Abstract
Background:
Femoroacetabular impingement (FAI) is a major cause of hip pain in young adults and athletes. Surgical treatment of FAI is recommended in cases of failed nonoperative treatment that have the typical clinical and radiographic findings. At present, the role of risk factors for revision surgery and progression to total hip arthroplasty (THA) in patients with FAI is still unclear.
Purpose:
To investigate the possible association between (1) rate of revision and progression to THA and (2) patient characteristics, type of lesion, family history of hip disease, type of intervention, radiographic parameters, physical examination, and pre- and postoperative scores.
Study Design:
Systematic review; Level of evidence, 4.
Methods:
The present systematic review was performed according to the PRISMA (Preferred Reporting Items for Systematic Reviews and Meta-Analyses) guidelines. In October 2020, the main online databases were accessed. All articles concerning surgical correction for selected patients with FAI were accessed. Patient characteristics, type of intervention, radiographic parameters, physical examination, and pre- and postoperative scores were assessed. The outcomes of interest were the possible association between these variables and the rate of revision and subsequent progression to THA using a multivariate analysis through the Pearson product-moment correlation coefficient.
Results:
Data from 99 studies (9357 procedures) were collected. The median follow-up was 30.9 months (interquartile range, 24.0-45.0). The mean ± SD age was 33.4 ± 9.3 years; mean body mass index (BMI), 24.8 ± 4.8; percentage right side, 55.8% ± 8.0%; and percentage female sex, 47.5% ± 20.4%. The overall rate of revision was 5.29% (351 of 6641 patients), while the rate of subsequent progression to THA was 3.78% (263 of 6966 patients). Labral debridement (P < .0001), preoperative acetabular index (P = .01), and BMI (P = .03) all showed evidence of a statistically positive association with increased rates of THA. No other statistically significant associations were found between patient characteristics, type of lesion, family history of hip disease, type of intervention, radiographic parameters, physical examination, or pre- and postoperative scores and the rate of revision and/or progression to THA.
Conclusion:
Although surgical procedures to treat FAI led to satisfactory outcomes, there was a revision rate of 5.29% in the 9357 procedures in the present systematic review. The rate of progression to THA after a median follow-up of 30 months was 3.78%. Patients who have a higher BMI and/or have a pathologic acetabular index and/or undergo labral debridement during correction of FAI are more at risk for a subsequent THA. We advocate additional education of this patient population in terms of expected outcomes and suggest surgical labral repair instead of debridement if needed.
In patients with femoroacetabular impingement (FAI), anatomic abnormalities of the femoral head and/or the acetabulum produce pathologically high contact forces between the femur and the acetabulum. FAI can be a cause of activity limitation, decreased hip function, and significant hip pain, especially in young adults and athletes, because of cartilage and labral damage.38,39 These repetitive insults to the cartilage and labrum result in early hip degeneration and osteoarthritis 106 ; 79% of patients with osteoarthritis of the hip displayed subtle developmental changes on radiographs obtained before adulthood.38,48 FAI can be classified into 3 types depending on the origin of the pathology, being on the femur (cam), acetabulum (pincer), or both (mixed). In previous cross-sectional studies of 4151 individuals, 19.6% of men and 5.2% of women exhibited a pistol grip deformity of the proximal femur, which was defined by calculating the triangular index. 42 Surgery is indicated in symptomatic patients with clinical and radiographic findings of FAI whose nonoperative treatment has failed for a minimum of 3 months. 62 In these patients, surgical options include femoral osteochondroplasty to improve the femoral head-neck offset; debridement, repair, or reconstruction of the labrum; and/or removal of an excessive acetabular rim.31,66,79 Ganz et al 39 first described the technique of surgical hip dislocation for the treatment of FAI in 2003, and several studies have shown good clinical outcomes using this technique.5,91 Given the long operating and recovery time of open hip dislocation surgery, a mini-open anterior technique was developed by Clohisy and McClure, 20 who accessed the hip joint through a Hueter approach. Over the past few years, arthroscopic management of FAI has become popular, with a decrease in complications and faster recovery.60,83,97
All surgical interventions aim to improve patients’ activity levels, relieve hip pain, and restore natural hip function. The various surgical techniques for management of FAI are all successful (surgical hip dislocation, mini-open, arthroscopy), but data on rates of revision and progression to total hip arthroplasty (THA) are limited. So far, prognostic factors for surgical outcome for FAI are still unclear. Thus, the present systematic review investigated the risk factors for revision surgery and progression to THA in patients who underwent surgery for symptomatic FAI. A multivariate analysis was conducted to investigate the association between (1) rate of revision and progression to THA and (2) patient characteristics, type of lesion, type of intervention, radiographic parameters, physical examination, and pre- and postoperative scores.
Methods
Search Strategy
The present systematic review was performed according to the PRISMA (Preferred Reporting Items for Systematic Reviews and Meta-Analyses) guidelines. 77 We followed the PICO protocol for the preliminary search:
P (problem): FAI
I (intervention): surgical correction
C (comparator): generalities, type of intervention, radiographic parameters, tests, scores
O (outcomes): revision rate and progression to THA
Literature Search
Two authors (F.M., A.B.) independently performed the literature search in October 2020, accessing the following databases with no time constraints: PubMed, Embase, Google Scholar, and Scopus. The following keywords were used in combination: hip, FAI, femoroacetabular impingement, arthroscopy, mini-open, open, surgery, dislocation, treatment, therapy, cam, pincer, mixed, labral, acetabulum, femur, pelvis, pain, debridement, repair, reconstruction, THA, complications, pain. The resulting titles and eventually the abstracts were screened by the 2 authors. The full text of the articles of interest was accessed. The references were also screened. Disagreements between the authors were solved by a third senior author (M.B.).
Eligibility Criteria
All the articles concerning surgical correction for patients with FAI were accessed. To be eligible for inclusion, articles had to report the rate of revision and/or progression to THA at last follow-up. Any kind of surgical intervention that did not involve THA was considered revision surgery. According to the authors language capabilities, articles in English, Italian, French, German, and Spanish were considered. Articles of level 1 to 4 according to the Oxford Centre of Evidenced-Based Medicine were considered. 55 Data from national registries were not considered. Reviews, letters, expert opinion, case reports, and editorials were not eligible. Animal, biomechanical, and cadaveric studies were also not considered. Articles regarding revision settings were not eligible. Studies with data based on combined treatments, as well as those focusing on rehabilitation protocols, were excluded. Studies including adjuvants or innovative surgical procedures were excluded. The studies were included regardless of the surgical exposure (arthroscopic, mini-open, open). Studies treating skeletally immature patients were included, as were those describing outcomes in patients who were obese. Studies with data on patients >60 years old or with clear evidence of advanced hip degeneration (Tönnis grade III) were not included. Case series of <10 patients were also excluded. Only studies reporting quantitative data under the outcomes of interest were analyzed.
Data Extraction
Data extraction was performed by 2 authors (F.M., A.B.). Data from the following endpoints were collected:
Generalities: author and publication year, journal, type of study, follow-up duration, number of patients and procedures, mean age, body mass index (BMI), sex, side of surgery, return to sport
Type of intervention: labral debridement, labral repair, labral reconstruction
Radiographic parameters: femoral offset (millimeters), acetabular inclination (Tönnis angle), α-angle (anteroposterior, groin-lateral), β-angle, sharp angle, center-edge angle, anterior center-edge angle, lateral center-edge angle, acetabular index, Tönnis grade, caudocranial femoral coverage (percentage), anterior coverage (percentage), posterior coverage (percentage), crossover sign, and joint space (medial, foveal, lateral)
Physical examination: range of motion (flexion, extension, abduction, adduction, internal and external); anterior, lateral, and posterior impingement test (percentage positive)
Pre- and postoperative scores: Harris Hip Score, modified Harris Hip Score, Non-arthritic Hip Score, 12-Item Short Form Health Survey (SF-12; physical and mental subscales), Hip Outcome Score (activities of daily living and sport-specific subscales), International Hip Outcome Tool–12 and −33, and visual analog scale
The present work investigated whether the aforementioned endpoints were associated with the rate of revision and subsequent progression to THA. Thus, every endpoint was independently analyzed, and its association with revision and progression to THA was assessed.
Methodological Quality Assessment
The methodological quality assessment was made through the Coleman Methodology Score (CMS). 23 The CMS analyzes studies under several items: number of patients, follow-up, type of surgical approach, and study design, as well as descriptions of diagnosis, surgical technique, and postoperative rehabilitation. Furthermore, outcome criteria, the procedure of assessing outcomes, and a description of the sample selection process are evaluated. The quality is scored from 0% (poor) to 100% (excellent), with values >60% considered satisfactory.
Statistical Analysis
The statistical analyses were performed by the main author (F.M.). For the analytical statistics, STATA software (Version 16; StataCorp) was used. The Shapiro-Wilk test was performed to investigate data distribution. For normal data, mean and standard deviation were calculated. For nonparametric data, median and interquartile range were calculated. Multiple pairwise correlations using the Pearson product-moment correlation coefficient (r) were performed to investigate the association between the endpoints were accomplished. According to the Cauchy-Schwarz inequality, the final effect ranks between +1 (positive linear correlation) and −1 (negative linear correlation). Values of 0.1 < | r | < 0.3 and 0.3 < | r | < 0.5 and | r | > 0.5 were considered to have poor, moderate, and strong correlation, respectively. Possible associations with the outcomes of interest were evaluated for each endpoint. Overall significance was evaluated using the χ2 test. A linear regression of the statistically significant correlations was made, and added-variable plots were displayed. Values of P > .05 were considered statistically significant.
Results
Search Results
The literature search resulted in 1174 articles. Initially, 509 articles were excluded because of duplication; 529 articles were then excluded because of the following: type of study (n = 187), nonoperative techniques (n = 91), combined treatments (n = 47), adjuvants and/ or innovative surgeries (n = 41), language limitations (n = 22), uncertain data (n = 7), or other (n = 134). A further 37 articles were excluded because they did not match the topic of interest or report quantitative data under the outcomes of interest. Finally, 99 articles were included for analysis: 3 randomized clinical trials, 36 prospective studies, and 60 retrospective studies. The literature flowchart is shown in Figure 1.
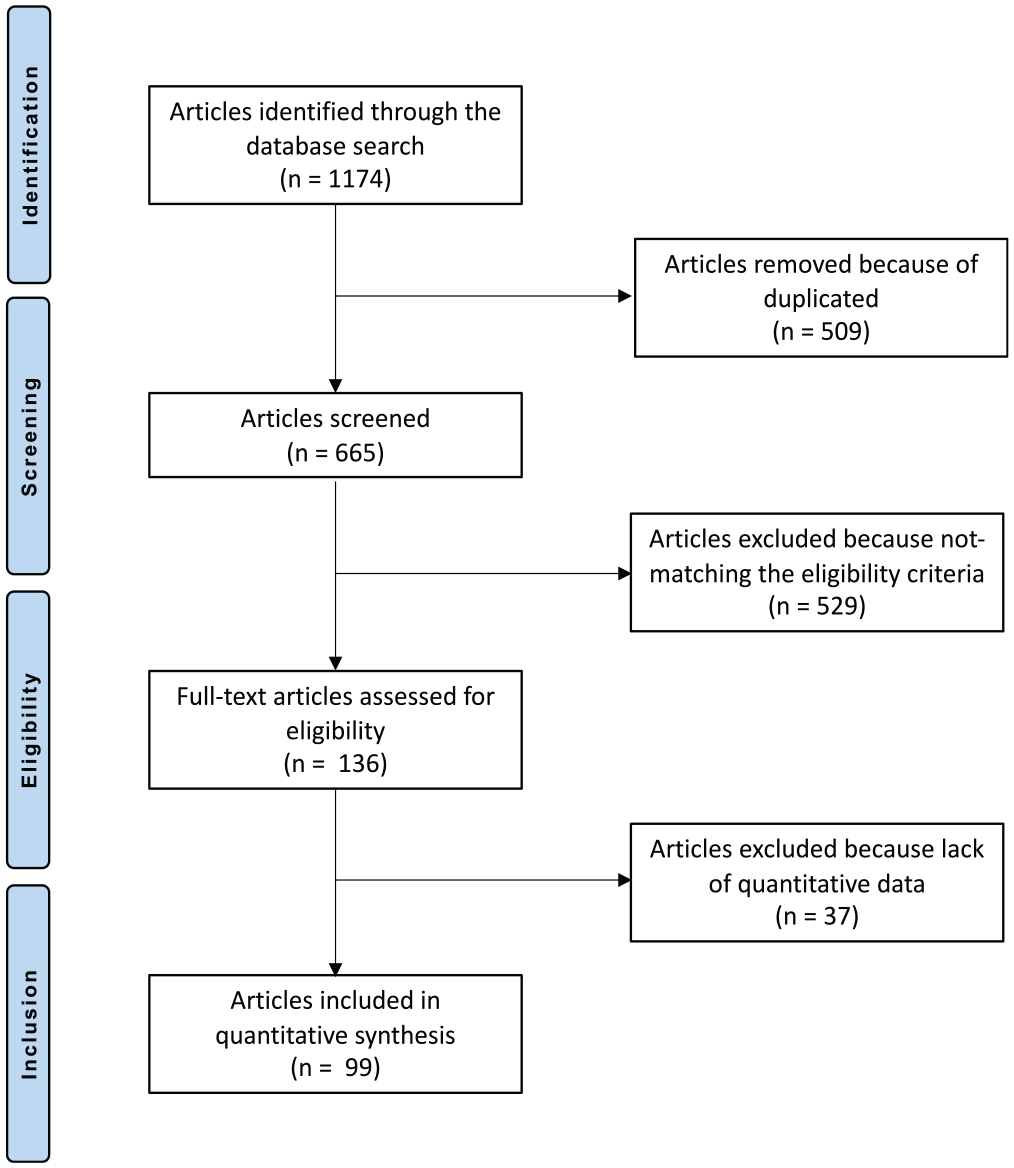
Flowchart of the literature search.
Methodological Quality Assessment
The CMS evidenced the overall limited quality of the studies. Indeed, 60% of studies were retrospective, 36% prospective, and only 3% were randomized trials. Eligibility criteria and rehabilitation protocols were frequently not indicated. General health measures were rarely cited. The procedure of assessing outcomes was often biased or not clearly described. The study size and mean follow-up were well-reported in most studies. The descriptions of diagnoses and surgical techniques were also commonly well-described. The overall CMS was 64.7 points (range, 40-85), attesting to the acceptable quality of the methodological assessment of the present study (Table 1).
Generalities of the Included Studies and Demographic Baseline of the Patients a
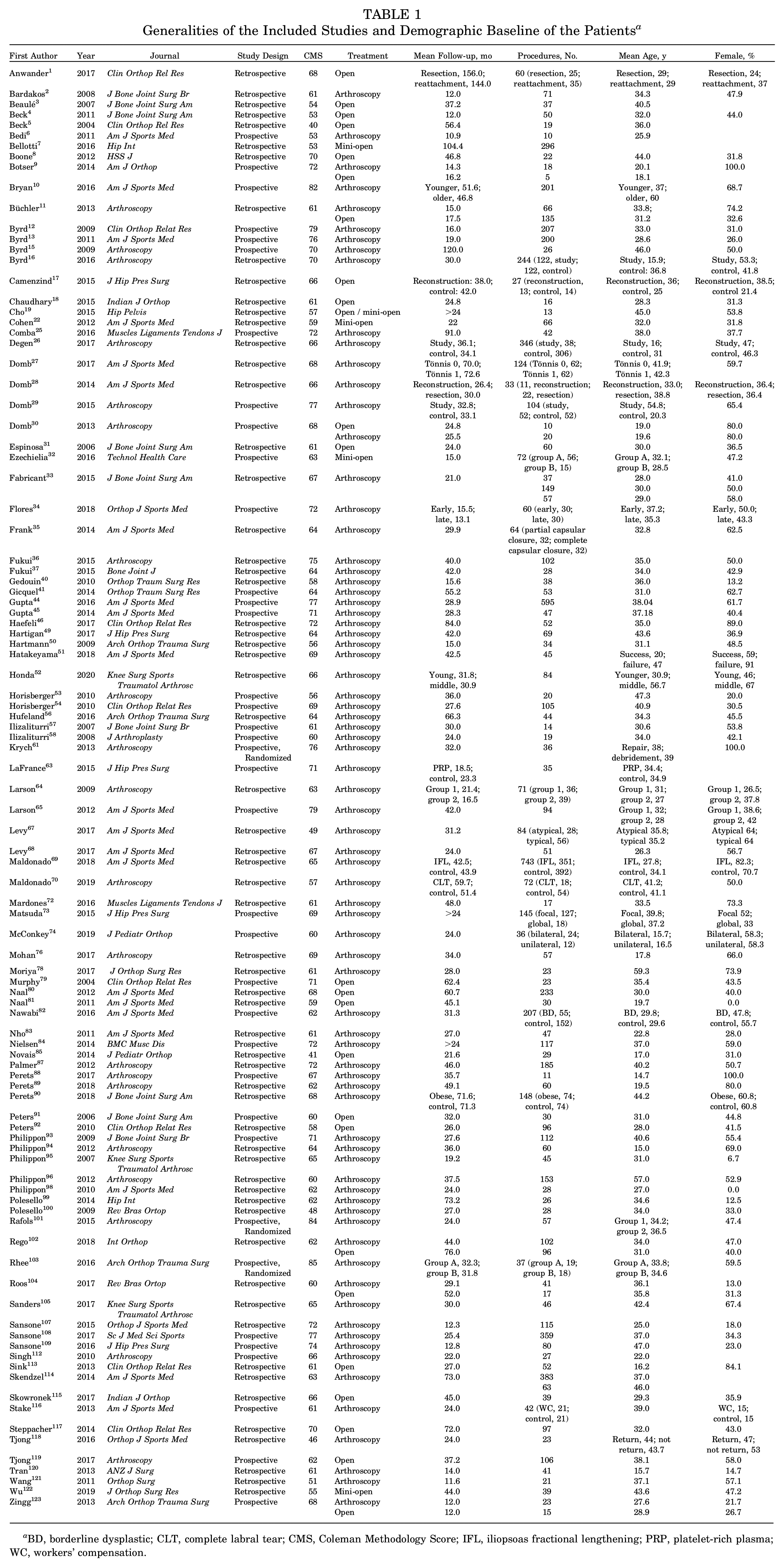
BD, borderline dysplastic; CLT, complete labral tear; CMS, Coleman Methodology Score; IFL, iliopsoas fractional lengthening; PRP, platelet-rich plasma; WC, workers’ compensation.
Patient Demographics
Data from 9357 procedures (8897 patients) were collected. The median follow-up was 30.9 months (interquartile range, 24.0-45.0). The mean ± SD age was 33.4 ± 9.3 years; mean BMI, 24.8 ± 4.8; percentage right side, 55.8% ± 8.0%; and percentage female sex, 47.5% ± 20.4%. Baseline characteristics are shown in Table 1.
Outcomes of Interest
The overall rate of revision was 5.29% (351 of 6641 patients), while the rate of subsequent progression to THA was 3.78% (263 of 6966 patients). Labral debridement showed evidence of a statistically significant positive and strong association with an increased rate of progression to THA (r = 0.77; P < .0001). Equally, a higher preoperative acetabular index showed evidence of a statistically significant positive and strong association with an increased rate of progression to THA (r = 0.89; P = .01). The BMI at baseline showed evidence of a statistically significant positive and moderate association with an increased rate of THA (r = 0.43; P = .03). No other statistically significant associations were found between patient characteristics, type of lesion, type of intervention, radiographic parameters, physical examination, or pre- and postoperative scores and the rate of revision and/or progression to THA. The added-variable plots of these regressions are shown in Figure 2. The multivariate analysis including all the endpoints is shown in Appendix Table A1 (available in the online version of this article).
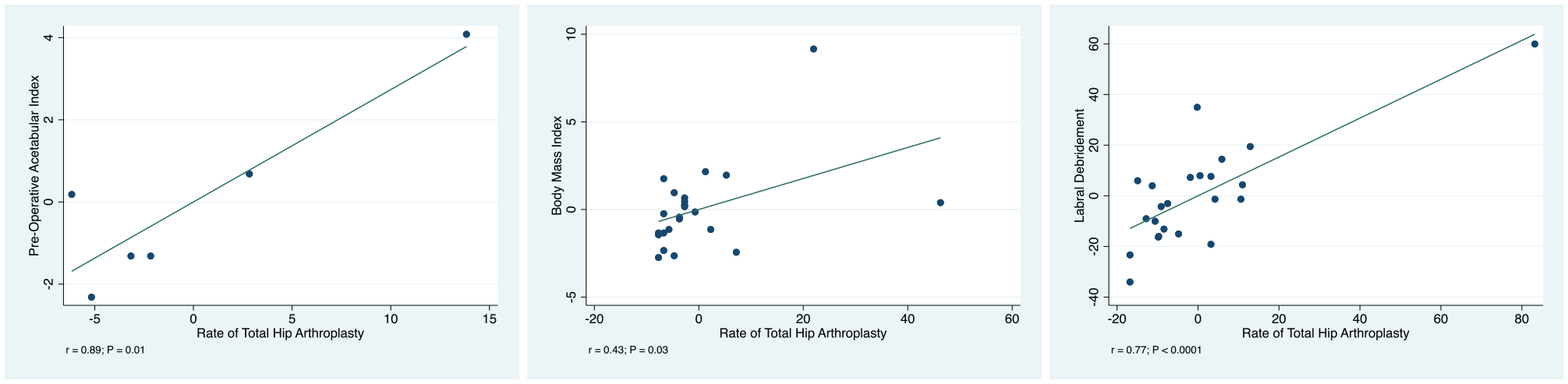
Added-variable plots of the associations: acetabular index, body mass index, and labral debridement.
Discussion
FAI is a frequent and well-recognized cause for hip pain, joint damage, and early-onset osteoarthritis in young adults and athletes. Over the past few decades, better understanding of the pathophysiology and natural course of FAI has led to earlier identification and improved treatment options for this condition. The present study described the rates of revision and THA progression after surgical treatment of FAI, identifying some variables associated with increased rates of progression to THA. The overall revision rate after surgical treatment of FAI was 5.29%, and 3.78% of 9357 procedures progressed to THA. To date, this is the largest systematic review to analyze revision and progression rates after surgical treatment of FAI, including a total of 99 studies. According to the main results of the present study, BMI at baseline, labral debridement, and acetabular index were significantly associated with an increased rate of progression to THA. No other statistically significant associations were identified between patient characteristics, type of lesion, type of intervention, radiographic parameters, physical examination, or pre- and postoperative scores and the rate of revision and/or progression to THA.
Surgical hip dislocation for the treatment of FAI—including labral repair, labral debridement, femoral osteochondroplasty, and acetabuloplasty—leads to improvements in hip range of motion, radiographic parameters, and clinical outcomes comparable with those of hip arthroscopy.30,80,91,117 Surgical treatment for FAI, regardless of the technique, improves hip function, with 68% to 96% of patients reporting good to excellent results after a minimum follow-up of 2 years. 21
One of the main findings of our study was an overall revision rate of 5.29% after surgical treatment of FAI (open hip dislocation, mini-open, and arthroscopic). These findings are similar to those from a registry study from the United Kingdom, which showed a revision hip arthroscopy rate of 4.5% at a mean 1.7 years. 71 In a systematic review of >6000 patients, the reoperation rate was 6.3% at a mean 1.6 years, and the most common reason for revision surgery was progression to THA. 47
No or mild hip osteoarthritis, labral repair, young age, and limited cartilage damage have been associated with good clinical outcomes, with a progression to THA in 0% to 26% of the cases. 21 A systematic review compared outcomes and rates of progression to THA between surgical hip dislocation and arthroscopy 86 : 7% of the hips were converted to a THA after a maximum follow-up of 12 years in the open group, as compared with 9.5% after 8.1 years in the arthroscopic group, with no statistical difference between them. Byrd and Jones14,15 reported THA progression rates between 0% and 29% at 2 years after hip arthroscopy. Schairer et al 110 used population-level data of State Ambulatory Surgery Databases and State Inpatient Databases for California and Florida from 2005 to 2012 to examine the progression rate of THA within 2 years after hip arthroscopy. They found an overall progression rate of 12.4% within 2 years after hip arthroscopy, with a significant difference between age groups. In patients <40 years old, the progression rate to THA was 3.0%, which is comparable with our findings of a 3.78% progression rate in patients with a mean age of 33.9 years. The rate of THA progression decreased steadily over time from 14.3% in 2005 to 10.3% in 2010. 110
Age seems to be a risk factor for THA progression: patients aged >50 years exhibited a progression rate of about 20%.71,110 This contrasted with the findings of the present systematic review, where age was not significantly associated with a higher rate of THA progression. Differences between our results and the findings of others might be explained by the fact that we included all types of surgical treatment for FAI, instead of focusing on arthroscopic procedures; other potential reasons include the type of data used, the type of analysis conducted (registry vs systematic), and the younger age of the patients in our study.
BMI at baseline was significantly associated with an increase in the rate of THA progression at a mean follow-up of 38 months. These findings confirm previous results, which found that obesity is an independent risk factor for THA progression after hip arthroscopy at a mean follow-up of 2 years. 110 In addition, Gupta et al 43 and Collins et al 24 confirmed, in small case series studies, that obesity is associated with higher rates of THA progression after arthroscopic procedures. Our results showed that BMI was a risk factor for THA progression, regardless of the surgical technique.
We were also able to show that the preoperative acetabular index was significantly associated with an increased rate of progression to THA. So far, no studies showed an association between the preoperative acetabular index and the progression rate to THA. However, high lateral center-edge angles and low acetabular indices, which require more complex surgical techniques for adequate treatment, are associated with higher rates of revision surgery. 59
Furthermore, we found that labral debridement was associated with an increase in the rate of THA revision for the 3 major surgical techniques analyzed in the present investigation. Schilders et al 111 demonstrated superior outcomes after labral repair as compared with labral debridement in 96 patients with a mean follow-up of 2 years. This was confirmed by Larson et al 65 in a case-control study, with better Harris Hip Score, SF-12, and visual analog scale outcomes in the labral repair group. Menge et al 75 compared 79 patients who underwent labral repair and 75 patients who underwent labral debridement at a mean follow-up of 10 years: no difference in clinical outcomes between the techniques was evident. However, when controlling for acetabular microfracture, Menge et al reported that labral debridement was associated with a significantly higher risk of progression to THA, confirming our findings.
This study presents several limitations. Although we have carefully followed recommended guidelines for the preparation of systematic reviews, the overall quality of the studies was low. Most of the studies were retrospective, and eligibility criteria and rehabilitation protocols were not frequently reported. The overall CMS of 64 shows acceptable quality. The mean follow-up of the studies was 30 months, which is longer than most previous studies, but revision and progression rates are likely to increase with long-term follow-up. Given these premises, the risk of biased results is moderate to high; thus, data from the present study must be interpreted with caution. The purpose of the present study was to investigate whether the aforementioned endpoints are associated with the rate of revision and subsequent progression to THA. Thus, every endpoint was investigated independently, and its risk of recurrence in revision and progression to THA was assessed. We did not perform any comparison between endpoints and their overall effect on the surgical outcomes. This may represent a limitation of the present study. However, in the current literature, there is a multitude of studies focusing on several aspects of FAI correction, evaluating and comparing all the endpoints and their effect on the surgical outcomes. Future studies should overcome these limitations, and high-quality investigations with longer follow-up should be performed.
Conclusion
Surgical treatment for FAI leads to satisfactory outcomes. In this systematic review of 99 studies and 9357 procedures, we found an overall revision rate of 5.29% after surgical treatment. After a median follow-up of 30 months, the progression rate to THA was 3.78%. Patients were at higher risk for a subsequent progression to THA if they had a high BMI, a pathologic acetabular index, or labral debridement during correction of FAI. Therefore, we do advocate additional education of this patient population in terms of its expected outcomes and surgical labral repair instead of simple debridement if needed and technically feasible.
Supplemental Material
sj-pdf-1-ajs-10.1177_03635465211011744 – Supplemental material for Revision Surgery and Progression to Total Hip Arthroplasty After Surgical Correction of Femoroacetabular Impingement: A Systematic Review
Supplemental material, sj-pdf-1-ajs-10.1177_03635465211011744 for Revision Surgery and Progression to Total Hip Arthroplasty After Surgical Correction of Femoroacetabular Impingement: A Systematic Review by Filippo Migliorini, Nicola Maffulli, Alice Baroncini, Jörg Eschweiler, Markus Tingart and Marcel Betsch in The American Journal of Sports Medicine
Footnotes
Acknowledgements
The authors thank Michael Berner for his support and motivation during the study conceptualization. They also thank Paolo Aretini, PhD, for his consistent support and motivation during the statistical analyses.
Submitted September 8, 2020; accepted December 22, 2020.
The authors declared that they have no conflicts of interest in the authorship and publication of this contribution. AOSSM checks author disclosures against the Open Payments Database (OPD). AOSSM has not conducted an independent investigation on the OPD and disclaims any liability or responsibility relating thereto.
An online CME course associated with this article is available for 1 AMA PRA Category 1 Credit™ at ![]() . In accordance with the standards of the Accreditation Council for Continuing Medical Education (ACCME), it is the policy of The American Orthopaedic Society for Sports Medicine that authors, editors, and planners disclose to the learners all financial relationships during the past 12 months with any commercial interest (A ‘commercial interest’ is any entity producing, marketing, re-selling, or distributing health care goods or services consumed by, or used on, patients). Any and all disclosures are provided in the online journal CME area which is provided to all participants before they actually take the CME activity. In accordance with AOSSM policy, authors, editors, and planners’ participation in this educational activity will be predicated upon timely submission and review of AOSSM disclosure. Noncompliance will result in an author/editor or planner to be stricken from participating in this CME activity.
. In accordance with the standards of the Accreditation Council for Continuing Medical Education (ACCME), it is the policy of The American Orthopaedic Society for Sports Medicine that authors, editors, and planners disclose to the learners all financial relationships during the past 12 months with any commercial interest (A ‘commercial interest’ is any entity producing, marketing, re-selling, or distributing health care goods or services consumed by, or used on, patients). Any and all disclosures are provided in the online journal CME area which is provided to all participants before they actually take the CME activity. In accordance with AOSSM policy, authors, editors, and planners’ participation in this educational activity will be predicated upon timely submission and review of AOSSM disclosure. Noncompliance will result in an author/editor or planner to be stricken from participating in this CME activity.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
