Abstract
Awake tracheal intubation (ATI) is advocated in situations where complex airway anatomy or deranged physiology make usual post-induction airway management hazardous. The safety of ATI has been described in many settings. Nevertheless, it is not always performed when indicated, and significant patient harm as a consequence is still reported. A survey was conducted to investigate anaesthetists’ practices and possible reasons for reticence in performing ATI. The survey also sought to explore solutions to limited opportunities for training and skills maintenance. The 17-question survey was sent to a random selection of 1400 consultant anaesthetists across Australia and New Zealand in 2023. The response rate was 36% (499 of 1400). Forty percent (198 of 499) (95% confidence interval (CI) 35 to 44) of participants had not performed an ATI in the last 12 months. The majority of participants (64% (317 of 499) (95% CI 59 to 68)) agreed that there were barriers in their own practice to performing ATI. There was strong agreement that proficiency in ATI should be within the skillset of on-call anaesthetists (81% (400 of 494) (95% CI 78 to 84)). There was also strong support for ATI to become a mandatory core skill (74% (368 of 497) (95% CI 70 to 78) of participants). Current volume of practice for trainees was almost universally considered insufficient (93% (459 of 496) (95% CI 90 to 95)). There is a disparity between the perceived importance of competence in ATI and the limited volume of practice expected of trainees and paucity of ongoing clinical exposure for consultants. Training and programs to maintain skills in ATI are urgently required to address this.
Introduction
Awake tracheal intubation (ATI) continues to be recommended for the most concerning of anatomic and physiologic presentations requiring airway management.1–4 Published studies with large numbers indicate a high overall success rate with the technique.5–9 When significant difficulty with airway management is predicted, ATI confers safety during tracheal intubation since the patient maintains gas exchange, airway patency and lower airway protection until after the tracheal tube has been placed and confirmed to be correctly located. 8 Awake tracheal intubation most often occurs in the topically anaesthetised airway of a patient using a flexible bronchoscope, but can also be achieved with other techniques such as videolaryngoscopy, including the combination of using a videolaryngoscope with a flexible bronchoscope.
Despite the utility of ATI, there is some indication that its use is declining in anaesthetic practice.8,10 This might be concerning, as studies of airway-related morbidity suggest that despite significant predictors of difficulty, ATI is sometimes not used when indicated.3,11,12
Videolaryngoscopy performed after the induction of general anaesthesia can address some difficult anatomic presentations, especially if performed with a hyperangulated blade. 13 There has likely been substantially increased use of videolaryngoscopy over the last 10 years, and this is appropriate given published evidence of higher first-attempt success13–17 and lower complication rates13,17 compared with direct laryngoscopy. However, not all challenging anatomic presentations can be successfully addressed with post-induction videolaryngoscopy. Furthermore, potential danger to the patient may also be posed when difficulty with ventilation by face mask and/or a supraglottic airway device is also predicted, or when there are patient-specific physiologic concerns such as a decreased ability to tolerate short periods of apnoea or the haemodynamic consequences of induction agents. Furthermore, potential danger to the patient may also be posed when difficulty with ventilation by face mask and/or a supraglottic airway device is also predicted, or physiologic concerns such as apnoea intolerance exist. None of these issues is addressed by using videolaryngoscopy after induction. Thus, there remains a subset of patients for whom ATI is the most appropriate method to secure the airway.
Increasing use of videolaryngoscopy after induction for both routine and difficult airway patients can come at the cost of fewer opportunities to maintain skills in ATI, or to teach ATI to trainees. This can potentially result in clinicians being uncomfortable in performing the technique. Indeed, ATI has been highlighted as a procedure performed with relatively low confidence compared with other airway techniques. 18
Little published literature exists on what factors might be most responsible for clinicians’ reticence to perform ATI. This is an important knowledge gap worth addressing, so that educational programs can emphasise aspects of performing ATI that might cause avoidance of this technique. Other similarly rare but life-saving competencies have mandatory continued professional training requirements set by the Australian and New Zealand College of Anaesthetists (ANZCA) (‘can’t intubate, can’t oxygenate’, major haemorrhage, anaphylaxis, and cardiac arrest). In keeping with this, we conducted a survey to investigate anaesthetists’ practices and potential reasons for reticence in performing ATI. We hypothesised that avoiding employing ATI occurs because of a variety of factors, which might include practice volume, training, perceived patient discomfort, practitioner discomfort, time pressure, equipment issues or departmental culture. We also sought to explore potential solutions to limited opportunities for training and skills maintenance in ATI.
Methods
Local research ethics committee approval was granted (HREC/97807/PMCC).
A group of local and international anaesthetists with an interest in airway research and education was convened in order to design the survey. Meetings were conducted to identify themes of interest and appropriate wording of the survey. Prior to finalisation, the survey was piloted locally, and feedback incorporated into the design. The survey was produced according to the quality standards of the ANZCA Clinical Trials Network, which facilitates survey dissemination after peer review. The intention was for dissemination of the results by way of peer-reviewed publication.
The survey was built and data stored using Redcap, a secure, password protected data platform. To maximise survey completion there were no mandatory questions, and the survey length was reduced to the minimum number of questions to adequately explore the research question. Simple demographic questions were asked last. All surveys, complete and incomplete, were included for analysis. Multiple entries per participant were not possible.
Participation was voluntary, non-remunerated and data collected was anonymous and confidential. The survey was open from 23 July to 23 August 2023. The 17-question survey (see Supplemental material online) was sent via email to a random selection of 1400 consultant anaesthetists across Australia and New Zealand, Fellows of the ANZCA. An email reminder followed two weeks later (further follow-up was restricted to avoid survey fatigue). Sample size was selected based on previous ANZCA survey response rates of approximately 25% and the need for 5% precision on our primary question of regret in not performing ATI. Data was analysed using Stata 18.5 (StataCorp LLC, College Station, Texas, USA). Data is presented as median (interquartile range) (IQR), (range), or proportion (%) as appropriate. The 95% confidence interval (CI) for proportions was calculated using the Wald method without continuity correction given the relatively large sample size.
Results
There were 499 completed surveys, giving a response rate of 36%. Given that there are currently 6178 ANZCA Fellows, this represents 8% of the entire Fellow community. Survey respondents were closely matched in gender but slightly more experienced than the ANZCA Fellow community as a whole. Respondents answered all questions in the survey in 98% of cases. The median number of ATIs performed or supervised in the last 12 months was 1 (IQR 0–3, range 0–36) (Figure 1).
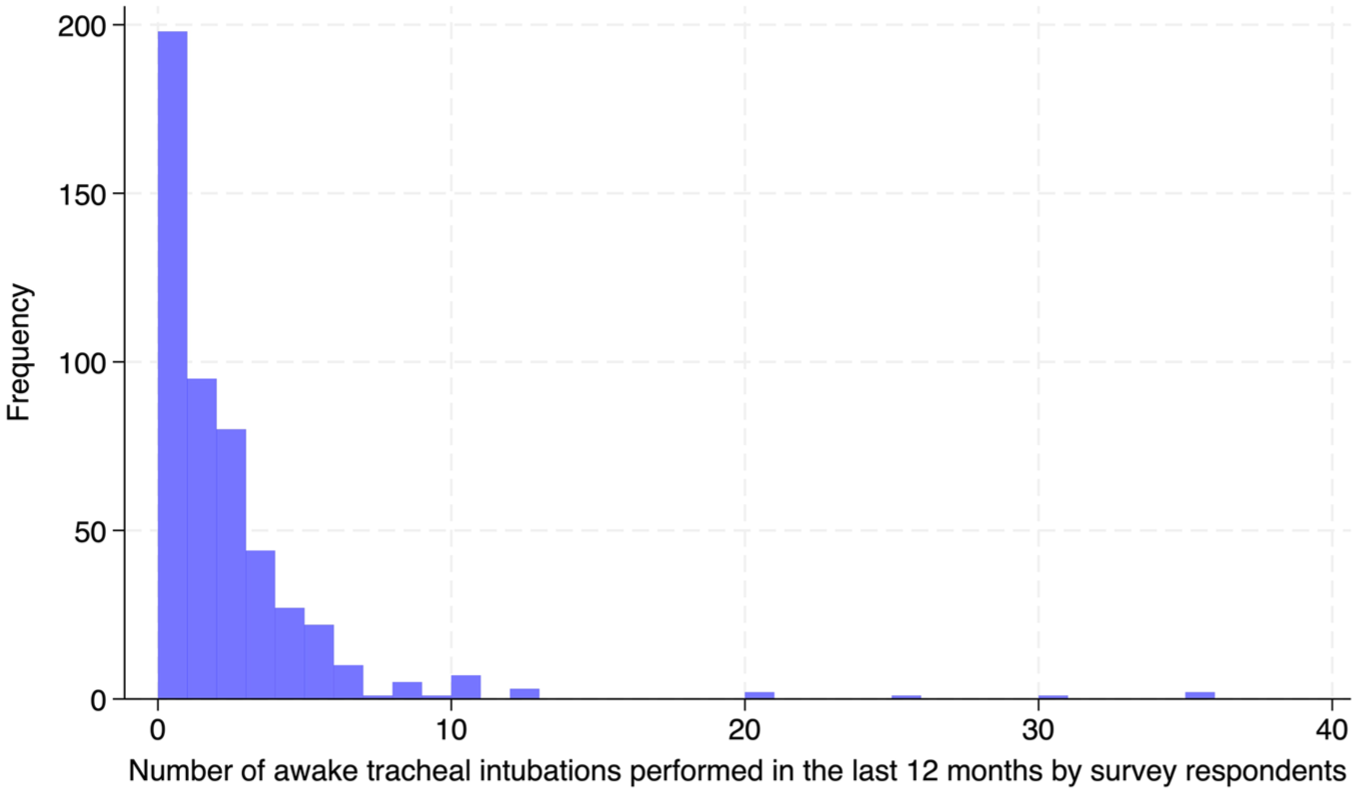
Number of awake tracheal intubations performed in the last 12 months.
The majority of participants, 317 of 499 (64%) (95% CI 59 to 68), agreed that there were barriers in their own practice to performing ATI (Figure 2). The most commonly agreed barriers to performing ATI were previous successful intubation without ATI (404 of 497 (81%) (95% CI 78 to 85)) and concern about causing the patient discomfort (297 of 495 (60%) (95% CI 56 to 64)). Less frequent barriers to ATI included availability of functioning equipment (151 of 496 (30%) (95% CI 26 to 35)), departmental culture or attitude towards ATI (116 of 494 (24%) (95% CI 20 to 27)) and surgeon preference (102 of 491 (21%) (95% CI 17 to 24)).
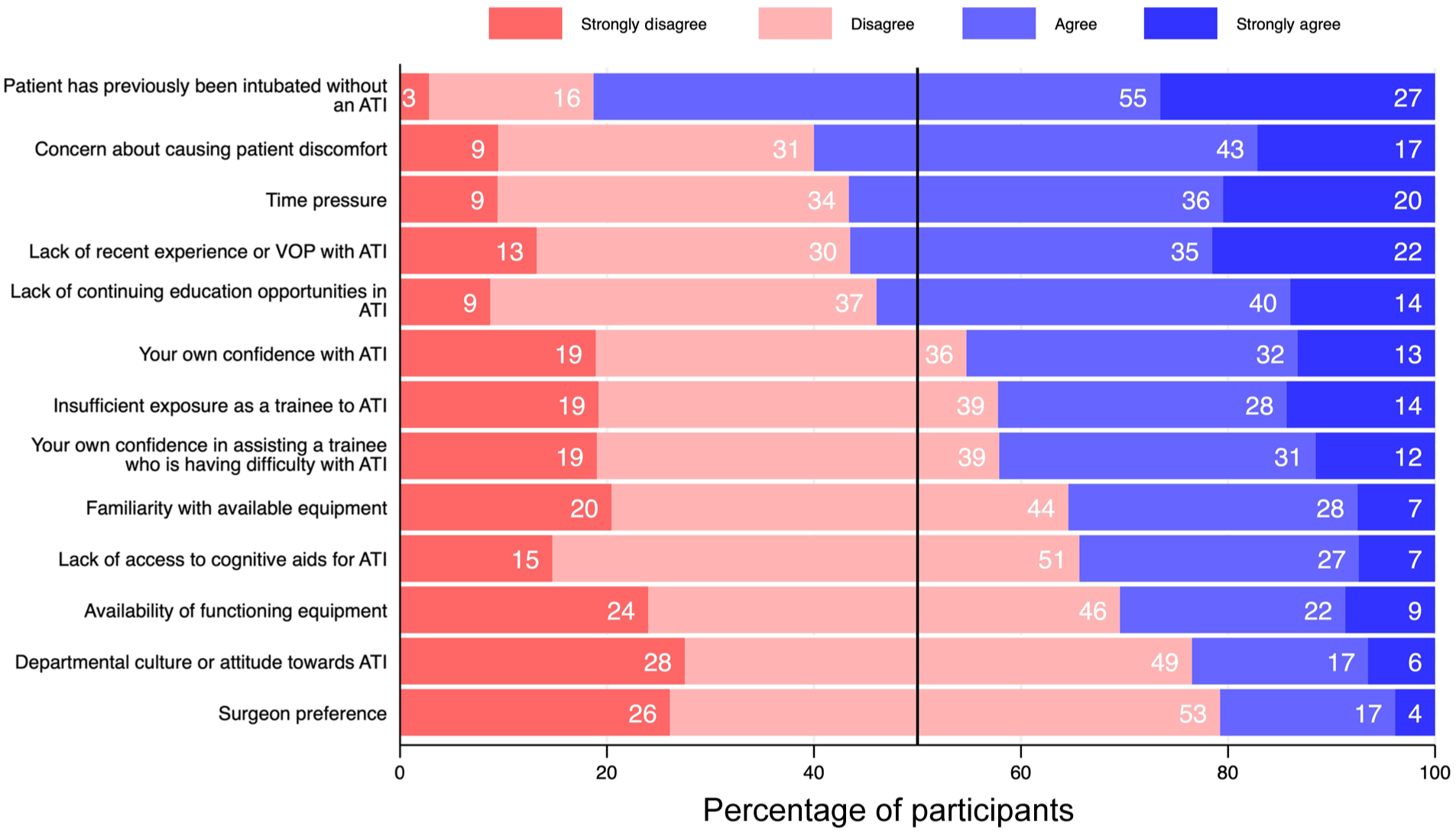
Potential barriers to performing awake tracheal intubation.
Most participants did not support the concept of an on-call airway service for ATI or complex airway cases (273 of 492 (56%) (95% CI 51 to 60)); see Figure 3.
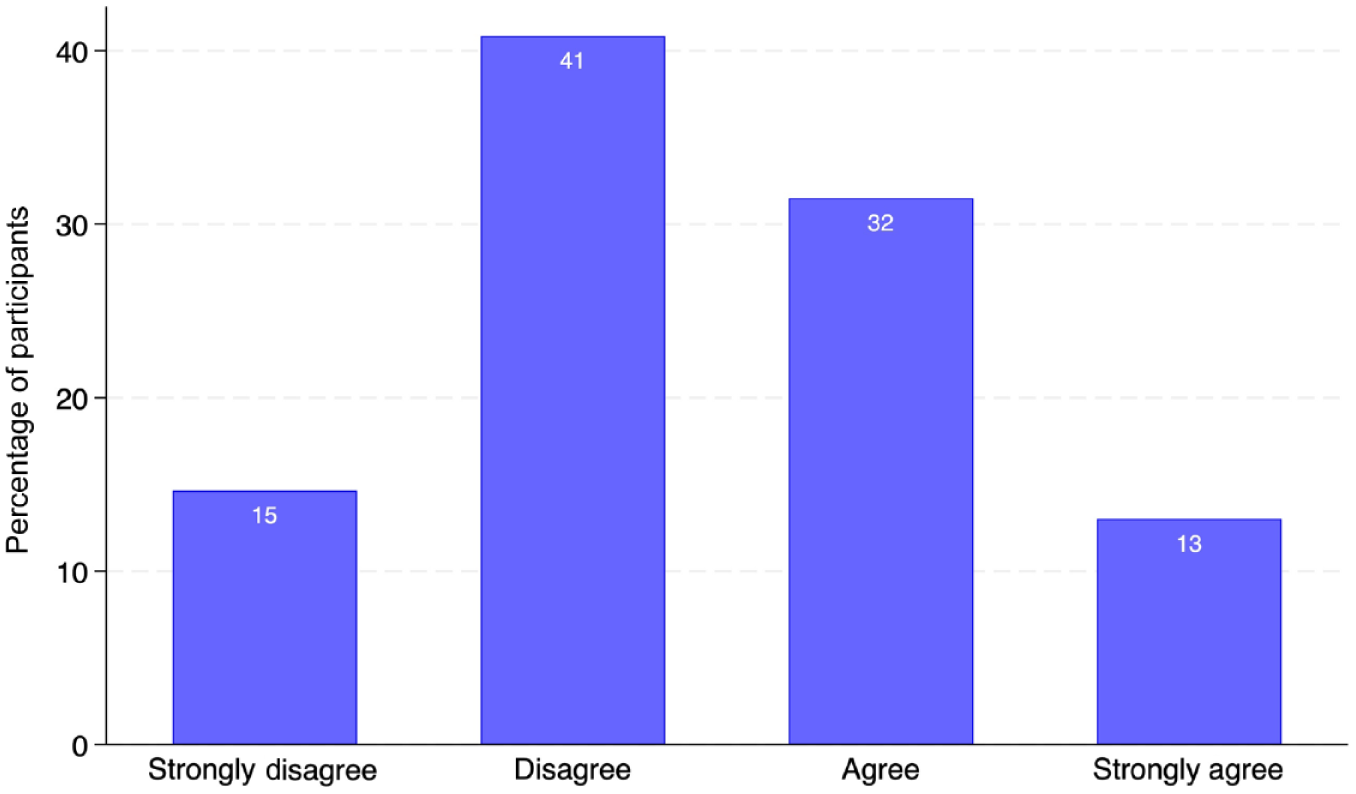
Support for an on-call airway service.
The majority of participants (459 of 496 (93%) (95% CI 90 to 95)) thought that more than five supervised ATIs on a patient are sufficient for a trainee to competently perform the procedure independently (Figure 4).
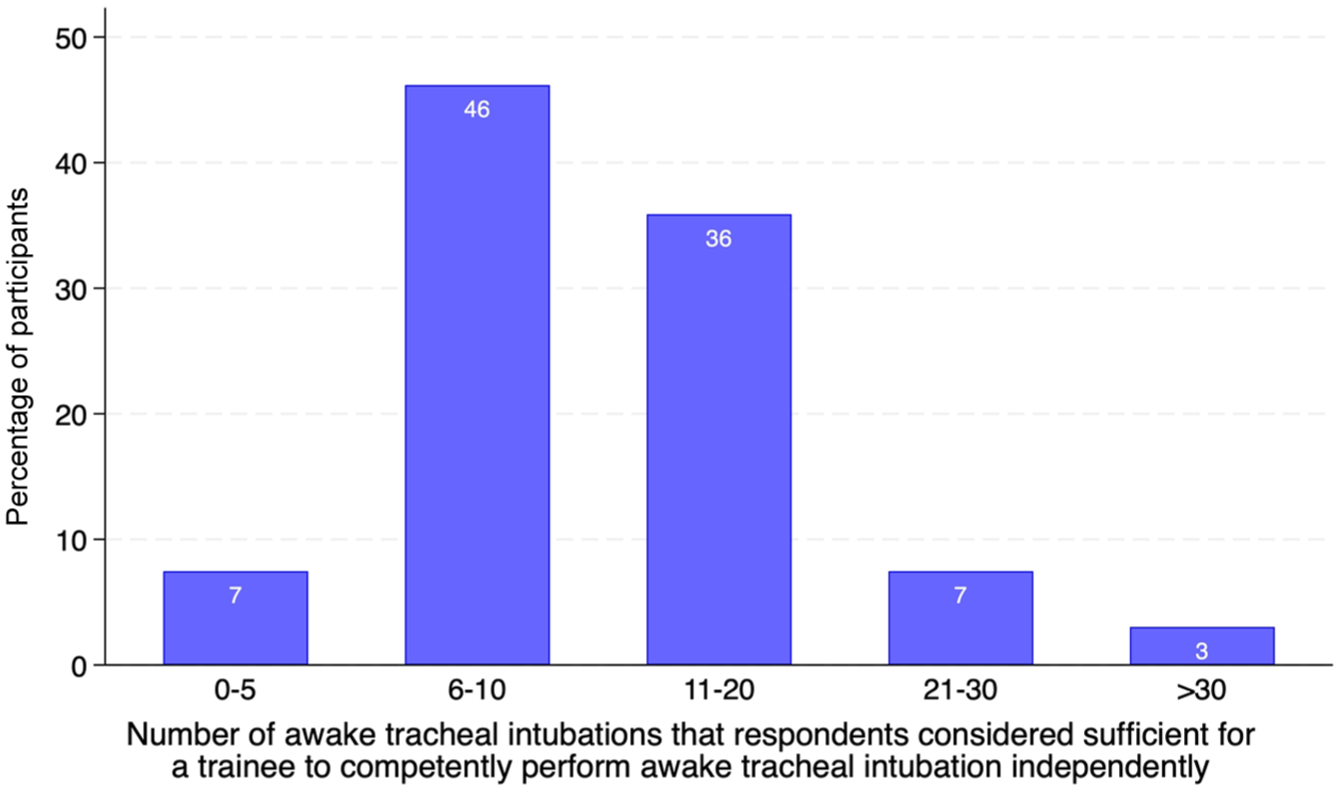
Number of awake tracheal intubations that are considered sufficient for a trainee to competently perform the procedure independently.
Further survey responses are presented in Table 1.
Survey responses of participants.
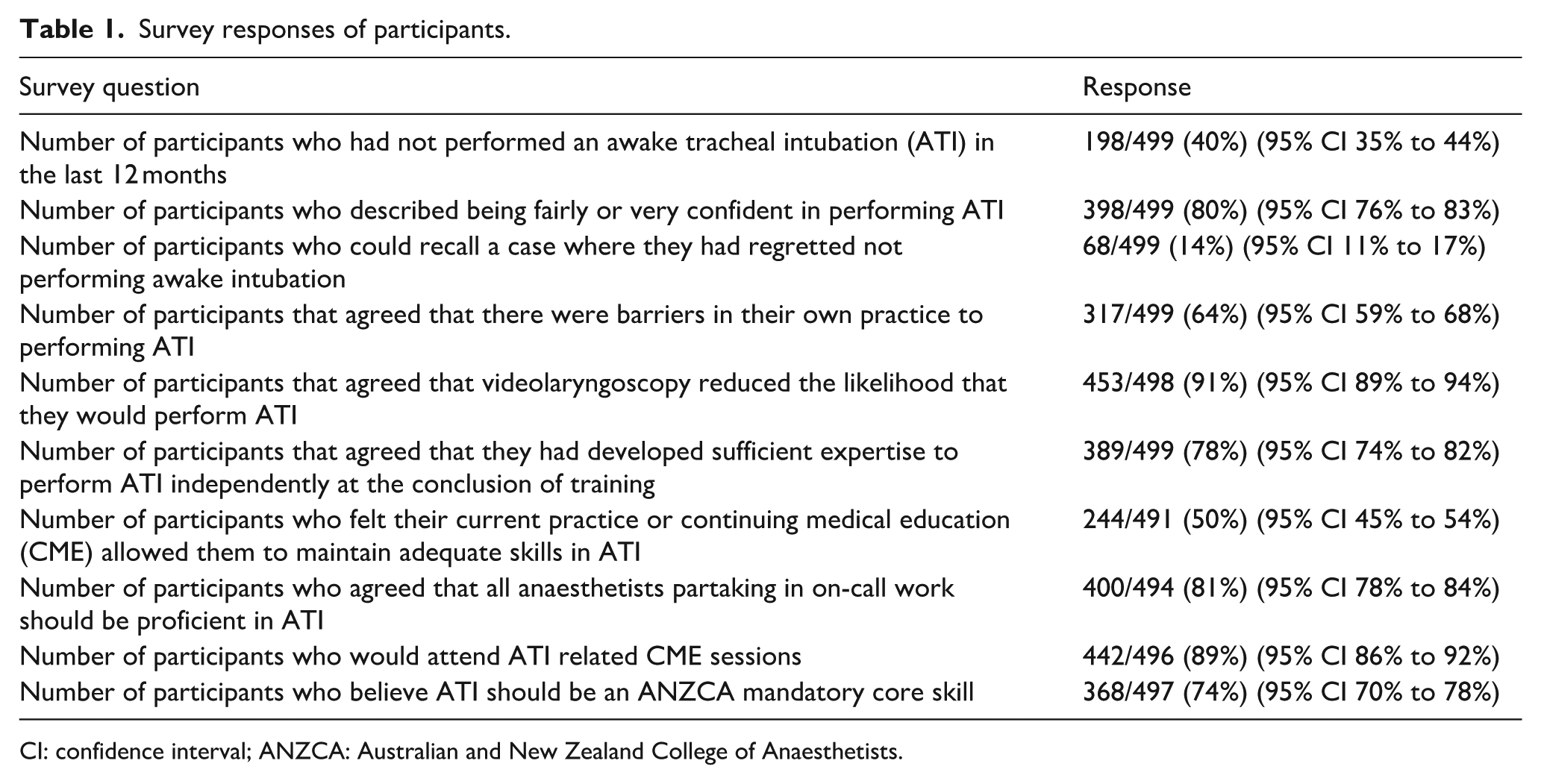
CI: confidence interval; ANZCA: Australian and New Zealand College of Anaesthetists.
Discussion
Our survey builds on a limited body of literature addressing anaesthetists’ practices and barriers to performing ATI. It also addressed solutions to limited opportunities for training and exposure. A random selection of 1400 consultant anaesthetists across Australia and New Zealand was sampled. Considering historical ANZCA survey response rates approximating 25%, the response rate of 36% suggests that this issue is pertinent to practising anaesthetists. Baseline demographic data suggests that a representative sample of anaesthetists across Australia and New Zealand was surveyed. However, generalisability is not assured; respondents with an airway interest may have been more likely to respond, introducing responder bias. If this were the case, the number of ATIs performed annually and the confidence in performing ATI may be reported as higher than the general community of anaesthetists. Due to brevity requirements, engagement with airway education, research or clinical exposure to complex airway cases was not measured.
Nearly 40% of respondents had not performed an awake intubation in the previous 12 months, and there was a median annual rate of performing one ATI per year. In 2016, surveyed members of the Difficult Airway Society described a similarly low rate of ATI. 19 Rates from tertiary centres approximate 1% of all endotracheal intubations.6,8,20
Procedural skill retention is affected by the volume and frequency of the procedure being performed. 21 Given the low numbers of ATI described, it is somewhat surprising that survey respondents nevertheless described a high level of confidence in performing ATI. It is possible that there was a bias towards respondents with an airway interest choosing to complete the survey. It follows that these respondents may have more confidence in performing awake techniques. By comparison, an international survey of 61 countries with the majority of respondents belonging to an airway special interest group assigned a confidence level of seven out of 10 to ATI. 18 It is worth noting that rates of ATI might vary significantly between institutions and countries. A large German hospital recently reported that awake bronchoscopic intubations constituted 4.3% of all airway management procedures. 9 This rate provides a much higher opportunity for training and skills maintenance in ATI than is typically observed in Australia and New Zealand.
Over 10% of respondents could recall a case in which they regretted not performing ATI. The circumstances of each case were not sought as part of the survey. It would be valuable to better understand characteristics of cases where ATI is avoided and patient harm occurs. The Fourth National Audit Project (NAP4) described cases of patient harm in which there were clear indications for ATI but it was not performed. 3 There has been little recent data to add to our understanding in this area. Indications for ATI are nuanced, and gathering prospective data on the frequency of uncommon clinical events is difficult outside of very large audits such as NAP4.
There was agreement that there are barriers to performing ATI (65%). Surgical preference was not viewed as an important determinant in deciding whether to perform ATI. Previous successful tracheal intubation after the induction of general anaesthesia reduced the use of ATI in the survey, although progression of conditions causing airway difficulty can mean that previously successful airway management can be falsely reassuring. Concerns about causing patient discomfort was one of the most frequently cited barriers to ATI in this survey (60%), suggesting the need for more education on the provision of topical airway anaesthesia techniques and/or the effective use of adjunctive systemic medications.
A recent observational longitudinal study has noted a 50% reduction in rates of ATI from 2014 to 2020. 8 Consistent with this finding, 91% of the respondents to our survey agreed that videolaryngoscopy reduced the likelihood that they would perform an ATI. While most respondents completed training with confidence in performing ATI, only half felt that their current practice and continuing medical education allowed them to maintain adequate skills. This is consistent with the previously observed finding that regular performance of ATI is required to support training and to maintain the skills of senior anaesthetists. 22 Among the respondents there was strong support for ATI becoming one of ANZCA’s mandatory core skills; it follows that there was also strong interest in ongoing training in ATI (89%).
The majority of respondents felt that participation in an on-call roster required proficiency in ATI; in contrast there was a mixed response to the concept of an on-call airway service for complex cases or ATI. This suggests that practitioners prefer autonomous practice over referrals to a dedicated difficult airway service. Consequently, the importance of maintaining individual competence in ATI is highlighted. On-call airway services have been established in centres with high-volume subspecialty head and neck practice. 23 The broad case mix typically observed in Australian and New Zealand hospitals combined with areas of geographical isolation and workforce shortage might explain the lack of support for such a service in our setting.
The current ANZCA volume of practice requirements for trainees requires performance of only five awake fibreoptic bronchoscopies or intubations in the course of their training. 24 This conservative requirement may be realistic in the current environment but is likely insufficient to achieve proficiency. In our survey, 93% of respondents considered that more than five ATIs were required for independent competence. Defining skill acquisition is complex and learners might progress at variable rates.25,26 It has been suggested that competence with a flexible bronchoscope can be achieved with 10 tracheal intubations in induced patients, and a further 15–20 in awake patients with normal airway anatomy, with 100 or more cases of bronchoscopic ATI required to become expert. 27 While simulated practice can also improve dexterity, 28 there are more components (e.g. topical airway anaesthesia, use of systemic medications) required to successfully perform an ATI than mere competence with a flexible bronchoscope.
Attaining and sustaining proficiency in ATI in an environment where it is practised less frequently is a challenge for individual clinicians and for the specialty of anaesthesia as a whole. Development of a personal and institutional focus on the value of proficiency in ATI is important. This enables clinicians to be proactive in skill development and to recognise and utilise appropriate opportunities for ATI.22,26 Support staff become used to ATI as a routine aspect of anaesthesia care such that it can be performed efficiently, smoothly, with minimal patient discomfort and as an opportunity to train members of their team. 29
There is a need for easily accessible regular multidisciplinary training and resources that encompasses all aspects of ATI, including indications, consent, equipment, endotracheal tube choice, bronchoscopy and videolaryngoscopy skills, ergonomics, topicalisation, techniques to optimise successful tube passage, oxygenation, judicious use of systemic medications, troubleshooting techniques and contingency plans. 1 In establishing ATI training programs, educators should acknowledge the progression from learning to practice to performance in real-world conditions and finally onto teaching of the next generation. 30 The development of such training could include the advice of local airway experts, supported by established guidance, for example, that offered in the Difficult Airway Society ATI guidelines with the accompanying cognitive aid, infographics and checklist. 1
Training in ATI can be part of an airway curriculum for anaesthesia trainees in teaching hospitals 31 and, equally, should be available to specialists to maintain skills. Notably, institutional culture did not appear to contribute to the avoidance of ATI in this survey. Accordingly, several practical options for training and maintenance of competence in ATI are proposed: workshops and continuing medical education courses;26,32 low- and high-fidelity medical simulators, ideally available continuously for skill maintenance and development and for practice immediately before performing ATI;26,28,33,34 rotations in specialised units where there is regular high-volume ATI; integrating required skills with other procedures, for example, topicalisation and bronchoscope manipulation during diagnostic bronchoscopy lists and in ear, nose and throat clinics, during thoracic cases, hands-on experience with a bronchoscope can occur during confirmation of double-lumen tube or bronchial blocker placement, 32 use of the flexible bronchoscope and videolaryngoscopy devices (and their combined use) on induced patients in specifically allocated lists will help development and maintenance of skills with these devices.1,22,26,35,36 When feasible, encouraging the inclusion of a second consultant anaesthetist in addition to trainees to increase exposure to ATI; and quality assurance programs should consider keeping track of a department’s use of ATI, and also monitor any recorded difficulties encountered in performing the procedure—this will help identify areas for system improvement and training.
Conclusion
The survey results highlight a concerning disparity between the skill expectations within the anaesthesia profession and the training and exposure currently provided. The present challenge of reduced exposure to ATI poses a significant risk of skill deterioration among anaesthetists. To ensure patient safety, adoption of a multifaceted approach that integrates the best available guidance and utilises a diverse array of teaching tools is imperative. Addressing this gap will ensure that anaesthetists receive the necessary training and exposure to maintain and enhance their skills in ATI.
Supplemental Material
sj-docx-1-aic-10.1177_0310057X251397168 – Supplemental material for Awake tracheal intubation: A survey of practices, barriers and skills maintenance
Supplemental material, sj-docx-1-aic-10.1177_0310057X251397168 for Awake tracheal intubation: A survey of practices, barriers and skills maintenance by Andrew Downey, Chad Oughton, Tim Makar, Yasmin Endlich, Jonathan M Graham, Louise Ellard and John A Law in Anaesthesia and Intensive Care
Footnotes
Acknowledgements
The authors would like to acknowledge the staff of the ANZCA Library for their assistance with performing the systematic review of the literature. The support of the anaesthetic departments at Peter MacCallum Cancer Centre and the Austin Hospital are acknowledged for their role in the pilot.
Author Contribution(s)
Declaration of conflicting interests
The authors have no conflicts of interest to declare.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Supplemental material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
