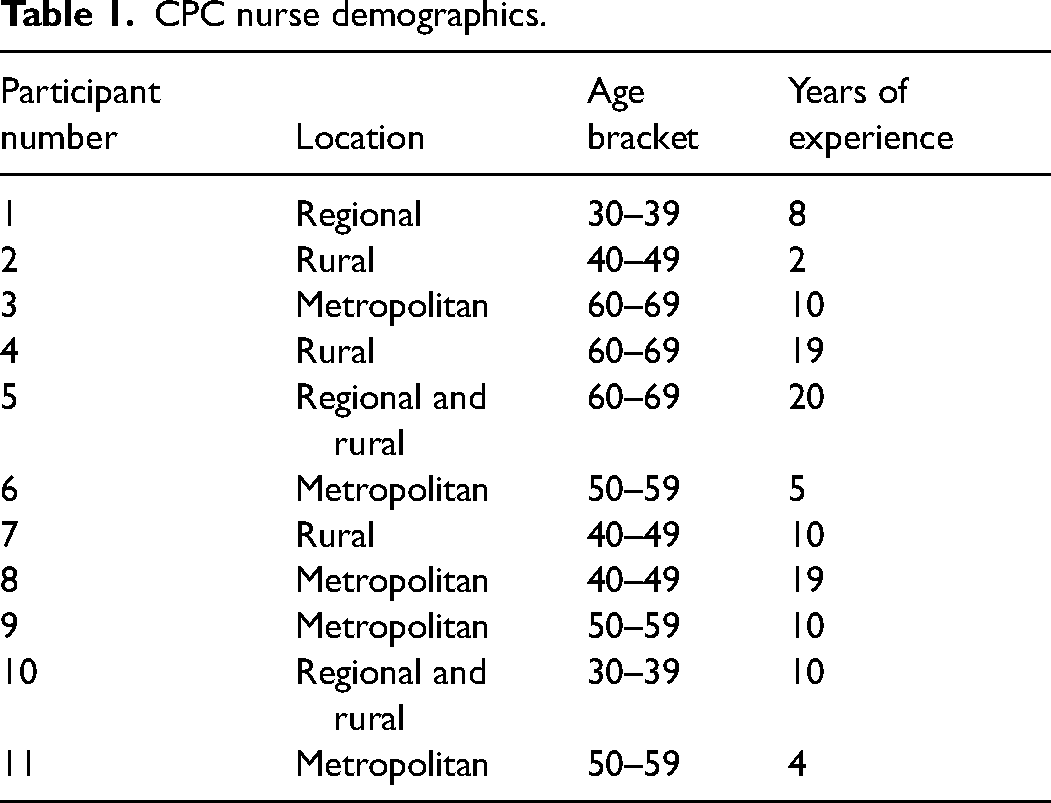
Themes Regarding Challenges Experienced
Within the domain of challenges experienced by CPC nurses caring for children at EOL, four key themes emerged: (i) access to resources and education, (ii) uniqueness of pediatric care, (iii) models and systems of care, and (iv) family psychosocial factors. These themes, along with subthemes, are shown in Figure 1 and are described as follows.
(i) Access to resources and education. This theme highlighted the challenges associated with access to resources, especially pediatric specific resources, including medications, equipment, pediatric services, and allied health and pediatric education. Comments pertaining to access related difficulties were more commonly made by rural and regional CPC nurses, but some metropolitan CPC nurses also reported access difficulties. For example, several respondents made comments regarding difficulties with access to equipment and medications, such as:So, none of our equipment was pediatric standard…so it was kind of, just making do with, with what equipment we had. Yeah, that was difficult. (Nurse 5 – Regional and Rural, 20 years CPC experience)
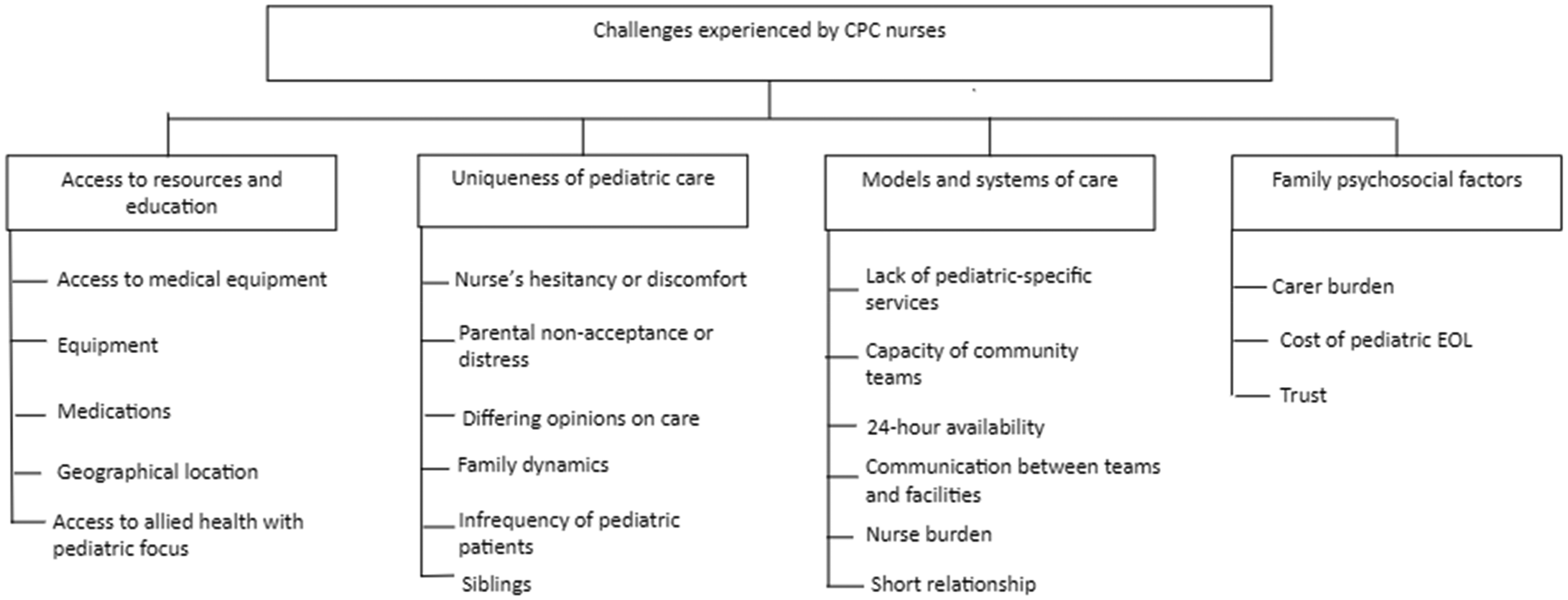
Themes and Sub-themes pertaining to the challenges experienced by CPC nurses.
Getting the original order through [was difficult] … even the simple logistics like that, but also having the medications available…. (Nurse 8 – Metropolitan, 19 years CPC experience)
One rural respondent highlighted their insufficient pediatric training:
I haven't had any training in pediatric EOL care. I've just winged it. (Nurse 4 –Rural, 19 years CPC experience)
One comment illustrated the fundamental challenges related to all aspects of access when caring for some rural families: She lives a long way out of town. She doesn't have much mobile phone reception and it's very difficult access. If she gets any sort of flood water or they get any heavy rain, we cannot get to her property. (Nurse 7 – Rural, 10 years CPC experience) (ii) Uniqueness of pediatric care. This theme related to the distinctive challenges associated with pediatric EOL care. It entailed the nurses’ hesitancy or discomfort caring for children at the EOL as seen in this quote:…one of the probably the biggest issues of people [nurses] saying ‘I don't want to go. I don't want to see children. I don't know about the medications. I wouldn't feel comfortable giving, you know, morphine or something to a child’ cause they're not, you know, used to dealing with children. (Nurse 9 – Metropolitan, 10 years CPC experience)
This theme also highlighted the challenges which CPC nurses described related to managing the unique involvement of parents. For example, nurses expressed challenges in managing and responding to parental distress and non-acceptance of the child's circumstances, as well as managing situations where parental opinions on care differed from the nurse's: Parents never want to let go, so they never want that time to come. Obviously, no, none of us would. … Parents are reluctant because, by giving more medication means things are getting worse and also … don't want them to be sedated, they want them to still be able to respond in some way. (Nurse 9 – Metropolitan, 10 years CPC experience) Sometimes the family interpreted their symptoms differently to what I might interpretate [sic] them. (Nurse 4 –Rural, 19 years CPC experience)
Other nurses reported unique challenges pertaining to the management of complex family interactions with the presence of extended family members and well-siblings. For example: Complex family relationships probably, and a very large extended family in the home environment that made it quite chao…, not chaotic, but a busy, and loud environment. (Nurse 5 – Regional and Rural, 20 years CPC experience) The dynamics with the other children, when there are other children in the families, they can be a bit challenging … (Nurse 4 –Rural, 19 years CPC experience)
CPC nurses reported a key factor associated with their challenges working with children at the EOL stemmed from the infrequency with which they are required to care for pediatric patients. Maintaining a level of consistency and skill base for the staff, and for them then to feel supported and appropriate in what care they're providing is difficult because it's not, it's not frequent enough, which is a good thing, but… (Nurse 8 – Metropolitan, 19 years CPC experience)
As a result of the infrequency of paediatric EOL patients that they see, one CPC nurse alluded to their lack of an established relationship with the primary clinical teams caring for the patients: I think the biggest thing is probably getting the trust in a new team, … it takes a long time to build trust. And then at the, probably I'd imagine, the most difficult time of the process you’re then at home and then you got this other nursing team in there that you've never met. (Nurse 8 – Metropolitan, 19 years CPC experience) (iii) Models and systems of care. This theme related to the challenges around the varied, and at times ad hoc, nature of caring for pediatric EOL patients within predominantly adult community care systems. The respondents noted various system shortfalls, such as lack of 24-h support and lack of pediatric-specific services.We're not available 24 hours a day. When do things happen? Tend to happen overnight. (Nurse 7 – Rural, 10 years CPC experience) The lack of pediatric specific services, so to get a pediatric speech, pediatric OT on site is, impossible I guess. (Nurse 5 – Regional and Rural, 20 years CPC experience)
Other systemic and organizational challenges noted included sub-optimal communication between teams and facilities, high levels of nurse burden, and having a short relationship with families. They're a bit scared to let go of [hospital-based pediatric palliative care team] and trust us, and we tend to come in when things are going really bad. (Nurse 9 – Metropolitan, 10 years CPC experience) There isn't the knowledge sharing across the team. Because of that, I will just give it to that nurse cause they're comfortable and then, that nurse is then also the one that is taking on, you know, that higher nursing burden. (Nurse 8 – Metropolitan, 19 years CPC experience)
(iv) Family psychosocial factors. This theme pertained to challenges associated with the family's psychosocial factors, as perceived by the CPC nurse, one CPC nurse reported challenges associated with managing issues stemming from significant levels of parent/carer burden and burnout from caring for their child at home.…the parents, feel like they can’t leave their side, so there's a massive carer burden, carer stress. They’re not doing any self-care, not looking after themselves. Yeah, I think that's the biggest challenge in that, you know, if it does prolong and it's a long EOL journey, they tend to burn out quite quickly and it's hard to kind of manage. (Nurse 1 – Regional, 8 years CPC experience)
Other family psychosocial stressors reported included financial pressures: I feel quite sorry for them because it's such a huge thing that they're going through. And it's expensive. It is so, so, so expensive. And if they've got to get carers and things in, nine times out of ten, they’re having to pay for that, out of their own pocket. (Nurse 4 – Rural, 19 years CPC experience)
Themes Regarding Perceived Benefits
Within the domain of perceived benefits, three key themes were identified, namely (i) patient and family autonomy, (ii) home environment, and (iii) nurses’ own well-being or satisfaction. Each of these themes and subthemes are presented in Figure 2 and will be further described.
(i) Patient and family autonomy. This theme related to the empowerment of the patient and their family in decision-making, respecting their wishes and providing them with a sense of control. Within this theme CPC nurses identified home-based care as fostering a sense of normality for the family. For example:I think, particularly if they've got other children in the house, um, it's sort of a little bit more normalised, the situation, and those other children can sort of still go about their daily routines… Parents can still be fiddling and doing washing or you know, sort of normal kind of activities. (Nurse 9 – Metropolitan, 10 years CPC experience)
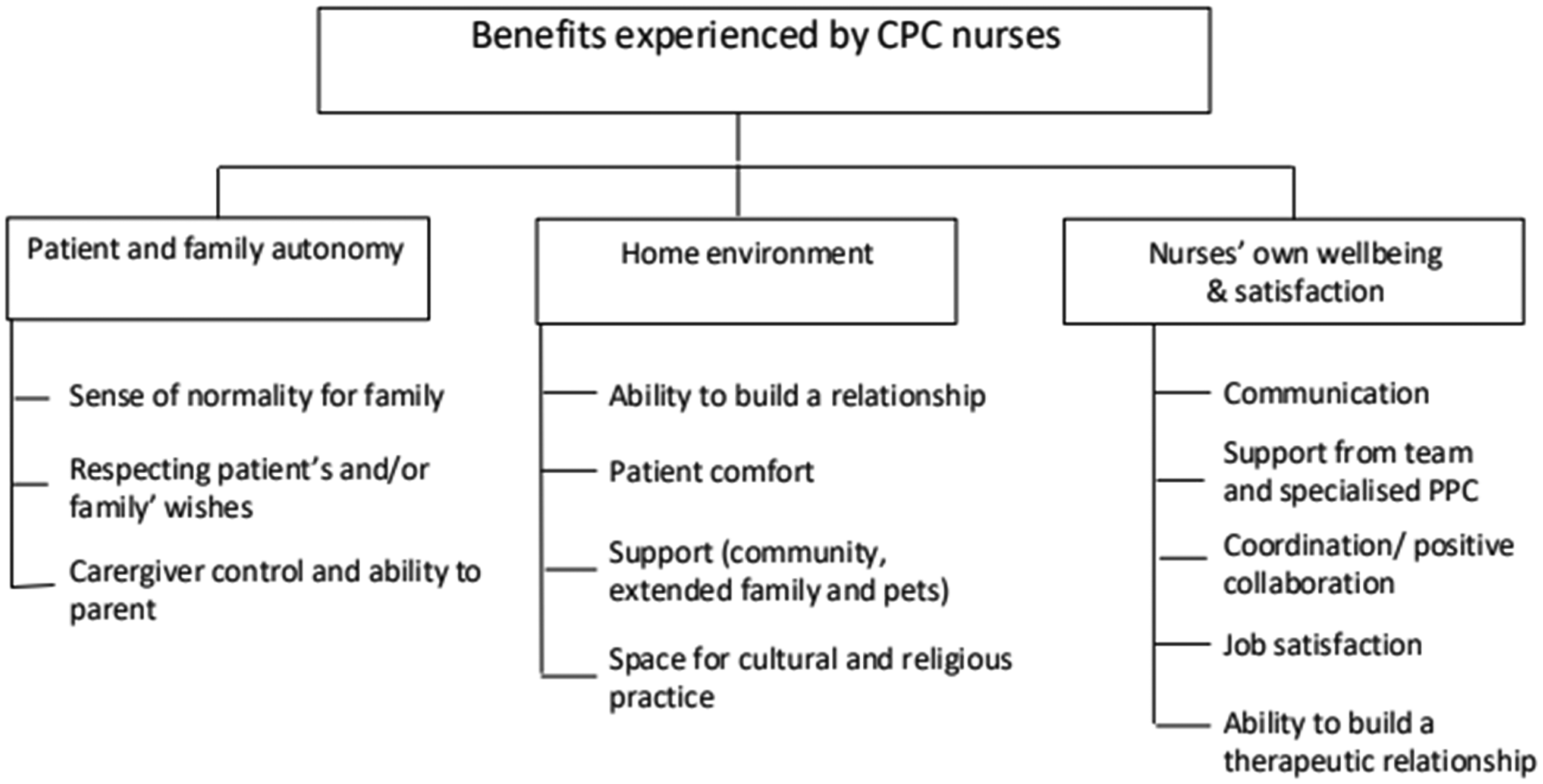
Themes and sub-themes pertaining to the perceived benefits noted by CPC nurses.
Respecting the wishes of patients and their families was also highlighted as a benefit of home-based EOL care, as was providing patients and caregivers a sense of control and empowerment during a time where so much control is lost. One rural CPC nurse noted that: Most young people want to die at home. They've spent a lot of their time in the hospital, and they want to be home. (Nurse 7 – Rural, 10 years CPC experience) Because we're giving the patient, we're giving the carer autonomy. And I think that's very important in this situation. They need to feel that they have got some control over something, because they've lost so much control over everything else. (Nurse 4 –Rural, 19 years CPC experience) (ii) Home environment. This theme related to the benefits of the home environment as a location of care that provides a greater ability for health professionals to establish rapport and build relationships with families while also promoting patient comfort.You sort of tend to walk in and if everyone around you is a little bit more relaxed and comfortable and the environment … you do stay for a cup of tea or whatever and things like that which you wouldn't necessarily do in a hospital, in a hospital room. (Nurse 7 – Rural, 10 years CPC experience) I think the benefit is that they're in their own home. You know, they're with their loved ones they’re with their family, they're in their bedroom, they're in their- wherever they want to be. They got their own clothes, their own toys, their own, you know, the family are there and it's, you know, it's just that they can be with everybody who they want to be. (Nurse 6 – Metropolitan, 5 years CPC experience)
CPC nurses also identified the home environment as facilitating opportunities to support the wider family unit, with opportunities for spending time together as a family, remaining close to family pets, and greater engagement in cultural and religious practices. This was illustrated in the following two quotes: Being at home in their own home with their siblings or their friends or family being able to visit. It's just a much more positive experience. (Nurse 8 – Metropolitan, 19 years CPC experience) That can happen in the home, in their space, that the whole family can be involved in. So I think it definitely opens up that ability for, for people to be able to express their religion, their culture. (Nurse 8 – Metropolitan, 19 years CPC experience)
(iii) Nurses’ own wellbeing and satisfaction. This theme encompassed nurses’ own perception of their wellbeing and job satisfaction in providing home-based pediatric EOL care. Respondents expressed satisfaction in situations which were marked by positive collaboration with other teams:So it was a pretty big collaboration and … we're all on the same page because I find as well even when we receive a referral from say Sydney Kids, they stay involved, like they're still a main support system for the family and patient. So, it is handy to be able to establish that regular catch up and, you know, we can bounce ideas off each other. (Nurse 1 – Regional, 8 years CPC experience)
One CPC nurse spoke highly of the support received when caring for a child at the EOL: Ultimately I think the support that we receive with children is phenomenal and probably far outweighs anything that we ever receive for adults. (Nurse 5 – Regional and Rural, 20 years CPC experience)
Moreover, CPC nurses described the benefits of establishing good rapport with families in their home environments and satisfaction when the team was able to manage the EOL care situation well: It's nice to see, you know, that their home in their own environment, but for children especially, … it's just a peaceful, more relaxed environment and they're … with their loved ones, where their family can lie with them in the beds they can, you know, just be with them. …it's a nice process to watch and be involved with… it's just very comforting and reassuring, special, it's special. (Nurse 6 – Metropolitan, 5 years CPC experience) For me, when you've been able to support your team to be able to provide that care and then… be like, yeah, that was a job really well done. It's a really sad and distressing situation, but this is what we've been able to do as a team. (Nurse 8 – Metropolitan, 19 years CPC experience)
Finally, there was recognition by some respondents that having exposure to pediatric EOL cases helped them to develop as a clinician: I think there's a benefit to our staff as well, um, getting that exposure and those experiences like it only makes you grow as a clinician and improve your own practice. (Nurse 1 – Regional, 8 years CPC experience)
Themes regarding future directions identified by nurses.
Three themes were identified regarding future directions identified by CPC nurses, namely (i) education and training, (ii) collaboration, and (iii) support. These themes and sub-themes are presented in Figure 3 and will be further described.
(i) Education and training
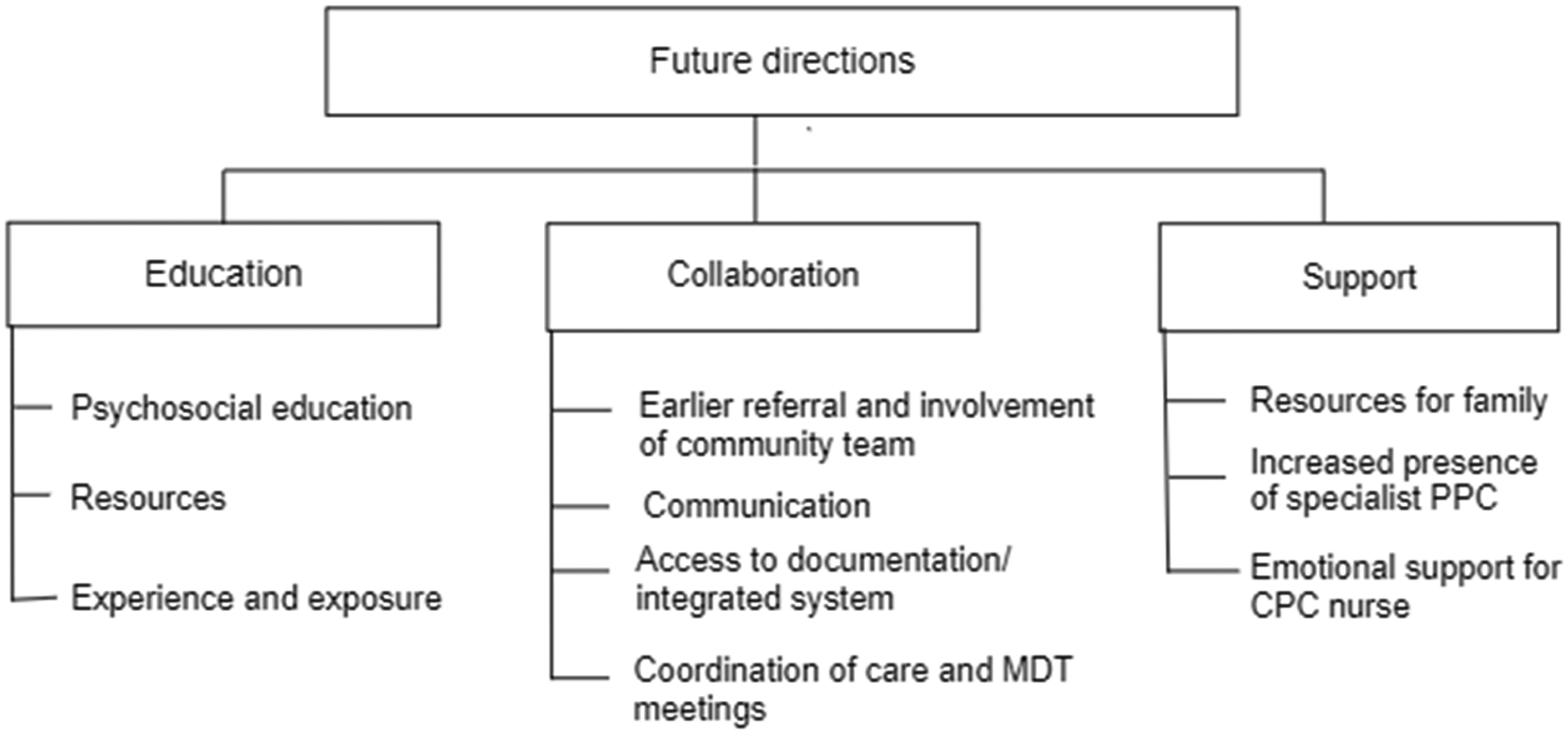
Themes and sub-themes pertaining to potential future directions identified by CPC nurses.
In addition to wanting more knowledge about available pediatric resources, many CPC nurses also expressed a desire for greater psychosocial education specific to the pediatric context. I mean, it's the same medications, the same administrations, it's the same assessments we do on everybody (ie adult patients), I think it's more around that emotional education [in pediatric EOL care context] of how to manage situations that are, you know, difficult. (Nurse 9 – Metropolitan, 10 years CPC experience)
Furthermore, many CPC nurses expressed a desire to gain greater experience and exposure to pediatric patients. I mean it would be really good if somehow, again, management probably wouldn't approve it, but we could rotate staff to come and, you know, just spend a day with [hospital-based pediatric palliative care team] and just go on your rounds and just see how you have those conversations with parents, see how you handle those situations where people are quite distressed. I think that would just give … a bit of guidance around it I suppose. (Nurse 10– Regional and Rural, 10 years CPC experience
(ii) Collaboration. This theme emphasized the importance of optimizing interactions within and across teams, as illustrated by this quote.Better collaboration between the specialty team and the local team is obviously a great way to improve patient outcome, and family outcome. (Nurse 1 – Regional, 8 years CPC experience)
More specifically, optimized interaction between teams was believed to lead to earlier community palliative care referrals. If there was a child that was approaching the palliative stage of any treatment… I think it would be good way then for us to be flagged and involved a little bit earlier. (Nurse 7 – Rural, 10 years CPC experience)
It was proposed that these early referrals could be actioned by making introductions between the family and the CPC nurses at the time of discharge from hospital: I know there's a lot of case conferencing and case reviews or planning that goes into getting a kid home, maybe even us being invited to participate in one of those sort of things. So the families can actually meet us prior to. (Nurse 6 – Metropolitan, 5 years CPC experience)
Several CPC nurses also expressed that it would be helpful to have an integrated system of documentation across hospital and community teams EMR [electronic medical records], wouldn't that be good if we had a system where, you know, we didn't have to rely on sending emails and phone calls and, you know, oh, let me send you a copy of our medication chart so you can write it on your charts…. (Nurse 8 – Metropolitan, 19 years CPC experience)
(iii) Support. In this theme, CPC nurses alluded to the need for comprehensive support systems, both for families and for the nurses themselves. This theme includes subthemes related to the availability of physical and emotional support and resources for families (eg, personal care, shopping, cleaning, and assistance with siblings).… support service, so the, you know, personal care, shopping, cleaning, looking after the siblings. Like all of that stuff needs to be much more responsive and that's going to be the biggest thing that you can do, yeah because at the moment it's just really slow and clunky. (Nurse 3 – Metropolitan, 10 years CPC experience)
Respondents also commented that CPC nurses would benefit from interactions with the specialist PPC team: Physical attendance is always going to trump every, you know, it will always be the ideal, especially in regional rural areas where the expectation is oh, we live in the country, we’ll be forgotten about. (Nurse 5 – regional and rural, 20 years CPC experience)
They also expressed a desire for greater emotional support for the role that they carry out. Maybe like um some communication or even like a little, debrief kind of thing before we go in… (Nurse 2 – Rural, 2 years CPC experience)
Discussion
This study provides information about the experiences of CPC nurses when providing home-based EOL care to children. This information is important given that CPC nurses are typically more familiar with caring for adult patients and may face unique issues when providing home-based EOL care to a child. The current qualitative data complements and extends on the quantitative data exploring these issues published previously. 34 Moreover, the current data provides valuable data on CPC nurse perspectives of home-based EOL care to complement the available literature documenting parental perspectives about home-based EOL care. 17 , 32 In line with the study's first primary aim, a thematic analysis was conducted to better understand the challenges and benefits of home-based pediatric EOL care as perceived by CPC nurses. Consistent with our second primary aim, CPC nurses shared insights into possible future directions for improving home-based pediatric EOL care. These are discussed as follows.
Challenges
“Access to resources and education” was a key theme that emerged from the CPC nurses’ discussion of challenges when working with pediatric patients. Participants reported challenges in accessing pediatric-specific education, as well as accessing medications and equipment needed for pediatric patients receiving EOL care. Other studies have reported similar gaps in access to resources and training in pediatric palliative care.12, 38 However, the current study noted that this was a particular challenge for those working in regional and rural locations. Moreover, CPC nurses commented that support from specialist, city-based pediatric teams were not always readily accessible by nurses working in regional and rural locations.
The second theme related to “the uniqueness of pediatric care” and the specific challenges encountered by CPC nurses when caring for children in a predominantly adult-focused palliative care team. Nurses expressed hesitancy and discomfort providing EOL care to children. A lack of confidence in caring for children at EOL has been widely documented in the literature.16, 34, 38 Caring for pediatric patients requires extensive interactions with caregivers and families.16, 38 Nurses in the current study reported finding it challenging to build trust and rapport with families when they became involved late in the patient's disease trajectory. Other unique pediatric challenges reported by the CPC nurses included managing family dynamics, parental distress, parental non-acceptance of the child's prognosis, and management of symptoms, particularly when nurses’ clinical assessment of the patient differed from the parents’ opinions. Some CPC nurses in the current study reported that they lacked experience and knowledge of how to involve well-siblings in a developmentally appropriate way. This is significant given that it is documented in the literature that well-siblings desire involvement in the lives and care of their sick brother or sister.39, 40 Moreover, many families express a desire for siblings to receive greater support. 17
The third theme related to “models and systems of care”, with focus on the fact that pediatric EOL care in NSW, Australia, is provided within the context of adult-based service models. Specific challenges in connecting with appropriate pediatric-specific resources and limited organizational flexibility to achieve holistic family-centered care were reported, highlighting the need for better inter-organizational collaboration.18,41 Staffing issues and resource limitations which contributed to the lack of 24-hour availability of services was noted by CPC nurses in the current study. Similar concerns have been highlighted elsewhere by families of pediatric palliative care patients.16, 17 It was reported by CPC nurses from several services that certain nurses took on all pediatric patients, resulting in, greater nursing burden and decreased learning opportunities for others.
Benefits
Despite the challenges acknowledged, CPC nurses also identified many benefits associated with home-based pediatric EOL care. “Patient and family autonomy” emerged as a key theme regarding perceived benefits. CPC nurses identified that a sense of normality, respecting patients’ and families’ wishes, and giving carers control in caring for their child, were more readily achieved in the home environment. This is important given that the ability to maintain familial functioning and autonomy is highly valued by parents and siblings.8, 24 Furthermore, nurses in the current study commented that providing families with greater autonomy and control in caring for their child is important given there are so many aspects of the situation that families are unable to control.
A second theme related to benefits of the physical and social “home environment”. Nurses believed that greater patient comfort could be achieved, and greater support from social networks was possible, when EOL care occurred in the home setting. The home setting was considered advantageous for cultural, spiritual, and religious needs, as it allowed families’ freedom, flexibility, and space for traditional family practices. Involvement of religious and cultural leaders in practices that hold spiritual or cultural meaning for the family may be challenging to accommodate within a hospital setting. 30
The third theme pertained to the “nurse's own satisfaction and well-being”. CPC nurses who were able to successfully navigate the complexities of care coordination, respecting families’ wishes, and facilitating meaningful interactions in the home setting, described feeling a sense of accomplishment and job satisfaction. It is documented in the literature that job satisfaction in pediatric palliative care arises from feeling that one has made a positive difference in the lives of children and their families.20, 42, 43
Future Directions as Identified by CPC Nurses
The insights shared by CPC nurses in the current study regarding potential areas for improvements in service provision are valuable in helping shape future refinements to service delivery. CPC nurses in the current study identified three key themes regarding areas of potential improvement in pediatric home-based EOL care: education and training of CPC nurses, better collaboration, and optimizing support. Considering the uniqueness of pediatric care and the infrequency of pediatric EOL patients, many CPC nurses desired more training and experience with pediatric patients at EOL. In particular, nurses expressed a desire for greater training specific to patient and family psychosocial management, which was felt to be very different from the adult EOL care context.
Improvements in intra-organizational and inter-organizational communication and collaboration were flagged as potential areas of improvement. Positive collaboration and care coordination are critical for optimizing family and patient outcomes.24, 44 As has been noted elsewhere, 45 CPC nurses in the current study suggested that earlier involvement of the community team would help improve their ability to build relationships with the patient and family. Additionally, improved access to shared documentation was mentioned by several participants, with a more integrated system allowing for timely access to notes from specialist PPC or other care providers. Structured debriefing sessions were suggested as a means for CPC nurses to reflect on and discuss their experiences of caring for pediatric patients and families, thus providing processes to support CPC nurse well-being, as well as maximizing knowledge sharing.
CPC nurses expressed the desire for greater support systems for the families and themselves. Several nurses commented on families having unmet practical needs, such as supports to assist with shopping and cleaning, allowing them more time to focus on their child. It is well documented that caregivers tend to put their own needs last,46, 47 however, over time this may result in a reduced capacity to care for their sick child.
Many CPC nurses mentioned that their ability to care for children at the EOL could be improved by more contact with specialist PPC teams, whether through face-to-face interactions or telehealth. Nurses in rural and regional areas expressed a desire for increased access to specialist PPC teams and associated resources. The need for greater access to pediatric-specific equipment, medications and pediatric allied health professionals was flagged as another area requiring improvement. Strategies to improve access in rural settings is an area warranting ongoing consideration.
Limitations
Although the current study had many strengths, such as providing rich data from a diverse group of CPC nurses, several limitations should be acknowledged. CPC nurses with an interest in pediatrics may have been more likely to participate in the study, with less information gleaned about CPC nurses who have more reluctance to care for pediatric patients at EOL. Studies such as this one may be affected by memory biases, with better recollection of negatively or strongly valenced experiences. 48 Some participants had a pre-existing, professional relationship with some members of the research team, which could have influenced their responses. However, a researcher previously unknown to all CPC nurses was responsible for recruitment and interviewing. Finally, it needs to be acknowledged that EOL care experiences were reported only from the perspective of CPC nurses. It is not known how these perspectives might differ from the perspectives of families.
Research Directions
Some CPC nurses reported that certain nurses took on most of the pediatric cases in their team. Future research could explore potential barriers or reasons why some CPC nurses do not care for children at EOL. To gain a deeper understanding of the evolving experiences and challenges faced by CPC nurses, prospective, longitudinal research could be valuable. The current research focused on the role of CPC nurses working in the context of home-based EOL care. The experiences of other multi-disciplinary team members providing home-based EOL care should also be considered, including doctors, physiotherapists, occupational therapists, child-life therapists, and social workers.
The results of the current study flag the potential value of interventions which enhance pediatric EOL training, CPC nurse support and inter-agency collaboration. Evidence-based development and subsequent evaluation of such interventions would be warranted. For example, evaluating the impact of tailored educational programs on nurses’ confidence in administering pediatric medications would allow for actionable insights to improve practice.
This study highlighted limitations of available supports for siblings in the context of home-based EOL care. Although there is a growing body of research investigating the needs of siblings,49–54 with various sibling interventions reported in the context of chronic pediatric health conditions,55–57 future research could specifically address the nature of sibling needs and supports in the home-based EOL care context.
Clinical Recommendations
The results of this study provide actionable clinical directions for improving home-based pediatric EOL care, enhancing the quality of care provided to children and their families while addressing the well-being of CPC nurses. CPC nurses caring for children at the EOL can benefit from increased exposure to pediatrics, such as through supported work experience and supervised clinical placements in local pediatric services. There is a need for increased professional development opportunities with a pediatric EOL focus, both as part of routine professional development and at the time of referral of a pediatric EOL patient. Enhanced training should encompass a range of skills related to psychosocial factors, clinical knowledge, and promoting nurses’ psychological well-being. Increased specialist pediatric outreach services, especially those offering in-person support, may be beneficial in assisting CPC nurses in overcoming the challenges they face, and a number of approaches have been suggested for how this may occur.58–60
To promote knowledge sharing within and between facilities, it would be valuable to encourage initiatives such as earlier involvement of CPC nurses, joint home visits (between CPC and specialist pediatric palliative care nurses), mentorship programs, and formal debrief sessions. Such debrief sessions within facilities would allow CPC nurses to address psychological concerns, access support, and share knowledge across the team.61, 62 On a broader, systemic level, statewide integration of medical record systems may also facilitate inter-agency coordination and collaboration.
Finally, each CPC services which offers care to children at the EOL should consider what challenges are related to providing pediatric care from within the context of an adult-based healthcare framework and to consider how these may be addressed and mitigated.
Conclusion
This study explored the experiences and perspectives of CPC nurses working in NSW, Australia, focussing on the challenges and perceived benefits of caring for pediatric patients in the home-setting at the EOL. Key challenges related to accessing resources and education, unique aspects of pediatric EOL care, family psychosocial factors, and organizational models and systems of care. The multitude of perceived benefits for patients and their families are also highlighted. Future clinical directions identified by CPC nurses highlighted a desire for improvements in education/training, intra- and inter-organizational collaboration with better integration of systems, and better support structures in place, these being central to building capacity and confidence to provide high quality pediatric EOL care.
Supplemental Material
sj-docx-1-pal-10.1177_08258597251341039 - Supplemental material for Challenges, Benefits, and Future Directions of Pediatric Home-Based End-of-Life Care: A Qualitative Study
Supplemental material, sj-docx-1-pal-10.1177_08258597251341039 for Challenges, Benefits, and Future Directions of Pediatric Home-Based End-of-Life Care: A Qualitative Study by Tiina Jaaniste, Mia Helyar, Marisa Eamens, Therese Smeal, Sandra Coombs and Martha Mherekumombe in Journal of Palliative Care
Footnotes
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The authors disclosed receipt of the following financial support for the research, authorship, and publication of this article: This work was supported by a SPHERE Palliative Care Clinical Academic Group Seed Funding Grant [notification of receipt date: 29 July 2022].
Supplemental Material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
