Abstract
Background
Mental health and substance use disorders typically onset during youth and commonly co-occur. Integrated treatment of two or more co-existing mental health and substance use disorders (i.e., concurrent disorders) is increasingly prevalent in real-world clinical settings. However, the depth of the evidence base on best practices remains unclear.
Objectives
This scoping review aimed to identify, map and summarize peer-reviewed studies of interventions for concurrent disorders in youth.
Methods
Six electronic health databases were systematically searched, in addition to a hand search of the reference lists of relevant systematic reviews. Only peer-reviewed studies of interventions treating concurrent disorders (i.e., simultaneous treatment of two or more disorders) in youth (10–29 years old) were eligible. Two independent reviewers conducted screening and data extraction. Results were charted according to studies employing pharmacological and non-pharmacological interventions.
Results
Thirty peer-reviewed studies were included, 19 (63.3%) were randomized controlled trials (RCTs). Most studies enrolled participants with an unspecified substance use disorder (n=17, 56.7%), while alcohol use was the primary substance use disorder in seven (23.3%) studies, followed by cannabis use disorder in six (20.0%) studies. Mood disorders (e.g., depression, dysthymia) were the most common concurrent mental health disorders comprising 15 (50%) studies, followed by nine (30.0%) studies of behavioural disorders (e.g., ADHD) and five (16.7%) studies of unspecified psychiatric disorders. Eighteen (60.0%) studies (n=1,699 participants) investigated the effectiveness of various non-pharmacological interventions, while 12 (40.0%) studies examined pharmacotherapies (n=765 participants).
Conclusion
Although several RCTs were identified, substantial clinical and methodological heterogeneity was evident among the studies (e.g., patients with multiple disorders, and multi-faceted interventions). Smaller systematic reviews focused on specific interventions (e.g., behavioural therapies) and concurrent disorders (e.g., depression and substance use) may be warranted. Due to considerable heterogeneity, more RCTs are needed before conducting larger systematic reviews or meta-analyses.
Plain Language Summary Title
Evidence-based interventions for youth with concurrent mental health and substance use disorders: A scoping review
Plain Language Summary
Why was the study done?
This study aimed to explore the treatment of concurrent mental health and substance use disorders in youth, as these conditions often occur together and are difficult for clinicians to treat. Best practices remain unclear.
What did the researchers do?
The researchers conducted a scoping review, systematically searching six electronic health databases for peer-reviewed studies focused on interventions for youth (ages 10-29) dealing with both mental health and substance use disorders. They screened and extracted data independently from eligible studies.
What did the researchers find?
The review included 30 studies, and 63.3% were randomized controlled trials (RCTs). A majority (56.7%) of the studies included participants with unspecified substance use disorders. The most common specified substance use disorders were alcohol (23.3%), and cannabis (20.0%). Mood disorders were prevalent in 50.0% of the studies, followed by behavioural disorders (30.0%) and unspecified psychiatric issues (16.7%). Non-pharmacological interventions were investigated in 60.0% of the studies, and pharmacological interventions were examined in 40.0%.
What do the findings mean?
The review found several studies, but they varied significantly in participant population and study design, highlighting a need for more RCTs for youth with concurrent disorders. Additional research will help establish clearer clinical practice guidelines and inform future systematic reviews and meta-analyses.
Introduction
Addressing the rising prevalence of mental health disorders and substance use disorders (SUDs) in youth is an urgent global health priority.1,2 Since the onset of the COVID-19 pandemic, the prevalence rates of these conditions have increased, impacting youth disproportionately, globally. 3 As a result, there is a need for research and policy focus to better support mental health in this age group. Mental health disorders and SUDs often co-exist and function in tandem, complicating both research and intervention strategies. 4 Herein known as “concurrent disorders,” having a diagnosis of a mental health disorder and SUD simultaneously is associated with a myriad of poorer health outcomes compared to having either condition alone. These may include increased mental health or substance use symptom severity (e.g., depression symptoms, more frequent substance use), elevated risk of substance-related overdose or poisoning, and increased risk of chronic physical health conditions such as diabetes or HIV. The presence of one or more concurrent disorders may compound deficits in executive function, which can impair decision-making processes that serve to regulate engagement in high-risk behaviours such as solitary or poly-substance use, unhealthy dietary habits, and unsafe sexual practices. 5
The onset of mental health symptoms typically begin in childhood or adolescence, while substance use and SUDs more commonly initiates later in adolescence or emerging adulthood. 6 Authors of a previous review suggested that over half of adults with SUDs are diagnosed with three or more comorbid mental health disorders. 7 Similarly, authors of a study found that 63% of 1167 adolescents enrolled in a community-based addiction treatment program in the United States met the diagnostic criteria for an additional mental health disorder. 8 Evidence also suggests disruptive behavioural/impulse-control disorders, mood and anxiety disorders, eating disorders, and personality disorders are the most commonly comorbid psychiatric disorders among youth and young adults with SUDs. 9
The period of rapid brain development during adolescence and young adulthood represents a particularly vulnerable developmental stage for the onset of mental health disorders and SUDs. 10 For instance, multiple childhood-onset mental health disorders, including depression, anxiety, and disruptive behaviour disorders have been shown to increase the risk of adolescent-onset SUD. 11 Early onset mental health disorders in youth are associated with earlier onset of substance use, increased risk of future opioid use disorders in young people, 12 increased utilization of SUD treatment resources and generally poorer SUD treatment response. 13 Conversely, problematic substance use during adolescence may worsen preexisting mental disorders or increase the risk of developing new mental health disorders. For example, regular cannabis use during adolescence has been shown to dramatically increase the risk of developing psychotic symptoms, depressive symptoms, anxiety symptoms and functional impairment in a dose-dependent manner. 14 The high prevalence of concurrent disorders may be further explained by shared genetic and environmental risk factors and common brain regions and neural circuits implicated in both disorders. 15
Clinical experts suggest that standard care for youth with SUD is often insufficient and may not adequately address underlying comorbidities and psychosocial issues, which may limit recovery potential and increase the risk of relapse. 15 However, treatment for concurrent disorders in youth is notoriously challenging due to the complicated interplay between multiple disorders, causing a further burden on individual patients, families and healthcare systems. 16 Moreover, the treatments that exist for these conditions in youth are poorly accessible due to costs, geographic location (e.g., urban/rural disparities) or are developmentally inappropriate (e.g., adult psychiatry services for young adults 18–25 years). 17 Insufficient or untimely intervention consequently increases the risk of poor outcomes such as academic underachievement, incarceration, unemployment, homelessness and long-term health complications such as cardiovascular disease, substance-related overdose and early death. 13
Treatment of concurrent disorders has traditionally involved treating the mental health and substance use conditions separately, which often results mixed outcomes. 17 As evidenced by previous systematic reviews and guidelines, integrated treatment (i.e., simultaneous) of concurrent disorders may promote enhanced health outcomes for adults with these conditions.18,19 Although there is growing empirical support for integrated treatments for concurrent disorders in adults, the evidence base for youth is still emerging. Youth may benefit the most from early intervention and treatment, and evidence-based interventions are urgently needed. 19 As a result, we believe that a scoping review is necessary to map the available evidence and guide the development of future studies required to inform clinical practice and health policy, which aligns with recommendations from the World Health Organization (WHO) for the early identification and treatment of mental health disorders. 20 The objective of this scoping review was to identify, map and summarize peer-reviewed studies of interventions for concurrent disorders in youth aged 10–29 years. Additionally, this study aimed to provide an overview of the existing knowledge on this topic, and identify gaps and limitations in the literature.
Methods
Study Design
A scoping review was conducted. For this study, we used an iterative team-based approach to guide the methodological framework based on steps suggested by Arksey & O’Malley, 21 Levac et al. 22 and Daudt et al. 23 The reporting of the results was guided by the Preferred Reporting Items for Systematic Reviews and Meta-Analyses extension for Scoping Reviews (PRISMA-ScR) Checklists. 24 The protocol for this scoping review was registered a priori on Open Science Framework (https://osf.io/ck8eu/).
Identifying the Research Question
Scoping reviews typically map a wide range of available evidence based on research questions that are more broad than typically found in a systematic review.21–23 Research questions from scoping reviews intend to provide a general understanding of the current state of the literature on a particular scientific topic rather than meta-analyzing the data from the included studies. 23 A panel of expert adolescent and young adult psychiatrists with real-world experience treating youth with concurrent disorders helped frame the research questions. The research questions for this scoping review were: “What peer-reviewed interventions exist for youth with concurrent disorders, and what is the summary of their findings?”
Data Sources
Prior to conducting the review, PubMed and The International Prospective Register of Systematic Reviews (PROSPERO) were searched for systematic reviews related to concurrent disorders in youth to avoid duplicating any pre-existing work. The following six health databases were systematically searched from 1980 until 8 February 2024: (i) MEDLINE, (ii) PsycINFO, (iii) EMBASE, (iv) Cochrane Database of Systematic Reviews, (v) Cochrane Central Register of Controlled Trials (CENTRAL) and (vi) Scopus.
Search Strategy
A librarian (MK) experienced with systematic searching for scoping reviews conducted searches in the following bibliographic databases from inception to 25 October 2021: Medline, EMBASE, PsycINFO via OVID; Cumulative Index to Nursing and Allied Health Literature (CINAHL) via EBSCOhost; Scopus; and Cochrane Library via Wiley. The search comprised natural language keywords and subject headings, such as MeSH. The comprehensive search strategy was derived from four main concepts: (1) SUDs including both drugs and alcohol; (2) mental health disorders; (3) concurrent or dual diagnosis; (4) adolescents or youth. Non-peer-reviewed publication types, such as editorials and letters, were removed from the results. No language limits were used during the search to increase sensitivity despite “published in English” being a requirement in the eligibility criteria below. See Appendix 1 for the complete search strategies.
Two search updates were completed in December 2022 and February 2024. The search strategy used for each update did not deviate from the original. Results were exported in complete batches and the synthesis review management software, Covidence was used to remove duplicate records (Covidence systematic review software, Veritas Health Innovation, Melbourne, Australia. Available at www.covidence.org). After the database searches were complete, the reference lists of relevant systematic reviews25,26 were searched to ensure the accuracy of the database searches and reduce the risk of missing potentially relevant articles.
Study Selection Process
The Population Intervention Comparator Outcomes Study-type (PICOS) model 27 was used to guide the development of the eligibility criteria.
Eligibility Criteria
Population
Studies of participants with a mean age between 15 and 24 were included based on the United Nations definition of youth. 28 If the participant age was reported as a range rather than a mean, studies with participants beyond 10 to 29 were excluded.
To be included, a study was required to report that all study participants had symptoms of at least one mental health disorder and one substance use disorder. This could be determined by diagnosis via established diagnostic criteria such as Diagnostic and Statistical Manual third edition (DSM-III), newer editions, the International Classification of Disease (ICD-7), or newer editions, a positive screen for a mental health and substance use disorder using a validated instrument (e.g., PHQ-9) or enrolment into an inpatient psychiatric hospital (equates to a mental health diagnosis) or residential addiction treatment facility (equates to a substance use disorder diagnosis).
Intervention
Any intervention targeting concurrent disorders in youth (as defined above) was eligible for inclusion, such as pharmacotherapy, psychotherapy, family-based interventions or combined approaches. All clinical settings (e.g., inpatient, outpatient, virtual) were eligible for inclusion.
Control
Studies with or without a control group were eligible for inclusion. For controlled studies, all types of control groups were eligible.
Outcomes
For eligibility, studies must have reported at least one clinically relevant patient health outcome (e.g., substance use, mental health, quality of life, education attainment, functional status). Studies of interventions that only aimed to promote healthcare provider outcomes (e.g., physician knowledge) were excluded.
Study Type
Only peer-reviewed primary research studies were eligible for inclusion. Conference proceedings/abstracts, posters, theses/dissertations, grey literature, systematic reviews, dissertations, protocols and studies without a full-text PDF were excluded.
Screening
Each article was initially screened by title and abstract; those abstracts deemed relevant were then reviewed by full-text pdf. Two independent reviewers were given the same a priori eligibility criteria to screen articles. A third reviewer (TM), who has previous experience with systematic reviews, resolved disagreements by discussion when necessary. Covidence software was utilized to facilitate the screening and extraction (Covidence systematic review software, Veritas Health Innovation, Melbourne, Australia. Available at www.covidence.org). To pilot the screening process, 10% of the identified studies were initially reviewed to ensure accuracy. For abstract screening, studies with “yes” and “maybe” votes were sent to full text for assessment, while studies with “yes” and “no” votes were reviewed by a third reviewer (TM). A similar process was used for full-text screening, with the added requirement of listing a reason for exclusion if the text garnered a “no” vote (see list of exclusions in the PRISMA diagram).
Data Extraction
Two reviewers developed the extraction sheet by randomly selecting two included studies to extract independently; then, a consensus meeting was held to confirm the extraction sheet before extracting the remaining articles. The reviewers extracted on two separate extraction sheets and then met and collated their responses on a third extraction sheet. A third reviewer (AEL) reviewed the final extraction sheet. Author (TM) was designated as the arbitrator for any disagreements that could not be resolved by discussion between the reviewers.
Collating, Summarizing, and Reporting the Results
Upon completion of data extraction, data most relevant to the objectives of our review were reported narratively. The data obtained from the included studies was charted in summary tables derived from our data extraction sheet. The data synthesis was reported narratively/qualitatively according to (i) study type, (ii) intervention type, (iii) patient population and (iv) clinically relevant outcomes. Studies were categorized into two groups based on whether the objective was to evaluate a pharmacological or non-pharmacological intervention. A meta-analysis was not conducted as this approach was outside the scope of our review. Our narrative reporting approach was adopted in anticipation of substantial heterogeneity among the included studies. Due to inconsistent reporting of participants’ age groups, a subgroup analysis comparing adolescents (10–17 years) and emerging adults (18–29 years) was not conducted.
Risk of Bias Assessment
The included studies were not critically appraised because the objective of our scoping review was to map the literature, not draw firm conclusions about safety or effectiveness, aligning with the latest scoping review reporting guidelines. 24
Stakeholder Engagement
Throughout the study, including during the research question setting process, study design and interpretation of results, clinicians with expertise in treating youth with complex mental health and substance use conditions were engaged to identify real-world challenges in treating this population. Prior, qualitative interviews were conducted (TM, AAA) as part of a study with emerging adults 18–25 with anxiety, depression and substance use in mental health settings in Alberta. Clinicians and clients suggested individuals may have complex and unique needs, and a variety of services and interventions may be available, which often leads to difficulty navigating the mental health system such as finding timely and age appropriate services. The results will be shared with youth mental health practitioners, and policymakers to inform youth mental and addiction service delivery. The results and manuscript will be presented at relevant academic conferences, presented to policymakers, and will inform future research (e.g., clinical trials and systematic reviews).
Deviations From Registered Protocol
One protocol deviation occurred as the authors decided to only include studies where all study participants of a potential eligible study were reported to have at least one mental health disorder and at least one substance use disorder. The original protocol included studies of participants with a mental health disorder, and at least 50% of the study population had substance use disorders, this however posed feasibility concerns.
Results
After identifying an initial n = 3,557 unique records, 30 studies were included, comprising 2,464 youth participants (Figure 1).
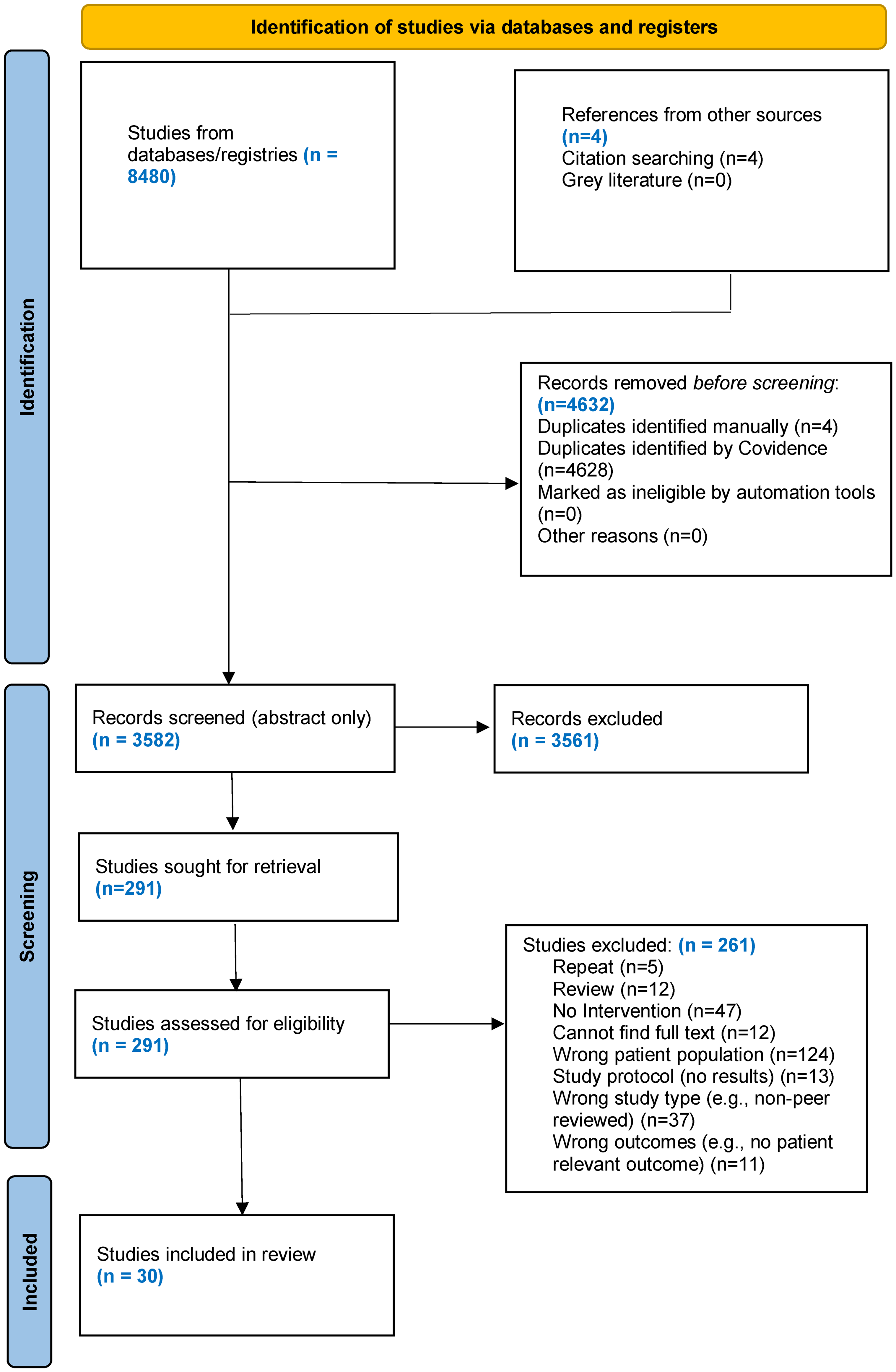
PRISMA flow diagram of the search process.
Characteristics of Included Studies
Table 1 displays the characteristics of the included studies. Most studies (n = 24, 80%) were conducted in the United States, while three (10%) were conducted in Australia, and one study (3.33%) was conducted in New Zealand and Italy, respectively. The most common study designs employed were randomized controlled trials (RCTs) (n = 19%), and the remaining 12 studies (40%) were observational designs, three (10%) of which were case studies. All studies identified were published in English. Males comprised 62.1% of the study sample (n = 1,530). Eighteen (60%) studies were sampled from outpatient addiction or mental health clinics, while seven (23.3%) were conducted in a psychiatric hospital, three (10%) in residential addiction treatment centers, one (3.33%) from acute care, one (3.33%) from social services, and one study (3.33%) recruited partcipants from both inpatient and outpatient settings. Affective disorders (anxiety, depression, dysthymia) were included as concurrent mental health diagnoses in 11 (36.7%) studies. Five (16.7%) studies reported participants having non-psychotic mental health disorders, while four (13.3%) reported various mental health disorders (e.g., psychiatric inpatients). Most studies (n = 17, 56.7%) enrolled participants with an unspecified SUD (i.e., participants may use a variety of substances), while alcohol was the primary drug of research in seven studies (23.3%), cannabis in six studies (20%), tobacco smoking in two studies (6.67%). Fourteen (46.7%) studies used interventions that targeted mental health disorders primarily, eight (26.6%) studies employed interventions focused on addressing SUD, and nine (30%) targeted both mental health and substance use simultaneously. Finally, reported participants’ ages ranged from 12 to 25 years; however, (n = 8) studies did not report an age range, only a mean age.
Characteristics of Included Studies.

Summary of Main Findings
Non-Pharmacological Therapies
Table 2 displays the summary of findings from the non-pharmacological studies. Eighteen (60%) studies (n = 1,699 participants) employed various non-pharmacological interventions targeting concurrent disorders. The included articles investigated interventions such as cognitive-behavioural therapy, motivational interviewing, motivational enhancement therapy (MET) and family therapy. Hides et al. 46 reported integrated cognitive-behavioural therapy to be an effective treatment for comorbid depression and SUDs in youth; however, no control group was implemented. Cornelius et al. 36 investigated the combination of MET and CBT in adolescents with comorbid alcohol use disorder and major depressive disorder compared to no MET and CBT. They reported significant improvement in depression and alcohol-related outcomes. Motivational interviewing compared to brief advice for psychiatric inpatients with tobacco addiction was assessed in the studies conducted by Brown et al.31,32 While the impact on smoking outcomes was inconclusive, patients showed improved smoking cessation-related self-efficacy after six months.
Summary of Findings (Non-Pharmacological Interventions).
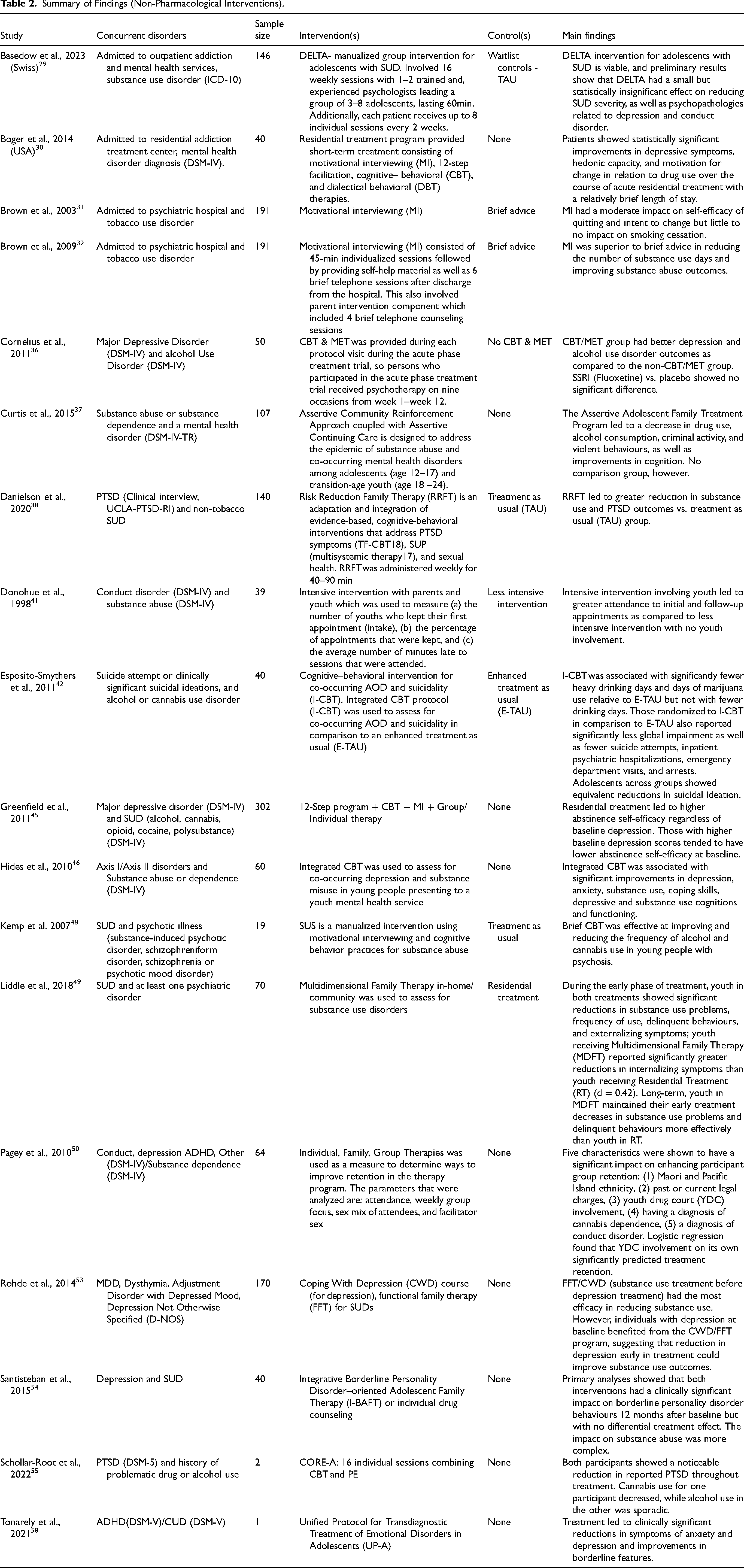
Family therapy may decrease substance use and mental health symptoms. Danielson et al. 38 compared risk reduction family therapy (RRFT) to treatment-as-usual in youth with comorbid PTSD and non-tobacco substance use; they reported greater reductions in both PTSD and substance use in the RRFT group. Liddle et al. 49 investigated multidimensional family therapy as an alternative to residential treatment for youth with concurrent substance use and mental health disorders. Participants reported reduced depression and anxiety symptoms after treatment. Furthermore, Boger et al. 30 and Greenfield et al. 45 demonstrated that a 12-step program consisting of motivational interviewing and CBT resulted in improvements in scores associated with substance use disorder; however, no control groups were used (Table 2).30,45 Studies looking at the effectiveness of integrated CBT concluded that it was effective in improving depression, anxiety and substance use compared to no CBT as well as reducing the number of heavy drinking days, days of marijuana use, suicide ideation and suicide attempts compared to enhanced treatment as usual.42,46 Finally, other treatments that utilized Individual, Family, Group Therapies, 50 Intensive intervention with parents and youth 41 and Assertive Community Reinforcement Approach coupled with Assertive Continuing Care 37 all reported positive outcomes for youth in relation to SUD; however, among these, only Donohue et al. 41 implemented a control group comparing Intensive intervention with parents and youth to a less intensive intervention.
Pharmacotherapies
Table 3 displays the summary of findings from the pharmacological studies. Twelve (40%) studies (n = 765 participants) were included. The two RCTs43,47 investigated the impact of the antidepressant fluoxetine on depression symptoms in adolescents with SUD and major depressive disorder. The study conducted by Findling et al. 43 reported no significant difference between the fluoxetine and the placebo groups, while the study conducted by Hirschtritt et al. 47 reported greater improvements in depression symptoms in the fluoxetine group compared to placebo.
Summary of Main Findings (Pharmacotherapies).
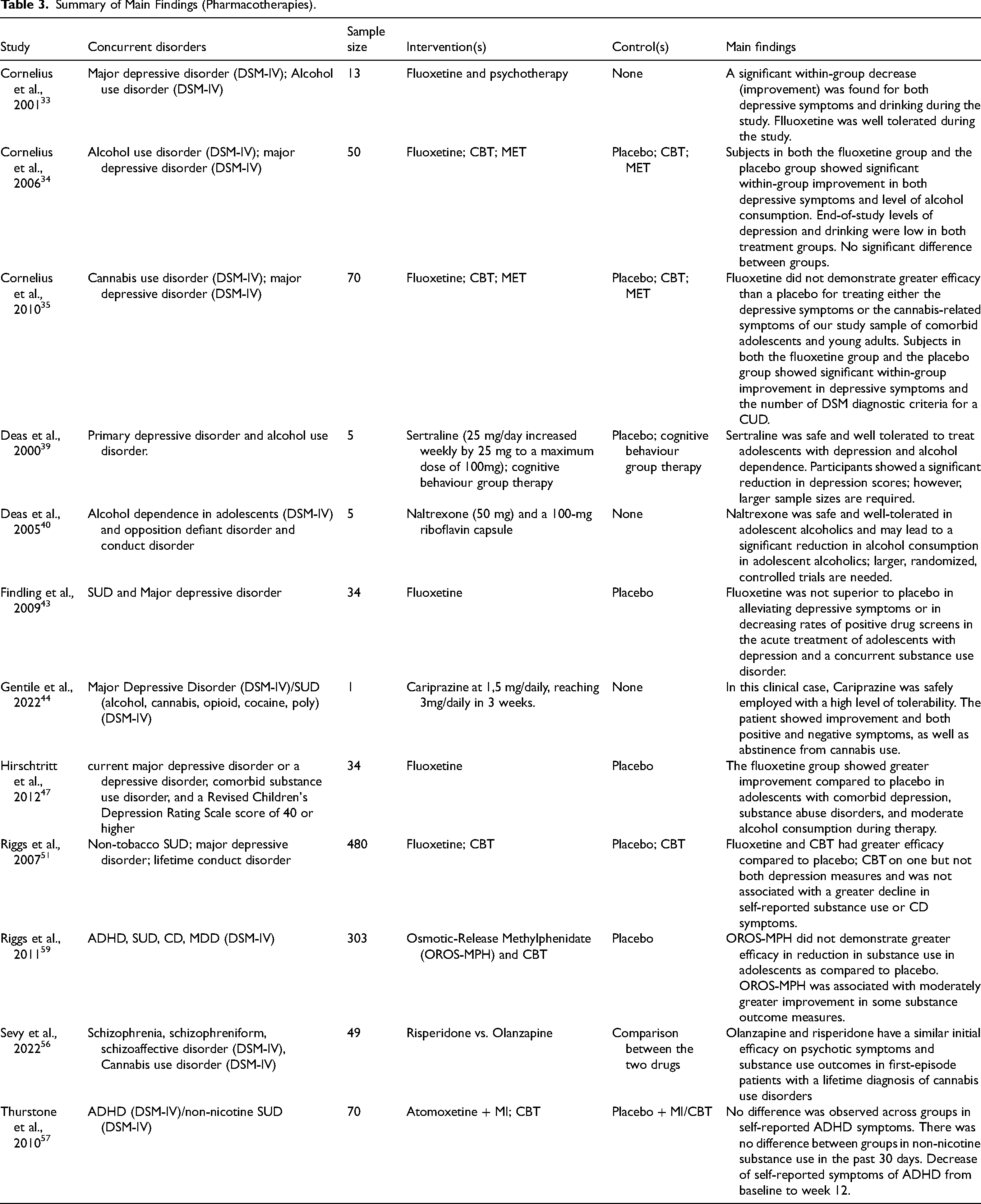
Deas et al. 40 investigated the effect of naltrexone and riboflavin for treatment-seeking adolescents with alcohol use disorder and a comorbid mental health condition. The findings supported the safety and efficacy of this intervention for reducing alcohol consumption, but no control group was utilized and the authors emphasized the need for larger studies. Finally, Sevy et al. 56 compared the effectiveness of the antipsychotic drugs risperidone and olanzapine for adolescents with alcohol use disorder and a concurrent psychotic disorder. The study outcomes revealed no significant difference between the two interventions but noted positive symptom improvements in both groups.
Seven studies utilized a combined intervention approach utilizing various pharmacotherapies combined with non-pharmacotherapy interventions.33,34,35,39,51,52,57 Six administered fluoxetine as part of their intervention,33–35,43,47 one administered atomoxetine (selective norepinephrine reuptake inhibitor), 57 and one administered methylphenidate (psychostimulant). 51 In addition to the pharmacotherapies, five used cognitive behavioural therapy,34,35,51,52,57 two used MET,34,35 and one used “psychotherapy.” 35 One study used a single-arm open-label design. 34 The studies investigated varying concurrent disorders. For substance use disorders, non-tobacco SUD was explored in three studies,51,52,57 alcohol use disorder in two studies33,34 and cannabis use disorder in one study. 35 Concurrent mental health disorders included major depressive disorder in six studies,33,34,43,51,52 ADHD in two studies52,57 and conduct disorder in two studies.51,52
Fluoxetine was well tolerated in each study; however, it did not show greater efficacy on primary outcomes compared to placebo for SUD or major depressive disorder. Initial results from Cornelius et al. 34 reported that fluoxetine plus psychotherapy was beneficial among youth with comorbid major depressive disorder and alcohol use disorder; however, these results were not replicated in a larger RCT. 35 Additionally, cognitive behavioural therapy and MET were performed in the control group, resulting in a treatment effect which would preclude observing an additive effect from both treatments compared placebo alone. Cornelius et al. 35 replicated this trial in a larger cohort of youth with comorbid cannabis use disorder and major depressive disorder and reported similar results—no significant difference compared to the control group; however, beneficial within-group treatment effects were reported in both groups.
Riggs et al. 51 reported that fluoxetine and cognitive behavioural therapy significantly improved scores on the Childhood Depression Rating Scale-Revised compared to placebo, but not on the Clinical Global Impression Improvement questionnaire. CBT may have contributed to the higher-than-expected treatment response and mixed efficacy outcomes. Riggs et al. 52 concluded that methylphenidate did not indicate superior efficacy in reducing substance use when compared to a placebo in adolescents concurrently undergoing individual CBT for substance use and ADHD. However, methylphenidate was associated with clinical improvement in secondary substance-related and ADHD outcomes. Thurstone et al. 57 reported no difference across groups in both self-reported ADHD symptoms and the use of non-nicotine substances in patients receiving atomoxetine combined with motivational interviewing compared to placebo; however, there was a decrease in the number of symptoms of ADHD reported by the patient between baseline and week 12.
Discussion
To our knowledge, this was the first scoping review to identify and summarize peer-reviewed studies of interventions for youth with concurrent disorders. To date, few studies have evaluated treatment approaches that aim to treat concurrent disorders simultaneously. Our findings revealed that a modest but limited number of studies have been conducted in this field, but significant heterogeneity was observed among the interventions, populations, and study types examined. However, some key themes and patterns were identified across the body of literature. For example, we found that depression was the most prominent concurrent mental health disorder studied, while alcohol and cannabis use disorders were the most commonly investigated concurrent substance use disorders. Non-pharmacological interventions, specifically CBT, were the most common interventions employed in youth with concurrent disorders. Motivational interviewing, CBT, family-based interventions and other integrated approaches were also employed. The results of the included studies appeared to suggest each of these interventions may help allieviate mental health symptoms, substance use outcomes and patient-reported outcomes such as self-efficacy and functional status. However, the specific outcomes and effectiveness may vary depending on the target population and the nature of the mental health condition or substance use disorder being addressed.
The included research studies investigating pharmacological interventions for youth with concurrent disorders found mainly positive outcomes. Three of the four pharmacological studies investigated therapies in adolescents with SUD and concurrent depression; thus, more research should be conducted to investigate the effect of these pharmacotherapies on other mental health conditions. It should be noted that the number of studies was small, and only two were RCTs. Of the RCTs, only one study reported a beneficial effect of the treatment. Furthermore, there are numerous ethical and logistical challenges when conducting RCTs on vulnerable populations such as youth with concurrent disorders. For instance, upholding patient autonomy during the informed consent process is an ethical concern when researching treatments for adolescents with SUDs. 60 SUDs are associated with intoxication and withdrawal phases that can adversely affect cognitive processes, including decision-making, attention, and perception. 61 The additive effect of mental health disorders (e.g., depression, ADHD) further increases questions about whether adolescents have the cognitive capacity to participate in research without parental consent 60 ; however, requiring parental consent for intervention inclusion may also lead to systemic biases that exclude individuals who may not be able to obtain parental consent or have a conflicting view of the interventional risks than their caregivers. 62 Finally, the period of adolescence is broadly defined and can range anywhere from 12 to 25 years old, which further complicates treatment approaches and the use of pharmacological interventions.
Several studies highlighted the importance of personalized treatment and the implementation of combination therapies to improve treatment outcomes.31,45,48,54 Greenfield et al. 45 concluded that a combination of a 12-step program, CBT, MI and individual/group therapy was effective in improving self-efficacy and sustaining recovery in emering adults with SUD and concurrent major depressive disorder. Similarly, Kemp et al. 48 highlighted the success of a manualized intervention using motivational interviewing and CBT for SUDs in young people with psychotic disorders. These studies suggested potential benefits of non-pharmacological interventions for concurrent disorders. Utilizing only one type of behavioural therapy may benefit people with SUD; however, outcomes were mixed and dependent on treatment modality. For instance, Brown et al. 31 suggested that motivational interviewing displayed modest effects on smoking cessation outcomes; thus, enhancement of this treatment approach would be required for adolescents with psychiatric comorbidities. Conversely, Santisteban et al. 54 reported that individual substance use counseling (i.e., monotherapy) did not reduce substance use in adolescents with depression; however, reductions in substance use were observed with integrative borderline personality disorder-oriented adolescent family therapy (I-BAFT), which utilized an approach comprising weekly family therapy, individual therapy and skills-building interventions.
Our findings were largely consistent with previous reviews.25,26 A meta-analysis analyzing the impacts of outpatient treatment on adolescents with SUDs found any intervention to be superior to no intervention. 63 Another systematic review and meta-analysis reported that brief alcohol interventions were moderately effective for youth aged 11–18. 64 However, neither of these meta-analyses specifically investigated concurrent disorders in youth. Therefore, this scoping review adds to the current literature by highlighting the sparsity in concrete intervention strategies for youth with concurrent disorders. 59 The significant heterogeneity in approaches demands that more research be conducted to investigate effective treatment protocols for this vulnerable population. Previous studies have outlined a pressing need to identify mental health concerns early to improve both substance use concerns and health outcomes. 65 For instance, mood disorders have been associated with developing SUDs within 10 years following an initial diagnosis. 66 Thus, establishing more uniform non-pharmacological, pharmacological and combined therapy protocols is required to inform clinicians on the best treatment approaches for specific conditions and prevent the development of more chronic difficulties into adulthood. 66 Finally, a significant body of literature has reported strong associations between adverse childhood experiences and the development of mental health and SUDs into youth and adulthood. 67 Therefore, research investigating the history of adverse childhood experiences and trauma in youth with concurrent disorders may provide insight into the developmental timeline of both mental health disorders and SUDs to better inform intervention strategies.
Strengths and Limitations of the Review
This scoping review provided a comprehensive overview of the literature on treatments for concurrent disorders in youth and highlighted their complexities. We conducted a broad search of the peer-reviewed literature and used robust eligibility criteria, which reduced the risk of selection bias and promoted replicability.
A few unavoidable methodological limitations of this scoping review should also be considered when interpreting the results. First, the search strategy may not be exhaustive as grey literature was excluded. Second, studies published in languages other than English were excluded for feasibility reasons. To explore the impact of these decisions, we searched the reference lists of previous systematic reviews25,26 and found no evidence of any citations of relevant non-peer-reviewed studies or inclusion of studies published in languages other than English. We also did not conduct backward reference searching of included studies; however, this is a small limitation because we examined the previous systematic reviews.
The decision to only include studies of youth with a confirmed mental health disorder diagnosis may have excluded some potentially relevant studies of youth with mental health symptoms who did not meet diagnostic criteria or were not assessed for the disorder. To inform this decision, we consulted with clinical pediatric psychiatric experts, who suggested that children are not as likely to be diagnosed with a SUD at early ages; therefore, confirming the mental health diagnosis would be imperative for identifying studies with the correct target population. Including only studies with a diagnosis of a mental health disorder promotes replicability as it is an objective measure that is easy to identify during screening.
Conclusions and Clinical Implications
In light of our limitations, our scoping review provides an overview of the preliminary evidence for pharmacological and non-pharmacological interventions for treating youth with concurrent disorders. Historically, treatment guidelines for concurrent disorders recommended treatment of the predominant condition first rather than both disorders simultaneously. More recently, recommendations from the WHO have encouraged the integration of primary care and mental health services, acknowledging the common overlap of mental health, substance use and physical conditions. 28 Clinically, there are many nuances to the treatment of concurrent disorders. For example, people with a SUD and major depressive disorder may demonstrate a blunted treatment response to antidepressant therapy compared to those without a concurrent SUD. 68 Conversely, people in treatment for SUD with anxiety or depression tend to experience greater symptom severity, higher levels of disability and lower treatment retention rates than those without anxiety or depression. 7 Also, people with concurrent disorders risk acquiring serious long-term physical complications such as HIV, hepatitis C, cardiovascular disease and psychosocial issues such as unstable housing, unemployment, physical abuse or trauma and poor quality of life. 69 Without adequate training in concurrent disorder assessment and differential diagnosis, arriving at accurate case formulations and treatment plans can be difficult. 70 Further, treatment plans must be informed by the best available evidence. Unfortunately, based on our findings, there is limited clinical evidence from peer-reviewed studies to strongly inform the treatment approach for youth with concurrent disorders. Evidence-based medicine is predicated on balancing clinical judgment, patient preferences and the existing literature. The results from our review suggest a broad but heterogeneous evidence base to provide additional support for clinicians treating youth with concurrent disorders.
Future Directions
Further research and exploration of these interventions and their long-term effects are necessary to refine treatment approaches, identify optimal strategies for different populations and enhance overall patient outcomes in non-pharmacological treatments. Additional peer-reviewed studies and systematic reviews are needed to inform evidence-based clinical practice guidelines. Smaller systematic reviews focused on specific interventions (e.g., behavioural therapies) and concurrent disorders (e.g., depression and substance use) may be warranted, but due to considerable heterogeneity, more research is needed prior to conducting larger systematic reviews or meta-analyses. Since critical appraisal was outside of the scope of this review, any future systematic reviews should consider critically appraising the included studies. As the most common studies were of youth with depression who had either general SUD—more specifically, cannabis use disorder or alcohol use disorder (which are the most common SUDs in youth), it will be useful to see future systematic reviews on targeted areas, for example focusing on behavioural therapies (e.g., CBT specifically) versus treatment as usual or no treatment.
Continued research is necessary to identify the most appropriate medications and non-pharmacological interventions for specific populations whilst considering the mental health condition and SUD being addressed. Early screening, as well as the collaboration and coordination of services across sectors, continues to be essential for enhancing health outcomes in youth with concurrent disorders, as there is a significant degree of overlap in mental health and substance use concerns in youth. 65
Supplemental Material
sj-docx-1-cpa-10.1177_07067437241300957 - Supplemental material for Evidence-based Interventions for Youth With Concurrent Mental Health and Substance Use Disorders: A Scoping Review: Interventions fondées sur des données probantes pour les jeunes atteints de troubles concomitants de santé mentale et liés à l’usage de substances psychoactives : une étude de la portée
Supplemental material, sj-docx-1-cpa-10.1177_07067437241300957 for Evidence-based Interventions for Youth With Concurrent Mental Health and Substance Use Disorders: A Scoping Review: Interventions fondées sur des données probantes pour les jeunes atteints de troubles concomitants de santé mentale et liés à l’usage de substances psychoactives : une étude de la portée by Tyler Marshall, Matthew Reeson, Alexandra Loverock, Ariana E. Lewis, Ian King, Raffay Ilyas, Celine Caruso Dixon, Dylan Viste, Brandon Azer, Ethan Chow, Fahad Safi, Megan Kennedy, Adam Abba-Aji and Andrew J. Greenshaw in The Canadian Journal of Psychiatry
Supplemental Material
sj-docx-2-cpa-10.1177_07067437241300957 - Supplemental material for Evidence-based Interventions for Youth With Concurrent Mental Health and Substance Use Disorders: A Scoping Review: Interventions fondées sur des données probantes pour les jeunes atteints de troubles concomitants de santé mentale et liés à l’usage de substances psychoactives : une étude de la portée
Supplemental material, sj-docx-2-cpa-10.1177_07067437241300957 for Evidence-based Interventions for Youth With Concurrent Mental Health and Substance Use Disorders: A Scoping Review: Interventions fondées sur des données probantes pour les jeunes atteints de troubles concomitants de santé mentale et liés à l’usage de substances psychoactives : une étude de la portée by Tyler Marshall, Matthew Reeson, Alexandra Loverock, Ariana E. Lewis, Ian King, Raffay Ilyas, Celine Caruso Dixon, Dylan Viste, Brandon Azer, Ethan Chow, Fahad Safi, Megan Kennedy, Adam Abba-Aji and Andrew J. Greenshaw in The Canadian Journal of Psychiatry
Footnotes
Acknowledgments
Thank you to Dr. Johnathan Stea and Dr. Bina Nair for their contributions to the expert panel during the early stages of this study.
Author Contributions
Conception: TM, AA, AJG. Methods and design: TM, AA, AJG, AL. Project management: TM. Search strategy and database searches: MK. Screening: TM, MR, AL, FS, EC, CCD, BA, RI, AEL. Extraction: TM, MR, AL, FS, EC, CCD, BA, RI, AEL, AJG. Data analysis: TM, MR, BA, RI, DV. Data charting: TM, MR, AL, FS, DV, IK, RI, EC, AEL. Manuscript writing, first drafts: TM, IK, BA, AL, AEL. Manuscript writing, revisions: TM, MR. Approval of final manuscript: all authors.
Declaration of Conflicting Interests
The authors declared the following potential conflicts of interest with respect to the research, authorship, and/or publication of this article: TM conceived the study and conducted the study before beginning employment with the Government of Alberta. The Government of Alberta had no role in the design, conduct, analysis or reporting of the data in this study.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Supplemental Material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
