Abstract
Airway management in critically ill patients remains an essential component of intensive care medicine and is associated with significant patient risks. We conducted a 6-year follow-up survey among intensive care unit (ICU) medical staff in Australia and New Zealand (ANZ) from June to September 2024 which explored current ICU airway management practices and compared these with our previous survey in 2019. Among 211 respondents (26% response rate), 79.6% were male and 70.6% were intensivists. Video laryngoscopy (VL) availability increased significantly to 100% (P=0.005). VL was the first-line choice for 82% of respondents (adjusted odd ratio (aOR) = 7.41; 95% confidence interval (CI): 4.33 to 12.67) and there was an increase in intubation checklist usage (aOR = 3.32; 95%CI: 1.88 to 5.86). The use of ketamine for induction doubled (33.2% versus 15.3%; aOR = 2.96; 95%CI: 1.65 to 5.31), and rocuronium (89.6%) was the most used neuromuscular-blocking agent. Only 15.1% consistently used a bougie or stylet, and half used bag–mask ventilation post-induction and prior to intubation. Only 54% of respondents were familiar with any guidelines, and less than half of respondents (46.4%) reported having any formal airway management training in the past 3 years. A majority (81%) supports mandatory airway management continuing professional development (CPD) for fellows of the College of Intensive Care Medicine of ANZ (CICM). Despite improvements in airway management among ANZ ICU clinicians, notable gaps persist between current practices and recent trial evidence and guideline recommendations, supporting the need for airway management CPD for CICM fellows.
Introduction
Airway management in critically ill patients remains an essential and defining component of intensive care medicine.1,2 Notably, airway management in critically ill patients is associated with significant risks such as severe hypoxaemia, severe hypotension, aspiration, brain injury and death due to a combination of patient, staff and environmental factors.2–5 Intensivists must therefore be adept at airway management in the critically ill to minimise these risks in this particularly vulnerable patient cohort. An important goal for intensivists should always be to maximise first-pass intubation success and avoid complications such as severe hypoxaemia and hypotension.2,6,7
Two recent systematic reviews confirm that video laryngoscopy (VL) improves glottic views, reduces failed attempts and complications such as severe hypoxaemia and has seen increased use, particularly accelerated during the COVID-19 pandemic.8,9 These findings were further supported by a recent large randomised–controlled trial (RCT) demonstrating the clinical benefits of VL. 10 Other RCTs established benefits of several specific interventions including pre-oxygenation with non-invasive ventilation (NIV), bag–mask ventilation (BMV) during the apnoeic phase post-induction, and the use of adjuncts such as an intubating stylet or bougie to maximise first-pass intubation success.10–14 Results from these studies have also been incorporated into international guidelines for airway management in the critically ill. 15 It is unknown whether the results of recent RCTs and published guidelines have translated into clinical practice among intensive care unit (ICU) medical staff in Australia and New Zealand (ANZ).
Our practice survey of airway management in ANZ ICUs in 2018 demonstrated low utilisation of several of these interventions. However, the COVID-19 pandemic brought a rapid and widespread shift in ICU airway practices, most notably the routine adoption of VL, updated protocols and enhanced infection control measures. Given the scale and speed of these changes, a timely re-evaluation was warranted. Hence this study, aimed to re-assess current airway management practices and preferences and compare these with the 2018 survey in the context of recent RCTs and guidelines pertinent to airway management in the critically ill. 16
Methods
Study design and participants
The study was a cross-sectional, web-based survey using a questionnaire sent to ICU medical staff in ANZ. A website link to the survey was sent to all medical members of both the College of Intensive Care Medicine of ANZ (CICM) and the Australian and New Zealand Intensive Care Society (ANZICS). ANZICS distributed the survey as a weblink to their medical members, both ICU consultants and trainees, with a reminder sent 2 weeks after the initial distribution. At the time of the survey, the mailing list included 825 ANZICS medical members. The survey was also distributed by CICM. CICM had the web link to the survey in their respective monthly newsletters, which were emailed to all ICU consultants and trainees. The website link provided a brief description of the survey, study aims, ethics approval details and contact details for the investigators. The survey utilised the SurveyMonkey platform (SurveyMonkey™, San Mateo, California, USA). The survey was open from June 2024 until September 2024. Survey responses were collated in October 2024 and subsequently analysed.
Survey instrument
The survey design and specific questions were prepared by the investigators after a review of the existing literature. The survey was piloted among senior colleagues, and changes to question syntax and content were made after the pilot period. The survey was nearly identical to our 2018 survey to allow for comparisons. Survey questions included respondent demographics, including level of experience, additional fellowship training with other colleges and their experience in anaesthesia. Participants were also asked about their access to and use of VL, intubating stylets and bougies, use of NIV for pre-oxygenation, as well as intubation checklists, continuous waveform capnography and their choice of induction and neuromuscular-blocking drugs. One question from the previous survey was deleted (i.e. ‘Do you believe that having airway management guidelines for critically ill patients in Australia and New Zealand would improve the safety and quality of intubations performed in ICU?’) because guidelines have been published since the 2018 survey. 17 Four new questions were also added: (1) Did your departmental/organisational or personal practices relating to airway management in the ICU change due to the COVID-19 pandemic? How commonly do you use the following in your ICU: (2) pre-induction fluid bolus? (3) pre-induction vasopressor infusion? and (4) peri-induction vasopressor (e.g. metaraminol boluses)? The 2024 and 2018 surveys are presented in Supplemental Table 1. Apart from the demographic information, the following three domains were chosen for the survey: (1) the respondents’ airway practices and the equipment that was readily available and used in the ICUs where the respondents primarily work; (2) organisational aspects; and (3) suggestions for training airway practice to maintain competency recommendations.
Statistical analysis
Data analysis consisted primarily of descriptive data, comparing responses from the 2024 survey with our previous survey in 2018. 16 Survey responses are reported as percentages of valid responses. Descriptive statistics for normally distributed data are presented using the mean and SD, while median and interquartile range (IQR) are used to describe non-normally distributed data. The responses for the 2024 survey on a five-point Likert scale (‘strongly disagree’, ‘disagree’, ‘neutral’, ‘agree’ and ‘strongly agree’) are graphically presented in the supplemental material. To simplify the comparative analysis between the 2018 and 2024 surveys, the five-point Likert scale responses were dichotomised, with ‘strongly disagree’, ‘disagree’ and ‘neutral’ being categorised in one group and ‘agree’ and ‘strongly agree’ in another. Similarly, ‘always used’ and ‘used the majority of the time’ were categorised in one group and ‘never used’, ‘sometimes used’ and ‘only used when necessary’ were categorised into another group in relation to respondent airway management preferences. If there were changes in practice between the 2018 and 2024 survey responses, multivariable logistic regression analysis was conducted to account for statistically significant differences in respondent characteristics or univariable analysis, adjusted for male doctors, their level of experience and ICU type. The interaction between variables and the collinearity between confounders were assessed with the variance inflation factor. The results were presented as odds ratio (OR) with 95% confidence intervals (95%CI) with a two-tailed P value of less than 0.05 considered significant. We also investigated the consistency of current practice with results from recent RCTs and guidelines and presented that descriptively. We performed the data analysis using IBM SPSS Statistics (version 29). Missing data was handled by a case-wise deletion in the individual analyses. The free-text comments were qualitatively and thematically analysed.
Ethical considerations
Monash Health Office for Research and Governance approved conducting this study under the low-risk/quality assurance pathway (ERM reference number: 105549, Monash Health reference number: RES-24-0000-064B). Participation was voluntary and consent was implied with the completion of the survey. No incentives were offered to participants.
Results
A total of 262 of the ANZICS members (825 active medical members) responded to the survey (response rate 32%). Participants who worked exclusively in the paediatric ICU and partially completed surveys were excluded. After exclusions, 211 complete survey responses were included for analysis (response rate 26%, Supplemental Figure 1).
Demographics
Respondent demographics are shown in Table 1. In the 2024 survey, 79.6% of respondents were male, 88.2% of respondents were based in tertiary or metropolitan ICUs, and 50.2% of respondents were based in Victoria. Only 8.5% of respondents were based in New Zealand. A total of 70.6% of respondents were consultant intensivists and 16.1% of respondents also held fellowship of the Australian and New Zealand College of Anaesthetists. Apart from more respondents from Victoria (P <0.001) and a lower proportion of physician intensivists (10.9% versus 21.5%; P=0.005) in 2024, there were no other baseline differences among the respondents when compared with the 2018 survey.
Characteristics of survey respondents included in the present study.
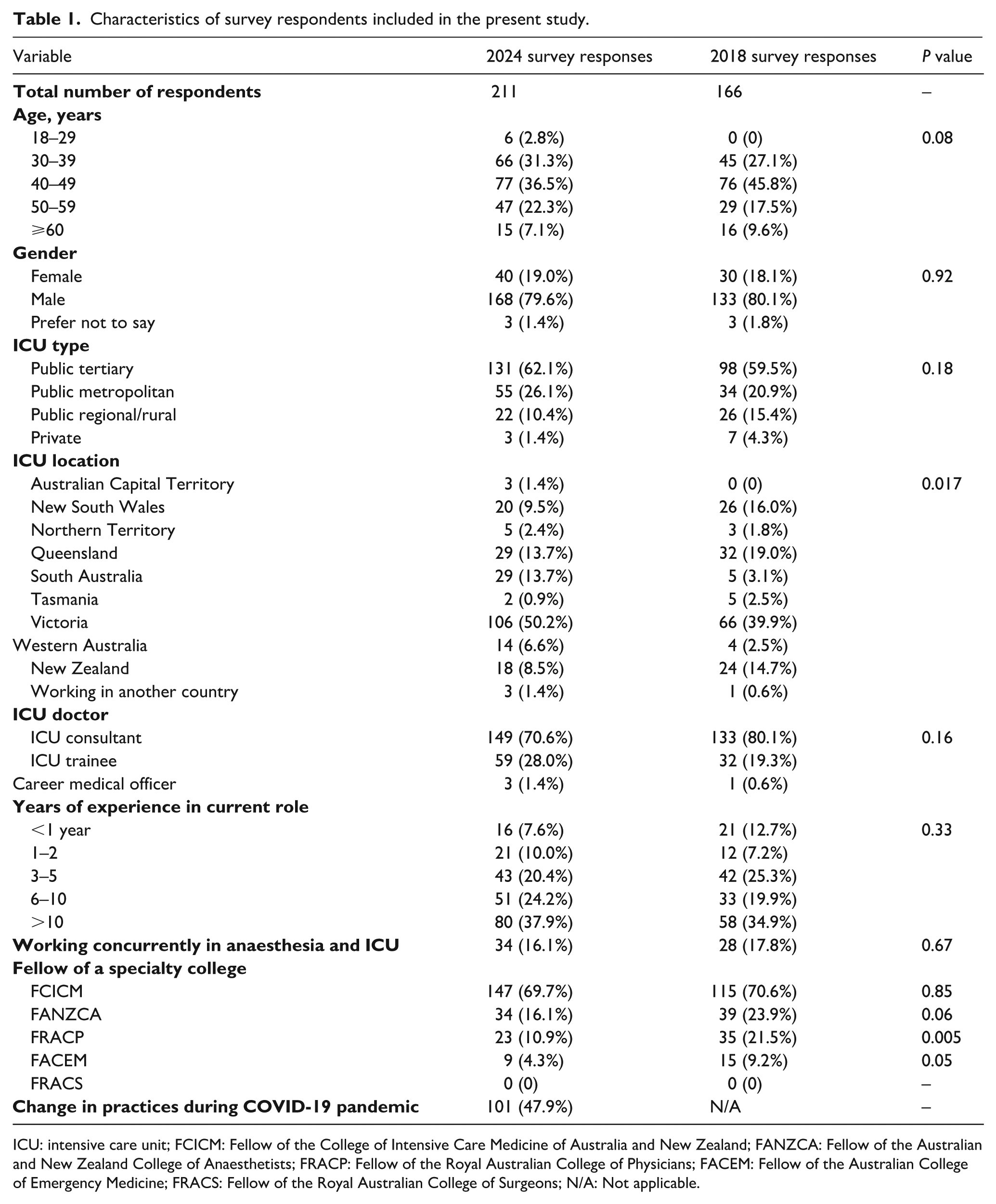
ICU: intensive care unit; FCICM: Fellow of the College of Intensive Care Medicine of Australia and New Zealand; FANZCA: Fellow of the Australian and New Zealand College of Anaesthetists; FRACP: Fellow of the Royal Australian College of Physicians; FACEM: Fellow of the Australian College of Emergency Medicine; FRACS: Fellow of the Royal Australian College of Surgeons; N/A: Not applicable.
Airway practices
The median number of intubations performed per annum by respondents was lower in 2024 when compared with the 2018 survey (8 (IQR 5–10) versus 10 (IQR 5–15); P=0.004; Figure 1). Similarly, the median number of intubations supervised by respondents was lower in 2024, when compared with 2018 (10 (IQR 5–20) versus 20 (IQR 10–25); P <0.001; Figure 1). The changes in equipment availability and airway practices are described in Tables 2 and 3, and the multivariable logistic regression adjusted for differences in respondent characteristics is presented in Figure 2 and Supplemental Tables 2–7. Respondents to the 2024 survey reported an increase in the availability of VL (100% versus 96.3%, P=0.005), hyper-angulated VL (93.4% versus 79.8%, P <0.001), equipment for the scalpel-bougie-tube cricothyroidotomy technique (93.8% versus 83.4%, P=0.001) and second-generation laryngeal mask airways (LMA) (95.3% versus 71.8%, P <0.001). Respondents also reported a decrease in the availability of needle cricothyroidotomy kits (73.0% versus 84.0%, P=0.011) compared with the 2018 survey. Although propofol continued to be the preferred primary induction agent, respondents opined that the use of propofol in 2024 was significantly lower than in 2018 (51.2% versus 67.5%, P <0.001; adjusted OR (aOR) = 0.46; 95%CI: 0.29 to 0.74). Concurrently, there was an increase in the use of ketamine in 2024, when compared with 2018 (33.2% versus 15.3%, P <0.001; aOR = 2.96; 95%CI: 1.65 to 5.31), as the primary induction agent. Rocuronium was reported as being the most preferred neuromuscular-blocking agent during intubation in 2024, when compared with 2018 (89.6% versus 57.7%, P <0.001; aOR = 8.61; 95%CI: 4.58 to 16.20).
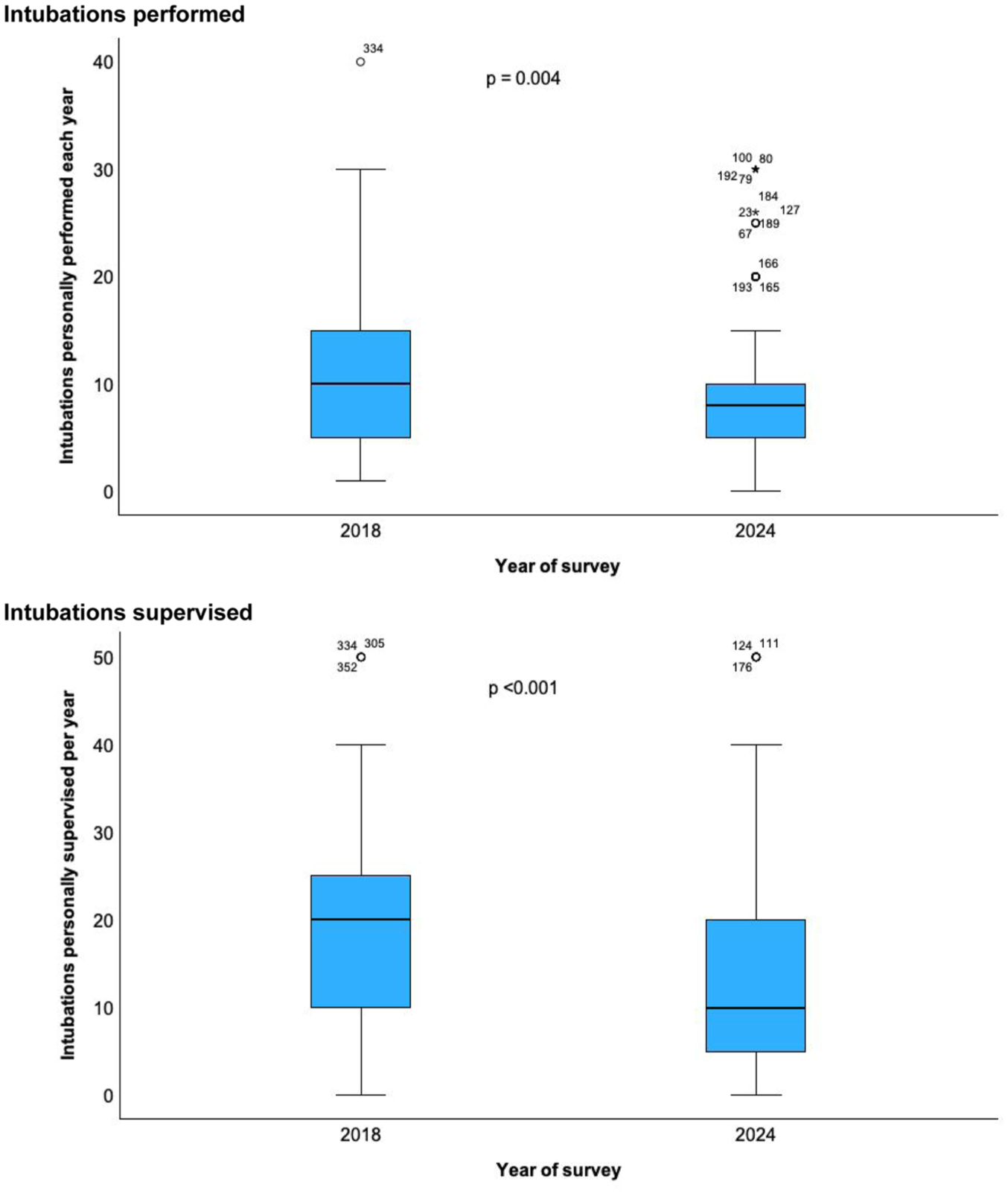
Intubations performed or supervised each year in the intensive care unit.
Available airway equipment in the intensive care unit.
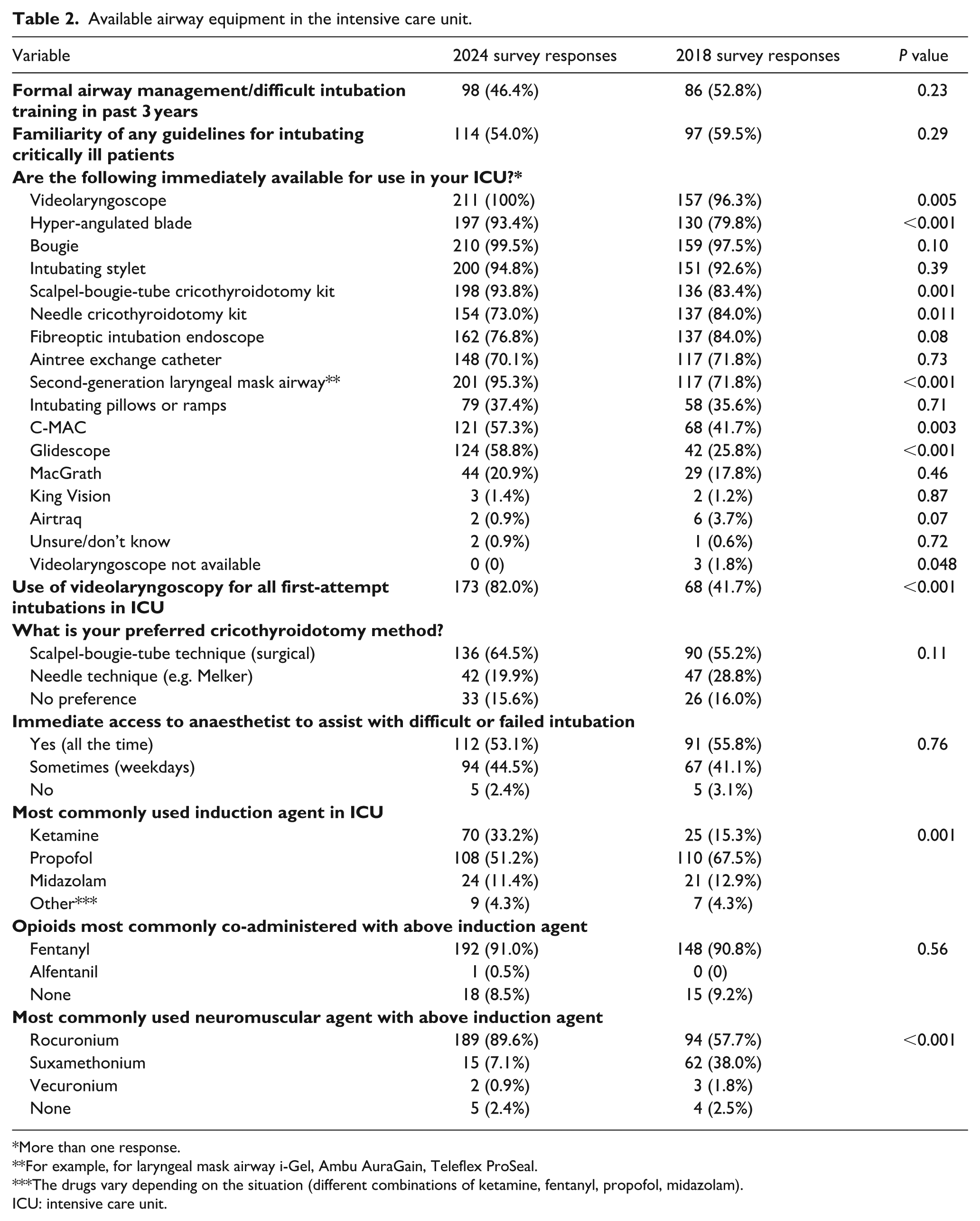
More than one response.
For example, for laryngeal mask airway i-Gel, Ambu AuraGain, Teleflex ProSeal.
The drugs vary depending on the situation (different combinations of ketamine, fentanyl, propofol, midazolam).
ICU: intensive care unit.
Airway practices in the intensive care unit.
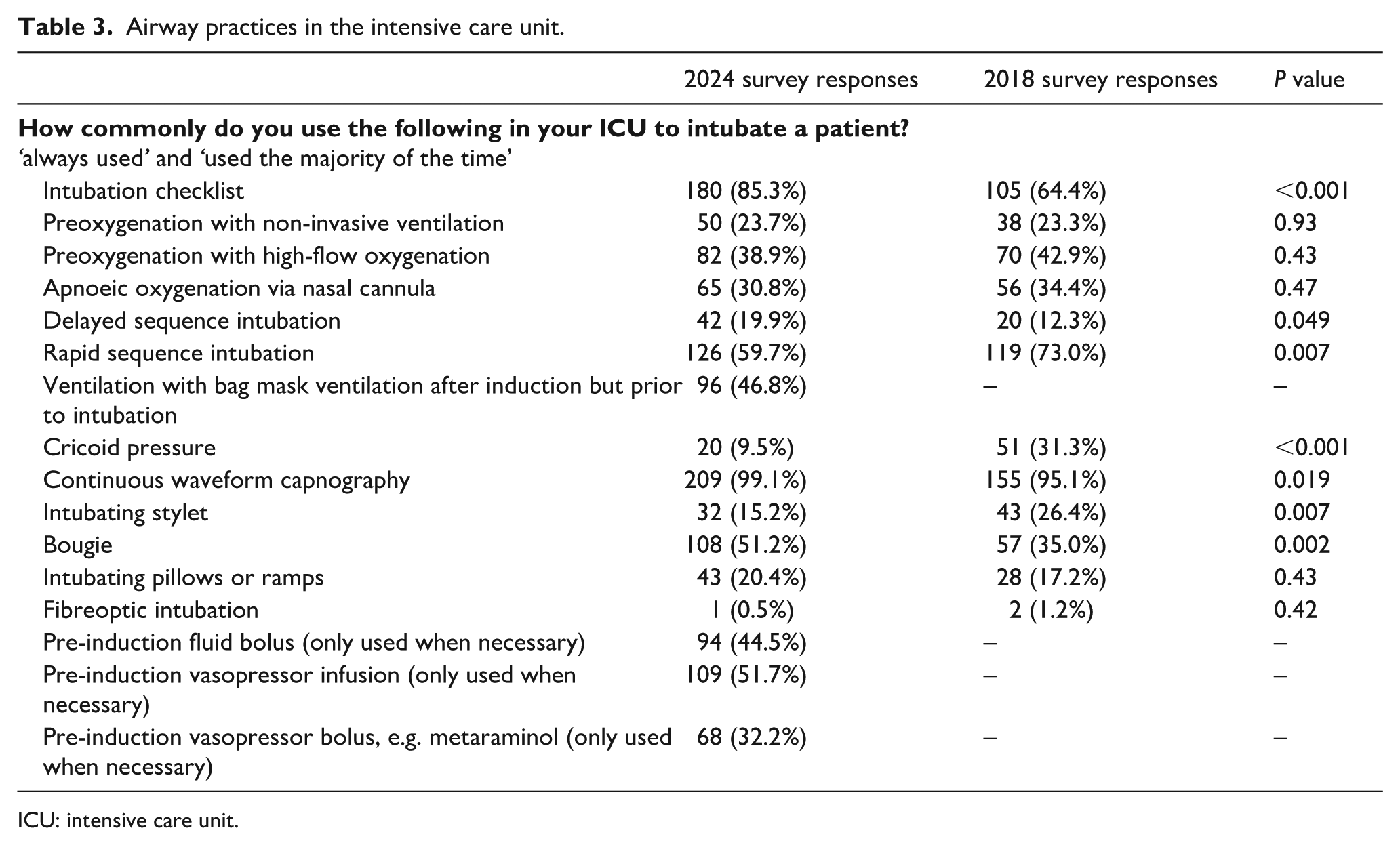
ICU: intensive care unit.
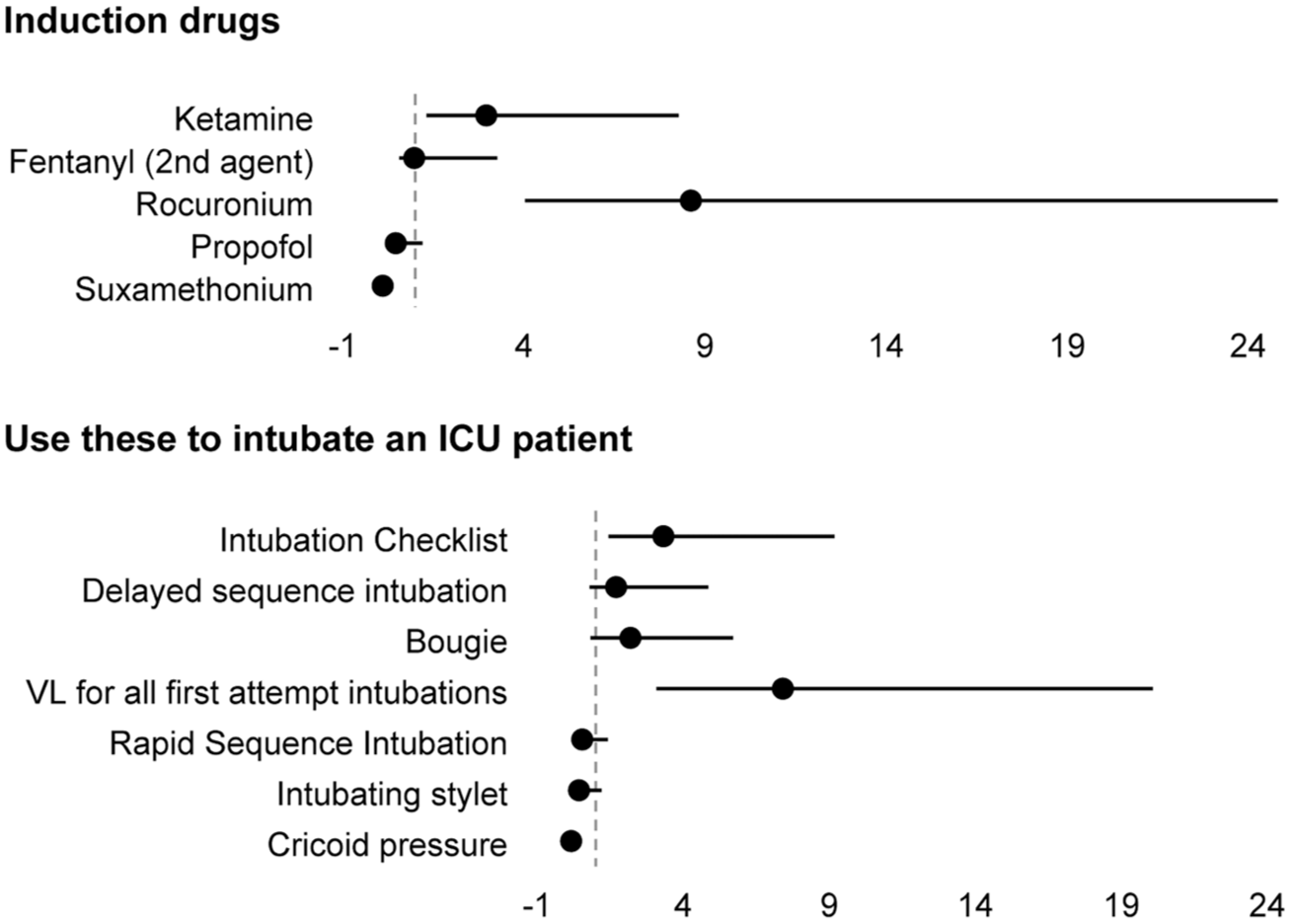
Multivariable logistic regression for the changes in airway practice in 2024, adjusting for age, sex, intensive care unit (ICU) doctor type, years of experience in current role, ICU category, ICU location and working concurrently in anaesthetics and ICU. Please refer to Supplemental Tables 2–7.
The use of VL for all first attempts at intubation nearly doubled (82% versus 43%, aOR = 7.41; 95%CI: 4.33 to 12.67). There was an increase in the use of intubation checklists (85.3% versus 64.4%, P <0.001; aOR = 3.32; 95%CI: 1.88 to 5.86), delayed sequence intubation (19.9% versus 12.3%, P=0.049; aOR = 1.70; 95%CI: 0.91 to 3.15), continuous waveform capnography (99.1% versus 95.1%, P=0.019; aOR = 12.61; 95%CI: 1.28 to 124.43) and the use of a bougie (51.2% versus 35.0%, P=0.002; aOR = 2.19; 95%CI: 1.37 to 3.52) in 2024 when compared with 2018. Conversely, there was a decrease in the use of rapid-sequence intubation (59.7% versus 73.0%, P=0.007; aOR = 0.54; 95%CI: 0.34 to 0.88), cricoid pressure (9.5% versus 31.3%, P <0.001; aOR = 0.16; 95%CI: 0.08 to 0.31) and intubating stylets (15.2% versus 26.4, P=0.007; OR = 0.43; 95%CI: 0.23 to 0.77) in 2024, when compared with 2018.
When we investigated the consistency of current practice with results from recent RCTs and guidelines based on the Likert scale responses, we observed that only 15.1% of respondents reported using an intubating bougie or stylet as ‘always’. The use of NIV for pre-oxygenation remained low (23.7%) and positive-pressure ventilation with BMV during the apnoeic period between induction and intubation was used by approximately half of the respondents (46.8%) and used as ‘always’ by only 11.8%. A total of 18.5% of respondents reported using a pre-induction fluid bolus, and a pre-induction vasopressor infusion or bolus was used by 15.6% and 31.2% of respondents, respectively. The scalpel-bougie-tube technique remained the preferred method for cricothyroidotomy (64.5%).
Airway training and guidelines
Only 54% of respondents reported having familiarity with any guidelines for airway management in the critically ill, and only 46.4% of respondents reported having any formal airway management training in the past 3 years. Both these were no different to the 2018 survey (Table 2). There was strong support for mandatory airway management continuing professional development (CPD) for CICM fellows, with 80.6% of respondents ‘agreeing’ or strongly agreeing’, which is consistent with the 2018 results. More than half of the respondents (52.6%) indicated that mandatory airway management should occur every 3 years (Table 4).
Airway training and suggested recommendations.
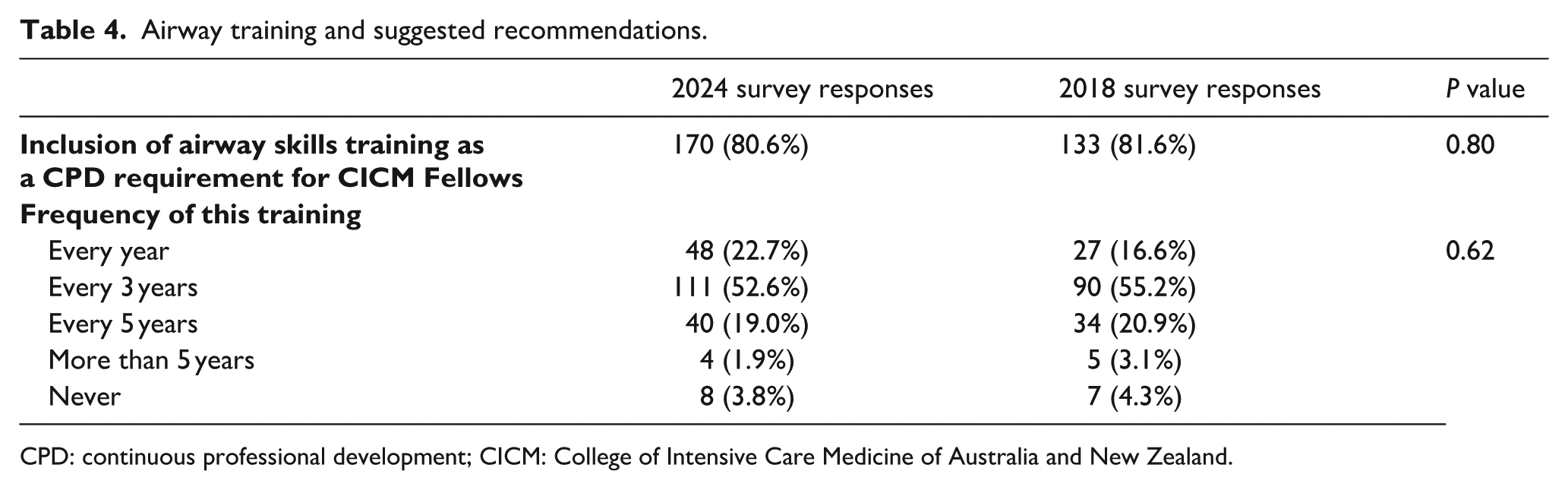
CPD: continuous professional development; CICM: College of Intensive Care Medicine of Australia and New Zealand.
Discussion
Summary of key findings
Our results from the 6-year follow-up survey demonstrate important changes in airway management practices in ANZ ICUs over the period from 2018 to 2024, most of which is reassuring. First, ANZ ICU medical staff report performing and supervising fewer intubations in the ICU in 2024 when compared with 2018. Second, there is a reported increase in the availability and use of VL and hyper-angulated VL. Third, there is a reported increased use of intubation checklists, delayed sequence intubation and bougies, with a decreased use of rapid-sequence intubation, cricoid pressure and intubating stylets. Fourth, most respondents reported using VL for all first attempts at intubation. Fifth, ketamine and rocuronium are reportedly more frequently used as induction and neuromuscular-blocking agents, respectively. However, our results also indicate that there are several important safety and quality gaps between current airway management practices in ANZ ICUs and evidence from large RCTs and national and international guidelines. Finally, there is strong support for mandatory airway management CPD for CICM fellows every 3 years.
Comparison with previous literature
Compared with the 2018 survey, there is a reduction in the observed intubation volume of practice; lower than previously published.16,18 The reasons are likely to be multifactorial but may relate to an increased use and efficacy of NIV and high-flow nasal oxygen which decrease the need for intubation and invasive mechanical ventilation in patients with respiratory failure.19–22 However, there is no established guideline recommending a specific minimum number or frequency of intubations that must be performed or supervised to maintain the necessary skills for intubations in intensive care.
The use of VL for first intubation attempts in ANZ ICUs has nearly doubled, likely driven by increased availability, familiarity and clinician confidence, due to the COVID-19 pandemic, in the ICU airway management practices across ANZ. The 2023 DEVICE trial, involving 1417 critically ill patients across 17 ICUs and emergency departments, showed a VL increased first-pass success to 85.1% compared with 70.8% with direct laryngoscopy, a significant improvement (absolute risk difference 14.3 percentage points; 95%CI 9.9 to 18.7; P <0.001). 10 While VL did not demonstrate a mortality benefit, it enhanced glottic view and reduced oesophageal intubation rates with the knowledge that repeated intubation attempts are linked to increased morbidity and mortality.6,7 The benefits of VL have also been reflected in the recently published guidelines from the Society of Critical Care Anaesthesiologists (SOCCA) Physiologically Difficult Airway Taskforce and multiple recent systematic reviews and meta-analyses.9,15,23 The increasing use of VL on first attempt at intubation in ANZ ICUs is encouraging. Apart from specific clinical scenarios such as major airway bleeding, high secretion loads or distorted anatomy, where direct laryngoscopy may be more effective, as a craft group ICU medical staff should aspire to use VL for all intubations in critically ill patients.
Recent multicentre clinical trials such as PreVent and PREOXI demonstrated significant reductions in hypoxaemia in the peri-intubation period for critically ill patients who received pre-oxygenation using BMV positive-pressure ventilation and NIV, respectively.13,24 Despite the evidence, the respondents in our study reported pre-oxygenation using BMV positive-pressure ventilation and NIV prior to intubation as ‘always used’ or ‘used the majority of the time’ by only 46.8% and 23.7%, respectively. An increased use of positive-pressure BMV during the apnoeic phase of induction and the use of NIV for pre-oxygenation therefore represent another opportunity for ICU medical staff to improve the safety and quality of care provided to patients.
Despite the high-quality evidence that the use of an intubating stylet or bougie improves first-pass intubation success in critically ill patients, a bougie or stylet was ‘always’ used on the first attempt by only 15.1% of respondents in our survey.11,12,14 This represents another opportunity for ANZ ICU medical staff to improve first-pass intubation success in ICU patients and minimise complications and improve safety and quality for patients. Moreover, the proactive first-line use of these techniques is also recommended by the 2024 SOCCA Physiologically Difficult Airway Taskforce. 15
Our study has also demonstrated significant changes in the choice of primary induction and neuromuscular-blocking agents used for airway management in the ICU since our 2018 survey. Although propofol remains the preferred induction agent, its preference by clinicians dropped in 2024. In contrast, the preference for ketamine as the primary induction agent has doubled. Although guidelines recommend using haemodynamically stable induction agents such as ketamine and etomidate to minimise hypotensive effects during intubation in critically ill patients, robust RCT data are lacking. 15 Propofol is associated with the highest risk of peri-intubation hypotension, which correlates with increased ICU and 28-day mortality. 25 Ninety percent of the ANZ ICU clinicians reported an increased use of rocuronium with a corresponding reduction in suxamethonium use. While rocuronium does not improve outcomes for intubated critically ill patients, its longer action duration supports optimal conditions for multiple intubation attempts, BMV, LMA insertion or front-of-neck access is required. 26 Additionally, its anaphylaxis risk is comparable with suxamethonium, without the associated hyperkalaemia and malignant hyperthermia risks. 27
Intubation checklists are a well-recognised safety intervention shown to reduce complications and standardise practice during high-risk procedures such as tracheal intubation in critically ill patients. 28 Our survey demonstrated a modest but encouraging increase in their uptake since 2018. However, despite widespread endorsement in guidelines, their consistent use remains variable. Common barriers include perceived time constraints, lack of integration into local workflows and variable staff training or buy-in. To improve uptake, checklists should be embedded into routine practice through simulation training, electronic prompts and leadership advocacy. Promoting a culture that values structured preparation, particularly during high-stress scenarios, may further normalise checklist use and enhance patient safety.
Another important finding in our study relates to clinician familiarity with guidelines and specific airway management training. Despite being an essential component of ICU practice and associated with significant patient risks, it is particularly concerning that only 54% of respondents have familiarity with any guidelines for airway management in the critically ill. This is despite the publication of multiple international guidelines in the past 6 years since our last survey and more locally, the Safe Airway Society of ANZ guidelines, which were published during the COVID-19 pandemic.17,26,29–31 It is also concerning that only 46.4% of respondents have completed any formal airway training in the past 3 years despite local evidence that airway training courses improve ICU clinician confidence. 32 This, combined with the lower volume of airway practice found in our survey, poses a significant safety concern. There is an opportunity for ICU clinicians and CICM fellows to improve their knowledge and familiarity with the guidelines so that they are confident and equipped to provide airway management to the critically ill to the highest standard and in concordance with the evidence base. 32 Based on the study results, it is essential to mandate airway management CPD for all CICM fellows and be renewed every 3 years, and there now appears to be sustained support for this.16,18 Enhancing awareness of formal guidelines, alongside structured backup planning and cognitive preparedness, is essential to maintaining airway management competency across the specialty.
Clinical implications
Despite advancements in airway management across ANZ, gaps remain between existing high-quality guidelines, RCT evidence and actual practices in ICU settings such as the underutilisation of VL for all attempts at intubation, the limited use of a bougie or stylet and the limited use of BMV during the apnoeic phase of induction.10,12–15 Notably, only half of the respondents were aware of any relevant guidelines. The new mandatory airway management CPD by CICM, starting in 2025, aims to bridge these gaps. To sustain and enhance compliance with best practices, we must conduct follow-up surveys every 3–5 years, ensuring continual improvement in airway management. The results from two surveys also advocate for setting up a prospective registry to delve deeper into ICU airway practices in ANZ. Such a registry would help monitor future trends and aim to bridge the current safety and quality gaps.
Strengths and limitations
This study has several strengths in that it provides a holistic overview of airway management in ANZ ICUs incorporating organisational factors, individual practices and educational considerations in the context of recent relevant studies and guidelines. We have uniquely been able to document important practice changes over time and identify patient-centred opportunities for practice improvement. Our multivariable analysis also accounts for changes in respondent characteristics. However, important limitations need to be acknowledged. First, the 26% response rate may restrict the generalisability of the findings, and this response rate is likely inflated due to the survey being made available to both ANZICS and CICM medical members. However, 262 remains a large survey sample size. Second, there was relatively low representation from trainees and no representation from nurses who may have provided additional insights. Third, there was a disproportionate number of responses from Victorian ICUs, which may reduce the generalisability of the findings across all regions of ANZ. This regional skew could reflect local engagement or distribution factors and may introduce bias in representing nationwide practice patterns. Fourth, inherent to any survey, responses were self-declared statements without independent corroboration and recall bias may potentially affect the reliability of the data. Fifth, there may also be reporting bias by non-random participant selection, especially from personnel with a special interest in airway management.
Conclusion
This survey of ANZ ICU medical staff found that there have been several evidence-based practice improvements such as the increased availability and use of VL, checklists and delayed sequence intubation. However, significant safety and quality gaps remain between current ANZ ICU medical staff practices and evidence from recent RCTs including the first-line use of VL, the use of BMV post-induction but prior to intubation and using a bougie or stylet during the first attempt at intubation. Respondents continue to support mandatory airway management CPD for CICM fellows.
Supplemental Material
sj-docx-1-aic-10.1177_0310057X251396401 – Supplemental material for A practice survey of airway management in Australian and New Zealand intensive care units: A 6-year follow-up study
Supplemental material, sj-docx-1-aic-10.1177_0310057X251396401 for A practice survey of airway management in Australian and New Zealand intensive care units: A 6-year follow-up study by Michael Toolis, Alastair Brown and Ashwin Subramaniam in Anaesthesia and Intensive Care
Footnotes
Author contributions
Declaration of conflicting interests
The authors declared the following potential conflicts of interest with respect to the research, authorship, and/or publication of this article: Ashwin Subramaniam is on the Editorial Board of Critical Care and Resuscitation and Michael Toolis is on the Clinical Council for the Safe Airway Society of Australia and New Zealand.
Funding
The authors received no financial support for the research, authorship and/or publication of this article.
Supplemental material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
