Abstract
Effects of ribavirin on the structure of peritubular sheath (PS) of seminiferous tubules and on testicular functions were studied. We found that ribavirin at a dose of 4 mg/kg/day for 4 weeks produced a significant reduction in testosterone level (6.3 ± 0.2; P < 0.001) and in spermatogenic score count (3.8 ± 0.2; P < 0.001) compared to control values. The thickness of PS (17.8 ± 1.13) and tubular lumen perimeter (1024.7 ± 67) was significantly increased compared to controls (10.7 ± 0.70; P < 0.001 and 808 ± 25; P = 0.004, respectively). The length of germinal epithelium (411.8 ± 39) and tubular external diameters (1661.8 ± 115) was significantly reduced compared to control values (708.4 ± 40; P < 0.001 and 2358.8 ± 169; P < 0.001, respectively). The basement membranes (BMs) were thickened with great deposition of collagen. Myoid cells showed altered structure and extracellular matrix revealed disorganization by excessive collagen I and IV accumulation. Testicular damage was established histologically. Evidence of apoptosis was detected in germ cells. There was a significant increase in integrated density of Casp-3 expression (38,121,743 ± 1,763,420; P < 0.001) in seminiferous tubules compared to control (24,788,409 ± 1,900,140). It is concluded that ribavirin can cause alterations of the testicular function and structure with increased apoptosis in the tissues after 4 weeks of administration. The damaging effect could be persuaded by destruction of the peritubular sheath.
Introduction
Human exposure to unsafe medications is still a major public health concern. Hepatitis C virus (HCV) is a worldwide health problem and it is considered a causal factor of chronic hepatitis C (CHC). According to the World Health Organization, at least 170 million people in the world experienced HCV infection. Only 15%–40% of those infected people show self-resolution otherwise progressed to cirrhosis and hepatocellular carcinoma. 1
At present, the combination of pegylated interferon-α and ribavirin is the base of the treatment of CHC. Ribavirin is a synthetic guanosine analogue that undergoes intracellular phosphorylation. 2 The combination is linked up with several extra-hepatic side effects. For example, depression, headache, and pyrexia happen in over 20% of patients. Less frequent side effects include retinopathy, hematological abnormalities, and thyroid dysfunction.3,4
A study of other possible side effects on the birth rate of males may be useful for the health community. Several years ago, it was shown by Narayana et al. 5 that intraperitoneal administration of ribavirin causes damage in the testes and affects fertility of male rats. However, the relation of the gonadal harmful effects to the structure of the seminiferous tubules envelop has not been demonstrated.
The seminiferous tubules comprise 80% of testicular volume. 6 The tubular lining of epithelial cells and Sertoli cells is surrounded by a peritubular sheath (PS). The PS of the rat’s seminiferous tubules has three components: the epithelial basement membrane (BM), myoid cells, and extracellular matrix (ECM). 7 The BM lies in contact with the epithelium and includes collagen type I and IV and laminin synthesized by Sertoli cells. 8 The myoid cells have abundant actin, myosin, and desmin filament disposition. 9 It is separated from the BM by large quantities of collagen with lamellar character.
Spermatogenesis depends on the peritubular and intertubular cellular components as well as the intra-testicular and extra-testicular hormonal controlling processes and functions of the intertubular vessels, the Leydig cells, and others. 10 The BM and the underlying collagen fibers have important biological functions. They form a selective barrier between the epithelium and the stroma and facilitate the interaction between the epithelium, the myoid cells, and cells in the interstitium. 11 Also, ECM proteins could serve as a reservoir for growth factors. 12
The biological significances of the PS and its impact on the testicular integrity divert our attention that oral ribavirin administration could affect the integrity of the seminiferous tubules through changes in their envelope structure.
This study aimed to evaluate the histomorphometric and ultrastructural changes of the PS and the seminiferous tubules of the rats after oral administration of ribavirin and the possible relation to the function of the testes indicated by the spermatogenic score count and the serum level of testosterone.
Materials and methods
Drugs
Ribavirin capsules (Viracure®) were used; every capsule contains 400 mg of ribavirin. The ribavirin capsule (400 mg) was dissolved in 50 mL saline. Each rat in the treated groups had received a daily oral dose of 0.5 mL containing 4 mg ribavirin using a feeding syringe for 4 weeks. This dose is parallel to the maximum dose of the drug recommended for human during treatment of HCV: 12 mg/kg (1200 mg for body weight ⩾ 75 kg). 13
Animals
In all, 36 healthy and sexually mature male albino rats, weighing 250–260 g, were purchased from the breeding center of experimental animals at College of Medicine, Zagazig University, Egypt. Prior to treating, the selected animals were acclimated to the environment for 7 days. They were housed in well-ventilated hygienic cages, fed standard balanced diet, and allowed water ad libitum with the environment controlled for 12/12 h light/dark cycle, and the temperature was adjusted at 22°C–24°C and the humidity at 50%–60%. All animal procedures were conducted in accordance with the principles of laboratory animal care (National Institutes of Health Guide for the Care and Use of Laboratory Animals (NIH Publications No. 8023, revised 1978)) and in accordance with local laws and ordinances.
Experimental design
In all, 36 rats were divided into three equal groups: Group I (control group): animals were orally gavaged with 1 mL of saline once daily for 4 weeks and then sacrificed. Group II (ribavirin treated for 1 week): animals were received ribavirin daily for 1 week and then sacrificed. Group III (ribavirin treated for 4 weeks): animals were received ribavirin daily for 4 weeks and then sacrificed by cervical decapitation.
Bioassay for serum-free testosterone
Samples of blood were obtained from the retro-orbital venous plexus immediately before the sacrifice. A volume of 2 mL of blood sample was placed into tubes containing ethylenediaminetetraacetic acid (EDTA), then allowed to clot for 30 min, and then centrifuged at 4°C for 20 min. Using reagents from Euskirchen, Germany, the serum levels were measured by enzyme-linked immunosorbent assay (ELISA) technique. 14
Processing of specimens
The testes from each rat were placed in Bouin’s solution for 24 h and then processed and embedded in paraffin blocks. Applying the previously described methods of Bancroft and Gamble, 15 5-µm-thick deparaffinized sections were stained with either (1) hematoxylin and eosin (H&E) to verify histological details, (2) periodic acid-schiff (PAS) stain to visualize the carbohydrate contents of BMs, or (3) Masson’s trichrome staining for the collagen fibers.
Score count for the evaluation of spermatogenesis 16 and its modification by DeKretser and Holstein 17 and Holstein et al. 10
Johnsen’s score is a quantitative histological grading system; in at least 50 seminiferous tubules, the degree of sperm maturation is graded between 1 and 10, according to the most advanced germ cell in the tubule, where 10 is the health status and 1 is the most damage, with the germ and somatic cell lost. The total score is then determined by dividing the total score by the number of evaluating tubules.
Testicular histomorphometry
Quantitative morphometric measures were done on 36 blocks: 12 from each group. All analyses were performed by one investigator blind to the group identity. Measurements were taken using an Image Analyzer (Leica QWin Standard, digital camera CH-9435 DFC 290, Germany). The following measurements were taken: (1) the thickness of the PS in PAS-stained sections using 100×, (2) the relative length of the germinal epithelium in H&E-stained sections using 20×, (3) lumen of the seminiferous tubules in H&E-stained sections using 10×, and (4) the seminiferous external tubular diameter in H&E-stained sections using 10×. For each parameter, five measurements were taken from each section.
Measurement of the thickness of the PS
The thickness of the PS was represented by the average distance (in micrometer) between the internal layer of BM to the external peritubular cell layer in four different sites of the tube wall. Peritubular cells were differentiated from the interstitial cells easily because the former were arranged around the tubules circularly, whereas the nearby interstitial cells were arranged irregularly.
Immunohistochemistry
Sections of 3 µm thickness were cut onto coated slides. Sections were stained with markers for apoptosis: caspase-3 (Casp-3) or for collagen IV using peroxidase-labeled streptavidin–biotin technique. After deparaffinization and rehydration, quenching of the endogenous peroxidase was done using 3% H2O2/methanol. Blocking of non-specific binding was reduced by incubation with 5% bovine serum albumin. The sections were then incubated for 45 min at room temperature with the primary antibody for collagen IV (anti-collagen IV monoclonal antibody; 239M-1, conc.: 150 µg/mL; Sigma-Aldrich, St. Louis, MO, USA) or Casp-3 (anti-Casp-3polyclonal antibody, PAA626Ra02, conc.: 200 µg/mL; Wuhan USCN Business Co., Ltd., Houston, USA). Later, sections were incubated with a secondary biotinylated antibody (biotin-conjugated goat anti-mouse IgG) for 1 h at room temperature. The products of the reaction were visualized by chromogen diaminobenzidine. Positive collagen IV signals appeared as brown staining in the cell membrane and ECM, while positive Casp-3 signals appeared as brown staining in the cytoplasm. For the negative control, the primary antibody was replaced by phosphate-buffered saline (PBS). 18
Immunoexpression of Casp-3 was evaluated by calculating the integrated density (ID) of the stained sections using the image analysis software, ImageJ 2.0.0-beta4 v (National Institutes of Health, USA).19,20 Briefly, after capturing five descriptive images per each slide at original magnification of 200×, we set the measurements to consider the ID, and then, the images were converted into gray scale shape. Using the selected tool, we drew five non-overlapped equal squares provided they have been scattered all over the field. The calculated ID was then exported into an Excel sheet.
Electron microscope study
Specimens for electron microscopy were immediately fixed in 2.5% phosphate-buffered glutaraldehyde (pH 7.4). And therefore, they were postfixed in 1% osmium tetroxide in the same buffer at 4°C, dehydrated, and then embedded epoxy resin. Ultrathin sections were stained with uranyl acetate and lead citrate. The sections were examined and photographed using the JEOL JEM 1200 EXII Electron Microscope (Joel CX 100 transmission electron microscope operated at an accelerating voltage of 60 KV Ltd.) at Research Laboratory, Faculty of Science, Ain Shams University (Egypt). 21
Statistical analysis of data
All statistical data were obtained and significance tests were posted out using IBM (version 21) statistical software package. Statistical significance was determined by one-way analysis of variance for differences between the means of different groups. Further analysis was carried out utilizing the post-hoc test to compare the parameters in the different groups with each other. A probability of P less than 0.05 was considered statistically significant. Correlation between the thickness of PS and the spermatogenic score count was done using Pearson correlation. All data were expressed as mean ± standard error (mean ± SE).
Results
Body and testicular weight
According to Table 1, no deaths were identified and no other harmfulness signs were observed in the rats treated orally with ribavirin (4 mg/kg body weight daily). All rats were weighed twice per week, and the body weight of animals after 4 weeks of treatment reduced significantly (260.8 ± 2.53) compared to the controls (303.8 ± 2.38; P < 0.001). Also, there was a significant reduction in the testicular weight after 4 weeks of treatment (1.37 ± 0.02) compared to the controls (1.63 ± 0.02; P < 0.001).
Score count for the evaluation of spermatogenesis.

Exposure to ribavirin for 1 week produced non-significant changes neither in the body weight (298.8 ± 1.98; P = 0.135) nor in the testicular weight (1.59 ± 0.01; P = 0.121) compared to the control values.
Serum testosterone level
As indicated in Table 1, after 4 weeks of ribavirin treatment, there was a significant decrease in the serum testosterone level (6.3 (0.2; P < 0.001)) compared to control values (11.6 (0.2)). No significant changes were detected after 1 week of treatment (10.9 (0.3; P = 0.051)).
Light microscopic examination
Morphology of the PS
Light microscopic examination of control adult albino rats’ testes revealed apparently thin stained BM with flattened myoid cells and thin homogenous red zone of PAS (Figure 1(aI, II)). The use of anti-collagen IV antiserum resulted in staining of the BM which appeared as a thin brown regular line surrounding most of the tubules (Figure 1(aIII)). After 1 week of ribavirin treatment, there were apparently thin irregular BM and the myoid cells possessed irregular thin nuclei (Figure 1(bI)). An irregular thin red zone of PAS was detected (Figure 1(bII)). Positive collagen IV immunoreaction was detected in the BM as a thin brown line with obvious irregularities in most of the tubules (Figure 1(bIII)). After 4 weeks of ribavirin treatment, there was apparently thickened BM with visible folds. Myoid cells with bulging nuclei were also detected (Figure 1(cI)). Thick positive-PAS reaction of the PS was distinctively separating the tubules from the surrounding interstitium (Figure 1(cII)). Diffused patterns of collagen IV staining were observed in the BM of most of the tubules. Some areas of collagen IV deposits were present in the form of invaginations into the seminiferous epithelium (Figure 1(cIII)).
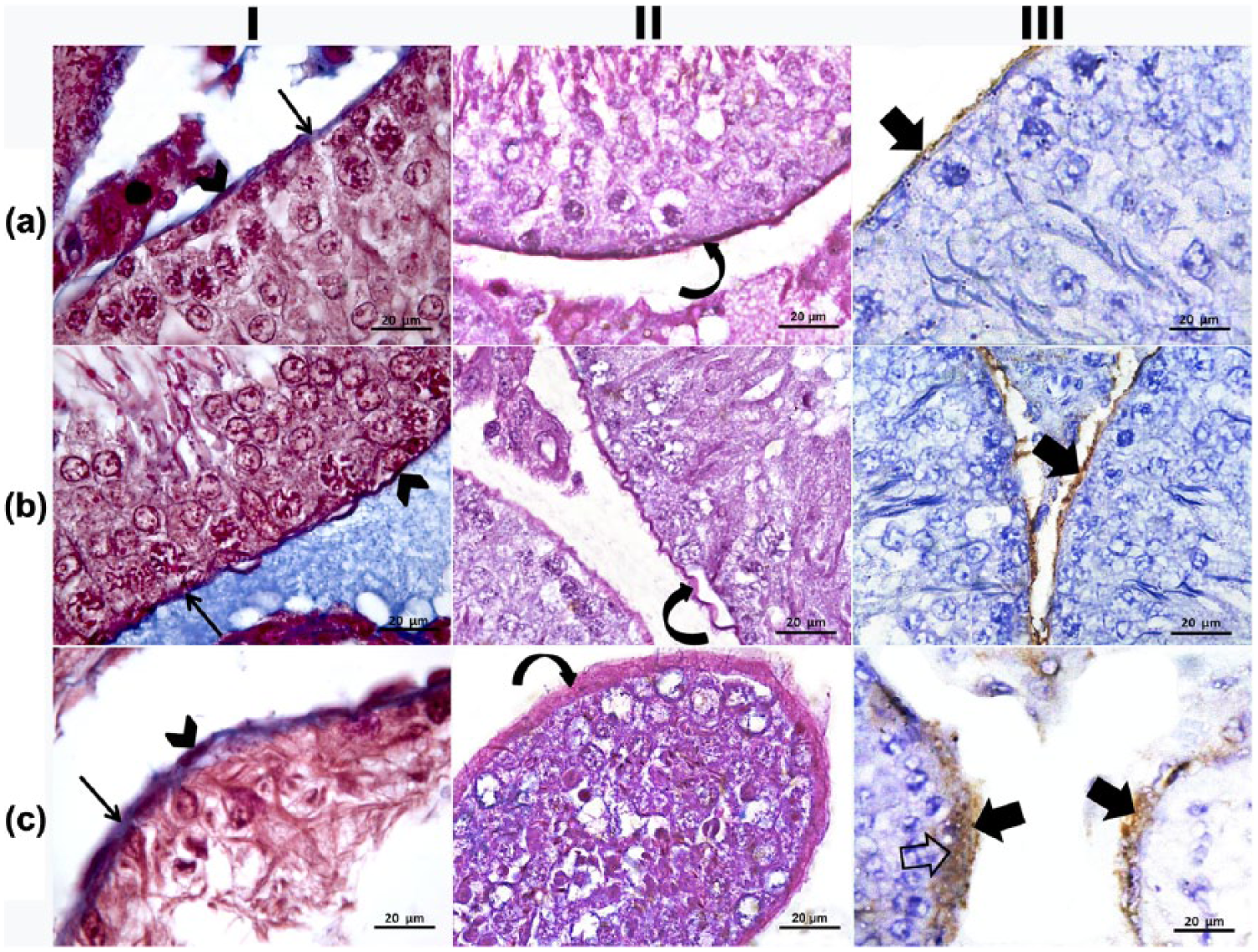
Photomicrographs of the wall of rat seminiferous tubules. (a) Control group (Group I) shows thin sheath (arrow) with flattened myoid cells (arrowheads) and thin homogenous red zone of PAS (curved arrow). Collagen IV is expressed in the thin basement membrane (thick arrow). (b) After 1 week of ribavirin treatment (Group II), there were thin irregular basement membrane (arrow), myoid cells with irregular thin nuclei (arrowhead), and irregular thin red zone of PAS. Collagen IV is expressed in the thin basement membrane (thick arrow). (c) Four weeks after ribavirin treatment (Group III), there is apparently thickened basement membrane with visible folds (arrow). Myoid cells are seen with bulged nuclei (arrowhead). Thick positive-PAS reaction (curved arrow) of distinct peritubular sheath is seen separating the tubules from the surrounding interstitium. Diffused patterns of collagen IV-immunoexpression were observed in the basement membrane of the tubules (thick arrow). Some areas of collagen IV deposits in the form of invagination into seminiferous epithelium (open arrow) are also seen (I: Masson trichrome; II: PAS stain; III: immunoperoxidase technique for collagen type IV).
Morphology of the seminiferous tubules
Cross sections of the control specimens revealed apparently normal spermatogenesis with regular cell organization in the seminiferous tubules. Intertubular spaces appeared narrow and contained groups of Leydig cells and blood vessels (Figure 2(a)). Each tubule was surrounded by a single layer of flat myoid cells, and the germinal epithelium was formed by different types of spermatogenic cells: spermatogonia, primary spermatocytes, spermatids, and Sertoli cells. Sertoli cells were observed with their large nuclei, lying on well-defined BM (Figure 2(b)). After 1 week of exposure to ribavirin, slight changes were observed in the intertubular cellular arrangement in the form of well-organized germinal epithelium with sperm tails. Small cytoplasmic vacuoles were seen between the germinal cells (Figure 2(d) and (c)). Examination after 4 weeks of treatment revealed many degenerated tubules resting on irregularly defined BM and surrounded by wide interstitial spaces (Figure 3(a)). Various tubules had a detectable reduction in the thickness of their germinal epithelium and apparently wide lumina (Figure 3(b)). Most of the spermatocytes appeared with darkly stained nuclei. Multiple disintegrated germ cells were observed with exfoliation (Figure 3(c)). Severely affected tubules showed very few degenerating germ cells resting on thick BM. Congested blood vessels were also seen in the wide interstitium (Figure 3(d)).

Photomicrographs of rat seminiferous tubules. (a and b) Control group (Group I) shows normal spermatogenesis with seminiferous tubules of regular contour and narrow intertubular spaces and Leydig cells (IC). Each seminiferous tubule lies on regular BM and surrounded by a single layer of flat myoid cells (crossed arrows), and its stratified germinal epithelium was formed of different types of spermatogenic cells, spermatogonia (arrowheads), primary spermatocytes (double arrowheads), spermatids (arrows), sperms (asterisks), and Sertoli cells (curved arrows). (c and d) After 1 week of ribavirin treatment (Group II), some seminiferous tubules (T) have shown organized lining of epithelium (G) with sperm tails (double arrows) in its lumen. Small vacuoles are seen between the germinal epithelium (arrows). There is a relatively wide interstitium (I) (hematoxylin and eosin stain).

Section of rat seminiferous tubules after 4 weeks of ribavirin treatment (Group III). (a and b) Many distorted seminiferous tubules (T). Some tubules show marked reduction in the thickness of the germinal epithelium (arrowheads). Most of the spermatocytes appeared with darkly stained pyknotic nuclei (arrows). Many vacuoles (V) of variable sizes are noticed within the germinal epithelium. (c) Germ cells’ disintegration with luminal exfoliation (X) is detected. (d) Severely affected tubules are lined by very few degenerating germinal epithelium (curved arrow) and relatively wide empty lumina (L). Note that the irregular membrane (crossed arrow) and wide interstitial spaces (I) contain congested blood vessels (double arrowheads; hematoxylin and eosin stain).
Immunohistochemistry
Immunohistochemical stained sections of the control group showed moderate expression of Casp-3 in the spermatogonia and in the interstitial cells with weak expression in the rest of spermatogenic cells (Figure 4(a)); 1 week after ribavirin treatment, there was a strong Casp-3 expression in the spermatogonia and primary spermatocytes. Moderate expression is seen in the rest of spermatogenic cells and in the interstitial cells (Figure 4(b)). Sections after 4 weeks of treatment showed strong Casp-3 expression in all spermatogenic cells and in the interstitial cells (Figure 4(c)).

Photomicrographs of rat seminiferous tubules. (a) Control group (Group I) shows moderate Casp-3 immunoexpression in the spermatogonia (arrowheads) and weak expression in the primary spermatocytes (double arrowheads), the spermatids (arrow), and sperm heads (curved arrows). (b) After 1 week of ribavirin treatment (Group II), strong Casp-3 expression appears in spermatogonia (arrowheads) and primary spermatocytes (double arrowheads) with moderate expression in the spermatids (arrow) and sperm heads (curved arrows). (c) Four weeks after ribavirin treatment (Group III), intense Casp-3 expression appears in the spermatogonia (arrowhead), primary spermatocytes (double arrowheads), spermatids (arrow), and sperm heads (curved arrow; immunoperoxidase technique for Casp-3).
As indicated in Table 2 and Figure 5, there was a significant increase in the ID of Casp-3 immunostaining after 4 weeks of exposure to ribavirin compared to control specimens (P = 0.001). No significant difference was detected after 1-week exposure (P = 0.193).
Body weight, testicular weight, and serum testosterone level in the studied groups.

SE: standard error.
The mean difference is significant at the 0.05 level. Significance of the difference between the control and 1-week ribavirin treatment = P1, between the control and 4-week ribavirin treatment = P2, and between 1-week and 4-week treatment = P3.

Histogram represents the quantitative analysis of integrated density of Casp-3 immunoexpression across the entire seminiferous tubules.
Electron microscopic examination
Ultrathin sections of the control rats’ testes showed Sertoli cells with large euchromatic nuclei. Primary spermatocytes had large rounded nuclei with small irregular clumps of heterochromatin. All cells were resting on thin, regular, and well-defined BM ensheathed by a single layer of flat myoid cells. Few collagen fibers were found between the BM and the myoid cell layer (Figure 6(a) and (b)). Spermatids had round euchromatic nuclei. Their cytoplasm contained peripherally located mitochondria ((Figure 6(c)). Cross sections in the mid pieces of sperms showed that the central axoneme was formed of nine doublets of microtubules with two central singlets and surrounded fibrous sheath and mitochondrial sheath (Figure 6(d)). There was a widening of the intercellular spaces between the germinal epithelium 1 week after ribavirin treatment. Spermatogonia appeared with oval euchromatic nuclei (Figure 7(a)). Primary spermatocytes showed large round nuclei with small irregular clumps of heterochromatin (Figure 7(b)). Sertoli cells had euchromatic nuclei and the spermatids appeared with round euchromatic nuclei and peripherally located mitochondria. All cells were resting on thin irregular BM with little collagen fiber between BM and myoid cells (Figure 7(c)). Most of the sperms appeared normal with central axoneme surrounded by nine electron-dense bundles of fibrous sheath. Few destructed sperms were also present (Figure 7(d)). Sertoli cells appeared with euchromatic nuclei and the spermatids had shrunken nuclei and most of their mitochondria lost their orientation 4 weeks after ribavirin treatment. Wide intercellular spaces were observed between the germ cells (Figure 8(a) and (b)). There were severely affected tubules which were lined by Sertoli cells rested on thick, irregular BM with excessive collagen fibers between BM and myoid cells (Figure 8(c)). Most of the sperms showed the marked affection of axoneme, fibrous sheath, and destructed mitochondrial sheath (Figure 8(d)).
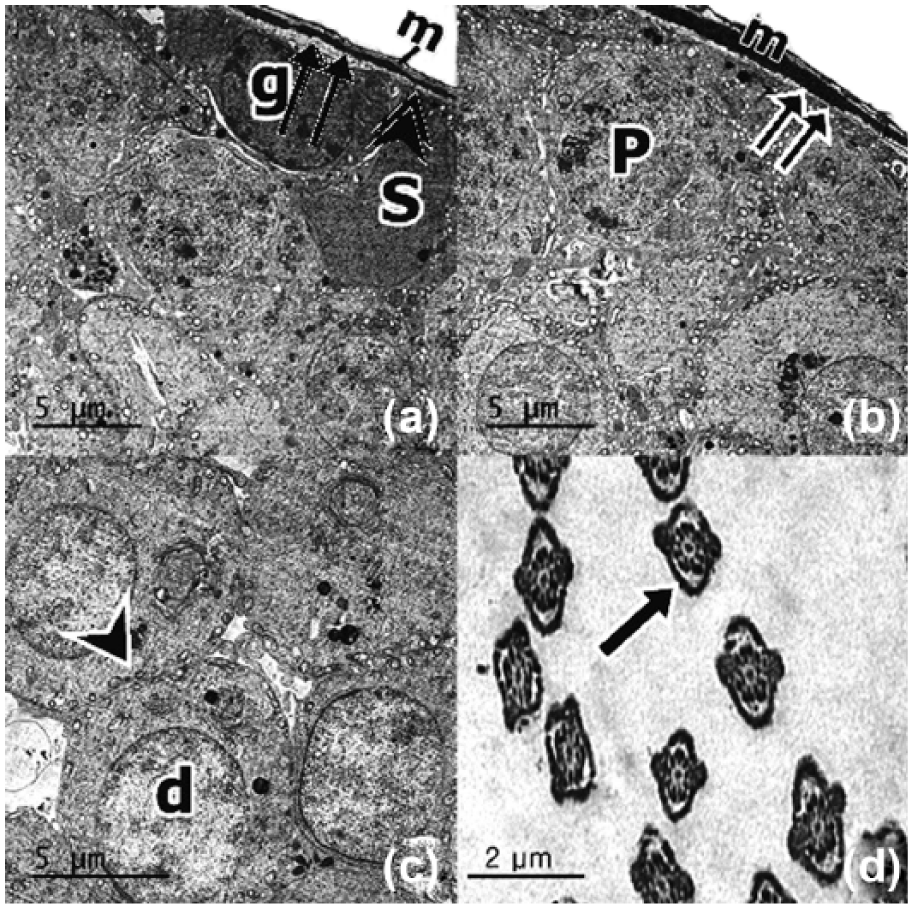
Transmission electron micrographs from the testis of a control adult albino rat (Group I). (a and b) Sertoli cells with large euchromatic nucleus are resting on the thin regular BM ensheathed by single layer of flat myoid cells (m). Notice the few collagen fibers (double arrows) between the BM (double arrowhead) and the myoid layer. Primary spermatocyte has large round nucleus (P) with small irregular clumps of heterochromatin. (c) Spermatids (d) with round euchromatic nuclei and peripherally located mitochondria (arrowhead). (d) Cross section in sperms show the central axoneme surrounded by nine electron-dense bundles of fibrous sheath and mitochondrial sheath (arrow).

Transmission electron micrographs from the testis after 1 week of ribavirin treatment (Group II). (a) Spermatogonium with oval euchromatic nuclei (g). Intercellular separation (I) between the germinal epithelium can be seen. (b) Primary spermatocyte shows large round nucleus (P) with small irregular clumps of heterochromatin. (c) Sertoli cell (S) with euchromatic nucleus can be noticed. Spermatids appear with round euchromatic nuclei (d) and peripherally located mitochondria (arrowhead) in their cytoplasm. All cells are resting on thin irregular BM with few collagen fibers (double arrows) between the BM (double arrowheads) and the myoid cell layer (m). (d) Cross section in sperms show the central axoneme surrounded by nine electron-dense bundles of fibrous sheath (arrow). Few sperms show destruction of mitochondrial sheath (curved arrow).

Transmission electron micrographs from the testis after 4 weeks of ribavirin treatment (Group III). (a) Sertoli cell cytoplasm has euchromatic nucleus (n). Wide intercellular spaces (I) can be seen between destructed spermatogenic cells (c). (b) Spermatids show shrunken nuclei (d) with loss of mitochondrial orientation (arrowhead). (c) Severely affected tubule is lined by Sertoli cells (S) only resting on thick irregular BM. There is increase in collagen fiber deposition (double arrows) between the basement membrane (double arrowheads) and the myoid cell layer (m). (d) Cross sections in most of the sperms show central axoneme surrounded by distorted and swollen mitochondrial sheath (curved arrow).
Testicular histomorphometric analysis
Statistical analysis of the image analyzing data revealed a significant increase in the thickness of PS after 4 weeks of administration of ribavirin (17.8 ± 1.13 µm; P < 0.001) compared to controls (10.7 ± 0.70 µm). No significant difference was recorded after 1 week of treatment (12.7 ± 0.76 µm; P = 0.118). In evaluating the score count for spermatogenesis, we found a significant difference between the control group (8.3 ± 0.1 µm) and the group received ribavirin for 4 weeks (3.8 ± 0.2 µm, P < 0.001). This difference was not significant after 1 week of treatment (7.9 ± 0.1 µm; P = 0.109; Table 3; Figure 9). Pearson correlation revealed significant negative correlation between the values of the thickness of PS and the corresponding values of the score count for spermatogenesis in the control group (r = −0.627; P = 0.029), after 1 week of receiving ribavirin (r = −0.889; P < 0.001), and after receiving ribavirin for 4 weeks (r = −0.727; P = 0.007; Figure 10).
Mean and standard error (SE) of integrated density of Casp-3 immunostaining in the studied groups.

The mean difference is significant at the 0.05 level. Significance of the difference between the control and 1-week ribavirin treatment = P1, between the control and 4-week ribavirin treatment = P2, and between 1-week and 4-week treatment = P3.
Profile of seminiferous tubule morphometric measures in the studied groups.

SE: standard error.
The mean difference is significant at the 0.05 level. Significance of the difference between the control and 1-week ribavirin treatment = P1, between the control and 4-week ribavirin treatment = P2, and between 1-week and 4-week treatment = P3.

Boxplot represents the thickness of the peritubular sheath and the score count for spermatogenesis in the studied groups. (*The mean difference is significant at the 0.05 level for F test.)

Scatter dots represent the relation of the thickness of the peritubular sheath to the score count for spermatogenesis in the studied groups (*correlation is significant at the 0.05 level (two-tailed); **correlation is significant at the 0.01 level (two-tailed).
Evaluation of the other morphometric measures of the seminiferous tubules in random fields, namely, germinal epithelial height, lumen, and external tubular diameter, revealed a significant difference between the control values and those obtained after 4 weeks of ribavirin treatment (P < 0.001). Nevertheless, the administration of ribavirin for 1 week did not produce significant changes in these measures (Table 3).
Discussion
Along with its needed effects, a drug may cause some undesirable effects. Testicular function includes the sperm production and the steroid hormone synthesis, mainly testosterone and to lesser extent estrogen. 22
In this study, there was a significant reduction in the rat’s body weight after the exposure to ribavirin for 4 weeks. Recently, many authors have reported a significant loss of body weight associated with the combined peg-IFN and ribavirin therapy. To our knowledge, there is no research on the impact of unaccompanied ribavirin on the body weight. Weight loss was found to be associated with the better virologic response.23–26 Some conditions have reported to explain weight loss, for example, nausea and vomiting that usually accompanied HCV therapy, decreased appetite, 27 altered insulin, leptin and proinflammatory cytokines, 28 reduced energy consumption, 29 and thyroid dysfunction.30,31 Still, the exact mechanism is unclear.
The normal organization of the seminiferous tubules in terms of shape, size, and internal architecture is crucial for maintaining spermatogenesis. This requires regular vascularization and interaction with surrounding tissues. This study clearly demonstrated hazardous effects of administration of ribavirin on the rats’ testes. Previous studies reported testicular toxicity and decreased sperm parameters and serum testosterone level with the use of purine nucleoside analogue (acyclovir). 32 We studied the effects of administration of ribavirin for 1 week and for 4 weeks on the structure of the seminiferous tubules with special emphasis on their PS and interrelated these effects to the mean testosterone level and to the state of spermatogenesis.
Exposure to ribavirin for 1 week revealed minimal affection in the structure and the function seminiferous tubules. Except for small cytoplasmic vacuoles between the germinal cells and few destructed sperms, the histological examination revealed organized germ cell–layers with different types of spermatogenic cells and apparently normal Sertoli cells. Cytoplasmic vacuoles could be due to non-specific injury to the germ cells. No obvious changes were observed either in the peritubular myoid cells or in the BM except for minor irregularities in some specimens. Morphometric parameters of the seminiferous tubules were nearly equivalent to those of controls. The function of the testes also was not affected as indicated by the mean serum levels of testosterone and the mean spermatogenic score count, which were comparable to the control values with no significant differences.
By the fourth week, ribavirin caused disruption of the structure and function of the seminiferous tubules. The histological observation revealed distorted tubules with destructed germ cells and widening of the intercellular spaces between the germ cells. Severely affected tubules were lined by Sertoli cells only that were resting on a thick irregular BM. Electron microscopic examination revealed destruction of the sperm axoneme and mitochondrial sheaths. The tail defects and cephalocaudal junction defects have a direct relation to unproductiveness. Narayana et al. 5 hypothesized that the epithelial gapping is caused by sloughing of the germ cells due to damage of the intercellular junction between the germ cells and the Sertoli cells. They also proved that ribavirin could alter the morphology of the sperms inducing the formation of sperm with microcephaly and cephalocaudal junction defects. These findings are in agreement with the older study of D’Souza and Narayana, 33 in which ribavirin has been found to induce cytotoxicity in rats in the form of significant decrease in the step 19 spermatids and meiotic figures and increase in the incidence of tubules with dead cells due to the induction of cell death and prevention of the cell division.
Morphometric measures revealed a significant decrease in both length of the germinal epithelium and in external diameters of the tubules with significant widening of their lumina compared to controls. These morphometric changes could be explained by sloughing of the epithelial cells, indicating the shrinkage of seminiferous tubules as a result of cell loss and represent a sign of gonadal toxicity.
The functions of the testes were also affected as indicated by the significant decrease in the serum testosterone level and the significant lowering of the spermatogenic score count. Hence, the relation between the testicular morphology and its function was concluded; 34 the deteriorating effect of ribavirin on the function of the testes in this study was supported by the histological picture. Furthermore, a close relationship between spermatogenic score count, histologic structure, and the histometrics of the testes was determined. Ribavirin was considered to be an endocrine-disruptor in the rat. Although a very low level of testosterone in the testis is sufficient to maintain normal spermatogenesis, an immediate response to its decrease may be a decrease in parameters such as the number of advanced spermatids. In line with our observations, ribavirin was found to exert a cytotoxic effect in the testes after intraperitoneal administration and acts as a germ cell mutagen in rats. 35 Furthermore, ribavirin caused quantitative and qualitative alterations of spermatogenesis with DNA packaging abnormalities. 36
In this study, we focused on the effects of ribavirin on the structural organization of the PS and whether it could reflect the integrity of spermatogenesis. Control sections revealed a regular morphology of the components of the PS, namely, the BM, the myoid cells, and the surrounding ECM. After 1 week of ribavirin administration, there was no apparent change in the arrangement of these components. However, exposure to ribavirin for 4 weeks produced a significant increase in the total thickness of the PS together and obvious disturbance of the arrangement of its components.
The first component to be affected is the BM; there was marked thickening of the BMs, showed clearly in the PAS and Masson Trichrome–stained sections, with deposition of homogenous materials and either folding or detachment of many areas.
Changes in BM could result from increased synthesis and/or altered proteolysis of its components. In this study, two simultaneous observations revealed increased synthesis: the first is the excessive deposition of collagen IV that was observed within the BM in the immunostained sections and indicated an enhanced synthesis of new collagen which was not apparent in the control specimens or after 1 week of treatment. The second observation is the significant increase in the thickening of the PS including the BM after 4 weeks of ribavirin treatment compared to controls. The disturbed function of the tubules despite the thickening of their BMs revealed that the harmful effects of BM degradation were not excluded by the new synthesis of its components. The BM has a principal role in maintaining the functional and structural integrity of tissues; it provides physical stability of organs and sends signals to cells through the surface receptors. Altered structure of BM has been linked to the severe impairment of the testicular function. 37 The protein constituents of the BM include laminin, type IV collagen, various heparin sulfate proteoglycans, and ectatin/nidogen. The major constituent of mammalian BM is type IV collagen. This collagen is secreted by the myoid cells and Sertoli cells. Previous reports have established that external stimuli may encourage myoid cells to produce more collagen and accordingly, the ECM, which are accountable for the thickness of the BM. Therefore, it may change its appearance to irregular wavy multilaminar shape. 38
Our data could be explained by Kokeny et al. 39 and Gupta et al. 40 who showed that ribavirin administration modulated the expression of genes responsible for protein biosynthesis, translation, and transcription initiation. Thus, ribavirin could have the relative contributions of disturbed synthesis and turnover of components of BM that might lead to the development of the pathology in the seminiferous tubules.
However, the present results showed the existence of Casp-3 immunostaining within the spermatogenic cells and in the interstitial cells with varied intensities among groups. This localization is established by many authors Meena et al. 41 and Pilutin et al. 42 Apoptosis is present normally within the spermatogenic cells with sequential phases and synchronization linked by intercellular bridges. 43 The apoptotic activity increased after 4 weeks of treatment. Another possible effect of ribavirin on the structure of BM is the enhancement of apoptosis that could be involved in the degradation of its components. This possibility matched the previously recorded data and confirmed the strong inducing effect of ribavirin on apoptosis. Kokeny et al. 39 and D’Souza and Narayana 33 observed that the cytotoxicity of ribavirin was imparted on rapidly dividing target tissue where cells were removed by cell death somewhat similar to apoptosis.
The second component of the PS is the myoid cells. The morphological observations showed a normal appearance of the peritubular myoid cells in the control specimens. After 1 week of administration of ribavirin, myoid cells follow the minor irregularities in the BM; however, after 4 weeks, the structural alteration of the BM was associated with bulging of the myoid cell nuclei. The whole components of the PS appeared homogenous with no demarcations between the layers. The prominence of the myoid cell nuclei could be attributed to shrinkage of seminiferous tubules owing to the germ cell loss. The altered structure of myoid cells might follow the apoptotic cascade. After 4 weeks of ribavirin administration, there was a marked increase in the Casp-3 expression within the tubular tissues with affection of all germ cells. Similar results were found in the study of Liu et al. 22
Peritubular myoid cells maintain the morphology of the seminiferous tubules by connecting to Sertoli cells and participating in the formation of the BM. Their contraction was an effective means of sperm transportation and seminiferous tubule fluid flowing to the rete testis. 44 Besides, myoid cells provide nutrition for germ cell development by synthesizing and secreting the ECM; therefore, altering the function of these cells influence the spermatogenic function of the testes and the sperm transport. 22
The last component of the PS is the ECM. Microscopic and statistical analysis of the testes after 4 weeks of treatment revealed that ECM was disorganized by excessive collagen accumulation, namely, collagen I and collagen IV; the latter process being termed seminiferous tubule hyalinization. This was supported by the significant increase in the thickness of the PS. The affection of the ECM by exposure to ribavirin could be explained by the cell–ECM interactions. Cells respond to environmental changes through variations in ECM which is considered as an effective strategy to adjust their behaviors and maintain tissue integrity and function. 12
In fact, the structure and function of all components of the PS are intermixed. The interaction between myoid and Sertoli cells is essential for the formation of BM between these two cell populations. This preserves the integrity of the testis cords. 45 Additionally, interruption of the cell–matrix adhesion between Sertoli cells and BM may influence apoptosis of Sertoli cells and atypically synthesized BM. In turn, damage to BM could affect the interaction of Sertoli cells and spermatogonia with BM such that their viability and function are compromised. 46 As well, BM’s defect could result in altered parameters of the seminiferous tubules and widening of the intertubular spaces. 47
Interestingly, the present data revealed a significant correlation between the spermatogenic score count and the measured thickness of the PS in the control as well as the experimental groups. This supported our suggestion that the deteriorating effect of ribavirin on the structure and function of the seminiferous tubules could exist through the impairment of the components of the peritubular tissues, namely, BM, myoid cells, and ECM. Generally, some authors accepted the relation between the impaired spermatogenesis and the morphological alterations of the lamina propria of the seminiferous tubules.48,49
We concluded that ribavirin possesses ameliorating effects on the testicular function and organization, and this could be attributed to the structural changes in the components of the PS precisely: BM, myoid cells, and ECM.
Footnotes
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
