Abstract
Using longitudinal data from Wave 9 (2018/19) and two COVID-19 sub-studies of the English Longitudinal Study of Ageing (N = 4994), we examined how partnership status and relationship quality in the early months of the pandemic (June/July 2020) related to depression, anxiety, and life satisfaction (November/December 2020) among older people. Associations were analyzed using logistic regression models while controlling for socioeconomic and demographic factors as well as pre-pandemic mental health. We found that respondents in poor-quality partnerships reported higher depression (OR = 2.79, 95% CI = 2.07–3.76), anxiety (OR = 2.62, 95% CI = 1.74–3.94), and low life satisfaction (OR = 2.19, 95% CI = 1.67–2.86) than those in fair partnerships. Results also indicate that better partnership quality was associated with better mental health, while being in a poor partnership was as detrimental to mental health as not having a cohabiting partner. Relationship quality is important for mental health, particularly when policies restricting contact and mobility may exacerbate relational issues.
• During the pandemic, unpartnered older people reported poorer mental health. • However, among those living with a partner, the quality of their relationships was important for their mental health during the pandemic. Poor-quality relationships were as detrimental as having no partner. • Respondents with poor-quality relationships with their partners were more likely to report depression, anxiety, and lower life satisfaction throughout the first year of the pandemic (when stay-at-home recommendations were in place).
• This research gives insights into the importance of relationship quality among older people and how living with someone with whom the relationship is poor could affect mental health, particularly at a time when other interactions are limited. • This study incorporates a longitudinal approach to better investigate the complex interplay between partnership and relationship quality and mental health and account for confounding characteristics. • Public health interventions and policies should also consider partnership and relationship quality to limit unintended side effects on mental health.What this paper adds
Applications of study findings
Introduction
The coronavirus disease 2019 (COVID-19) pandemic forced people worldwide to face stressful and overwhelming challenges that impacted their mental health and well-being. Acute stress symptoms and fear of infection were highly prevalent during the early phases of the pandemic (Li et al., 2021). Furthermore, depression, anxiety, and insomnia persisted at a high prevalence rate throughout the pandemic (Nochaiwong et al., 2021). In the UK, mental health conditions worsened in the first year after the first national lockdown, with the deterioration in mental health remaining substantial even after the lockdown was lifted (Patel et al., 2022). Approximately one in five adults had moderate-to-severe depression in early 2021, which was more than double what was observed pre-pandemic (Williams et al., 2021). Older adults, who were at a higher risk of serious illness and death from COVID-19, were vulnerable to pandemic-related mental health issues (Armitage & Nellums, 2020; Lithander et al., 2020), particularly among those with more at-risk health profiles (Di Gessa & Price, 2021, 2022; Steptoe & Di Gessa, 2021).
Public health actions were necessary to reduce the spread of COVID-19. The UK government announced its first lockdown in March 2020, which included the closure of educational institutions, community facilities (e.g., libraries), and all non-essential shops and services. People were also instructed to stay indoors, limit travel and movements, work from home and homeschool if possible, and avoid or at least limit interactions with individuals outside their immediate households, including relatives, friends, and the general public. Given that the risks of serious illness and death from COVID-19 increased with age and that many pre-existing diseases strongly correlated with age, recommendations and policies from Governments targeted particularly older people (Ayalon, 2020; Perra, 2021). From March 2020, in the UK, all those aged over 70 years and “vulnerable” were advised to stay indoors and limit their interactions with others for at least three months. Although some rules were relaxed for a few months in the early summer of 2020, many restrictions remained in place, and in September 2020, gatherings of more than six people were banned. In October, a three-tier system of COVID-19 restrictions started in England, with areas assigned to different levels of restrictions based on transmission levels, rates of infection, age distributions, and the capacity of local healthcare services. A second national lockdown was reintroduced in England in November 2020 for a month, followed by a stricter tier system and a third lockdown in January 2021 (https://www.gov.uk/coronavirus).
While the aim and main benefits of these policies were to contain the spread of the disease and save lives, they also substantially disrupted people’s lives and affected the mental health of the population both directly and indirectly (Brooks et al., 2020; Di Gessa et al., 2023; Di Gessa & Zaninotto, 2023; Pfefferbaum & North, 2020; Price & Di Gessa, 2024; Wels et al., 2023). In particular, during the COVID-19 pandemic, concerns arose about the mental health of individuals living alone, whose in-person social interactions were drastically reduced (Rudert & Janke, 2023) and who were considered at a higher risk of experiencing mental health difficulties. Evidence suggests that those living alone were generally at a higher risk of poorer mental health than those living with others, especially those who were cohabiting with a partner (Ahmad et al., 2020; Kikuchi et al., 2022; McElroy et al., 2023; Nkire et al., 2021; Robb et al., 2020). It has been hypothesized that, during the COVID-19 pandemic, individuals living with their partner could, to some extent, compensate for the lack of social contacts outside the home (Hiekel & Kühn, 2022). Previous research has often found that being married or living with a partner was generally associated with better mental health and well-being (Carr & Springer, 2010; Umberson & Thomeer, 2020). However, studies increasingly call attention to the role that the quality of the relationship plays on health, with research conducted before the pandemic showing that it is those with higher marital relationship quality who report lower stress and depression levels (Holt-Lunstad et al., 2008; Miller et al., 2013; Robles et al., 2014; Teo et al., 2013). People’s relationships might have been directly affected by the COVID-19 pandemic and related policies (Stanley & Markman, 2020). Lockdown measures and restricted mobility increased time availability at home for family members and couples, resulting in the possibility of spending more time together and enjoying themselves in a domestic setting, but also in the risk of getting stuck in negative or conflictual interactions, as suggested by several reports of increased domestic violence around the world (Brink et al., 2021; Usher et al., 2020).
To date, few studies have investigated the role of partnership status and quality during the COVID-19 pandemic on mental health. The pandemic could exacerbate problems within couple relationships by amplifying pre-existing inter-partner conflict and reducing emotional support from friends and relatives under lockdown conditions. Existing studies that have examined couple relationships and mental health during the pandemic show that those with poorer quality relationships fare worse than couples with no conflicts and supportive partners (Ahmad et al., 2020; Nkire et al., 2021; Pieh et al., 2020; Robb et al., 2020; Sachser et al., 2021). For instance, a study during the early pandemic period (April 2020) in Austria showed that co-residing adults in a poor-quality relationship were more likely to report depression and anxiety than those in a good-quality relationship (Nkire et al., 2021). However, most of these studies were cross-sectional, making it difficult to disentangle the role of the pandemic and whether poorer mental health precedes or follows poorer quality relationships. Moreover, these studies often used non-representative convenience samples, with results that cannot be generalized. Finally, most studies have overlooked the quality of relationships among older people, who, especially during the early phases of the COVID-19 pandemic, were the primary targets of policy recommendations and were advised to stay indoors and limit their physical interactions with others. These policies might have forced many older couples to live in much closer and continual contact than in pre-pandemic times, exacerbating potential relational issues as well as influencing their mental health.
Thus, this study contributes to the literature by using a nationally representative study that employed a longitudinal design with pre-pandemic and follow-up data: the English Longitudinal Study of Ageing (ELSA). Using ELSA, we investigate the relationship between partnership status and quality and mental health (namely, depression, anxiety, and well-being) among older adults in England during the COVID-19 pandemic. First, we explore the association of partnership status and quality during the early pandemic (June−July 2020) with mental health conditions during the late pandemic (November−December 2020) while accounting for potential confounding factors, including pre-pandemic mental health. Second, focusing on partnered respondents, we examine how changes in partnership quality relate to mental health.
Data and Methods
Study Design and Population
We used data from the English Longitudinal Study of Ageing (ELSA), a longitudinal biennial survey that represents individuals aged 50 and older residing in private households in England. The study sample is periodically refreshed with new participants to ensure it remains representative of those aged 50 and over. Each sample is drawn from households that previously responded to the Health Survey for England, an annual cross-sectional survey that uses a clustered stratified probability sampling technique and is designed to monitor the health of the general population. ELSA started in 2002, with an initial individual response rate of 67% (Banks et al., 2021; Steptoe et al., 2013). During the pandemic, ELSA members were invited to participate online or via computer-assisted telephone interviews in two COVID-19 sub-studies, which collected information in June/July and November/December 2020, respectively (75% response rate in both waves and 94% longitudinal response rate). Additional information about the survey’s sampling frame, methodology, and ethical approvals is available at https://www.elsa-project.ac.uk. Informed consent was obtained from all participants. All data can be accessed through the UK Data Service (SN 8688 and 5050).
The main analyses focused on core members who participated in both COVID-19 sub-studies and had available information in Wave 9 (N = 4994). To investigate changes in relationship quality before and after the pandemic, we further restricted our analyses to core members whose partnership status did not change between Wave 9 and the first COVID-19 sub-study (in June/July 2020) and who had information on relationship quality prior to COVID-19. In Wave 9, questions about the quality of the relationships were included in the self-completion questionnaire, with a response rate of ∼80%, which reduced the sample to N = 4280.
Exposure Variables: Cohabiting Partnership and Quality
All participants were asked whether they lived with a spouse/partner when ELSA COVID-19 sub-study Wave 1 was collected. Those living with the spouse/partner were further questioned about the quality of their relationship. This was assessed using a set of seven statements: three addressing positive aspects of the relationship (“How much your partner understands the way you feel about things”; “How much can you rely on your partner if you have a serious problem”; and “How much can you open up to your partner if you need to talk about your worries”) and four addressing negative aspects (“How much your partner criticizes you”; “How much your partner lets you down”; “How much your partner gets on your nerves”; and “How often your partner makes too many demands on you”). For all statements, the response choices were four-point Likert scales (“Not at all” (0), “A little” (1), “Some” (2), “A lot’ (3)). In line with previous research utilizing these questions (Khondoker et al., 2017; Liao & Scholes, 2017), the total score of partnership quality was calculated by reverse-coding negative feelings and then summing all items. Total scores range from 0 to 21, with higher scores indicating higher partner relationship quality. In the present study, Cronbach’s alpha for partner relationship quality items was 0.83, suggesting good internal consistency. Since no validated cut-off point exists for this score, quartile points were used to divide participants into four groups: poor partnership quality (total score <15), fair partnership quality (15 ≤ total score <18), good partnership quality (18 ≤ total score <20), and excellent partnership quality (total score ≥20). Based on partnership status and relationship quality, respondents were grouped into five mutually exclusive categories: not living with a spouse/partner and living with a spouse/partner with whom the quality of the relationship is poor, fair, good, or excellent. Additionally, to address the second research objective regarding the relationship between changes in partnership quality and mental health, we calculated changes in relationship quality over time. Using the same cut-offs on data collected in Wave 9 and focusing on those who did not experience changes in partnership status, we defined changes in partnership quality from pre-pandemic to early pandemic by quartile shifts: no change, improvement (one quartile up or more), deterioration (one quartile down or more), and remaining without a partner at both times.
Outcome Variables: Depression, Anxiety, and Life Satisfaction
Participants’ mental health was assessed through depression, anxiety, and life satisfaction. Depression was examined using a short version (eight items) of the Centre for Epidemiology Studies Depression scale (CES-D-8), which has good validity and reliability (Cronbach’s α > 0.95) (Radloff, 1977; Steffick, 2000). The CES-D-8 scale consists of eight binary (no/yes) questions that ask respondents whether they experienced any depressive symptoms, such as feeling sad or having restless sleep, during the week prior to the interview. In line with previous studies, respondents who scored 4 or higher were classified as having elevated depressive symptoms (Steffick, 2000). Anxiety was assessed using the seven-item Generalized Anxiety Disorder scale (GAD-7) at the COVID-19 sub-study waves. The GAD-7 has good validity and reliability (Cronbach α = 0.90 in this study) (Spitzer et al., 2006). This scale evaluates the presence of seven symptoms of anxiety in the past 2 weeks, such as becoming easily annoyed or irritable or not being able to stop or control worrying, with responses ranging from “not at all” (0) to “nearly every day” (3). The total GAD-7 scores range between 0 and 21, with significant symptoms of anxiety defined as a score of 10 or higher (Spitzer et al., 2006). Lastly, we considered life satisfaction assessed by the Office for National Statistics (ONS) well-being scale with the question “On a scale of 0 to 10, where 0 is ‘not at all’ and 10 is ‘very’, how satisfied are you with your life nowadays?” This allows respondents to integrate and weigh various life domains in the way they choose (Pavot & Diener, 1993). Respondents were classified as having low life satisfaction if they scored six points or less (Office for National Statistics, 2018).
Covariates
Our analyses controlled for several demographic, socioeconomic, behavioral, and physical health factors. We controlled for age, sex, and ethnicity (White/Non-white). As indicators of socioeconomic status, we controlled for employment status during the pandemic (Retired/Employed/Other); financial situation since the pandemic (Worse off/Same/Better off); food insecurity (Always enough food/Not always enough food); pre-pandemic educational level (recoded into “Below secondary” vs “University or above,” following the International Standard Classification of Education); perceived social position (Melchior et al., 2013); and whether respondents had access to a garden at home. For behavioral and physical health factors, we considered physical activity since the pandemic (Less than usual/Same/More than usual) and impairment with any activities of daily living, such as bathing and shopping. Social connections with non-cohabiting immediate family and relatives/friends were assessed based on the frequency of phone calls (twice or less often a week vs three times or more). Finally, we further controlled for pre-pandemic measures of mental health, as these might influence both the ability to form (high-quality) relationships during the pandemic and mental health outcomes during the pandemic. In Wave 9, we used the same measures of depression and life satisfaction (see above for derivation); however, since GAD-7 was not included in pre-pandemic Waves, we used the ONS anxiety scale (with high levels of anxiety defined as a score of 6 or more).
Analytical Strategy
Following descriptive analysis, we used logistic models to examine associations between cohabiting partnership status and quality assessed in June/July 2020 and mental health in November/December 2020 (the first objective). All models were adjusted for the demographic, socioeconomic, and health variables detailed above, along with relevant pre-pandemic mental health measures. To better understand how and to what extent relationship quality matters, we selected “fair quality” of partnership as a reference category in our analyses. This category was chosen to highlight differences between the extremes in the range of partnership and quality (no partner or low quality on the one hand, and high quality on the other) and simplify the interpretation of results. Furthermore, in our models, we used a two-step strategy, initially adjusting for demographic, socioeconomic, and health characteristics (Model 1), and then further adjusting for pre-pandemic measures of the relevant mental health under study (Model 2). To address the second objective, we performed logistic regression models examining changes in relationship quality between pre-pandemic and early-pandemic (June/July 2020) and mental health measured in November–December 2020 (late pandemic). Even for these analyses, we accounted for all covariates described above as well as relevant pre-pandemic mental health. Longitudinal sampling weights were employed to account for different sampling probabilities and non-response (NatCen, 2020). All computations were performed using Stata version 18 (Stata Corp, Union Station, Texas, USA).
Results
Sample Characteristics, by Partnership Status and Quality During COVID-19.
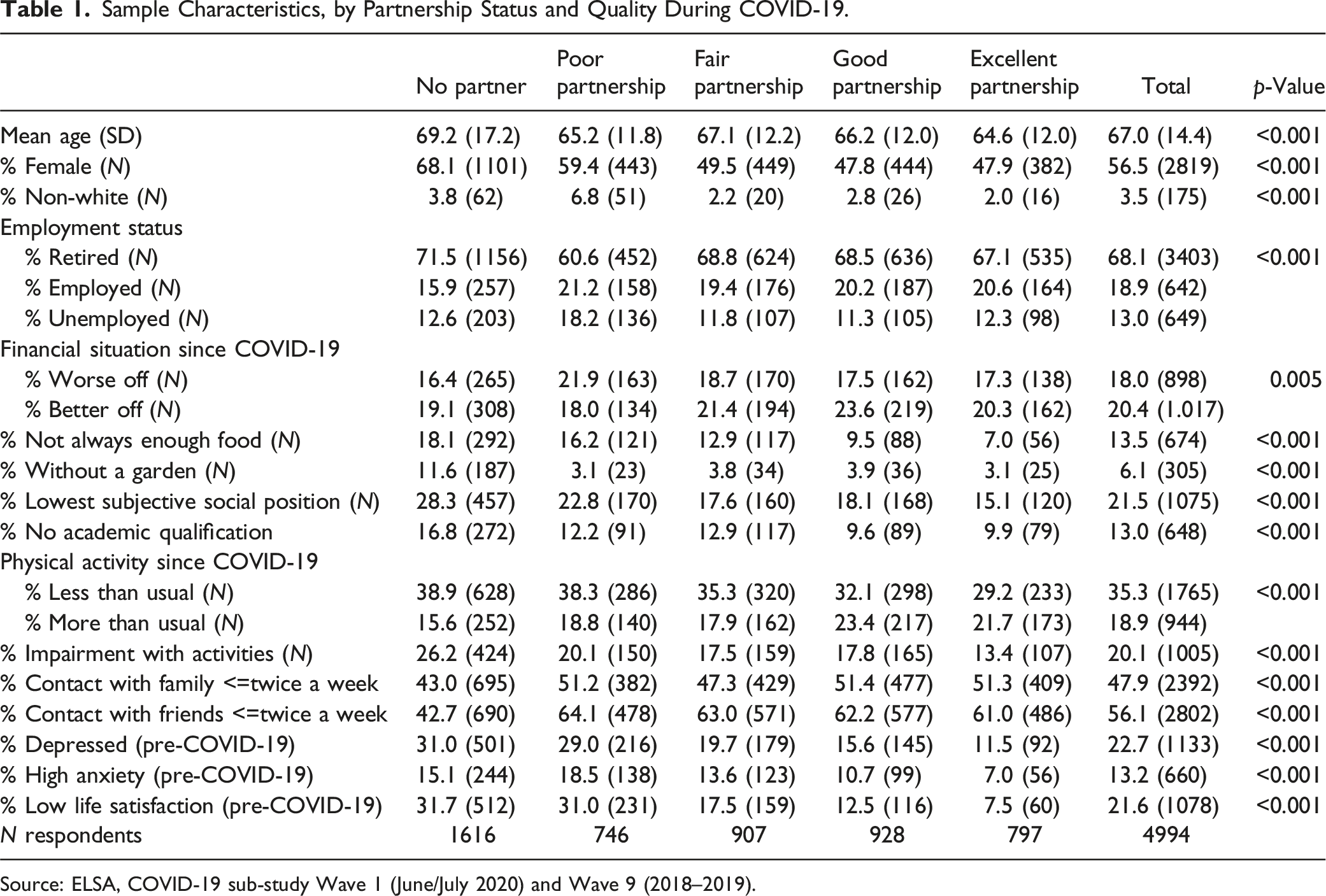
Source: ELSA, COVID-19 sub-study Wave 1 (June/July 2020) and Wave 9 (2018–2019).
Associations Between Partnership Status and Quality in June/July 2020 and Mental Health in November/December 2020.
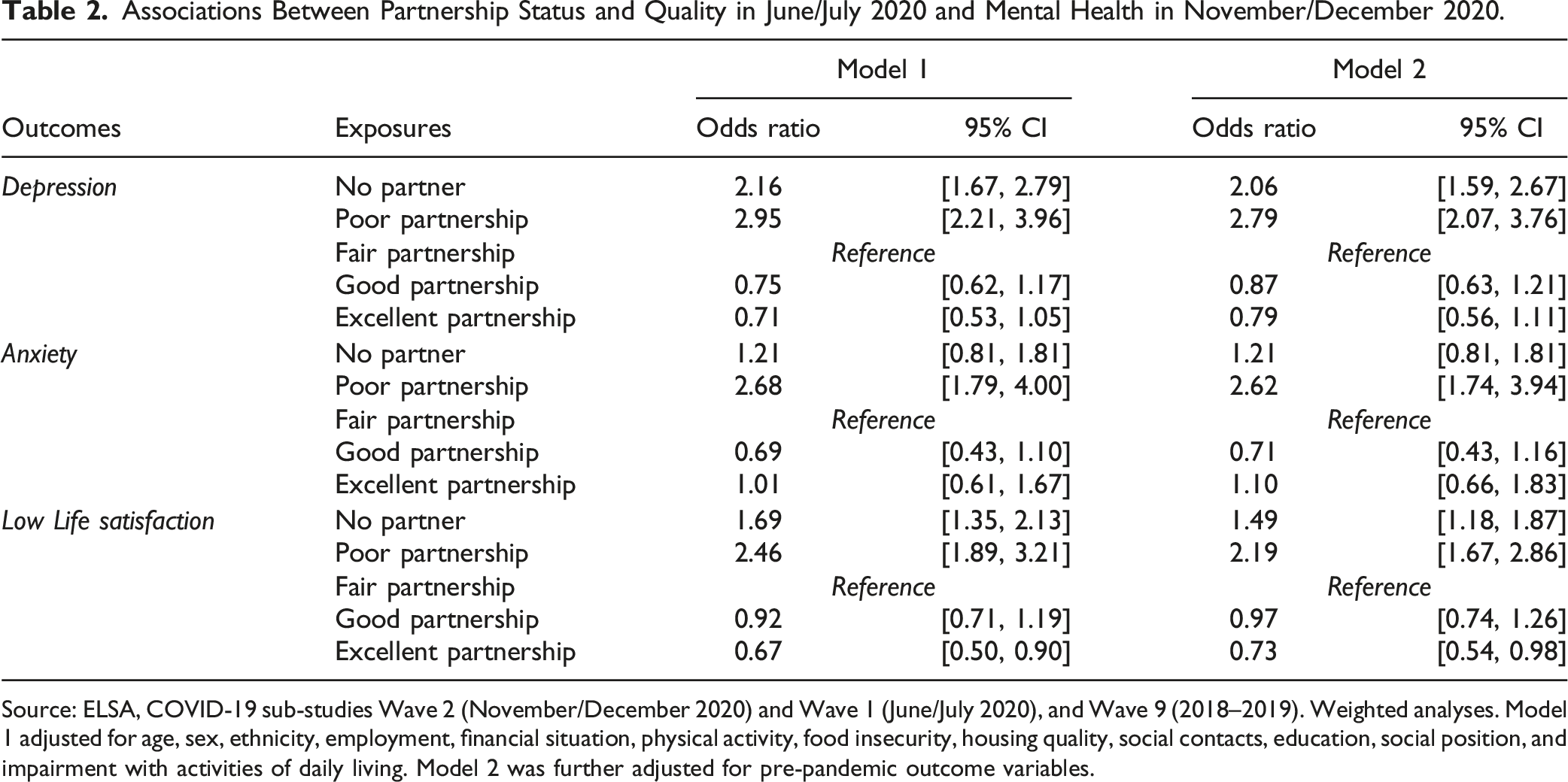
Source: ELSA, COVID-19 sub-studies Wave 2 (November/December 2020) and Wave 1 (June/July 2020), and Wave 9 (2018–2019). Weighted analyses. Model 1 adjusted for age, sex, ethnicity, employment, financial situation, physical activity, food insecurity, housing quality, social contacts, education, social position, and impairment with activities of daily living. Model 2 was further adjusted for pre-pandemic outcome variables.
Associations Between Changes in Partnership Status and Quality (Between Pre-pandemic and June/July 2020) and Mental Health in November/December 2020.
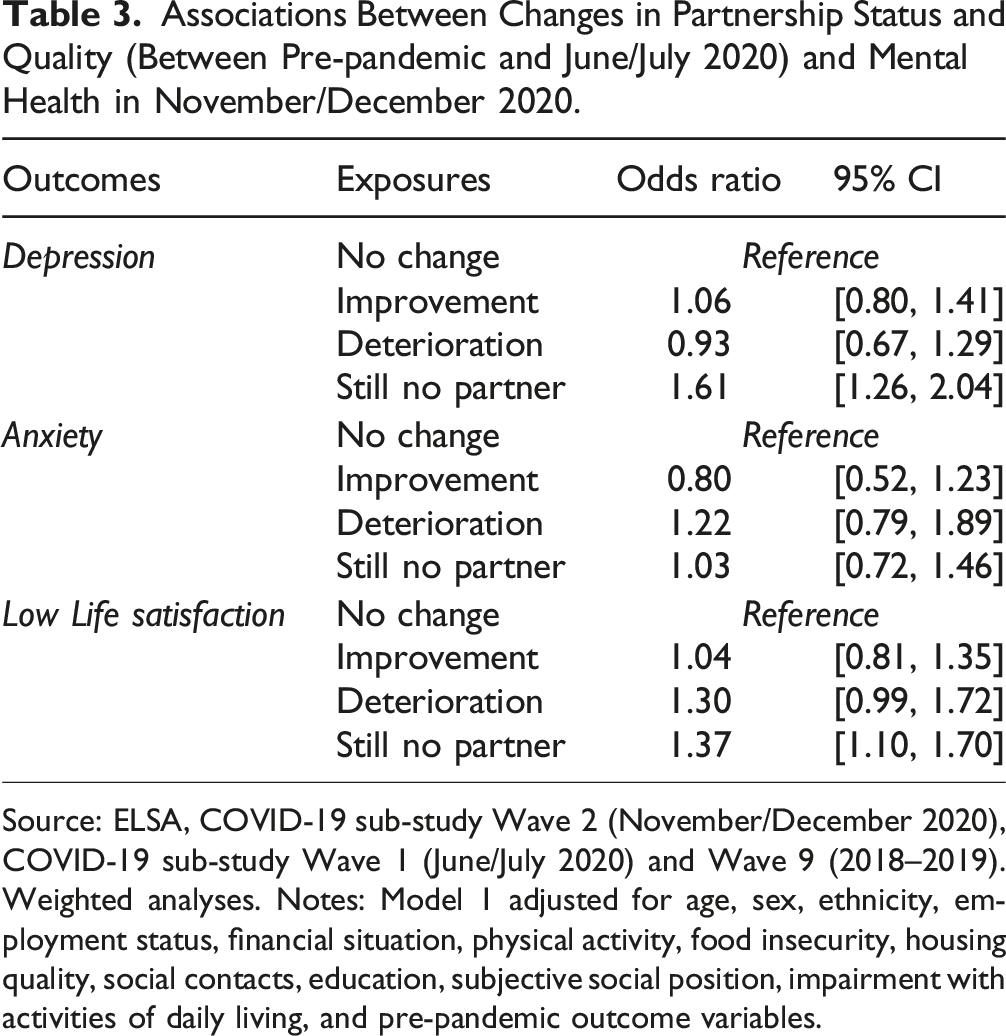
Source: ELSA, COVID-19 sub-study Wave 2 (November/December 2020), COVID-19 sub-study Wave 1 (June/July 2020) and Wave 9 (2018–2019). Weighted analyses. Notes: Model 1 adjusted for age, sex, ethnicity, employment status, financial situation, physical activity, food insecurity, housing quality, social contacts, education, subjective social position, impairment with activities of daily living, and pre-pandemic outcome variables.
Discussion
During the pandemic, shortly after the UK Government announced the first lockdown on 23 March 2020, stay-at-home orders were issued, particularly advising older individuals to remain indoors and limit their interactions with others. Policies restricting social contact and human interaction have posed risks to mental health and well-being. However, few studies have so far investigated the mental health of older couples and whether and to what extent the quality of their relationship with a cohabiting partner influenced mental health during the initial months of the pandemic. Using data from England, our study showed that not having a co-residential partner was associated with poorer mental health during the pandemic, consistent with other studies that have examined mental health in relation to marital status and/or living arrangements both before and during the pandemic (McElroy et al., 2023). However, we also found that among those co-residing with their partner, not everyone experienced similar levels of mental health, with older individuals reporting poor partnership quality being more likely to report worse mental health compared to those with a more supportive partner. Our results align with findings from previous cross-sectional studies (Ahmad et al., 2020; Nkire et al., 2021; Pieh et al., 2020; Robb et al., 2020; Sachser et al., 2021) conducted during the pandemic, which identified an association between poor relationship quality and high depressive symptoms. Our study, employing a longitudinal approach and controlling for pre-pandemic mental health levels, suggests that poor-quality relationships during the pandemic might have exacerbated mental health issues, consistent with prior longitudinal studies (Teo et al., 2013). Overall, our findings support the marital discord model, which posits that poor relationship functioning may lead to increased acute and chronic stress and diminished availability of social support (Hollist et al., 2007), consequently resulting in poorer mental health outcomes (Davila et al., 2003; Whisman & Uebelacker, 2009). However, we did not identify strong associations between changes in relationship quality and mental health, except for low life satisfaction being more prevalent among those whose partnership quality declined between the pre-pandemic and early pandemic periods. This could partly be explained by the fact that relationship quality was relatively stable in our sample, as most respondents reported very similar levels of relationship quality throughout the period considered in our study. This is consistent with other studies suggesting that relationship satisfaction and quality do not change abruptly and tend to plateau, particularly in late adulthood (Bühler et al., 2021).
This study draws strength from using longitudinal data from the nationally representative ELSA. To our knowledge, it is the first study to consider how relationship quality among older couples has contributed to mental health and well-being during the first year of the COVID-19 pandemic. Our analysis supports the idea that although living with a partner is protective for mental health, not all couples fared equally. Those in less supportive and lower-quality relationships experienced greater levels of psychological distress and lower levels of life satisfaction compared to those with supportive and understanding partners. However, our contribution should be considered in light of several limitations. First, the questions regarding relationship quality lack a temporal framework, making it unclear whether respondents assess their relationship with their partner overall (over the years) or at a specific moment in time. Also, in this study, we focused solely on the quality of the relationship with the partner respondents live with, as ELSA did not inquire about the quality of relationships with partners residing in different households. While most of the ELSA respondents completed the questionnaire online, it is still possible that their answers could be biased due to social desirability or because their partners were present during their phone interviews or while completing the questionnaire. Moreover, the classification of respondents into the four categories of partnership quality is data-driven and based on a sum score of all items—future studies might want to consider the specific role that positive and negative feelings play. Furthermore, ELSA suffers from non-random cumulative attrition, an unavoidable problem in longitudinal studies that can only partially be corrected by using weights in the analysis. Because the quality of social relationships relates generally to mortality (Holt-Lunstad et al., 2010), we may have selected those with better relationship quality with their partners. Those in care homes are also excluded by the ELSA design. Finally, this study focused by design on older adults, so the results cannot be generalized to younger age groups.
This study elucidates that it was not only older people living without a partner who showed vulnerability to mental health issues during the pandemic but also those living with a partner but in a poor-quality relationship. Currently, the allocation of services and delivery of interventions (such as telephone helplines, social support groups, and social activities) aimed at improving mental health or well-being among older people living in the community are primarily targeted at those socially isolated and living alone (Biering, 2019; Davidow et al., 2021; Markowitz & Weissman, 2012). Our findings highlight that services and interventions to increase mental health in later life should also target partnered older people, particularly those in poorer quality relationships, both during and beyond national crises.
Footnotes
Acknowledgments
Research reported in this publication was supported by the National Institute On Aging of the National Institutes of Health under Award Number R01AG017644. The content is solely the responsibility of the authors and does not necessarily represent the official views of the National Institutes of Health. ELSA is funded by the NIHR Policy Research Programme (HEI) 198_1074_03. The views expressed are those of the author(s) and not necessarily those of the NIHR or the Department of Health and Social Care.
Author Contributions
Concept and Design: ET and GDG; data analysis: ET; supervision of project: GDG; drafting of the manuscript: ET and GDG; critical revision of the manuscript: GDG and MS.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: The English Longitudinal Study of Ageing is funded by the National Institute on Aging (Ref: R01AG017644) and a consortium of UK government departments: Department for Health and Social Care; Department for Transport; Department for Work and Pensions, which is coordinated by the National Institute for Health Research (NIHR, Ref: 198-1074). Funding has also been provided by the Economic and Social Research Council (ESRC). The ELSA COVID-19 sub-study was funded by the UK Research and Innovation ESRC COVID-19 Rapid Response Initiative (ES/V003941/1).
Ethical Statement
Data Availability Statement
All data can be accessed through the UK Data Service (SN 8688 and 5050).
