Abstract
Background:
Inappropriate infant and young child complementary feeding practices related to a lack of maternal knowledge contributes to an increased risk of malnutrition, morbidity, and mortality. There is a lack of data regarding the effect of nutrition education on maternal knowledge, feeding, and hygiene practices as part of a supplementary feeding intervention targeting infants and young children with moderate acute malnutrition in low-income countries like Uganda.
Objective:
To determine whether nutrition education improves knowledge, feeding, and hygiene practices of mothers with infants and young children diagnosed with moderate acute malnutrition.
Methods:
A cross-sequential study using a pretest–posttest design included 204 mother–infant pairs conveniently sampled across 24 randomly selected clusters. Weekly nutrition education sessions were embedded in a supplementary porridge intervention for 3 months. Mean scores and proportions for knowledge, feeding, and hygiene practices were determined at baseline and end line. The difference between mean scores at the 2 time points were calculated with the paired t test analysis, while the proportions between baseline and end line were calculated using a z test analysis.
Results:
Mean scores for knowledge, dietary diversity, and meal frequency were higher at end line compared to baseline (P < .001). Handwashing did not improve significantly (P = .183), while boiling water to enhance water quality improved (P < .001).
Conclusion:
Nutrition education in conjunction with a supplementary feeding intervention targeting infants and young children with moderate acute malnutrition improved meal frequency, dietary diversity and water quality.
Keywords
Introduction
Globally, undernutrition contributes to an estimated 60% of under-5 mortality. 1 In developing countries, approximately one-third of infant and young child (IYC) deaths are associated with underlying causes of undernutrition, 2 with an estimated two-thirds being due to inappropriate complementary feeding practices. 3,4 In sub-Saharan Africa, IYC between 6 and 23 months with moderate acute malnutrition (MAM) are more vulnerable to inadequate food intake due to inappropriate feeding and hygiene practices, as it can result in high morbidity and mortality rates. 5 Childhood infections, such as diarrhea and poor feeding practices including low meal frequency and a lack of dietary diversity, contribute to delayed recovery from MAM. 6,7 However, good hygiene practices, especially handwashing with soap, reduce the risk of diarrhea by 23%. 8 Nutrition education on appropriate feeding and hygiene practices that target mothers of IYC has been reported to significantly improve knowledge, nutritional status, and minimize disease when combined with the provision of supplementary foods in the management of MAM. 2,6
Optimal feeding and hygiene practices, therefore, have the potential to prevent growth faltering among breastfed IYC with MAM. 7,9 However, it has been reported that supplementary feeding interventions either lack or provide inadequate nutrition education. 5 Further, where nutrition education was conducted in low-income countries, there is a paucity of data documenting the impact thereof on mothers’ knowledge regarding IYC complementary feeding and hygiene practices. 2,5,6 It is possible that the nutrition education given to mothers could be inadequate to facilitate an improvement in their knowledge. 2 -6 Seemingly, the changes implemented by mothers as a result of nutrition education have not been adequately documented in low-income settings. Therefore, the aim of this study was to determine the effect of nutrition education on nutrition knowledge, complementary feeding, and hygiene practices as part of the management strategy of IYC aged 6 to 18 months diagnosed with MAM based on the Health Belief Model constructs in Uganda.
Methods
Study Design
A cross-sequential approach employing a pretest–posttest design was used to determine knowledge, feeding, and hygiene practices among breastfeeding mothers of IYC diagnosed with MAM who received nutrition education for a period of 3 months while receiving a supplementary porridge for their IYC. Seven to 9 mother-IYC pairs were conveniently sampled from 24 randomly selected clusters. In 12 of the clusters, mothers fed their IYC with a malted sorghum–based porridge (MSBP), a novel supplementary porridge formulated as part of the overarching cluster randomized controlled trial of which nutrition education was a component, while in the remaining 12 clusters IYC were fed with a corn soy–based supplementary porridge (CSB+) serving as a control.
Study Setting
This study was embedded in a community-based cluster randomized controlled trial that determined the effect of MSBP versus CSB+ supplementation, in conjunction with nutrition education of breastfeeding mothers, on IYC with MAM feeding and hygiene practices. Study participants resided in 4 subcounties of a rural district of Arua in West Nile, North Western Uganda. The region is characterized by a high prevalence of wasting (13.6%) among IYC. 10
Participant Recruitment
Two-hundred and four (N = 204) mothers of IYC aged between 6 and 18 months were recruited to participate in either the MBSP or CSB+ supplementation arm of the study. Each supplementation arm consisted of 12 clusters that were randomly allocated to either a treatment or control group in a ratio of 1:1. A cluster consisted of 8 to 10 mother-IYC pairs recruited per cluster. A week after enrollment, participants were approached and recruited to participate in the nutrition education study.
Nutrition Education
The nutrition education intervention was implemented based on the premise of the Health Belief Model, 11 to improve maternal complementary feeding and hygiene practices. It was believed that when mothers acquire knowledge through nutrition education, it will be internalized to result in behavioral change. 12,13 The nutrition education was conducted in Lugbarati, the local language spoken by 2 health workers who served as research assistants on a weekly basis for a period of 3 months. The contents of the education sessions with a duration of up to 60 minutes included information on appropriate feeding and optimal hygiene practices, using a standardized counseling card. 14 Face-to-face group education and discussion sessions in addition to practical demonstrations regarding the preparation of the supplementary porridges were used throughout the nutrition education intervention. Key messages conveyed included breastfeeding before giving the IYC the supplementary porridge or other household foods. In addition, active feeding practices such as feeding the IYC 3 times a day were encouraged, as well as feeding an appropriate amount of supplementary porridge of an appropriate consistency to ensure an optimal energy and nutrient intake. Regular handwashing to prevent IYC diarrhea was also promoted, as was the use of previously boiled water for drinking. The promotions of other appropriate IYC food preparation techniques that are known to prevent disease were also included. Before introducing a new topic, a review of content previously covered and an overview of previous group discussions were held to obtain feedback from mothers and discuss what was learnt during the previous session, as well as how this information was being implemented at the participant’s home.
Data Collection and Measurement
Face-to-face interviews were conducted with mothers after they signed an informed consent form in the local language at their nutrition education sites. Pretest and posttest data were collected using a semi-structured questionnaire that was administered by the same trained research assistant to avoid personal intervariability 15 and ensure validity. The Ugandan Demographic and Health Survey (2016) questionnaire was adapted for the purpose of this study. 10 Participant sociodemographic data were collected after expert input was gained on the questionnaire developed for the purpose of this study. The questions in the guidelines for assessing nutrition-related knowledge were adapted and modified after expert input to facilitate data collection regarding mother’s feeding and hygiene practices. 16 The mother’s knowledge scores for either feeding practices or hygiene practices were a sum of the correct responses out of a total score of 8. A score of 1 to 3 was classified as poor knowledge, while a score of 4 to 8 was classified as a high knowledge for either complementary feeding practices (dietary diversity and meal frequency) or hygiene practices (water quality and food safety).
A 24-hour recall was used to determine the dietary diversity score of IYC. The minimum dietary diversity score was determined with reference to the World Health Organization 7 recommended food groups. 14 Each of the 7 food groups was allocated a score of 1. However, breast milk was not allocated a score. 17 The dietary diversity scores were recorded as adequate for IYC who consumed 4 or more food groups. 17,18 The number of times the IYC consumed solid, semisolid, or soft foods (other than liquids) within 24 hours was determined using meal frequency questions. 17
Data Quality
The survey questionnaire was translated into the local language (Lugbarati) and back-translated into English in order to ensure content validity. Four research assistants used for data collection were trained in appropriate questionnaire administration techniques prior to data collection. Two experienced research assistant responsible for conducting nutrition education were trained on appropriate IYC feeding practices, water quality, food preparation, and food hygiene messages. A pilot study was conducted among 24 breastfeeding mothers in an area with characteristics similar to the study area to pretest the survey instruments prior to commencement of data collection. Where inconsistencies were found, questions were adjusted by paraphrasing prior to commencement of data collection. Face-to-face interviews were conducted in Lugbarati, the local language spoken by mothers and trained research assistants. The response to each questionnaire was reviewed for completeness and consistency before leaving the field. After data collection, all questions were coded and cleaned before double data entry was performed to ensure accuracy. Mothers’ knowledge and feeding practices regarding meal frequency, dietary diversity, and hygiene practices were analyzed as mean scores and proportions at baseline and end line (3 months).
Data Analysis
Stata/SE 15.0 statistical software was used to generate descriptive statistics. Baseline and end line data were analyzed and presented as proportions and mean scores. The z test was used to compare mothers’ knowledge proportions regarding water quality, IYC feeding, and hygiene practices between the MSBP and CSB+ groups. The paired t test was used to compare feeding and hygiene practice mean knowledge scores between baseline and end line data. A P value of ≤ 0.5 was considered statistically significant.
Ethical Considerations
Ethical approval to conduct this study was obtained from the Biomedical Research Ethics Committee (BE218/18) of the University of KwaZulu-Natal South Africa, the Higher Degrees, Research and Ethics Committee (REC/11353/394) of the School of Public Health, Makerere University Uganda, and the Uganda National Council of Science and Technology (SS4705). Informed consent forms were signed by participants who were literate, while illiterate participants made a thumbprint on the informed consent form prior to participation in the study. All participants were guaranteed confidentiality and anonymity as they were assigned a coded number for identification purposes.
Results
Sociodemographic Characteristics
The majority of mothers (84.3%) were younger than 35 years, while 70.1% had a primary school education. Thirty-one (15.1%) had no formal education. In addition, 21.1% were underweight (body mass index less than 18.5 kg/m2).
Baseline Characteristics
There was no significant difference in IYC feeding and hygiene practices between the proportions of participants who were in the MSBP group compared to those in the CSB+ group. Nearly one-fifth (19.1%) of mothers reported that they practiced appropriate IYC feeding practices, whereas 16.2% had adequate knowledge regarding food safety and water quality practices.
Mean Knowledge Scores Regarding Feeding and Hygiene Practices
There was a significant difference between mothers’ mean knowledge score regarding IYC feeding and hygiene practices at 3 months end line compared to baseline, irrespective of the supplementary porridge received, with a significant difference (P < .001) between mothers’ mean knowledge score regarding complementary feeding and hygiene practices at 3 months when compared to baseline and end line (Table 1).
Mean Knowledge Scores Regarding Appropriate IYC Feeding and Hygiene Practices at Baseline Versus 3 Months.
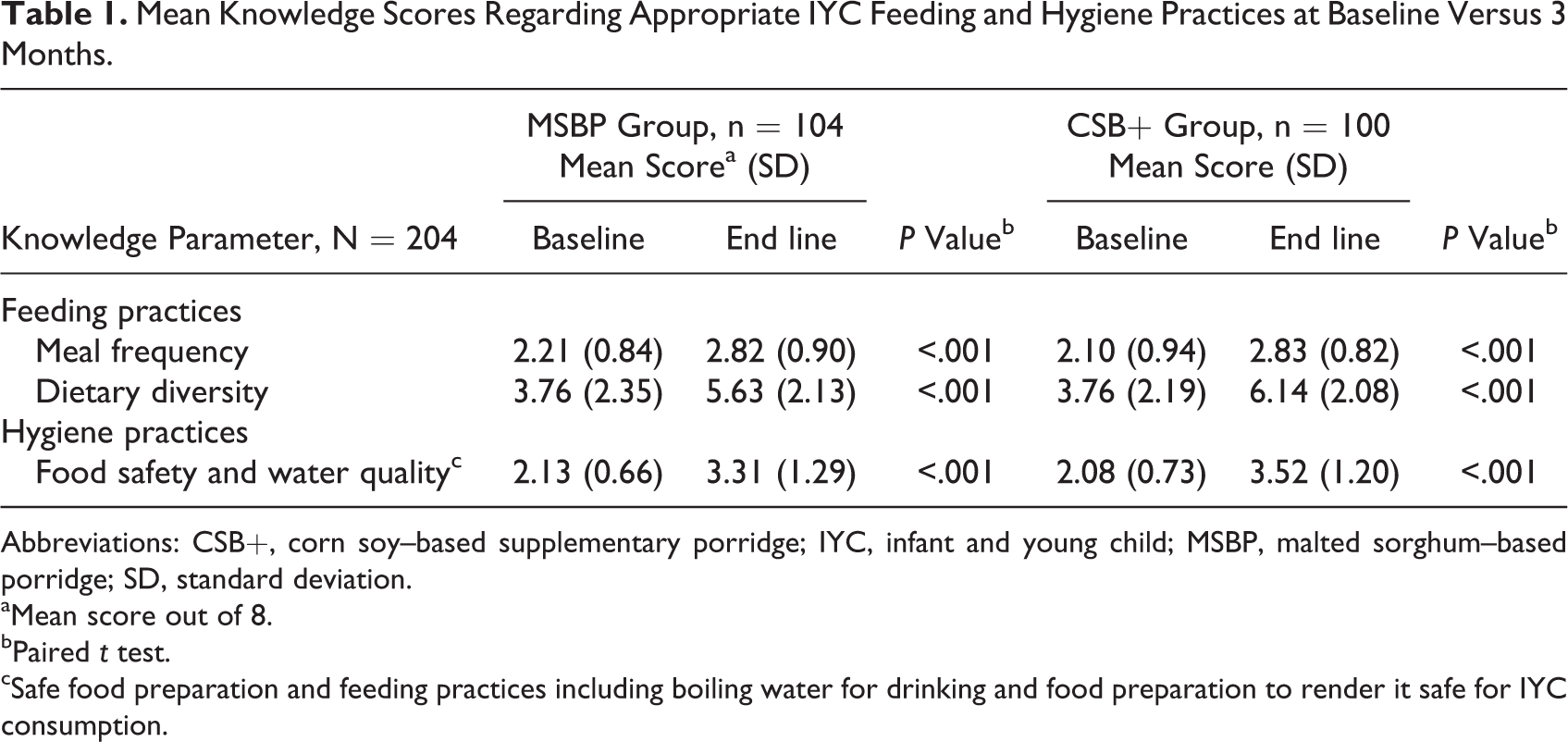
Abbreviations: CSB+, corn soy–based supplementary porridge; IYC, infant and young child; MSBP, malted sorghum–based porridge; SD, standard deviation.
aMean score out of 8.
bPaired t test.
cSafe food preparation and feeding practices including boiling water for drinking and food preparation to render it safe for IYC consumption.
Feeding and Hygiene Practice Proportions
As shown in Table 2, appropriate IYC feeding and hygiene practice proportions differed significantly at 3 months when compared to baseline (P < .001) for all variables, except for handwashing. The IYC dietary diversity score at 3 months improved 6-fold when compared to baseline. In addition, there was a significant difference between baseline and 3-month dietary diversity scores (P < .001). The z test results reported in Table 3 indicated that the IYC feeding practice of feeding 3 or more meals per day differed significantly between mothers in the CSB+ group compared to those in the MSBP group at 3-month follow-up. However, the practice of making water and food safe for consumption differed significantly between MSBP mothers compared to their CSB+ counterparts at baseline. The remainder of other IYC feeding and hygiene practices did not differ between groups at end line.
Comparison of the Proportions of Feeding and Hygiene Practices at 3 Months.
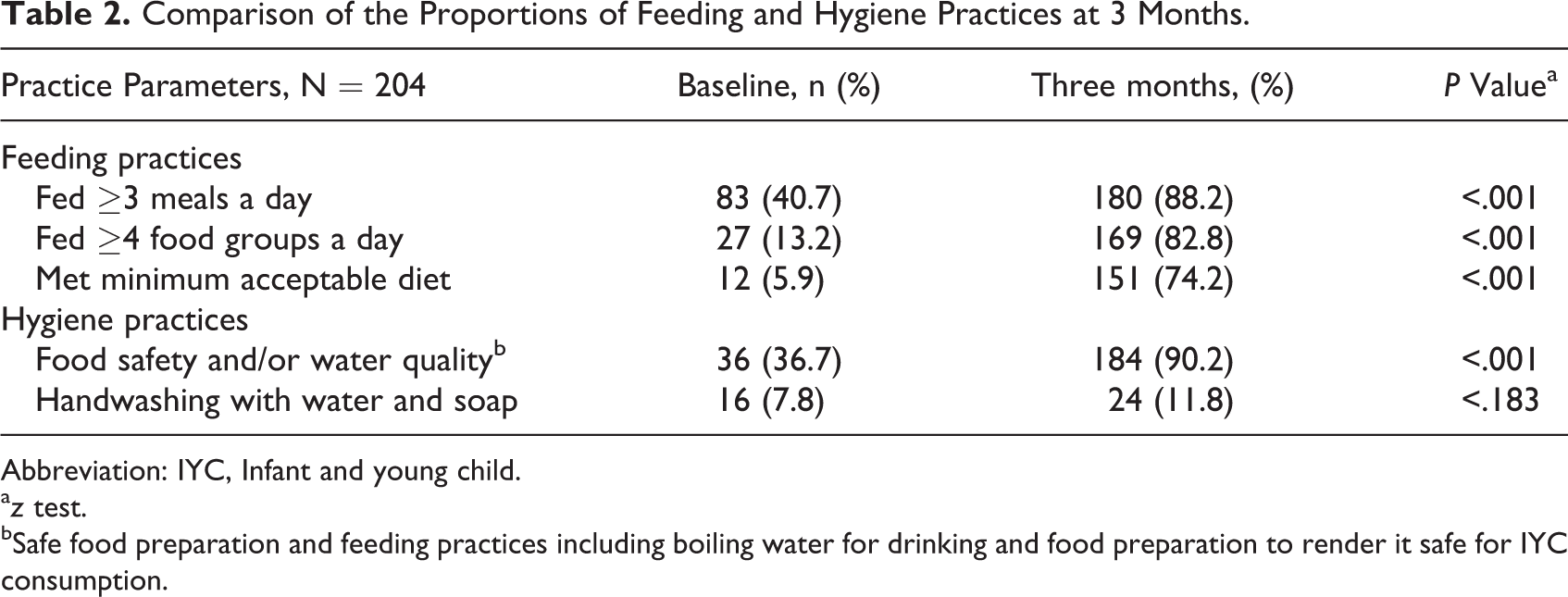
Abbreviation: IYC, Infant and young child.
az test.
bSafe food preparation and feeding practices including boiling water for drinking and food preparation to render it safe for IYC consumption.
IYC Feeding and Hygiene Practices Between Baseline and 3-Month Follow-Up by Supplementary Groups.
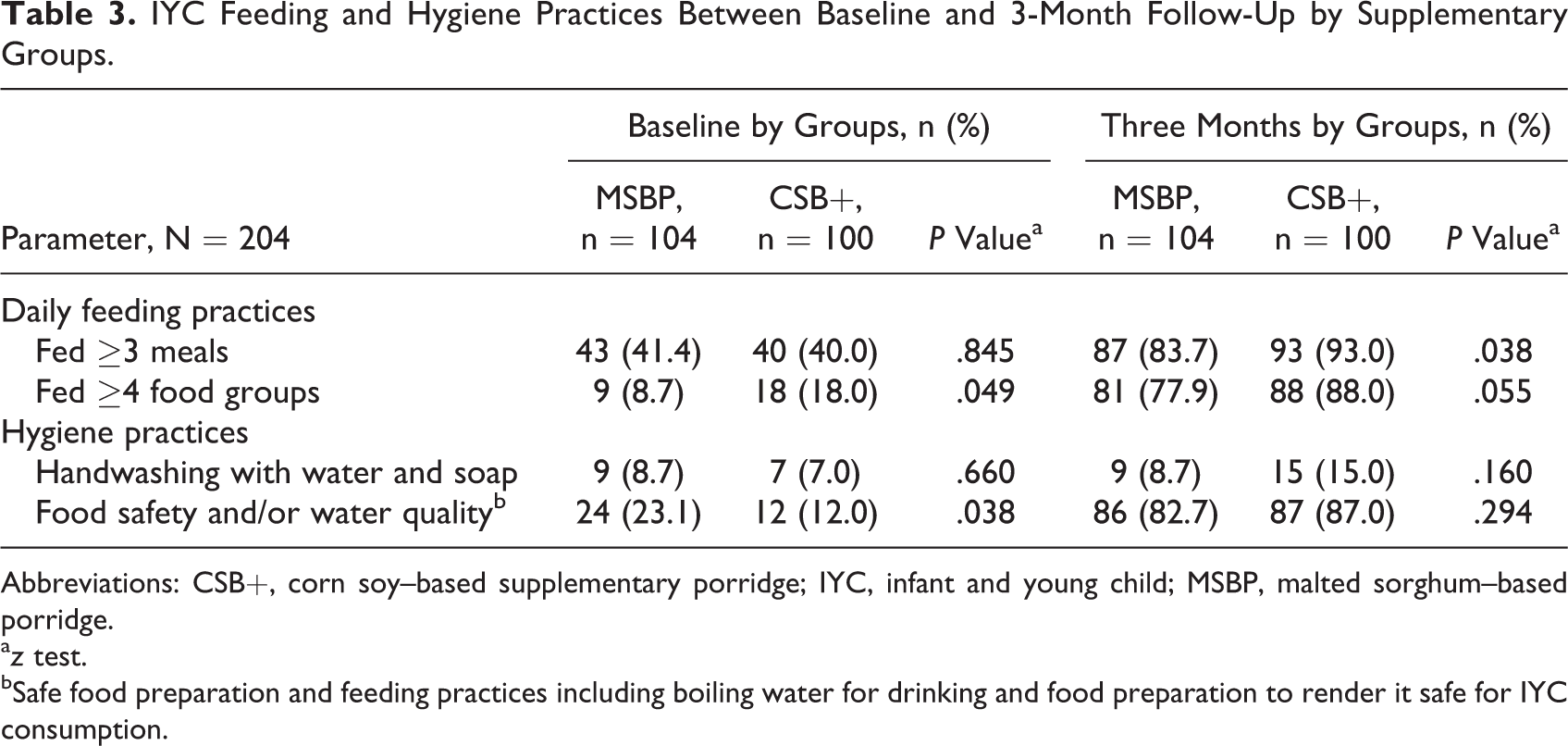
Abbreviations: CSB+, corn soy–based supplementary porridge; IYC, infant and young child; MSBP, malted sorghum–based porridge.
az test.
bSafe food preparation and feeding practices including boiling water for drinking and food preparation to render it safe for IYC consumption.
Discussion
This is the first known study that investigated feeding practices and measures of hygiene following nutrition education in the management of IYC with MAM in Uganda. Following nutrition education for a period of 3 months, an improvement in IYC complementary feeding and hygiene practices that differed significantly from baseline values was observed. However, handwashing, in both the MSBP and CSB+ supplementation groups, did not significantly improve after the 3-month intervention period.
Sociodemographic and Baseline Characteristics
The majority of participating mothers were younger than 35 years, similar to the findings of the 2016 Ugandan Demographic and Health Survey. 10 Mothers’ level of education was also comparable to national statistics. 10 As a lack of knowledge among mothers of IYC with MAM hinders appropriate complementary feeding practices, this finding provides evidence that the provision of nutrition education to mothers of IYC with MAM could improve their complementary feeding practices. 2 In addition, IYC who were being fed the minimum acceptable diet (MAD) at baseline was 5.9% compared to the national average of 14.0%. 10 This finding could be related to the fact that IYC with MAM seldom receive a diverse diet and are often fed less frequently than their healthy counterparts. However, results of the current study compare favorably with that of a study conducted in Ethiopia among IYC aged 6 to 23 months with a reported MAD of 10.8%. 19
Change in Mother’s Knowledge
The majority of mothers had a primary school education or no formal education, suggesting that they could have experienced difficulty in comprehending available nutrition education messages. Results from this study indicated that at the end of the intervention period, mothers’ knowledge regarding IYC feeding practices differed significantly from baseline. The latter is consistent with results documented in Kenya, where it was reported that nutrition education regarding appropriate IYC feeding practices contributed to an improvement in mothers’ knowledge. 20 It is possible that the significant change in mother’s knowledge at 3-month follow-up could have been ascribed to the targeted nutrition education messages provided in their mother tongue.
In addition, nutrition education improved mothers’ knowledge regarding meal frequency and the variety of food groups that are appropriate for IYC. This suggests that an improvement in mother’s knowledge about appropriate IYC feeding practices could contribute to improved food intake among their offspring, 5 with a concomitant improvement in IYC nutritional status. 21,22 However, despite targeted nutrition education messages, not all mothers showed an improvement in knowledge after the 3-month intervention period. It is possible that the implementation of newly acquired knowledge regarding appropriate IYC feeding practices could have been compromised by household socioeconomic factors, including mother’s level of education. 23
Change in Mothers’ Feeding Practices
Complementary feeding practices of mothers, especially in terms of dietary diversity and meal frequency, significantly improved at follow-up compared to baseline (P < .001). This illustrates that a nutrition education intervention with a duration of 3 months is able to improve complementary feeding practices of mothers with IYC diagnosed with MAM as part of the management process. 24 Findings of this study concur with those of a meta-analysis 2 that illustrated how nutrition education could be beneficial to IYC complementary feeding practices. Results of this study also compare favorably with those documented in Peru that indicated how a nutrition education intervention promoting appropriate complementary feeding practices in IYC could promote growth 22 and improve IYC feeding practices for the management of MAM. 2,20 This view is supported by an investigation of the factors associated with complementary feeding practices in Uganda that reported how mothers, when given nutrition education, are able to improve their IYC feeding practices. 25
The improvement in mothers’ knowledge and practices regarding dietary diversity as a result of nutrition education documented in this study has the ability to enhance the nutritional status of IYC with MAM. 26 Study findings also compare favorably with that of a study conducted in Ethiopia where it was reported that bimonthly nutrition education for a period of 6 months improves IYC dietary diversity practices, 5 as well as a study conducted in Peru where an improvement in IYC dietary diversity as a result of an 18-month nutrition education intervention was documented. 22
Change in Mothers’ Hygiene Practices
No significant difference was found between mothers’ hygiene practices in terms of handwashing with soap after contact with excreta, and before feeding IYC after the intervention period when compared to baseline (P = .183). The prevalence of handwashing at 3-month follow-up (11.8%) was lower than the mean of 14% for the African continent, despite being within the estimated prevalence of 9% to 24% for Uganda. 8
These results show that a targeted nutrition education intervention with a duration of 3 months was not adequate to bring about a significant change in handwashing practice among mothers of IYC with MAM. This finding suggests that nutrition education alone may not be sufficient to change personal hygiene habits in rural low-income settings. It is possible that mothers’ existing handwashing practices were too entrenched or that water was not freely available, a variable which was not determined in this study. 8 Alternatively, mothers could have been reluctant to change handwashing behavior, as it was not appealing or not a sustainable behavior as a result of living under conditions where handwashing was not a social norm, or they were not washing hands with soap for quite some time. 27
The results of this study compare favorably with that which was documented in Bangladesh, where a gap between knowledge and practice still prevails when it comes to handwashing practices. 27 Hence, continuous motivating activities are required to improve handwashing practice with soap. 27 Despite the health benefit of reducing the prevalence of diarrheal diseases, a systematic review on global handwashing practices 8 concludes that handwashing with soap after contact with excreta is poorly practiced. Due to a lack of awareness regarding its importance, 8 it is possible that a 3-month intervention is insufficient in bringing about significant change regarding handwashing habits among mothers of IYC diagnosed with MAM.
In contrast, the practice of safe food preparation techniques and feeding practices, including boiling water for drinking and food preparation, to render it safe for IYC consumption differed significantly between baseline and 3-month follow-up (P < .001). It is, therefore, possible that the nutrition education intervention could have improved the mother’s attitude 28 toward appropriate food preparation techniques and boiling water, which is vital in the management of IYC with MAM.
Limitations
There could have been some form of social desirability bias when it came to the evaluation of dietary diversity, as it is possible that mothers could have given information which they thought was appropriate, yet they did not implement this knowledge and/or beliefs. 18 However, this phenomenon was addressed by building rapport with mothers and probing them to remember food items such as snacks given to IYC between main meals, in addition to special meals and mixed dishes consumed within 24 hours prior the data collection. In addition, it should be noted that the positive effect of nutrition education on mothers of IYC with MAM was not compared to that of a control group of mothers with IYC with MAM for ethical reasons. However, the study documented a high proportion of mothers with improved knowledge regarding hygiene and feeding practices, despite the fact that this change cannot be attributed to the nutrition education intervention in isolation.
Conclusion
Infant and young child feeding practices in terms of dietary diversity, meal frequency, and hygiene practices through handwashing with soap, and making food and water safe for consumption significantly improved at 3-month follow-up (postintervention) compared to baseline. Thus, targeted nutrition education with a duration of 3 months has the ability to change knowledge and practices of mothers with IYC diagnosed with MAM when combined with a supplementary feeding program.
Recommendation
Health workers should continue the promotion of dietary diversity, increased meal frequency, food safety, and improved water quality among mothers to enhance the effectivity of supplementary foods given to IYC as part of the management of MAM. However, an approach other than the constructs of the Health Belief Model should be considered to significantly improve handwashing practices among mothers. This is important because a limitation of the Health Belief Model is related to a lack of perceived benefit by the mothers. 23,29
Footnotes
Authors’ Note
Richard Kajjura designed the study, performed data collection and management, conducted the statistical analysis, interpreted the results, and drafted the manuscript. Susanna Kassier and Frederick Veldman revised the study design, assisted with the interpretation of results, and revised the draft manuscript. All authors read and approved the final manuscript. This research received no specific grant from any funding agency in the public, commercial, or not-for-profit sectors other than the PhD Fellowship, from PowerFour International, Inc, USA.
Acknowledgments
The authors are grateful to the mothers who participated in the intervention, as well as the research assistants who collected the data. Dr Hedwig Acham of Makerere University and Dr Lindie Ncube of Sefako Makgatho Health Sciences University are acknowledged for the scientific assistance.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article:
