Abstract
The COVID-19 pandemic has negatively impacted the well-being of healthcare workers (HCWs). HCWs are highly exposed to shift work and their work schedules have been subject to increasing unpredictability since the start of the pandemic. This review aims to: (1) map the studies providing information about factors associated with sleep characteristics in HCWs working in the context of the COVID-19 pandemic during the first and second waves and (2) examine the state of the evidence base in terms of the availability of information on the influence of atypical work schedules. A literature search was performed in PubMed. Studies containing information about factors (demographic; psychological; occupational; COVID-19-specific; work schedule; lifestyle; medical; or other) associated with various sleep characteristics among HCWs working in the context of the COVID-19 pandemic were included. Particular attention was paid to the availability of information on the role of atypical work schedules on HCW sleep. Fifty-seven articles met the inclusion criteria. Most studies were reports of quantitative cross-sectional surveys using self-report measures. Associations between female sex, frontline HCW status, psychological factors, and poorer sleep were observed. Six studies included a measure of shift work in their analyses, 5 of which reported an association between shift work status and sleep. A wide range of factors were investigated, with female sex, frontline HCW status, and psychological factors repeatedly demonstrating associations with poorer sleep. Sleep was predominantly measured in terms of self-reported sleep quality or insomnia symptoms. Few studies investigated the influence of atypical work schedules on HCW sleep in the context of the COVID-19 pandemic. Research on this topic is lacking in terms of reliable and consistent measurements of sleep outcomes, longitudinal data, and knowledge about the influence of covariates such atypical work schedules, comorbidity, and medical history on HCW sleep.
One of the occupational groups whose members experience very high levels of sleep problems are healthcare workers (HCWs). Prior to the COVID-19 pandemic, an estimated 42.7% of healthcare support workers and 38.1% of healthcare practitioners and technical workers reported short sleep duration, compared with 36.5% in the general population (Shockey and Wheaton, 2017). The incidence of sleep disorders was also elevated, with reported estimates of 3.3% prevalence among HCWs compared with 1.6% for the general population (Kim et al., 2018). Since the onset of the COVID-19 pandemic, this situation seems to have further deteriorated (Pappa et al., 2021). In a meta-analysis, Cénat et al. (2020) reported a significantly higher prevalence of insomnia symptoms in HCWs (k = 6, 36.52, 95% confidence interval [CI] = 32.99-40.20) relative to the general population (k = 8, 16.45, 95% CI = 8.39-29.74) (z = 2.69, p < 0.05). The estimated pooled prevalence rates for sleep problems among HCWs have ranged from 36% to 45% (Muller et al., 2020; Pappa et al., 2020; Jahrami et al., 2021b; Xia et al., 2021). This is of concern, as sleep-related impairment may affect the ability of HCWs to perform critical tasks related to patient care (Trockel et al., 2020).
Atypical work schedules refer to a range of irregular work schedule configurations including overtime and shift work (Barthe et al., 2011). Working shifts that impose non-standard sleep/wake times may cause shorter duration of sleep, sleep fragmentation, and sleepiness due to a conflict between the required sleep-wake cycle and the individual’s endogenous circadian system (Boivin et al., 2012; Wright et al., 2013; Boivin and Boudreau, 2014). HCWs are one of the groups with the highest exposure to shift work, with estimates as high as 40% in the European Union and 35% in Canada (Rydz et al., 2020; Vanttola et al., 2020). HCWs have experienced considerable changes to their work schedules since the start of the COVID-19 pandemic, including longer hours, more shift work, and general alterations in staff scheduling to minimize interactions between different staff members (Walton et al., 2020; Hoedl et al., 2021; Mehta et al., 2021). Studies have demonstrated that sleep loss results in more occupational injuries (e.g., injuries sustained while moving patients) and errors (e.g., medication administration) among HCWs working atypical shifts than those working regular shifts (Rogers et al., 2004; Caruso and Hitchcock, 2010; Weaver et al., 2015; Booker et al., 2018). Shift work status is thus a key factor to consider when examining sleep characteristics for HCWs in the context of the COVID-19 pandemic.
In the wake of the COVID-19 pandemic, much research on sleep problems in HCWs has rapidly emerged. Previous studies have quantified the prevalence of sleep problems and provided important summaries of risk factors for poorer sleep among HCWs such as frontline HCW status and lack of social support (Bhat and Chokroverty, 2021; Pappa et al., 2021). Yet no previous review has systematically synthesized the risk factors associated with sleep problems in HCWs. More specifically, the extent to which existing research studies account for the role of atypical work schedules in determining the associations between potential risk factors and sleep characteristics remains to be seen. Thus, the first aim of this scoping review was to assess the extent and nature of the research investigating factors associated with sleep characteristics in HCWs working in the context of the COVID-19 pandemic. The second aim of the review was to closely examine these studies based on the state of existing knowledge about the potential impact of atypical work schedules on sleep among HCWs.
Materials and Methods
This scoping review followed the methodological framework for scoping reviews (Arksey and O’Malley, 2005), and the organization of the manuscript was guided by the Preferred Reporting Items for Systematic Reviews and Meta-Analyses (PRISMA) Extension for Scoping Reviews (PRISMA-ScR) checklist (Tricco et al., 2018) (see Appendix A). Scoping review methodology was used as the most suitable method for reviewing a large body of heterogeneous literature not amenable to a more precise systematic review. The project was approved by the research ethics boards of the Douglas Mental Health University Institute and that of the funding agency.
Search Strategy
A keyword search was conducted on 12 February 2021 using PubMed, and updated soon after on 26 February 2021. The search strategy was developed and categorized around 3 concepts, “COVID-19,” “health care worker,” and “sleep.” Variations for each key word were combined with the “OR” operation to maximize results, for example, “SARS-CoV-2,” “frontline health worker,” and “insomnia.” Search terms are presented in greater detail in Appendix B.
Eligibility Criteria
Eligibility criteria for the selection of articles in the present review included original research studies published in English or French that reported on factors associated with sleep among HCWs who were working in the context of the COVID-19 pandemic. Only studies in which data collection took place during either the first or the second wave of infection were included. In the present review, the first wave referred to the period from 1 February 2020 to 31 July 2020, and the second wave referred to the period from 1 August 2020 to 26 February 2021 (Looi, 2020; Vahidy et al., 2020; Fan et al., 2021; Iftimie et al., 2021; Saito et al., 2021). No geographic restrictions were imposed. Both quantitative and qualitative studies were considered. The studies of interest included samples of HCWs over 18 years of age where the majority of participants were in direct contact with persons seeking healthcare. Only studies that reported on factors potentially influencing sleep among HCWs, defined in terms of a series of characteristics including poor sleep quality, symptoms of insomnia, increased sleep latency (difficulty initiating sleep), and sleep problems or sleep dysfunction/disturbances/disruptions, were included in the present review. Studies that were measuring factors associated with burnout or fatigue only (not sleep) were excluded from the review.
Studies reporting quantitative data were required to demonstrate a statistical relationship between the factor being tested and a measure of sleep. Where qualitative data were reported, the influence of the factor on sleep had to be clearly identifiable. Study protocols or feasibility studies were not included. Articles were excluded if they were theses or dissertations, did not provide an abstract, conference presentations, or books or book chapters. Review articles were not included in the current synthesis, although the reference lists of review articles whose topic was closely related to that of the present review were screened for titles that may not have been captured by the keyword search.
Screening Procedure
After removal of duplicates, the PubMed search generated a total of 417 results. The reference lists of all relevant review articles were then screened and a further 12 records retrieved, producing a total of 429 records for review. A calibration exercise was conducted before title and abstract screening to refine the eligibility criteria. Two raters (N.P. and M.F.) separately evaluated the titles and abstracts of 10 studies for inclusion or exclusion. Inter-rater agreement was then compared. This process was repeated until sufficient inter-rater agreement was achieved (80%). At this point, the article titles and abstracts were screened for eligibility according to the established inclusion criteria. Disagreements were resolved by discussion and, where necessary, a third party (D.B.B.) was consulted. For articles meeting the inclusion criteria, the full texts were retrieved, resulting in a total of 125 articles for full-text review. The same calibration exercise that was conducted before title and abstract screening was conducted prior to beginning full-text screening. The full-text screening resulted in a total of 57 articles for the final synthesis. A flow chart detailing the study selection process is provided in Figure 1.
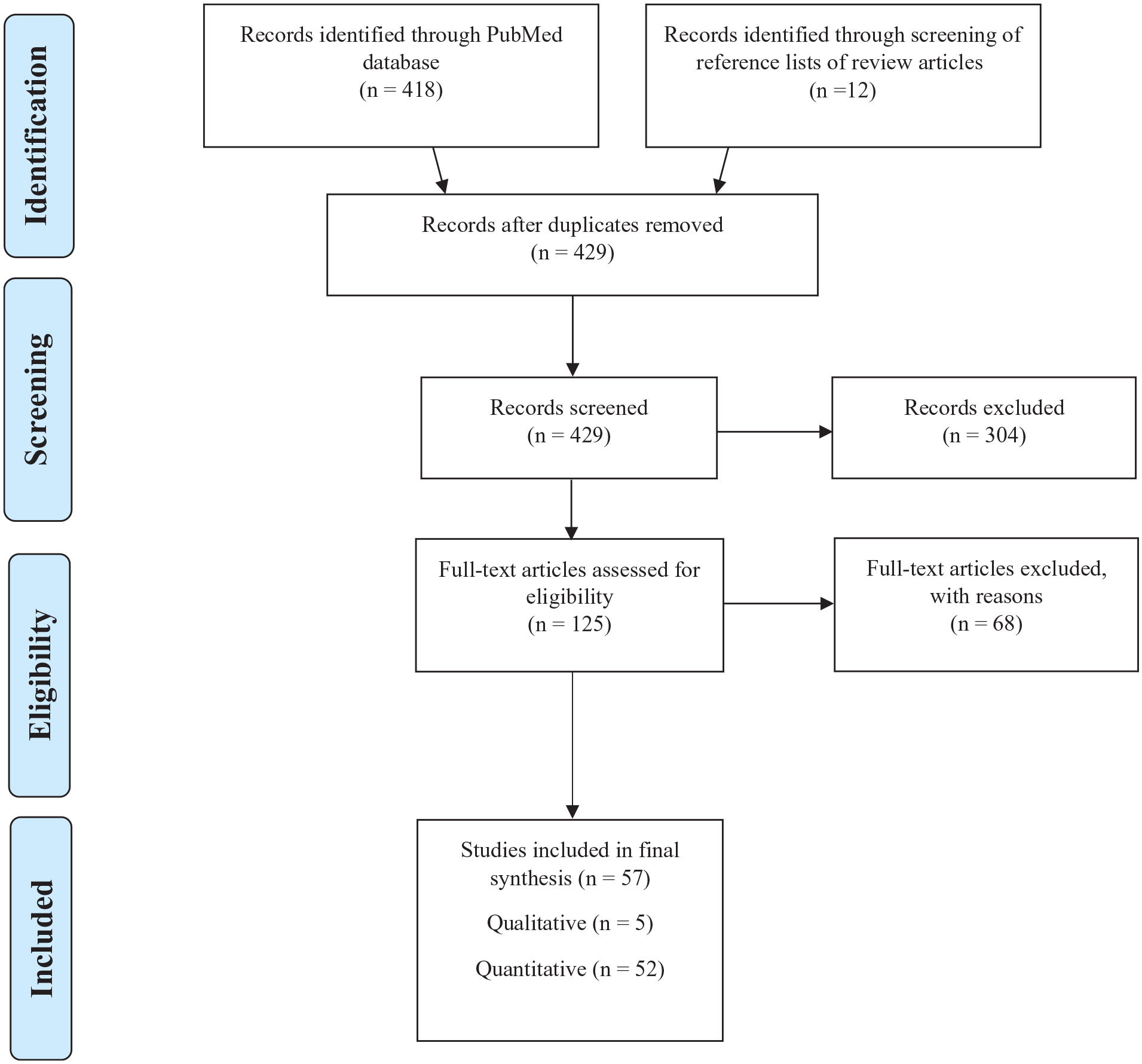
Flow diagram of database searches and study selection illustrating factors associated with sleep.
Data Extraction
A data extraction sheet was developed that included the following: author(s), year, journal, article title, study objectives, country, participants/setting, data collection period, method, data analysis, factors measured, and main findings. All factors whose association with sleep was investigated across studies were categorized as: demographic; psychological; occupational; COVID-19-specific; work schedule; lifestyle; medical; or other. These categories were developed in consultation with the research team. For studies, particularly qualitative studies that did not explicitly describe data according to one of these categories, influencing factors were abstracted by the first author and assigned to a category. A calibration exercise was conducted to ensure sufficient inter-rater agreement (80%) on the designation of certain concepts to each category.
Results
Description of Study Samples and Contexts
Fifty-seven studies (51 quantitative, 5 qualitative and 1 mixed-methods) met the inclusion criteria. All quantitative studies were descriptive in nature and consisted of cross-sectional surveys except for a single study where sleep was measured at baseline and at 1-month follow-up using the Pittsburgh Sleep Quality Index (PSQI; Zhao et al., 2020). In 4 of the 5 qualitative studies, data were collected using semi-structured interviews carried out either in-person or virtually (e.g., using Skype) (Cui et al., 2020; Sun et al., 2020; Whelehan et al., 2021; Yıldırım et al., 2021), whereas one study did not describe how the data were collected (Fan et al., 2020). Some proportion of the sample in all studies included workers in direct contact with COVID-19 patients, although the exact percentage of individuals who were working under these conditions was not always specified. Some study samples consisted of nurses/physicians only. Other studies conducted investigations of sleep in specific samples such as anesthesiologists (Jain et al., 2020) or non-consultant hospital doctors working in a surgery department (Whelehan et al., 2021). Some studies comprised a mixture of several different types of HCWs (e.g., doctors, pharmacists, paramedics, emergency department attendants, medical technicians) (Al Ammari et al., 2020; Giardino et al., 2020; Gupta et al., 2020; He et al., 2020; Huffman et al., 2020; Khanal et al., 2020; Que et al., 2020; Robles et al., 2020; Sagaon-Teyssier et al., 2020; Sharma et al., 2020; van Roekel et al., 2020; Wang et al., 2020a; Zhang et al., 2020a). Twenty-three of the 57 studies took place in China, 12 of which occurred in the context of emergency department settings at the outbreak of the virus. Data collection for all studies took place in 2020. The most recent data collection period was between July and October 2020 (Abdellah et al., 2021).
Measurement of Sleep Characteristics
Most studies used self-report instruments to measure sleep in terms of insomnia symptoms and/or sleep quality. As expected, there was heterogeneity in the measures of sleep utilized across studies. The Insomnia Severity Index (ISI) was the sleep measure most frequently adopted (Morin et al., 2011), followed by the PSQI (Buysse et al., 1989). Other measures of sleep included the Visual Analogue Sleep Scale (Snyder-Halpern and Verran, 1987; Verran and Snyder-Halpern, 1988) and the Athens Insomnia Scale (AIS) (Soldatos et al., 2003). A full list of instruments and sleep measures with corresponding cutoff scores (where specified) is presented in Table 1.
Measures of sleep characteristics adopted in included studies.

Abbreviation: GI = gastrointestinal.
In studies that used the ISI, scores were presented in a variety of ways. Most frequently, a global score ranging from 0 to 28 was interpreted using the following criteria: ISI scores of 0-7 indicating absence of insomnia, 8-14 indicating sub-threshold insomnia symptoms, 15-21 indicating moderate insomnia, and 22-28 indicating severe insomnia. In studies that used the PSQI, the cutoff score for poor sleep varied from >5 to >7, with one study using >10 as the cutoff (Zheng et al., 2021).
Factors Associated With Sleep
A wide range of variables were measured in terms of their association with the sleep of HCWs. An overview of the included articles as well as a summary of the factors in each study for which a relationship with a sleep characteristic was measured using a test of association (correlation or regression analysis) is presented in Table 2. Female sex, psychological factors, and job position were the factors that demonstrated the most prominent associations with sleep characteristics across studies. These specific results are reported in greater detail in this section.
Overview of included studies (n = 57).
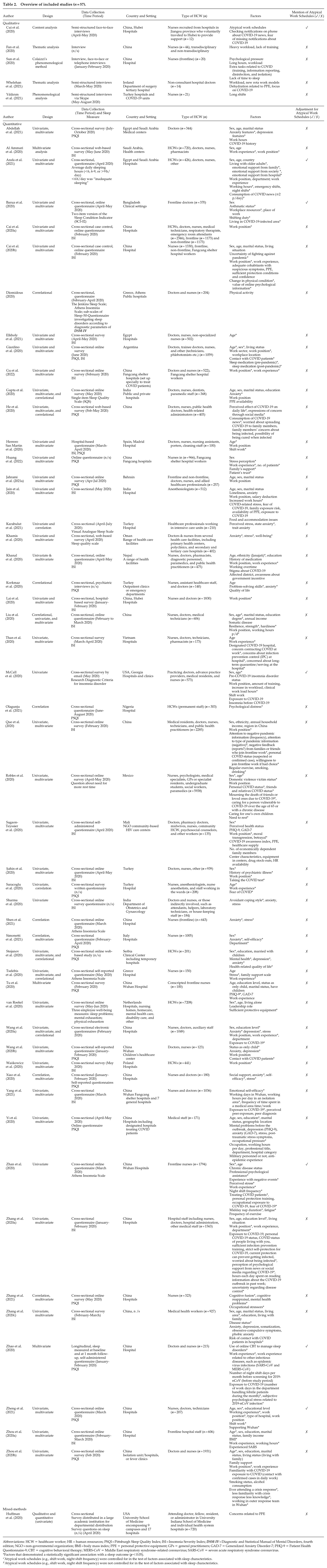
Abbreviations: HCW = healthcare worker; HR = human ressources; PSQI = Pittsburgh Sleep Quality Index; ISI = Insomnia Severity Index; DSM-IV = Diagnostic and Statistical Manual of Mental Disorders, fourth edition; NGO = non-governmental organization; BMI = body mass index; PPE = personal protective equipment; GPs = general practitioners; GAD-7 = Generalized Anxiety Disorder-7; PHQ-9 = Patient Health Questionnaire-9; CBT = cognitive behavioral therapy; MERS-CoV = Middle East respiratory syndrome–related coronavirus; SARS-CoV = severe acute respiratory syndrome coronavirus.
Factors that demonstrated a statistically significant association with a sleep outcome (p < 0.05).
Atypical work schedules (e.g., shift work, night shift frequency) were controlled for in the test of factors associated with sleep characteristics.
Atypical work schedules (e.g., shift work, night shift frequency) were not controlled for in the test of factors associated with sleep characteristics.
Female Sex
Nine studies identified a significant association between female sex and poorer sleep (Giardino et al., 2020; McCall et al., 2020; Robles et al., 2020; Sagaon-Teyssier et al., 2020; Şahin et al., 2020; Stojanov et al., 2020; van Roekel et al., 2020; Zhan et al., 2020; Simonetti et al., 2021). Some studies reported stronger associations, for instance, in a sample of HCWs in Argentina (n = 1059), the odds of reporting a PSQI score greater than 5 were 6.4 times higher for females than for males, 95% CI = 4.46-9.20, and the odds of reporting an ISI score greater than 7 were 4.31 times higher for females than males (Giardino et al., 2020). Yet, in other studies, the strength of the associations was much weaker (Zhan et al., 2020; Simonetti et al., 2021).
Psychological Factors
The influence of psychological factors such as stress, as well as symptoms of anxiety and depression, on sleep was investigated in many of the studies reviewed. These variables were most often assessed using correlation analysis. Four studies reported a significant association between depressive symptoms and sleep (Stojanov et al., 2020; Tu et al., 2020; Wang et al., 2020a, 2020b). Relationships between anxiety symptoms and sleep were identified in both small (Gupta et al., 2020; Khamis et al., 2020; Korkmaz et al., 2020; Stojanov et al., 2020; Xiao et al., 2020; Abdellah et al., 2021; Karabulut et al., 2021; Shen et al., 2021) and larger study samples (Wang et al., 2020a; Simonetti et al., 2021). Associations between stress and sleep were reported in 4 studies (Huang et al., 2022; Khamis et al., 2020; Tselebis et al., 2020; Xiao et al., 2020). The influence of social support on sleep was also assessed. Results of a path analysis conducted by Xiao et al. (2020) indicated that social support provided to medical staff reduced their anxiety and stress levels, and positively affected self-efficacy but did not directly affect sleep (n = 180). A similar pattern was observed in Tselebis et al. (2020) where family support among nursing staff did not directly influence rates of sleep disturbance but followed an indirect pathway via stress (n = 150). In a sample of 285 HCWs, Que et al. (2020) found that those who reported an unwillingness to join frontline work, if given the choice, were at a greater risk of reporting symptoms of insomnia (odds ratio [OR] = 3.39, 95% CI = 1.86-6.17). In a sample of 323 nurses, cognitive fusion, defined as a process of constructing thoughts toward stressors and not being able to distinguish between thoughts and facts (Gross and John, 2003; Hayes et al., 2009), was positively associated with sleep difficulty (β = 0.148, p = 0.022) (Zhang et al., 2021). A range of other psychological factors affecting HCWs such as status of receiving professional psychological assistance, experience with negative events (Zhan et al., 2020), and history of psychiatric illness (Şahin et al., 2020) also demonstrated associations with sleep characteristics.
Job Position
Six of the 8 studies that tested frontline HCW status as a risk factor found statistically significant associations between frontline HCW status and sleep characteristics in both medium (Jahrami et al., 2021a; Wańkowicz et al., 2020) and larger sample sizes (Al Ammari et al., 2020; Cai et al., 2020a, 2020b; Que et al., 2020), with some studies reporting strong associations (Cai et al., 2020a; Que et al., 2020). Sixteen studies in the review investigated associations between some measure of work experience or seniority, and sleep. A pattern indicating a relationship between greater work experience and poorer sleep was observed—7 studies with widely ranging sample sizes reporting significant associations (Gu et al., 2022; Huang et al., 2022; Khanal et al., 2020; Than et al., 2020; Tselebis et al., 2020; Zhan et al., 2020; Zheng et al., 2021). Various types of jobs were investigated as predictors of sleep (e.g., doctor vs other; resident vs consultant). While heterogeneity among these associations was reported, 3 studies found that being a nurse was associated with poorer sleep. In multivariate regression models adjusted for age and sex, Zhou et al. (2020b) found that being a nurse was associated with poorer sleep (n = 1931), and Gu et al. (2022) observed that the OR for higher scores on the ISI was 3.03 (95% CI = 1.97-5.32) in nurses, compared with doctors (n = 522). Based on a logistic regression model conducted by Giardino et al. (2020), being a non-doctor predicted a higher score on the PSQI (n = 1095), although the analysis did not control for sex. In models adjusted for age and sex, Zhang et al. (2020a) reported that, compared with other medical staff, being a doctor was associated with less risk of insomnia symptoms (n = 1563).
Assessment of the Role of Atypical Work Schedules
Shift Work
Among the 52 quantitative studies, only 6 included some measurement of shift work status. Four of these studies used binary (yes/no) measures of shift work status (Barua et al., 2020; McCall et al., 2020; Herrero San Martin et al., 2020; Arafa et al., 2021). Zhan et al. (2020) assessed shift work in terms of frequency of night shifts per week. Zhao et al. (2020) assessed the number of night shift days per month before HCWs started screening for COVID-19 in patients. In a cross-sectional survey conducted by Zheng et al. (2021), participants were asked whether they were working shifts as usual, working more night shifts, or more day shifts. Only 5 studies that investigated other factors as predictors of sleep characteristics adjusted for shift work status in their multivariate analyses. No study sample consisted exclusively of HCWs working atypical work schedules.
Associations between shift work and poorer sleep were reported in both univariate (Arafa et al., 2021; Zheng et al., 2021) and multivariate analyses (Barua et al., 2020; Herrero San Martin et al., 2020; Zhan et al., 2020; Zheng et al., 2021). Arafa et al. (2021) found that in models adjusted for age, sex, profession, and country, individuals working nights shifts were 1.81 times more likely to sleep less than 6 h per day than those who were not working night shifts (95% CI = 1.17-2.80, n = 426). In their investigation of the factors associated with sleep among frontline HCWs (n = 100), Herrero San Martin et al. (2020) found that, after conducting univariate analyses on a range of variables, only shift work retained a significant association of the risk of obtaining worse scores on the ISI in the multivariate analysis. The same study also assessed parasomnias such as sleep terrors and confusional arousals and found that being a shift worker was associated with higher frequency of reporting such sleep-related symptoms (OR = 2.40, 95% CI = 1.06-5.42; p = 0.034), although other sleep disorders were not assessed. In a univariate analysis conducted among 207 HCWs, Zheng et al. (2021) found that working more night shifts was associated with poorer sleep quality (OR = 2.94, 95% CI = 1.37-6.31, p = 0.01). This association was retained after controlling for confounding factors, while results of the multivariate logistic regression analysis indicated that HCWs working more night shifts were 3.10 times more likely to report poorer sleep quality than those not working night shifts (95% CI = 1.31-7.34). In a multinomial logistic regression analysis, Barua et al. (2020) observed that shift work was associated with the odds of moderate sleep disturbances (2.21, 95 % CI = 1.24-3.94), but was not significantly associated with the odds of reporting insomnia (n = 370). McCall et al. (2020) conducted a study on rates and predictive factors for short-term insomnia disorder in a sample of 573 HCWs before and during the COVID-19 pandemic. Results for the overall sample suggested that the presence of shift work was not a significant risk factor for new cases of insomnia disorder during the pandemic. However, this analysis did not measure whether a change in the intensity of shift work over the course of the pandemic had an impact on sleep. One study did measure shift work status before the pandemic (Zhao et al., 2020), reporting that the number of night shifts worked per month (before starting screening for COVID-19) was not associated with sleep quality at baseline or at 1 month follow-up (n = 215). However once again, the change in intensity of shift work since the start of the pandemic and its association with sleep was not assessed. Among the qualitative findings, a sample of nurses who volunteered to work in Hubei Province during the COVID-19 pandemic described how the new shift schedules requiring night shifts disturbed their sleep (Cui et al., 2020).
Longer Working Hours
Working hours were measured in 8 quantitative studies (Jain et al., 2020; Khanal et al., 2020; Liu et al., 2020; McCall et al., 2020; Yi et al., 2020; Zhou et al., 2020a; Abdellah et al., 2021; Arafa et al., 2021). Four of these studies found that extended working hours were associated with poorer sleep. Arafa et al. (2021) found that working more than 6 h per day was associated with inadequate sleep (n = 426). Jain et al. (2020) reported that HCWs with an increase in working hours were 3.16 (95% CI = 1.48-6.74) times more likely to report an ISI score greater than or equal to 8 compared with HCWs not subject to increased working hours (n = 512). Analyses conducted by Liu et al. (2020) and Zhou et al. (2020a) reported that greater working hours were associated with a higher score on the ISI (n = 606 in both studies).
Discussion
In this scoping review, the state of research activity investigating factors associated with sleep in HCWs during the first and start of the second waves of the COVID-19 pandemic was assessed. Fifty-seven studies were included in the final synthesis. A comprehensive overview of risk factors for poor sleep, as investigated in relevant studies, was provided. This may be useful in providing clinicians with a visualization of available information on this subject and its development. The article also evaluated the extent to which the impact of atypical work schedules was considered in research investigating sleep among HCWs during the pandemic, and in so doing, identified a number of knowledge gaps in this area. The review of the literature revealed certain methodological issues regarding the measurement of sleep characteristics across the studies reviewed. A summary of the findings of this scoping review are summarized in Appendix C.
Methodological Issues
Most studies assessed sleep in terms of sleep quality or insomnia symptoms, with PSQI and ISI being the instruments most frequently adopted. Fifteen different instruments were used to measure sleep in the various studies. The choice of sleep measure may have an important impact on the generalizability and application of findings (Moul et al., 2004). There was a lack of consistency regarding the reporting of results. Some studies adopted the same measure of sleep (e.g., ISI), but their scores differed in terms of interpretation (different cutoff points) or presentation (insomnia vs insomnia symptoms) (Al Ammari et al., 2020; Cai et al., 2020b). This variation in the measurement of sleep and interpretation of sleep scores makes it difficult for clinicians to precisely distinguish risk factors for moderate sleep disruption from factors suggesting more severe cases of insomnia, which has implications for assessment and intervention. Nearly all studies assessed sleep using self-report measures. Although self-report measures are useful in assessing patient perceptions of sleep, other physiological and neurophysiological measures of sleep, such as actigraphy and polysomnography, have also demonstrated effectiveness (Girschik et al., 2012; Sadeh, 2015). Future studies on the sleep of HCWs may consider using measures such as these in addition to self-report measures. All but one quantitative study consisted of cross-sectional data, and as such, any conclusions drawn from these cross-sectional studies regarding risk factors for sleep among HCWs would be somewhat limited. Longitudinal data are needed to assert causal factors for sleep disturbances in this population. A small amount of longitudinal studies have been conducted since the present literature search was conducted (Abdalla et al., 2021; Jordan et al., 2021; Rossi et al., 2021; Topriceanu et al., 2021). Just two of these studies (Abdalla et al., 2021; Rossi et al., 2021) assessed predictors of poorer sleep over time, with similar risk factors to those identified in cross-sectional studies (e.g., frontline HCW status, more working hours) being reported. However, in contrast to the findings of cross-sectional studies, Rossi et al. (2021) reported that male sex was associated with an increase in insomnia symptoms. More longitudinal studies are needed to ascertain possible sex differences in the sleep of HCWs over time. Several studies failed to control for variables such as sleep medication status, sleep history, and comorbidity in assessing associations between the factors investigated and sleep. For instance, only one study adjusted for pre-existing insomnia status (before the pandemic) in their analyses (McCall et al., 2020). Sleep problems are also common in chronic conditions such as diabetes (Khalil et al., 2020). These and several other variables reported in many of the studies may have confounded associations between the factors investigated and sleep, such as the failure to control for hypertension or antidepressant medications. Moreover, many studies did not control for important lifestyle factors such as alcohol consumption, smoking, exercise, body mass index (BMI), and hypertension when assessing predictors of sleep (Rod et al., 2020; Romero Starke et al., 2020; Zhang et al., 2020b).
Emergent Risk Factors
As previously mentioned, most of the studies reviewed here were quantitative descriptive studies consisting of cross-sectional survey data, yet there was considerable heterogeneity across studies in terms of the methodologies, scales, and statistical analyses adopted. Thus, it was not possible to combine results, infer causality, or make conclusions about which factors have a greater influence on sleep than others. However, a number of overall patterns of association could be observed among the studies reviewed. It appears that female sex and frontline HCW status were the factors most consistently related to poorer sleep during the COVID-19 pandemic. These findings are consistent with existing studies which assert that women and frontline HCWs have been disproportionately vulnerable to mental health problems since the start of the COVID-19 pandemic (Cabarkapa et al., 2020; De Kock et al., 2021; Liu et al., 2021). Other sex differences such as COVID-19 mortality risk may also explain differences in sleep, although the increased mortality risk for males does not speak to our findings (Peckham et al., 2020). In addition to biological factors, gender issues are likely involved. Indeed, women remain more responsible for domestic tasks than men; increased child supervision due to stay-at-home orders and additional tasks related to COVID-19 such as increased household sanitization may have added to the domestic workload of women and subsequently impacted health outcomes such as sleep (Bigalke et al., 2020). Women represent almost 70% of the global healthcare workforce (Boniol et al., 2019) and may be a subgroup of HCWs in need of extra support during the pandemic. Numerous studies have also observed a relationship between psychological factors and sleep in HCWs. While the inferences that may be made based on these cross-sectional findings are limited, the results draw some attention to social support as a potentially important variable in disentangling the complex interrelationships between psychological factors and sleep among HCWs in the context of a pandemic. This is important information for sleep clinicians insofar that it highlights the importance of a biopsychosocial approach in assessing and treating health conditions that may be associated with sleep. The influence of other novel psychological phenomena, such as anxiety syndrome features associated with COVID-19, has yet to be fully understood. In the present review, there was some evidence to suggest that greater work experience or seniority was associated with poorer sleep among HCWs, although some studies also found inverse associations. Results of previous studies provide some support for an association between greater work experience and less stress (Lam et al., 1999; Casu and Giaquinto, 2018); however overall, this finding is largely consistent with the findings of more recent research, where similarly heterogeneous associations between seniority and sleep (Sigursteinsdóttir et al., 2020) and seniority and stress-related outcomes (e.g., psychological distress and burnout) (Vargas et al., 2014; Gómez-Urquiza et al., 2017) were observed in HCWs.
Age has been demonstrated as an important factor driving differences in COVID-19 mortality (O’Driscoll et al., 2021), which may have implications on sleep. However, a consistent pattern of association between age and sleep characteristics was not observed in the studies included in the present review. The relationship between these factors may also be partly obscured by the relationship between age and shift work, a relationship that requires further clarification (Ritonja et al., 2019). However, given that shift work status was not measured in the majority of studies, it is unclear how accounting for this factor would affect the relationship between work experience/seniority and shift work. Staff shortages induced by the COVID-19 pandemic have also led to increased responsibility and work scheduling changes among HCWs. More knowledge is needed to ascertain whether there is an association between work experience and sleep to identify subpopulations of HCWs who are potentially in need of extra support. As the pandemic progresses, further development of the findings presented here will be necessary to further clarify the factors influencing sleep and the general well-being of HCWs.
Atypical Work Schedules and Gaps in Knowledge
Five studies in the present review found that shift work status independently predicted poorer sleep in HCWs. Herrero San Martin et al. (2020) identified shift work as the only independent predictor of sleep in a multivariate analysis. These findings add to a considerable body of evidence asserting that shift work is a major risk factor for poorer sleep. While many studies discussed the increase in shift work during the COVID-19 pandemic, this review demonstrated that very few of the quantitative studies accounted for atypical work schedules in their statistical analyses, which may detract from the interpretive value of certain findings. For instance, despite the increased prevalence of shift work among nurses and frontline HCWs compared with other HCWs, some studies did not control for shift work status when assessing sleep characteristics for these groups (Al Ammari et al., 2020; Cai et al., 2020a, 2020b; Gu et al., 2022; Jahrami et al., 2021a; Que et al., 2020; Wang et al., 2020b; Zhou et al., 2020b). Overall, study samples did not distinguish between shift workers and non-shift workers. Even among studies in which the analyses did account for shift work status, the change in intensity or frequency of shift work, pre- versus post-pandemic, was not measured. In addition, measures of shift work status in studies included in the present review did not provide enough detail to decipher whether participants had been carrying out shift work before the pandemic, and if so, for how long. Moreover, individual variation in tolerance to shift work was not accounted for in the present analyses (Ritonja et al., 2019; Höller et al., 2021). In addition, studies in which shift work was measured did not provide information related to recovery time between shifts. Quality recovery time may have been exceptionally challenging for HCWs during the pandemic due to stressful work environments as well as extra domestic duties created by stay-at-home orders. More detailed information about shift work recovery and chronicity would help distinguish shift work disorder from normal sleep complaints due to episodic or occasional atypical shifts. Such information about the history and chronicity of shift work would be of use to clinicians in terms of diagnosis, risk assessment, and treatment for HCWs with sleep problems. A recently published study did identify a cross-sectional association between shift work and insomnia symptoms (Aslan and Dinç, 2021); however, just as with the studies included in the present review, shift work frequency or chronicity was not accounted for in measurement of the shift work variable.
The observed associations between extended working hours and poorer sleep in HCWs, as reported in the studies presented, provide some evidence of a relationship among these factors. Working hours were measured in only 8 studies, which was surprising given the considerable increase in working hours for HCWs since the start of the pandemic. Only one study examined how the work schedules of HCWs had changed over the course of the pandemic (Jain et al., 2020). The work schedules of HCWs have been subject to substantial change since the start of the pandemic (Mehta et al., 2021), yet the impact of these changes on the sleep of HCWs has yet to be thoroughly investigated. Changes in work schedule may result in greater unpredictability and a reduced sense of control for the HCW. There have been some media reports of increased mandatory overtime since the start of the pandemic, although precise statistics describing this phenomenon, and how it varies from country to country, are lacking. Perceived control is a key element in determining how an individual responds to stress at work (Johnson et al., 2006). HCWs’ perceived control over their work schedule may influence the relationship between stress and sleep. Future research on sleep among HCWs should take this into consideration.
Limitations
Certain limitations in the present scoping review must be acknowledged. The literature search was conducted in one database only (PubMed). Given the rapid advancement of COVID-19-related research, the authors chose to restrict the search to PubMed as one of the most extensive databases available to capture the greatest number of relevant titles in the shortest space of time. Despite a thorough search of this database, some relevant studies may have been overlooked (e.g., studies published in languages other than English or French). Despite efforts to calibrate the data-charting process, the categories used to organize the variables measured in the review were developed by the present authors and, as such, may be subject to disagreement from authors of articles in the review regarding the categorization or interpretation of their data. It should also be noted that the data reported on studies included in the current review were collected in the very early stages of the pandemic (first and start of the second waves of infection); therefore, the associated findings cannot be generalized to other waves of the pandemic. The fear and uncertainty attributed to the novelty of the virus at that time may have accounted for a greater impact of psychological symptoms and their sequelae (such as sleep) than would occur at the present time. Since the collection of the data in the studies included in this review, there is more information about the COVID-19 virus and vaccinations have become available in some contexts. Future syntheses of research on this topic should make efforts to understand the distinct challenges for HCWs at each wave of infection and to distinguish the associated impact on HCW well-being at each stage.
Conclusion
This article provides a systematic overview of the literature describing the factors associated with sleep among HCWs in the context of the COVID-19 pandemic during the first and start of the second waves. There is a clear need for longitudinal data to ascertain how certain risk factors impact the sleep of HCWs over time, especially those factors unique to the context of the current pandemic. In addition, efforts toward greater consistency regarding the measurement of sleep as an outcome (e.g., list of accepted measures, consensus on cutoff scores) would facilitate better appraisal and interpretation of knowledge on this topic. Existing research on factors associated with sleep in HCWs mainly consists of cross-sectional studies using self-reported measures of sleep quality or insomnia symptoms. Some evidence has indicated that female sex and frontline HCW status may be associated with poorer self-reported sleep, while other findings suggest that being a nurse or having more work experience may be associated with more sleep problems. Not surprisingly, psychological factors such as stress or symptoms of anxiety and depression appear to be related to quality of sleep among HCWs. Social support may also indirectly influence sleep through its effect on other psychological variables. Few studies have assessed the influence of atypical work schedules on sleep. The six studies in this review that measured atypical work schedules did so by asking participants about their status or frequency of shift work. There was a lack of information about changing shift schedules, history of shift work, and recovery between shifts. Given the notable changes in work schedules induced by the COVID-19 pandemic, more research is needed to obtain additional information about the influence of atypical work schedules on the sleep of HCWs.
Footnotes
Appendices
Review of the research on the factors associated with COVID-19 HCW sleep: Main findings.

Abbreviation: HCW = healthcare worker.
Acknowledgements
We thank Rafael Pérez Medina Carballo for his help with the calibration of the data extraction sheet. We thank Dr. Judith Sabetti for writing assistance. A special thanks to NRC personnel Patricia Debergue and Stéphanie Grenier for their support with this project. The authors disclosed receipt of the following financial support for the research of this article: this work was supported by the National Research Council of Canada (NRC) through the Pandemic Response Challenge program (grant number PR010.1). NRC personnel took part in some meetings during which progress on the scoping review was discussed. However, they had no role in the design of this scoping review, interpretation of data, writing of the report, or decision to submit the article for publication.
Conflict Of Interest Statement
The author(s) declared the following potential conflicts of interest with respect to the research, authorship, and/or publication of this article: D.B.B. provides consultation and medico-legal advice on shift work–related cases.
