Abstract
Objective
To evaluate the specific contribution of the real-time postural feedback component during training on balance and mobility in individuals with Parkinson’s disease (PD).
Method
Five databases were searched in June 2025. Studies comparing the same basic balance and gait training with versus without feedback were included. Meta-analysis was conducted and the quality of evidence was assessed.
Result
Eleven studies were included. Narrative analysis indicated that additional feedback may immediately improve dynamic balance and modulate gait speed but not static balance. Meta-Analysis Showed providing feedback significantly augmented post-training improvement in standing balance (SMD = 0.880, 95% CI = 0.345∼1.416, moderate-quality), but not on walking stability (SMD = 0.516, 95% CI = −0.025∼1.058, moderate-quality), Berg Balance Scale (MD = −0.079, 95% CI = −2.159∼2.000, very-low-quality), Timed-Up-and-Go (MD = 0.939, 95% CI = −1.414∼3.293, low-quality), and walking speed (MD = 0.002, 95% CI = −0.057∼0.062, low-quality).
Conclusion
Providing real-time postural feedback may have immediate effects on dynamic balance and walking speed and a post-training effect on standing balance in PD.
Registration
CRD42024522330.
This is the first systematic review and meta-analysis to specifically summarize the unique contribution of real-time postural feedback during training on balance, mobility, and falls in individuals with Parkinson’s disease. Adding real-time postural feedback during training may improve the immediate effect (performance during the provision of feedback) of dynamic balance, while all post-training outcomes, except standing balance, did not reach significant changes, potentially due to the reliance on feedback and the mismatch between targeted outcomes and feedback provided. This study highlights the need for further research with larger sample sizes to strengthen the certainty of the evidence.
The findings suggest that gradually reducing the real-time postural feedback during the training may help to improve the post-training effect of balance for individuals with Parkinson’s disease. Future devices designed to provide feedback during training may need to ensure that the feedback is closely aligned with the targeted outcomes. This study provided a preliminary reference for therapy providers to manage the postural feedback during training to achieve more sustained improvements.What This Paper Adds
Applications of Study Findings
Introduction
Parkinson’s disease (PD) is a rapidly increasing global health issue, currently impacting 6.1 million individuals around the world (Ou et al., 2021). It is a progressive neurodegenerative disorder with the symptoms of resting tremor, muscle rigidity, and postural instability during stance and gait (Allen et al., 2013; Hou et al., 2017).
Due to the difficulties in controlling movements and responding to environmental changes, falls are common in the daily life of the population with PD. A systematic review indicated that 18 to 65% of individuals with PD reported recurrent falls annually, whereas only around 10% of recurrent falls were reported in the general older population each year (Allen et al., 2013; Carpenter et al., 2014). In addition, individuals with PD who had a history of recurrent falls exhibit a notably high annual fall frequency, with reports indicating an average of at least 4.7 falls per year (Allen et al., 2013). This elevated fall frequency undeniably heightens the risk of fall-related injuries among individuals with PD, consequently impacting their quality of life. Furthermore, the direct medical expenses in the United States resulting from falls and related injuries in people with Parkinson’s disease have been estimated at $25.4 billion, with an additional $14.2 million attributed to indirect costs (Appeadu & Gupta, 2023). Therefore, preventing falls in people with Parkinson’s disease is essential for preserving their quality of life and minimizing economic costs.
Falls are commonly associated with postural instability and gait disturbance in individuals with PD (Palmisano et al., 2022). These two disabling motor symptoms have been reported with a low response to medication (Feng et al., 2019; Giardini et al., 2018; Wilson et al., 2020). Recently, physical exercise was shown to improve balance and gait in individuals with PD (Ernst et al., 2023; Feng et al., 2020; Santos et al., 2017). For instance, activities such as Taichi and tango dancing have demonstrated beneficial effects in managing symptoms of Parkinson’s disease. Among various interventions, balance training stands out for its lasting impact, with improvements persisting for as long as 12 months. Additionally, engaging in these exercises has the potential to lower the incidence of falls by as much as 60% (Mak et al., 2017). In addition, treadmill training was also shown to improve the ability of dual-task walking for individuals with PD (Gaßner et al., 2022). These make physical exercise potentially the most effective non-pharmacological approach to improve balance and gait deficits, and prevent falls in individuals with PD (Appeadu & Gupta, 2023; Kim et al., 2013; Smania et al., 2010).
The ability to maintain postural stability and walk effectively depends on the integration of information from multiple sensory systems, including visual cues, somatosensory feedback from muscles and joints, and input from the vestibular system responsible for balance (Giardini et al., 2018). Hence, there is a trend to use sensory augmentation as an assistance for enhancing balance and gait during traditional training. The concept of real-time postural feedback has emerged as a novel approach to augment or replace sensory input in individuals with sensory impairments (Dockx et al., 2016). By delivering instant information on postural movements, this method supports the improvement and coordination of motor skills (Dockx et al., 2016). Advancements in sensor technology and posture detection capabilities have enhanced the ability to monitor body movements, enabling the provision of real-time postural feedback to individuals engaged in balance or mobility exercises (Liang et al., 2024).
Theoretically, with additional real-time postural feedback, individuals with PD may correct posture and attend to their body motions during training and gain further improvement on balance and mobility. Virtual reality training is one of the popular technologies to enhance sensory integration with augmented visual feedback. Lei et al. (2019) published a systematic review that compared the effects between postural feedback-based virtual reality training and traditional training, indicating that virtual reality training had better performance on balance and gait than traditional training in individuals with PD. In addition, a systematic review showed that external sensory-cued therapy could elevate daily living performance after training and a follow-up period of up to 1 year (Cassimatis et al., 2016).
However, the studies included in these reviews tended to compare the feedback-based balance and mobility training versus conventional training or no intervention (Cassimatis et al., 2016; Lei et al., 2019). In addition, research adopting external sensory-cued therapy training tended to offer an instructional cue (e.g., project laser to ground with a given distance from the body and rhythmic cues), rather than cues based on body posture or performance (Harrison et al., 2025; Pallavi et al., 2025). These study designs cannot isolate the effect of real-time postural feedback. The value of incorporating real-time postural feedback within balance or mobility training remains largely unclear (Dockx et al., 2016; Radder et al., 2020; Santos et al., 2019).
Therefore, this systematic review aimed to summarize the latest evidence on the effects of adding real-time postural feedback during balance and mobility training. The postural feedback should focus on the movement performance during the training, such as body sway and walking performance. To delineate the role of feedback, we targeted studies that adopted an experimental group/condition doing a basic balance or gait training with real-time postural feedback, and a control group/comparison condition doing the same basic balance/mobility training but without feedback. The immediate effect of the provision of feedback during a balance/mobility task and the post-training effect after a feedback-instilled training course were evaluated.
Methods
This systematic review was reported in accordance with the Preferred Reporting Items for Systematic Reviews and Meta-Analyses (PRISMA) guideline (Page et al., 2021; Salamh & and Kolber, 2025). The protocol of this systematic review was pre-registered on the PROSPERO website after the consolidation of the PICO model and search strategy (CRD42024522330).
Sources of Data and Searches
A comprehensive literature search of electronic databases, including PubMed, Cumulative Index to Nursing and Allied Health Literature (CINAHL), Embase, and Scopus, was performed to shortlist relevant articles. Search terms were related to the PICO model (Population, Intervention, Comparison, and Outcomes), of which Population was individuals with PD, Intervention was balance or gait training with concurrent real-time postural feedback, Comparison was a control group adopting the same balance or gait training as the intervention group but without real-time postural feedback, and Outcomes was balance and gait performances during the provision of feedback (immediate effect), or after a course of training (post-training effect), and falls. The full search strategy is shown in the Supplemental Table S1, which was checked and modified by the librarian of the university before the comprehensive search. The initial search was conducted on 11 July 2023, and the last search was performed on 3 June 2025. A forward citation search for all included articles was performed on 2 September 2025 to look for relevant articles.
Titles and abstracts were screened by two researchers (either two from HYC, CMF, SMLA, or SGSL) independently to sort out the relevant studies. Full texts of relevant studies were checked for final inclusion according to the inclusion and exclusion criteria. Any discrepancy during the screening was solved by discussion with the principal supervisor (FMHL).
Study Selection
The inclusion criteria are presented according to the PICOS (Population, Intervention, Comparison, Outcomes, and Study design) framework. Population: people with PD; Intervention: balance or gait training plus immediate postural feedback; Comparison: the same balance and gait training without the feedback component; Outcomes: balance, gait performance or falls; Study Design: (1) within-subject design, comparing the performance of targeted outcomes with and without the provision of feedback while performing the tasks (immediate effect), or (2) randomized controlled trials to illustrate the effect after training with or without feedback provided (post-training effect).
Studies were excluded if they: (1) could not fulfill the inclusion criteria; (2) were protocols; (3) had no full text; (4) were not published in English.
Methodological Quality Assessment and Quality of Evidence
The methodological quality of the included Randomized Controlled Trials (RCTs) was assessed using the PEDro scale (https://pedro.org.au/). The PEDro scores were categorized as follows: excellent (9–10), good (6–8), fair (4–5), and poor (0–3) (Cashin & McAuley, 2020). Additionally, the appraisal tool of the National Heart, Lung, and Blood Institute (NHLBI) study quality assessment was used for the methodological quality of the studies with a within-subject design (Chouksey et al., 2025; NHLBI, 2014). The overall score of this tool was categorized as high (9–12), fair (5–8), and poor quality (0–4) (Hairul Hisham et al., 2025). The methodological quality of all the RCT-designed articles and the studies with a non-RCT design were rated and verified by the two researchers independently (either two of HYC, CMF, SMLA, or SGSL). For the outcomes with a pooled effect size by meta-analysis, a GRADE profile (Grading of Recommendations Assessment, Development and Evaluation) was used to rate the quality of evidence. Specific criteria for rating the quality of evidence are presented in Supplemental Table S2 (Liang et al., 2025).
Data Extraction and Analysis
Original data of each included study were extracted and double-checked by two researchers independently (either two of HYC, CMF, SMLA, or SGSL). Subject characteristics (age, gender, and stage of PD), training dosage (type of feedback, basic training component, duration, and frequency of training), outcome measures, and the main results were retrieved. The stage of Parkinson’s disease (PD) refers to scales that measure the progression of PD in relation to functional disability. The Hoehn and Yahr (H&Y) scale is most commonly used, classifying disease severity into five stages (1–5), with higher stages indicating more severe motor symptoms (Hairul Hisham et al., 2025).
Balance and mobility were the targeted outcome measures in our study. Berg balance scale (BBS) scores, static standing balance (i.e., bipedal and unipedal stance), balance confidence, and fall efficacy scores were used to evaluate overall balance performance. Timed-Up-and-Go (TUG), walking speed, and quality of gait were extracted to examine individuals’ mobility performance.
To evaluate the isolated effect of additional real-time postural feedback on the balance and gait of PD patients, meta-analyses were conducted for outcomes that were measured by at least three articles by using the software of Comprehensive Meta-Analysis (Version 3.3.070). A random-effect model was used for the meta-analysis due to the heterogeneity in study design, subject characteristics, and training settings. Statistical heterogeneity of the meta-analysis was measured by the index of inconsistency (I2). Mean difference (MD) or standardized mean difference (SMD) with their 95% confidence intervals (CI) was computed to illustrate the isolated effect of real-time postural feedback on targeted outcome measures. Results that were not included in the meta-analysis would be synthesized by the narrative analysis to report their study design and findings.
Results
The database search found a total of 2260 records. One hundred and five records remained after the titles and abstracts screening. After the full-text screening, eleven articles (Byl et al., 2015; Carpinella et al., 2017; Ghoseiri et al., 2009; High et al., 2018; Khatavkar et al., 2024; Mayo et al., 2024; McMaster et al., 2022; Nanhoe-Mahabier et al., 2012; Pompeu et al., 2012; Winkler et al., 2022; Yang et al., 2016), fulfilled all the inclusion criteria and were included in this systematic review (Figure 1). No eligible study was found in the citation searching. A total of 226 individuals with PD were included across these articles. PRISMA flow diagram for studies selection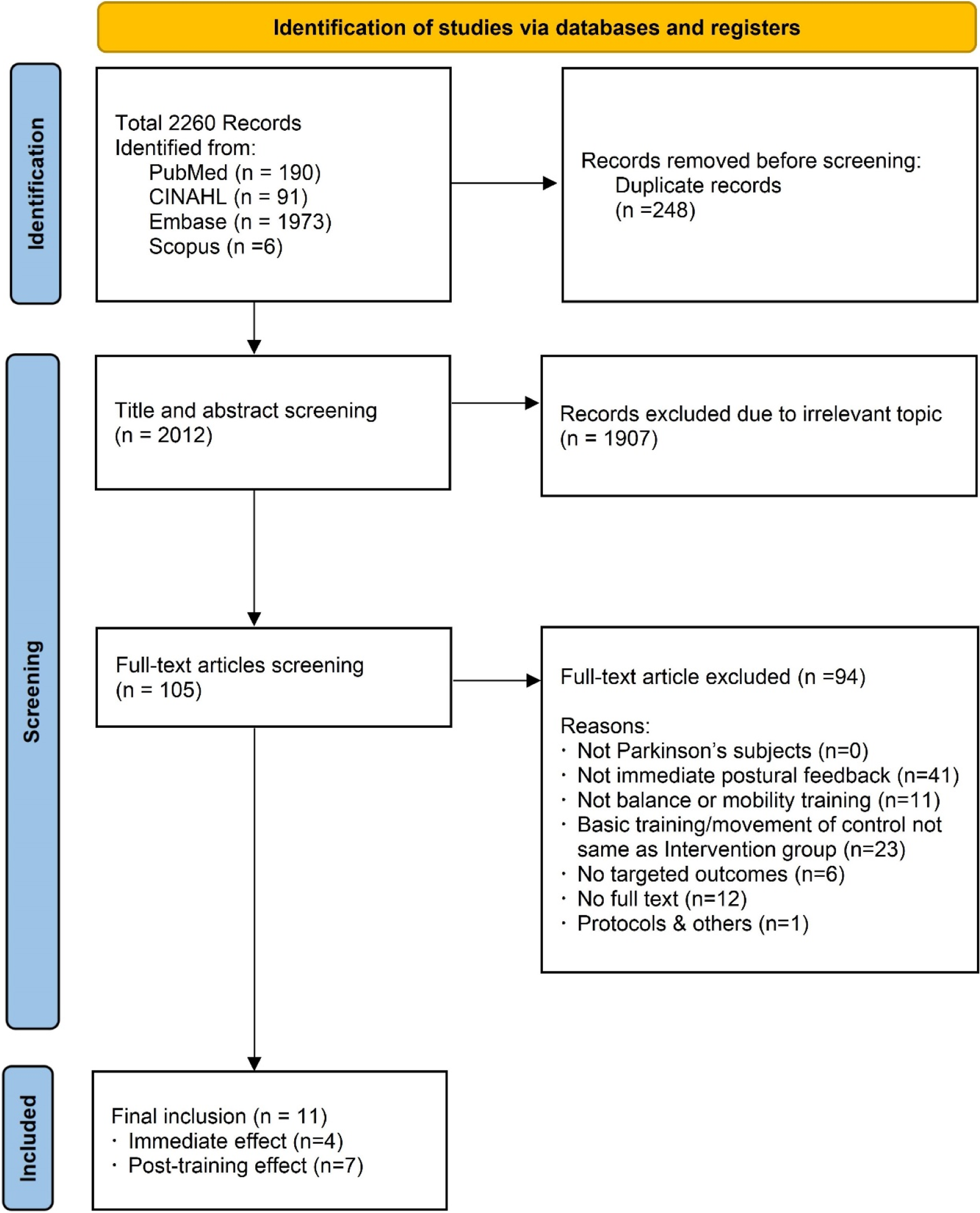
Characteristics of the Selected Studies
The mean ages of individuals ranged from 58.6 to 75.6 years. Disease severity ranged from Hoehn and Yahr (H&Y) stages 1 to 4, encompassing participants from minimal unilateral involvement (stage 1) to severe disability with preserved ability to stand or walk unassisted (stage 4). Four studies (Ghoseiri et al., 2009; High et al., 2018; Khatavkar et al., 2024; McMaster et al., 2022) adopted a within-subject design that investigated the immediate effect by comparing the balance and mobility performance across the conditions of with and without real-time postural feedback, whereas seven studies (Byl et al., 2015; Carpinella et al., 2017; Mayo et al., 2024; Nanhoe-Mahabier et al., 2012; Pompeu et al., 2012; Winkler et al., 2022; Yang et al., 2016) were randomized controlled trials evaluating the post-training effect.
Among the studies investigating the immediate effect, three studies underwent the walking or balance task with vibrotactile postural feedback on heel time, stride angle of ankle joint, and body sway that was provided by wearable devices, including a vibratory waist belt (Ghoseiri et al., 2009; High et al., 2018) or an instrumented shoe and vibratory insole (Khatavkar et al., 2024), one study provided visual feedback of mediolateral lean of the trunk during walking by a screen located at the end of the walkway (McMaster et al., 2022).
For the studies that evaluated post-training effect, three studies provided pure visual postural feedback via the screen of the training system, including a balance system with a force plate (Yang et al., 2016), Nintendo Wii (Pompeu et al., 2012), and a self-developed system with smart shoes and pants for postural monitoring (Byl et al., 2015). One study (Nanhoe-Mahabier et al., 2012) delivered pure vibratory feedback on trunk sway via a headband, and one study (Mayo et al., 2024) offered pure acoustic feedback for a good step, defined as having sufficient angular velocity at the ankle joint, that was detected by smart shoes with sensors. Multicomponent postural feedback incorporated acoustic with visual feedback (Carpinella et al., 2017), or vibrotactile feedback was adopted by two studies (Winkler et al., 2022).
Study Characteristics of Shortlisted Studies
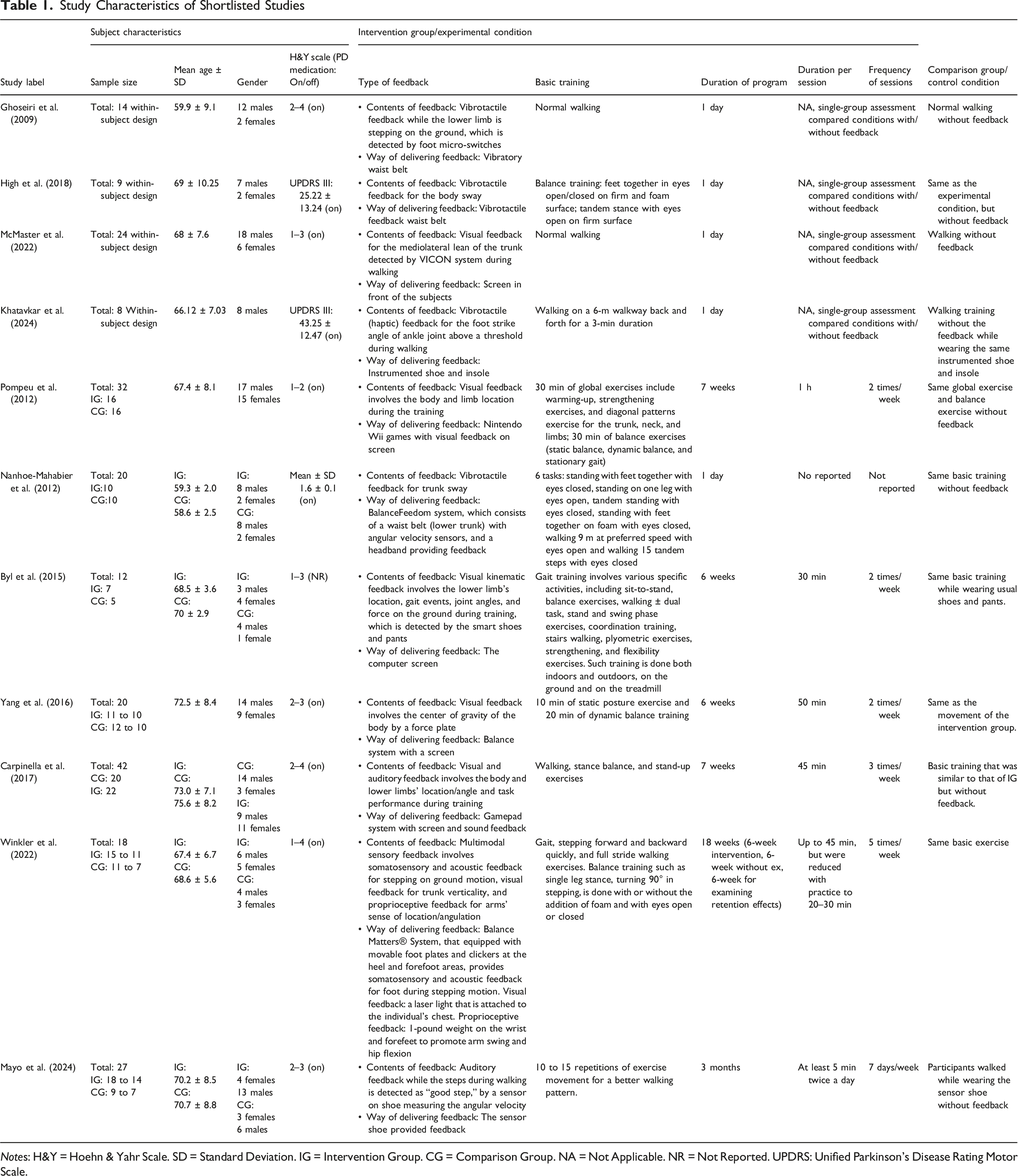
Notes: H&Y = Hoehn & Yahr Scale. SD = Standard Deviation. IG = Intervention Group. CG = Comparison Group. NA = Not Applicable. NR = Not Reported. UPDRS: Unified Parkinson’s Disease Rating Motor Scale.
The Methodological Quality of Studies and Evidence of Quality
The Methodological Quality of Randomized Controlled Trials by the Scale of Physiotherapy Evidence Database
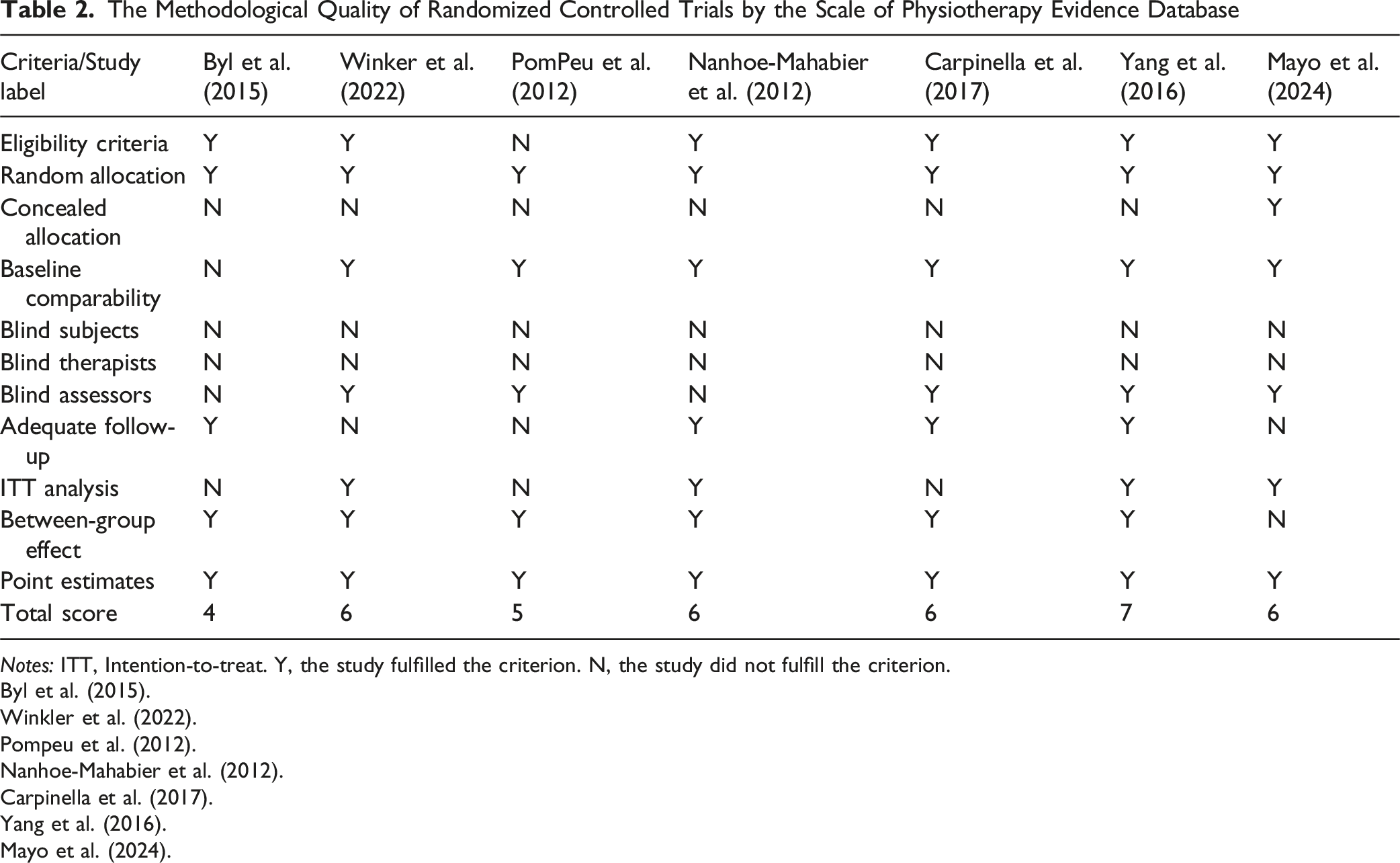

Notes: ITT, Intention-to-treat. Y, the study fulfilled the criterion. N, the study did not fulfill the criterion.
Quality of Evidence for Outcomes by Grade of Recommendation, Assessment, Development, and Evaluation Approach
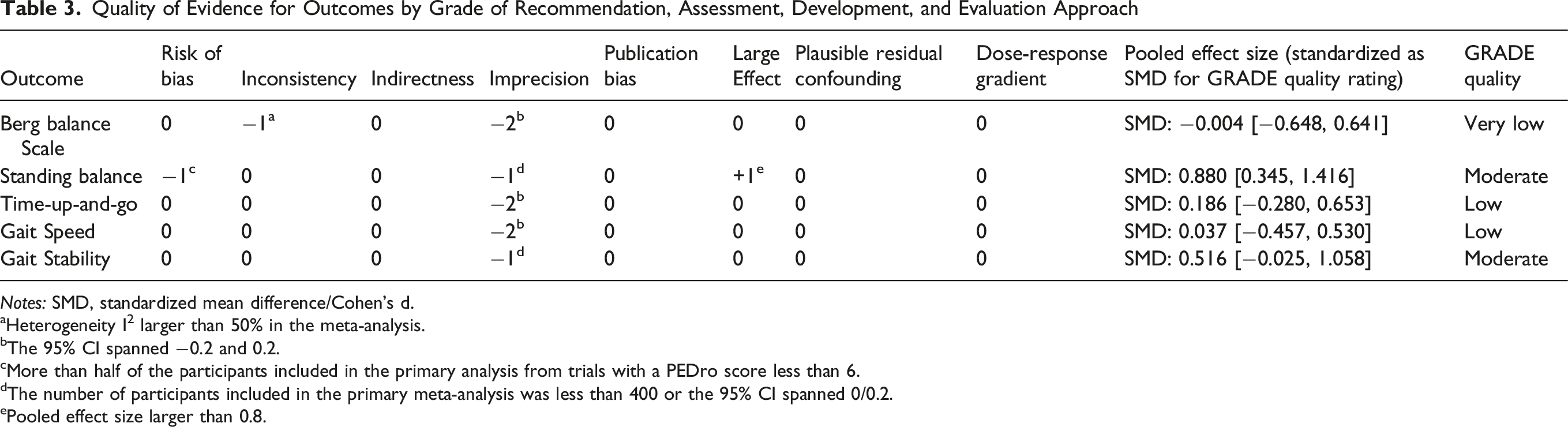
Notes: SMD, standardized mean difference/Cohen’s d.
aHeterogeneity I2 larger than 50% in the meta-analysis.
bThe 95% CI spanned −0.2 and 0.2.
cMore than half of the participants included in the primary analysis from trials with a PEDro score less than 6.
dThe number of participants included in the primary meta-analysis was less than 400 or the 95% CI spanned 0/0.2.
ePooled effect size larger than 0.8.
Immediate Effect of Real-Time Postural Feedback on Balance and Gait
Four studies (Ghoseiri et al., 2009; High et al., 2018; Khatavkar et al., 2024; McMaster et al., 2022) (n = 45) investigated the immediate effect of adding real-time postural feedback during static and dynamic balance (High et al., 2018; Khatavkar et al., 2024; McMaster et al., 2022) or gait speed (Ghoseiri et al., 2009; McMaster et al., 2022).
Only one study, which was rated as high quality, assessed static balance and reported an insignificant result. High et al. (2018) (n = 9) measured the static standing balance with the postural sway of the center of pressure (i.e., path length, sway velocity, sway area) under the condition with vibrotactile feedback or without feedback. The vibrotactile feedback was provided to the individuals with PD, when the sway from the center of their base of support exceeded 10% during balance tasks. No significant difference was found across conditions.
In contrast, two studies that were rated as high quality reported significant improvement in dynamic balance. McMaster et al. (2022) measured the mediolateral trunk lean (degree) during walking, showing that providing real-time visual feedback of the mediolateral lean of the trunk during walking to individuals with PD significantly reduced the mediolateral lean of the trunk during walking, when compared with the walking condition without feedback (3.48 versus 4.19°, p < 0.05, n = 24). In addition, Khatavkar et al. (2024) reported that walking on a 6-m walkway back and forth for 3 min with the vibrotactile (haptic) feedback on foot given when the foot strike angle above a threshold, significantly improved the foot strike angle (2.93 versus −5.43°, p = 0.0362, n = 8) and toe clearance distance (94.29 versus 87.60, p = 0.0019, n = 8) during walking, compared with the condition of the same walking without walking performance feedback.
For mobility outcome, two studies that were rated as high quality measured the walking time of a 10-m pathway or the walking velocity, and illustrated the significant but opposite results. Ghoseiri et al. (2009) indicated that the additional real-time heel-contact events sensory feedback by vibration on the waist during walking significantly improved gait speed compared with the walking condition without feedback (10.72 versus 12.14 s, p = 0.001, n = 14). However, McMaster et al. (2022) showed that the gait speed significantly decreased under the condition of visual feedback of body alignment (mediolateral lean of the trunk) when compared with the condition without visual feedback during walking (1.01 versus 1.12 m/s, p < 0.05, n = 24).
Post-training Effect of Real-Time Postural Feedback on Balance
Balance performance was measured in five randomized controlled trials mainly by the Berg Balance Scale (BBS) (Byl et al., 2015; Carpinella et al., 2017; Pompeu et al., 2012; Yang et al., 2016), and standing body sway or velocity (i.e., unipedal stance test and double leg stance test) (Carpinella et al., 2017; Nanhoe-Mahabier et al., 2012; Pompeu et al., 2012).
For the Berg Balance Scale, four studies were included in the meta-analysis. It revealed that adding real-time postural feedback during balance training (Carpinella et al., 2017; Pompeu et al., 2012; Yang et al., 2016) or gait training (Byl et al., 2015; Carpinella et al., 2017) had no difference relative to the training without feedback in individuals with PD on the Berg Balance Scale (MD = −0.079, 95% CI = −2.159 to 2.000, I2 = 63.85, n = 104, Figure 2a), with very low quality of evidence. Results of the meta-analyses; (a) Berg Balance Scale (n = 104); (b) Standing balance (n = 89); (c) Time-Up-and-Go Test (n = 72); (d) Gait speed (n = 67); (e) Gait stability (n = 55)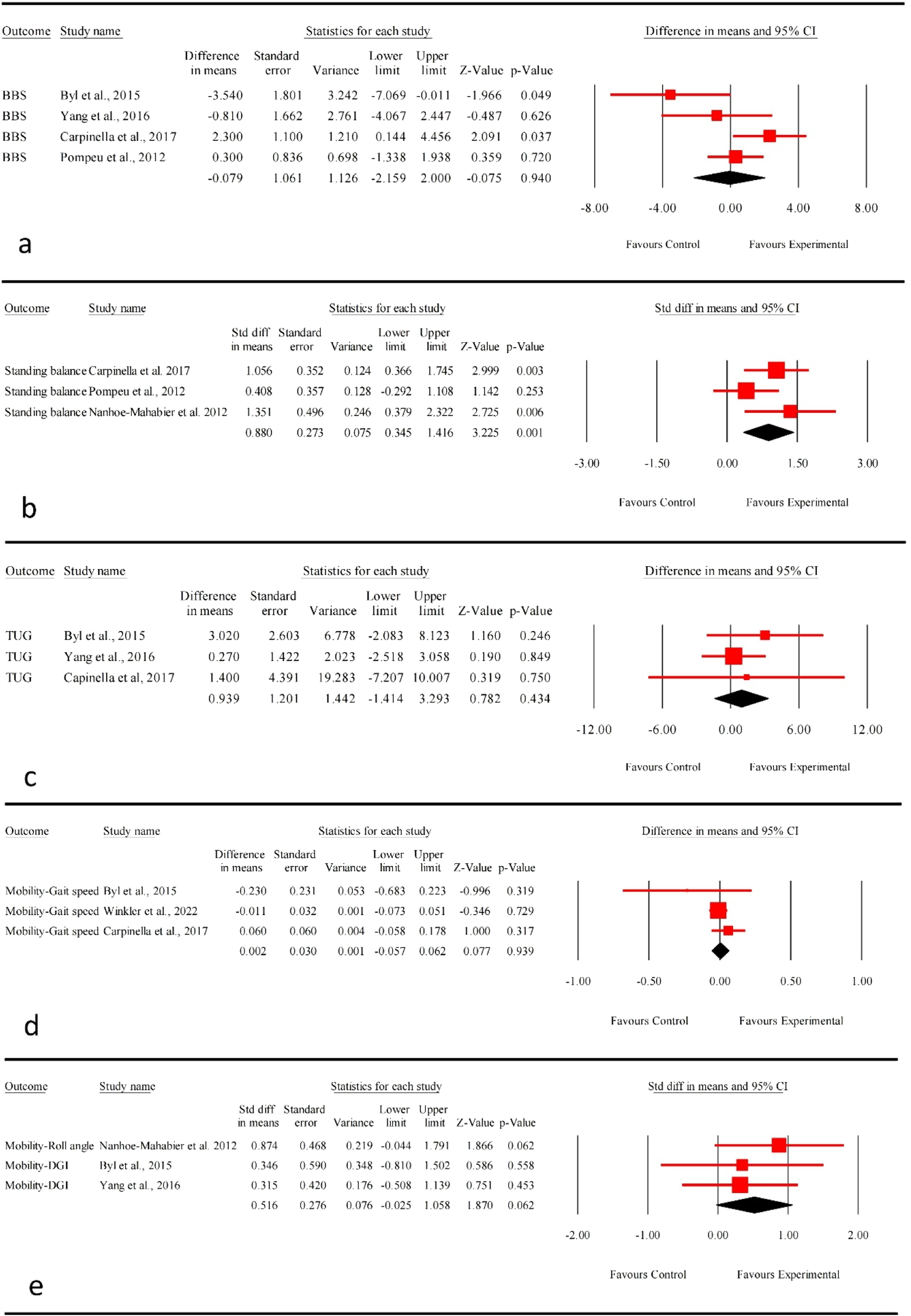
For standing balance (Carpinella et al., 2017; Nanhoe-Mahabier et al., 2012; Pompeu et al., 2012), the meta-analysis with three included RCTs indicated that the real-time postural feedback group had a significant positive effect on standing balance when compared with non-feedback training (SMD = 0.880, 95% CI = 0.345 to 1.416, I2 = 30.81, n = 89, Figure 2b) in individuals with PD, with moderate quality of evidence.
Post-Training Effect of Real-Time Postural Feedback on Mobility
Mobility performance was measured by six studies (Byl et al., 2015; Carpinella et al., 2017; Mayo et al., 2024; Nanhoe-Mahabier et al., 2012; Winkler et al., 2022; Yang et al., 2016) using the Timed-Up-and-Go test (TUG), gait speed, gait stability, and standardized walking obstacle course test.
For TUG, this functional mobility test was measured by three studies (Byl et al., 2015; Carpinella et al., 2017; Yang et al., 2016), which were included in the meta-analysis. It showed that the additional real-time postural feedback has no significant effect on TUG performance (Byl et al., 2015; Carpinella et al., 2017; Yang et al., 2016) (MD = 0.939, 95% CI = −1.414 to 3.293, I2 = 0, n = 72, Figure 2c), with low quality of evidence. Besides, Winkler et al. (2022) reported an insignificant result on dual-task TUG.
Gait speed was measured by three studies (Byl et al., 2015; Carpinella et al., 2017; Winkler et al., 2022). The meta-analysis showed that no effect was observed after adding real-time postural feedback during training on gait speed when compared with training without feedback (MD = 0.002, 95% CI = −0.057 to 0.062, I2 = 5.205, n = 67, Figure 2d), with low quality of evidence.
Gait stability was measured in three studies (Byl et al., 2015; Nanhoe-Mahabier et al., 2012; Yang et al., 2016) by the Dynamic Gait Index (DGI) (Byl et al., 2015; Yang et al., 2016) and the roll angle during walking (Nanhoe-Mahabier et al., 2012). The meta-analysis showed an insignificant result after adding real-time postural feedback when compared with training without feedback (SMD = 0.516, 95% CI = −0.025 to 1.058, I2 = 0, n = 55, Figure 2e), with moderate quality of evidence.
Other mobility outcomes reported included walking obstacle course and 6-min walking test with contrasting results (Mayo et al., 2024). A significantly worse obstacle course performance was noted after the walking training with feedback, compared with the walking training without feedback (with feedback: 4.3 seconds; without feedback: −6.1 s, n = 22). In contrast, the group that received walking training with feedback showed a significantly greater improvement in six-minute walk test performance (with feedback: 66.4 m; without feedback: −19.4 m, n = 20).
Post-training Effect of Real-Time Postural Feedback on Falls
Falls-related outcome was reported by only one RCT using the Activities-Specific Balance Confidence Scale (ABC) (Carpinella et al., 2017). The study adopted virtual and auditory real-time postural feedback during the balance and walking training, indicating an insignificant effect on ABC (p = 0.186) after training.
Discussion
This systematic review was the first review that summarized evidence on the isolated effect of adding real-time postural feedback during balance or mobility training on balance, mobility, and falls in individuals with PD. The results showed that real-time postural feedback boosted the immediate performance of dynamic balance and modulated walking speed with no effect on static balance. For post-training effect, adding real-time postural feedback only significantly improved standing balance with no effect on mini-BESTest, TUG, gait speed, and gait stability. Furthermore, with only a single study reporting a non-significant effect of ABC, the effect of real-time postural feedback on falls-related outcomes remains inconclusive. With the heterogeneity observed in the results, the discussion of this review will be centered around the potential reasons for the heterogeneity of the results.
Outcome-Matching Feedback Could be Important for a Significant Immediate Effect
Our results suggested that additional real-time postural feedback may improve performance on dynamic balance immediately. This aligned with mechanistic studies showing that the external feedback or cues of the performance enhanced the functional connectivity between the supplementary motor area (Zadeh et al., 2024), which is the foundational structure of the complex motor planning and motor coordination (Nachev et al., 2008).
However, this enhancement was not observed in static balance and gait speed. A potential reason for this phenomenon could be the mismatched feedback content with the targeted outcomes. In general, outcomes that do not align with the feedback provided have reported unfavorable immediate effects (McMaster et al., 2022). In contrast, outcomes that demonstrated favorable immediate effects were often coupled with outcome-matching, specific feedback (Ghoseiri et al., 2009; Khatavkar et al., 2024; McMaster et al., 2022). For instance, providing feedback on trunk lean angle during walking could improve dynamic balance during walking but not gait speed (McMaster et al., 2022). The only exception to this observation came from a study that failed to improve standing balance even by providing outcome-matching feedback, which was potentially due to a small sample size (n = 9) (High et al., 2018). Therefore, it appears that outcome-matching feedback could be important for the improvement observed.
To date, there is no review article that focuses on the real-time postural feedback on immediate effects in individuals with PD directly. Nevertheless, our findings generally align with other similar reviews recently published. For example, a recent narrative review pooled results from four studies that combined immediate and post-training effects of real-time electromyographic biofeedback in Parkinson’s disease (PD) and reported overall benefits on motor outcomes, including postural instability (Diotaiuti et al., 2025). Another systematic review has demonstrated that the immediate effect of dynamic balance was improved by external real-time postural feedback in healthy older adults (Liang et al., 2024).
Overall, considering only four studies included for immediate effect with a small sample size, even though the studies were rated as high quality, a strong conclusion cannot be drawn. Real-time postural feedback appears to be able to improve balance and gait performance when the feedback provided matches with the targeted outcomes.
Gradual Reduction in the Provision of Feedback May Lead to Better Post-Training Outcome
The meta-analyses suggested that additional feedback improved standing balance, but not BBS, the comprehensive balance performance evaluation scale, and other mobility outcomes including TUG, gait speed, and gait stability.
The heterogeneity of the post-training effect could be potentially explained by the different dosages of the real-time postural feedback component during balance or walking training. The only two (Carpinella et al., 2017; Nanhoe-Mahabier et al., 2012) studies that have reported significant improvement both reduced the provision of real-time postural feedback over the training course. Nevertheless, all insignificant studies have provided feedback continuously without modulation during training (Byl et al., 2015; Mayo et al., 2024; Pompeu et al., 2012; Winkler et al., 2022; Yang et al., 2016). This may explain why the improvement was observed only in the meta-analysis of standing balance: it is the only outcome assessed in both studies that reduced feedback provision during training (Carpinella et al., 2017; Nanhoe-Mahabier et al., 2012).
Indeed, previous studies have suggested that providing frequent external feedback during task performance could potentially disrupt learning through the implicit mechanism in the long term (Maxwell et al., 2001; Orrell et al., 2006a, 2006b), which is important for improving balance performance (Orrell et al., 2006a). With external feedback provided throughout the training course, participants could have accommodated to completing balance or mobility tasks under the provision of postural feedback, and gradually developed reliance. However, after the training sessions, the improvement based on the feedback provision would be eliminated in the post assessment, as no feedback was provided during the assessment tasks.
Therefore, it appears that the initial feedback provided insight into the improvement required. Gradually reducing real-time feedback hereafter may allow individuals with PD to learn motor skills and wean off the reliance on extrinsic feedback (Liang et al., 2024), potentially leading to a significant post-training improvement. Given that the level of evidence was moderate for the meta-analysis of static balance, it suggested that additional real-time postural feedback may improve the post-training effect of static balance. However, this needs to be confirmed by larger studies.
Outcome-Matching Feedback Could Also be Essential for Post-Training Improvement
Another potential explanation for the heterogeneity of the meta-analyses could be the mismatch between the feedback provided and the targeted outcome. Postural feedback, such as body sway and limb location, was found to significantly improve standing balance, which is highly relevant to the feedback provided (Carpinella et al., 2017; Nanhoe-Mahabier et al., 2012; Pompeu et al., 2012). However, postural feedback is consistently unable to improve mobility reflected in speed-related measures, including TUG and gait speed, which do not match with the nature of the feedback provided (Byl et al., 2015; Carpinella et al., 2017; Mayo et al., 2024; Winkler et al., 2022; Yang et al., 2016).
A recent systematic review investigated the effect of haptic cues on gait in individuals with PD and indicated the improvement in gait speed (Maddumage Dona et al., 2025), which differs from our review finding. It may be attributed to that the rhythmic cue emphasizes the improvement of automaticity, whereas postural feedback in our review focuses on the segment alignment during the task. Therefore, rhythmic cue could improve walking speed, while postural feedback, which was included in the present review, improves postural stability but not speed.
Overall, our review suggested that the real-time postural feedback provided may need to match the outcomes targeted for improvement of the post-training effect. Given the limited number of included studies, further studies with a large sample size are needed to verify.
Practical Implications
Our review shows that providing real-time postural feedback might improve the immediate effect of dynamic balance in people with various severities of Parkinson’s disease (H&Y stage 1–3/UPDRS III 22-61) if the feedback provided matches the intended outcomes. For the feedback provision, the visual and vibratory feedback were shown to be effective, delivered by dedicated training systems or wearable devices.
Incorporating feedback in balance or walking training may also augment the improvement post-training in people with various severities of Parkinson’s disease (H&Y stage 1–4). The feedback provided may need to match closely with the target outcome. It appears that the intensity of the feedback, provided by a vibratory, auditory or combination of visual and auditory stimuli, may need to be gradually reduced to achieve a post-training improvement.
Given the limited included studies and the limitations of the study design, a strong practical recommendation cannot yet be made, and these preliminary findings warrant further investigation and validation.
Limitations
The systematic review has several limitations. Firstly, most of the real-time postural feedback of the included studies was provided to participants with PD by vision or a multi-component sensory model. The results of this review cannot be generalized to other feedback delivery models. Secondly, despite our search keywords containing falls, with only one study reporting the falls-related outcomes (ABC), we cannot conclude the post-training isolated effect of real-time postural feedback during balance or gait training on falls. Thirdly, the small sample size of the included studies (range: 8 to 42) may lead to insufficient power to detect significant changes in immediate effect (e.g., static standing balance) and post-training effect (e.g., walking stability). Finally, the quality of evidence for outcomes was rated as very low to moderate. The results may change as the new study with a large sample size is included in the future.
Conclusion
Our findings suggest that providing real-time postural feedback may have an immediate effect on improving dynamic balance and modulating gait speed. Adding postural feedback to a course of balance training appears to augment the improvement in standing balance. The provision of feedback may need to match with the targeted outcomes to yield significant immediate and post-training improvement. Gradually reducing the postural feedback provided over the course of training may help to improve its post-training effect. Given the limited studies investigating the isolated effect of real-time postural feedback and the very low to moderate quality of the evidence for the meta-analysis, further research with a large sample size is warranted.
Supplemental Material
Supplemental Material—Does Adding Real-Time Postural Feedback During Training Boost Balance and Mobility in Individuals With Parkinson’s Disease? A Systematic Review and Meta-Analysis
Supplemental Material for Does Adding Real-Time Postural Feedback During Training Boost Balance and Mobility in Individuals With Parkinson’s Disease? A Systematic Review and Meta-Analysis by Guoshi Liang, Hou Yee Ching, Chiu Man Fu, Sin Man Agnes Lau, Wayne Lap Sun Chan, Meizhen Huang, Freddy Man-Hin Lam in Journal of Applied Gerontology
Footnotes
Ethical Considerations
Ethics approval and informed consent were not needed as the research resources were the literature.
Author Contributions
Guoshi Liang: Data curation, Formal analysis, Investigation, Writing—original draft.
Hou Yee Ching: Data curation, Formal analysis, Writing—original draft.
Chiu Man Fu: Data curation, Formal analysis, Writing—original draft.
Sin Man Agnes Lau: Data curation, Formal analysis, Writing—original draft.
Wayne Lap Sun Chan: Conceptualization, Validation, Writing—review & editing.
Meizhen Huang: Conceptualization, Methodology, Writing—review & editing.
Freddy Man-Hin Lam: Conceptualization, Methodology, Supervision, Writing—review & editing.
Funding
The authors disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This work was supported by the Start-up Fund of The Hong Kong Polytechnic University (P0034487, 2020); and the Departmental General Research Fund of The Hong Kong Polytechnic University (P0042679, 2022).
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Data Availability Statement
Data are available from the corresponding author on reasonable request.
Footnote
This study followed the guidance of the Preferred Reporting Items for Systematic Reviews and Meta-Analyses (PRISMA) and was registered in PROSPERO (CRD42024522330).
Supplemental Material
Supplemental material for this article is available online.
