Abstract
Background:
Patellar dislocation in pediatric athletes often involve additional injuries not identified on plain films.
Purpose:
To identify the rate of medial patellofemoral ligament (MPFL) injury and adjunctive injury findings identified by magnetic resonance imaging (MRI) in first-time patellar dislocations in the pediatric population.
Study Design:
Systematic review; Level of evidence, 4.
Methods:
This review was registered with the International Prospective Register of Systematic Reviews (PROSPERO) (CRD: 42024559285). PubMed, EMBASE, and SPORTDiscus were searched for studies on MRI findings after first-time pediatric patellar dislocations. Abstracts and articles were screened using predefined inclusion and exclusion criteria. The inclusion criteria were (1) first-time patellar dislocation, (2) explicit documentation of MRI findings, (3) patients <18 years, and (4) written in English. The exclusion criteria were (1) abstract only, case reports, or review articles; (2) overlapping or repeated patient sets; in such cases, the article containing the more comprehensive variables was retained. Data were extracted regarding patient characteristics and MRI findings. Pooled rates were calculated using only the studies that reported the specific variable in question. Bias was assessed using the Newcastle-Ottawa Scale for cohort and case-control studies, and the Joanna Briggs Institute Critical Appraisal tools for the cross-sectional studies and case series.
Results:
A total of 322 studies were initially identified. After screening by 2 independent reviewers, 12 articles were included in the data extraction. Findings include complete MPFL tears in 47% of cases, while partial MPFL tears were present in 41% of the time. Osteochondral (OC) injury was present in 50% of the MRIs. Among these, chondral lesions were reported in 75% of MRIs, OC lesions in 21%, and OC fractures in 37%. The location of these lesions was isolated to the medial patella facet 66% of the time, compared with the lateral femoral condyle, which was the location for 31% of the lesions. Additionally, loose bodies were found in 34% of MRIs.
Conclusion:
This study highlights the frequent occurrence of significant MRI findings in pediatric first-time acute patellar dislocations, showing that obtaining MRI after first-time patellofemoral instability events in the pediatric population should be standard of care.
Lateral patellar dislocations are most common in the pediatric population, with an incidence of 147/100,000 person-years. 30 Men, aged 13 to 15 years, are at particularly high risk, with the majority of dislocations sustained during sports.11,13 Specific anatomic risk factors for patellar dislocation include trochlear dysplasia, younger skeletal age, ligamentous laxity, lateral patellar tilt, tibial tuberosity to trochlear groove distance of >20 mm, and quadriceps dysplasia.3,8,9 Patella alta has been shown to increase the risk of patellar dislocation, but also decrease the risk of O fractures after first-time and recurrent dislocations.8,17
The majority of first-time patellar dislocations will result in a tear of the medial patellofemoral ligament (MPFL). 44 Other associated injuries after lateral patellar dislocation, including osteochondral fractures (OC), are also common. 18 Rates of cartilage damage on magnetic resonance imaging (MRI) after first-time patellar dislocation have been reported 26 to be as high as 84%. The rate of OC fracture has recently been estimated 17 to be around 25%. A lateralized tibial tubercle and male sex are risk factors for OC fracture after patellar dislocation.17,28
A recent survey of orthopaedic surgeons and primary sports medicine physicians indicated an 82% consensus that the presence of an OC fracture, as seen on radiograph, after a first-time patellar dislocation constitutes a surgical indication. 27 Studies suggest, however, that OC lesions go undetected on plain films in 44% to 78% of cases.5,19,33 Despite this diagnostic limitation, only 51% of orthopaedic surgeons and primary sports medicine physicians obtain an MRI after a pediatric first-time patellar dislocation. 27 This number has been reported as low as 36% in an international survey among orthopaedic surgeons. 7
Neglecting cartilage injuries after patellar dislocation can lead to gradual degeneration of the patellofemoral cartilage and the development of generalized knee osteoarthritis. 29 Approximately half of patients who experience a patellar dislocation will have radiographic evidence of osteoarthritis within 25 years. Early MRI detection of these injuries is essential, as it enables appropriate management to prevent further joint damage and recurrent instability.13,32
This study aimed to systematically review the literature to identify the rate of MPFL injury and the findings of adjunctive injuries identified by MRI in first-time patellar dislocations in the pediatric population. Specifically, we hypothesized that MRI would reveal adjunctive, clinically relevant injuries that have the potential to influence surgical decision-making.
Methods
Study Protocol and Search Strategy
This review followed the PRISMA (Preferred Reporting Items for Systematic Reviews and Meta-Analyses) guidelines. 24 The protocol for this study was registered at the International Prospective Register of Systematic Reviews (PROSPERO CRD: 42024559285).
PubMed, EMBASE, and SPORTDiscus were searched for studies relating to MRI findings after first-time pediatric patellar dislocations. The complete search strategy is outlined in the Appendix (available in the online version of this article). We included all date ranges on the initial search, which was performed on June 17, 2024. An additional search was conducted using the same strategy on October 13, 2024, to identify any additional articles published since our initial search. Abstracts and articles were evaluated on previously established inclusion and exclusion criteria. Two independent reviewers (J.M.R. and C.C.W.) performed the title/abstract and full-text screening, with any persistent disagreements being resolved by the senior author (L.E.L.). The inclusion criteria were as follows: (1) first-time patellar dislocation, (2) explicit documentation of MRI findings, (3) patients <18 years, and (4) written in English. The exclusion criteria were as follows: (1) abstract only, case reports, or review articles; (2) any overlapping or repeated patient sets; in such cases, the article containing the more comprehensive set of variables was retained. Data regarding patient characteristics and MRI findings were then manually extracted. A formal meta-analysis was not performed. Instead, pooled rates were calculated using a summative weighted mean. This approach was used to summarize the available data across studies reporting the variable in question.
Quality Appraisal and Risk of Bias
Bias was assessed using the Newcastle-Ottawa Scale (NOS) for cohort and case-control studies. A star was awarded when an article matched the criteria. There are 3 categories (selection, comparability, exposure) in the NOS and a possible total of 9 stars. A score of 6 to 9 stars is considered good quality, 3 to 5 fair quality, and 0 to 2 poor quality. 41
The Joanna Briggs Institute (JBI) Critical Appraisal Checklist for Analytical Cross-Sectional Studies was used for the cross-sectional studies. The questionnaire consists of 8 questions, which were answered with “yes,”“no,”“unclear,” or “not applicable.” We considered a score of “yes” for >5 times to be high quality, 3 to 4 times moderate quality, and 0 to 2 times low quality. 20
The JBI Critical Appraisal Checklist for Case Series was used for the case series. The questionnaire consists of 10 questions, which were answered with “yes,”“no,”“unclear,” or “not applicable.” We considered a score of “yes” for >7 times to be high quality, 4 to 6 times moderate quality, and 0 to 3 times low quality. 21
Results
Article Screening
After removing duplicate articles, a total of 322 studies were identified as potential articles to be included. After a title and abstract review, a total of 68 full-text articles were screened. The 56 excluded full-text articles were excluded for the following reasons: adult population (24); insufficient MRI documentation (12); recurrent/chronic dislocations (6); abstract only (4); review article (3); overlapping/repeated patient set (3); not in English (2); and retracted article (2). Twelve articles met the inclusion criteria and were included in our review (Figure 1) (Table 1).
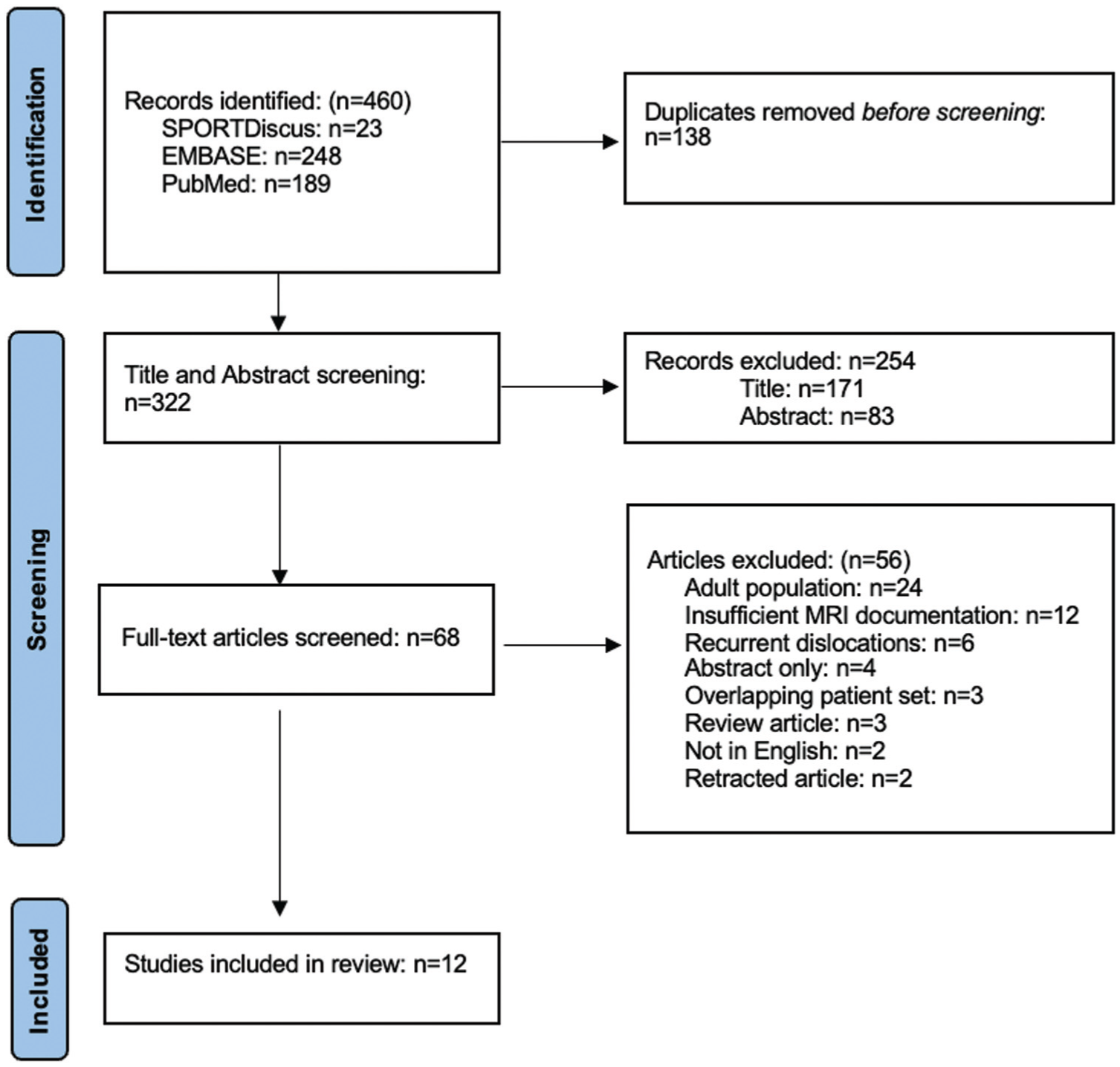
The PRISMA flow diagram shows the selection process for studies. 24 PRISMA, Preferred Reporting Items for Systematic Reviews and Meta-Analyses.
General Characteristics of Included Studies a
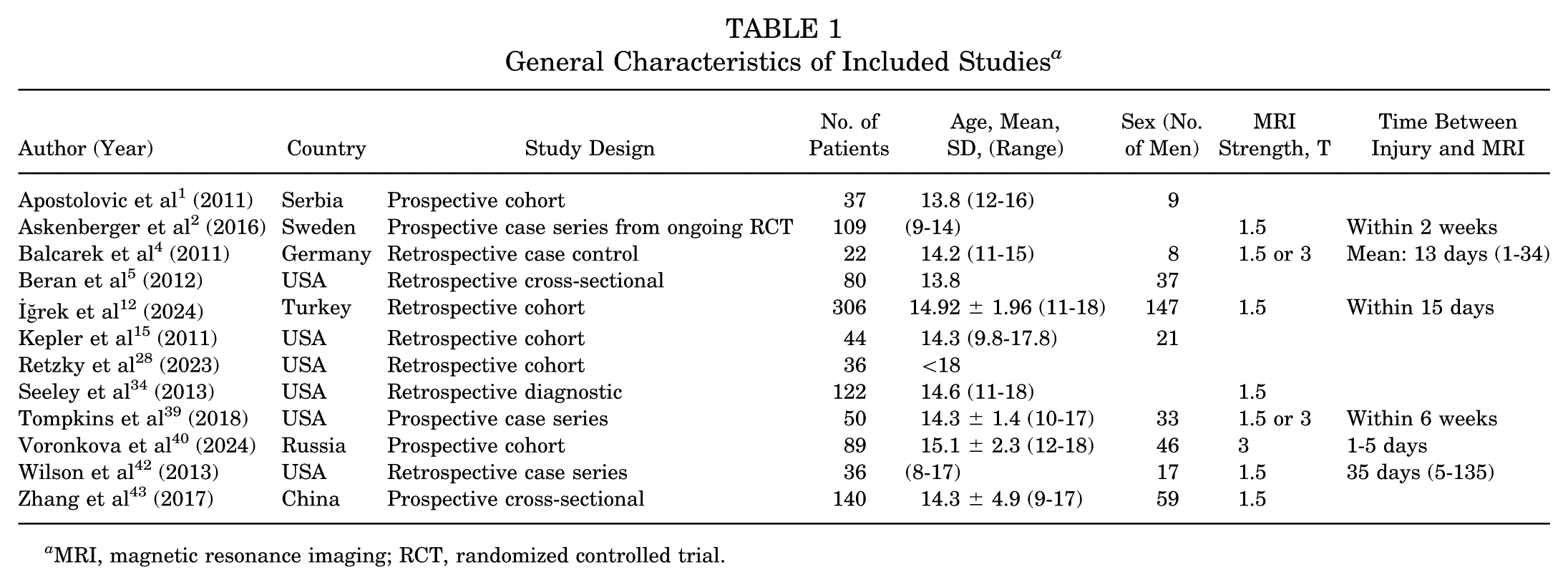
MRI, magnetic resonance imaging; RCT, randomized controlled trial.
MPFL Tears
Four studies reported the degree of MPFL tears (Table 2). Within these 4 studies, 248 knees were examined, with 116 (47%) exhibiting a complete MPFL tear and 101 (41%) showing a partial MPFL tear. In these 4 studies, an MPFL tear was not visible on MRI in 31 (13%) of patients.4,39,42,43
Degree of MPFL Tear a
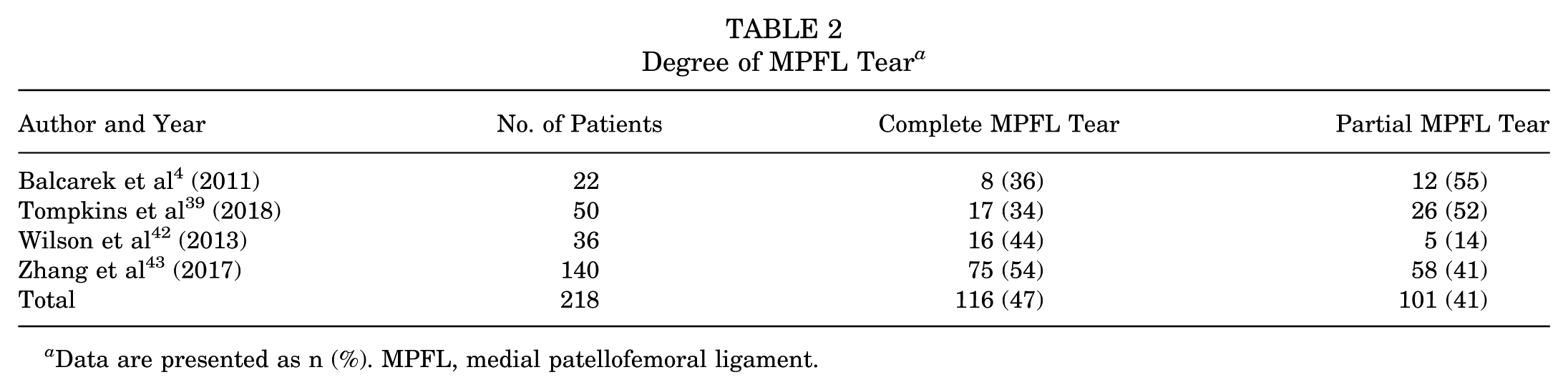
Data are presented as n (%). MPFL, medial patellofemoral ligament.
Chondral/OC Injuries
Data regarding chondral/OC injuries were extracted from 11 articles (Table 3). There was a cumulative total of 517 (50%) out of 1034 patients who had a chondral/OC injury of some degree. Six of the studies specifically reported chondral-only injuries, which were present in 75% of MRIs.4,15,39,40,42,43 Kepler et al 15 reported the mean size of the chondral injuries to be 7.6 mm. Three studies specifically reported OC lesions, which were found to be present in 21% of MRIs.2,5,15 Kepler et al 15 reported the mean size of OC lesions to be 12.5 mm, and all OC lesions listed in the Askenberger et al 2 study were greater than 1cm in size. Four studies specifically reported OC fractures, which were present 37% of the time.4,12,28,34 The study by Kepler et al 15 was the only study that listed both chondral injuries and OC lesions, with chondral injuries being more common, occurring in 41% of the MRIs compared with 23% with OC lesions. The study by Balcarek al 4 was the only study to report both chondral lesions and OC fractures, with chondral lesions being more common, occurring in 23% of cases, compared with OC fractures, which occurred in 5%.
Severity and Location of Chondral/OC Injuries a
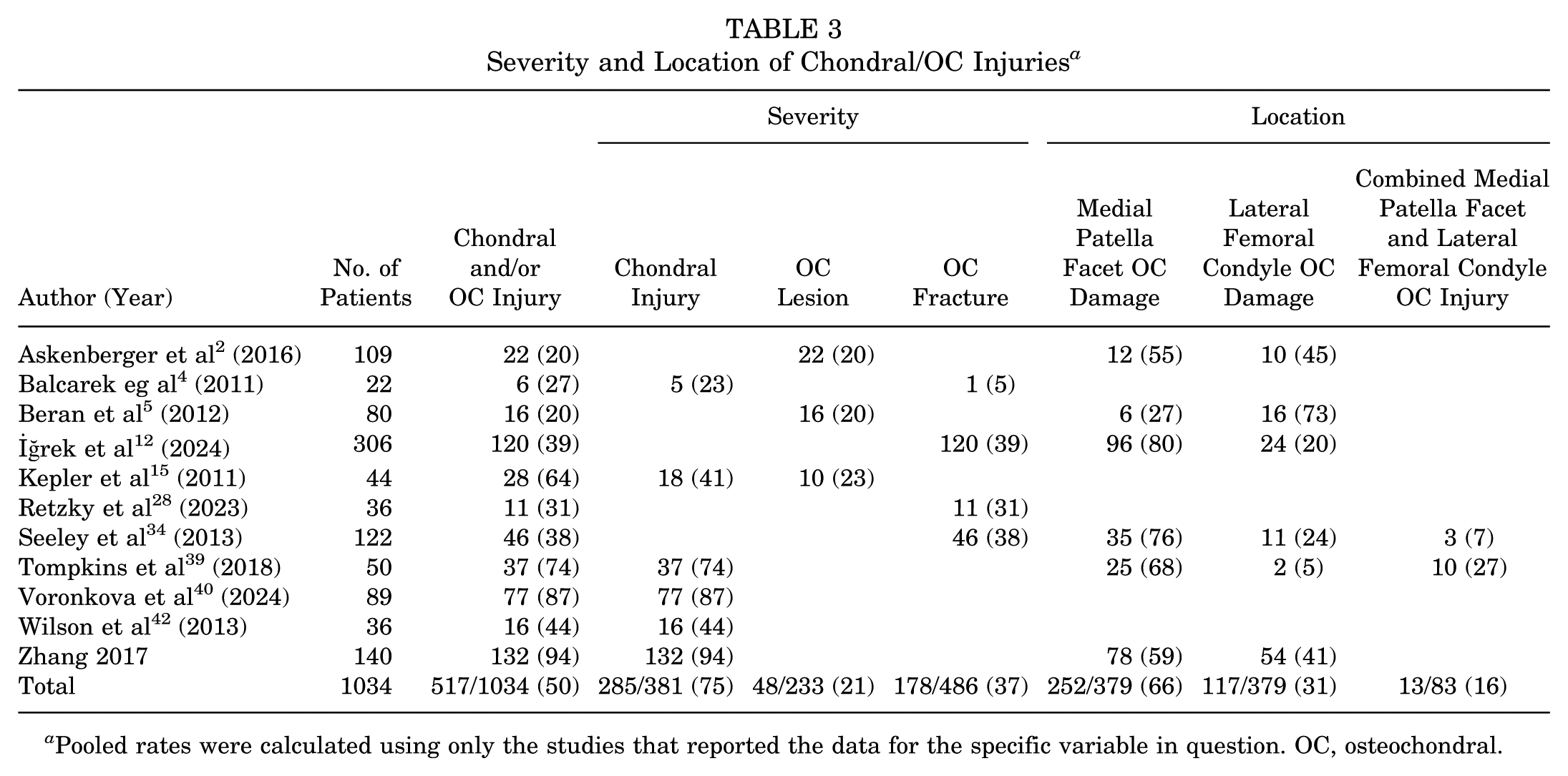
Pooled rates were calculated using only the studies that reported the data for the specific variable in question. OC, osteochondral.
Six studies reported the location of OC injuries, with a higher prevalence of injuries occurring on the medial patellar facet (66%) compared with the lateral femoral condyle (31%). Two studies reported the simultaneous occurrence of OC injuries on both the medial patellar facet and the lateral femoral condyle in the same patient, which occurred in 16% of injuries34,39 (Table 3).
Regarding definitions of chondral injury, OC lesion, and OC fracture, of the 6 studies included in the chondral injury analysis, Voronkova et al, 40 Balcarek et al, 4 and Zhang et al 43 used the Outerbridge classification scale. Tompkins et al 39 described lesions as either full- or partial-thickness. Kepler et al 15 and Wilson et al 42 explicitly stated chondral and cartilage injuries, respectively. OC lesions were explicitly mentioned in 3 studies. Askenberger et al 2 reported OC lesions >1cm2; Beran et al 5 reported MRI evidence of true OC defects in all 16 knees; and Kepler et al 15 explicitly used the term “OC lesions.” All 4 studies included in the OC fracture analysis explicitly mentioned OC fractures.4,12,28,34
Loose Bodies
Three studies reported findings of loose bodies (Table 4). These 3 studies1,34,42 had a combined patient population of 119, with 40 loose bodies identified, resulting in a prevalence of 34%. All 14 of the loose bodies reported by Apostolovic et al 1 were >8 mm in size.
Loose Bodies Reported a
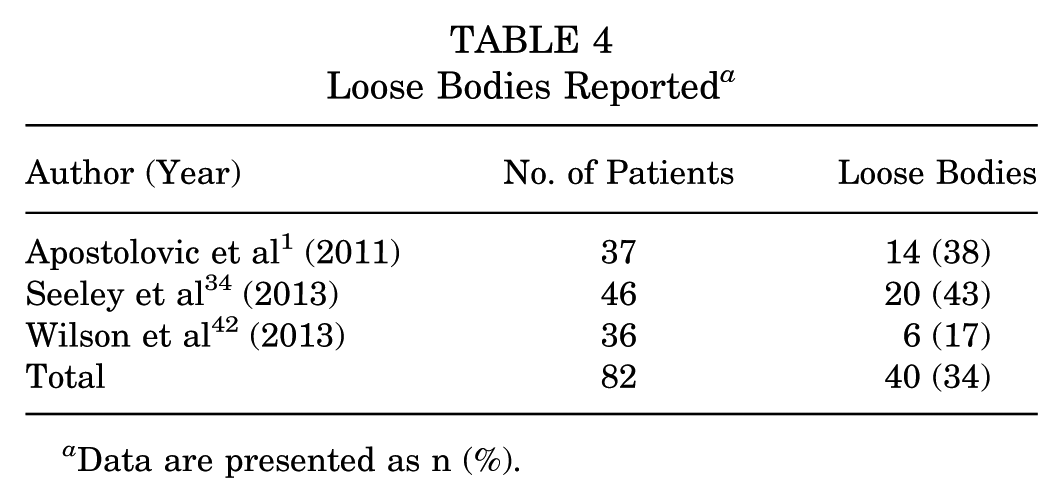
Data are presented as n (%).
Other Findings
Additional notable findings are presented in Table 5. Three studies34,42,43 reported injuries sustained to the vastus medialis oblique (VMO), with a prevalence of 42%. Zhang et al 44 reported the rate of vastus lateralis (VL) injury to be 33%. There were 2 studies that reported a cumulative total of 2 (2%) patients who sustained a meniscal injury.5,42 Beran et al 5 reported 1 (1%) patient who sustained a patellar sleeve fracture. 5 Two studies39,42 evaluated medial collateral ligament (MCL) injury, with a prevalence of 1%. Wilson et al 42 reported one (3%) anterior cruciate ligament (ACL) injury, 1 (3%) popliteus injury, and 6 (17%) patients with Hoffa fat pad edema.
Other Notable Findings a
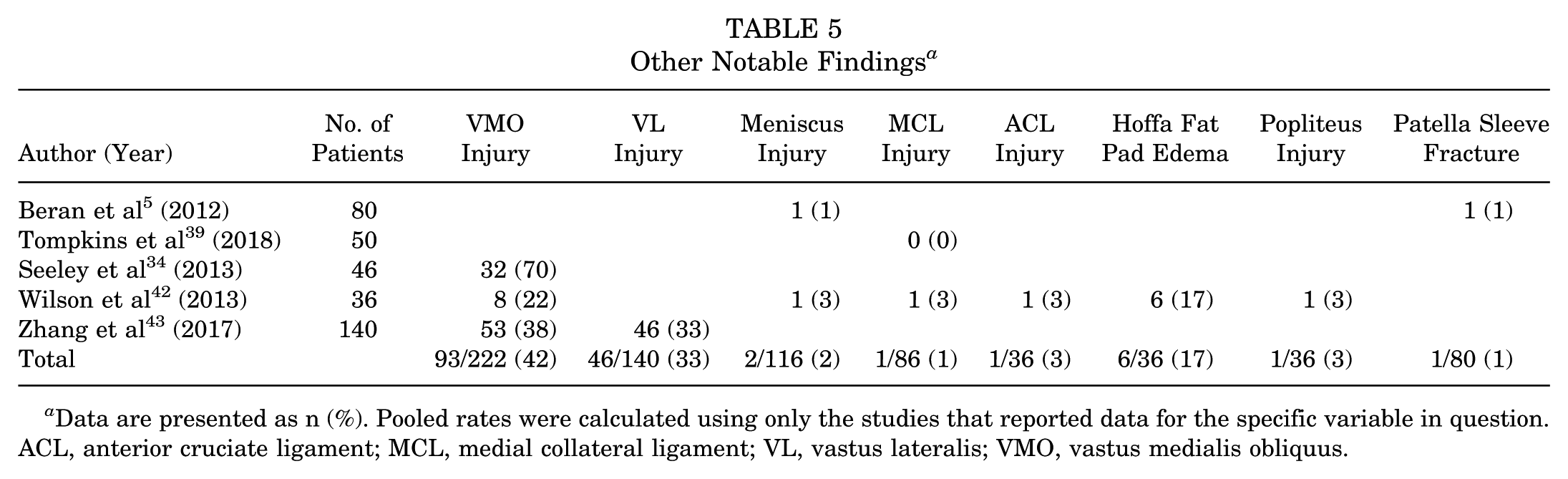
Data are presented as n (%). Pooled rates were calculated using only the studies that reported data for the specific variable in question. ACL, anterior cruciate ligament; MCL, medial collateral ligament; VL, vastus lateralis; VMO, vastus medialis obliquus.
MRI Techniques
Eight studies reported the strength of the MRI magnet, with 5 studies using a 1.5 T magnet, 1 using a 3.0 T magnet, and 2 using a combination of 1.5 T and 3.0 T magnets.2,4,12,34,39,40,42,43 The time between injury and MRI ranged from 1 day to 135 days, depending on the study (Table 1). Three studies reported the positioning of the knee during the MRI, with Balcarek et al 4 and Zhang et al 43 having their patients be in full extension, while Igrek et al 12 had the patients’ knees at 30° of flexion.
Quality Assessment
All 6 cohort and case-control studies were determined to be good quality (6-9 stars) according to the NOS (Table 6). All 3 cross-sectional studies were determined to be of high quality according to the JBI Critical Appraisal Checklist for Analytical Cross-Sectional Studies (Table 7). Finally, all 3 case series were determined to be high quality according to the JBI Critical Appraisal Checklist for Case Series (Table 8).
Newcastle-Ottawa Scale Quality Assessment a
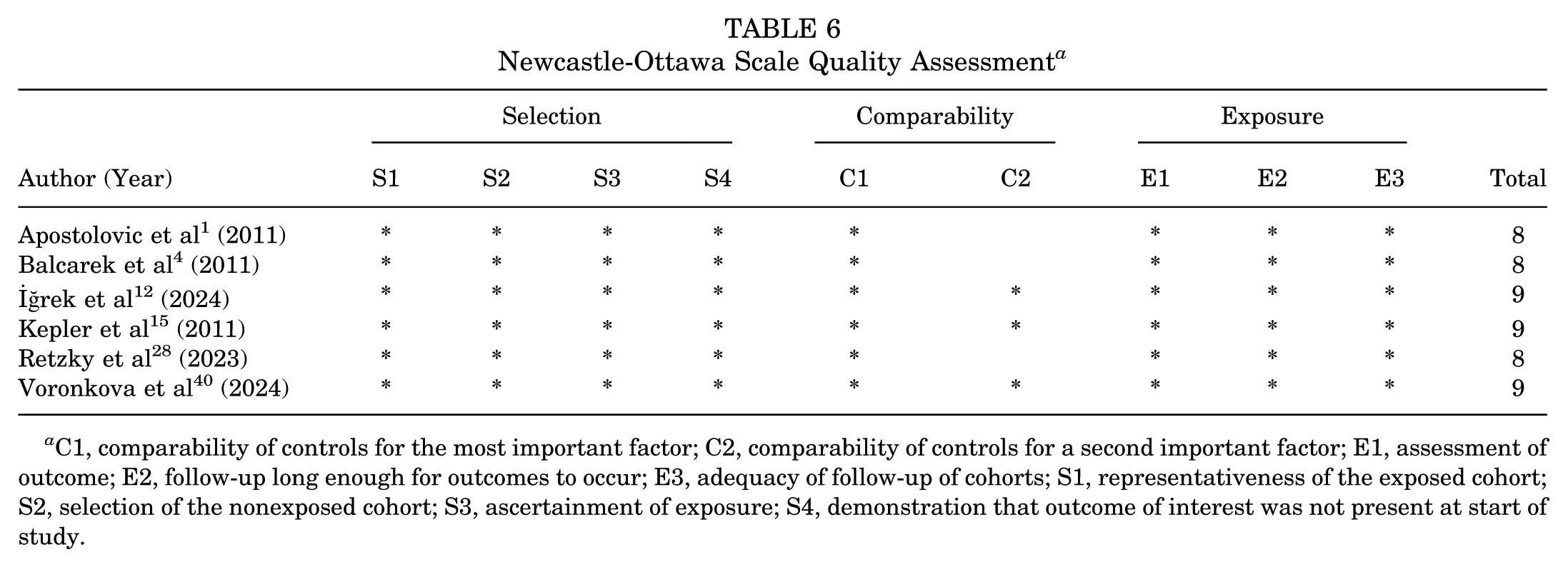
C1, comparability of controls for the most important factor; C2, comparability of controls for a second important factor; E1, assessment of outcome; E2, follow-up long enough for outcomes to occur; E3, adequacy of follow-up of cohorts; S1, representativeness of the exposed cohort; S2, selection of the nonexposed cohort; S3, ascertainment of exposure; S4, demonstration that outcome of interest was not present at start of study.
JBI Critical Appraisal Checklist for Cross-Sectional Studies a
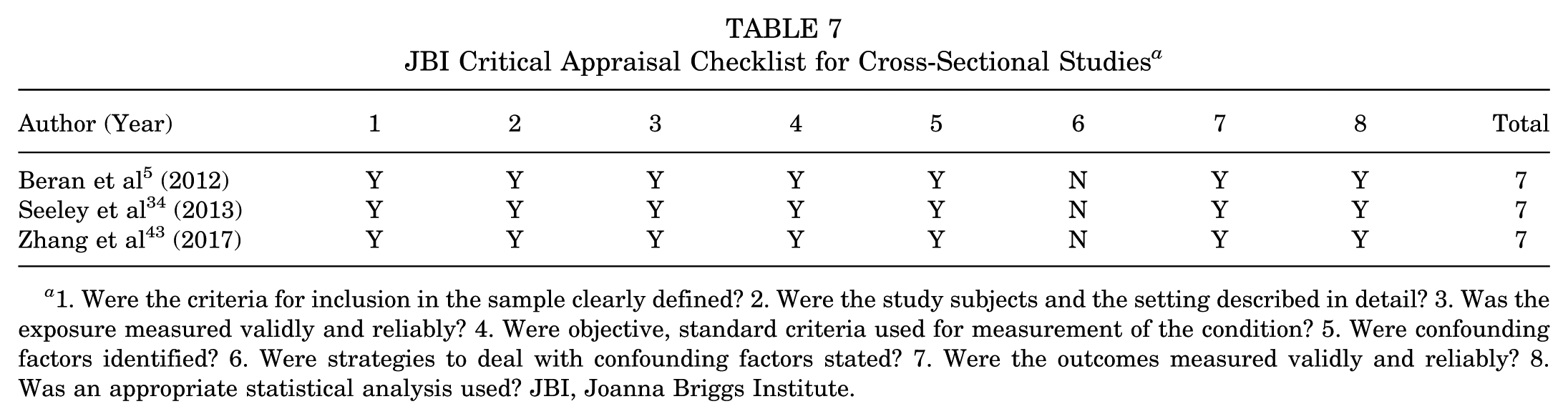
1. Were the criteria for inclusion in the sample clearly defined? 2. Were the study subjects and the setting described in detail? 3. Was the exposure measured validly and reliably? 4. Were objective, standard criteria used for measurement of the condition? 5. Were confounding factors identified? 6. Were strategies to deal with confounding factors stated? 7. Were the outcomes measured validly and reliably? 8. Was an appropriate statistical analysis used? JBI, Joanna Briggs Institute.
JBI Critical Appraisal Checklist for Case Series a
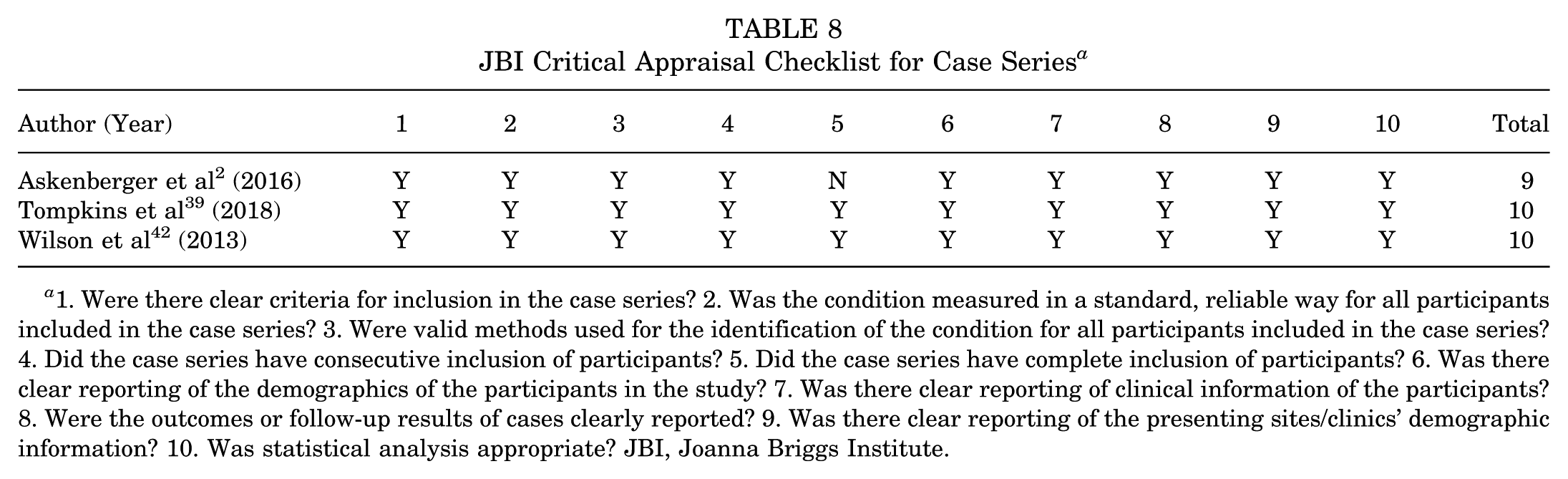
1. Were there clear criteria for inclusion in the case series? 2. Was the condition measured in a standard, reliable way for all participants included in the case series? 3. Were valid methods used for the identification of the condition for all participants included in the case series? 4. Did the case series have consecutive inclusion of participants? 5. Did the case series have complete inclusion of participants? 6. Was there clear reporting of the demographics of the participants in the study? 7. Was there clear reporting of clinical information of the participants? 8. Were the outcomes or follow-up results of cases clearly reported? 9. Was there clear reporting of the presenting sites/clinics' demographic information? 10. Was statistical analysis appropriate? JBI, Joanna Briggs Institute.
Discussion
The results of this study demonstrate a relatively high frequency of adjunctive MRI findings in pediatric patients with first-time acute patellar dislocations. As expected, complete or partial MPFL tears were identified in most patients (88%). Of particular interest was the rate of chondral and OC lesions identified on MRI, given the potential surgical implications of these findings.18,38 The rate of all-inclusive chondral/OC lesions, which was described in all 11 studies, was 50%. Where specified, 21% of patients were noted to have OC lesions, and 37% had OC fractures. Furthermore, loose bodies were identified in 34% of patients in the 3 studies that specifically noted loose bodies.
The current indications for MRI in first-time patellar dislocations are controversial, with some authors advocating for MRI only in the radiographic presence of hemarthrosis or OC lesion, and others advocating for universal use of MRI.14,36 In a scoping review by Sinikumpu et al, 36 they advocated for the universal application of MRI, citing both the discovery of potentially operative injuries unique to MRI (OC lesions and loose bodies primarily), as well as evaluation of anatomic risk factors, which predispose to recurrent dislocation (trochlear dysplasia and tibial tubercle-trochlea groove distance). 36 Radiographs have notoriously poor sensitivity in identifying both OC lesions and loose bodies, cited as low as 30% when compared with arthroscopic identification. 37 Given the relative consensus that a large (≥1 cm) OC fragment is an indication for surgery, accurate identification of these fragments is imperative in the acute setting. 18 The results of this study suggest that approximately one-third of patients with first-time acute patellar dislocation have an OC lesion, fractures, and/or loose bodies identified on MRI, with the sizes frequently >1cm. Although arthroscopy remains the gold standard for diagnosis, modern 3T MRI demonstrates a high sensitivity for deep chondral/OC injuries of the knee, which encompass the majority of surgically relevant articular injuries.10,16 Nonoperative management of first-time patellar dislocations remains a mainstay of treatment. It is important, however, to recognize that the associated OC injuries, trochlear dysplasia, and recurrent patellar dislocations are all independent risk factors for the subsequent development of patellofemoral osteoarthritis. 31 The goal of surgical intervention is to prevent recurrent instability, as well as prevent arthrosis from altered patellofemoral biomechanics or loose body abrasion. 23 MRI is critical in the decision point between operative and nonoperative management of patellar dislocations, as it is the optimal modality to detect operative OC lesions while providing an accurate assessment of trochlear dysplasia and other anatomic risk factors for osteoarthritis and recurrent instability.36,37 Given the relatively high rates of potentially operative adjunctive findings demonstrated in this study, MRI should be the standard of care after first dislocations.
The data we collected were unable to detect any specific patient characteristics that would justify a routine MRI. However, by obtaining an MRI after a first-time patellar dislocation, one could evaluate anatomic risk factors that place a patient at increased risk for recurrent patellar dislocation and subsequent increased risk for patellofemoral osteoarthritis.3,17 Surgical treatment should especially be considered in this patient population to decrease the risk of subsequent dislocation.9,22
A relatively high rate of VMO (42%) and VL (33%) injuries was also identified in the studies where this was documented. While these findings are of limited surgical consequence, the dynamic contribution of balanced quadricep activation to patellar instability is well described.6,25,35 Furthermore, VMO atrophy has been described in patients with recurrent patellar dislocations, and this may be in part due to initial acute injury. Identification of quadriceps injury, particularly to the VMO, may be of rehabilitative relevance, although research in this area is limited. 35 Regardless, the high rate of VMO injuries demonstrated in this study highlights the importance of quadricep strengthening and rehabilitation after first-time patellar dislocation. MRI may facilitate improved patient selection for intensive rehabilitation protocols.
Finally, a low rate of associated meniscal and non-MPFL ligamentous injuries was identified. In total, 2 patients were identified with concomitant meniscal injuries, one with an MCL injury, and another with an ACL injury. This provides reassurance regarding the rarity of concomitant operative ligamentous/meniscal injuries, except in the setting of atypical injury mechanisms.
To the best of our knowledge, this is the first study to synthesize and collectively quantify the pathologic findings of MRI in pediatric patients with first-time acute patellar dislocations. This study provides valuable information regarding the relative rates of imaging findings, which may inform early intervention and improved prognostication. Yet, there are inherent limitations to this study. First, despite standard search parameters, studies may have been missed if not published in the English language or indexed in the databases searched. Secondly, the included studies varied widely in their methodology, sample sizes, and reporting, which limits the detail of the pooled analyses and may introduce biases. Specifically, performance bias cannot be excluded given the variation in MRI machines (1.5 T vs 3 T) and protocols (time variation from 1 to 135 days after injury). These factors can influence detection and are a potential source of heterogeneity. Furthermore, reporting bias may exist given that the data extraction was based on completeness and accuracy of the included studies, all of which varied in the granularity of details reported in MRI findings. For example, only 3 studies reported loose body findings, despite a relatively high rate of occurrence (34%). Voronkova et al 40 specifically excluded injuries that involved cartilage detachment, but the number of patients excluded on this basis was not disclosed. Variation in study aims (eg, operative vs nonoperative treatment) and corresponding exclusion criteria, along with differences in time from injury to MRI and in MRI techniques, may all contribute to underreporting and variability in reported outcomes. While the MRI findings were well-documented, it remains unclear what effect the MRI had on management and recurrence. Additionally, variable grading systems and descriptors were used in reporting (ie, severity of chondral injury), limiting the ability to provide a nuanced description of findings and requiring limited interpretation by the authors to assimilate intra-study data. Pooling data in this way helped protect against the overestimation or underestimation of findings inherent to the wide variation of sample sizes present in this study. Finally, this study does not have any direct analysis of clinical outcomes or follow-up data related to the findings described. It is further unable to state conclusively how often the MRI findings described directly affected the treatment plan, instead relying on inferences of general surgical indications from outside studies. The findings in this paper do, however, provide a framework for the potential utility of MRI in the acute setting and how its use may affect clinical decision-making.
Conclusion
There is a high frequency of adjunctive MRI findings after first-time pediatric patellar dislocation, with OC lesions, fractures, and/or loose bodies present in approximately one-third of patients. In contrast to the poor sensitivity of plain radiographs in identifying these intra-articular injuries, these advanced imaging findings show that obtaining an MRI after first-time patellofemoral instability events in the pediatric population should be the standard of care.
Supplemental Material
sj-pdf-1-ajs-10.1177_03635465251383851 – Supplemental material for Frequency of Adjunctive MRI Findings on First-Time Patellar Dislocations in Pediatric Patients: A Systematic Review
Supplemental material, sj-pdf-1-ajs-10.1177_03635465251383851 for Frequency of Adjunctive MRI Findings on First-Time Patellar Dislocations in Pediatric Patients: A Systematic Review by Jake M. Reed, Colby C. Wollenman, Breann K. Tisano, Kevin M. Dale and Lance E. LeClere in The American Journal of Sports Medicine
Footnotes
Submitted February 11, 2025; accepted July 23, 2025.
One or more of the authors has declared the following potential conflict of interest or source of funding: L.E.L. is a member of the boards of directors of AOSSM and an editorial board member of the American Journal of Sports Medicine, Arthroscopy, and the Video Journal of Sports Medicine. AOSSM checks author disclosures against the Open Payments Database (OPD). AOSSM has not conducted an independent investigation on the OPD and disclaims any liability or responsibility relating thereto.
An online CME course associated with this article is available for 1 AMA PRA Category 1 Credit™ at https://education.sportsmed.org/Public/Catalog/Home.aspx?CourseSearch=1&Criteria=9&Option=25. In accordance with the standards of the Accreditation Council for Continuing Medical Education (ACCME), it is the policy of The American Orthopaedic Society for Sports Medicine that authors, editors, and planners disclose to the learners all financial relationships during the past 12 months with any commercial interest (A ‘commercial interest’ is any entity producing, marketing, re-selling, or distributing health care goods or services consumed by, or used on, patients). Any and all disclosures are provided in the online journal CME area which is provided to all participants before they actually take the CME activity. In accordance with AOSSM policy, authors, editors, and planners’ participation in this educational activity will be predicated upon timely submission and review of AOSSM disclosure. Noncompliance will result in an author/editor or planner to be stricken from participating in this CME activity.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
