Abstract
Background:
Malnutrition remains a public health burden in the Philippines, with the country struggling to meet global nutrition targets.
Objective:
This study aims to review the Philippine Plan of Action for Nutrition (PPAN) and its progress in addressing malnutrition in the Philippines.
Methods:
A narrative literature review of the PPAN and its implementation from 1974 to 2022 was conducted, including an analysis of relevant data on the nutrition status and programs for Filipinos.
Results:
The study found that the PPAN has been largely supportive in addressing malnutrition in the Philippines over the years. However, obstacles hindering the achievement of its nutrition-related goals have been identified. Challenges include inadequate coordination of programs at the local level, concerns regarding data quality, and insufficient training of personnel involved in implementing the PPAN. The results also indicate that the country has made limited progress toward achieving the global nutrition targets set by the Sustainable Development Goals 2030.
Conclusion:
This study highlights the need to revisit and refine the PPAN to respond to the changing nature of malnutrition in the country. Recommendations to address the remaining gaps in the planning, implementing, and monitoring of the PPAN are discussed. Finally, the paper offers some valuable insights from the experiences of the PPAN that can be applied to other countries facing comparable nutrition contexts.
Plain language title
Understanding the Evolution of the Philippine Plan of Action for Nutrition
Plain language summary
This study is a review of the Philippine Plan of Action for Nutrition (PPAN), which is a comprehensive plan initiated in 1974 to address nutritional issues in the Philippines. The study looks at how the PPAN has been implemented over the years and its effectiveness in addressing malnutrition. It also discusses challenges and issues with the PPAN, such as compliance problems at the village level, and the need for stronger political will and context-specific approaches. Additionally, the study provides recommendations for the next iterations of the PPAN in order to achieve sustainable nutrition outcomes, as well as lessons learned for other countries facing similar nutrition problems. Overall, this study highlights the need to reexamine and adapt the PPAN in order to effectively address the changing nature of malnutrition in the Philippines.
Introduction
Malnutrition is defined as a lack of proper nutrient and energy intake in the body. 1 It can manifest as undernutrition, characterized by wasting, stunting, underweight, and micronutrient deficiencies, or overnutrition, which leads to overweight and obesity and increases in the risk of health problems. These conditions are often made worse by poverty, disease, conflict, and natural disasters and affect millions of people globally. Addressing malnutrition in all its forms remains an ongoing challenge for any country, requiring concerted efforts and targeted interventions. There is widespread recognition that multisectoral policy approaches and proper nutrition governance can affect positive nutrition outcomes. 2
In the Philippines, malnutrition continues to present a substantial public health challenge. Since 1974, nutrition has been a priority in the country, resulting in the creation of the Philippine Plan of Action for Nutrition (PPAN), its premier blueprint for integrated nutrition programs. 3 Through this framework, several programs and interventions have been implemented that aim to address key nutrition targets and priorities. However, numerous gaps and challenges prevail, thwarting the country’s progress toward attaining its envisioned nutrition outcomes. For almost half a century, the nation has encountered relentless difficulties tackling nutrition-related issues, including stunting, undernutrition, and micronutrient deficiencies. Data from the World Bank shows little improvement, with 1 in 3 children suffering from stunting, 38% of infants 6 to 11 months old, and 26% of children 12 to 23 months old having micronutrient deficiencies, and 20% of pregnant mothers being anemic. 4 The latest Global Nutrition Report also indicates the country is making slow progress toward achieving global nutrition targets, especially concerning malnutrition in children younger than 5 years. 5 While there has been a slight decrease in indicators for undernutrition, it is not sufficient to meet the targets set by the sustainable development goals (SDGs) by 2030. 6 There is also the increasing prevalence of overweight individuals, as evidenced by a rise in fasting blood glucose levels from 3.4% in 2003 to 5.6% in 2015 and 7.6% in 2018. 7
Thus, there is a need to examine the PPAN from its earliest roots until its present adaptation to be cognizant of its development and the strategies used to implement its health programs. Specifically, this review has the following objectives: To examine the current status of malnutrition in the Philippines and the effectiveness of the PPAN in addressing it. To identify gaps and challenges in the implementation of the PPAN and its programs in addressing malnutrition in the Philippines. To propose viable and effective recommendations for future recalibrations of the PPAN.
This information can be useful for policymakers, health care professionals, and researchers to understand the current situation, identify the areas that need improvement, and develop and implement more effective strategies to combat malnutrition in the Philippines.
Methods
The search strategy for this review involved retrieving the PPAN documents published online by the National Nutrition Council (NNC) of the Philippines, as well as the latest available nutrition survey data from the Food and Nutrition Research Institute (FNRI). An electronic search was also conducted in various databases, including PubMed, Scopus, Google Scholar, EMBASE, and Web of Science, to identify relevant literature. Studies published between 1974 and 2022, regardless of design, were considered. Relevant reports, recordings of senate hearings, and video presentations from national and international agency partners such as the World Health Organization, United Nations, and Emergency Nutrition Network have also been included. The data range was purposely wide to capture the historical and developmental aspects of the PPAN. The search for literature was specific to nutrition health outcomes, programs, and strategies, and only those published in English and Filipino were included.
Results
Early Beginnings of the PPAN
Nutritional status is a key indicator of a population’s health. Following World War II, the Philippine government centralized nutrition efforts through the establishment of the Philippine Institute of Nutrition (now known as the Food and Nutrition Research Institute) and various nutrition initiatives managed by the National Coordinating Council on Food and Nutrition. However, these efforts lacked clear policy, coordination, and coverage. In recognition of the need for a central body to coordinate all nutrition activities of the government and private sector, the NNC was created via Presidential Decree (PD) No. 491 on June 25, 1974. 8 It was composed of representatives from various government agencies, entrusted with overseeing 4 main intervention schemes: food production, food assistance, health protection, and nutrition information and education (Table 1). The same Presidential Decree also established the Philippine Nutrition Program, the precursor of the PPAN, which targeted vulnerable groups such as infants and preschoolers (0-6 years old), school children (7-14 years), pregnant women and lactating mothers, heavy manual laborers, and those afflicted with nutrient deficiency diseases. 9
Summary of Main Goals/Objectives, Intervention Schemes/Health Programs, and Enabling/Facilitating Mechanisms of the Philippine Plan of Action for Nutrition From 1974 to 2022.

The Food Production scheme centered its efforts on implementing small-scale initiatives to cultivate food in residential spaces, such as backyards, schoolyards, and community gardens, with a particular focus on households harboring underweight preschoolers. Within the Food Assistance scheme, the primary objective revolved around facilitating weight recovery among underweight preschoolers and schoolchildren while simultaneously providing essential support to pregnant and lactating women to meet their energy requirements. Under the purview of Health Protection, the growth patterns of children were meticulously monitored, while activities aimed at promoting breastfeeding, immunization, and other health-related measures were actively encouraged. Meanwhile, the Nutrition Information and Education scheme targeted parents, farmers, and at-risk farm families, aiming to disseminate crucial knowledge and foster a comprehensive understanding of the significance of proper nutrition. However, the efficacy of these endeavors was hampered by the dearth of adequately trained health care personnel, particularly in remote regions of the country, consequently impeding the comprehensive coverage of these vital activities. 9
National nutrition surveys conducted by the FNRI at this time indicated a notable reduction in the prevalence of underweight preschoolers. Specifically, the prevalence rate declined from 21.9% in 1978 to 17.2% in 1982. 14 However, the subsequent years spanning from 1983 to 1985 witnessed a setback in the efforts to enhance nutritional status due to formidable economic challenges. The Philippines encountered an unemployment crisis and severe recession, with rising debt levels and a troubling poverty incidence of 44.2%. 15 These economic challenges had far-reaching consequences for the well-being of the population, including the nutrition situation. As a result, the prevalence rate of underweight preschoolers increased to 17.7% by 1987. With the gradual recovery of the economy, there was a marked improvement in the nutrition situation, as evidenced by a decrease once again in the prevalence rate to 14% by 1990. 14 Unfortunately, the sustained progress achieved during that period was not maintained in subsequent years, as indicated by the latest national nutrition survey conducted by the FNRI in 2019. The survey reported that underweight prevalence among preschoolers remains at 19.1%, with medium severity according to the global cutoff for public health significance. 10
Philippine Plan of Action for Nutrition 1993 to 1998
The first publication of the PPAN, also known as the Medium-Term Philippine Food and Nutrition Plan for the period of 1993 to 1998, was released in the early 1990s. As a component of the Philippines 2000 initiative, it sought to enhance the quality of life for Filipinos, with the ultimate objective of achieving a Nutritionally Improved Country (NIChood) by the year 2000. At the time of its formulation, the Philippines continued to face significant challenges related to malnutrition, necessitating the development of the PPAN to address this pressing issue through improved policies and interagency coordination. The 4 main target outcomes were to reduce malnutrition levels, improve food security, improve mental performance, and increase productivity. To achieve these outcomes, the PPAN incorporated 5 major impact programs and 5 enabling mechanisms (Table 1).
The Home and Community Production program involved setting up home and school gardens using biointensive gardening technology that focused on soil quality to achieve maximum yields from a limited amount of land. 16 This program also included small animal raising and aquaculture, which sought to increase the household supply of calories, proteins, vitamins, and minerals such as vitamins A, C, and iron. By generating surplus produce for families to sell, the program also aimed to improve household food security. In 1993, the Fourth National Nutrition Survey indicated that 35.3% of 6-month to 6-year-old children exhibited deficient to low serum retinol levels, and subclinical vitamin A deficiency was a significant public health concern in 11 out of 15 regions in the country. 17 In response to these findings, the Micronutrient Supplementation and Food Fortification program was launched to address deficiencies in Vitamin A, iodine, and iron. This involved fortifying common foods such as rice, margarine, flour, and salt, in collaboration with food producers who received tax incentives to import fortificants. 18 Figure 1 illustrates the trajectory of results pertaining to anemia and vitamin A deficiency since the launch of this program, revealing positive outcomes, albeit further progress is required to meet global public health goals.
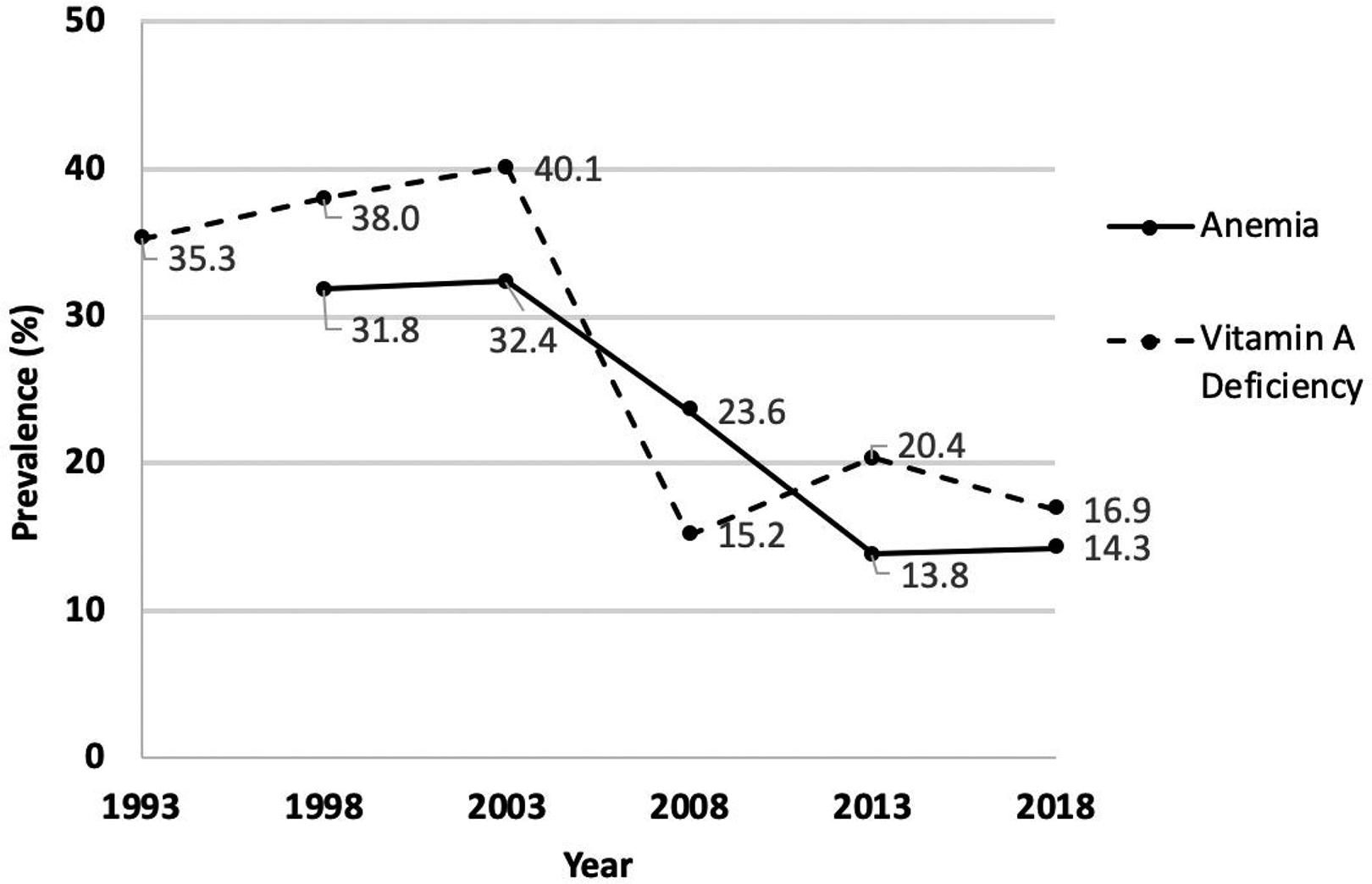
Trends in anemia and vitamin A deficiency among children, 6 months to 5 years old in the Philippines from 1993 to 2018 (Adapted from: FNRI’s 2018 Expanded National Nutrition Survey). 19
Another effort to target malnutrition resulting from poverty was the Credit Assistance for Livelihood initiative. It focused on facilitating credit access and offering livelihood opportunities to small businesses, with the objective of empowering individuals and communities to address persistent food shortages and long-term nutritional issues. In terms of promoting healthy food and feeding practices, the Nutrition Education program was promulgated to encourage the consumption of nutrient-dense foods and exclusive breastfeeding during the first 6 months of life. Given the epidemiological shift in the country during this period, it was important to focus on healthy lifestyle to address both prevalent malnutrition and emerging issues of overweight and diet-related diseases. While a generally decreasing trend was observed in preschool underweight prevalence, echoing similar patterns observed in neighboring Asian countries like Thailand, Myanmar, Indonesia, and Malaysia, the rate of improvement in the Philippines was relatively slow. 20 Within the Asia-Pacific region alone, a double burden of malnutrition persisted, aggravated by an upward price trend that led to food insecurity. 2 Evidence suggests that these price increases had a detrimental impact on children’s nutrition, particularly among girls and those residing in low-income households. 21 Hence, the Association of Southeast Asian Nations (ASEAN) has been integrating various strategies to promote healthy lifestyles and address food and nutrition security. A need for greater regional collaboration in maternal, neonatal, and child health was also warranted. This growing recognition underscored the potential of concerted efforts and cooperation among ASEAN member countries in addressing the unique challenges and improving the overall health outcomes of vulnerable populations. 22 The culmination of these efforts led to the official establishment of the ASEAN Community in 2015, with the overarching goal of attaining food and nutrition security at national and regional levels, thus contributing to the realization of a Healthy ASEAN. 11 This objective was pursued through the implementation of targeted advocacies, effective mechanisms, and collaborative health initiatives. Cooperation with ASEAN Dialogue Partners, external entities, and stakeholders played an important role in reinforcing the significance of promoting a healthy population as a catalyst for robust economic growth among ASEAN member states. The Community regularly convenes to stay updated and produce reports that provide valuable references for shaping and advancing ASEAN health cooperation in the field of nutrition. 22
The final impact program of this PPAN, Food Assistance, was designed to serve as a social safety net for nutritionally vulnerable groups during periods of food scarcity. This encompassed regular supplementary feeding schemes, food discount schemes, and timely disaster relief operations in times of displacement. On the other hand, enabling mechanisms were developed to ensure the successful implementation of these health programs. These mechanisms focused on building capacity through Manpower Development, promoting nutrition-related bills or local ordinances through Nutrition Advocacy, and generating resources through Planning, Management, Coordination, and Surveillance. Local government units were the main supporters of the PPAN and were responsible for its local implementation, while the international community was engaged in technical guidance and financial support. Due to its multisectoral nature, the NNC provided overall policy direction and coordination for planning, executing, managing, monitoring, and evaluating the PPAN. 14
Philippine Plan of Action for Nutrition 1999 to 2004
The next PPAN, which covered the years 1999 to 2004, served as a component of the Philippines’ social reform and development chapter. It aimed to maintain the successes of prior strategies and reinforce those that were found to be effective but fell behind in addressing nutritional issues. This PPAN placed specific emphasis on chronic energy deficiency, low birthweight, overweight, and iron deficiency anemia, not only among children, pregnant, and lactating women but also other affected groups such as adolescents, adults, and older persons. It became an integral part of the 2025 long-term Philippine National Development Plan Directions for the 21st Century, or Plan 21. 20 The impact programs and enabling mechanisms from the previous PPAN continued to be implemented, with the exception that “Resource Generation and Mobilization” was merged under “Overall Planning Coordination, Monitoring, and Surveillance” initiative (Table 1).
According to the 6th National Nutrition Survey, undernutrition decreased among various age groups of children during this period. 23 Considerable efforts were also directed toward iodine supplementation, resulting in a reduction in iodine deficiency disorders among 6 to 12-year-olds from 35.8% in 1998 to 11.4% by 2003. 24 However, due to limitations in the sample population size, the analysis of regional prevalence was inconclusive; making it challenging to draw definitive conclusions regarding changes in specific regions. Similarly, protein-energy malnutrition (PEM) and other deficiencies continue to affect a substantial proportion of the population, while nutrition-related degenerative diseases, including diabetes mellitus and cardiovascular disorders, emerged as significant causes of morbidity and mortality. Among adults, 12.3% exhibited chronic energy deficiency, while 23.9% were classified as overweight or obese. Anemia remained a public health concern among pregnant and lactating women, with prevalence rates of 43.9% and 42.2%, respectively. 23 Based on these results, efforts were undertaken to maintain successful programs while also addressing those which lagged behind. For example, the Food Assistance and Nutrition Education programs proved to be more complex and required ongoing support. There was a need to enhance collaboration among stakeholders to strengthen and standardize the knowledge and practices of key implementers of nutrition interventions. In addition, a study found that Behavior Change Communication at this time lacked a comprehensive conceptual framework as a unified communication program, and nutrition education activities were typically conducted as isolated initiatives by different agencies. 25
A number of factors may have contributed to some of the gains in health outcomes during this period. One possibility is the implementation of Republic Act No. 8172, or the “Asin (English:Salt) Law,” which promoted nationwide salt iodization and related purposes in December 1995. 12 Another potential factor is the effect of strengthening the National Nutrition Program through the Accelerate Nutrition Improvement (ANI) Act, which mandated the fortification of processed foods, nutrition labeling, and modernization of school health and nutrition. 26 Furthermore, the 9-point Nutrition Action Agenda was adopted to create a more conducive environment for nutrition, and the NNC Network was organized following the country’s commitment to embracing a devolved health care system as enshrined in the Alma Ata Declaration of 1978. 13 Other programs implemented concurrently, such as the Sangkap Pinoy (English:Filipino Ingredients) Seal 27 and the Barangay (English:Village) Integrated Development Approach for Nutrition Improvement for the Rural Poor, 28 were also key in reducing malnutrition prevalence. However, some initiatives were not as successful, such as the Enhanced Retail Access for the Poor Sari-Sari Store, which saw better access in urban areas than rural areas and a large proportion of patrons coming from middle-income and rich families instead of the poor. 29
Philippine Plan of Action for Nutrition 2005 to 2010
At the turn of the century, the Philippines made a commitment to eradicate hunger and malnutrition by 2015, as outlined in the subsequent PPAN spanning from 2005 to 2010. This pledge was made in alignment with the global health goals established under the Millennium Development Goals (MDGs), a set of 8 objectives unanimously agreed upon by member countries in September 2000. 30 This particular PPAN served as a guide for local and national policymakers and program planners to promote healthy eating, address existing nutritional issues, and enhance the quality of life for Filipinos through greater nutrition, better health, and increased productivity. It also followed the agenda of the Philippine President at the time, prioritizing regions with high rates of hunger and poverty, and emphasizing the community’s responsibility in ensuring the right to food and nutrition for their members. 31
Table 1 shows that this new PPAN underwent several changes in its health programs, including the addition of new programs and the renaming of previous ones into component programs. A new program called Nutrition in Essential Maternal and Child Health Services was added to reach vulnerable groups nationwide. Moreover, in accordance with Presidential Decree 1569, community-based volunteer workers called barangay nutrition scholars (BNS) continued to offer basic nutrition services to the communities. For instance, BNS continued to weigh all preschoolers to identify those who were underweight, and connect the families of malnourished children to local service providers and nutrition facilities. 32 Monitoring systems at the local level, such as Operation Timbang (English:Weight) (OPT) and the BNS’s Family Survey, were conducted annually to generate information vital for local nutrition assessment and planning. 33 Assisted by the Municipal Nutrition Action Officers (MNAO), regular assessments were conducted to evaluate the progress of program implementation and provide technical assistance. The MNAOs also supervised the nutrition committees in all barangays and were an important resource during planning activities. Nutrition Month, celebrated every July, likewise served as a platform for national efforts of health promotion and education to reach a wider audience. These advocacy campaigns continue to be widely observed in schools, communities, and workplaces.
Considering that the country’s population growth rate remained one of the highest in Asia, significant public health implications may arise from the persistent burden of undernutrition in a given population, particularly among vulnerable young children. Analysis from the 2008 National Nutrition Survey revealed that although a notable decrease in the prevalence of underweight-for-age among children younger than 5 years can be noted since 1990, the overall decline fell short of the desired pace, with an average annual percentage point reduction of 0.37, below the targeted 0.55 annual percentage point decrease from 2000, as outlined in the MDG 1. 34 Besides, the occurrence of natural disasters such as the eruption of Mt. Mayon in 2006, and the typhoons Ketsana and Parma in late 2009 worsened the situation by displacing already food-insecure populations. 35,36 The resulting displacement, loss of homes, property, and livelihoods, coupled with the detrimental impact of disasters on agricultural production and incomes, further heightened the risk of increased hunger incidence. Ongoing coordination and partnerships with local foundations and international organizations, including the United Nations Children’s Fund (UNICEF), World Health Organization (WHO), and Food and Agriculture Organization (FAO), remained crucial for effective rebuilding, program administration, and the improvement of nutritional outcomes among the target populations. 24
Philippine Plan of Action for Nutrition 2011 to 2016
In continuation of the commitment to achieve the MDGs, the PPAN 2011 to 2016’s overall goal was to improve the quality of the country’s human resource base and to substantially decrease child and maternal mortality. 34 It aimed to enhance the well-being of all Filipinos by promoting fair and equal access to sufficient and high-quality social services and resources. Subsequently, previous health programs and enabling mechanisms were either added to or changed to achieve the nutrition outcomes based on priorities of action (Table 1). The PPAN also aimed to address maladaptive nutrition and promote interventions such as enforcing the Milk Code, setting up human milk banks, and promoting exclusive breastfeeding. 37 Enacted in 1986, the Philippine Milk Code (Executive Order [EO] 51) set out to provide safe and adequate nutrition by (1) protecting and promoting breastfeeding and (2) regulating the marketing of breastmilk substitutes, breastmilk supplements, and other related products. According to the Global Nutrition Report, the Philippines is “on course” for the exclusive breastfeeding target, with 54.9% of infants aged 0 to 5 months exclusively breastfed. 5 Some advancements were also made in reducing anemia among women of reproductive age, with 12.3% affected.
Despite these efforts, the Philippines still faced impactful issues with malnutrition at this time, especially in the Luzon and Visayas regions. In particular, the Bicol province had the highest percentage of stunted children (39.8%), while Mindoro, Marinduque, Romblon, and Palawan had the highest number of preschool children who were underweight (27.5%) and wasted (9.8%). 38 Among households with migrant mothers, a lower proportion of children were found to be exclusively breastfed compared to those from nonmigrant households, and these children experienced an earlier introduction to milk substitutes as well. 7 Challenges also persisted in achieving the target for stunting, as 30% of children younger than 5 years of age were still affected, surpassing rates observed in surrounding ASEAN countries like Thailand, Malaysia, Vietnam, and Brunei. 22 In conjunction, the prevalence of wasting in the Philippines has shown a consistent upward trend, increasing from 6% in 2003 to 7.9% in 2013, which is classified as “poor” according to the WHO Crisis Classification. 38
As a response to the constant challenge of malnutrition in the Philippines, a range of additional measures were implemented to address the issue comprehensively. These measures included a referral system for cases of acute malnutrition with infections, provision of iron-folic acid supplements, and continued implementation of the Essential Health Care Program (EHCP). 34 The EHCP focused on various aspects of health promotion, such as promoting cleanliness and hygiene, conducting biannual deworming, and enforcing policies regulating the sale of unhealthy food and drinks in schools. Recognizing the importance of physical activity, infrastructure enhancements were undertaken by the government to facilitate active lifestyles. This involved the installation of walking, running, and bicycle lanes to promote regular exercise and reduce sedentary behavior among the population. Efforts were also underway to strengthen the monitoring and evaluation of the Philippine Food and Nutrition Surveillance System by incorporating early warning mechanisms. 34 This proactive approach would enable the identification of specific regions or areas at risk of worsening nutritional situations, hence facilitating prompt interventions and targeted support. A study by Ignacio and Bullecer 39 in 2016 underlined the participatory approaches and appreciative inquiry processes in the conduct of nutrition programs in communities located in Ifugao, Bulacan, and Siquijor. This research further emphasized the importance of community engagement and involvement to effectively implement the PPAN at the grassroots level.
Philippine Plan of Action for Nutrition 2017 to 2022
The latest PPAN was specifically designed to align with the Philippine Development Plan 2017–2022 and to support the “Health for All” pillars established by the Philippine Department of Health. It reaffirms the nation’s commitment to nutrition to the international community, as articulated in the 2030 SDGs that superseded the MDGs. The main goals of this PPAN were to improve the nation’s nutritional status in order to help attain Ambisyon (English:Ambition) 2040 by strengthening its human resource base, lessening inequity in human development outcomes, and lowering child and maternal mortality. 40 Following evaluations of previous iterations of the PPAN, a transformation of the nutrition strategies and initiatives took place, leading to the introduction of new categories, namely: nutrition-specific, nutrition-sensitive, and nutrition-supportive programs (Table 1). Nutrition-specific programs were implemented to directly tackle the immediate determinants of malnutrition. For example, the Infant and Young Child Feeding program focused on promoting optimal feeding practices during the critical stages of early childhood. Likewise, the Overweight and Obesity Management and Prevention Program sought to address the emerging issue of excessive weight gain among certain population segments. 40 In contrast, nutrition-sensitive projects were designed to address the underlying causes of malnutrition, which extend beyond the direct nutritional aspects. For instance, the Coconut Rehabilitation Program targeted improving food security and agricultural productivity, particularly in areas where coconut farming plays a pivotal role in the local economy. 41 Whereas, the implementation of Diskwento (English:Discount) Caravans in depressed areas aimed to enhance access to affordable food options, thereby improving food availability and reducing food insecurity. 42
This recent PPAN places emphasis on the first 1000 days of life, with particular attention given to reaching geographically isolated and disadvantaged areas, as well as indigenous populations. Efforts were also made to identify priority areas for resource allocation and interventions while ensuring that other regions in the country are not neglected. The development of the PPAN benefited from extensive consultations with various sectors at both the national and subnational levels, which helped strengthen its effectiveness and relevance. A situation analysis supported by Nutrition International also identified key entry points for multisectoral engagement within the PPAN framework. 43 The Expanded National Nutrition Survey conducted in 2019 provided valuable perspectives into the nutrition landscape of the country, revealing a modest reduction in stunting and a significant reduction in wasting compared to the findings of the 2015 nutrition survey. 10,44 In January 2018, a tax on sweetened beverages was imposed by the Philippine government to curb the burden of obesity, 45 with initial evaluations suggesting that such an effort is likely to be effective. 46
However, the gains achieved were yet again short-lived as the advent of the COVID-19 pandemic in 2020 disrupted food systems globally. Ong and colleagues 47 evaluated commonly distributed food aid during the pandemic and found that while it addressed acute hunger, it lacked sufficient nutrients to support and maintain optimal health. This deficiency is particularly concerning for vulnerable populations, including women and children, as well as the indigent, who face an increased risk of involuntary hunger. Similar findings have been reported by Lasco and colleagues, 48 who found that the economic and financial repercussions of the pandemic had a detrimental impact on overall nutrition and food sources among island community members. Between December 2019 and May 2020, hunger rates in the Philippines nearly doubled from 8.8% to 16.7% and reached 30.7% by September 2020. 49 The average hunger rate for the full-year 2020 was a new record 21.1% of families, surpassing the previous record of 19.9% in 2011 and 2012, and is double the average of 9.3% prior to the pandemic in 2019. 50
In terms of PPAN implementation, an external formative evaluation identified persistent challenges. 51 One of these was the widespread misconception about stunting among community members, village implementers, health care workers, and local chief executives that resulted in misguided actions to address the issue. A noticeable disconnect was also observed between higher level policy directives and their slow dissemination and implementation at lower levels. The evaluation further found inconsistencies in fidelity and compliance levels of intervention implementation, with issues related to governance, funding, management, and human resources plaguing nutrition planning and implementation. Similarly, data quality issues were identified with OPT Plus, the primary monitoring and evaluation tool used to track malnourished children at the village level. 51 With scholars arguing that the Philippines is now experiencing a triple burden of malnutrition together with other countries in East Asia and the Pacific, 52,53 eliminating such bottlenecks is imperative so that citizens reach their full physical growth and development potential, and actively contribute to equitable prosperity and the sustainable development of their communities. At present, the outcome targets of the PPAN 2017 to 2022 pertain to the final outcomes from which the plan’s success will be measured (Table 2). Whether these goals have been achieved remains to be seen in subsequent national nutrition surveys and reports moving forward.
Outcome Targets of the PPAN 2017 to 2022. 40
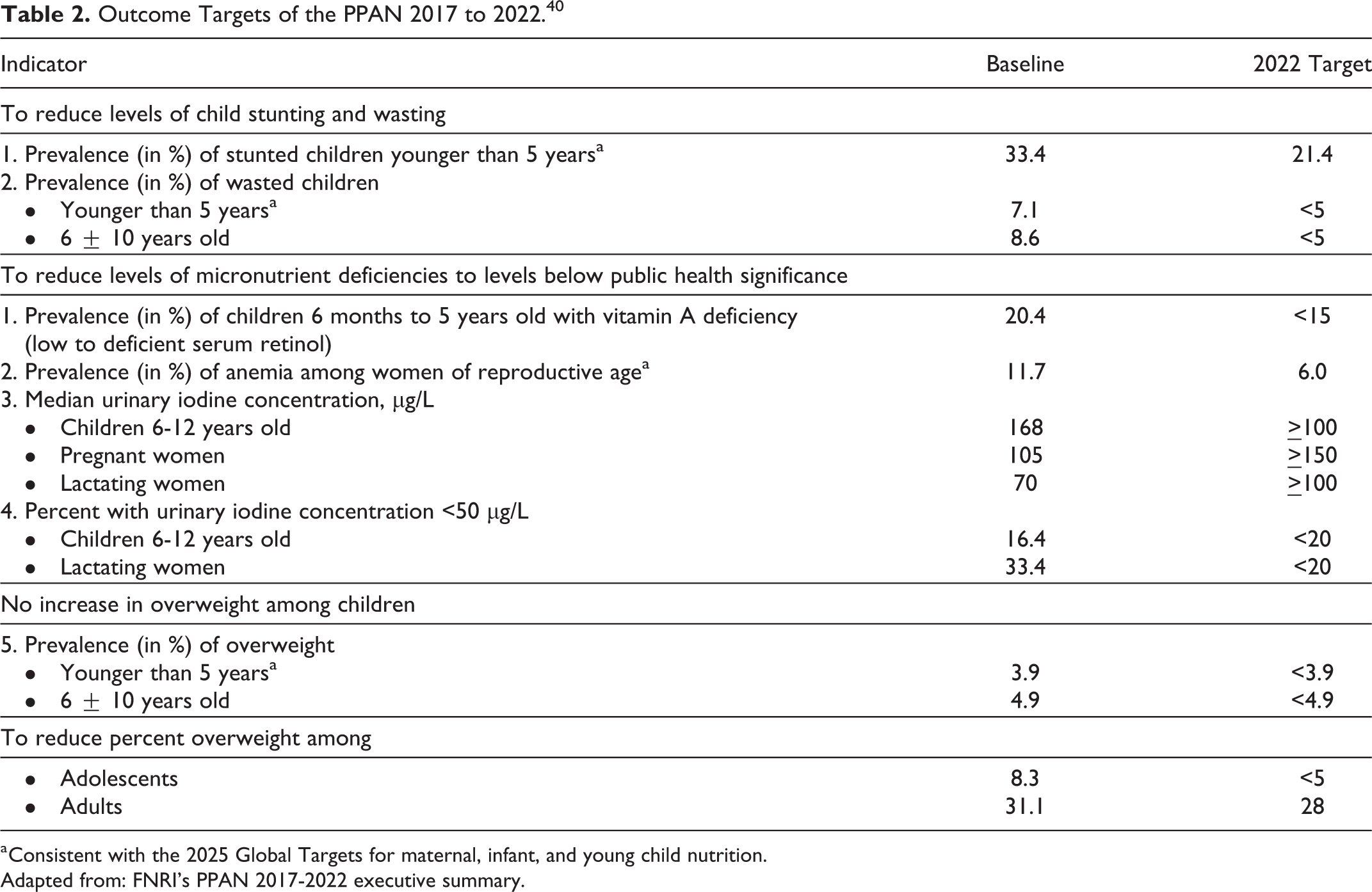
a Consistent with the 2025 Global Targets for maternal, infant, and young child nutrition.
Adapted from: FNRI’s PPAN 2017-2022 executive summary.
Discussion
For decades, the Philippines has been steadfastly committed to resolving nutrition problems in the country. The creation of the PPAN is a testament to its unceasing perseverance to formulate and implement evidence-based strategies to improve the nutritional outcomes of Filipinos. The strengths inherent in the evolution of this framework are manifold. First, it demonstrated a recognition of the necessity for a centralized coordinating body to facilitate all nutrition-related activities conducted by the government and private sector. This step indicated an acknowledgment of the need for improved policy formulation, coordination, and coverage. Second, the PPAN endeavored to target vulnerable groups, including infants, preschoolers, school children, pregnant women, lactating mothers, and individuals afflicted with nutrient deficiency diseases. The desired outcomes encompassed reducing malnutrition levels, enhancing food security, improving cognitive function, and increasing productivity. These objectives manifested an awareness of specific population groups and outcomes warranting attention. Third, the PPAN embraced a multisectoral approach by involving representatives from diverse government agencies, private sector organizations, and international partners. Enabling mechanisms were devised to ensure the effective implementation of health programs, including capacity building, nutrition advocacy, planning, management, coordination, and surveillance. These approaches acknowledged the importance of collaboration and resource mobilization for the successful execution of policies.
Fourth, the PPAN aligned with broader national development plans and global commitments, such as the Philippines 2000 initiative, the MDGs, and the SDGs. This integration guaranteed that nutrition goals were integrated within larger developmental frameworks, emphasizing their significance for overall human development and well-being. Fifth, regular national nutrition surveys were conducted to monitor health outcomes and inform policy formulation. These surveys furnished critical data on the prevalence of malnutrition, rates of anemia, and other nutritional indicators, which guided the development and adjustment of strategies under the PPAN. Sixth, the PPAN evolved over time to address emerging issues and adapt strategies in response to the evolving health landscape. For instance, as the epidemiological landscape shifted within the country, the focus broadened from prevalent malnutrition to encompass emerging concerns related to overnutrition and diet-related diseases. The strategies were consequently modified to encompass a broader range of nutritional challenges. Seventh, successful programs from previous iterations of the PPAN were preserved and refined in subsequent plans. Initiatives such as home and community food production, micronutrient supplementation and food fortification, and credit assistance for livelihood were sustained and expanded based on their efficacy in addressing malnutrition. Eighth, policy reforms and legislative measures, such as the “Salt Law” promoting salt iodization and the ANI Act mandating the fortification of processed foods, played pivotal parts in improving nutrition outcomes. These measures established a more conducive environment for nutrition and provided regulatory frameworks for addressing nutritional concerns. Observing nutrition month every July has also shown to be an effective approach to raising awareness about proper nutrition throughout the country.
In spite of these efforts and various initiatives, malnutrition unfortunately remains a significant public health burden in the Philippines. For example, rates of stunting still fall short of the 2030 SDG target, which requires a 2.5 percentage point decrease per year. 54 The implementation of PPAN health programs has also been hindered by issues such as data manipulation, health misconceptions, and a disconnect between higher level nutrition actors and barangay frontline implementers. 51 Data quality issues are a critical problem as this can lead to under or overreporting of data from health program strategies that impact how the population’s nutritional status is reflected in reports, how resources are allocated, and how policies are developed. 55 The Philippines ranks 69th out of 121 countries in terms of hunger, according to the 2022 Global Hunger Index. 56 Even with an overall decline in the number of families experiencing starvation since 2000, many Filipinos still face challenges in accessing food due to poverty and low income, especially in rural areas. 55 Factors such as rising food and nonfood prices, underemployment, and frequent natural and human-induced disasters contribute to this vulnerability. In fact, the World Risk Index places the Philippines as the number one most at-risk country for disasters, with a score of 46.82. 57 Due to its geographical location within the Pacific Ring of Fire, the country is inherently exposed to a heightened risk of natural disasters and calamities, which amplifies the likelihood of hunger and further burdens already food-insecure populations. The COVID-19 pandemic has also exacerbated the situation by damaging the economy and public health system, and by hindering progress made by previous PPANs due to lockdowns and the low nutritional value of food aid distributed. 47,48 Consequently, it becomes imperative to establish comprehensive policies and strategies aimed at effective disaster risk management in order to address these pressing concerns as well.
However, it should not be discounted that the underlying causes of malnutrition are complex and multifaceted and are influenced by the Social Determinants of Health, such as access to markets, education, and social protection, as well as factors such as transportation, employment, agriculture, food systems, and political stability. 58 According to the 2011 Updating Survey on National Nutrition, factors such as having more than 2 children in a household and short birth intervals of less than 2 years between children were associated with stunting. 59 The observed changes in nutrition outcomes cannot also be exclusively ascribed to the PPAN as these could be influenced by other factors, such as secular changes and broader socioeconomic developments. For instance, advancements in health care, access to education, and improved sanitation and hygiene practices in the Philippines have so far led to promising nutrition results. 60,61 Although the country is still classified as lower middle-income by the World Bank, poverty rates have decreased compared to previous decades. National strategies like the Pantawid Pamilyang Pilipino Program (4Ps) (English:Bridging Program for the Filipino Family) were introduced to eradicate extreme poverty to improve child health and nutrition with better access to nutritious food and improved living conditions. 62
Avenues for Recalibration of Future PPANs
Based on the results of this review, the following pathways can be considered for future iterations in PPAN development:
Strengthening coordination and good governance. Recognizing that stunting is not only a measure of development but also a reflection of the quality of governance, efforts should be made to enhance coordination and governance structures.
63
This can be achieved by establishing clear lines of authority, improving communication channels, and strengthening the multisectoral approach to nutrition planning and implementation. Amendments to PD 491 (Nutrition Act of the Philippines) and EO 234 (Reorganizing the NNC) can be made to update the functions and policies of the NNC in this new era.
Addressing implementation gaps. Comprehensive evaluations, both internal and external, should be conducted to assess the effectiveness of various interventions. Identifying bottlenecks in service delivery and developing strategies to overcome barriers to implementation are essential. Continued research, along with the development of innovative solutions and the promotion of evidence-based intervention models, can also be prime drivers in achieving the PPAN goals. The focus should be on improving the coverage, quality, and sustainability of nutrition interventions across different regions and population groups.
Sustaining political will to support human resource capacity. Investments in training and capacity-building initiatives should be more substantial to enhance the knowledge and skills of health care personnel, particularly in remote regions with a shortage of adequately trained professionals. Supporting and incentivizing BNSs through amendments in policies, such as PD 1569 (Barangay Nutrition Program Law) is crucial to ensure their effectiveness in frontline roles.
Enhancing local executive and community participation and ownership. One of the biggest challenges in the sustainability of nutrition programs is the change in administration, wherein newly elected officials may not prioritize or continue the nutrition programs implemented by their predecessors.
64
While the PPAN represents an enduring national commitment, it is important to continuously advocate for the long-term benefits of nutrition programs to local executives. Thus, consistent efforts should be made to convince them about the significance of prioritizing nutrition in their local agendas. This approach will help bridge any potential gaps between national and local priorities, thereby reinforcing the extended impact of nutrition programs and securing their continued support. Empowering communities and promoting their participation in nutrition programs through involvement in planning, implementation, and monitoring is also essential in fostering ownership and accountability.
Improving data collection and monitoring systems. Ongoing investments should also be made in appropriate and easy-to-operate instruments for data collection. Enhancing the capacity of health information systems to collect and analyze nutrition-related data is necessary. Ensuring the availability of accurate and timely data on nutritional status, and establishing mechanisms for regular monitoring and reporting of program indicators are critical for informed policy decisions.
Adapting to emerging and reemerging nutrition challenges. As the Philippines is one of several countries tackling the triple burden of malnutrition, effectively addressing these nutrition challenges requires a comprehensive strategy. This strategy should encompass more effective disaster risk management strategies to mitigate the impact of calamities and pandemics, and sustain the gains from nutrition initiatives. The strategy should also incorporate and consider the unique needs of specific population groups across all life stages. In combating misinformation or misconceptions about nutrition, employing more nuanced health communication techniques becomes paramount. Recognizing that nutritional requirements differ among men and women, various generations, and different occupations, the forthcoming PPAN should consider refining future programs and policies by considering these key factors. By proactively identifying and adapting to these evolving challenges, nutrition initiatives can ensure a resilient and robust response to safeguard the nutritional well-being of the population.
Learning from best practices and international experiences in nutrition. Drawing lessons from the successful experiences of other countries, particularly those with similar contexts in ASEAN member states, can inform and improve PPAN nutrition initiatives. Studying and benchmarking effective strategies, policies, and program models can also be beneficial. Retaining collaboration and knowledge exchange with international organizations and development partners can provide valuable insights, experience, and technical assistance to enhance PPAN activities.
In comparison to other ASEAN countries, the Philippines currently lacks nutrition education in teacher training, hampering teachers’ ability to educate students about the significance of healthy diets and physical activity. 22 Additionally, the country faces a deficiency in policies aimed at reducing salt/sodium consumption, limiting saturated fatty acid intake, and eliminating industrially produced trans fatty acids. 5 Nevertheless, the PPAN still offers valuable lessons for other ASEAN members striving to address malnutrition and enhance nutrition outcomes. Firstly, it draws attention to the importance of establishing a comprehensive policy framework and strategic plan for nutrition, providing a structured roadmap that sets clear goals, objectives, targets, and specific interventions and strategies to achieve them. Developing their own national nutrition policies and strategic plans can guide ASEAN countries in coordinating their efforts and ensuring coherence in their nutrition initiatives. Secondly, the PPAN adopts a holistic approach to combating malnutrition by addressing both undernutrition and overnutrition. It acknowledges the significance of promoting a healthy diet, preventing diet-related diseases, and tackling the social determinants of health through enabling mechanisms. Other ASEAN countries can draw from this approach and formulate integrated strategies that target the various forms of malnutrition prevalent in their populations. Lastly, the PPAN demonstrates a proactive and adaptable approach to addressing malnutrition. Throughout the years, the PPAN has consistently refined its programs and strategies, taking into account the findings from previous evaluations of nutrition outcomes in diverse surveys. This responsiveness allows the PPAN to address the evolving nutrition challenges faced by the population. Therefore, the PPAN serves as a valuable example of how a comprehensive policy framework and strategic plan can guide national nutrition initiatives. Although there is still a lot of room for improvement, the experiences of the Philippines provide an opportunity to learn from both the effective approaches and the identified areas for improvement. This collective learning and exchange of best practices among ASEAN countries can ultimately contribute to significant progress in combating malnutrition throughout the region and reinforce the importance of collaborative efforts toward attaining a healthy ASEAN by 2025, as espoused in the ASEAN Community commitment of 2015.
Conclusion
Since its inception in 1974, the PPAN has been the Philippines’ comprehensive blueprint for addressing its nutritional issues. The PPAN has been steadfastly committed to global developmental goals with its dedicated organizational structure, targeted objectives, adaptable health programs, and enabling mechanisms. This review provides a comprehensive analysis of the evolution of the PPAN’s programs and strategies over the years, shedding light on the experiences, accomplishments, and remaining challenges encountered during its implementation so far. From the perspective of a lower middle-income country grappling with nutrition issues, valuable insights can be gleaned regarding the transformative actions and actors that have emerged over time to address population nutrition problems. Based on the findings, it is imperative to reexamine the PPAN and its strategies, placing greater emphasis on bolstering support and implementing context-specific approaches at the village level to address compliance issues. The responsiveness of the PPAN’s agenda and the continuous data quality monitoring and evaluation of its diverse program outcomes are vital to effect evidence-guided decisions on nutrition across multiple levels, in light of the Universal Health Care Act. Recognizing the multifaceted nature of malnutrition and acknowledging that no single system can single-handedly address its various drivers will facilitate accelerated progress toward sustainable nutrition outcomes.
Footnotes
Author’s Note
This study did not require ethics approval as it is a review paper and does not involve primary data collection or experimentation on human subjects.
Acknowledgments
The author expresses their sincere gratitude to Gina Mae C. Candelario, CPA, for her invaluable feedback, which was greatly instrumental to the successful completion of this review.
Declaration of Conflicting Interests
The author declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author received no financial support for the research, authorship, and/or publication of this article.
