Abstract
Aim: Trigeminal neuropathies are a group of clinical disorders that involve injury to primary first-order neurons within the trigeminal nerve. We review the spectrum of etiologies underlying both painful and non-painful trigeminal neuropathies, with attention to particularly dangerous processes that may elude the clinician in the absence of a meticulous evaluation. Complications and management issues specific to patients with trigeminal neuropathy are discussed.
Methods: Retrospective literature review.
Results: Facial or intraoral numbness, the hallmark of trigeminal neuropathy, may represent the earliest symptomology of malignancy or autoimmune connective tissue disease as sensory neurons are destroyed. Such numbness, especially if progressive, necessitates periodic evaluation and vigilance even years after presentation if no diagnosis can be made.
Conclusions: In the routine evaluation of patients with facial pain, the clinician will inevitably be confronted with secondary pathology of the trigeminal nerves and nuclei. The appearance of numbness, even when pain continues to be the most pressing complaint, necessitates clinical assessment of the integrity of all aspects of the trigeminal pathways, which may also include neurophysiologic, radiographic, and laboratory evaluation.
Introduction
The trigeminal nerves and nuclei form a complex physio-anatomical network in relationship to the skull base, and various head and neck structures. Pain, while often the earliest and quite often the most pressing symptom, is only one feature of trigeminal disease, which may also include loss of sensation and/or masticatory weakness. Trigeminal neuropathy (TNO) is characterized by numbness in the skin or mucosal membranes in the distribution of the trigeminal nerves, and/or neuropathic weakness in the muscles of mastication. TNO should not be confused with trigeminal neuralgia (TNA), which is characterized by brief attacks of lancinating pain but without sensory impairment or motor weakness. In TNO, pain may dominate the clinical picture early on, but as the disorder underlying it progresses and neurons are destroyed, numbness and weakness usually appear. In untreated idiopathic TNA, neurons are preserved, although their myelin sheaths may be destroyed and there is ultimately gain of function, whereas in TNO as the condition advances, loss of function in the affected nerve branches becomes evident. However, TNA may be due to secondary pathology as well, and the absence of numbness does not exclude secondary pathology, as may be the case with lesions of the trigeminal dorsal root entry zone causing pain (1). When an underlying abnormality is identified in TNA, it is termed by the International Headache Society as ‘symptomatic trigeminal neuralgia’. Although it might be argued that the designation of TNO versus symptomatic TNA may be a function of how early the lesion is detected and the diagnosis is made, it is likely that in some cases of symptomatic facial pain, numbness may never be reported.
Differential diagnosis of trigeminal neuropathy

Pain is very likely to be a feature when sensory loss is associated with nasopharyngeal carcinoma or metastasis (6), although pain may be seen among the entire spectrum of pathogenic mechanisms. In one retrospective series of 76 patients with trigeminal nerve lesions on neuroimaging, the combination of pain and numbness was almost exclusively seen in individuals with peripheral lesions, whereas pain alone as a symptom was evenly distributed among the various possible anatomical localizations (7). Health care professionals who evaluate patients with craniofacial pain should be aware of the appropriate evaluation, diagnosis, and management of secondary disorders involving the trigeminal pathways.
Trigeminal nerve anatomy and function
The largest of the 12 cranial nerves, the trigeminal nerve carries sensory input from the supratentorial dura mater, face, cornea, and nasal, oral, and sinus mucosa (8). The trigeminal nerve has three main branches distal to the trigeminal ganglion: the ophthalmic (V1), maxillary (V2), and mandibular (V3) nerves, the latter of which also carries efferent motor fibers to the muscles of mastication. V1 and V2 both pass through the cavernous sinus. V1 exits the skull through the superior orbital fissure to enter the orbit, and V2 through the foramen rotundum to enter the pterygopalatine fossa (PPF). V3 courses downward from the trigeminal ganglion through the foramen ovale to enter the nasopharyngeal masticator space, where it branches to supply the muscles of mastication, and sensation to the lower lip, chin, tongue, and mandibular teeth.
Understanding the extracranial anatomy is important as the trigeminal nerves are recognized as physical conduits of both neoplastic and infectious processes centrally, and TNO often results from peripheral pathology (9–12). The PPF is the hub of many important connections and is easily identified radiographically on axial imaging by its location posterior to the maxillary sinus and anterior to the pterygoid process of the sphenoid bone. The PPF is normally hyperintense on T1-weighted MRI images because of high fat content. The PPF is in communication with the masticator space via the pterygomaxillary fissure, with the orbit through the infraorbital fissure, the nasal cavity by the sphenopalatine foramen, oral cavity through the palatine foramina, and the middle cranial fossa via the foramen rotundum as described above (13). The masticator space is medial to the PPF and most easily identified radiographically on coronal MRI as the fascial space enclosing the muscles of mastication: masseter, medial and lateral pterygoids, and temporalis.
In the brainstem, cranial nerve V has three sensory nuclei: a principle sensory nucleus, which mediates tactile sensation, a spinal trigeminal nucleus mediating pain and temperature, and a mesencephalic nucleus, which contains unipolar first-order ganglionic cells, which receive proprioceptive input from V3. A fourth, motor nucleus lies medially to the principle sensory nucleus in the mid-pons. The spinal trigeminal nucleus (STN) extends from the pontomedullary junction into the dorsal upper cervical spinal cord, providing an anatomical substrate for ipsilateral facial pain and/or numbness following cervical spine insult (14). The STN is composed of three subnuclei: oralis, interpolaris, and caudalis, the latter of which is thought to be the most critical with regards to processing of nociceptive information.
Finally, the trigeminal nerves serve as neural scaffolds in the transmission of smaller autonomic fibers to their ultimate destinations. The lacrimal nerve (V1) travels laterally in the orbit to the lacrimal gland, after receiving post-ganglionic parasympathetic fibers transmitted by the zygomaticotemporal nerve (V2), which originated from the pterygopalatine ganglion. The nasociliary nerve (V1) serves as a conduit for sympathetic fibers originating in the superior cervical ganglion. Autonomic involvement manifesting as a Horner’s syndrome may rarely be seen in TNO (6). Several branches of V2, including the palatine nerves, serve as conduits to transmit postganglionic parasympathetic fibers from the pterygopalatine ganglion to the hard and soft palates, nasal cavity, and lacrimal gland, as mentioned above. The auriculotemporal nerve (V3) carries postganglionic fibers to the parotid gland.
Detection of trigeminal neuropathy
In the routine evaluation of a patient with facial pain or headache, the clinical history provides valuable insight into an underlying pathological trigeminal process (Figure 1). In addition to pain, the examiner should inquire about symptoms of hypo- or complete anesthesia, dry eyes, diminished taste, and weakness or difficulty with chewing. The latter complaint should be interpreted with caution, as subjective difficulty with chewing may reflect pure sensory loss independently of any motor deficit (15). A history of conductive hearing loss and serous otitis media may reflect Eustachian tube dysfunction from weakness of the tensor veli palatini muscle, which is innervated by the medial pterygoid nerve, a branch of mandibular nerve (V3). Cold temperature (e.g. cool wind) may trigger episodic visual blurring from corneal edema in the eye ipsilateral to an underlying TNO (16).
Diagnostic approach to trigeminal neuropathy. The diagnostic evaluation of a patient with trigeminal neuropathy (TNO) may require a diverse array of testing, which should be guided by the clinical history and examination. In our opinion, all patients with TNO should, at the minimum, undergo MRI imaging of the head, with attention to the course of the trigeminal nerves, in addition to basic laboratory evaluation, including antibody markers of connective tissue disease. If clinically suspected, the physician should obtain a formal lip biopsy to pursue a diagnosis of Sjögren's syndrome. Finally, a patient in whom no etiology can be identified requires ongoing surveillance for the development of malignancy or connective tissue disease. Abbreviations: CT: computerized tomography, MRI: magnetic resonance imaging.
The physical exam in a patient with facial pain and/or numbness should include a comprehensive neurological evaluation, in addition to inspection of the ear, nose, and throat structures, and a cerebrovascular examination (17). Visual inspection or manual palpation may reveal atrophy of the temporalis and/or masseter muscles. Distal V3 lesions may only cause atrophy in muscles innervated by the mylohyoid nerve, namely the mylohyoid muscle and the anterior belly of the digastric. Accidental tongue bites, dental caries, erosion of the ala nasi, and cutaneous or mucosal ulcers may represent accidental injury and long-standing sequelae of trigeminal sensory neuropathy. Movement of the jaw during the interview should be observed for symmetry, as the jaw will deviate towards the side of a weakened pterygoid muscle (17). Oral breathing may dominate in patients with jaw-drop, and lead to drying of the mouth and thickening of secretions (18). A limited ability to open the mouth fully may be seen in patients with malignancies involving the masticator space (7). Jaw protrusion and deviation may be triggered by eye blinking in patients with rostral brainstem or bilateral cerebral disease (so-called palpebromandibular synkinesia) (19).
The sensory exam in TNO may reveal partial or complete sensory loss, or occasionally allodynia and hyperalgesia. Allodynia and hyperalgesia may also be observed in TNA and this aspect of the clinical exam may have a limited utility in distinguishing the two disorders, unless it reveals cutaneous or intraoral trigger for pain, which would increase the likelihood of TNA. The predictive value of clinical neurosensory testing has some limitations and may depend on when it is carried out and which nerve is being evaluated (20–22). For example, following inferior alveolar nerve injury (V3), clinical sensory testing is frequently normal at 3 months, whereas neurophysiological testing, including tactile and thermal quantitative sensory testing can detect alterations at 1 year (23). Remarkably, at 1 year, clinical sensory testing has a false negative rate up to 94% (23). Not only may clinical localization be unreliable with focal pathology (24), but trigeminal dysfunction may also be falsely localizing, as it has been noted to occur in the setting of intracranial hypertension (25). Therefore, when a lesion is suspected, neuroimaging is crucial.
The examiner should be cognizant of the possibility of a central neurological process mimicking a TNO. The finding of dissociated sensory loss between pain and fine touch may have limited utility in distinguishing principle sensory nucleus (pontine) versus spinal trigeminal nucleus (medullary) lesions (24). Further, impaired intra-oral with relative preservation of facial sensory fields may be seen with rostral spinal trigeminal nucleus lesions (26). A careful sensory exam, including the distal extremities, may detect a subtle cheiro-oral syndrome in a patient presenting with peri-oral sensory symptoms and direct the examiner to consider a central localization.
Several reflex tests involving the trigeminal nerve may be helpful in localizing a potential lesion. The masseteric T reflex, also called the ‘jaw jerk’ reflex, allows assessment of afferent neurons of the trigeminal mesencephalic nucleus, in series with the ipsilateral efferent arc through the pontine trigeminal motor nucleus. A hyperactive jaw jerk may reflect pathology rostral to the level of the trigeminal motor nucleus. Further, as assessed by electromyography (EMG), a latency difference greater than 1 ms between left and right-hand sides may reflect a lesion along the reflex arc, but may also be seen in patients with craniomandibular dysfunction (27).
The blink reflex (BR) is a cutaneous trigeminofacial reflex during which bilateral eyelid closure occurs in response to cutaneous stimulation of the face (28). EMG of the orbicularis oculi muscle can be used to characterize the BR in response to electrical stimulation of the skin. A subclinical ipsilateral response of short duration is detected early following stimulation (R1), followed by a late bilateral response which is more prolonged, and corresponds to the clinical blink (R2). A third ultralate component (R3) may be seen with high-intensity stimuli. R1 is most sensitive in detecting extra-axial lesions in either the afferent trigeminal or efferent facial nerve pathway, in addition to pontine pathology. R2 depends on polysynaptic bulbar pathways in the pons and medulla, habituates to repetitive stimulation, and is modulated by higher-order input. Isolated abnormalities in R2 may be seen in lateral medullary syndromes.
A corneal reflex (CR) may be assessed at the bedside by having the patient look away while the cornea is touched from the side by a moist cotton tip, or a drop of fluid or blown air released from a syringe. The reflex may be misinterpreted if the patient is blinking to threat if the direction of gaze is on the oncoming stimulus. In contrast to the BR, the CR differs in that it is more purely mediated by nociceptive fibers, and has only a bilateral component analogous in morphology and latency to R2 (28). Caution should be observed in carrying out the CR in patients with suspected Creutzfeld-Jakob disease, AIDS, or herpetic keratitis (17). Additional variants of the above reflexes include the glabellar, corneomandibular, and the peri-oral reflexes.
While the patient should always be given the benefit of the doubt, knowledge of the caveats of the sensory dermatomes may clue the examiner in to a functional examination. For example, documentation of abnormalities on pinprick over the angle of the jaw, lobule of the ear, and mastoid region (greater auricular nerve, C2) may be useful in this regard. In patients with sensory deficits extending outside of the trigeminal distribution, a multi-focal process in addition to the possibility of a non-organic pathophysiology should be considered. Further, while patients may be able to suppress pain behavior with corneal stimulation, this is extremely difficult with unexpected noxious stimulation of the nasal mucosa with a cotton tip.
To be optimal, a radiographic evaluation of TNO should include visualization of the complete trajectory of the trigeminal nerves from the brainstem and roots, through the gasserian ganglion, cavernous sinus, skull base, and along the extra-cranial pathways (Figure 2). MRI with and without gadolinium contrast with attention to the skull base, and extension to the upper cervical spinal cord is generally the imaging modality of choice, although different sequences may be used to tailor the inspection of the different trigeminal segments (29). Computerized tomography (CT) imaging has an important role in the assessment of peripheral nerve segments, especially in the context of trauma, and in characterizing lesions with involvement of skull base foramina. In a review of 17 patients with enhancing trigeminal nerve lesions, smoothly contoured, minimally enhancing lesions suggested a benign etiology, whereas enlarged, irregular margins was associated with malignancy (30). However, overlap of imaging findings was seen, cautioning against an over-reliance on radiographic features. In addition to inspection of neural elements, neuroimaging allows for a radiographic assessment of masticatory muscle bulk, some of which is not accessible by the clinical exam.
Clinical and radiographic findings in trigeminal neuropathy. (A) Coronal T1-weighted gadolinium bolus MRI, demonstrating abnormal right trigeminal nerve enhancement (arrow) in a patient with an eventual diagnosis of idiopathic TNO. (B) Axial T1-weighted gadolinium bolus MRI, showing a typical appearing trigeminal schwannoma (arrow) at the left trigeminal ganglion. (C) Advanced findings of skin fibrosis in a 43-year-old woman with trigeminal neuropathy secondary to scleroderma. (D) Axial gradient spin echo MRI demonstrating hemorrhage into the dorsal root entry zone and cisternal segment of the left trigeminal nerve (arrow). (E) Axial T2-weighted MRI of the cervical spine in a patient with syringomyelia extending into the upper cervical segments (arrow) whose presentation included TNO. (F) Perineural extension of squamous cell cancer into the right cavernous sinus (arrow) is seen on this T1-weighted gadolinium MRI. (G) Coronal CT of the face revealing metastatic small cell lung cancer to the angle of the mandible in a patient who presented with jaw numbness.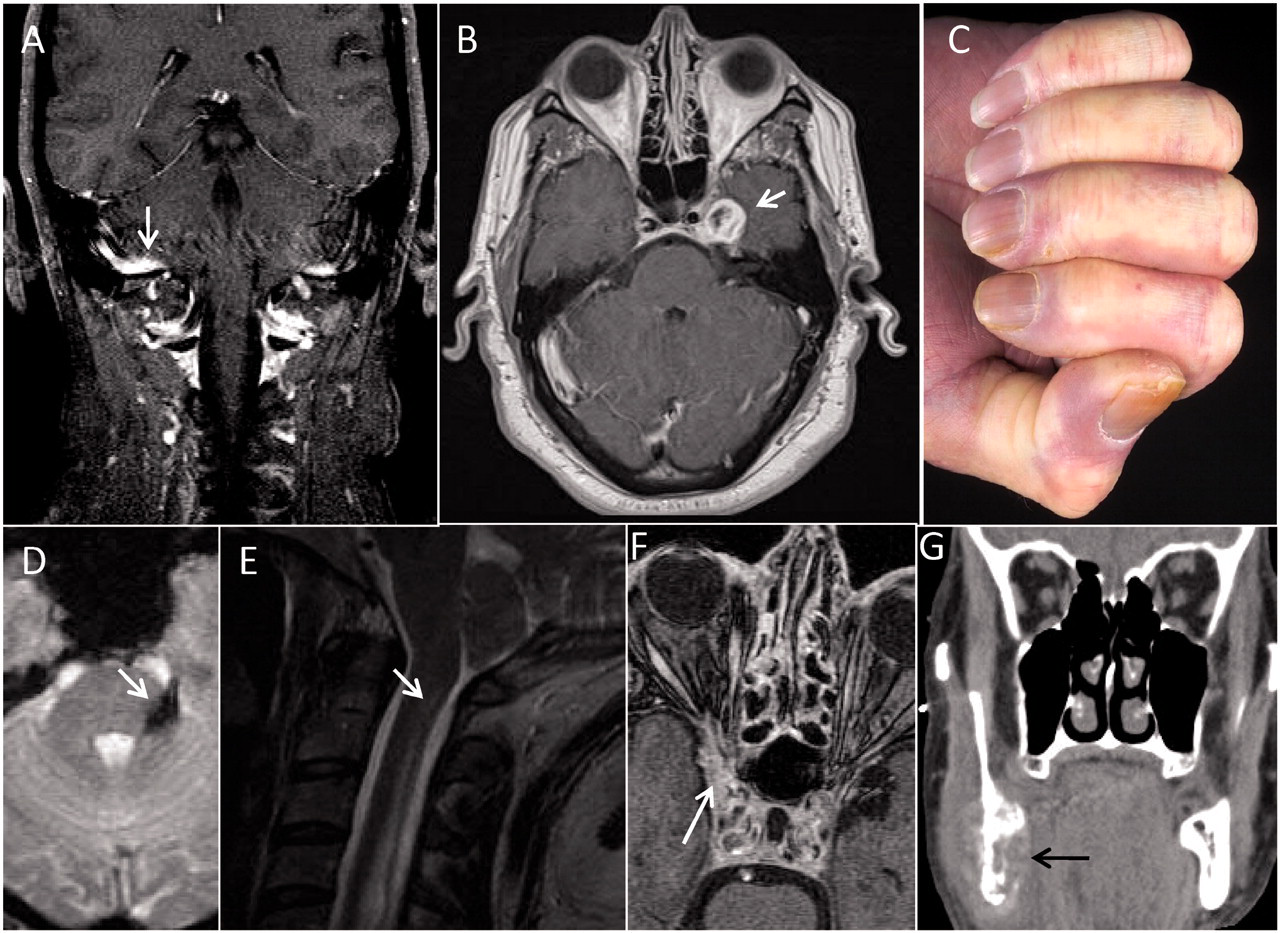
Laboratory evaluation in individuals with TNO should be tailored to the individual circumstance, but may include measurement of the complete blood count, erythrocyte sedimentation rate, lyme and syphilis serology, antibodies to extractable nuclear antigens including SS-A and SS-B, in addition to other autoimmune markers of connective tissue disease. If Sjögren's syndrome is suspected, then salivary gland (lip) biopsy is warranted.
Etiologies by pathophysiological process
Traumatic
Trauma is thought to be the most common mechanism leading to TNO, and may be either accidental or iatrogenic (3,31,32). The inferior alveolar and lingual nerves are particularly susceptible to injury in the context of oral surgery, especially if the lower third molar is involved (22,32,33). In a review of 1377 mandibular molar extractions, 60 patients were identified with either dysesthesias or paresthesias (34). In 14 of these instances the deficits were ongoing at the time of publication (>6 months), while in 64% complete resolution occurred within 6 months (34). In a survey of 226 individuals who had received compensation because of trigeminal nerve damage (78.6% after third molar removal), paresthesia was the most commonly reported symptom (70%), with at least 20% reporting pain in the affected region (35). Respondents with sensory deficits in the lower lip and tongue frequently self-reported difficulties with speech, eating, and tongue-biting. These sequelae underlie why numbness in the trigeminal distribution is often more distressing than similar symptoms involving spinal dermatomes (2).
The trigeminal ganglion and its divisions may be damaged in the context of both blunt closed and penetrating head injuries (31). In a series of 66 such cases, extracranial injury to the maxillary division by blunt trauma was the most common mechanism of TNO (31). Basilar skull fracture may manifest with isolated complete sensorimotor TNO (36), isolated trigeminal motor neuropathy (37), and transient bilateral TNO with complete jaw-drop (38).
Other rarer etiologies of traumatic TNO include denture trauma at the mental foramen (3), anterior superior alveolar injury from repetitive trumpet playing (39), following laser in situ keratomileusis (40), and sialolithiasis leading to lingual nerve compression (41). In this latter report, episodic hemilingual numbness was seen in association with submandibular swelling and salivation.
Neoplastic
Trigeminal neuropathy may be the presenting manifestation of malignancy, by several distinct mechanisms, including compression at intra- or extra-cranial portions of the nerve, peri-neural spread, or metastasis. The clinical presentation does not seem to reliably differentiate benign and malignant processes. An exception to this includes the ‘numb chin' sign of mental neuropathy, which is considered a life-threatening sign due to the frequent association with breast, lung, and lymphoproliferative malignancies (42). Malignant mental neuropathy is associated with a mortality in excess of 78% (42).
Intracranial involvement of the trigeminal pathways by tumor may occur at various anatomical levels including the brainstem, prepontine cistern, cerebellopontine angle (CPA), trigeminal ganglion, and cavernous sinus. When brainstem tumors cause TNO, it almost always occurs in association with other neurological signs and symptoms, although a single patient with isolated facial numbness who was later found to have a primary brainstem lymphoma has been reported (43). Notably, this patient was initially dismissed as having an ‘idiopathic trigeminal neuropathy' after a plain head CT was read as normal, but then later re-presented with multiple cranial neuropathies. Carcinomatous leptomeningitis, which most commonly occurs with lung cancer, breast cancer, lymphoma, and melanoma, affects cranial nerves in 80% of patients at presentation (44). Headache was the chief complaint in 19/50 patients in one retrospective series, and clinical exam revealed evidence for TNO in 6/50 at presentation (44).
CPA masses include acoustic and trigeminal schwannomas, meningiomas, epidermoid cysts, and cholesteatomas. Lesions at this anatomical level may involve the trigeminal nerve in isolation or in combination with nearby cranial nerves. Among a cohort of 40 patients with CPA meningiomas managed surgically, TNO was seen in six (16.2%) at presentation, with an additional six patients developing TNO post-operatively (45). Radiosurgery for vestibular schwannoma is implicated in the delayed development of TNO at a median time of 5 months (46). Involvement of the cavernous sinus can manifest as TNO with or without additional cranial nerve involvement as a consequence of tumor extension, from meningioma, or metastatic disease, typically from breast, lung, or melanoma (47).
Trigeminal schwannomas, benign and malignant, often arise from the region of the trigeminal ganglion (2). One-half arise in the middle cranial fossa, one-fourth in the posterior fossa, and the remaining one-quarter involve both. The most common clinical presentation of a trigeminal schwannoma is with facial numbness and paresthesias, but both painful neuralgia and dysesthetic pain may also be seen. The tumors have a tendency to adhere to the dura, and may erode into the floor of the middle or posterior fossa. Gangliocytoma is another malignant tumor which can arise from the trigeminal ganglion. However, neoplastic disease at the level of Meckel's cave, the dura covered impression of the apical petrous portion of the temporal bone which contains the trigeminal ganglion, is more commonly due to meningioma or schwannoma. Amyloidoma of the trigeminal ganglion and trigeminal nerves may radiographically mimic schwannoma, and is an important diagnostic consideration (48). The reasons why amyloid light-chain lambda deposition has a predilection for the trigeminal nerves are not known.
Nasopharyngeal carcinoma (NPC) may spread by many distinct mechanisms and result in trigeminal dysfunction at several anatomical foci. The tumor frequently arises in the lateral wall of the nasopharynx, but growth is directed rostrally because of the dense pharyngobasilar fascia, which circumscribes the posterolateral nasopharynx (49,50). The undersurface of the sphenoid is not protected by fascia, and may be invaded by this tumor. Alternatively, the foramen lacerum and petrooccipital fissure may allow extension into the middle or posterior fossae. NPC may encounter branches of the trigeminal nerve following lateral extension over the pharyngobasilar fascia into the masticator space, or following spread through the sphenopalatine foramen into the pterygopalatine fossa (50). A propensity for perineural spread has been appreciated with this tumor, a mechanism by which it may track through the cavernous sinus (49).
Perineural spread, however, is most commonly due to adenoid cystic carcinomas and dermatological malignancy in the head and neck, and more rarely by lymphoproliferative disease (50–52). Pain and paresthesias are common presenting symptoms in patient with perineural spread of their tumor (51). In individuals with a prior history of malignancy thought to be in remission, TNO may represent a sign of tumor recurrence (51). The auriculotemporal nerve (V3) may allow the transmission of parotid malignancy to the cavernous sinus through the foramen ovale (12). Likewise, tumors originating from the palate or in the sinuses may spread along V2 to reach the pterygopalatine fossa and then pass through the foramen rotundum (11). The palatine nerves (V2) are often involved because of the high-density of minor salivary glands in the hard palate, and the propensity of adenoid cystic carcinoma to track along nerves (50). Although the directionality of spread is typically retrograde, anterograde spread may also occur, such that a tumor of the hard palate may reach the trigeminal ganglion and then spread to the masticator space, for example (50).
Metastatic disease may also localize to the skull base, where orbital, parasellar, and trigeminal ganglion syndromes can occur with symptoms of facial pain and numbness (53). In a review of 43 patients with skull base metastasis, 15 had lesions in the middle cranial fossa at the trigeminal ganglion or branches as the predominant manifestation (53). Painless numbness in V2/V3 spreading from the midline laterally to the anterior ear was the most common presentation, although masticatory weakness and atypical facial pain were also seen. CT imaging of the skull base was normal in three patients with known primary malignancies, who improved with radiation therapy. An unusual case of jaw-drop as the isolated manifestation of bilateral TNO from metastatic lung cancer has been reported (54).
Vascular
Vascular hemorrhage or ischemia of the brainstem may underlie an acute onset of facial numbness. Pontine hemorrhages may mimic TNO in isolation or in combination with other neurological deficits, and are most commonly sequelae of hypertension, or more rarely vascular malformation (55,56). Acute pontine ischemia at the trigeminal dorsal root entry zone may result in facial numbness and trigeminal neuralgiform pain (57). Patients with ventral pontine infarcts can present with ipsilateral mid-face sensory signs, in association with dysarthria, and contralateral hemiparesis (8,58). The anatomy of midfacial sensory loss has been attributed to involvement of the dorsal trigeminothalamic tract (8). Kim et al. have reviewed 50 cases of dorsolateral medullary ischemia with sensory abnormalities and found the ipsilateral face-contralateral body pattern of sensory loss to be present in only 26% (24). Isolated ipsilateral trigeminal loss was seen in 8%.
Vascular malformations have been reported to cause TNO, including cavernous hemangioma at Meckel's cave (43). Cavernous hemangiomas may occur along the entire course of the trigeminal nerve, including extension extra-cranially (59). Whereas involvement of V1 and V2 would be expected in cavernous sinus syndromes, involvement of V3 may also rarely occur in the setting of non-traumatic cavernous fistula (60). The mechanism is thought to be related to engorgement of the inferior petrosal sinus, and vascular compression at the foramen ovale.
Inflammatory/autoimmune
Sensory trigeminal neuropathy is a well accepted complication of autoimmune connective tissue and inflammatory disease (15,61–66). Undifferentiated and mixed connective tissue diseases are most commonly associated with TNO, followed by scleroderma (62). Sjögren's syndrome is another condition classically associated with TNO (66). Motor involvement is almost never a feature, all three trigeminal distributions may be involved, and the presentation may be either unilateral or bilateral (61,63). Neuropathic or neuralgiform pain may be present. The finding of trigeminal sensory neuropathy in the context of a connective tissue disease is generally not considered an indication by itself for the initiation of immunosuppression (63). When prednisone is given for TNO in the setting of a connective tissue disorder, symptomatic improvement is rare (62,66).
In a retrospective review of 442 consecutive patients with progressive systemic sclerosis (PSS), TNO was identified in 16 (4%) (61). TNO may be present as an isolated feature of PSS, preceding the onset of other symptoms by 1–6 months. In patients with both TNO and PSS, myositis and elevated anti-ribonucleoprotein antibodies in high titers are a disproportionately frequent finding. Of 41 patients reviewed with PSS and TNO, pain and/or paresthesias was present in 25 (61%), with three patients experiencing lancinating pain and nine patients reporting trigger points in the face or with chewing (61). Numbness and pain are most often reported as evolving over the course of months (15), but acute presentations have also been described, suggesting multiple pathogenic mechanisms (67). Raynaud's phenomenon involving the tongue is an unusual etiology of paroxysmal sensory symptoms of the face in PSS (68). Further, bony mandibular resorption is a known complication of PSS, and has been reported to result in painful compression neuropathy of the inferior alveolar nerve (69).
Mori et al. have reported in detail a series of 92 individuals with Sjögren's syndrome-associated neuropathy, 15 of whom had isolated TNO, and three had multiple cranial neuropathies, including involvement of the trigeminal nerve (66). In 93% of the total patients, the neuropathy preceded a diagnosis of Sjögren's, highlighting the need for ongoing surveillance in patients carrying a diagnosis of TNO. Among the subgroup with TNO, pain was present in only 2/15 (13%), the progression was often chronic, and an association with autonomic features, including pupillary abnormalities, orthostatic hypotension, and hypohidrosis, was noted (66). Three patients with TNO were treated with steroids, only one of whom had definite objective and subjective improvement. A lack of improvement of TNO in Sjögren's with immunosuppression has also been reported by other authors (70).
Multiple sclerosis may be a relatively common cause of facial pain and/or numbness (5). Although brainstem lesions are thought to be common in multiple sclerosis (MS), isolated cranial nerve palsies are more unusual, occurring in one large series in 10.4% of patients (71). The trigeminal nerve was the most frequently involved nerve. Trigeminal sensory neuropathy was more common than trigeminal neuralgia, and V2/V3 were most commonly affected. Of the cases observed, the majority occurred at the time of disease presentation, with the remainder occurring in the context of relapses.
Neurosarcoidosis most commonly manifests as granulomatous inflammation of the basilar meninges, occasionally extending rostrally into the hypothalamus and pituitary. Facial nerve palsy is the most common manifestation; however, TNO has been reported as a rare, sometimes isolated manifestation (72). Radiographically, neurosarcoid involvement of the trigeminal nerve and/or trigeminal ganglion may mimic more common mass lesions, such as schwannoma.
Neurophysiological studies in patients with chronic inflammatory demyelinating polyneuropathy indicate that more than half the patients have evidence for trigeminal sensory neuropathy, although this is mostly subclinical (73). Likewise, lingual neuropathy may be the initial sign of Guillain-Barré syndrome (74). Cogan's syndrome was observed in a single case report to present with multiple cranial nerve involvement, including bilateral trigeminal neuropathies (75).
Infectious
Infection is not thought of as a common mechanism for TNO, although worldwide leprosy continues to be an important etiology of cranial neuropathy, particularly of the facial and trigeminal nerves (76,77). Cranial nerve involvement seems to occur most commonly in lepromatous leprosy of longer duration, although it may occur in any subtype, and may be the presenting feature of leprosy (77). Involvement of the maxillary division occurs most frequently (76).
Herpes simplex virus has been implicated in many cases of presumed idiopathic Bell's Palsy, which is typically thought of as an acute, peripheral seventh nerve palsy. However, additional cranial nerve involvement may be seen, including ipsilateral TNO in up to 25% of patients (78). Further, transient sensory TNO may occur concurrently with ipsilateral herpes simplex labialis infection (79).
The varicella zoster virus may be reactivated from a dormant state in the sensory ganglia. This is manifest in the clinical syndrome known as ‘shingles’ with a painful, vesicular rash in the trigeminal distribution, most commonly V1. In rare cases, zoster may be associated with peripheral facial palsy and a vesicular rash in the ear (so-called Ramsay-Hunt syndrome). MRI lesions in the spinal trigeminal nucleus and tract may be seen, suggesting a pathway across the brainstem from the fifth to seventh cranial nerves (80). Post-herpetic neuralgia may develop, which is characterized by pan-modality sensory loss and allodynia in the distribution of a prior zoster attack (81). The incidence of postherpetic neuralgia is estimated to anywhere from 9% to 14% (82), although at 1 year only 3 out of 100 patients with zoster were found to have persistent severe pain (82). The risk of postherpetic neuralgia increases with age, with approximately 75% of patients at age of 70 being affected at 1 month following the initial attack (82).
Lyme disease, caused by the tick born spirochete Borrelia burgdorferi, has been reported to manifest with TNO (83). Trigeminal nerve enhancement may be seen on MRI with gadolinium contrast administration, a finding which may not have an overt clinical correlate (83,84). Neurosyphillis may also be included in the differential diagnosis of TNO, and may mimic a tumor involving the trigeminal ganglion (85,86). Remarkably, TNO has been seen as the isolated manifestation of a 1.5-cm by 1.5-cm pontine abscess (87).
Fungi, including granulomata of actinomycosis and aspergillus, may present as mass lesions at the trigeminal ganglion (9,88,89). Mucormycosis may be transmitted centrally by perineural spread along the trigeminal nerves (10).
Degenerative
Kennedy's disease, or spinal-bulbar muscular atrophy, is an X-linked degenerative sensorimotor neuronopathy, associated with signs of androgen insensitivity. Either jaw-drop or isolated jaw-closure weakness may be a presenting feature (90). Sensory loss is considered minimal in this disorder, although neurophysiological assessment has disclosed abnormal trigeminal reflexes consistent with a ganglionopathy (91).
A new syndrome, facial onset sensory and motor neuropathy (FOSMN), has been described in four male patients with a mean age of onset of 43 who all presented with trigeminal distribution sensory symptoms, and evolved to more generalized sensory, and then motor symptoms (92). Neurophysiological and pathological studies were consistent with a neurodegenerative sensorimotor neuronopathy.
Toxic/metabolic
Trichloroethylene toxicity has been reported in the context of both general anesthesia and industrial exposure (degreasing solvent) to result in TNO progressing over hours to days. Other cranial nerves may be involved, and recovery may be incomplete (2,93). Hydroxystilbamidine isethionate treatment of trigeminal neuralgia induced bilateral TNO in 7/61 total TNO cases reviewed from the Mayo Clinic (3). The predominant symptom in these patients was troubling and difficult to treat facial paresthesias. Chemotherapy treatment with oxaliplatin may be complicated by both sensory neuropathy and acute neurosensory toxicity (94). This latter syndrome is reversible and may present with painful peri-oral dysesthesias, jaw pain, and ear pain. Unilateral TNO in combination with peripheral facial weakness has been reported following the spider bite of Loxosceles rufescens (95).
In a study of trigeminal-facial and trigeminal-trigeminal reflexes in patients with severe axonal diabetic polyneuropathy, neurophysiological abnormalities were seen in 13/23 patients, only five of whom were symptomatic (73). These studies were normal in patients with mild diabetic polyneuropathy. Bilateral corneal anesthesia with erosions has been reported in a 27-year-old woman with diabetes, which was interpreted as a presenting feature of diabetic neuropathy (96).
Congenital
Congenital skull base anomalies and/or inherited bone disease may also manifest with either symptomatic trigeminal neuralgia or TNO. Chiari malformation, cranial osteodysplasia, achondroplasia, and osteogenesis imperfecta have been reported in this regard, in association with stretching of the nerve roots, and/or deformity of the posterior fossa (97–101). Basilar impression is the most common craniocervical deformity, which typically manifests with occipital headache, but trigeminal symptoms may be seen in excess of 50% of cases (97).
Another congenital cause of facial numbness is congenital trigeminal anesthesia (CTA). CTA may be classified into three subgroups: (a) isolated, typically bilateral numbness limited to the ophthalmic distribution, (b) CTA associated with mesenchymal or ectodermal defects, or (c) CTA associated with additional bulbar deficits (102). Based on a very limited amount of pathological data, it is thought that primary neural hypoplasia of bulbar nuclei may underlie the trigeminal anesthesia in many cases, particularly group (a) (102).
Idiopathic
In the evaluation of a patient with a pure trigeminal sensory syndrome, in which no underlying process can be identified, a diagnosis of idiopathic trigeminal sensory neuropathy can be ascribed (2). In a review of 61 cases of TNO at the Mayo Clinic, seven cases were considered to be idiopathic, despite an extensive evaluation (3). Patients with this disorder have involvement of one or more divisions of the trigeminal nerve, with symptoms often persisting anywhere from several weeks to years (2). Motor involvement with muscle wasting may rarely be seen in idiopathic TNO (103). The symptoms may occur unilaterally, bilaterally, and in one patient have occurred on both sides in a sequential manner (104). Despite considerable overlap, acute and chronic idiopathic subtypes are distinguished (6,15,67). In Blau et al.'s series of 10 patients with pure sensory TNO, none of the patients reported facial pain, and half recovered completely over a time range of 2 weeks to 9 months (67). Peñarrocha et al. have described burning pain in association with both acute and chronic forms (33). The pathogenesis is unknown, but some authors have speculated that either a viral or autoimmune etiology may be present (15,105).
Complications and management of trigeminal neuropathy
Pain
Chronic trigeminal pain is perhaps the most immediately troubling symptom to many patients. In TNO, the pain may involve any of the three divisions and may be either unilateral or bilateral. With time, numbness within trigeminal territory develops and for years may co-exist with pain. Further, in chronic TNO developing over 12–24 months, pain can spread and may no longer be localized strictly in the territory of a single trigeminal nerve branch. Treatment of pain in TNO is guided largely by the available scientific evidence for treatment of general neuropathic pain, as well as neuralgia-like pain (82). The nature and management of pain in these two conditions is quite distinct. Neuralgiform pain, as exemplified by trigeminal neuralgia, is brief, shock-like, and may be triggered by non-painful stimuli. Neuropathic pain, more characteristic of post-herpetic neuralgia, is frequently accompanied by allodynia, dysesthesia, and hyperesthesia. Neuropathic pain is more constant, without pain-free intervals, and is often burning in quality. For many years, amitriptyline in doses of 50–150 mg per day and gabapentin (1200–3600 mg per day) were the standard therapy for postherpetic neuralgia; however, more recently trials have demonstrated efficacy for duloxetine HCl (60–120 mg per day) and pregabalin (300–600 mg per day). Carbamazepine (400 to 800 mg per day) has traditionally been the treatment of choice in trigeminal neuralgia, whereas both amitriptyline and opioids are often ineffective (82). Surgery may play a dominant role in medication refractory trigeminal neuralgia, whereas it has no accepted role in the management of postherpetic neuralgia or in TNO. Watson has recommended treating patients with TNO and pain with these above strategies based on the characteristics of their pain as predominantly neuralgiform or neuropathic (82). For neuropathic pain, pregabalin or gabapentin may be considered second line agents, followed by opioids, phenytoin, and topical agents, such as lidocaine and capsaicin. Baclofen and phenytoin may be used individually or as add-on agents to carbamazepine in the treatment of neuralgiform pain.
Numbness
Intraoral numbness is a particular troubling complication of TNO because of the inherent difficulties it causes in eating, management of saliva, and the problems associated with trauma to denervated tongue and buccal mucosa. Unfortunately, there is no treatment for numbness as it implies dead or at least profoundly injured primary afferent neurons.
Neurotrophic keratitis
Neurotrophic keratitis (NK) is a degenerative corneal disease that may rarely develop in the setting of trigeminal deafferentiation from the cornea (106). NK is not specific for TNO, and may occur as a result of diverse pathology, including herpetic keratitis, following repeated corneal surgery, anesthetic abuse, and chemical burns (107). The condition is difficult to manage, and may lead to ulceration and perforation of the cornea. Treatment of NK is guided by the stage of the disease, and is oriented at preventing further progression of corneal damage, and promoting healing (106). Concurrent use of topical medications, systemic medications, such as neuroleptics and antihistamines, and other ocular surface diseases may further worsen the progression of the disease (106). Frequent eye exams, and regular application of preservative-free artificial tears for corneal protection are critical in optimizing treatment success the prevention of visual loss.
Trigeminal trophic syndrome
Trigeminal trophic syndrome (TTS) is rarely seen as a result of compulsive self-manipulation following TNO (6,108). The classical clinical manifestations include anesthesia, facial paresthesias, and secondary persistent or recurrent facial ulcerations. The skin lesions are most commonly unilateral, crescent-shaped, and involve the ala nasi. However, 13% of lesions may occur at sites other than the nose, including the forehead, palate, and ear (109). For unknown reasons, the latency from onset of TNO to the development of erosions or ulcers is highly variable, and the presentation of TTS may be delayed by years (110). Patients may be unaware of the pathological behavior (109). Midface dermatological neoplasia, infectious, and autoimmune conditions should be considered in the differential diagnosis (108). Conservative treatment measures include psychological counselling, prophylactic mechanical interventions (e.g. gloves), and appropriate wound care to prevent superimposed infection. Pharmacological trials are appropriate with agents such as amitriptyline and gabapentin, although treatment with carbamazepine is regarded as the first line medication option (108). Psychotropic medications targeting the compulsive behavior may be warranted. Benefit has also been reported with transcutaneous electric stimulation and cervical sympathectomy to promote healing (108,111,112).
Miscellaneous
Other management considerations include screening for dental caries, for injury to insensate skin and mucosal membranes, and for malnutrition in the setting of severely impaired taste and/or masticatory strength. If facial synkinesias are identified, these can be managed with biofeedback retraining exercises, or selective chemodenervation with botulinum toxin type A may be necessary (113). Cold-induced corneal edema and visual blurring can be prevented by simple provision of contact lenses (114). Psychiatric co-morbidity may be present, commonly in the form of depression, and may represent an additional important component of patient management.
Conclusions
Trigeminal neuropathy most commonly manifests as numbness in the face or mucous membranes, sometimes in association with masticatory weakness, paresthesias, and/or pain. Although many patients may be eventually labeled as having idiopathic TNO, the diverse and potentially life-threatening etiologies that may underlie TNO demand a complete evaluation. A patient labeled as having idiopathic TNO deserves a high index of suspicion for missed diagnoses, which may only reveal themselves with time. Treatment should be aimed at targeting the underlying pathophysiology, if identified, and treatment of complications, which may be uncomfortable, disabling, or potentially life-threatening to the patient.
Footnotes
Funding
This research received no specific grant from any funding agency in the public, commercial, or not-for-profit sectors.
Conflict of interest
None declared.
