Abstract
Objective:
To examine variations between immigrants and nonimmigrants in 1) prevalence of common mental disorders and other mental health variables; 2) health service utilisation for emotional problems, mental disorders, and addictions, and 3) health service satisfaction.
Methods:
This article is based on a longitudinal cohort study conducted from May 2007 to the present: the Epidemiological Catchment Area Study of Montreal South-West (ZEPSOM). Participants were followed up at 4 time points (T1, n = 2433; T4, n = 1095). Core exposure variables include immigrant status (immigrant vs. nonimmigrant), duration of residence, and region of origin. Key outcome variables included mental health status, health service utilisation, and health service satisfaction. Data were analysed both cross-sectionally and longitudinally.
Results:
Immigrants had been in Canada for 20 years on average. Immigrants had significantly lower rates of high psychological distress (32.6% vs. 39.1%, P = 0.016), alcohol dependence (1.4% vs. 3.9%, P =0.010), depression (5.2% vs. 9.2%, P = 0.008), and various other mental disorders. They had significantly higher scores of mental well-being (48.9 vs. 47.1 score, P = 0.014) and satisfaction with social (34.0 vs. 33.4 score, P = 0.021) and personal relationships (16.7 vs. 15.6 score, P < 0.001). Immigrants had significantly lower rates of health service utilisation for emotional problems, mental disorders, and addictions and significantly higher rates of health service satisfaction at all time points. Asian and African immigrants had particularly low rates of utilisation and high rates of satisfaction.
Conclusions:
Immigrants had better overall mental health than nonimmigrants.
According to the latest census, approximately 20% of Canada’s population are immigrants. 1 This proportion is rising, and immigrant integration is a key government priority. 2 The recently published ‘Mental Health Strategy for Canada’ notes that immigrants ‘face significant barriers to their seeking or obtaining help…health organizations need to be attuned to differences…and take into account cultural diversity’.3(p60) As such, it is vitally important to document and analyse the nature and extent of any mental health variations experienced by immigrants.
In the study of immigrant health, immigrant life experience is often categorised into 3 stages: 1) premigration, 2) the migration journey, and 3) postmigration. 4 Economic immigrants to Canada—for example, those from Western Europe or the United States—may have an unproblematic immigration experience. However, immigrants from other regions may be exposed to chronic or acute stressors during these stages. In the premigratory stage, immigrants from certain regions may have been exposed to civil instability, poverty, natural disaster, or other adverse social conditions. 5,6 This is especially so for refugees, who may also experience a difficult migration journey. 7 In the postmigratory stage, immigrants (especially non-European ones) may face unemployment, underemployment, and racism. 8,9 This can even apply to skilled immigrants, especially when there is a discrepancy between aspiration and achievement. 10 –12
A large body of European research suggest that rates of psychosis are significantly elevated in immigrants from Africa and the Caribbean. 13 –15 A recent Ontario study indicated slightly higher rates of psychotic disorders in refugees and Caribbean immigrants but not in other immigrant populations. 16 The European research attributes this elevation to several factors, including a chronically negative postmigration experience for racialized immigrants.
The Healthy Migrant Effect
The above-described research indicates that immigrants frequently experience negative stressors that can affect their mental health. However, a large number of Canadian studies indicate that immigrants generally have better mental health than the native-born population: this is known as ‘the healthy migrant effect’. 17 For example, one large-scale study found that overall health (including mental health) was significantly better in immigrants than the Canadian-born. 18 Likewise, another study found that immigrants had significantly lower rates of depression and alcohol use than the Canadian-born, especially recent immigrants. 19 Numerous studies have confirmed this healthy migrant effect in Canada. 20 –24
This healthy immigrant effect has been attributed to various factors. First is the phenomenon of immigrant self-selection, meaning that people who successfully emigrate (especially economic migrants) are likely to be physically strong and mentally resilient, given the challenges and barriers to embarking on a successful immigration journey. 6 Second, New World countries such as Canada and Australia demand that potential immigrants undergo strict medical exams, with the unhealthy having their applications rejected. 18 Third, roughly 20% of immigrants to Canada leave within the first year of arrival; those remaining may be especially well adapted. 25
Some studies examining the healthy immigrant effect indicate that immigrant health declines over time to the same level as native-born people or even worse, due to the ongoing impact on some of the negative postmigratory factors previously described. 26 –28 Also, some studies in Canada have not found the presence of a healthy immigrant effect. These studies are more consistent with the European-based research on immigrant mental health previously discussed. 29,30
Health Care Utilisation and Service Satisfaction
Research from the United Kingdom and the United States consistently indicates that immigrants and minorities have lower rates of mental health service utilisation and also report a lower quality of care and higher dissatisfaction with mental health services. 31,32 This has led to numerous inquiries and commissions in those jurisdictions. 33
Some research in Canada indicates that immigrants underuse mental health services in comparison with the native-born population, but it is not clear whether this is due to dissatisfaction with services or other factors. 34,35 First, underutilisation could be due to decreased need associated with the healthy immigrant effect. 28 Second, factors such as cohesive families, religiosity, and social support within tight-knit ethnic communities could confer resilience. 9 All of these provide ‘informal’ mental health care, which many immigrants may find preferable to formal care. 36 Third, immigrants may have different ‘explanatory models’, where mental and emotional distress is not perceived as an illness but as an inevitable part of everyday life. 37
That said, some qualitative studies indicate that non-European immigrants to Canada are frequently dissatisfied with formal mental health services, perceiving these services to be overly impersonal and medication focused. 38,39 Similarly, other studies report a high stigma associated with mental illness, which might act as a deterrent to service utilisation. 35,40
In summary, the corpus of research on immigrant mental health is inconsistent. Some research indicates that immigrants have higher risk and rates of mental illness, while other research suggests a healthy migrant effect. Likewise, numerous studies indicate a lower rate of service utilisation among immigrants, but it is uncertain whether this is related to decreased need, dissatisfaction with services, or other sociocultural factors. Dissimilarities in the literature may be related to immigrant heterogeneity, with factors such as region of origin and duration of residence mediating immigrant mental health outcomes.
Better understanding these aspects of immigrant mental health is essential to achieving priority 4.2 of the ‘Mental Health Strategy for Canada’, which is to ‘improve mental health services and supports by and for immigrants’.3(p60) As such, the aim of this study is to compare and contrast variations between immigrants and nonimmigrants in 1) the prevalence of common mental disorders and other mental health variables; 2) health service utilisation for emotional problems, mental disorders, and addictions; and 3) health service satisfaction. Utilisation and satisfaction will be stratified by immigrant region of origin and duration of residence to assess their influence on core outcomes. This will allow for a nuanced analysis contributing much-needed knowledge to the Canadian literature.
Methods
Study Design and Sample
This study is based on data collected from the ongoing longitudinal cohort Epidemiological Catchment Area Study of Montreal South-West (ZEPSOM). Methods for the recruitment, interview, and measurement have been described elsewhere. 20,41 –43 In brief, a sample of 2433 participants aged 15 to 65 years were randomly recruited from southwest Montreal at baseline (May 2007 to November 2008) from a total population of 269,720 residents. Immigrants in this catchment area represent 17% of the population. 41 This cohort has been followed every 2 years. The present study includes T2 (n = 1823, retention rate 74.9%; July 2009 to November 2010), T3 (n = 1305, retention rate 71.6%; December 2011 to July 2013), and T4 (n = 1095, retention rate 83.9%; February 2014 to May 2015). These time points were chosen because many measures of interest were only introduced at T2.
T2 included 441 immigrants (mean age 42.2 years and 39.9% male) and 1379 nonimmigrants (mean age 45.1 years and 36.3% male). T3 included 282 immigrants and 1021 nonimmigrants. T4 included 227 immigrants and 866 nonimmigrants. Thus, the proportion of immigrants for each cohort was between 21% and 25%, higher than the national average and the neighbourhood average. 1,41 In this catchment area, there are various health care services, including a psychiatric hospital and 2 health and social service centres. 44 The protocol was approved by the Douglas Hospital Research Ethics Committee, and all participants gave informed consent. Participants had the choice to conduct the surveys in either English or French.
Measurements
Basic characteristics, including age, gender, immigration status, years of residence in Canada, marital status, household income, and level of highest education, were collected using the Canadian Community Health Survey questionnaire (CCHS 1.2). 45 For this study, there are 3 core exposure variables. The first is a binary variable indicating if the participant was an immigrant or Canadian-born. The second is a categorical variable labelling immigrants by their duration of residence. This variable had 5 categories: nonimmigrants (serving as reference group in the regression analysis), 1 to 5 years of residence, 6 to 10 years of residence, 11 to 15 years of residence, and 16 or more years. The third variable was a categorical variable indicating region of birth with 6 categories: Canada (served as reference group in regression analysis), Asia, Europe, Africa, Latin America/Caribbean, and other (including nations such as the United States and Australia).
Twelve variables were chosen to measure various aspects of mental health and illness. Mood disorders (depression and mania) and anxiety disorders (panic attacks, social phobia, and agoraphobia), alcohol dependence, and mental health problems were identified using the version of the Composite International Diagnostic Interview (CIDI) employed in the CCHS 1.2, which is a Canadian adaptation 45 of the World Mental Health Survey Initiative. 46 Psychological distress was measured using the K-10 scale. 47 This scale consists of ten 5-point Likert-type units asking participants to estimate the frequency of symptoms of psychological distress experienced during the past month. A cutoff point of 9 was used for identifying subjects with high psychological distress. We also used the Satisfaction Life Domains Scale. 48,49 This 20-item scale has 5 dimensions 1) daily life and social relations, 2) housing-neighbourhood, 3) personal relationships, 4) spare-time activities, and 5) autonomy. Finally, we used the Mental Health Continuum–Short Form (MHC-SF). 50 This consists of 14 items that measure emotional, social, and psychological aspects of well-being and positive mental health.
To measure health care utilisation and satisfaction, we used an adapted version of the CCHS 1.2 questionnaire. 51 This allowed us to measure the type of health care services utilised and frequency of utilisation in the past 12 months for ‘emotional problems, mental disorders and addiction’. This includes hospitalisation, as well as consultation with psychiatrists, psychologists, general practitioners, nurses, and social workers. 20 It also measures satisfaction with health services utilised in the past 12 months. Service utilisation was measured as a continuous variable (the frequency of service utilisation in the past 12 months). Service satisfaction was also measured as a continuous variable from 0 (extremely dissatisfied) to 10 (extremely satisfied).
Statistical Analysis
Selected characteristics were compared between immigrants and nonimmigrants at baseline (T2) with Student’s t test for continuous variables and chi-square tests for categorical variables.
To assess the cross-sectional and longitudinal associations between immigration-related exposures and mental health services utilisation and service satisfaction, we created and included 6 new outcome variables in a regression analysis. For both utilisation and satisfaction, the 3 outcomes were baseline (T2) score, the 2-year change score from T2 to T3, and the 4-year change score from T2 to T4. Since 3 immigration-related exposures were assessed (immigration status, duration of residence, and region of birth), a total of 18 multiple linear regression models were constructed. Each included 1 of the 3 exposure variables and 1 of the 6 outcome variables. Age, gender, household income, highest education, and mental well-being were all adjusted in the regression models. In addition, the models for 2-year or 4-year change scores also adjusted for the baseline scores. Significance was set at 0.05 (2-tailed). All analyses used SAS version 9.4 (SAS Institute, Cary, NC, USA).
Results
The comparison of basic characteristics at baseline is described in Table 1. Interestingly, immigrants have been in Canada for 19.6 years on average. Immigrants had significantly higher education levels, but their household income was significantly lower than nonimmigrants. Additionally, immigrants were significantly younger but significantly more likely to be married.
Comparison of Basic Characteristics between Immigrants and Nonimmigrants at Baseline (T2).
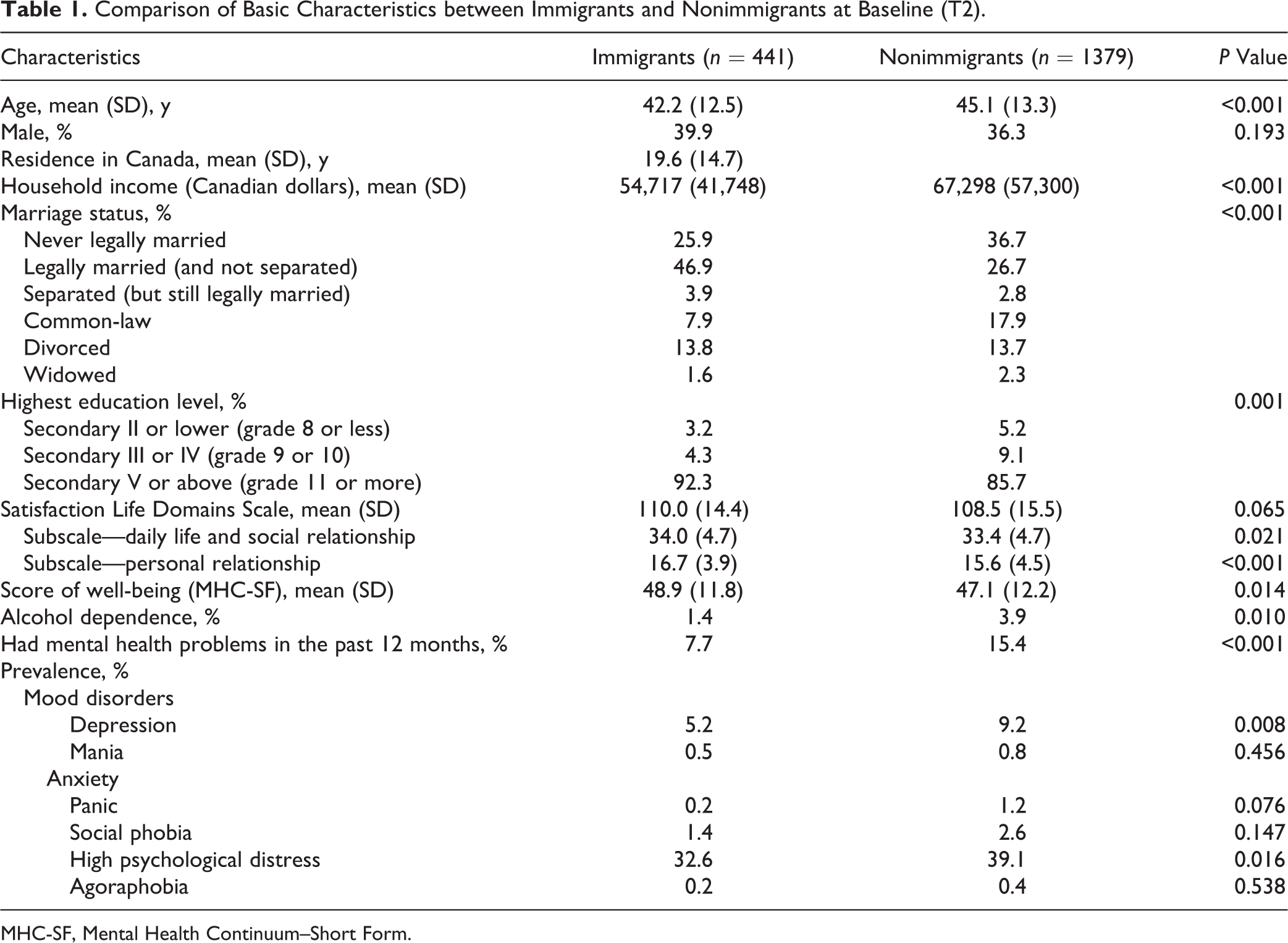
MHC-SF, Mental Health Continuum–Short Form.
In terms of mental health, immigrants fared significantly better on 7 of the 12 variables measured. There were no significant differences in the other 5 variables, although consistent and clear trends can be observed in favour of better mental health for immigrants. For example, the percentage of immigrants reporting mental health problems in the past 12 months was less than half that of nonimmigrants. Immigrants also had a significantly lower prevalence of high psychological distress, depression, and alcohol dependence. They had significantly higher scores of well-being, as well as satisfaction with daily life, social relationships, and personal relationships.
Table 2 shows the mean frequency of health services utilisation in the past 12 months and mean health services satisfaction score overall, as well as by duration of residence and region of birth. At all 3 time points, immigrants (as a whole) reported a lower frequency of health care services utilisation but higher health services satisfaction scores than nonimmigrants. Interestingly, there was a linear increase in rates of health services utilisation for both immigrants and nonimmigrants from T2 to T4. This was particularly marked for immigrants, whose rate tripled from T2 (2009-2010) to T4 (2014-2015).
Health Service Utilisation Count and Satisfaction Score at T2, T3, and T4.
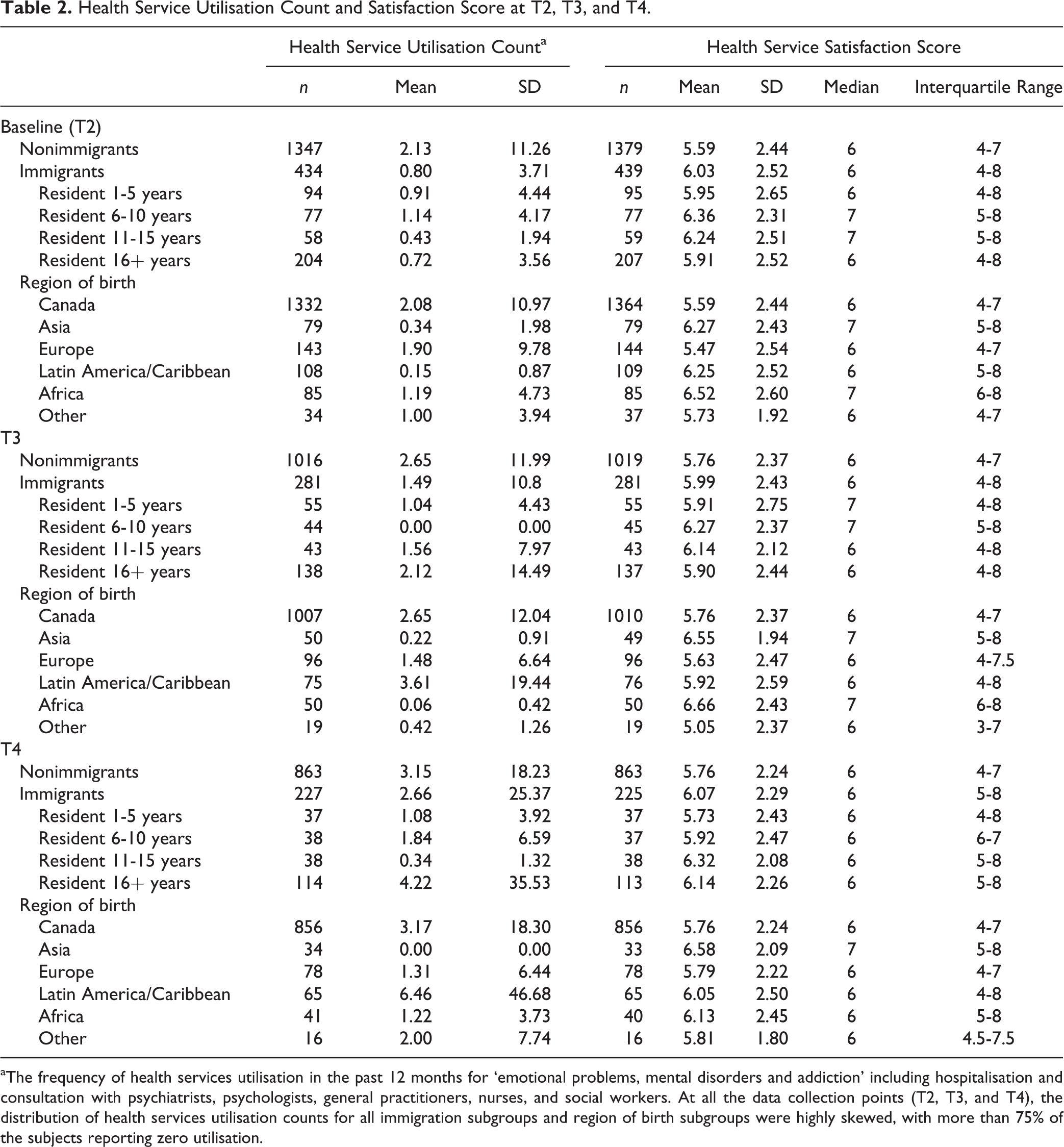
aThe frequency of health services utilisation in the past 12 months for ‘emotional problems, mental disorders and addiction’ including hospitalisation and consultation with psychiatrists, psychologists, general practitioners, nurses, and social workers. At all the data collection points (T2, T3, and T4), the distribution of health services utilisation counts for all immigration subgroups and region of birth subgroups were highly skewed, with more than 75% of the subjects reporting zero utilisation.
At T3 and T4, immigrants who had resided in Canada 16+ years had higher rates of service utilisation in comparison to recent immigrants. Participants born in Asia or Africa generally reported lower frequency of health care services utilisation but higher services satisfaction scores (at all time points) than people born elsewhere. At T3 and T4, immigrants from Latin America/Caribbean had the highest rates of service utilisation, even higher than nonimmigrants.
Table 3 details the results from the adjusted multiple linear regression models for assessing the cross-sectional and longitudinal associations between immigration-related exposures and health services utilisation. At baseline, immigrants reported significantly lower frequency of health service utilisation compared to nonimmigrants. Specifically, the frequency of health service utilisation in the past 12 months was on average 1.47 units lower in immigrants (P = 0.02). No significant longitudinal associations were found between immigration status, duration of residence, region of origin, and utilisation.
Multiple Linear Regression Models for the Association between Health Service Utilisation (Continuous Outcome), Immigrant Status, and Country of Birth.
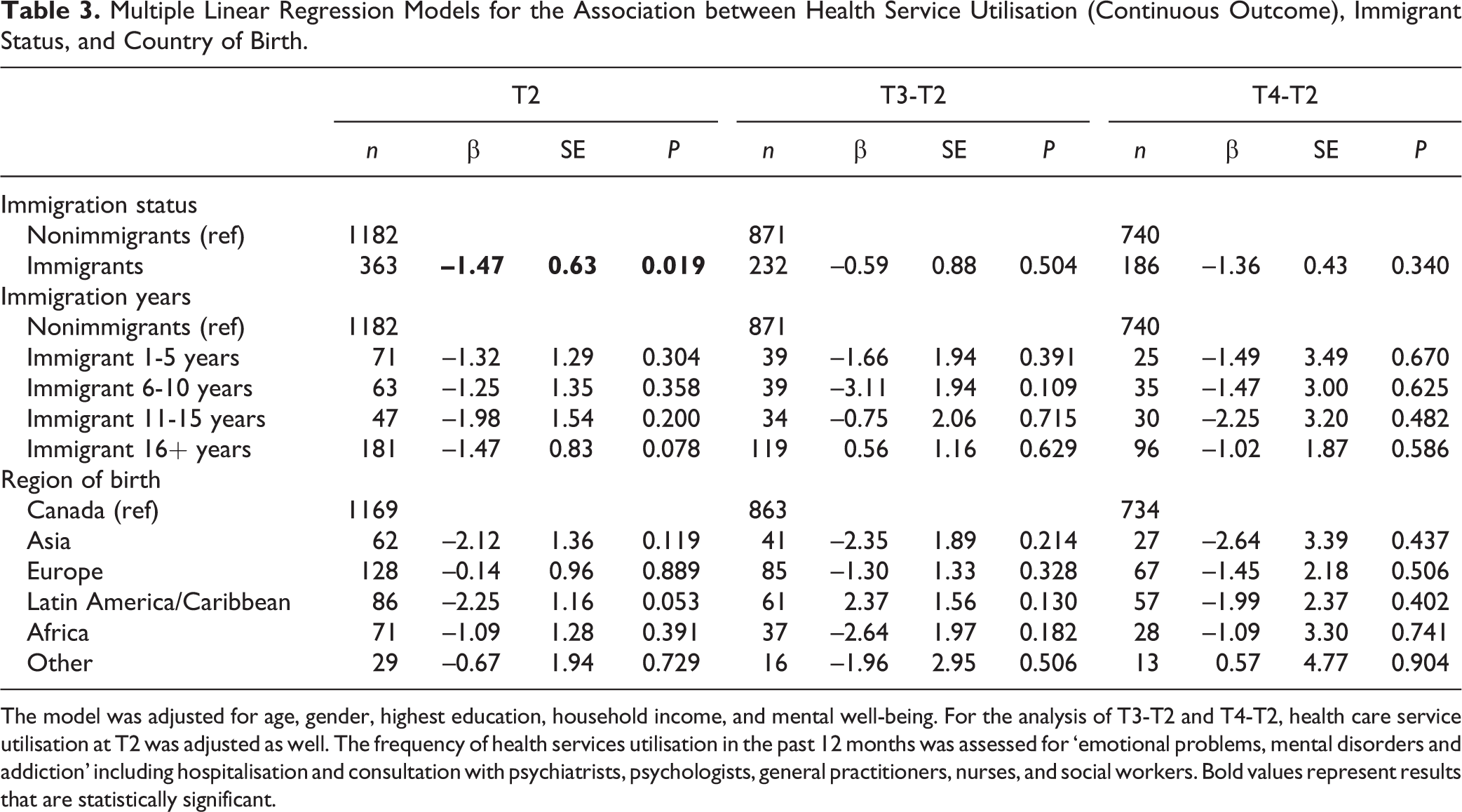
The model was adjusted for age, gender, highest education, household income, and mental well-being. For the analysis of T3-T2 and T4-T2, health care service utilisation at T2 was adjusted as well. The frequency of health services utilisation in the past 12 months was assessed for ‘emotional problems, mental disorders and addiction’ including hospitalisation and consultation with psychiatrists, psychologists, general practitioners, nurses, and social workers. Bold values represent results that are statistically significant.
Table 4 displays the results from multiple linear regression models for assessing the baseline and longitudinal associations between immigration-related exposures and health services satisfaction. These results were similar to the findings for health service utilisation, where only baseline effects of immigration-related exposures were detected. At baseline, immigrants reported higher scores in service utilisation satisfaction compared to nonimmigrants. Specifically, the satisfaction score was on average 0.34 units higher in immigrants than in nonimmigrants (P = 0.02). Analysis of duration of residence revealed that this cross-sectional effect appeared only in immigrants who have been in Canada for more than 5 years. Recent immigrants (immigrated for 1-5 years) had similar satisfaction scores to nonimmigrants. Immigrants with residence longer than 5 years reported higher satisfaction scores. Participants born in Asia, Latin America/Caribbean, and Africa all reported higher satisfaction scores at baseline compared to the Canadian-born. No significant results were found when assessing the longitudinal effects of immigration variables on services satisfaction score.
Multiple Linear Regression Models for the Association between Health Services Satisfaction, Immigrant Status, and Region of Birth.
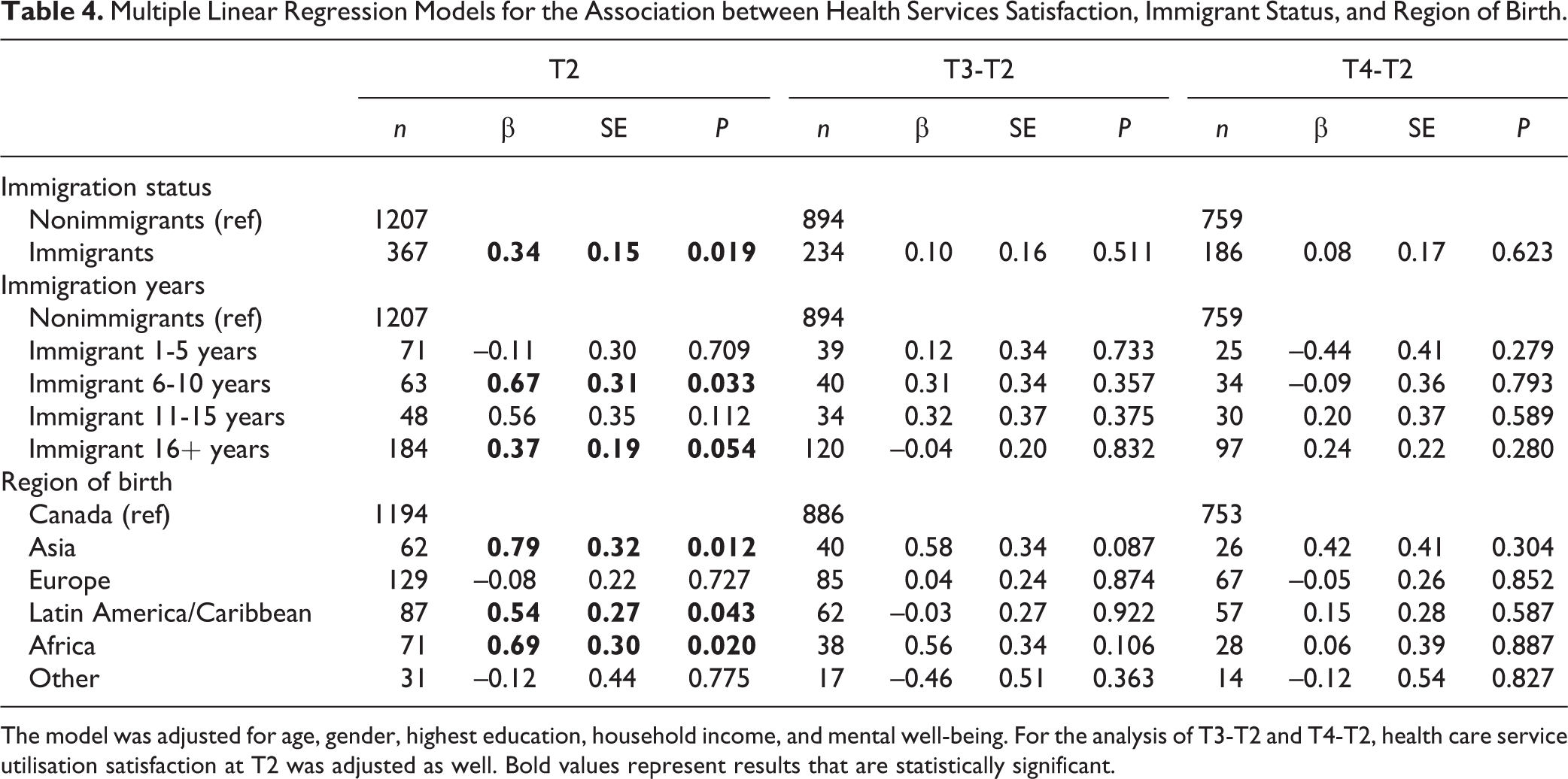
The model was adjusted for age, gender, highest education, household income, and mental well-being. For the analysis of T3-T2 and T4-T2, health care service utilisation satisfaction at T2 was adjusted as well. Bold values represent results that are statistically significant.
Discussion
A key finding of this study is that immigrants’ mental health was significantly better than nonimmigrants on 7 of the 12 relevant variables measured. They had significantly fewer mental disorders, lower scores of psychological distress, and higher scores of mental well-being. These findings are consistent with the numerous Canadian-based studies discussed earlier indicating that immigrants have overall better mental health than nonimmigrants. 17,18,20 –24 This is in contrast to some of the US and UK literature, which indicates that immigrants and minorities often have worse mental health.13-15,31,32
Most immigrants in this study had lived in Canada over 10 years, with a mean duration of residence of 20 years. Some literature on the healthy migrant effect suggests that immigrant health declines over time due to some of the postmigratory factors discussed earlier. 27,28 However, the present study indicates that immigrants as a whole maintain better or at least similar mental health in comparison to the native-born population.
These findings can be explained by various factors. Selection effects may be partially responsible, with the most healthy people immigrating and staying in Canada. Other social factors may also contribute to immigrants’ better mental health. For example, immigrants were much more likely to be married and educated and showed higher satisfaction with the quality of their social and personal relationships. Close-knit families and ethnic communities may provide social support and a sense of belonging, both of which are consistently associated with lower psychological distress and better mental health. 52 –54
Indeed, data from the Canadian Ethnic Diversity Survey show that immigrants maintain a strong sense of belonging to their ethnocultural group and were likely to be involved in ethnic or immigrant organisations. 55 All this is fostered by the federal government’s ongoing and entrenched policy of multiculturalism, which encourages immigrants to maintain association with their traditions and ethnic groups. 56 This may all combine to reduce social isolation, decrease alienation, and promote mental health.
Another key finding is that immigrants utilised health services in response to emotional problems, mental disorders, and addictions at a significantly lower rate than nonimmigrants. Immigrants from Africa and Asia have especially low rates of utilisation, as did more recent immigrants. This is consistent with other research discussed earlier. 16,35,36 Some research suggests that this underutilisation is due to stigma associated with utilisation of mental health services, as well as dissatisfaction with these services, which are perceived to be too impersonal and medication focused. 38,40,57 Other research suggests that immigrant underutilisation is due to a preference for informal mental health care provided by the family and ethnic community, 9 as well as different explanatory models where mental and emotional distress is not perceived as an illness but as an inevitable part of everyday life. 37 The higher satisfaction scores for immigrants in this study suggest that underutilisation may be more due to these latter factors than due to service dissatisfaction.
Interestingly, there was a linear increase in service utilisation from T2 to T4 for immigrants and nonimmigrants, with the rate tripling for immigrants. This may reflect greater mental health awareness due to provincial and national programs including Bell Let’s Talk, the Quebec Mental Health Action Plan, and the Mental Health Commission of Canada’s ongoing antistigma campaign.3
The rate of service satisfaction in immigrants was significantly higher than that of nonimmigrants and was markedly higher among Asian and African immigrants. Again, this stands in contrast to US and European studies, which generally show that immigrants and minorities report lower rates of service satisfaction in comparison to nonimmigrants. 31 –33 This may reflect common sentiments of immigrant belonging and satisfaction in Canada (compared to the United States and Europe) due to the enduring policy of multiculturalism, as well as more harmonious ethnic relations in Canada. 56 That said, the overall rate of satisfaction scores for immigrants and nonimmigrants indicates that there is room for service improvement for both groups. Qualitative research could usefully explore this (dis)satisfaction.
The study has some limitations. First, we did not stratify the outcome variables measuring prevalence of mental health and illness by region of origin or duration of residence. Doing so would have led to 360 separate cells (6 regions × 5 durations × 12 outcome variables). This would have led to very small cell numbers, risking both alpha inflation and overall validity. Second, we did not differentiate between economic migrants and refugees. Research indicates that the latter group has experienced significantly more premigratory and migratory journey stressors and that their mental health tends to be poorer. 6 Third, data were collected from only one area in the city of Montreal. Results may be different for immigrants and nonimmigrants living elsewhere. Fourth, questionnaires were only available in English or French. Immigrants unable to speak either of these languages were therefore excluded from the research. These immigrants may have been the least integrated and the most dissatisfied. Fifth, the distribution of health services utilisation counts were highly skewed (see Table 2) and could not be made closer to normal distribution by different approaches of transformation. This may result in the study being underpowered in detecting significant differences between immigration subgroups in health services utilisation.
Finally, a note on attrition. Attrition rates were 28.4% (T3) and 16.1% (T4). Analysis revealed that immigrants had higher rates of attrition. At T3, attrition was 36.1% in immigrants and 26.0% in nonimmigrants. At T4, attrition was 19.5% in immigrants and 15.2% in nonimmigrants. Most recent immigrants (duration of residence ≤5 years) had the highest attrition rate, perhaps related to the fact that roughly 20% of immigrants leave within the first year of arrival. 25 Region of origin was not related with attrition. We tested if attrition was associated with 1) mental health problems in the past 12 months, 2) health care service utilisation, and 3) health service satisfaction (detailed results available on request). None of these tests yielded significant differences between immigrants and nonimmigrants. Attrition was related to a key exposure variable (immigration status) but not any outcome variable. As such, we believe the internal validity of this study is not compromised by attrition.
Conclusion
This study indicates that immigrants tend to have better mental health, lower utilisation of services, and higher service satisfaction. The results overlap with other research indicating that immigrants to Canada have better mental health than nonimmigrants. Policy imperatives contained in the Mental Health Strategy for Canada state that mental health services must be responsive to cultural and ethnic diversity. 3 The rates of underutilisation, as well as the less than perfect rates of service satisfaction, suggest a need for targeted strategies to engage immigrants with mental health care and likewise improve services for them. This is especially so for Asian and African immigrants. This could be a key activity for the Mental Health Commission of Canada, whose mandate was recently renewed for a further 10 years.
Footnotes
Acknowledgements
We thank the Canadian Institute of Health Research and all the individuals who participated in the research.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: The study was funded by the Canadian Institute of Health Research (CTP-79839).
