Abstract
Background:
Schools can play an important role in promoting healthy child diet and body weight. However, this issue is understudied in Latin American and other populations undergoing nutrition and epidemiologic transition.
Objectives:
2018 Ecuadorian National Health and Nutrition Survey data were used to examine the association of school food sources with healthy and unhealthy food intake and body mass index (BMI) in primary (n = 12632) and secondary students (n = 6617).
Methods:
Data on school food environment characteristics were collected by questionnaire, intakes of fruits, vegetables, plain water, sweetened beverages, processed snacks, and fast foods by food frequency questionnaire, and BMI using measured weight and height. Data were analyzed using multivariable methods.
Results:
The major school food sources were competitive foods sold by commercial outlets (73%), School Breakfast Program (SBP; 52%), and home-packed items (37%). Most (69%) competitive food outlets sold fruits and vegetables but only 44% offered free clean drinking water and 60% sold prohibited “red traffic light” foods. Primary and secondary students who bought competitive foods consumed sweetened beverages, processed snacks, and fast food more frequently than nonpurchasers (P = .0001). Those who packed home foods had higher fruit and vegetable intakes (P = .0001). Plain water intakes were reduced among all SBP participants (P = .0001). However, primary students in the SBP consumed fast foods less frequently (P = .0001) and had lower average BMI and odds for being obese compared to nonparticipants (P = .0001).
Conclusion:
The findings from this nationally representative study underscore the important contribution of the school food environment to child nutrition.
Keywords
Introduction
Middle childhood and adolescence are critical life course periods when eating habits are established that can influence future nutrition and health risks. 1 Primary and secondary students spend a substantial proportion of their waking hours at school where most consume at least one meal and/or snack. 2 The school food environment includes the physical spaces, infrastructure, and conditions in and around school campuses where foods and beverages are available, obtained, purchased, and/or consumed by students as well as policies regulating their accessibility. 3 It has the potential to influence child eating habits, nutrition, and health by promoting access to more nutritious foods and beverages and restricting access to those that are less healthy. 4,5
School feeding programs are a major source of on-campus foods and beverages consumed by children in many populations. These can provide students with regular access to meals and also serve as a social safety net for children from low-income households. 2,5 Competitive foods, that is, foods and beverages sold on campus that are separate from school feeding programs and items brought from home to consume on campus are two other major sources of school food. 2,3
Participation in School Breakfast Programs (SBP) and other school feeding programs has been linked to reduced hunger and improved concentration at school in diverse populations although evidence for the impact of these on child diet and obesity is mixed. 2,6 -9 Likewise, findings also are mixed regarding the impact of other school food sources such as competitive foods 10,11 and foods brought from home. 12 -14
Since most prior studies examining the influence of school food environments on the diet and nutrition of school-age children and adolescents were conducted in high-income populations such as the United States and Canada, it is unclear the findings are generalizable to low- and middle-income countries (LMIC) in Latin America such as Ecuador which have different legal frameworks, policies and practices governing school food environments as well as food systems, and population attributes. 15,16
Ecuador, like many other Latin American LMICs, is in nutritional and epidemiologic transition. In addition to decreasing physical activity and other lifestyle changes, diets have been shifting from those emphasizing fruits, vegetables, legumes, whole grains, and other minimally processed foods to an increasing consumption of energy-dense, processed/ultraprocessed foods, fast foods, and sweetened beverages. 17,18 Child overweight and obesity have been rapidly rising while micronutrient malnutrition and stunting persist. 17,19,20
The SBP is Ecuador’s major national school feeding program. The main goal of the universal SBP is to improve school attendance by reducing hunger and secondarily to supplement child nutrition.
21,22
The SBP provides breakfast and/or snacks for all children aged 5 to 14 years enrolled in nonresidential state, municipal, or public-religious schools.
21
-23
The SBP rotates 5 different combinations of ready-to-consume prepackaged, multifortified food products and beverages that provide an average of 200 to 280 kcals (Combos 1-4) or 100 to 130 kcals (Combo 5; Table 1). These foods include high-protein whole grain cereal bars, cookies, and granola flakes, some of which are micronutrient fortified. Two of the beverages in the rotation feature whole milk and 2 others feature a milk-based drink. One of the criticisms is that several of these products contain added sugar (e.g., flavored milk drinks, fruit nectar, flavored cereal). Sometimes, a seasonal fruit may be provided.
21
In Ecuador, most students attend either a morning (07:15
Although lunch is the main meal of the day, the prior School Lunch Program was phased out around 2013 in order to permit the SBP to offer universal coverage. 23
Foods and Beverages Provided by the Ecuadorian School Breakfast Program.a
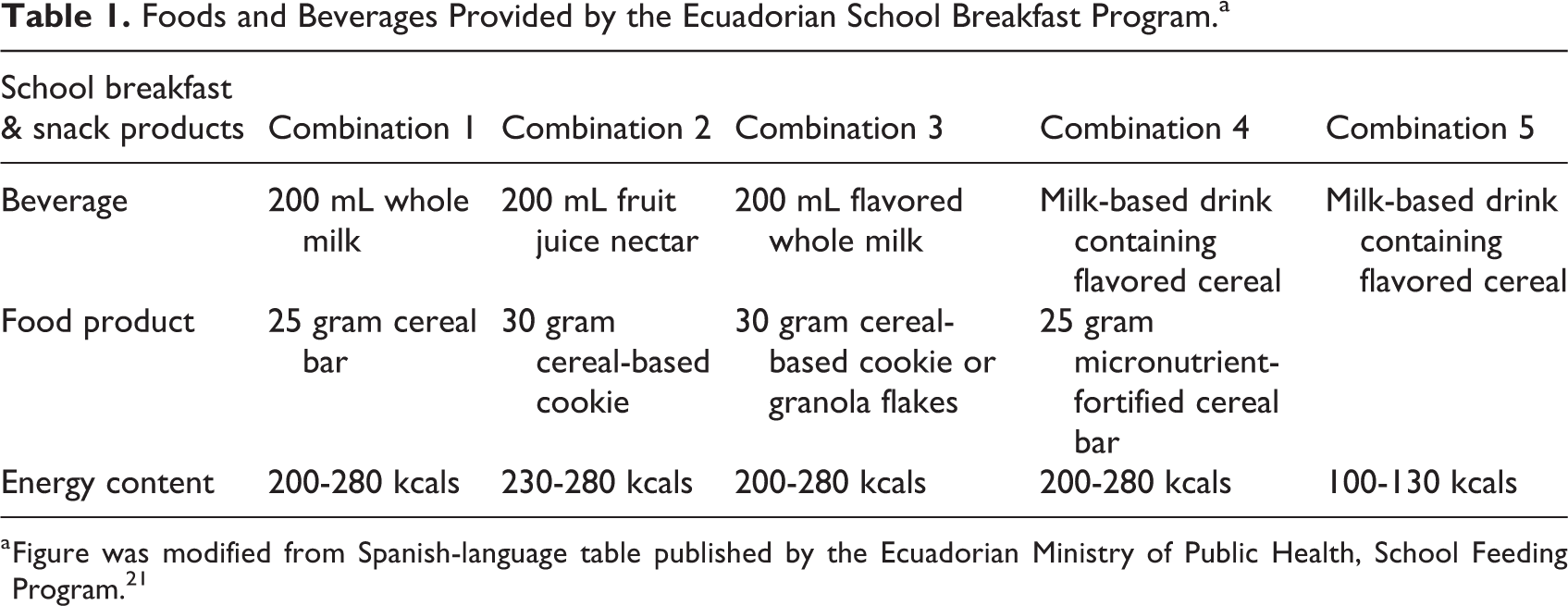
a Figure was modified from Spanish-language table published by the Ecuadorian Ministry of Public Health, School Feeding Program. 21
Competitive foods sold at on-campus “school bars” operated by small independent vendors are a major source of school food in Ecuador. While many of the items sold may be processed (e.g., sandwiches, hamburgers, cerviche, toasted dried corn) or ultraprocessed (e.g., chips, doughnuts, packaged fruit juices, chips, energy drinks, soft drinks), others may not be such as the fresh fruits and vegetables they are required to offer for sale by governmental regulations. Governmental regulations prohibit these from selling processed foods and beverages with a “red traffic light” nutritional label signifying a high content of added fat, sugar, and/or salt. 24 They also obligate school bars to offer fruits and vegetables for sale and to provide free, safe drinking water. 24
Although technical studies of the caloric and nutrient content of Ecuadorian SBP foods and beverages, packaging quality, program delivery system, and program financing have been conducted, the program’s impact on child diet and nutrition has not. 22,23 Studies are also lacking regarding the dietary and nutritional impacts of competitive foods and beverages purchased on campus by Ecuadorian students as well as those brought from home. The examination of the school food environments and their nexus with child nutritional indicators is important for informing more effective school food policies, regulations, and programs.
We analyzed data from the most recent Ecuadorian national nutrition and health survey to characterize the food environments of primary and secondary schools and to investigate the association of school food sources with child dietary intake and anthropometric indicators. The specific study objectives were (1) to describe food environments of schools attended by Ecuadorian primary and secondary students including the SBP, competitive food outlets and compliance with “red traffic light” foods, fruit/vegetable sales, and plain drinking water regulations, and foods brought from home, (2) to investigate the association of 3 major school food sources (i.e., SBP foods, competitive foods purchased at school bars, foods brought from home) with (2a) child intakes of healthy foods and beverages (i.e., fruits, vegetables, plain water) and whether intakes of these met dietary recommendations and (2b) less healthy foods (i.e., sweetened beverages, processed snack foods, fast foods) and whether intakes of these exceeded recommended limits, and (3) to examine the association of the 3 major school food sources with child body mass index (BMI) and BMI-for-age categories (i.e., underweight, overweight, obesity).
We hypothesized that schoolchildren who purchased competitive foods from their school bars would consume unhealthier foods and beverages more frequently than nonpurchasers and that they also would be more likely to exceed recommended limits for these. We also hypothesized that the more frequent intake of these energy-dense foods would displace those of healthier foods and beverages so their intakes would be lower than that of nonpurchasers. In addition, we posited that the more frequent intakes of energy-dense foods and beverages by competitive foods purchasers would place them at higher risk for overweight and obesity compared to nonpurchasers.
We also hypothesized that compared to nonparticipants, SBP participants would have similar or lower intakes of sweetened beverages, processed snacks, and fast foods as well as the 3 healthier foods assessed in the study (i.e., fruits, vegetable, plain water) because of contribution of SBP foods to fullness. Moreover, we hypothesized that the relatively small caloric contribution of foods provided by the SBP would not contribute to a higher risk for overweight or obesity. Finally, we postulated that children who brought food from home to consume at school would be more likely than others to have lower intakes of energy-dense foods but higher intakes of healthier foods because of the control exerted by parents over those items.
Methods
Study Design and Setting
Data from the 2018 Ecuadorian National Nutrition and Health Survey (Spanish acronym: ENSANUT) were used to examine our study hypotheses. 25 The ENSANUT is a nationally representative survey conducted every 5 years by the Ecuadorian National Institute of Statistics and Census (Spanish acronym: INEC) as part of its ongoing integrated health and nutrition data collection system. Details of the survey design, sampling method, sample size, data collection techniques and measures, data quality control, and other methodological considerations of the de-identified database have been previously described in detail including its low nonresponse rate (1.19%). 26 Briefly, the survey used a probabilistic, 2-stage stratified cluster sampling design to collect data during face-to-face interviews during 2018 to 2019 from a nationally representative sample of persons living in 46638 households in all Ecuadorian provinces. The sampling frame for the survey was drawn from the 2010 Ecuadorian Population Census and data collected during 2010 to 2017 census updates. The research universe consisted of all households and noninstitutionalized persons from those households. 26 The de-identified database was designated as “Research not subject to human subject regulations” by the Indiana University Institutional Review Board.
A total of 23621 survey participants aged 5 to 17 years were potentially eligible for inclusion in the analyses. Since the focus was on the school food environment, we sequentially excluded children who were not attending school (n = 1149) resulting in a sample of 22472. We also eliminated cases where data were missing on school food sources (n = 20), weight or height measurements (n = 775). In addition, we excluded those missing data on school bars selling competitive foods (n = 21) and their characteristics including the sale of red traffic light foods (n = 2083), fruits and vegetables (n = 239), and clean water (n = 85). This resulted in a total of 19249 cases available for analysis; 12632 primary and 6617 secondary school-age students.
Measures
Data used for the analyses were obtained from the ENSANUT 2018 main household and child risk factors modules. The household module collected data from household heads on child and household sociodemographic characteristics. This module also included data on child weight and height measurements. The second module collected data on school food environment characteristics, child food and beverage intake, and physical activity. These data were obtained from children aged 11 to 17 years and from both children and parents for those aged 5 to 10 years. 25
School food environment
Data collected on the school food environment included a specific question on whether the school had an on-site school bar selling competitive foods and another one on whether the foods sold included processed “red traffic light” nutrition label foods (i.e., foods with high sugar, fat, or sodium content) which are prohibited by Ecuadorian Ministry of Public Health/Ministry of Education (Spanish acronyms: MSP/ME) regulations. In addition, information was obtained from questions asking whether the school bars in their academic institution offered fruits and vegetables for sale or provided clean drinking water free of cost to children as they are required to do by MSP/ME regulations. Other school food environment behavior questions included whether the child participated in the national SBP and if so, how many days per week they received foods. Additional data collected on school food sources included whether the child purchased competitive foods or brought foods from home to consume at school. Children who reported bringing foods from home were further questioned as whether or not the packed foods included any fruit, home-prepared items, or processed foods.
Dietary intake
An abbreviated food frequency questionnaire was used by the survey to collect data on child intake of 6 food and beverage groups during the prior 7-day period. The questions included how frequently the child participants had consumed fruits (e.g., apples, bananas, watermelon, papaya), vegetables (e.g., lettuce, tomato, carrots, broccoli, green beans). They were also asked about how many servings of fruit (number of fruits or fruit portions) or vegetables (one cup raw or ½ cup cooked) that had consumed during this time. Other data were collected on the number of glasses of plain water, without colorants, sweeteners, flavorings, consumed daily during the past 7 days.
Data also were collected on the number of days during the past week that children had consumed sweetened beverages (e.g., soft-drinks, energy-drinks, processed fruit juice), processed food (e.g., crackers, cookies, potato chips, corn snacks, chocolates, other candy), and fast foods (e.g., French fries, hamburgers, tacos, hot dogs, pizza, salchipapas [fried potatoes/hot dogs]). In this study, we assumed that children who reported consuming any of these items ate a minimum of one serving/day. We compared child intakes of the 6 food and beverage groups to recommendations for these published by the Ministry of Public Health/Ministry of Education 27,28 and Ecuadorian National Food-Based Dietary Guidelines. 29
Anthropometric indicators
Trained survey anthropometrists measured child weight (kg) and height (cm) using a standard protocol. 26 These measurements were used to calculate BMI. The World Health Organization (WHO) reference tables for female and male children aged 5 to 19 years were used to classify BMI-for-age. 30 Children having a BMI that was < 1 standard deviation (SD) of the WHO Growth Reference median for their age were classified as underweight. Those with a BMI of > 1 SD or > 2 SD of the reference median for age were classified, respectively, as overweight or obese.
Data Analysis
The summary statistics for school food environments and participants are presented as numbers with weighted percent or weighted means ± standard error. We constructed unadjusted and adjusted general linear model (GLM) models to examine the mean intakes of fruits, vegetables, plain water, sweetened beverages, processed snack foods, and fast foods by all 3 school food sources, that is, SBP (any vs none), school bar (any vs none), brought from home (any vs none). We also constructed unadjusted and adjusted bivariate logistic regression models to examine the association of all 3 school food sources (SBP, school bar, brought from home) with recommendations 27 -29 for daily intakes of fruit (< 3 vs > 3 servings/day), vegetables (< 2 vs > 2 servings/day), plain water (0-7 glass vs 8 glasses/day) as well as for fast foods (0 servings vs > 1 servings/day), processed snack foods (0 servings vs > 1 servings/day), and sweetened soft drinks/energy drinks/processed fruit juices (0 servings vs > 1 servings/day).
We constructed unadjusted and adjusted GLM models to examine differences in mean BMI by the 3 school food sources. Next, we constructed bivariate and multivariable logistic regression models to investigate the association of each of the 3 school food sources with BMI categories (underweight, overweight, obesity). The models estimated the unadjusted (odds ratio) and adjusted odds ratios (AOR) with 95% confidence intervals for each outcome. Conceptually relevant covariates included in the statistical models were based on their availability in the database. These included child age (years), sex (male, female), ethnicity (indigenous, Afro-Ecuadorian, mestizo), and child physical activity (total min/day spent walking/biking to and/or from school, in physical education classes, and in recreational physical activity). Household-level covariates included maternal education (primary school or less vs other), number of children living in the home, and urbanicity (urban, rural). We also constructed a household material resources index based on motor vehicle ownership (car, motorcycle), and major household appliance ownership (e.g., refrigerator, stoves, washing machines, home computers). In addition, we included the other sources of school foods in each of the models.
We stratified the analyses by primary (5-12 years) and secondary school (13-17 years) separately as these 2 life course groups (i.e., middle childhood, adolescence) have differing metabolic requirements which can influence appetite, food preferences and behaviors, dietary intake, and body composition. 1 Published studies and our sensitivity analyses suggested that the 2 groups differ with respect to some of their sociodemographic, food environments of their schools, the diet and anthropometric outcomes of interest in this study, and certain covariates such as physical activity. We performed summary data, bivariate, and multivariate analyses using STATA (Stata Statistical Software: Release 16. StataCorp LLC, 2019). Sample and design weights provided by the ENSANUT survey were applied to account for its complex design. 25 P values < .05 (2-sided) were regarded as statistically significant.
Results
Participant Characteristics
Table 2 compares the sociodemographic characteristics of the 12632 primary and 6617 secondary school student participants. In addition to age, primary students spent a greater amount of time engaged in physical activities, more attended the morning school session, had better educated mothers, and fewer major household assets compared to secondary school students. However, the 2 groups did not differ on gender, ethnicity, urbanicity, or the region of Ecuador where they lived.
Sample Characteristics (n = 19249).
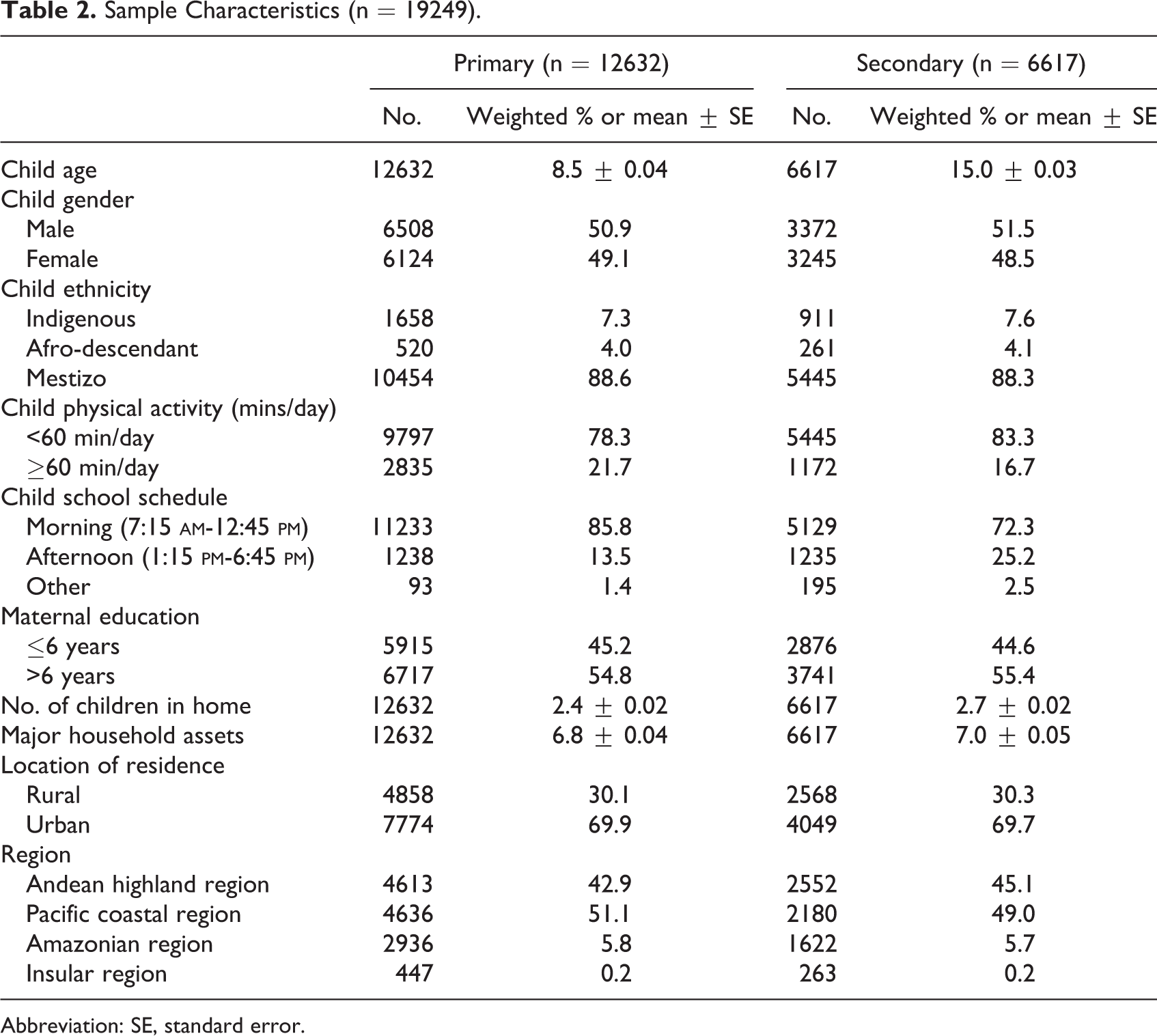
Abbreviation: SE, standard error.
School Food Environment
Most schools attended by the child participants were reported to have an on-campus school bar selling competitive foods and beverages (Figure 1). These commercial establishments were reported as more common in secondary than primary schools. More secondary than primary schools were reported to sell prohibited “red traffic light” processed foods. More also sold fruits and vegetables as per regulations but fewer provided free clean drinking water as required compared to primary students.
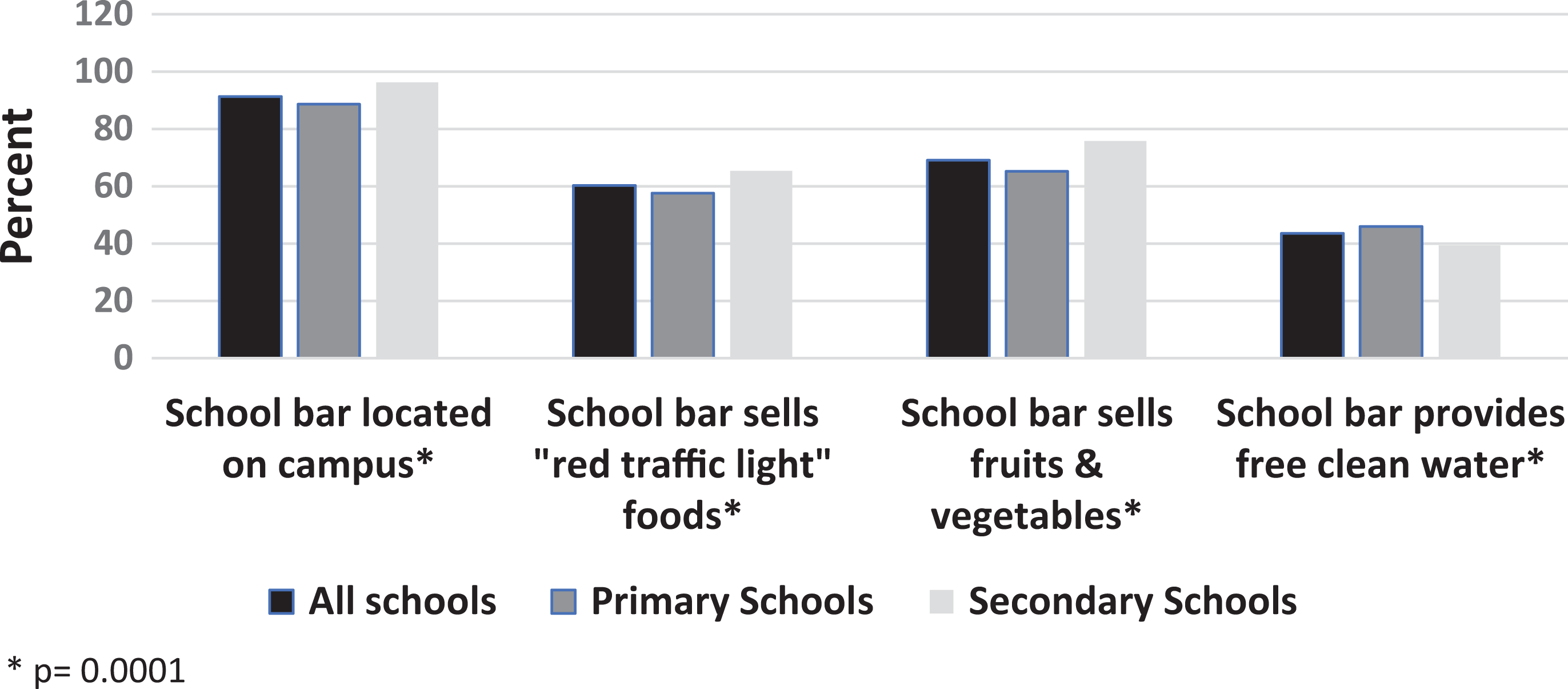
On-campus competitive food outlet (school bars) characteristics compared by primary versus secondary schools (n = 19249).
Competitive foods were the single most frequently reported source of school foods followed by those from the SBP, and foods brought from home (Figure 2). A larger proportion of secondary compared to primary students reported purchasing these. In contrast, more primary school students reported participating in the SBP and bringing foods from home to eat at school. Of children who brought any foods from home, 82%, 65.5%, and 47% reported bringing fruits, home-prepared items, and processed foods, respectively. The specific types of foods brought from home did not differ between the 2 student groups except for home-prepared foods which were more common among primary (79.9%) compared to secondary (65.5%) students (P = .0001).
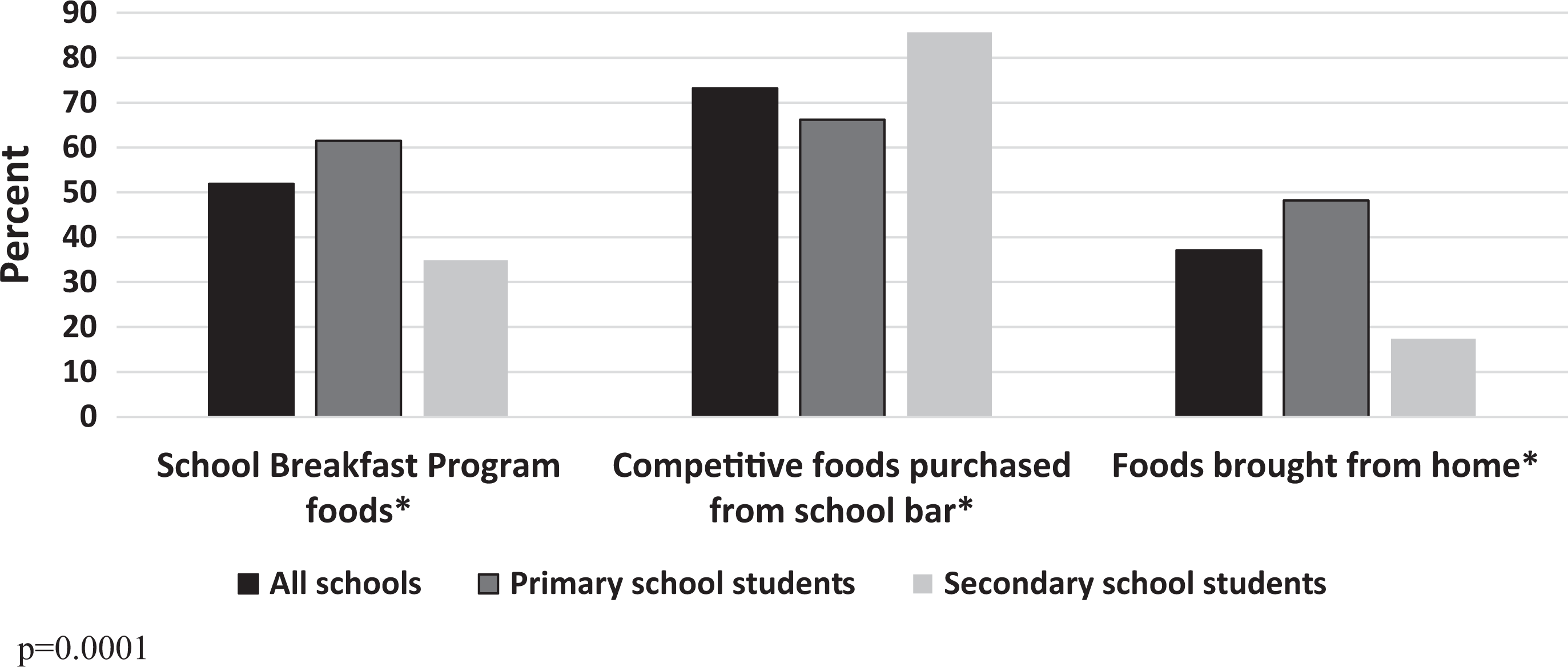
Sources of school food compared by primary versus secondary schools (n = 19249).
School Food Sources and Diet
Fruits, vegetables, and plain water
Primary school students had relatively low mean daily intakes of healthier foods and beverages including fruits (1.01 ± 0.02), vegetables (0.66 ± 0.01 servings/day), and plain water (3.89 ± 0.04 glasses/day). Fewer than 10% of primary students met the minimum dietary intake recommendations for fruits (7.0%), vegetables (7.7%), or plain water (8.7%).
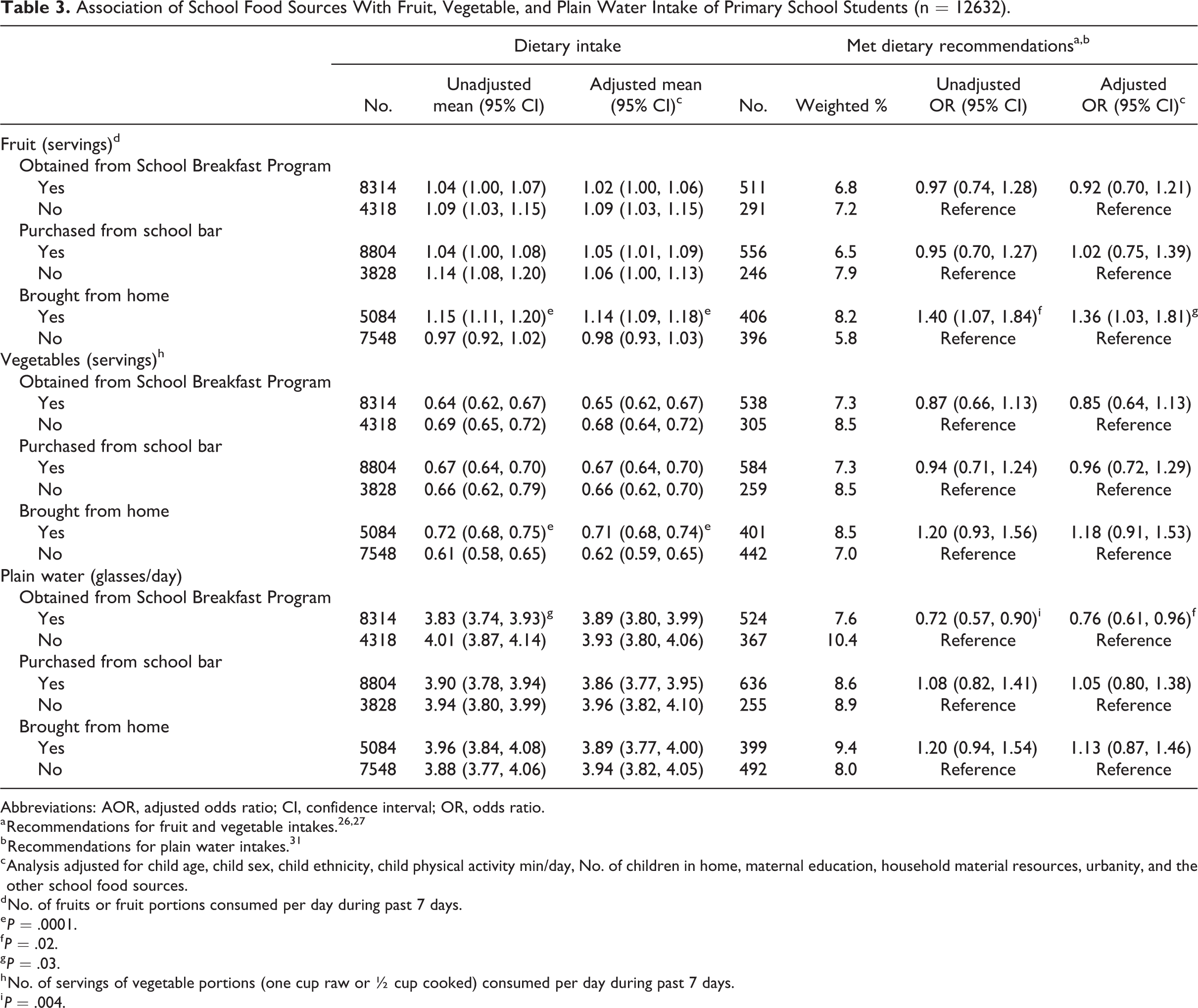
As Table 3 indicates, primary students who brought food from home to eat at school had higher unadjusted and adjusted mean intakes of both fruit and vegetables compared to those who did not pack food from home and were also around 40% more likely to meet fruit intake recommendations. No differences were identified in their water consumption patterns different from children participating in the SBP who had lower unadjusted and adjusted mean intakes of plain water and a 24% reduced adjusted odds of meeting plain water intake recommendations. No associations were identified for the mean fruit, vegetable, and plain water unadjusted or adjusted intakes or the proportion who met recommendations among children who purchased any competitive foods versus nonpurchasers.
Association of School Food Sources With Fruit, Vegetable, and Plain Water Intake of Primary School Students (n = 12632).
Abbreviations: AOR, adjusted odds ratio; CI, confidence interval; OR, odds ratio.
b Recommendations for plain water intakes. 31
c Analysis adjusted for child age, child sex, child ethnicity, child physical activity min/day, No. of children in home, maternal education, household material resources, urbanity, and the other school food sources.
d No. of fruits or fruit portions consumed per day during past 7 days.
e P = .0001.
f P = .02.
g P = .03.
h No. of servings of vegetable portions (one cup raw or ½ cup cooked) consumed per day during past 7 days.
i P = .004.
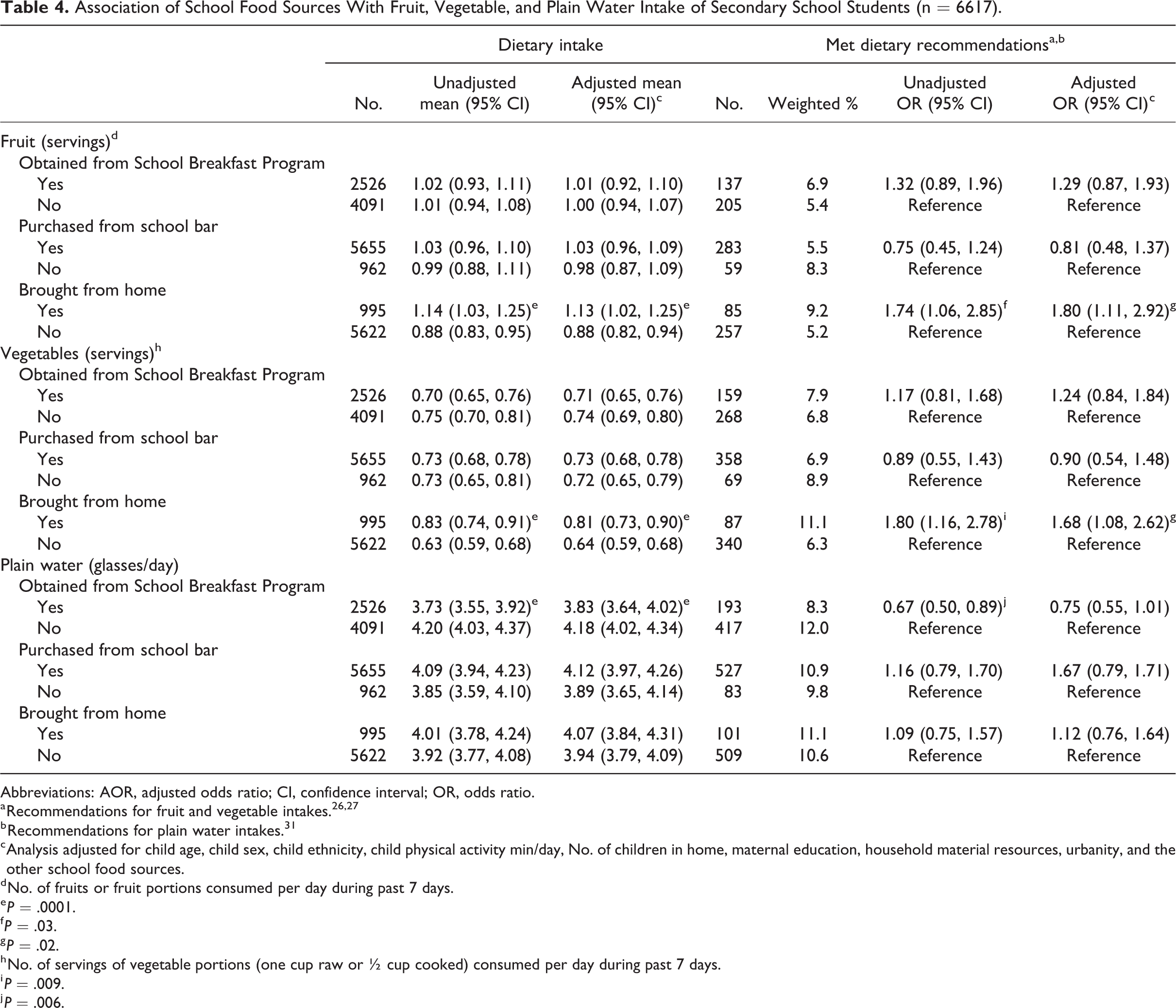
Secondary school students reported relatively low mean daily intakes of foods and beverages including fruits (0.94 ± 0.02 servings/day), vegetables (0.67 ± 0.02 servings/day), and plain water (4.10 ± 0.05 glasses/day). Fewer than 11% met recommendation for fruit (5.9%), vegetables (7.2%), or plain water (10.7%). As Table 4 shows, similar to primary students, secondary students who brought food from home to eat at school had higher unadjusted and adjusted mean fruit and vegetable but not plain water intakes compared to those who did not bring food from home and they also had a higher unadjusted and adjusted odds for meeting fruit intake recommendations. As the table also indicates, SBP participants had lower mean daily plain water compared to nonparticipants but not fruits or vegetables. No significant differences were identified for the fruit, vegetable, and plain water intakes of students who purchased on-campus competitive foods versus nonpurchasers.
Association of School Food Sources With Fruit, Vegetable, and Plain Water Intake of Secondary School Students (n = 6617).
Abbreviations: AOR, adjusted odds ratio; CI, confidence interval; OR, odds ratio.
b Recommendations for plain water intakes. 31
c Analysis adjusted for child age, child sex, child ethnicity, child physical activity min/day, No. of children in home, maternal education, household material resources, urbanity, and the other school food sources.
d No. of fruits or fruit portions consumed per day during past 7 days.
e P = .0001.
f P = .03.
g P = .02.
h No. of servings of vegetable portions (one cup raw or ½ cup cooked) consumed per day during past 7 days.
i P = .009.
j P = .006.
Sweetened beverages, processed snack foods, and fast foods
Primary school students reported consuming sweetened beverages, processed snack foods, and fast foods an average of 1.78 ± 0.03 days/week, 2.23 ± 0.03 days/week, and 0.98 ± 0.02 days/week, respectively. More than half exceeded dietary recommendations for sweetened beverages (72%), processed snacks (82.9%), and fast foods (55.2%).
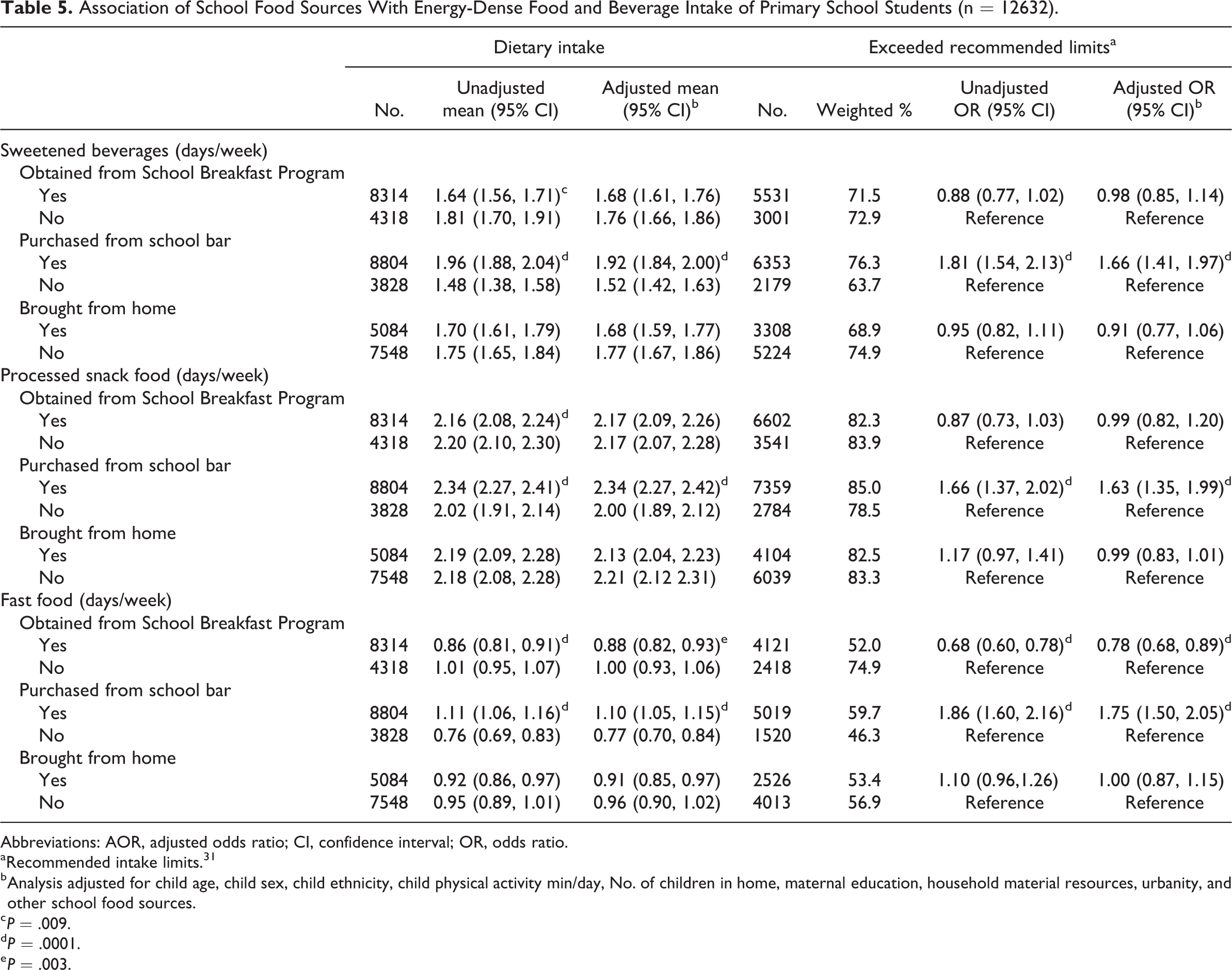
Table 5 shows that primary school students who purchased competitive foods had significantly higher unadjusted and adjusted mean intakes of all 3 energy-dense foods and beverages. They also had an adjusted odds for exceeding recommended limits for these foods and beverages that was increased by 25% or more compared to noncompetitive food purchasers. Primary school SBP participants had lower unadjusted and adjusted mean intakes of fast foods as well as a 22% reduced odds for exceeding recommended limits for these items. Although SBP participants had lower average unadjusted intakes of sweetened beverages and processed snacks than nonparticipants, after covariate adjustment, these associations were no longer evident in the statistical models. Table 5 also shows that neither the unadjusted nor adjusted mean intakes of the 3 categories of energy-dense foods differed significantly between children who brought food from home versus those who did not pack food from home.
Association of School Food Sources With Energy-Dense Food and Beverage Intake of Primary School Students (n = 12632).
Abbreviations: AOR, adjusted odds ratio; CI, confidence interval; OR, odds ratio.
a Recommended intake limits. 31
b Analysis adjusted for child age, child sex, child ethnicity, child physical activity min/day, No. of children in home, maternal education, household material resources, urbanity, and other school food sources.
c P = .009.
d P = .0001.
e P = .003.
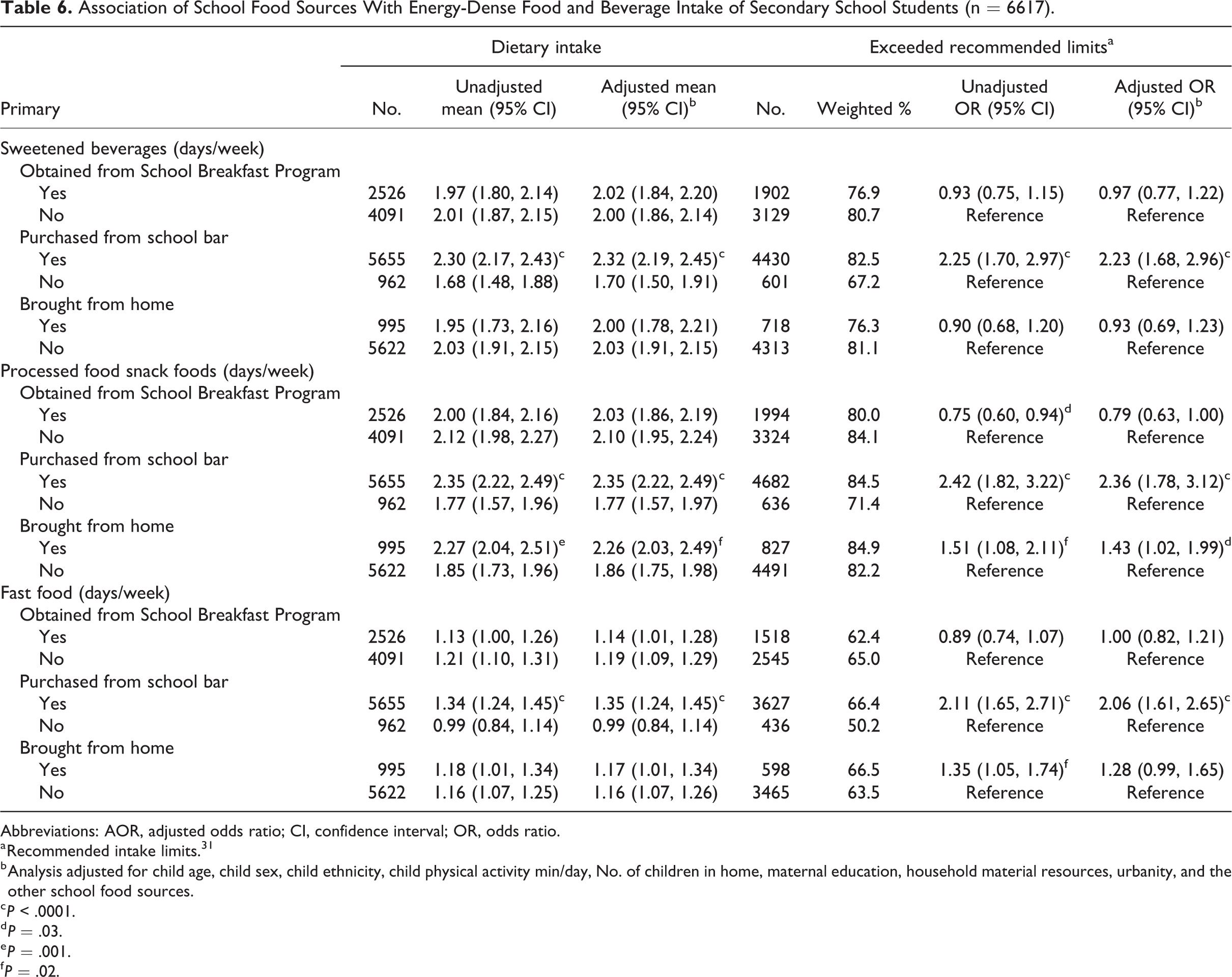
Secondary school students consumed sweetened beverages, processed snack foods, and fast foods averaged 2.24 ± 0.04 days/week, 2.15 ± 0.04 days/week, and 1.30 ± 0.04 days/week. More than 60% exceeded recommended limits for sweetened beverages (80.3%), processed snack foods (82.2%), and fast foods (64.1%). Table 6 indicates that secondary school students who bought competitive foods from their school bar had higher unadjusted and adjusted intakes of sweetened beverages, processed snack, and fast foods compared to nonpurchasers and their odds for exceeding recommended intake limits for all 3 food groups was more than doubled. The table also shows that students who brought food from home had both higher mean unadjusted and adjusted intakes of processed snack foods and an unadjusted and adjusted odds of exceeding recommended intake limits for this food group that was at least 40% higher than those who did not pack home food to eat at school.
Association of School Food Sources With Energy-Dense Food and Beverage Intake of Secondary School Students (n = 6617).
Abbreviations: AOR, adjusted odds ratio; CI, confidence interval; OR, odds ratio.
a Recommended intake limits. 31
b Analysis adjusted for child age, child sex, child ethnicity, child physical activity min/day, No. of children in home, maternal education, household material resources, urbanity, and the other school food sources.
c P < .0001.
d P = .03.
e P = .001.
f P = .02.
School Food Sources and BMI
The mean BMI of the 5 to 12 year old primary school students was 18.4 ± 0.03. The BMI-for-age measurements classified 2.4% as underweight, 22.3% as overweight, and 15.6% as obese.
Compared to nonparticipants, primary children participating in the SBP had a significantly lower unadjusted BMI compared to nonparticipants (18.1 ± 0.04 vs 18.8 ± 0.06; P = .0001). Likewise, after they were adjusted for child age, sex, and other model covariates, their mean BMI was also reduced compared to nonparticipants (18.2 ± 0.04 vs 18.6 ± 0.06; P = .0001). As Table 7 shows, their unadjusted and adjusted odds for obesity were reduced, respectively, by 31% and 24%, compared to nonparticipants although they were similar regarding their odds for underweight or overweight.
Primary school children who purchased competitive foods from their school bar had a higher unadjusted mean BMI compared to those who did not (18.6 ± 0.04 vs 17.9 ± 0.06; P = .0001). However, after adjustment for model covariates their mean BMI was similar (18.3 ± 0.04 vs 18.4 ± 0.06; P > .05). They also did not differ in their unadjusted or adjusted odds for underweight, overweight, or obesity (Table 7). Primary school students who brought food from home to eat at school had a lower unadjusted mean BMI (18.0 ± 0.05 vs 18.6 ± 0.05; P = .0001) than those who did not bring any food from home but their covariate adjusted mean BMIs did not differ significantly (18.3 ± 0.05 vs 18.4 ± 0.04; P > .05) nor did either their unadjusted and adjusted underweight, overweight, and obesity odds (Table 7).
The mean BMI of the secondary school students aged 13 to 17 years in the study was 21.9 ± 0.06. Their BMI-for-age measurements suggested that 1.9% were underweight, 23% were overweight, and 6.4% were obese. Those who participated in the SBP had a lower unadjusted (21.6 ± 0.07 vs 22.1 ± 0.06; P = .0001) but not adjusted BMI (21.8 ± 0.07 vs 22.0 ± 0.06; P > .05) compared to nonparticipants. They also did not differ regarding their odds for underweight, overweight, nor obesity (Table 5). Secondary students who bought competitive foods at school had similar unadjusted (21.9 ± 0.05 vs 21.9 ± 0.12; P > .05) and adjusted mean BMIs to nonpurchasers (21.9 ± 0.05 vs 22.0 ± 0.11; P > .05) as well as unadjusted and adjusted odds for underweight, overweight, or obesity (Table 7). The unadjusted (22.0 ± 0.11 vs 21.9 ± 0.05; P > .05) and adjusted BMIs (21.9 ± 0.11 vs 21.9 ± 0.05; P > .05) of students who brought food from home to eat at school were similar to those who did not bring food from home as were their unadjusted and adjusted odds for underweight, overweight, and obesity odds (Table 7).
Association of School Food Sources With BMI-for-Age Categories in Primary and Secondary School Students.
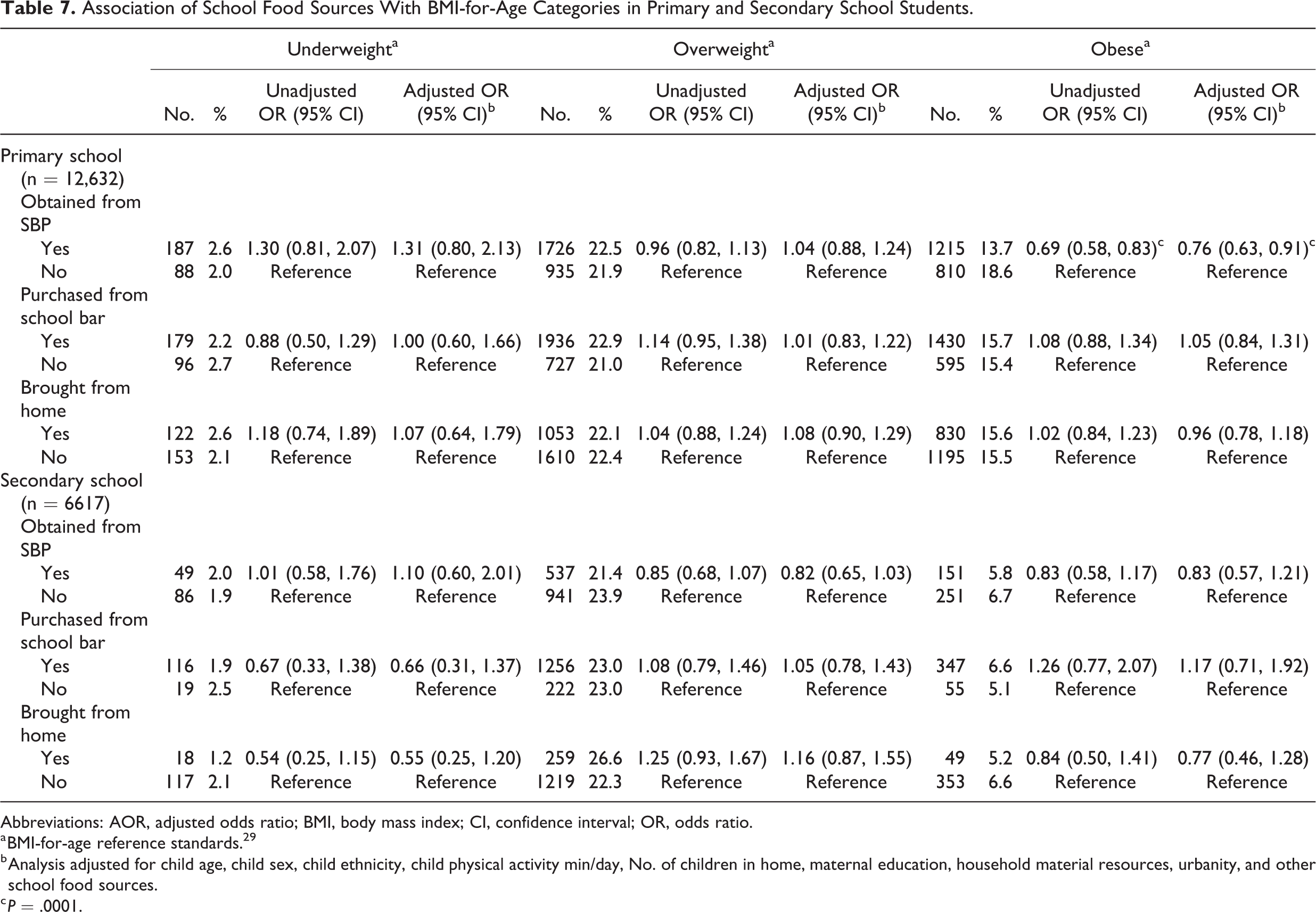
Abbreviations: AOR, adjusted odds ratio; BMI, body mass index; CI, confidence interval; OR, odds ratio.
a BMI-for-age reference standards. 29
b Analysis adjusted for child age, child sex, child ethnicity, child physical activity min/day, No. of children in home, maternal education, household material resources, urbanity, and other school food sources.
c P = .0001.
Discussion
The study findings underscore the importance of the school food environment on the diets of primary and secondary school children. Of the 3 major school food sources examined, competitive foods purchased on campus had the largest apparent overall impact on the consumption of less healthy energy-dense foods including sweetened beverages, processed snacks, and fast foods in both primary and secondary students. In contrast, foods brought from home had the greatest overall impact on primary and secondary student fruit and vegetable intakes. The overall impact of SBP participation on child diet was less apparent except for lower fast food intakes in primary students and plain water intakes in both student groups which were unexpectedly reduced in participants compared to nonparticipants. However, different from the other 2 food sources, SBP participation was associated with a 25% reduction in the adjusted odds for obesity in primary students.
The high proportion of competitive food outlets on Ecuadorian campuses concurs with studies identifying these as ubiquitous in other Latin America country schools. 32 -36 The high proportion of schools selling “red traffic light” foods whose sale is legally banned in Ecuador 37 is even higher than that found in a smaller 2014 survey. 38 Similar findings have been reported in school located in other countries throughout the region even in those prohibiting their sale. 33,34,36,39 -42
The reasons for the high level of noncompliance with red traffic light food regulations is unclear. While it is possible that some Ecuadorian vendors may lack a clear understanding of regulations, this seems unlikely since to operate a school bar in Ecuador selling competitive foods, vendors are required to pass a structured course that includes specific training on red traffic light and other regulated foods. 43 The findings from studies conducted in Chile and Costa Rica indicated that the reasons given by vendors for their noncompliance included poor enforcement by authorities, the desire to be able to make higher profits, and the notion that if they don’t sell these items, children will go elsewhere to buy them including off campus. 42,44 In any case, the continuing sale of prohibited red traffic light foods in Ecuadorian schools normalizes their consumption and directly contradicts national food-based guide recommendations, 28 national and school nutrition education mass media, and other messaging directed at children, 31 parents, 27,45 teachers, 28 nutrition educators, 46 and others. 31
We identified the purchase of competitive foods from school bars as an important source of the less healthy energy-dense foods examined in this study for both primary and secondary students. This finding is consistent with other studies conducted in Colombia, 35 Brazil, 32,47,48 Mexico, 49 and Guatemala. 50 We also found that while 69% of these outlets sold fruits and vegetables and 44% provided free clean drinking water as required, this did not appear to have a measurable impact on the intakes of these healthier items by children who bought competitive foods. Fruit and vegetable consumption among school-age Ecuadorian children is reported to be relatively low. 17 Thus, it is unclear that the apparent lack of impact on the consumption of fruit, vegetables, and plain water was because children do not like to consume these or their higher intakes of energy-dense foods displaced these in the diet as has been reported for other Latin American school students. 49,51,52 This is an important question that requires attention in future studies.
Another notable finding was that even though primary and secondary students who purchased competitive foods had higher intakes of energy-dense foods and beverages and also exceeded recommended limits for these, they were not more likely to be overweight or obese compared to nonpurchasers. Since they consumed these foods 2 days or fewer per week, it is possible that the intake of these foods at school was insufficient to have caused them to have developed overweight or obesity. The very few studies that examined the association of competitive school food policies, availability, and/or purchases with either obesity risk or other anthropometric indicators in adolescent secondary students have reported mixed results. 41,53,54
The higher fruit and vegetable intakes identified for Ecuadorian schoolchildren who brought food from home triangulates with the other data from this survey identifying fruit as the most common food brought from home (82%) followed by home-prepared dishes (66%) some of which may have included vegetables. Different from this study, most authors reporting on foods brought from home by Latin American schoolchildren focused on those eaten for lunch rather than breakfast and snacks. However, if one includes studies of all foods brought from home for any meal or snack, then our findings are generally consistent with those reporting that foods brought from home by Mexican schoolchildren tended to be healthier than those bought at school 55 and another noting that Brazilian adolescents often pack fresh fruits and vegetables from home as well as processed foods. 56 However, they differ from other studies reporting that Mexican and Guatemalan primary school students tended to bring less healthy, energy-dense foods. 55 -57
Ecuadorian mothers usually have major responsibility for household food selection, preparation, and serving. That, along with modeling eating behaviors by them and other family members, can be an important influence on the shaping the child food behaviors. These findings suggest that Ecuadorian moms appear to have strong positive influence on the food brought from home, especially for younger primary school students. We surmise that integrated school nutrition education and mass media campaigns focused on the importance of fruits, vegetables, and other healthy foods in child diets may have had a positive impact on the foods that mothers select for their children to bring to school. It is also the authors’ experience that Ecuadorian teachers play an important role in reinforcing what constitutes acceptable foods brought from home. However, we also note that since secondary students were more likely to bring processed snack foods from home, they may have had more autonomy than younger primary schoolchildren regarding the foods selected to bring to school.
School Breakfast Program participation appeared to have a relatively small, mixed impact on intake of the food and beverage groups assessed in this study. On the one hand, both primary and secondary students in the SBP had lower water intakes than nonparticipants. Primary but not secondary school SBP participants also were less likely to meet water intake recommendations. On the other hand, primary students in the SBP ate fast foods less frequently and were less likely to exceed recommended limits for this less healthy food group. It is possible that the SBP foods and beverages could have displaced plain water and fast food in participant diets. The lack of prior studies published on the impact of any type of school feeding programs, especially for child water intake, makes comparisons of our findings difficult with other Latin American child groups. Very few studies have specifically focused on the dietary impacts of school breakfast or snack programs in Latin American countries. 58 -60 The foods types provided by these programs were very diverse ranging from fortified foods to fruits to cereals to sweets. Also different from our study, their focus was on dietary energy and micronutrient intakes. 58 -60 Although micronutrient biomarkers were not collected by present survey, it is possible that the multifortified foods provided by the Ecuadorian SBP may have a beneficial influence on the vitamin A, iron, and zinc intakes of child participants. This should be investigated by future studies since these have been identified as micronutrients of concern for both school-age children and adolescents in Ecuador. 17
Like red traffic light label and other types of foods sold in many Ecuadorian school bars, those provided by the SBP (except ultra-high temperature (UHT) whole milk) normalizes the consumption of processed and ultraprocessed foods and beverages. They directly conflict with national food-based guidelines 31,45,46 and school-based nutrition education messaging 27 -29 on the importance of diverse, culturally appropriate diets based on fresh and minimally processed foods. In addition, the aseptic packaging used for SBP foods and beverages is reported to create large amounts of inorganic waste that further contributes to Ecuador’s growing solid waste problem and environmental degradation. 61,62 Plate waste also seems to be common due to the reported dislike of many of the processed products and the limited offerings in the rotation resulting in flavor fatigue. Although not covered in the present survey, this issue has been a topic of serious concern expressed by school administrators, teachers, mothers, and children in published articles 23,61,63 and mass-media articles. 64,65 In 2020, the Ecuadorian national congress approved a new school food law authorizing changes in the SBP. Although its implementation has been delayed due to COVID and funding-related challenges, the changes include the provision of more varied, fresh and nutritious foods, including fruits, vegetables, and traditional grains sourced from small- and medium-size local farms. 66
The few studies examining the association of SBP programs and BMI among Latin American primary school children have reported mixed findings. One reported a lack of difference in the prevalence of obesity in Mexican primary schoolchildren participating in a SBP. 67 In addition, the pre- and post-test results of another study reported cold breakfast foods provided by the SBP was associated with increased weight gain in Mexican primary school children but not to the point of overweight or obesity. 68 In our study, primary school students who participated in the SBP had a lower adjusted mean BMI and an odds for obesity that was decreased by 24% compared to SBP nonparticipants. We surmised that this could be because child SBP participants are more likely to come from poorer households as indicated by their lower material resource scores. Our post hoc analysis indicated that child SBP participants resided in households with fewer material resources compared to those who purchased competitive food at school or brought it from home to eat (material resources score = 6.4 vs 6.8 vs 6.9; P = .001). Being from a lower resource Ecuadorian household could impact their dietary energy intakes enough to reduce their risk for obesity. There is some evidence of this since SBP participants had significantly lower overall intakes of high-calorie sweetened beverages, snack and fast foods compared to nonparticipants. This could have because these foods were not available in their homes and/or because children had less pocket money to be able to purchase these foods. Alternatively, it could have been because SBP breakfast foods provided satiety which made the children less likely to consume energy-dense foods and beverages from any course.
The strengths and limitations of this study should be considered when interpreting its findings. Some strengths of the nationally representative survey include its large sample size, low nonresponse rate, use of standardized data collection procedures, and quality control methods. 25 One limitation was its cross-sectional design which permits inference but not establishment of causal effects. Except for measured weight and height, the data collected on school food sources, diet, and other indicators were self-reported by the child participants and/or their parents. Self-reported data can result in recall bias, under-or over-estimation of the intakes of certain foods and beverages, and other types of biases (e.g., social approval, social desirability). Another limitation was that although the survey asked about all-source dietary intake, it collected data on only 6 food and beverage groups and covered a relatively short time frame, that is, past 7 days. Future studies should include a larger number of foods and longer time periods in order to provide a more complete estimate of child diet. The survey also did not collect data on potential additional sources of food that students may have consumed at school such as that obtained from other children, street food vendors, micromercados, and restaurants. Future studies should collect data on these. Data should also be collected on the foods that children consume while at home or obtain from other nonschool sources in order to better understand the relative contribution of school food sources to overall diet. Another limitation was that for children who brought food from home, data were not collected on who had primary responsibility for packing food from home, that is, child, parent, or both. Furthermore, the analysis of the impact of school food sources on child nutrition was limited to diet and weight and height measurements. Future investigators should examine other important nutrition indicators such as waist circumference and micronutrient status.
In conclusion, the findings from this study underscore the important influence of the school food environment on the intakes of both healthier and less healthy foods. These suggest that competitive items purchased from school bars appeared to have the greatest overall negative dietary impact on child diet while foods those brought from home had the greatest overall positive impact. The SBP appeared to have a small, mixed impact on intakes of the 6 food and beverage groups assessed in the study. Our findings address an existing gap in the literature on the school food environments in Latin American LMICs, including Ecuador. They provide data that can be used to inform policy and potential intervention strategies that can be used to promote healthier eating and improve the nutritional status of primary and secondary schoolchildren.
Footnotes
Authors’ Note
Conceptualization (MMW, RXA), data analysis (MMW), initial draft (MMW), article review and editing (MMW, RXA), approval of version to be published (MMW, RXA), public responsibility for article (MMW, RXA). The data that support the findings from this secondary data analysis are publicly available from the Ecuadorian National Institute of Statistics and Census at: https://www.ecuadorencifras.gob.ec/salud-salud-reproductiva-y-nutricion/. Informed consent was obtained from the participants involved in the survey. The de-identified database used for the secondary analyses is classified as “research not subject to human subjects regulations” by the Indiana University Institutional Review Board (![]() ).
).
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
