Abstract
Background:
Eggs are nutrient rich and have the potential to improve maternal nutrition during pregnancy and birth outcomes, but cultural beliefs may inhibit consumption during pregnancy.
Objective:
To understand knowledge, attitudes, beliefs, practices, facilitators, and barriers related to consuming eggs during pregnancy in Kenya.
Methods:
The study had 3 phases. Phase I included in-depth interviews and free-listing and pile-sorting exercises with pregnant women (n = 36), husbands (n = 12), and mothers-in-law (n = 12) of pregnant women, and health providers (n = 24). Phase II involved egg preparation exercises with pregnant women (n = 39). Phase III involved a weeklong trial of egg consumption with pregnant women (n = 24). We used thematic content analysis methods to analyze qualitative data and tabulated quantitative data.
Results:
All participants recognized eggs as nutritious for pregnant women; 25% of pregnant women consumed eggs the previous day. However, participants believed eating too many eggs during pregnancy (1 or more eggs daily) leads to a large baby and delivery complications. Unaffordability and unavailability also inhibit consumption. Health workers are the most trusted source of information on maternal nutrition. Almost all women complied with the household trial, said they would continue eating eggs and would recommend eggs to other pregnant women in moderation.
Conclusions:
Although participants believed consuming eggs during pregnancy is beneficial, cultural norms, practices, and beliefs may prevent pregnant women from eating them daily. Interpersonal communication from health workers and agricultural policies to promote affordability could lead to increased consumption.
Introduction
Globally, an estimated 15% to 20% of all births are low birth weight, representing 20 million births per year. 1 Low birth weight is a major predictor of perinatal mortality and morbidity, and the vast majority occur in low- and middle-income countries. Because of its importance for global health, the reduction in low birth weight is 1 of 6 nutrition targets endorsed by the World Health Assembly; the goal is to achieve a 30% reduction by 2025. 1 The challenge is that low-cost, sustainable, and scalable nutrition interventions to improve maternal nutrition during pregnancy and reduce low birth weight have yet to be identified.
Because they are nutrient rich and often locally available, eggs have great potential to improve nutrition among pregnant women living in low-resource settings. 2 Eggs are a nearly complete protein and contain essential fatty acids, micronutrients, and other bioactive compounds. Essential fatty acids, and docosahexaenoic acid in particular, are critical for visual acuity and early brain development. 3 Limited evidence suggests that consumption of essential fatty acids during pregnancy might have benefits for birth weight and length and gestational age. 4 Eggs have 1 of the highest concentrations of choline per kilocalorie, 5 and inadequate intake during pregnancy has been associated with neural tube defects, 6 changes in brain structure and function in offspring, 7 and adverse pregnancy outcomes. 8 Eggs are a good source of bioavailable vitamin A, other carotenoids and vitamins E, D, B2, B12, and folate. Eggs are also high in selenium, which plays important epigenetic and antioxidant roles that may be especially important during pregnancy. 9 Two 50-g eggs provide more than 15% of a pregnant woman’s daily needs of protein, iron, vitamin A, vitamin B2, vitamin B12, and phosphorus and more than half for selenium and choline. 10
Consumption of eggs during pregnancy could be an important food-based intervention to improve maternal nutrition during pregnancy and birth outcomes. 2 However, despite its promise, egg consumption during the preceding 24 hours is <20% among reproductive-age women who have given birth in the past 3 years in low- and middle-income countries where data are available. 2 Data on egg consumption among reproductive-age women are not available for Kenya, but consumption is low among children; in 2014, only 18% of children aged 6 to 23 months consumed an egg the previous day, 11 and egg consumption in mother–child dyads is correlated. 12 Because knowledge and beliefs influence behaviors, 13 cultural beliefs about the acceptability of pregnant women consuming eggs are often thought of as a barrier to consumption in some settings, although most reports are anecdotal. Our study attempted to address this gap in the literature through a qualitative study that used multiple methods for triangulation of data to assess knowledge, attitudes, beliefs, practices, facilitators, and barriers related to consuming eggs during pregnancy in Kenya.
Methods
Study Setting
We conducted the study in Kenya for a number of reasons, including poor nutritional status among reproductive-age women, a high prevalence of low birth weight in some regions of the country, 11 and the presence of a national researcher highly experienced in conducting formative research. Within Kenya, we conducted the study in an urban and rural site, selected in consultation with the Ministry of Health. In Nairobi, Kangemi was selected to represent low-income multiethnic slum areas in an urban setting, while Ndeiya in Kiambu County just north of Nairobi represented a low-income rural setting. We conducted interviews in participants’ homes, health facilities, or another private location.
Study participants and sampling strategy
The study population included pregnant women aged 18 to 39 years and key influencers of their behavior, 14 -18 including husbands, mothers-in-law, community health workers, and health-care providers. Pregnant women who were allergic to egg protein on self-report were excluded from the study.
The sampling strategy was purposive, and pregnant women were recruited through local health clinics. Husbands and mothers-in-law were recruited through pregnant women participants. If husbands or mothers-in-law of pregnant women participants declined to participate, we recruited additional husbands and mothers-in-law of pregnant women in the community. The study was conducted in 3 phases (described below). During the informed consent process, pregnant women were encouraged to participate in all 3 phases. If a pregnant woman was unable to participate in all study phases, we recruited another pregnant woman as a substitute. After describing the study, we obtained written or thumbprinted informed consent from each eligible participant.
We selected sample sizes for each phase of the study according to the research techniques described below. For in-depth interviews (phase I), we used a sample size of 6 participants per subgroup of interest to achieve saturation, the point at which additional interviews provide no new information in qualitative research. 19 We interviewed 18 pregnant women at each site within the age-groups 18 to 24, 25 to 29, and 30 to 39 years. We interviewed 6 mothers-in-law of pregnant women, 6 husbands of pregnant women, 6 community health workers, and 6 health-care providers (ie, nurses, midwives, and clinical officers) in each site. For phase II (egg preparation exercises), we included 19 pregnant women in the rural site and 20 pregnant women in the urban site. For phase III (household trials), we included 12 pregnant women per site.
Study design and research tools
We used quantitative and multiple qualitative and applied ethnographic methods to triangulate the data. Phase I consisted of in-depth interviews, a 24-hour dietary recall, and free-listing and pile-sorting exercises. Phase II involved egg preparation exercises, and phase III involved household trials of egg consumption.
Phase I
The interview guide was grounded in a focused ethnographic approach and the cultural–ecological model of food and nutrition. 20 We also drew from modules of a focused ethnographic study with pregnant women in Ghana. 21 While traditional ethnography involves the study of culture and society through immersion and long-term, field-based research, focused ethnography aims to study culture more expeditiously to answer specific questions to inform decision-making about potential future public health or nutrition interventions. 22 Specifically, the goal is to identify an intervention that may be appropriate for, feasible, and successful in the local context; identify bottlenecks that may inhibit successful intervention implementation; and/or inform the design and content of a behavior change communication strategy. 22
The interview guide for all study participants included basic sociodemographic information adapted from the 2014 Kenya Demographic and Health Survey. 11 The guide for pregnant women used the open recall method described in Minimum Dietary Diversity for Women: A Guide to Measurement to assess dietary diversity, including egg consumption. 23 All interview guides included questions about foods perceived to be good or bad to eat during pregnancy (including eggs specifically), sources of nutrition information during pregnancy, facilitators and barriers to eating well during pregnancy, roles others can play in supporting pregnant women to eat well during pregnancy, ways eggs are typically prepared (pregnant women and mothers-in-law only), and food sources and expenditure. The guide for health workers included similar questions and questions about their activities related to working with pregnant women.
During the in-depth interviews (phase I), we conducted free-listing and pile-sorting exercises. 20,24,25 Each participant listed the foods that are good or not good to eat during pregnancy. The research assistant selected pictures of foods, dishes, and beverages the participant named in the free-listing exercise, and the participant was invited to put the pictures that “go together” in the same pile. Participants could create as many piles and iterations of piles as they wished and were asked to explain why they put the cards together. Health workers completed the free-listing but not the pile-sorting exercise.
For the egg preparation exercise (phase II), we used methods described in the Process for the Promotion of Child Feeding (ProPAN) field manual. 26 Foods available in households and in the community that are affordable and culturally appropriate per data collected in phase I were made available. Food was prepared at central venues identified jointly by the research team and community leaders in each site. In groups of 6 to 7, pregnant women prepared egg recipes. We collected data on the ingredients and amounts used, steps followed to prepare the dishes, preparation and cooking methods, and length of time for preparation and cooking. After the groups finished, participants tasted the foods prepared, and research assistants led discussions about reactions to the dishes (ie, their taste, smell, and appearance), feasibility of preparing them at home, and any suggestions for their modification or improvement.
The household trial of egg consumption (phase III) was also conducted in line with the ProPAN field manual. 26 Research assistants visited the pregnant women’s homes and discussed the goal of consuming 1 egg per day, recommended several egg recipes found to be the most appropriate and acceptable during phase II, and encouraged them to meet the goal of eating 1 egg per day for the next week. Each woman was provided with 7 eggs and instructions they were to be consumed only by her during the trial period. One week later, the research assistant returned to explore how many days she ate an egg, how she prepared the eggs, if the eggs were shared with any household members, and barriers and facilitators to daily consumption.
Data collection and analysis
Data were collected between May and July 2018. All interview guides and data collection tools were developed in English, translated into Kiswahili, and piloted in localities with characteristics similar to the study sites. Interviews and egg preparation exercises were conducted in the participant’s preferred language: English, Kiswahili, or local language. The study coordinator conducted observations of the research assistants and reviewed data collection forms to ensure quality and fidelity. With 1 exception, interviews were tape-recorded, transcribed, and translated into English. Quantitative data were entered into databases developed for the study. All recordings and data collection forms were kept in a secure location at the University of Nairobi; data were transferred to RTI International through a secure server for analysis.
We used thematic content analysis methods to analyze phase I and III interview transcripts 27 and developed deductive codes based on the interview guides and inductive codes, as needed, through the coding process. We used NVivo version 11 (QSR International, Victoria, Australia) to code transcripts, double coded 10% of the data to ensure intercoder reliability, and discussed and recoded any discrepancies identified through the double-coding process. We then developed data matrices for each participant group, with 1 row for each participant and columns for each relevant code and demographic variable (ie, age, urban/rural location). 28 The cells contained a summary of the findings from that interview for each code along with illustrative quotations. We used the matrices to sort the data and make comparisons among groups and participant characteristics.
We analyzed quantitative data using Stata version 13.0 (StataCorp LP, College Station, Texas). Demographic and socioeconomic data were tabulated, and the minimum dietary diversity for women (MDD-W) scores were calculated. 23 The frequencies for all foods free-listed as good and not good for pregnant women were tabulated, and the average order in which they were listed by each participant group calculated. We reviewed reasons given for free-listing by each participant group. The most frequently listed foods by each participant group were analyzed. For the pile-sorting exercise, we calculated the average number of piles created by each participant group. The reasons given for all piles were reviewed, and each pile was assigned appropriate category(ies) based on emergent themes. We calculated the percentage of each participant group’s piles in each category based on the total number of piles each group created. Piles and reasons for piles were then analyzed for specific references to eggs and their associations with other foods. Quantitative data from egg preparation exercises were tabulated and the group-level feedback reviewed. In all analyses, we looked for similarities and differences between participant groups and urban/rural sites.
Because our study intended to explore specifically how knowledge, attitudes, and cultural beliefs might affect pregnant women consuming eggs in Kenya through the perspectives of pregnant women, husbands, mothers-in-law, and health workers, we focused our analysis on the diet, culture (idea system), and social organization components of the cultural–ecological model of food and nutrition, although we explored other components as themes emerged.
We conducted the study according to the guidelines in the Declaration of Helsinki, and it was approved by the Ethical Review Committee of the University of Nairobi and Kenyatta National Hospital (P148/03/2018) and institutional review board at RTI International (STUDY00020093).
Results
We present demographic results first, followed by the themes that emerged in all study phases. We combined results when responses were the same across all groups of participants, geographies, and age-groups. Differences among them are noted. Figure 1 shows how each theme that emerged maps to the different components of the cultural–ecological model. Given the interrelated nature of the model and the specific results from our study, some themes pertain to multiple components of the model.
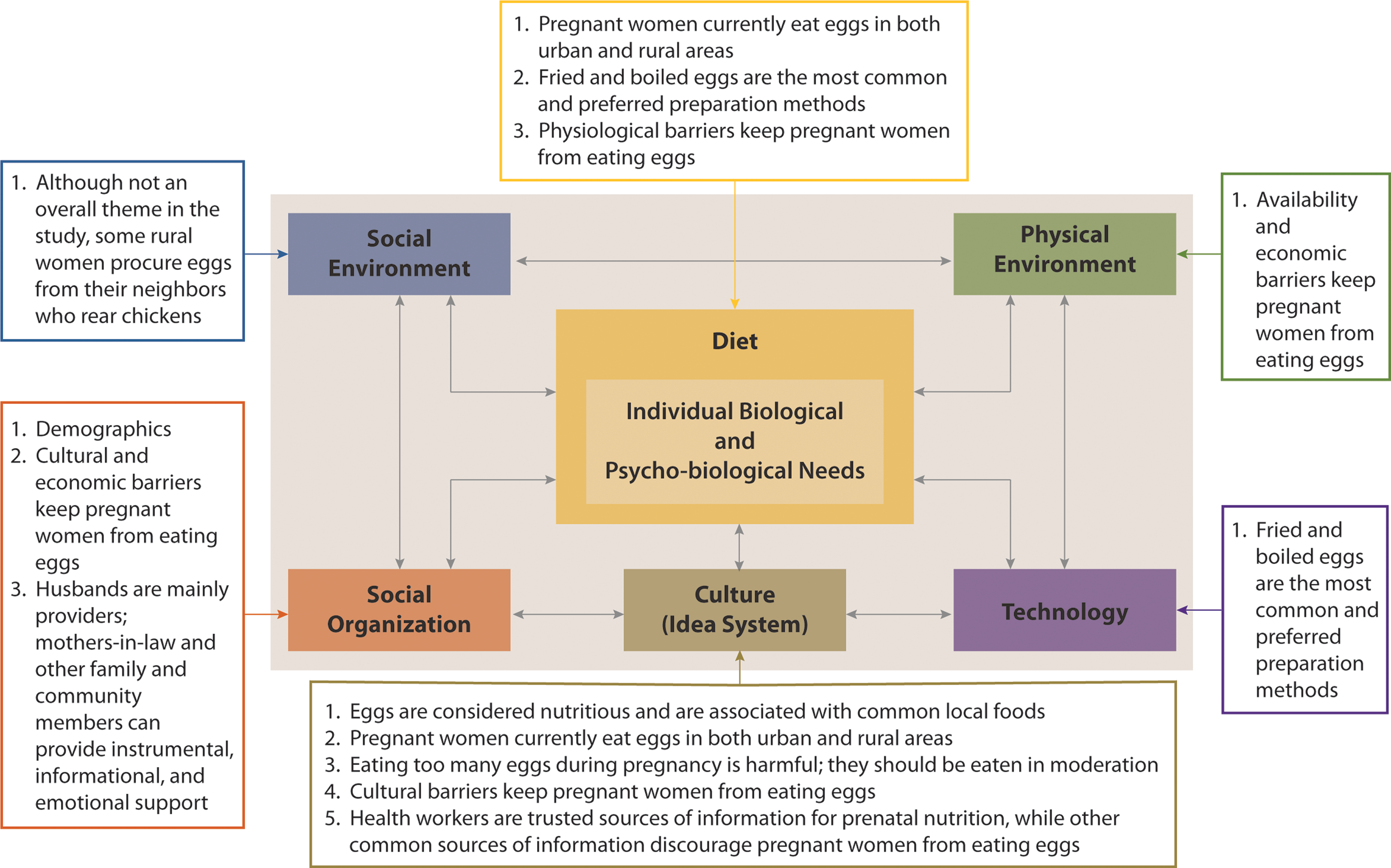
Results in relation to the cultural–ecological model of food and nutrition. Model from Pelto and Armar-Klemesu. 20
Demographics
A total of 46 pregnant women participated in the study. Thirty-six participated in the in-depth interviews and free-listing and pile-sorting exercises. Seven could not continue participation because of other commitments. Ten additional pregnant women were recruited to participate in phase II. Of all pregnant participants, 24 participated in the household trial. Of the 12 husbands and 12 mothers-in-law, 4 husbands and 8 mothers-in-law were not related to a pregnant participant.
On average, pregnant women were younger than husbands, and husbands in rural areas were considerably older than husbands in urban areas (42.8 years vs 27.9 years; Table 1). Mothers-in-law in rural areas had more children than in urban areas (6.3 vs 3.8). Almost all pregnant women were married and had, on average, 1.6 children. Occupations varied widely across participant groups and sites. More urban pregnant women were housewives (84% vs 24%), while more rural pregnant women were agricultural workers or petty traders (43% vs 0%). All urban husbands were either salaried workers or casual laborers, while most (80%) rural husbands were casual laborers. Urban mothers-in-law were split between agricultural workers or petty traders and salaried workers, while all rural mothers-in-law were agricultural workers or petty traders. Most participants were either Kikuyu or Luhya, with Kikuyu more prominent in rural areas (except for mothers-in-law) and Luhya more prominent in urban areas. Of the pregnant women who reported receiving antenatal care, almost all received services from a nurse at a government health center. Mothers-in-law owned the most chickens, and chicken ownership was generally more common in rural areas.
Characteristics of Pregnant Women, Husbands, and Mothers-in-Law.
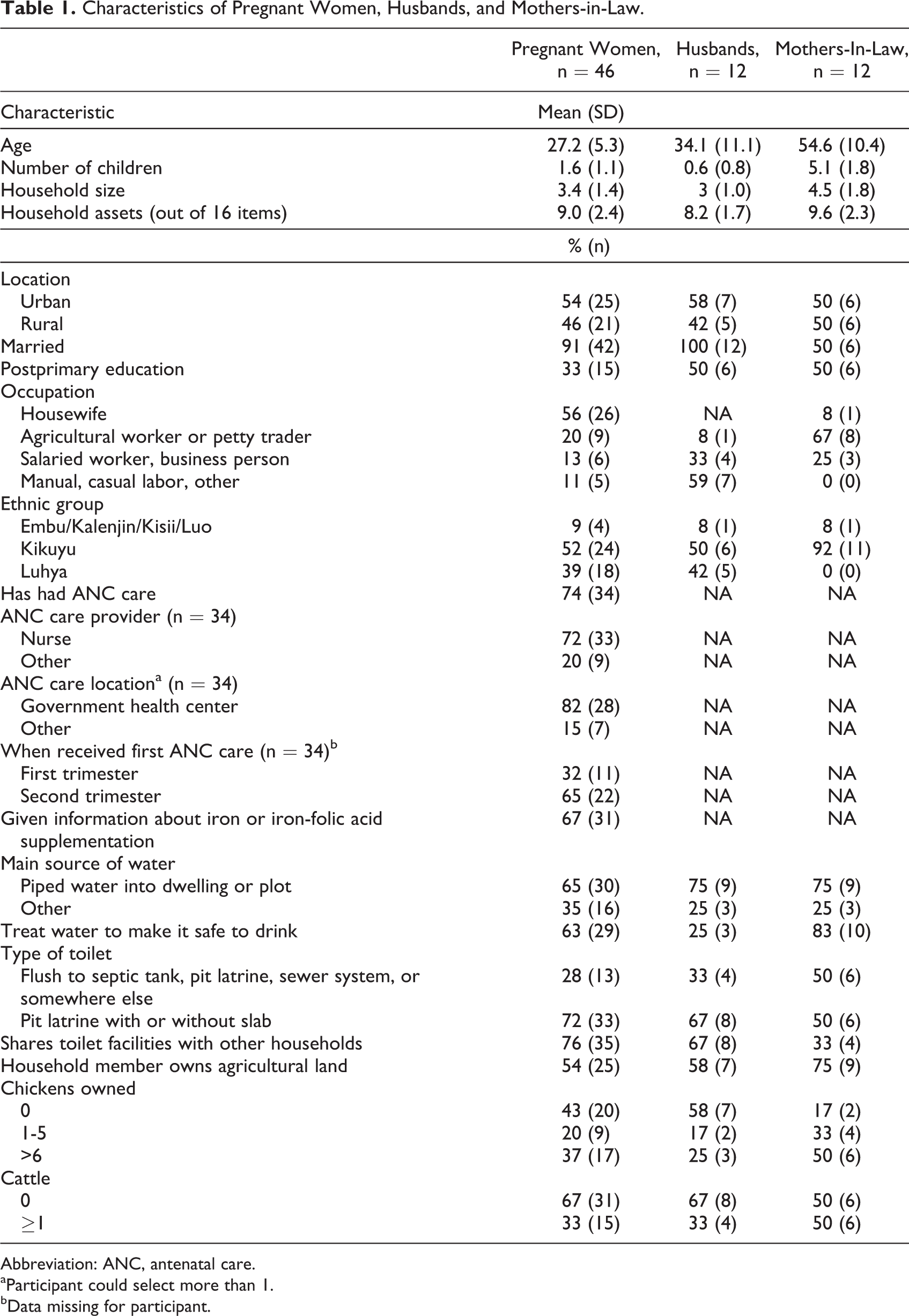
Abbreviation: ANC, antenatal care.
aParticipant could select more than 1.
bData missing for participant.
Health workers were, on average, older than pregnant women and husbands; rural health workers were older than urban health workers (41.7 years vs 36.2 years; Table 2). Almost all health workers had a postprimary education and worked in or through a government health center. Just over half were Kikuyu, driven in large part by the rural health workers.
Characteristics of Health Workers.a
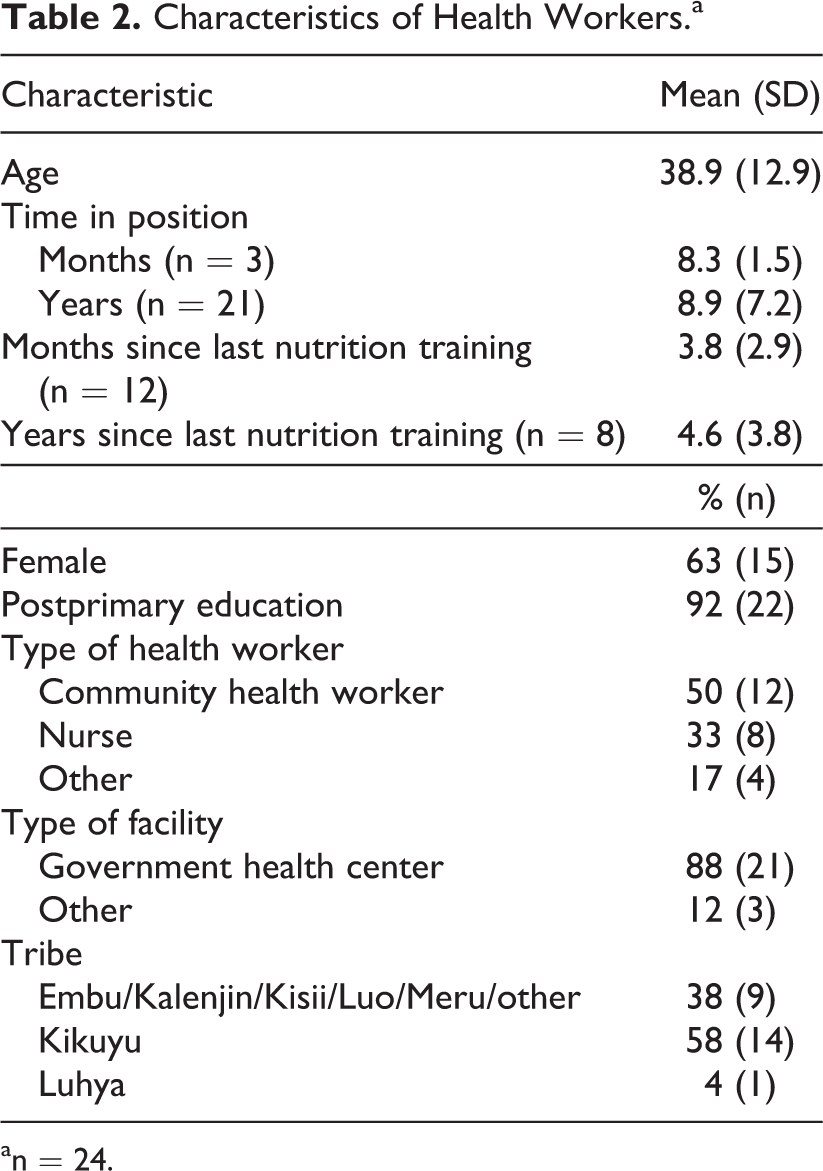
an = 24.
Eggs are considered nutritious and are associated with common local foods
Pregnant women and husbands both created an average of 6.4 piles, while mothers-in-law created an average of 6.8 piles. Reasons given for putting foods and drinks together included their perceptions of nutritional value or lack thereof and positive or negative health effects and items that can be prepared and/or eaten together, are or are not recommended for a pregnant woman to consume, are part of the same food group or category (ie, drinks), and whether the participants like or are currently consuming them. Pregnant women most commonly sorted items according to whether foods could be prepared and/or eaten together (43% of piles), while husbands most commonly sorted piles according to their nutritional value (53% of piles), and mothers-in-law most commonly sorted piles according to items’ perceived positive or negative effects on health (41% of piles).
Ugali (boiled stiff maize porridge, a staple food in Kenya) was most commonly cited across all participant groups as a food eggs could be eaten with. Pregnant women and husbands also included indigenous vegetables, fruits, and sweet potatoes as foods with which eggs can be eaten. Regarding their nutritional value, eggs were included in piles of foods said to be sources of protein, vitamins, minerals, and other nutrients or were generally healthy foods, along with milk, fish, indigenous and other vegetables, and fruits. With respect to health effects, pregnant women and mothers-in-law placed eggs in piles with many of the aforementioned foods because they could “boost blood,” prevent diseases, give energy, contribute to weight gain of a pregnant woman and fetus, and “build the body.” I think [eggs] help the woman and the baby. It especially makes the baby grow and also get good health…It has proteins, they give proteins and energy to both the mother and the child.—Rural Pregnant Woman Eggs have vitamins and protein. They aid in body development for the child and also formation of blood cells and folic acid (and iron) that aid in growth and development of the child.—Urban Husband When you take an egg in the morning, you have taken so many nutrients from it. It has protein…it has so many nutrients in itself, so you get the nutrients that you are supposed to get when you are pregnant. It will also help the baby.—Rural Facility-Based Health Worker
Most Frequently Free-Listed Foods as Good for Pregnant Women.
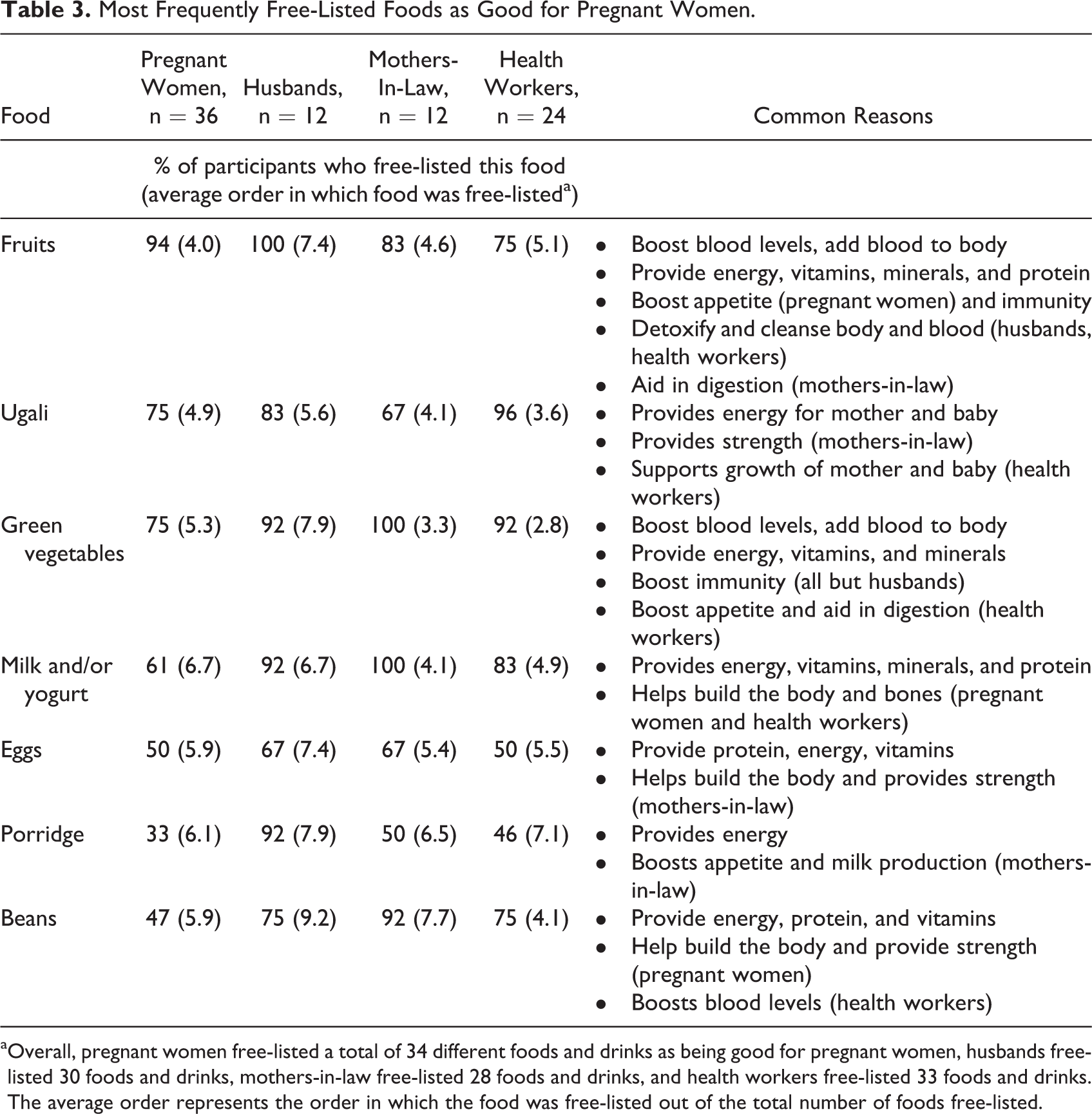
aOverall, pregnant women free-listed a total of 34 different foods and drinks as being good for pregnant women, husbands free-listed 30 foods and drinks, mothers-in-law free-listed 28 foods and drinks, and health workers free-listed 33 foods and drinks. The average order represents the order in which the food was free-listed out of the total number of foods free-listed.
Pregnant women currently eat eggs in both urban and rural areas
The majority of pregnant women, husbands, and mothers-in-law reported some level of current egg consumption among pregnant women; most responses characterized consumption as being eating 2 to 3 eggs 1 to 2 times per week, followed by eating eggs every other day. More women in the younger age-groups than older age-groups said they consume eggs multiple times per week. Only 25% of pregnant women reported consuming an egg in the previous 24 hours
Pregnant Women’s Dietary Diversity (DD) from Phase I.
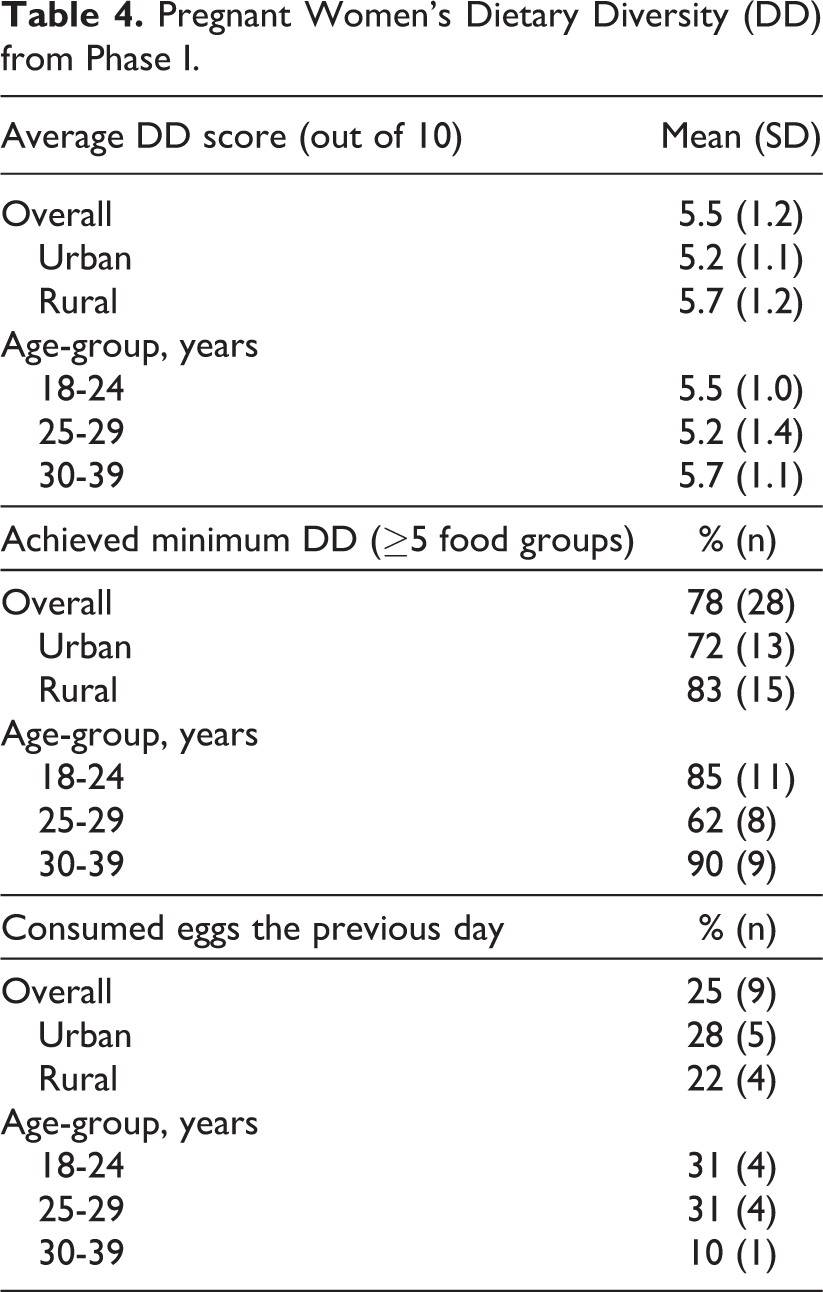
The average overall MDD-W score was 5.5, and the majority (78%) of pregnant women met the criteria for minimum dietary diversity; results for both variables were slightly higher for rural and older pregnant women. All pregnant women consumed a grain, root, or tuber the previous day. “Other vegetables” was the next most commonly consumed food group (97.2% of pregnant women), followed by dairy (88.9%); dark green leafy vegetables (63.9%); other fruits (52.8%); pulses (52.8%); other vitamin A-rich fruits and vegetables (36.1%); and meat, poultry, and fish (30.6%). None of the pregnant women consumed nuts or seeds in the previous 24 hours.
Of the women who shared how their egg consumption had changed throughout their pregnancy, approximately half said they ate eggs earlier but had discontinued or decreased intake (more so rural and women in the 18-24 and 25-29 years groups) because of loss of appetite, preference for other foods, inability to afford eggs, or negative side effects. The other half said they did not eat eggs before or early in their pregnancy because of feeling sick but had since started eating eggs (more so urban women).
Eating too many eggs during pregnancy is harmful; they should be eaten in moderation
Almost all of participants’ negative perceptions of eggs were in the context of pregnant women eating too many as opposed to eating them at all. By far, the most common of these negative associations was that eating too many eggs during pregnancy leads to a large baby, complications during delivery, and the potential need for an “abnormal delivery” (eg, cesarean section). Participants who free-listed eggs as a food that is not good for pregnant women also cited this belief (Table 5).
Most Frequently Free-Listed Foods as Not Good for Pregnant Women and Eggs.
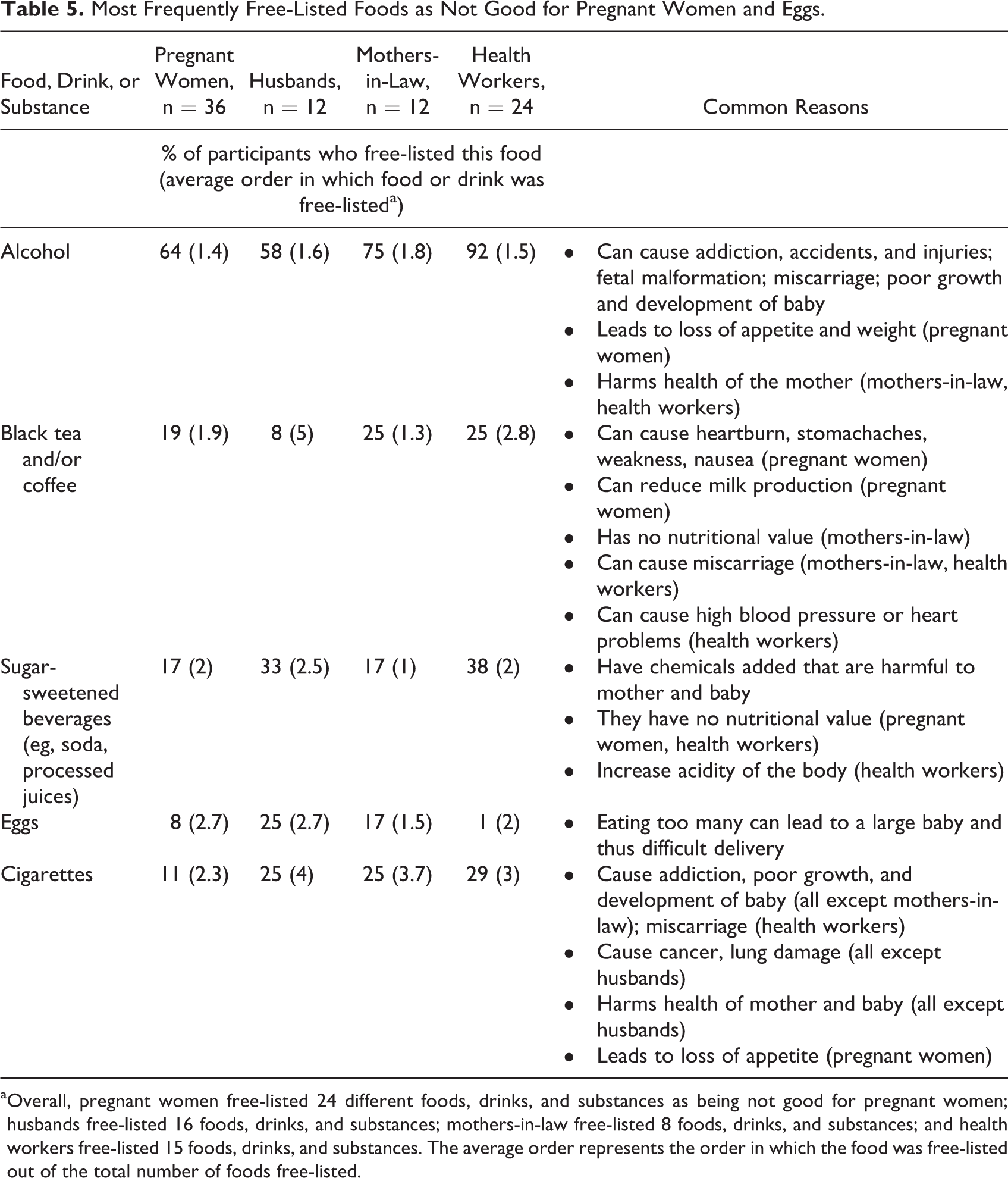
aOverall, pregnant women free-listed 24 different foods, drinks, and substances as being not good for pregnant women; husbands free-listed 16 foods, drinks, and substances; mothers-in-law free-listed 8 foods, drinks, and substances; and health workers free-listed 15 foods, drinks, and substances. The average order represents the order in which the food was free-listed out of the total number of foods free-listed.
All participant groups also associated eating too many eggs during pregnancy with heart and breathing problems for both the woman and the fetus, including “heart disease,” high blood pressure, an enlarged heart, and “panting.” Other common negative associations of eating too many eggs during pregnancy included the development of allergies, the child being “dumb” or having delayed speech (urban areas only), and pregnant women gaining too much weight (more so in urban areas). They usually say you should not eat a lot [of eggs] because the child will be big and bring problems during delivery. They also say it causes blood pressure.—Urban Husband [Eggs] make the heart grow big, and eggs are very strong. It can be too much, that is what I know.—Rural Pregnant Woman I may stop [eating eggs] for a while because of the way I have eaten them now…I can stop for about 2 weeks, then I will go back to my usual frequency, 2 or 3 eggs in a week”—Urban Pregnant Woman If they won’t react with me or have any other side effects, I can continue eating [eggs] but I won’t eat everyday…because I hear that they are very strong, so they can give me problems. But I would like to continue eating, maybe 4 in a week, but that is if I can get the eggs or they are readily available.—Rural Pregnant Woman
Fried and boiled eggs are the most common and preferred preparation methods
During interviews, pregnant women most commonly reported frying eggs (beaten or unbeaten, known as “mayai macho,” “egg with an eye,” and “drop egg”) with cooking oil and salt. Boiling eggs was the second most popular preparation method, followed by an omelet with onions and/or tomatoes and oil and salt. Boiling (more so urban) and frying (more so rural) were also the most common preparation methods reported by household trial participants. Many pregnant women reported preparing eggs in more than 1 way.
Pregnant women prepared 9 unique recipes during phase II. Fried eggs scored highest in taste among both urban and rural participants, fried and boiled eggs scored among the highest for smell and equally as well as other recipes on appearance, and fried eggs scored among the highest for overall acceptability. Fried and boiled eggs were the easiest to prepare because of their short preparation time and/or limited number of ingredients, but participants still enjoyed trying new and different preparations.
Cultural, physiological, economic, and availability barriers keep pregnant women from eating eggs
The main barriers to egg consumption during pregnancy are beliefs about eating too many eggs during pregnancy and perceptions that eggs cause nausea and/or vomiting. To a lesser degree, all participant groups also cited women not liking eggs, eggs being too expensive (more so among rural pregnant women and health workers), and unavailability in markets or a lack of household chickens (more so in rural areas). Although most participants indicated that the recipes from the egg preparation exercises would be easy to make at home regularly, the availability and/or affordability of ingredients could determine whether some of the recipes are feasible. Furthermore, many of the household trial participants who wanted to eat eggs daily said they could if eggs are affordable and available (more so rural). Those [who wouldn’t follow advice to eat eggs during pregnancy] are probably afraid, that it may affect them. Or that the baby may grow too big inside.—Urban Pregnant Woman First, she may like not like [eggs]. Second, maybe she is not able to buy the eggs. Maybe she does not have money to buy eggs each and every day.—Rural Husband I am planning to eat eggs daily if they are available.—Rural Pregnant Woman
Barriers to egg consumption during pregnancy were similar to barriers to eating good foods in general, the most common being lack of money. Many pregnant women and health workers also said lack of family support—financial or emotional—and household conflict or stress were barriers to pregnant women eating well. A few rural husbands, mothers-in-law, and urban and rural health workers cited pregnant women’s “ignorance” as a barrier, described as lacking knowledge or deciding not to follow the nutrition advice health workers offer.
All participant groups described having money, family, and community support (all except mothers-in-law) and a family farm (more so in rural areas); the availability and affordability of food (more so in urban areas); and nutrition education as facilitators to pregnant women eating well. The availability of eggs from the study was the main facilitator to eating eggs reported by the household trial participants (more so rural), followed by the ease of boiling and frying preparation methods (also more so rural). Several participants also noted that the absence of negative side effects encouraged them to eat an egg every day and to know eggs are okay to eat. I was happy for the eggs…As for me, the eggs did not have any bad effect on me, so I ate all of them.—Urban Pregnant Woman
Husbands are mainly providers; mothers-in-law and other family and community members can provide instrumental, informational, and emotional support
All participant groups named providing money and foods for the pregnant woman as husbands’ main role. A few participants across groups also said husbands could encourage their wives, ensure they eat well by checking on them, advise on what they should eat, and help them with chores so that they can save energy for cooking and eating (husbands and health workers only). All participant groups also described these same roles for mothers-in-law and other family and community members (eg, a pregnant woman’s parents, siblings, cousins, and neighbors), although rural participants more commonly cited providing nutrition advice. Mostly urban health workers also said family and other community members could come with the pregnant woman to antenatal clinic visits or help her get medical attention if needed. I am the source. She does the cooking. My work is to provide the food.—Rural Husband It is [family’s and community members’] role to support me physically and mentally. If they are available, they go buy me the food I am supposed to eat.—Urban Pregnant Woman Like when I am buying food for my household, I also buy her share so that we eat together with her. I buy everything, so we can cook together. I also explain to her when she is going to cook for herself, to ensure she mixes several things, so I just advise her.—Rural Mother-in-Law
Health workers are trusted sources of information for prenatal nutrition, while other common sources of information have discouraged pregnant women from eating eggs
Health workers described providing nutrition education as 1 of their main roles, mostly as group nutrition education during antenatal clinic visits or through home visits and community-based gatherings, such as churches or peer-support groups. Indeed, they were cited by pregnant women, husbands, and mothers-in-law as a main source of information about foods that pregnant women should and should not eat although more so by pregnant women and mothers-in-law. Furthermore, almost everyone described multiple sources of information. Pregnant women and mothers-in-law listed their own mothers and mothers-in-law, grandmothers, other pregnant women and mothers, friends, neighbors, and their own experiences during pregnancy, as other common sources of information about foods that are beneficial for pregnant women. Husbands also listed their mothers (urban), elderly and other relatives, friends, and neighbors (rural) as sources of information; however, school and media (eg, television, radio, and social media) were their most frequently listed sources of information. I do hear [about nutrition] from radios, TVs, and from churches, too, where we usually have health lessons.—Rural Husband [I trust] my two mothers because you know, they have brought up children for a long time…they have also been expectant. They were also told about how they should eat, how they should not eat…because after they were told what to do or not do, they later found out themselves whether it was right or wrong. You see, now that’s why they are also telling me the same.—Rural Pregnant Woman [I trust information from] the doctor. It is because he is a professional. [I trust] the other professionals like nurses, clinical officer, all of them. Even the nutritionist.—Rural Husband I usually feel that the hospital is more trustworthy. You know, the doctor has his knowledge.—Urban Mother-in-Law Just a friend. Some will tell you that they went through Cesarean section because of eating many eggs during pregnancy…even those who have given birth, they can tell you not to take a lot of eggs.—Urban Pregnant Woman Mostly women or friends. They will tell you that eggs are not good. [They say] that they make the child to grow big and you will be unable to give birth.—Rural Pregnant Woman The older women usually discourage us not to eat them…even we pregnant mothers do discourage each other.—Rural Pregnant Woman
Discussion
Because of their unique nutrient profile, eggs have the potential to improve maternal nutrition during pregnancy and birth outcomes, but cultural beliefs are often thought of as a barrier to egg consumption. Our study showed that almost half of pregnant women, three-fourths of husbands, two-thirds of mothers-in-law, and half of health workers spontaneously listed eggs as good for pregnant women. Only 8% of pregnant women, 25% of husbands, 17% of mothers-in-law, and 4% of health workers spontaneously listed eggs as not good for pregnant women. Similarly, in rural Zambia, 82% of women agreed eggs were good for pregnant women and only 8% voiced concerns. 29
The main concern about eggs during pregnancy in our study was that eating too many could lead to a large baby, delivery complications, and potentially a Cesarean section. Although some participants also raised this concern about other protein- and fat-rich foods, our study did not systematically explore cultural beliefs related to eating other foods during pregnancy beyond eggs; thus, we do not know whether this concern is unique to eggs or protein- and fat-rich foods or if it applies to eating too much of any food. “Eating down,” the practice of a woman eating less during pregnancy than prepregnancy, has been reported in Asian countries, such as Bangladesh, 30,31 India, 32 -34 Pakistan, 35 and Nepal. 36 In Bangladesh and Nepal, nausea, loss of appetite, and not feeling well were the most common reasons for food aversions and eating less during pregnancy. A smaller percentage of participants in these studies cited cultural or religious beliefs as reasons for avoiding certain foods, including concerns about eggs leading to a large baby and difficult delivery, which was also true for dhal and fish in rural Bangladesh. 31 A recent study from Niger found that although taxonomies of foods for pregnant women exist, including eggs highlighted as a body-building food, limited food availability, accessibility, and affordability alongside nausea and vomiting were the main barriers to women consuming the culturally ideal foods. 37 These results suggest that “eating down” is a multifaceted issue and that both physiological conditions and cultural beliefs must be considered when providing nutrition education for pregnant women and communities. Increasing weekly consumption of eggs could also mean that other food(s) could be partially displaced from a pregnant woman’s diet. Other than nuts and seeds, which no pregnant participants consumed the day prior to the phase I interview, eggs were the least consumed food group. This suggests that any of the other 8 food groups could be candidates for displacement by eggs. Participants associated eggs with fish and milk (among other foods) as sources of protein, vitamins, and minerals, so it is possible that eggs could replace these foods, thereby altering the nutrient density of the diet for some nutrients such as iron and choline. Alternatively, eggs could also replace a less nutritious food, thus improving the overall nutrient density of the diet.
In Kenya, 58% of pregnant women attended 4 or more antenatal care visits during their pregnancy, making health workers a frequent source of contact for women during pregnancy. 11 Our study found health workers to be the most trusted source for information about nutrition during pregnancy, and the percentage of pregnant women who free-listed eggs as a good food to eat during pregnancy was the same as the percentage of health workers who said this. Even participants who expressed concerns about the amount and frequency of egg consumption during pregnancy indicated they would accept the advice to eat eggs during pregnancy if a health professional recommended it. In Nigeria, nutrition education and counseling during antenatal care visits played a positive role in improved breastfeeding practices. 38 -40 These findings could translate to improved eating practices during pregnancy as well.
Traditionally, programs pertaining to infant and young child feeding (IYCF) have focused on the mother as the sole actor; however, research in recent years has explored the role of others, such as grandmothers and fathers. 14 -17 Although not as well documented as for IYCF, family members also influence women’s diet during pregnancy. A recent review found family members, especially mothers and mothers-in-law, and friends were a source of information about recommended foods during pregnancy. 41 However, some research has also found father and grandmother involvement to have a negative impact on IYCF. 18 Social norms, knowledge, attitudes, and beliefs can influence the type of support offered by influencers, 42 and the types of support offered by influencers can influence whether any behavior changes have positive or negative effects. 43 In our study, most key influencers acknowledged the existence of some sort of cultural belief surrounding eating too many eggs, which could lead them to discourage or prevent pregnant women from eating eggs. Indeed, some influencers not involved in the study (ie, friends and other pregnant women in the community) were reported to discourage pregnant women from eating eggs. Conversely, having key influencers acknowledge that eggs are nutritious could lead to encouraging pregnant women to eat eggs. While the literature and anecdotal evidence support the prominence of mothers-in-law in influencing a woman’s pregnancy decisions, our study did not decipher specific roles for mothers-in-law beyond what was reported for “other family and community members.” This may indicate that in the study sites, mothers-in-law play a generally supportive role rather than a gatekeeping role for the information a pregnant woman receives and/or her eating behaviors.
Low levels of egg consumption among young children and reproductive-age women may be a function of economic barriers in addition to cultural ones. 44 Animal source foods, such as fresh milk and eggs, are very expensive sources of calories in low-income countries. 45 Young child consumption patterns are strongly associated with the caloric price of these foods; this is also likely to be true for pregnant women. Although other demand-side factors are likely to be important, the price of eggs suggests an important role for agricultural policies, including in production, marketing and trade, to improve the affordability and availability of eggs in low-income countries. 46,47 Even increases in availability from community-based, small-scale egg production centers can increase consumption. 29 Our study showed that economic and availability considerations are important for consuming eggs. Moreover, these economic considerations differed somewhat between urban and rural participants in our study: rural participants described unavailability of eggs either in the markets or from not having their own chickens and unaffordability as barriers to consuming eggs more than urban participants. Egg affordability and availability may vary seasonally, which could be also addressed through agricultural policies and practices. Decreasing the cost and increasing the availability of eggs by increasing supply would facilitate increased egg consumption among pregnant women, not only because eggs would be more affordable for them as individuals but also for their entire household given that our results show all members of the household typically eat eggs when they are available. However, while decreasing the cost and increasing the availability of eggs through increasing supply is necessary, it may not be sufficient if cultural barriers to their consumption among young children and pregnant women exist.
Social and cultural barriers may be overcome with well-informed and carefully conducted social marketing and behavior change communication (BCC) strategies. 3,48 -51 Many of our results suggest that reservations about the number of eggs pregnant women should consume could be overcome through well-crafted BCC messages, distributed through appropriate people and channels, delivered to both pregnant women and influencers of their behavior, and guided by the Theory of Planned Behavior 52 or Health Belief Model. 53 The BCC messages could emphasize facilitators that already exist (eg, pregnant women currently eat eggs, and many believe eggs are beneficial), include problem-solving or encouraging language to more fully develop potential facilitators from our results (eg, encourage other women in the community to support pregnant women eating eggs), and address barriers in an appropriate way (eg, believing eating too many eggs is problematic). For example, BCC messages could capitalize on participants’ perceptions of eggs as nutritious and healthy, emphasizing their ability to provide protein, vitamins, minerals, and strength, while also positioning them alongside other foods participants believe to be nutritious and healthy and that can be eaten with eggs. To address potential physiological concerns with eating eggs, messages could include general tips for how to reduce or prevent nausea and ways to stimulate appetite. To prevent possible fatigue from repeatedly eating eggs in a similar manner (ie, boiled or fried), messages could suggest women prepare eggs in a variety of ways and eat them with a variety of other foods, as their time and resources allow, so they can enjoy eggs in different ways. Most importantly, BCC messages would need to address beliefs related to the idea that consuming too many eggs during pregnancy leads to a big baby and delivery complications. The BCC messages could also include rationale as to why eating eggs throughout the entire pregnancy is safe. Messages could also encourage a gradual increase in intake to avoid a drastic change in consumption patterns that pregnant women may not be comfortable with. As with any BCC intervention, the exact messages need careful pretesting in the target population(s) to be sure they are understood as intended.
Because our study found that a variety of people offer nutrition advice to pregnant women, it would be important for an intervention aimed at increasing pregnant women’s egg consumption to incorporate outreach to the community at large, in addition to the people closest to pregnant women. Educating the key influencers of a woman’s eating behaviors and other community members not only helps facilitate effective support at an individual level but also can help shift social norms in support of appropriate prenatal nutrition at a community level.
Our results point to health workers as an important channel through which to deliver messages and educate women and communities about egg consumption during pregnancy. The fact that most participants expressed reservations about eating too many eggs during pregnancy suggests that health workers likely need additional training to effectively deliver counseling to pregnant women and their families about eating eggs. Furthermore, because husbands cited media (eg, television, radio, and social media) as a main source of information, this avenue could be explored for educating men on nutrition during pregnancy.
The differences we found in knowledge, beliefs, and practices between the urban and rural sites also indicate a need for tailoring messages according to urbanicity. Different ethnic groups may also maintain different cultural beliefs about foods during pregnancy, which may require specific messaging to address. Although we did not analyze our results according to ethnic groups, our sociodemographic data indicate our participants’ 2 predominant ethnic groups were largely divided by urban and rural locations; thus, the results for urban versus rural participants may hold true for Luhya versus Kikuyu participants, respectively.
Our study had several limitations. It was conducted in only 1 urban and 1 rural site, and we did not analyze results by ethnic group, because this variable was not part of our sampling strategy. Because of the ethical complexity of including minors in a study, we did not include young adolescents, 14 to 17 years, who may be the most nutritionally vulnerable pregnant population. Nevertheless, our study also had many strengths. The different methods allowed for triangulation of data, and findings from each phase corroborated results from other phases. In addition to pregnant women, we also interviewed key influencers of their behavior.
In conclusion, our study suggests there is a potential to build an intervention promoting egg consumption among pregnant women in Kenya. Although their egg consumption is currently low, pregnant women, as well as key influencers of their behavior, see eggs as nutritious foods to consume during pregnancy. We also found health workers to be potentially the most effective channel through which to deliver messages to women and communities at large about consuming eggs during pregnancy. Furthermore, the 1-week household trial of egg consumption showed pregnant women are willing to consume eggs regularly. Our study highlights the importance of formative research for informing the development of a communications strategy to create demand for eggs among this vulnerable population.
Footnotes
Acknowledgments
The authors would like to thank our research assistants, transcribers, qualitative research assistant and data manager, the Nutrition and Dietetics Unit within the Ministry of Health, and the study participants for their contributions to the study.
Authors’ Note
CKL and CS conceptualized and designed the study and research questions, with input from FT, AW, VLF, and MEB. FT and AW oversaw data collection. CS conducted quantitative and qualitative data analysis with input from CKL and VLF. CKL and CS prepared the first draft of the manuscript. All authors read, provided feedback for, and approved the final version.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: The research was funded by RTI International through Independent Research and Development funds. The authors employed by RTI International have no financial interest in the results of the study.
