Abstract
Communication applications offer healthcare professionals a simple, instantaneous and direct form of connection within a healthcare team. This cross-sectional survey aimed to examine current usage patterns among Australian medical practitioners and assess their understanding of data security and ethical considerations. Among 151 respondents, most of whom were anaesthetists (77%) practising in metropolitan centres (82%) across South Australia, Queensland, and New South Wales, the Apple iPhone was the most popular device type (77%) while WhatsApp was the preferred application for facilitating patient-based discussions (75%). Doctors sent an average of one to 10 patient-related messages per week, although junior doctors were significantly more likely to exceed this number. The majority (66%) of doctors felt comfortable sharing non-identifying patient information, in comparison to 32% who felt comfortable sharing identifying patient information. Participants demonstrated inconsistent understanding of consent and documentation requirements when transmitting patient data. These findings highlight the routine use of communication applications in Australian hospitals and emphasise the need for greater clinician education on privacy obligations and the development of clear, ethical guidelines for their use in healthcare.
Introduction
The delivery of safe and high-quality patient care is incumbent on effective communication between medical professionals.1–3 For many years, hospitals have relied on the traditional pager to facilitate communication between staff. Unfortunately, pager technology is known to be uncertain, inconvenient, and only permits one-way transmission of non-specific, typically unencrypted, messages.1,4 Even small delays in the transmission of clinical information can result in significant consequences within the hospital environment, where messages tend to be time-critical and involve large multidisciplinary teams spread across distant sites.2,5 Indeed, pager-related communication delays are estimated to be responsible for approximately 20% of all medical errors. 1
Communication applications, such as WhatsApp, Microsoft Teams and Facebook Messenger, offer a rapid, free and widely accessible alternative to the traditional medical communication model. Such applications provide instant and direct connection between healthcare team members through multimedia and text messaging, voice and video calls, group-based discussions, and more. As a result, communication applications have been widely adopted to aid in clinical decision making, enhance patient handover, monitor unwell patients, and communicate urgent results or changes in management plans.6–13 Recent data suggest communication applications have flattened traditional hierarchies between senior and junior clinicians, thus increasing connectedness among team members.6,8 In one tertiary centre, implementation of a communication application within a surgical department significantly reduced the number and complexity of after-hours emergency procedures. 14
As adoption of communication applications has grown, so too have concerns regarding the safety, ethics, and legality of digital data sharing.15–18 While clinicians are generally aware of the requirements for patient confidentiality and adequate medical record keeping, many are unaware of the security features of commonly used applications and whether they satisfy privacy regulations.2,9,11 Consumer communication applications available at present are required to comply with Australian Privacy Principles, as outlined in the Privacy Act of 1988.2,17–21 However, there have been notable breaches and controversies regarding the handling of personal data, such as the Meta and Cambridge Analytica data privacy case, which have highlighted systematic failures in protecting user information and have led to enforceable undertakings by the Office of the Australian Information Commissioner (OAIC).22,23 To fulfill such privacy requirements, communication applications must incorporate robust features such as end-to-end encryption, remote user access controls, formal audit trails, and secure data storage on a secure, preferably local, server.20,21 Although several studies have explored the benefits of communication applications in the delivery of efficient patient care,1,6,8,14,24–27 there remains a paucity of published evidence regarding Australian clinician perspectives and practices regarding patient consent and the handling of sensitive personal information when using these platforms. Additionally, limited data exists regarding the use of such technologies in critical care settings, despite the well-recognised importance of timely and effective communication in acute and perioperative care.3,28 This national cross-sectional survey, conducted primarily among staff specialist anaesthetists, aims to provide a contemporary snapshot of communication application usage and to identify knowledge gaps relating to data security and ethical practice.
Methods
This is a cross-sectional survey of Australian clinicians. The research was approved by the Human Research Ethics Committee of the Southern Adelaide Local Health Network (SALHN) with a multi-centre waiver (approval number: SALHN HREC OFR 163.23). Participant anonymity and confidentiality were protected at all times. Reporting of this study adhered to the recommendations of Strengthening the Reporting of Observational Studies in Epidemiology (STROBE). 29
Study design and setting
A brief questionnaire was distributed to Australian medical professionals over a 4-month period (June to September 2024). Chief investigators were recruited voluntarily through a professional development network for anaesthetists (the Australian Society of Anaesthetists National Scientific Congress Clinical Audit Program) and subsequently tasked with survey dissemination to medical staff at their site of practice. Distribution strategies consisted of disseminating a uniform resource locater (URL) link through email and professional groups, word of mouth, and placement of quick response code placards in common rooms within the workplace. All medical practitioners, including anaesthetists, surgeons, physicians, and junior medical officers, employed at the investigator’s principal site of practice were deemed eligible to participate in the study. Non-clinicians or allied health staff were excluded.
Study aims
The primary aim of this study was to define the prevalence of communication application use among Australian medical professionals, with a particular focus on those working in perioperative and acute care settings. This included the type of device used, information transmitted, frequency of use, preferred application, engagement in workplace discussion groups, and perceived benefits. Secondary aims of this study were to examine clinicians’ level of comfort when considering clinical vignettes depicting the transmission of: (a) non-identifying; (b) identifying; and (c) photographic patient details. Additionally, clinicians’ knowledge and attitudes towards data security and privacy regulations governing the use of communication applications in the workplace were explored.
Outcome measures
The 25-question anonymous digital survey elicited demographic details (e.g. age, gender, specialty and subspeciality, level of training) as well as trends in communication application usage (i.e. device used, information transmitted, preferred application, total number of patient-related messages sent per week). Participants were asked to indicate whether they felt comfortable (yes/no) posting identifying, non-identifying, or photographic patient details via each communication application. Eight communication applications were considered throughout the survey: WhatsApp, Facebook Messenger, Dropbox, Gmail, Slack, Microsoft Teams, iMessage and Short Messaging Service (SMS)—which were selected based on commonly reported clinical and personal communication platforms within our institution. Finally, the participant’s understanding of data security and privacy regulations was elicited, including awareness of local hospital policies, personal device security practices, and familiarity with encryption and metadata removal software. All questions were structured as predefined (multiple choice) response options to ensure standardized data collection.
Statistical analysis
All statistical analyses were performed using STATA version 18.0 (StataCorp LLC, Texas, USA). As the survey consisted of categorical multiple-choice items, responses were summarized using frequencies and percentages. Comparisons of discrete variables across respondent demographics (e.g., age group, specialty, and level of training) were performed using chi-squared tests. All tests were two-sided and significance was set at P < 0.05.
Results
Characteristics of respondents
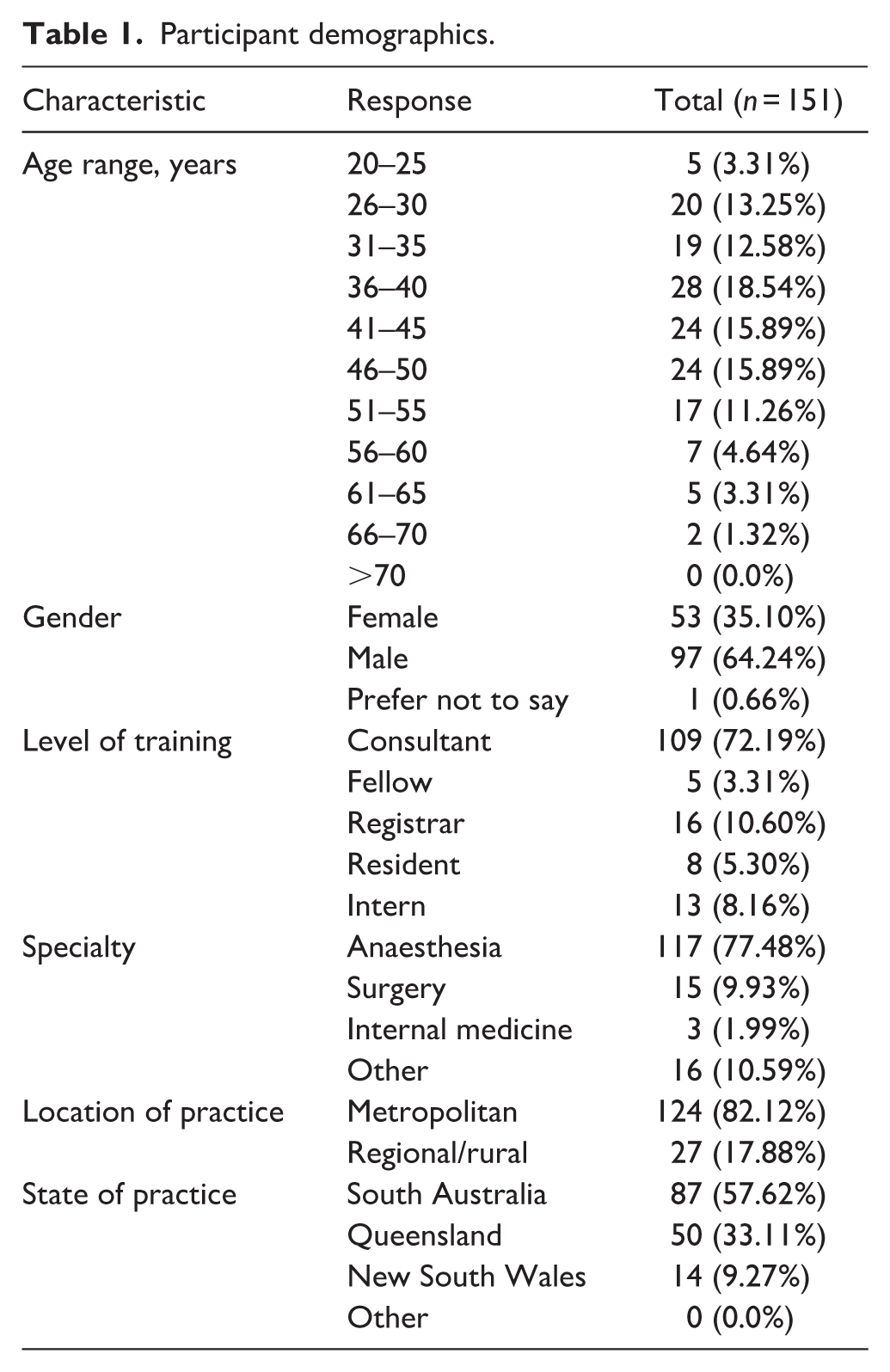
Eight anaesthetist investigators practising across six Australian hospitals recruited a total of 151 survey participants. The majority of respondents practised in South Australia (n = 89, 58%), although participants from Queensland (n = 50, 33%) and New South Wales (n = 14, 9.27%) were also included. Of 151 medical professionals surveyed, 124 (82%) practised in a metropolitan centre, while 27 (18%) practised regionally or rurally. In keeping with a specialist anaesthetist-led recruitment process, most respondents were consultants (n = 109, 72%) practising in the field of anaesthesia (n = 117, 77%). Almost twice as many men (n = 97, 64%) participated as compared with female medical professionals (n = 53, 35%). All included doctors were aged between 20 and 70 years, with a median age range of 41 to 45 years. Table 1 displays the key demographic information elicited from participants.
Participant demographics.
Trends in the usage of digital devices
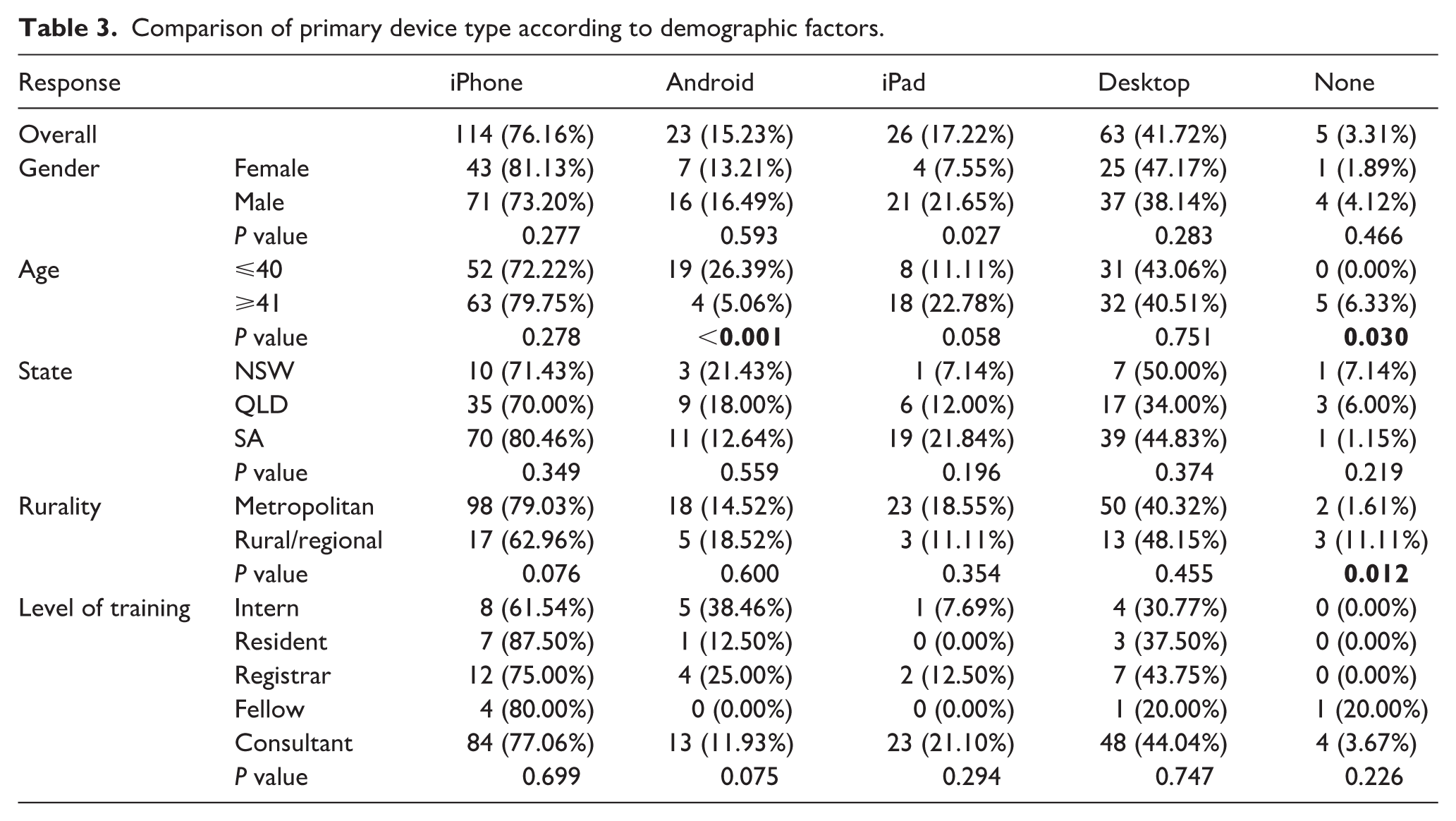
Regardless of a participant’s gender, age, state, level of training or rurality, the Apple iPhone was the most frequently utilised device when accessing and communicating patient data (Table 2). No significant differences between states were found with regard to digital device usage (Table 3). Participants living outside of metropolitan regions in Australia were significantly more likely to forgo the use of digital devices in a professional setting (11.1% vs. 1.6%, P = 0.012). Younger participants (40 years old or less) were significantly more likely to report using non-Apple devices, such as Android (26.4% vs. 22.8%, P ⩽ 0.001) (Table 3).
Trends in communication application usage.
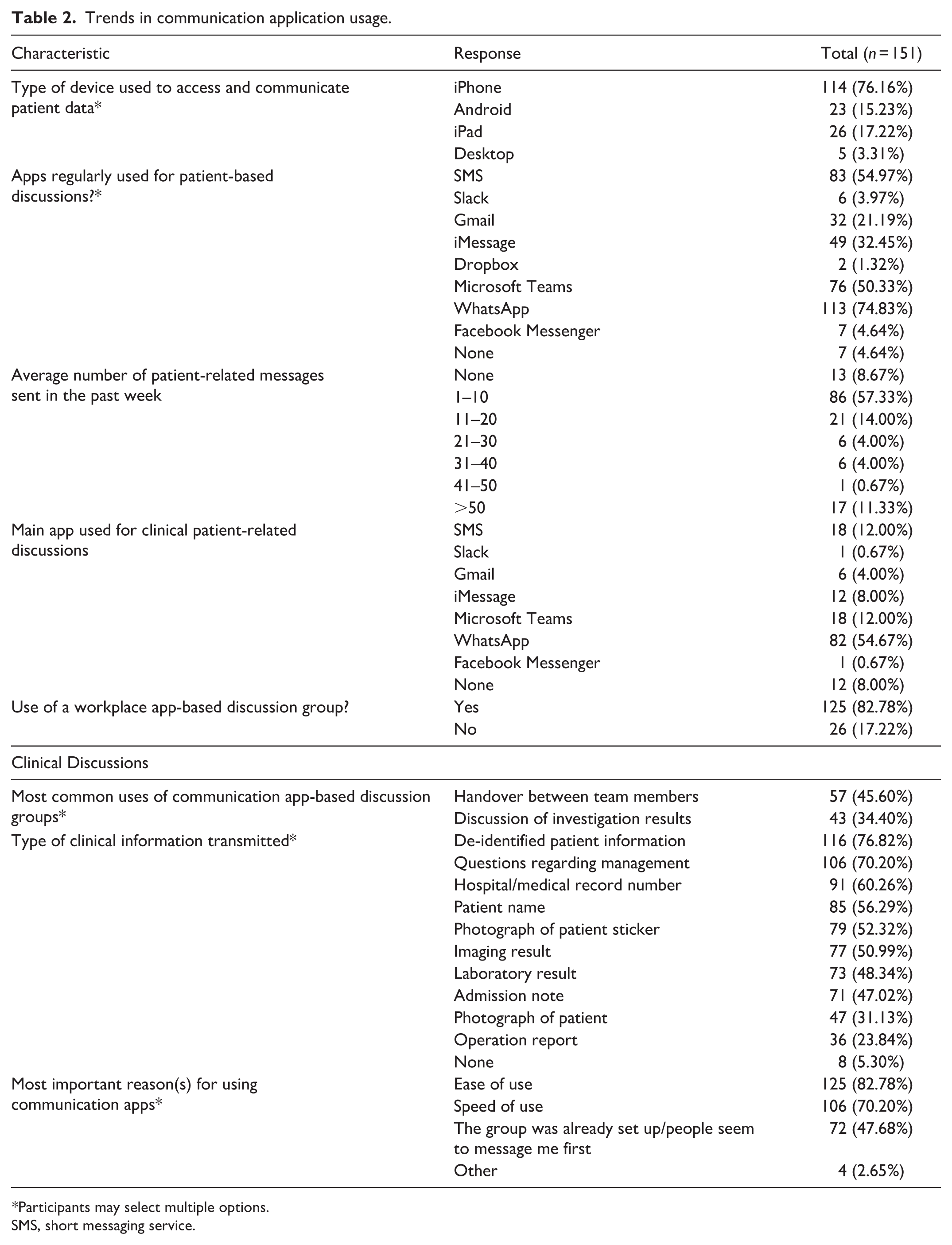

*Participants may select multiple options.
SMS, short messaging service.
Comparison of primary device type according to demographic factors.
Trends in the uptake of specific communication applications
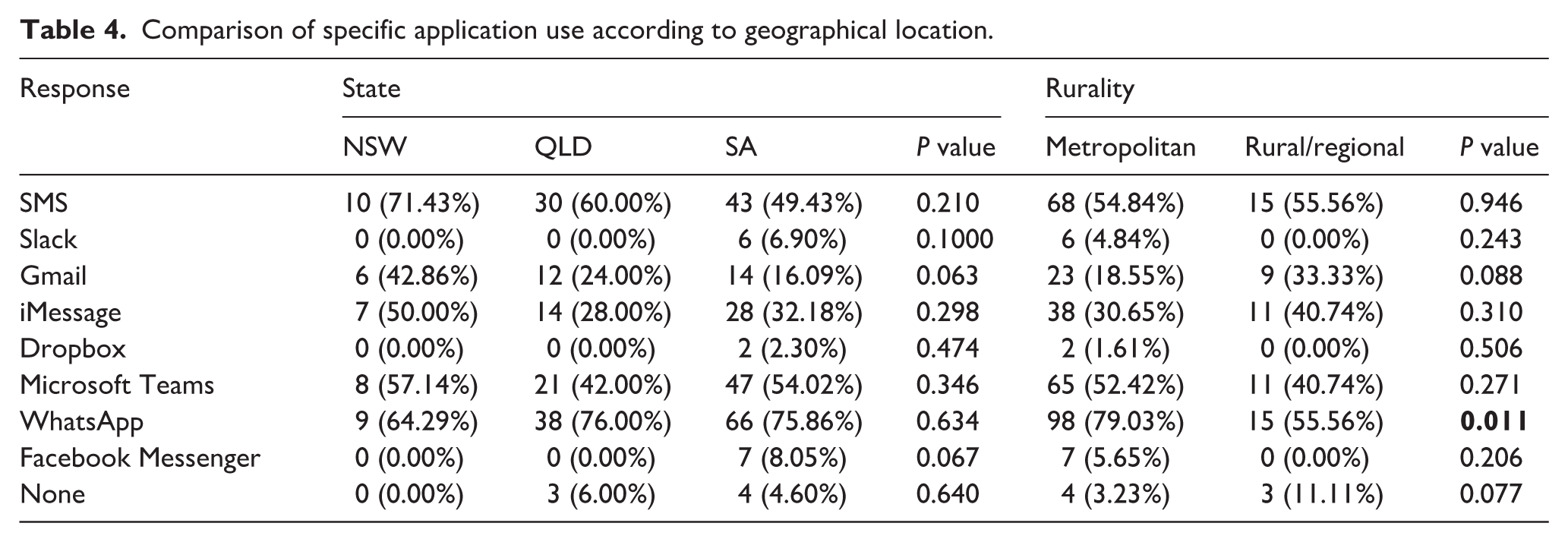
The communication application most frequently used to facilitate patient-based discussions was WhatsApp (n = 113, 75%), followed by Microsoft Teams (n = 76, 50%). Indeed, when asked to select a single most preferred application for clinical and patient-related discussions, WhatsApp was the most common response regardless of participant age or training level (Table 2). Conversely, approximately 5% of doctors (n = 7) reported never using any communication applicationss for the purpose of clinical discourse. This phenomenon occurred more commonly in older participants (6.33% of those aged above 40 vs. 0% of those 40 years or below, P = 0.03) and in those residing outside of metropolitan centres (11.11% vs. 1.61%, P = 0.012) (Table 4).
Comparison of specific application use according to geographical location.
Trends in frequency and purpose of communication application usage
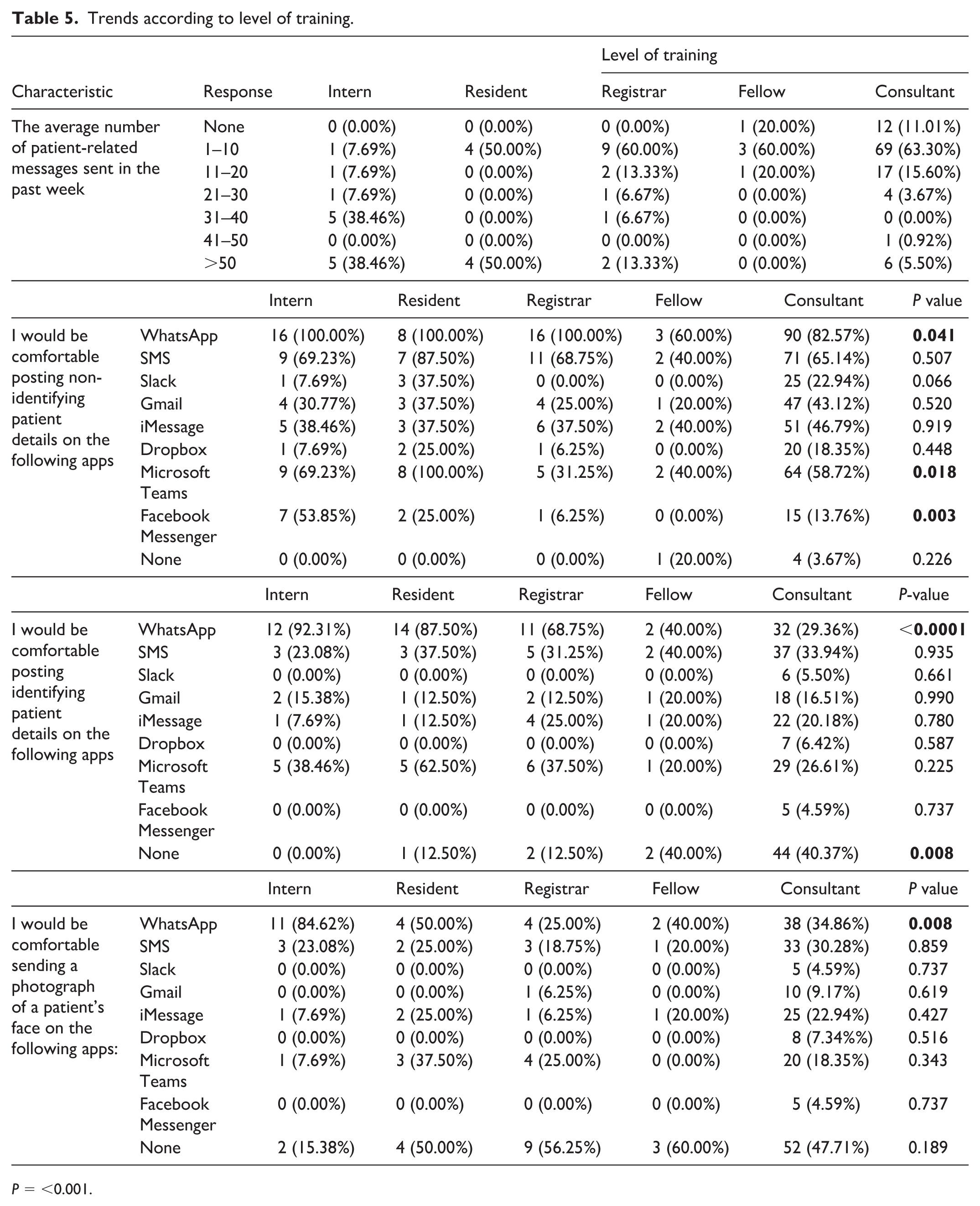
When asked to estimate the average number of patient-related messages sent in the past week, most participants (n = 86, 57%) reported sending between one and 10 messages. Interns were significantly more likely to report sending greater than 30 patient-related messages per week (77% of interns vs. 6% of consultants, P ⩽ 0.001). Approximately 9% of the overall cohort (n = 13) reported sending no messages at all, all of whom were consultants or fellows (Table 5).
Trends according to level of training.
P = <0.001.
Engagement with workplace discussion groups was prevalent among the cohort, with 83% of participants (n = 125) reporting active participation in such groups. Doctors reported utilising digital discussion groups primarily for the purpose of patient-related dialogue (n = 98, 78%), clinical handover (n = 57, 46%) and to discuss pertinent results (n = 43, 34%). In most cases, participants felt communication applications allowed for improved ease and speed of communication (Table 2).
Views regarding the sharing of patient information
Most Australian doctors surveyed (n = 100, 66%) revealed they would feel comfortable posting non-identifying patient information via communication applications (Table 2). Doctors were most comfortable sharing non-identifying details via WhatsApp (n = 130, 86%) and SMS (n = 100, 66%). Women were more likely to share non-identifying details via Gmail (53% of women vs. 31% of men, P = 0.008) while junior doctors were more likely to share non-identifying details via Teams (81% of interns/residents vs. 33% of registrars/fellows, P = 0.018).
When considering the sharing of identifying patient details (e.g. patient full name, medical record number), there was a significant reduction in overall comfort levels (Table 6). This trend was observed regardless of participant age, location of practice or level of training. Despite increasing discomfort, the majority of doctors stated they had previously shared a patient’s medical record number (60%), full name (56%), or identification sticker (52%) via digital means (Table 2). WhatsApp remained the most trusted app for transmitting identifying patient details (n = 64, 42%), including clinical photographs. Forty-nine (33%) of those surveyed did not feel comfortable posting identifying patient details on any communication application and this percentage increased with age (18% of those under 40 years vs. 46% of those over 40 years, P ⩽ 0.001). Participants felt similarly uncomfortable in sharing clinical photographs of their patients’ faces, with only 32% of doctors (n = 59) stating they would do so when faced with a hypothetical clinical scenario (Table 6). Correspondingly, 31% (n = 47) of doctors admitted to using communication applications to send patient photographs in the past (Table 2).
Views regarding sharing of patient information.
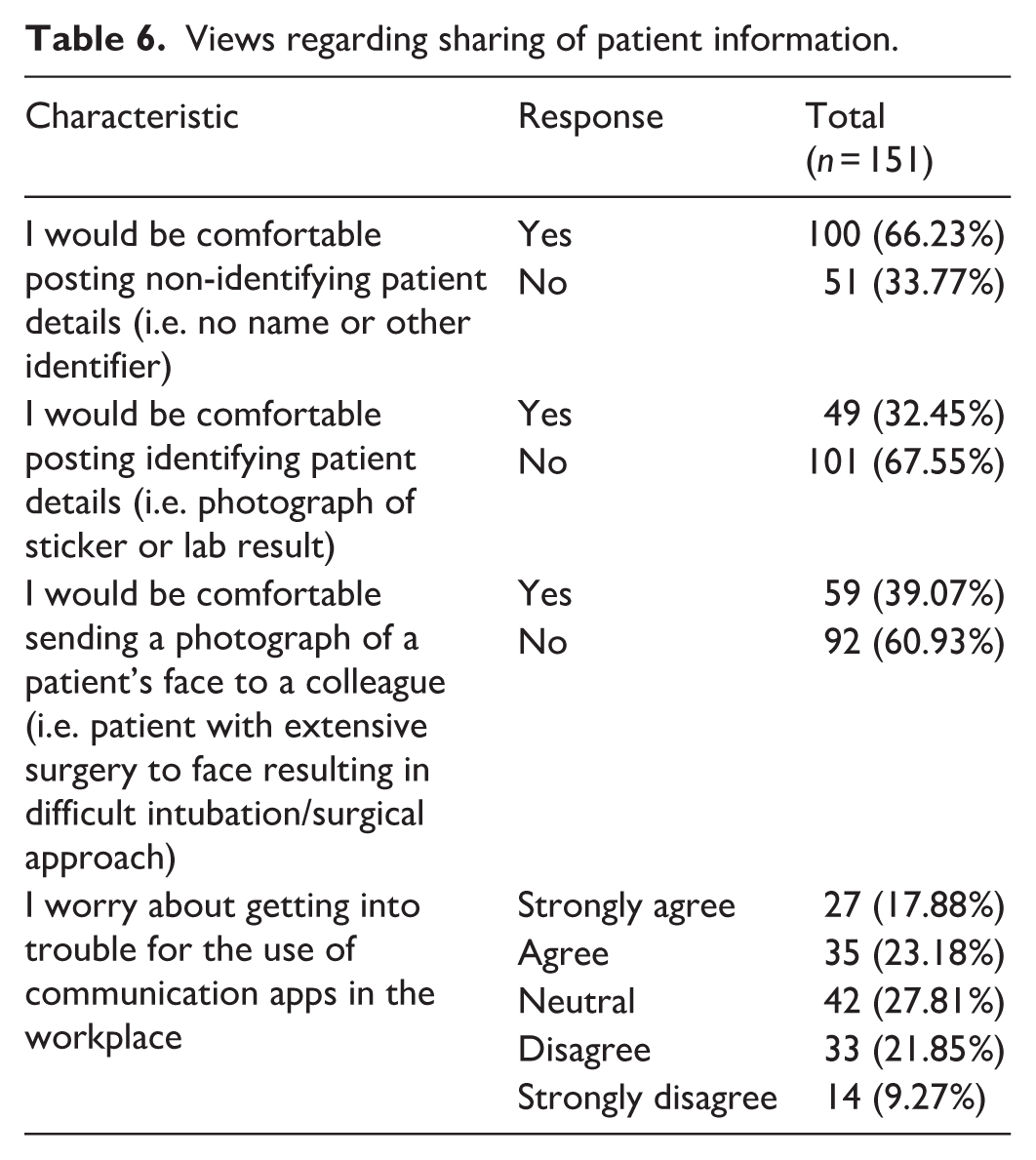
Doctors responded with varying degrees of agreement when prompted with the statement, ‘I worry about getting into trouble for the use of communication apps in the workplace’. Twenty-eight per cent of participants (n = 42) felt neutral towards this statement, while 41% (n = 62) either agreed or strongly agreed and 31% (n = 47) either disagreed or strongly disagreed (Table 6).
Understanding of privacy requirements and data storage
When knowledge regarding consent and documentation requirements for patient photography and image transmission was assessed, 5% (n = 8) considered no patient consent to be required, 35% (n = 53) considered only verbal consent to be required, and 8% (n = 13) considered both verbal and written consent to be required. Additionally, 32% (n = 48) regarded additional documentation in patient notes to be a requirement and 19% of doctors (n = 29) considered taking patient photographs on a personal device to always be unacceptable, regardless of patient consent (Table 7). Approximately 30% of participants (n = 45) were aware of local hospital policies regarding the use of communication applications to transmit patient data (Table 7).
Understanding of privacy requirements and personal practices.

Personal device security and access was also ascertained. Overwhelmingly, biometrics were the most frequently reported security feature used by doctors (79%, n = 119), followed by personal identification number (PIN)-codes (14%, n = 21) and passwords (5%, n = 8). A notable proportion of doctors felt ‘unsure’ when asked to describe how data on their personal device or preferred messaging application were secured and backed up (Table 7). The majority of those surveyed (81%, n = 123) were not familiar with the removal of metadata from patient-related photos and thus did not routinely utilise this technology. Those familiar with the removal of meta-data were more likely to be aged under 40 years; however, this finding was not statistically significant (24% of those under 40 vs. 14% of those over 40 years, P = 0.135).
Discussion
Communication application usage is widespread among doctors practising in Australian hospitals, with many citing ease and speed of use as key reasons for adoption. Our findings align with existing evidence indicating the adoption of communication applications is particularly prevalent among junior doctors and those practising in metropolitan regions.7,9,12,30 The comparatively lower uptake among regional clinicians is of note and may reflect structural differences in clinical environments, such as smaller teams in which verbal communication is more practical, and greater reliance on formal referral pathways to tertiary centres via telephone, potentially reducing the need for informal digital communication tools.
While our cohort was predominantly composed of staff specialist anaesthetists, our data contributes to a growing body of evidence that WhatsApp is the most popular application for medical discourse among doctors, followed by Microsoft Teams.2,13,24,27 Nikolic et al. 2 proposed that the growing popularity of WhatsApp is due to its user-friendly and reliable interface, cost-free access and already extensive integration into Australian hospital culture. In comparison with earlier studies, our finding of an average of one to 10 messages sent per day is somewhat below the median of 10 to 12 messages reported in previous Australian research. 2 This discrepancy may be explained by the inclusion of a relatively older (more than 70% aged 36 years or older) and more senior (72% consultants) cohort, most of whom were practising in anaesthesia (78%). Evidence to date has largely focussed on surgical and internal medical specialties, with limited data capturing uptake trends within the field of anaesthesia. Given that anaesthetists are more likely to work within fixed, theatre-based teams and remain in a single location for extended periods, it is plausible that their need for digital communication tools may be less pressing than for junior clinicians or ward-based doctors who move between multiple locations and teams throughout the hospital.
With the advent of digital medical photography, there is a need to balance technological advancements with ethical and legal considerations. Medical indemnity providers have identified clinical photography as an area of rapidly growing medicolegal risk for healthcare professionals.18,31 According to the Australian Privacy Act 1988, patient information should be used only for the purposes for which it was originally collected and to which the patient consented. 21 Failing to obtain or properly document informed consent for photography may leave clinicians open to legal liability.15,18 Although no specific legislation governs this practice, medicolegal advisers and the Australian Medical Association (AMA) strongly recommend documenting the consent process, including the purpose and intended recipients of the image, in the patient’s medical record whenever clinical photographs are taken using personal devices. 32 Despite this guidance, Kunde et al. 15 report a trend among clinicians toward bypassing written consent when capturing and transmitting patient images. This trend is echoed in our study, in which 76% of clinicians acknowledged the need for verbal patient consent but only 40% deemed written consent to be necessary. Alarmingly, eight clinicians believed no consent was required at all. It is reassuring, however, that nearly all participants reported securing their devices with biometrics (79%), PIN codes (14%), or passwords (5%), in line with AMA recommendations to implement access controls to prevent unauthorised use. 31 This is of note because, if collected correctly and stored systematically, digital records can potentially offer greater security than traditional paper records, which are vulnerable to being misplaced, photocopied, or altered. 17
Our study contributes to a growing body of evidence highlighting a concerning lack of clinician awareness regarding hospital policies on the use of personal mobile devices.2,5,9 Less than one third of participants were familiar with local hospital policies governing the use of communication applications for sharing patient information, a figure notably below previous Australian estimates. 2 Further, almost half of clinicians surveyed expressed concern about potential repercussions of using personal mobile devices in the workplace, yet these worries did not appear strong enough to deter them from using these applications altogether. This striking discrepancy between clinicians’ reported concerns and their actual behaviour suggests that perceived convenience and workflow efficiency may outweigh privacy and legal considerations for Australian doctors in their day-to-day practice. Additionally, our findings highlight the critical need for clear, accessible institutional policies that specify approved messaging platforms and delineate appropriate use in line with privacy legislation. According to the OAIC, organisations have a responsibility to implement governance measures, such as risk assessments, staff training, and robust internal policies, when staff use messaging applications for professional communication. 23 Hospitals should therefore consider providing staff with secure, approved communication platforms that comply with Australian privacy principles in order to support safe, efficient clinical communication. Where such tools are mandated, institutions may also need to subsidise or fund their use to promote compliance and reduce reliance on unregulated consumer applications. Consistent with the findings of Nikolic and colleagues, 2 only 10% of Australian doctors were aware that their preferred communication applications (i.e. WhatsApp) may be associated with inadvertent overseas disclosures of health information, particularly through device back-ups when appropriate privacy controls are not enabled. 23 While the hosting of encrypted message content by such applications does not itself constitute a privacy breach, the potential for data exposure via cloud back-ups underscores the importance of clinician awareness and device-level data protection settings.
While guidelines exist for the use of clinical photography, mobile phones and social media in the workplace (e.g. AMA and NSW Health Codes of Conduct),32,33 formal Australian healthcare guidelines catered specifically to the use of communication applications are lacking. Recently, questions have been raised about the need to obtain patient consent whenever any form of information is shared via these applications, similar to the consent requirements currently in place for clinical photography. 2 Ongoing discussions, including input from legal and medical advisory bodies, are urgently needed on this issue as it is likely that imposing such formal requirements could significantly undermine the speed and efficiency that currently make communication applications attractive in a healthcare setting. Looking ahead, the integration of artificial intelligence (AI) into clinical communication platforms may further disrupt this space. While AI offers potential gains in productivity and patient safety (e.g. automated clinical summaries and handovers, triaging of messages based on urgency, intelligent decision support), it will likely also introduce new complexities around data privacy–further reinforcing the need for clear, adaptive regulatory frameworks.
Limitations
Our cross-sectional survey has several limitations of note. Firstly, the study relied entirely on self-reported data, which is susceptible to selection and recall biases. When compared with demographic data from the Medical Board of Australia, our sample was more likely to consist of male doctors aged below 50 years, residing in South Australia and working in the field anaesthesia. 34 These demographic differences may limit the generalisability of our findings to other medical specialties, regions or healthcare settings. While our cohort of 151 doctors is larger and more geographically diverse than previous Australian studies in this field, it may still lack the statistical power to detect meaningful differences between subgroups, particularly given the broad diversity of healthcare institutions and clinical practice across the country. Respondents were restricted to selecting from only eight pre-determined communication applications when answering survey questions, thereby limiting the detection of trends pertaining to the use of other applications among Australian doctors. Nevertheless, our findings were concordant with existing literature and we are confident overall trends would remain consistent should this study be replicated in a separate cohort of Australian doctors.
Conclusion
Communication application usage among anaesthetists and other medical staff in Australian hospitals is well-established and offers numerous benefits over traditional forms of healthcare communication. The growing adoption and benefits of these applications must be carefully balanced against potential risks to patient safety, confidentiality and legal standards. Currently, clinician knowledge of local hospital policies regarding communication application use in the workplace is low, highlighting a pressing need for the establishment of formal Australian guidelines in this field.
Footnotes
Author contributions
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
