Abstract
Background:
South Sudan has experienced ongoing civil and environmental problems since gaining independence in 2011 that may influence childhood nutritional status.
Objective:
To estimate the prevalence of undernutrition among children in South Sudan in 2018 and 2019 compared to the prevalence in 2010.
Methods:
Data on height and weight were collected using a 2-stage stratified sample framework in which households were randomly selected at the county level and nutritional status was calculated for all children under 5 years of age to determine height-for-age, weight-for-height, and weight-for-age Z-scores (HAZ, WHZ, and WAZ) and the prevalence of stunting, wasting, and underweight. Linear and logistic regression analyses were used to determine factors associated with nutritional status and the odds ratio for nutritional outcomes.
Results:
In 2010, the mean HAZ, WHZ, and WAZ was −0.78, −0.82, and −1.15, respectively, and the prevalence of stunting, wasting, and underweight was 30%, 23%, and 32%, respectively. In 2018 and 2019, the mean HAZ, WHZ, and WAZ was −0.50, −0.70, −0.77 and −0.53, −0.77, −0.76, respectively. The prevalence of stunting, wasting, and underweight in 2018 and 2019 was 17%, 14%, 15% and 16%, 16%, 17%, respectively. Age was negatively associated with all nutritional indices and girls had higher HAZ, WHZ, and WAZ and a lower mid upper arm circumference (P < .01) compared to boys. The risk of poor nutritional outcomes was associated with vaccine status and varied by state of residence.
Conclusions:
Following independence in 2010, the prevalence of undernutrition in South Sudan decreased, but the risk for undernutrition varied by state and efforts to address food security and health need to ensure equitable access for all children in South Sudan.
Introduction
Civil conflicts throughout the world continue to cause destruction for many countries. The health of women and children are often directly and indirectly negatively affected by conflict, leading to an increased prevalence of undernutrition, low birth weight, and childhood stunting and wasting. 1 -4 Indeed, approximately 54 million children are classified as stunted throughout Africa, a continent that continues to experience both ongoing and sporadic conflicts. 5 Despite the existence of many aid programs delivered by large organizations, such as the World Food Program (WFP), the United Nations Children’s Fund (UNICEF), the United States Agency for International Development, and other nongovernmental organizations (NGO), progress to reduce the prevalence of stunting and wasting in conflict areas has not been sufficiently documented.
South Sudan has suffered ongoing civil and environmental problems since gaining independence in 2011. Civil discord and political strife have resulted in internally displaced persons dependent on foreign aid and national nutrition assistance programs to ensure adequate dietary intake. At the same time, poor infrastructure, domestic violence, and ongoing economic troubles have contributed to widespread food insecurity in South Sudan. 6 The delivery of humanitarian aid (aid) in conflict zones is a difficult task at best with security, access, and logistical challenges. Even within the context of national household surveys, poor infrastructure, migration, and violence threaten data collection that provides important data on the people in such areas of the world. To that end, a recent series in The Lancet 7 found that systems that provide food (either agricultural or aid system) are vulnerable to destruction, looting, and corruption. 7 Logistics of aid delivery, such as roads, available staff, and infrastructure, are often in poor conditions or precarious arise as armed groups may attempt to control or disrupt the delivery of aid. The unfortunate result of these issues is a generation of children exposed to chronic food insecurity, stress, and inadequate medical care that can lead to various forms of undernutrition.
Childhood stunting is the most prevalent form of malnutrition worldwide, affecting over 149 million children under 5 years of age in 2020. 5 In 2010, it was estimated that 30% of children under 5 years of age in South Sudan were stunted. 8 Stunting has a complex etiology that involves diet, household environment, socioeconomic, and cultural factors. 9 The health of the mother reflects the household dietary intake and overall ability to access nutritious food and receive adequate health care, thus her status is directly related to the nutritional status of her child or children. 10,11 Social and environmental factors including sexual abuse, failed agricultural systems, civil conflict, poor sanitation, and general poverty also contribute to poor growth and undernutrition. 12 -14 Preventing growth deficits in vulnerable communities is important as childhood undernutrition has been linked to an increased risk of chronic diseases later in life. 15 In areas that continue to suffer from ongoing civil conflict, there is little hope that such challenges will end without a significant cost to human capacity. Addressing these challenges within existing aid programs, such as through integrated WASH programs, 16,17 can alleviate some of these problems.
In South Sudan, the prevalence of stunting is still high in some regions due to a confluence of climate and conflict factors that limit food production, delivery, and a diet suitable for pregnant women and growing children. 18 As South Sudan begins its second decade of independence, it is necessary to determine how the prevalence of undernutrition has changed following the introduction of several nutrition-sensitive programs throughout the country. Therefore, the focus of this study was to determine changes in the prevalence of stunting and wasting in South Sudan from 2010 to the most recent pre-COVID-19 national surveys. In addition, determinants of stunting and wasting in 2018 and 2019 were analyzed to better understand factors that promote or prevent chronic undernutrition of children in South Sudan.
Methods
Study Setting and Sample
Data for this study were collected using the annual Food Security and Nutrition Monitoring System (FSNMS), a national survey to monitor key food security indicators, acute and chronic malnutrition among children below 5 years and mothers, as well as identifying geographic areas and socioeconomic groups that are food insecure. The 22nd and 24th rounds of the FSNMS were conducted in July/August 2018 and July/August 2019, respectively, and included surveys of households across South Sudan with a sampling plan provided by the National Bureau of Statistics for statistically representative results on food security at county level. As well, data from 2018/2019 will be compared to an earlier survey completed in 2010.
The sampling frame for each survey was the same such that clusters were selected at the county level of which there are 79 in South Sudan. The sampling size was determined based on 95% confidence intervals and a margin of error of 10%. Random selection of clusters or enumeration areas (EAs) was done at the first stage of a 2-stage stratified sample framework and households were randomly selected at the second stage. For the first stage, EAs were randomly selected by National Bureau of statistics. In each county, 9 EAs were selected based on population proportion to size. At the second stage, 9 clusters or EAs were selected in each county and 12 households were selected per enumeration area, regardless of presence of children under 5 years of age, for a total of 108 households per county. In 2010, the data collection was between April and July, whereas the FSNMS 2018/2019 were conducted in July-August. In South Sudan, the lean season starts in April/May and ends in August. Household selection was done through listing of household in the EA after which enumerators were randomly selected for each EA. Large EAs were subdivided into segments and one segment was randomly selected and household listing conducted. In each selected household, all children under 5 years of age were included in the assessment. Children less than 2 years were measured lying down, whereas those 2 years and older (up to 60 months) were measured standing up. All anthropometric variables were converted to Z-scores using the World Health Organization growth standards.
Access constraints due to insecurity delayed or prevented data collection from various counties across the country. While access improved for households in Jonglei, Upper Nile, and Unity, previously known for elevated risk of insecurity, access to Central Equatoria and Western Bahr el Ghazal became a challenge during the FSNMS in July-August 2018. Insecurity also prevented access to Lainya, Yei, and Morobo counties in Central Equatoria and Wau county of Western Bahr el Ghazal. Terekeka was partially completed before the team was evacuated to Juba following a security incident. FSNMS data collection was also halted in Maban after attacks on humanitarian agencies by the community.
During the Round 22 of the FSNMS, 7692 households were surveyed. Only 24 households were surveyed in Maban. Other counties where insecurity limited the number of households include Wau (47 households), Terekeka (72 households), Raja (73 households), and Mundri West (77 households). For Round 24 of the FSNMS, 8505 households were surveyed. Access constraints due to heavy rains and impassable roads were the main challenges during this round of data collection. Worst affected area in terms of impassable road was Duk County. However, access situation in the Round 24 (August 2019) improved compared to Round 22, allowing data collection in Lainya, Yei, and Morobo counties in Central Equatoria and Nagero county of Western Equatoria.
Measures
Anthropometric Measurements
Anthropometric measurements were conducted using standardized techniques. 19 Height was measured to the nearest mm (Harpenden anthropometer, Siber-Hegner), as was the upper arm circumference. All these measurements were taken twice and the means were computed for analyses. Body weight was obtained in simple measure using an electronic balance (Seca 769, Seca GmbH) with a precision of 100 g. Training of enumerators for each survey was provided in 33 locations across the country following the Training of Trainers in Juba. The trainings were facilitated by WFP, Food and Agriculture Organization, UNICEF, Food Security Cluster, the Government, and Famine Early Warning Systems Network (FEWSNET) staff. Electronic tablets were used for data collection in the field and data were uploaded to the Open Data Kit. After data were uploaded, data quality checks were carried on a regular basis and feedback was provided to the teams in the field to improve the quality of data as appropriate. Teams that conducted all anthropometric measures were supervised by skilled investigators who verified techniques and procedures on a regular basis and retraining was provided when quality control was found to be below defined standards.
Statistical Methods
For anthropometric outcomes, Z-scores were calculated based on World Health Organization child growth standards. 20 A preliminary analysis of the data included all children measured, after which those with extreme values (Z-scores < −5.00 and > 5.00) were excluded. A relatively small proportion of children had values exceeding these thresholds (in round 22 n = 143/1.4% and n = 22/0.2% for height-for-age and weight-for-age, respectively; in round 24 n = 512/3.9% and n = 252/2% for height-for-age and weight-for-age, respectively). There was no significant difference in the mean of the main outcomes, therefore additional analyses were conducted on the dataset without the extreme values. For all analyses, we used state-level population weights. Although these weights cannot account for sample selection within states, they do ensure that the sample matches the state-level population shares in the country as a whole. All analyses, including descriptive statistics and regression analysis, accounted for the complex design of the survey by adjusting standard errors to reflect potential clustering within EAs. To compare the proportion of children who were classified as stunted, wasted, or underweight between the survey in 2010 and those in 2018 and 2019, a chi-square test was used to determine statistically significant differences.
After conducting descriptive analyses for general characteristics of the study sample, comparison between group means in different survey years was conducted using t tests to determine the statistical difference between anthropometric variables by age. Linear regression analyses were run with nutritional status as the outcome variable for rounds 22 and 24 of the survey. We included the following demographic covariates that were available in these 2 rounds of the survey: age, state, and sex (a dichotomous indicator for whether the child was female). Since there were few other covariates present in both surveys that were potential predictors of nutritional status, these data were not deemed suitable for assessing how the impact of other predictors of nutritional status beyond these 3 demographic variables has changed over time. In round 22, we were additionally able to assess whether access to public health campaigns (measles, deworming, and vitamin A receipt) and child illness, which have been previously shown to be associated with child nutritional outcomes, 21,22 were relevant in this sample. However, we verified that exclusion of these other covariates did not much affect the coefficients on age, sex, and state. Logistic regression analyses were used to determine the odds ratios for stunting and wasting associated with the included variables. All statistical analyses were performed using Stata (version 15.2) and R (version 3.5.0) and statistical significance was set at P < .05.
Results
Anthropometric characteristics for children in 2010 are summarized in Table 1. The mean age of participants was 28.2 months and the mean height-for-age Z-score (HAZ), weight-for-age Z-score (WAZ), and weight-for-height Z-score (WHZ) was −0.95 ± 1.94, −1.15 ± 1.94, and −0.82 ± 1.64, respectively. The mean HAZ, WAZ, and WHZ for boys and girls was −1.04 ± 1.96 and −0.87 ± 1.93; −1.25 ± 1.47 and −1.04 ± 1.41; and −0.92 ± 1.66 and −0.71± 1.61; respectively. The proportion of children who were stunted, wasted, or underweight was 30%, 23%, and 32%, respectively. Boys were more likely to be classified as stunted, wasted, or underweight by 4% to 5% points compared to girls. Data on anthropometric measures by age are summarized in Table 2. The mean HAZ, WAZ, and WHZ for children less than 24 months of age was −0.62 ± 2.03, −0.95 ± 1.53, and −0.84 ± 1.67, respectively. The mean HAZ, WAZ, and WHZ for children 24 to 59 months was −1.20 ± 1.85, −1.28 ± 1.37, and −0.79 ± 1.61, respectively. The proportion of children less than 24 months who were stunted, wasted, or underweight was 27%, 24%, and 24%, respectively, while the proportion for those 24 to 59 months was 25%, 21%, and 28%, respectively.
Anthropometric Characteristics of Children in South Sudan in 2010.a
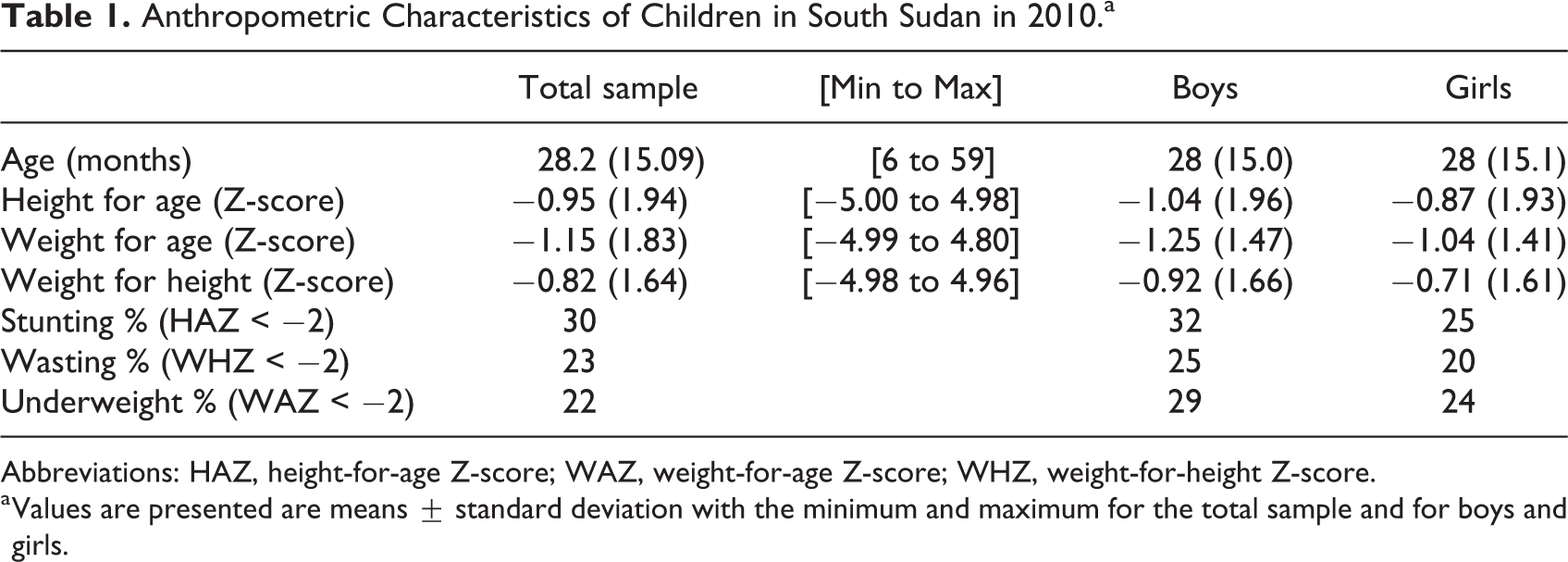
Abbreviations: HAZ, height-for-age Z-score; WAZ, weight-for-age Z-score; WHZ, weight-for-height Z-score.
a Values are presented are means ± standard deviation with the minimum and maximum for the total sample and for boys and girls.
Anthropometric Characteristics of Children by Age in South Sudan in 2010.a
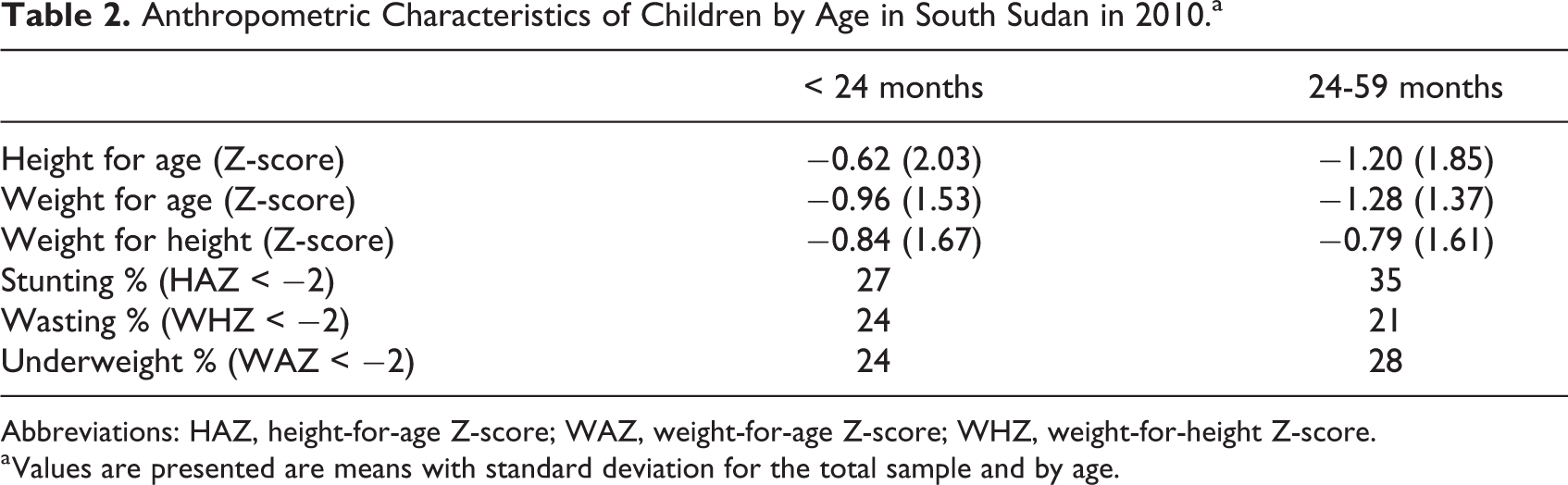
Abbreviations: HAZ, height-for-age Z-score; WAZ, weight-for-age Z-score; WHZ, weight-for-height Z-score.
a Values are presented are means with standard deviation for the total sample and by age.
Anthropometric characteristics for children in 2018 and 2019, overall and split by early and later childhood, are summarized in Tables 3, 4, 5, and 6. The mean HAZ, WHZ, and WAZ for all children in 2018 was −0.50, −0.70, and −0.77, respectively, and lower for boys compared to girls. The prevalence of stunting, wasting, and underweight was 17%, 14%, and 15%, respectively. The mid upper arm circumference (MUAC) was 14.4 cm for all children with comparable values for boys and girls. All anthropometric indicators were significantly lower for children younger than 24 months of age (Table 4) compared to children between 24 and 59 months of age. The prevalence of stunting was not significantly different between the age while the prevalence of wasting and underweight was higher in older children.
Anthropometric Characteristics of Children in South Sudan in 2018.a
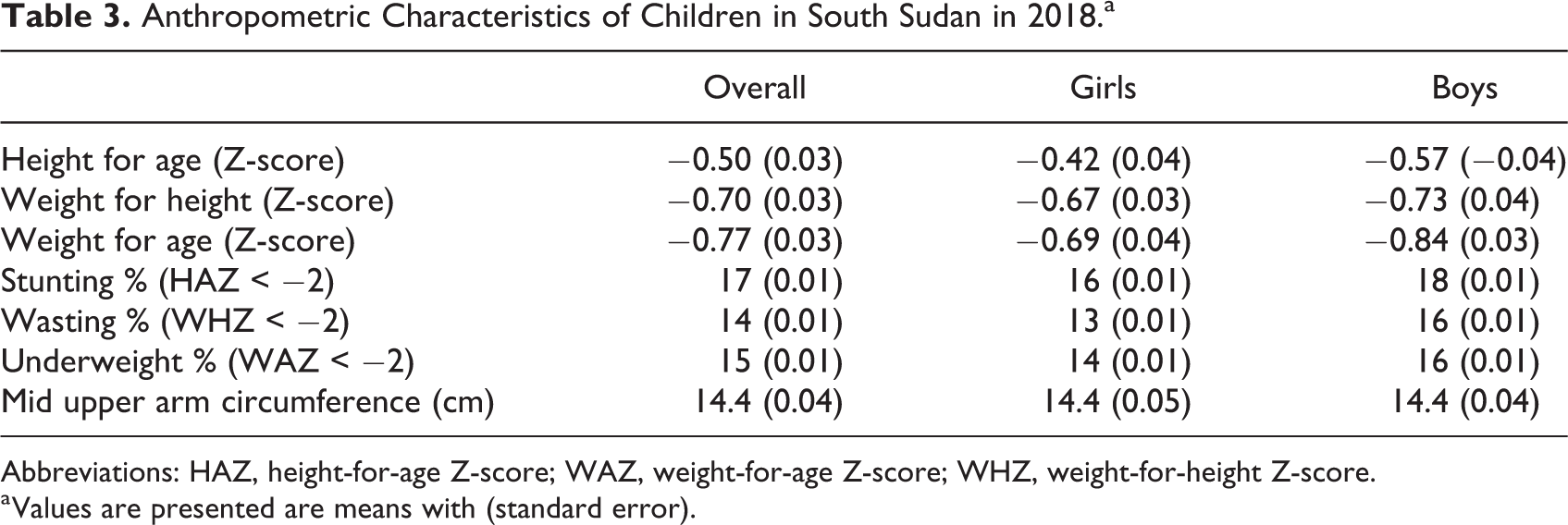

Abbreviations: HAZ, height-for-age Z-score; WAZ, weight-for-age Z-score; WHZ, weight-for-height Z-score.
a Values are presented are means with (standard error).
Comparison of Anthropometric Characteristics of Children Aged ≤ 24 Months and Children 24 to 59 Months of Age in South Sudan in 2018.a
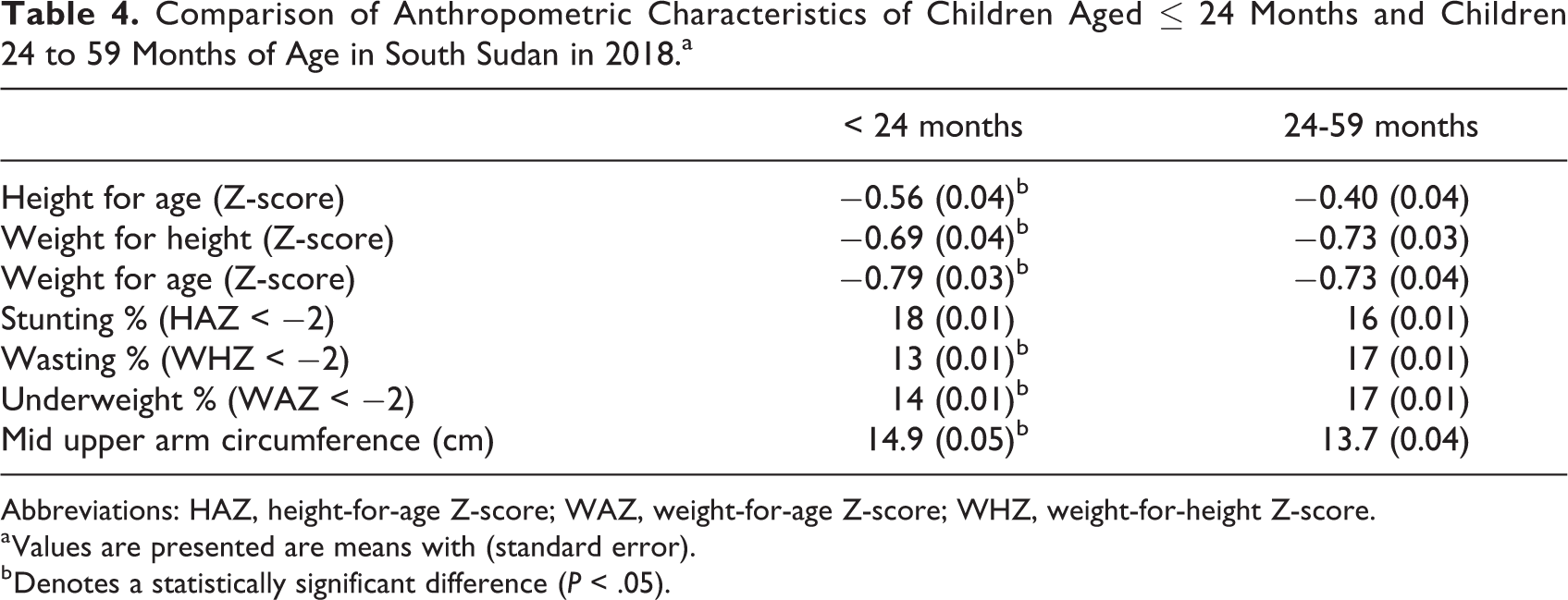
Abbreviations: HAZ, height-for-age Z-score; WAZ, weight-for-age Z-score; WHZ, weight-for-height Z-score.
a Values are presented are means with (standard error).
b Denotes a statistically significant difference (P < .05).
Anthropometric Characteristics of Children in South Sudan in 2019.a
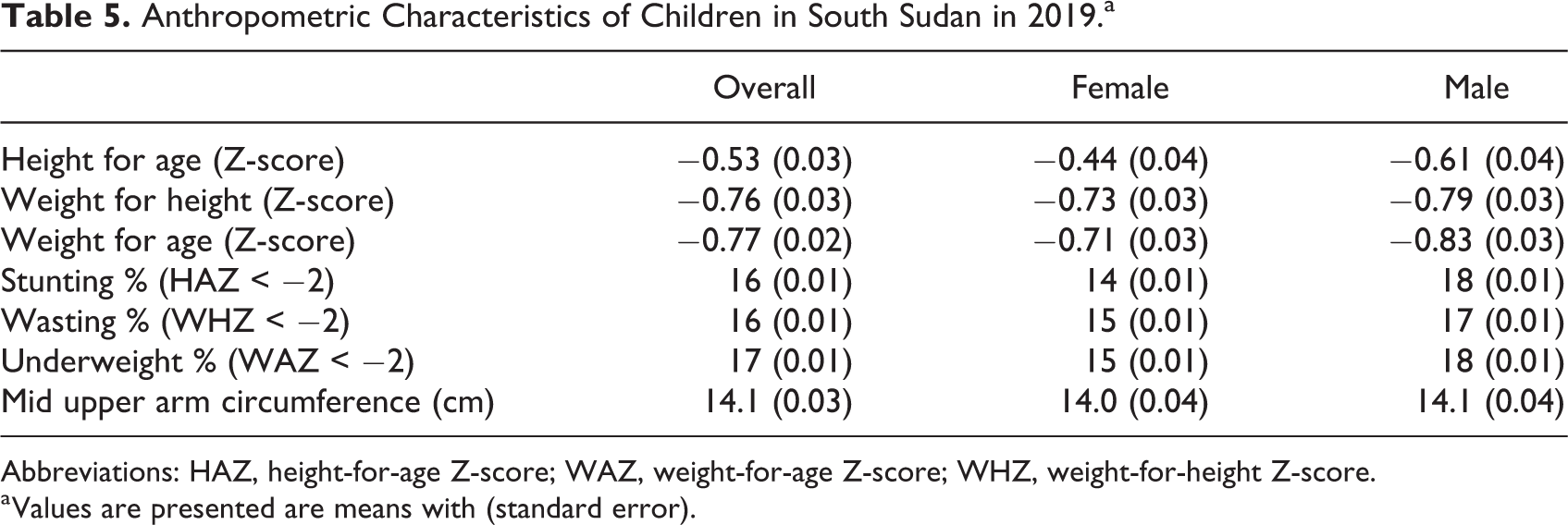
Abbreviations: HAZ, height-for-age Z-score; WAZ, weight-for-age Z-score; WHZ, weight-for-height Z-score.
a Values are presented are means with (standard error).
For children in the 2019 survey (Table 5), the mean HAZ, WHZ, and WAZ for all children was −0.53, −0.76, and −0.77, respectively, and the prevalence of stunting, wasting, and underweight was 16%, 16%, and 17%, respectively. Girls had similar nutritional status yet lower prevalence estimates of stunting, wasting, and underweight compared to boys. Similar to 2018, the MUAC was 14.1 cm for all children with comparable values for boys and girls. For younger children, HAZ and WAZ were significantly greater and WHZ was significantly lower compared to older children (Table 6). The younger children had a lower prevalence of stunting and a higher prevalence of wasting and underweight compared to older children.
Comparison of Anthropometric Characteristics of Children Aged ≤ 24 Months and Children 24 to 59 Months of Age in South Sudan in 2019.a
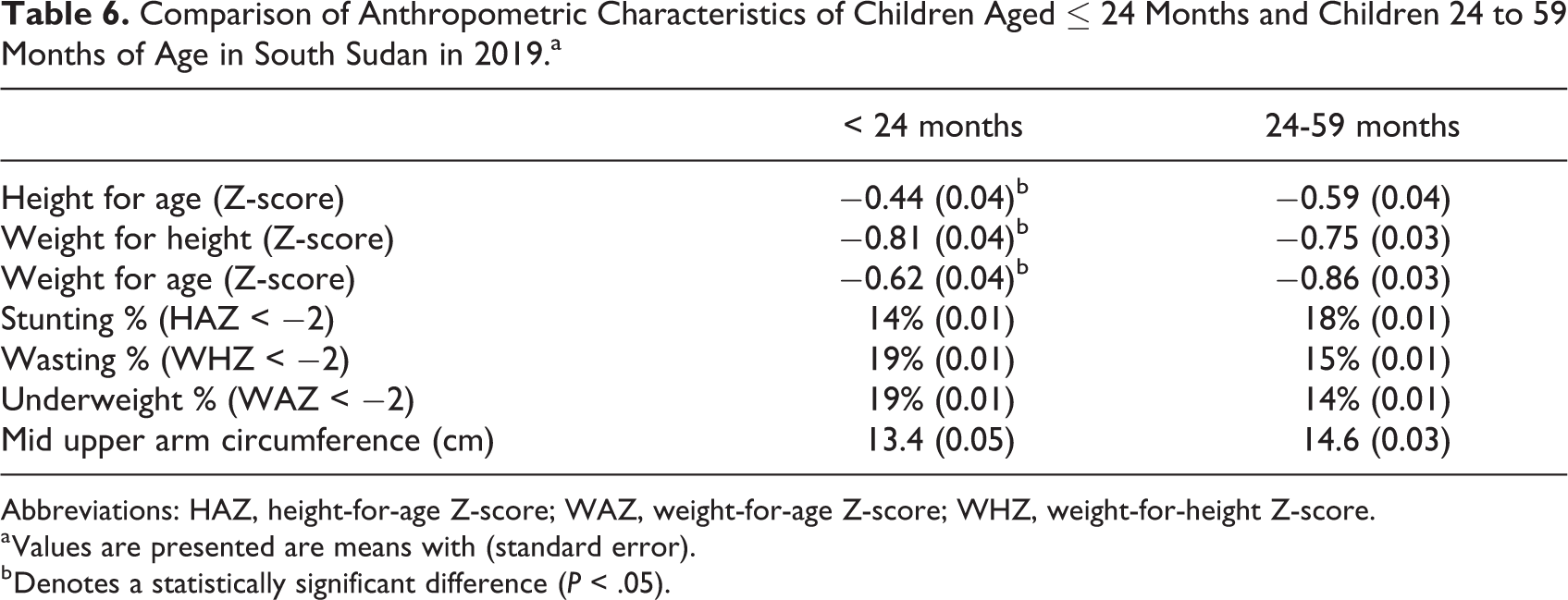
Abbreviations: HAZ, height-for-age Z-score; WAZ, weight-for-age Z-score; WHZ, weight-for-height Z-score.
a Values are presented are means with (standard error).
b Denotes a statistically significant difference (P < .05).
The results from linear regression analyses for 2018 and 2019 are summarized in Tables 7 and 8, respectively. For both years, age was negatively associated with all nutritional indices and being female was associated with a higher HAZ, WHZ, and WAZ and a lower MUAC (P < .01). In 2018 only, children who received the measles vaccine had a greater MUAC (0.27) and children who reported no recent illness had a higher WAZ. On the other hand, children receiving vitamin A in the past 6 months had a slightly lower WHZ and WAZ. In terms of the relationship between state and nutritional status, in 2018 all states had a negative relationship with WHZ and MUAC, yet only Eastern Equatoria had a negative relationship with all indices while only Lakes had a positive relationship with HAZ. Yet, in 2019, HAZ was positively associated with Jonglei, Lakes, Unity, Upper Nile, and Warrap (Table 8). There was a negative relationship between WHZ and any one of the states, while WAZ was negatively associated only with living in Eastern Equatoria, Jonglei, Lakes, and Upper Nile. Western Equatoria was the only state that showed a positive correlation with WAZ in 2019. The results for the linear regression and logistic analyses conducted by sex are provided in Supplemental Table 1.
Relationship Between Key Determinants and Nutritional Status Using HAZ, WHZ, WAZ, and MUAC for Children in South Sudan in 2018.a
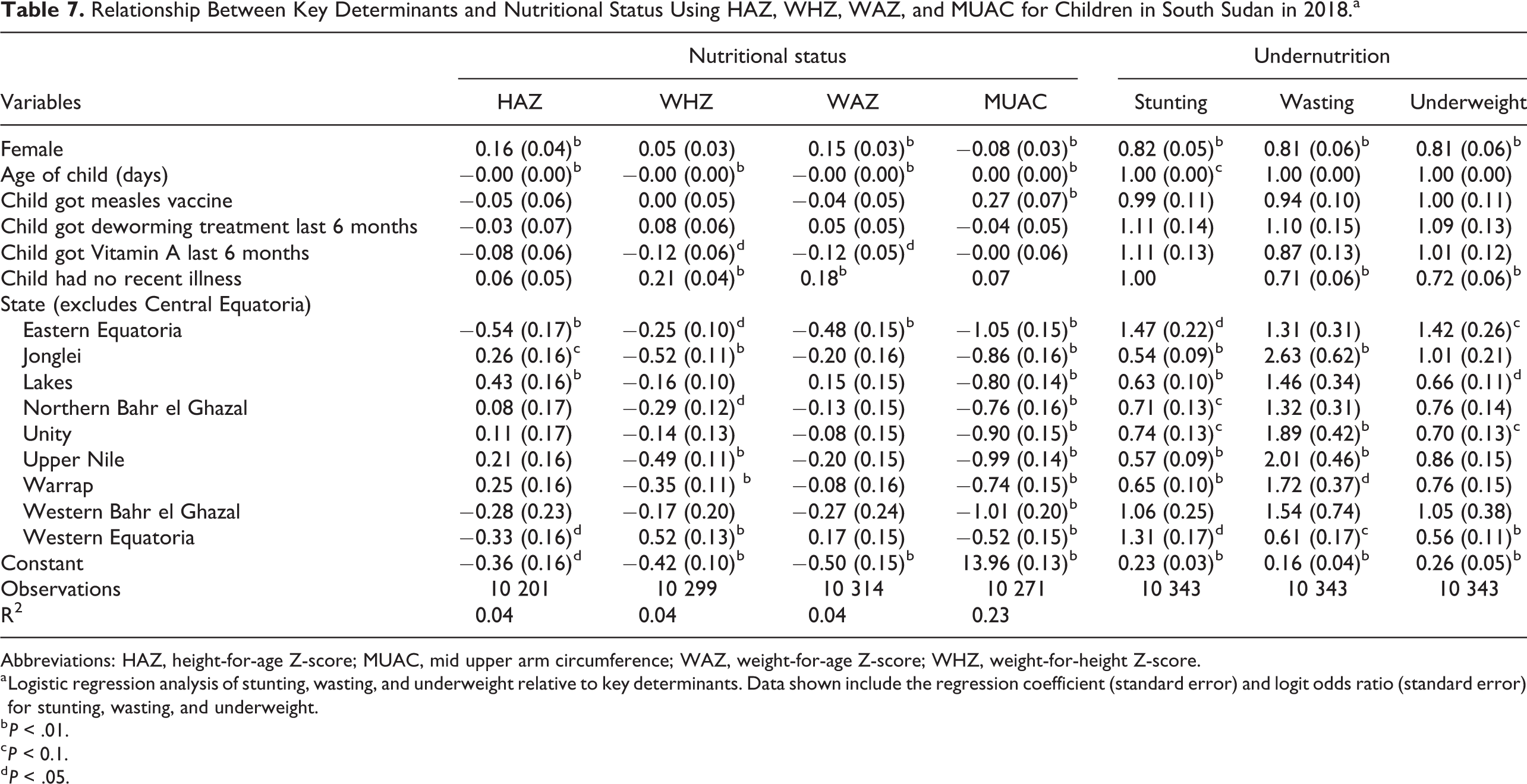
Abbreviations: HAZ, height-for-age Z-score; MUAC, mid upper arm circumference; WAZ, weight-for-age Z-score; WHZ, weight-for-height Z-score.
a Logistic regression analysis of stunting, wasting, and underweight relative to key determinants. Data shown include the regression coefficient (standard error) and logit odds ratio (standard error) for stunting, wasting, and underweight.
b P < .01.
c P < 0.1.
d P < .05.
Relationship Between Key Determinants and Nutritional Status Using HAZ, WHZ, WAZ, and MUAC for Children in South Sudan in 2019.a
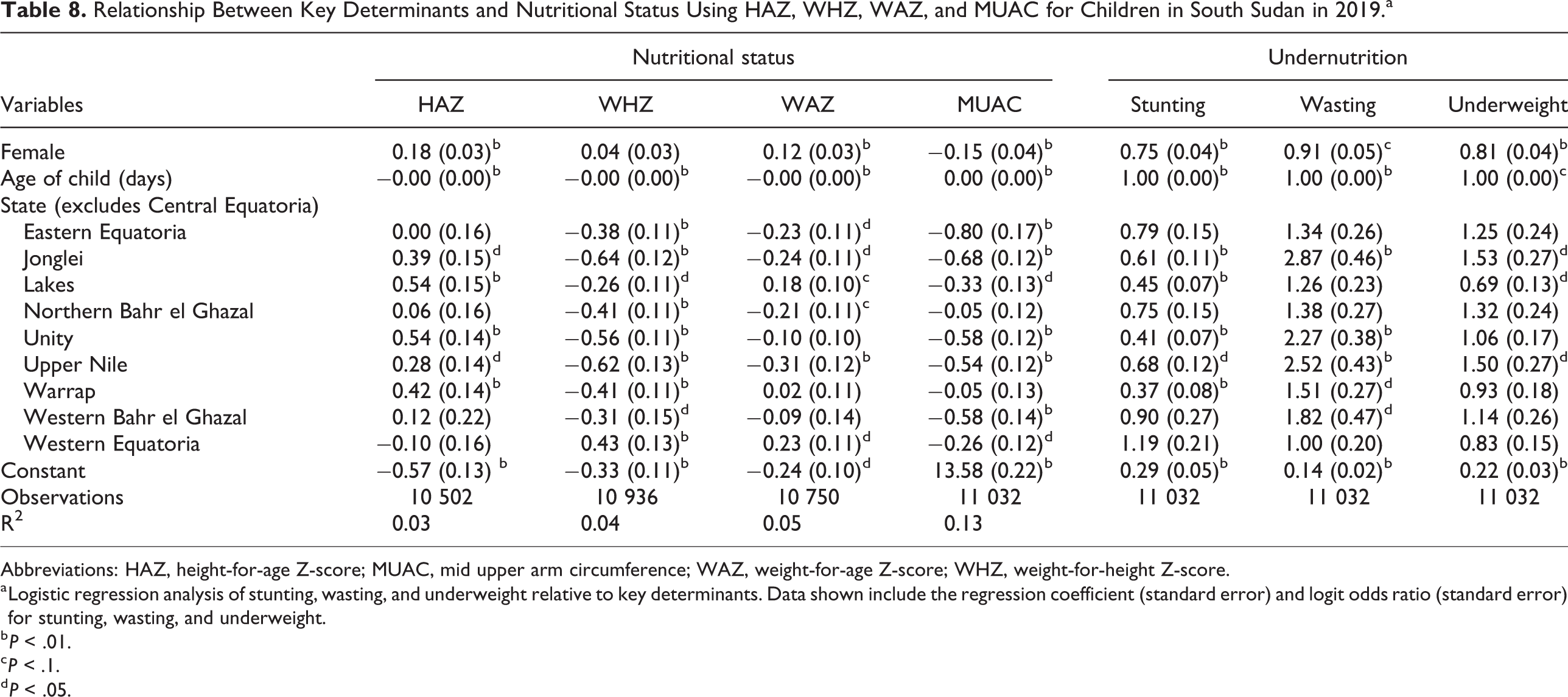
Abbreviations: HAZ, height-for-age Z-score; MUAC, mid upper arm circumference; WAZ, weight-for-age Z-score; WHZ, weight-for-height Z-score.
a Logistic regression analysis of stunting, wasting, and underweight relative to key determinants. Data shown include the regression coefficient (standard error) and logit odds ratio (standard error) for stunting, wasting, and underweight.
b P < .01.
c P < .1.
d P < .05.
Logistic analyses were done to determine the risk of stunting, wasting, and underweight in both 2018 and 2019 are presented in Tables 7 and 8, respectively. The risk of stunting, wasting, and underweight was lower for females in both 2018 (0.82, 0.81, and 0.81, respectively) and 2019 (0.75, 0.91, and 0.81, respectively). Children who had no recent illness were 29% and 28% less likely to be wasted or underweight, in 2018 only. In 2018, the risk of stunting was higher in Eastern Equatoria and Western Equatoria, while the risk of stunting was lower for children living in Jonglei, Lakes, Northern Bahr el Ghazal, Unity, Upper Nile, and Warrap. The risk of wasting was significantly higher in Jonglei, Unity, Upper Nile, Warrap, and Eastern Equatoria in both 2018 and 2019. The risk of underweight was significantly higher in Eastern Equatoria in 2018 and lower in Lakes, Unity, and Western Equatoria. In 2019, the risk of stunting was lower in Jonglei, Lakes, Unity, Upper Nile, and Warrap compared to other states and the risk of wasting was higher in Jonglei and Upper Nile, but lower in Lakes (Table 8).
Discussion
Since gaining independence in 2011, South Sudan has undergone many social and civil changes including the cessation of armed conflict with Sudan, an agreement to generate income from natural resources, and the development of a coordinated nutrition surveillance program. 6 At the same time, ongoing civil unrest accompanied by widespread internal and external migration limited broader structural changes that would improve health indicators for children. 23,24 Indeed, South Sudan continues to experience challenges that limit progress of many social and health programs, such as flooding, random violence, and a depressed economy. Briefly, compared to 2010, the prevalence of stunting decreased from 33% and 29% for boys and girls, respectively, to 18% and 16% in 2018 and 18% and 14% in 2019 (Figure 1). These data are consistent with other countries in the region. 18,25 It is evident that more progress is required to improve the nutritional status of children living in all parts of South Sudan and continued monitoring of states is important to provide equal benefits across the country.
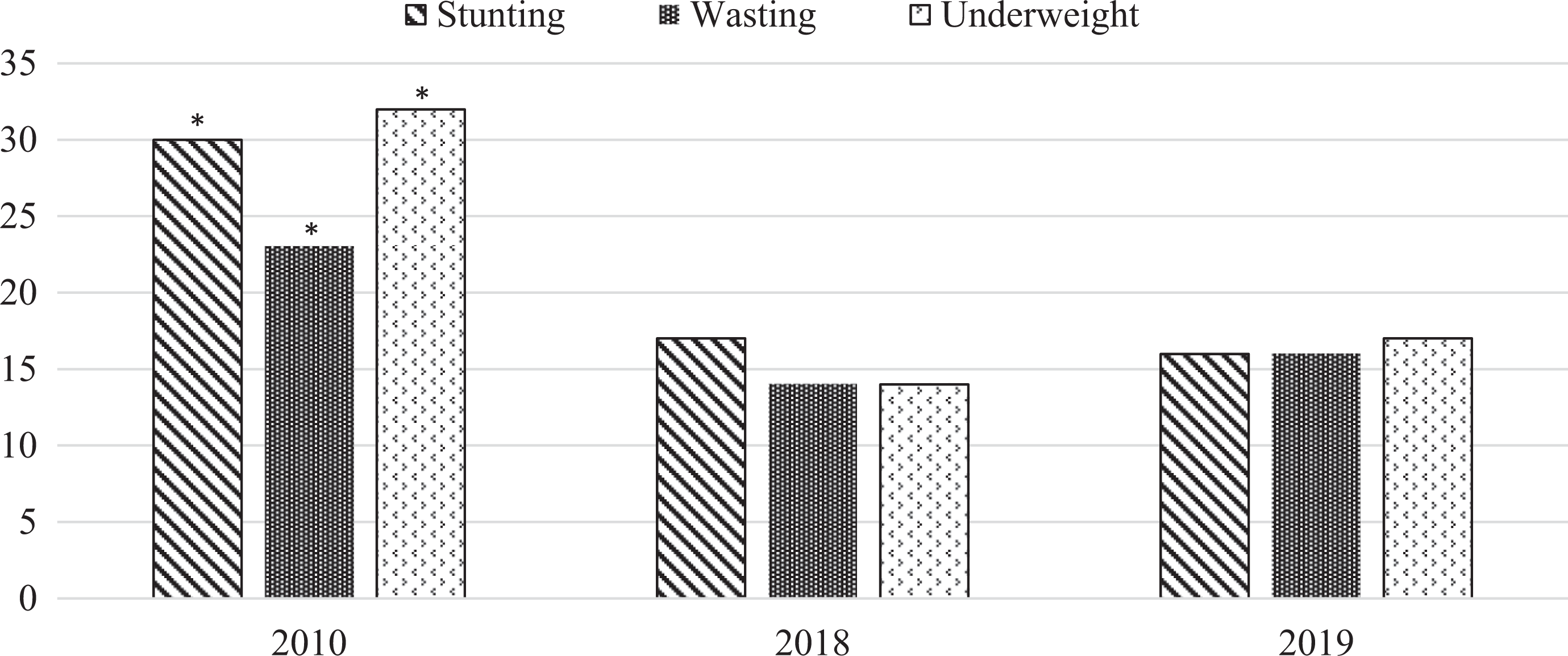
Prevalence of stunting, wasting, and underweight in South Sudan between 2010 and 2018 and 2019.
Following independence, the prevalence of wasting and stunting decreased, suggesting an overall improvement in nutritional status across the country. In particular, girls had a significantly a lower risk of stunting compared to boys and the state in which in a child lives may increase or decrease the risk of stunting. However, like stunting, reductions in wasting were not uniform across all states and the risk of wasting was variable between states (Figure 2). Understanding these differential changes by state requires more intensive investigation as to participation rates for nutrition programs, implementation processes and policies, as well as dependency on aid over domestic agricultural programs. As well, there is an uneven reality of treatments and programs available in South Sudan as some states have few if any health clinics, others are home to internally displaced persons from other states which stresses an already overburdened health system, yet others have no food aid or supplies to support refeeding programs. 26 Thus, uneven advances in nutritional status appear to be common and due to general lack of funds, random civil disruption, internal displacement, and lack of a sustainable agriculture sector. 27 At the same time, treatment programs designed to protect against wasting may be differentially promoted in some states and not others. 28 It is also important to recognize that participation in WASH programs has gained popularity over the past decade as numerous research studies have been published that support the protective effects of triple-duty programs to improve diet and nutritional status in marginal communities. 29 -33
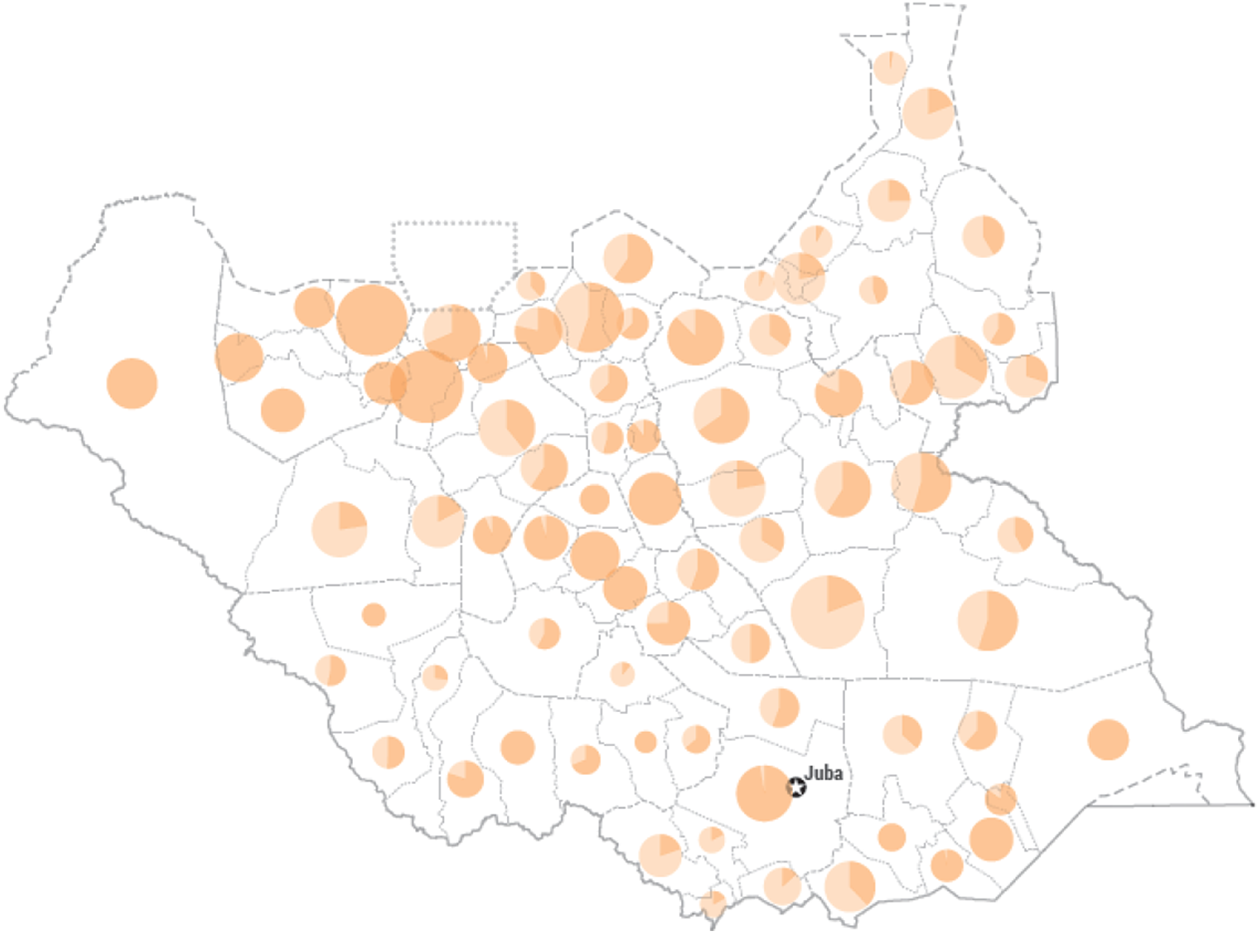
Areas in need of nutrition assistance in South Sudan in 2020 according to the Humanitarian Response Plan for South Sudan 2021 (www.unocha.org/south-sudan). 34
Since 2011, security and agricultural production have been met with several challenges that have resulted in poor food production, distribution, and a sustained prevalence of internally displaced persons as well as differential administration of domestic or international nutrition aid or programs. 34 Each challenge in and of itself has contributed to crises in a few states, but most especially in Eastern Equatoria, Upper Nile, Unity, and Jonglei. Furthermore, violence has reduced the number of primary care clinics throughout the country and logistical challenges hampered many relief efforts by WFP, NGOs, and South Sudanese health professionals. As well, militant groups operated throughout South Sudan and exacerbated an already deteriorating situation with regard to food insecurity and malnutrition. It is estimated that the prevalence of subacute malnutrition in South Sudan increased from 235 044 children in 2014 to 269 140 in 2018. 6 According to the UNICEF report, the increased prevalence of malnutrition during this time period may be attributed to ongoing internal community conflicts, delayed rainfall, and poor agricultural production, as well as an increase in food security from 34% to 60% in areas most affected by the drought. 6
Regardless of the severity of ongoing humanitarian crises, national surveys clearly indicate that malnutrition is decreasing across South Sudan. The government of South Sudan engaged in a coordinated program with UNICEF and NGO’s to scale-up nutrition programs in an effort to reduce the prevalence of malnutrition. 6 This effort was designed to employ “lessons learned” during the first half of the decade and make modifications in the delivery and maintenance of nutrition programs. In particular, efforts were made to consolidate treatment protocols, centralizing program administration, simplifying protocols given the continued decline in both health clinics and professionals, digitizing records, integrating nutrition screening in the rapid response mechanisms, and introduction of cognitive development sessions for children. 6 There are an estimate 1.9 million people in need of some form of nutrition assistance and monitoring throughout South Sudan 34 and needs are quite variable by state and county which may explain the disparate influence of state on childhood nutritional status. Data from the FSNMS have been crucial in making decisions on appropriate responses and preventive measures that include informing Integrated Food Security Phase classification analysis, identifying priority areas, the determination of number of people in-need, and estimating resource requirements for nutrition interventions. In addition, FSNMS data have been used for both short- and long-term nutrition programing including evidence-based planning, bottleneck analyses, setting annual and multiyear nutrition program plans and targets, and priority resource allocation. The joint FSNMS assessment continues to provide an advocacy platform for a collective and unified voice among the key food security and nutrition stakeholders in the country.
There are a number of strengths and limitations that need to be discussed relative to data collection and analyses. First, the national surveys analyzed both used the same methodologies for selecting households to include in the survey. Households were not substituted if security issues limited or halted data collection and these households were subsequently not included in the survey. Therefore, the nutritional status of children in these areas may have modified the national mean for HAZ and WHZ, most likely by reducing the mean given that such civil unrest tends to promote undernutrition and food insecurity. 35,36 The issue of missing data is not a trivial matter. However, we caution against speculation as to how these missing data may impact the national estimates presented in this article. In the case of missing counties, which accounted for 6% of the target sample, the impact on the national prevalence would be minimal as the sample size was adequate for all remaining counties and the issues that prevented data collection were transitory and not chronic, suggesting that any potential impact on nutritional status would be minimal. Still, there is the possibility that missed households or counties could have influence the national prevalence, but to say if it would have lowered or raised the prevalence is pure speculation. Second, the training and quality control of all enumerators was verified by the NGO that oversaw data collection and all protocols were consistent with nutrition surveillance policies agreed to by the South Sudan Ministry of Health. Third, while not all mothers had official birth certificates for their children, birth dates were verified by the enumerators using established methods with multiple clarifying questions and input from other community members (e.g., neighboring women or local midwives) who were able to confirm birth dates not verified by birth certificates. Still, such issues may influence nutritional status to some degree, but most likely did not result in any differential bias given the large sample size of each survey. Finally, as with any comparison of multiple national surveys, the data presented at not panel data and inferences from a comparison of randomized national surveys needs to be treated with caution. Nonetheless, given that the surveys followed similar randomization protocols, there is sufficient confidence in the data to draw relatively broad conclusions about trends in nutrition status from 2010 to 2018/2019.
In summary, following independence and a series of ongoing civil conflicts, the prevalence of stunting and underweight in South Sudan has decreased by nearly 50% between while the prevalence of wasting and underweight has decreased by 25%. Access to humanitarian aid and living in specific states that host a high number of internally displaced persons and/or are recipients of humanitarian aid may have created a differential impact on the risk of stunting and wasting. Therefore, it is imperative that countries in conflict or dire economic situations monitor the nutritional status of recipients to ensure that aid is being directed to the most vulnerable. Nonetheless, South Sudan appears to have a robust nutrition monitoring system in place and continues to implement programs to improve food security throughout the country to improve maternal child nutrition and lower the prevalence of all forms of undernutrition throughout the country.
Supplemental Material
Supplemental Material, sj-pdf-1-fnb-10.1177_03795721221128126 - Childhood Stunting and Wasting Following Independence in South Sudan
Supplemental Material, sj-pdf-1-fnb-10.1177_03795721221128126 for Childhood Stunting and Wasting Following Independence in South Sudan by Daniel J. Hoffman, Ismail Kassim, Biram Ndiaye, Mark E. McGovern, Huyen Le, Kiross Tefera Abebe and Mohamed Ag Ayoya in Food and Nutrition Bulletin
Footnotes
Authors’ Note
DJH, BN, MAA, and IK conceived of the study. DJH and MM analyzed the data. DJH and HL wrote the manuscript and MM, BN, MAA, and IK provided editorial input. All authors reviewed and approved the final version of the manuscript.
Acknowledgments
The authors would like to acknowledge the field teams in South Sudan for their work in data collection coordinated by the government of South Sudan, UNICEF, the WFP, FAO, and especially the men, women, and children of South Sudan whose willingness to participate in these surveys is appreciated with our gratitude.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: Financial support was provided by the Rutgers Department of Nutritional Sciences, Program in International Nutrition and the New Jersey Institute for Food, Nutrition, and Health. DJH is a paid consultant for UNICEF South Sudan.
Supplemental Material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
