Abstract
Over the last decades public discussion of opioids has changed radically.
Introduction
Unfortunately […] opium has gathered a disgraceful public image since Victorian times.1
2018 data shows that every day, 128 people in the United States die after overdosing on opioids. The misuse of and addiction to opioids […] is a serious national crisis that affects public health as well as social and economic welfare.2
There is a war on opioids in this country [USA].3
Pain has a long history of relative neglect in the medical disciplines.4 Both acute and chronic pain have long been treated with opium and more recently opioids, whose use is more commonly accepted in post-surgical pain management, cancer, and end-of-life pain. Opioids have a more controversial role in treating other kinds of chronic pain, especially chronic non-cancer pain (CNCP). However, the last three decades have seen a major shift around chronic pain. It has finally been fully recognised in ICD-11, the
Opioids: Chronology and attitudes
The history of opioids and ‘painkillers’ has been comprehensively covered elsewhere.6–9 For our present purposes we need only document selected indicative dates and events to identify the major chronological moments for the language analysis to follow.
The various opium-related substances all began as medicines, narcotics, soporifics and analgesics, and as early means of anaesthesia.10 The medical history of opium goes back at least to the ancient Sumerians in the 5th millennium BC, and has long been established in the Western world, for instance in the form of laudanum (opium mixed with alcohol) used by the physician Paracelsus in the 16th century (c). The English poet Coleridge started taking laudanum for pain, and became addicted. De Quincey’s
The medical use of opioids has been closely related to the history of pain. Bourke documents the progression of pain from ‘prayer to painkillers’, as pain has been gradually passed from being a matter of theology and divine punishment to a symptom susceptible to human intervention and substantial control.4 Most recently pain has become recognised not merely as a symptom of other medical dysfunction, but as a medical condition in its own right, especially in CNCP. This reconceptualisation is captured in the July 2020 revision of the definition of pain by the International Association for the Study of Pain.12 Such a revision, however, would not have been possible without a major shift of perspective on CNCP in the 1990s.
The recent history of pain in medicine, public health and ‘big pharma’ has been dominated by developments in the USA. The gathering realisation that pain was being medically under-treated was marked by the 1996 declaration by the President of the American Pain Society that pain is the ‘fifth vital sign’, a body condition ranking with body temperature, blood pressure, heart rate and breathing, as a key indicator to be checked by physicians in medical examinations. This declaration was shortly followed in 2000 by the introduction of new pain management standards by the Joint Commission on the Accreditation of Healthcare Organizations, which relaxed key restrictions on physicians in the prescribing of pain-controlling drugs, thereby creating another problem.13
This relaxation included opioids. During the 1990s a number of large pharmaceutical companies, mainly in the USA, developed and aggressively marketed new ranges of opioid drugs for the treatment of pain, especially targeted at the market for non-cancer pain. This advertising push followed a long tradition of medical advertising in the USA, some of which in days of yore was doubtless closer to snake oil than the real oil,14,15 and some of which certainly contained disclosed or undisclosed quantities of substances like morphine. The 1990s opioid campaigns, however, were motivated by ambitious financial rewards. Propelled by opioids like oxycodone, now revised in a slow-release formulation called OxyContin, the drug companies spent US$3.6bn on advertising in 2006. Their primary target was physicians, who responded by writing 6.2 million prescriptions for opioids in 2002.15
The advertising tone was upbeat and reassuring, as illustrated in one OxyContin television advertisement from its multi-billion-dollar manufacturer Purdue Pharma,16 which was sent to 15,000 doctors in 1998 with reassuring endorsements from patients who reported ‘getting their lives back’ thanks to OxyContin. Other Purdue advertising material at this time claimed that less than 1% of patients who took opioids became addicted;17 van Zee claims that the real lifetime figure is between 3% and 16%,18 though firm data are still lacking. According to Manchikanti et al.,13 ‘These positions are based on unsound science and blatant misinformation, and accompanied by the dangerous assumptions that opioids are highly effective and safe, and devoid of adverse events when prescribed by physicians’.
In 2019, 71,130 Americans died from drug-related overdoses or 21.6 per 100,000 of population (the parallel figures for Australia were 2,227 deaths and 8.7 per 100,000).19,20 Eventually the situation became intolerable. Purdue Pharma was faced with multiple class actions, and eventually filed for Chapter 11 bankruptcy in 2019,21 a category of bankruptcy that dissolved the company and re-established it as a public trust to respond to claimants and their communities. From the point of view of ‘big pharma’, the first, less regulated phase of the opioid boom was over.
But much damage had already been done. The growth of opioid use has been particularly marked and disquieting in the USA, where 5% of the world’s population is now consuming 80% of the world’s prescribed opioids. As a result, the involvement of opioids was publicly declared an ‘epidemic’ by the USA’s Centers for Disease Control and Prevention (CDC).22–24 This position, and the language accompanying it, has been supported by a number of other American institutions like the Food and Drug Administration and the National Institute on Drug Abuse.2,25
This theme was picked by up the Trump administration, which declared a ‘Public Health Emergency’,2 and produced an important programme of legislation in 2018: the Substance Use-Disorder Prevention that Promotes Opioid Recovery and Treatment (SUPPORT) for Patients and Communities Act, with goals including teaching addiction medicine and standardising delivery of treatment. This initiative was endorsed by the American Society of Addiction Medicine;27 (see also Boyles28). It was reported to be the ‘single largest legislative package addressing a single drug crisis in history’.26 And the STOP Act, in full the ‘Synthetics Trafficking and Overdose Prevention Act of 2018’, included US$6bn of funding to target opioid abuse, and over US$1bn for research into opioids and pain issues.29
Epidemic, pandemic, Covid and opioids
By an unanticipated piece of serendipity, the status of the ‘epidemic of opioids’ has potentially been furthered by the pandemic of Covid-19. The world has not experienced a pandemic since the ‘Spanish Flu’ of 1918–1919, which is beyond the memory of almost anyone alive today. But Covid-19 has imposed on our lives the constraints, threats, risks and privations, and in some cases the mortality, of a genuine pandemic that crosses national boundaries. True, the opioid ‘epidemic’ is indeed more serious in the USA, where public policy allows the direct marketing of named drugs to the general public. And it is American public policy and medical bodies that have been leading the campaign against the opioid problem, which they have framed as an ‘epidemic’, since they are addressing it as an American problem, even though in geographical outreach it is an international pandemic.
Both pandemics and epidemics come equipped with metaphors: war and struggle, victors and vanquished, sacrifice, deprivation of liberty and movement, and more. In the opioid domain, different countries and jurisdictions are moving, though with only limited signs of coordination, to restrict over-the-counter access to medicines containing opioids, to tackle the problems of populations with opioid abuse, and to address the problem of illegal drug supply. The language is often aggressive and confrontational, sometimes apocalyptic. There is an undeniable stigma that is increasingly being attached to users of opioids in our communities.
But unlike Covid—at least, as Covid has played out in the USA—the opioid epidemic has not polarised the public at large. It was not politicised, at least initially. At the governmental level, judging by public statements from major parties, concern over the opioid epidemic looks to have bipartisan support. But as we shall see below, there is a major split among the medical profession, and among the people living with pain who are directly impacted by the arguments directed against opioids.
Language, denotation, connotation and values
We now turn to the resources provided by language for the formation and negotiation of themes and attitudes, both in general and with a special focus on opioids, the word
One of the fundamental burdens of this communication of attitudes falls to words, and words combined with other words. In the discipline of semantics—the study of meaning—a key distinction is drawn between denotation, or the literal, objective meaning-content of words, and their connotation, or subjective and emotional overtones. The word
The word
Language data can also be used to reveal attitudes and shifts in public discourse relating to the opioid ‘epidemic’. But more than just revealing these aspects, language use is central to the delivery and management of appropriate medical care for people in pain, and this language use around
Pain, communication and the ‘epidemic’ of opioids
The vocabulary and tone used in these messages about opioids is characterised by dramatic language:
Communicating about pain itself is seldom straightforward. Its private and subjective nature interposes problems of description and communication, for instance between patients and pain physicians. Pain is further compromised by its different interpretation in different languages and cultures. Communication—and under-communication—about pain has also only recently begun to attract serious research interest,31–34 and understanding pain talk remains an under-investigated area of medicine. This situation is substantially exacerbated by the current aggravated public controversy over opioids.
To address these issues, we will draw eclectically on a number of sources:
the medical, clinical, pharmacological and related literatures on pain and opioids; the more restricted research literature on communication and pain and opioids; the extensive material in the media, information media, social media, public policy and medical policy about opioids and their current social use, misuse and consequences; material addressing what is often referred to as the ‘epidemic’ of opioid use in our society, and policy initiatives aimed at getting control of it.
The ultimate target audience of this paper is practising healthcare professionals treating people with pain, the people in pain themselves, and those engaged in public health policy and its discussion. The goal of the paper is to help clarify the now thoroughly confused discussion space of opioids in pain medicine, and to help these stakeholders establish a basis for productive working communication about opioids and their potential role in the management of pain.
As a linguist with no medical qualifications, I take no position for or against opioids in their medical role. In the medical literature there are those who advocate for a medically supervised and controlled use of opioids for specific purposes, especially the control of cancer pain or pain in a palliative setting and select acute pain contexts; for example,35 ‘The success of carefully controlled and monitored narcotics for the benefit of cancer patients in pain spread to other problems, such as the control of postoperative pain and pain in childbirth’.
Patients undergoing such therapeutic regimens can feel ambivalent about their treatment because of the widespread negative public rhetoric about opioids. Others argue strongly against opioids. And there is a growing body of people, including medical professionals who are concerned that not enough is being done to help people with opioid problems to address them and hopefully give up their addiction. These groups are currently talking in substantially different ways. So my goal is to identify different ways of talking about opioids in contemporary public discourse, using the medical literature on opioids and attitudes towards them, together with large databases of public English; to associate these different ways of talking about opioids with different evaluations of the role of opioids in medicine and epidemiology; and to analyse how these different ways of talking influence the ability of language to capture and project different positions on the role of opioids in contemporary life.
The vocabulary of drug-related terms
In the USA, and increasingly in Australia, there is a special acronym ‘OUD’ standing for ‘opioid use disorder’, parallel to ‘AUD’ for ‘alcohol use disorder’. ‘Disorder’ refers to an illness that disrupts normal physical or mental functions. It is not inherently severely prejudicial, except insofar as it picks up the idea of departure from ‘normal’ patterns. But as we will see below in discussing stigma, OUD is involved in significant judgements of social negativity in the USA.
Before we investigate the connotation fate of
The use of drugs or opioids is accompanied by Tolerance occurs when the body shows a diminished response to a drug after continued use. Larger doses of the drug are needed to achieve the same effect as before.
Dependence (less commonly dependency) usually refers to physical dependence or reliance on a substance, accompanied by tolerance and withdrawal. But dependence need not imply addiction. A diabetic on insulin is dependent on the insulin for maintaining their levels of health, but is not addicted.
The process of ceasing to take a substance to which a person has become addicted, together with the accompanying physical and mental responses. An
In the non-therapeutic sense,
There are obvious overtones of negativity and condemnation. In order to mitigate these effects, the American Psychiatric Association, in the 5th edition of their authoritative
Opioid and substances of addiction
In terms of the English lexicon there are six typical English words of special interest in the current context.1 One, and the most recent, is
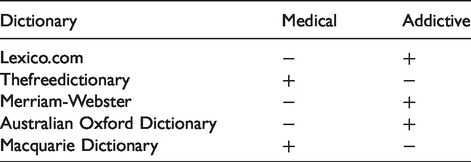
In order to reveal the current standing of these terms in relation to their medical and addictive meanings, we list their definitions in five representative current dictionaries, one British, two American and two Australian:
Dictionaries by convention list the most common current meanings first, and other meanings in decreasing order of frequency and prominence. Our goal here is to investigate whether there is any pattern in the relative ranking of medical/pharmaceutical versus addictive meanings, bearing in mind that all these terms were originally medical definitions relating to pharmacology and physiology. In the tables that follow ‘+’ indicates that there is a dictionary listing under a given category, ‘−’ that there is no listing, and ‘1’ and ‘2’ show whether a given meaning is given first place (and so is a preferred reading) or second (ranked below ‘1’).
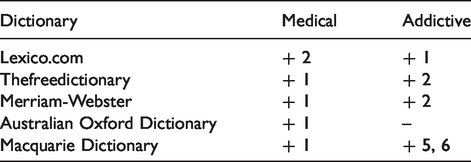

Meaning: Originally, a drug inducing drowsiness, stupor or insensibility. But nowadays the most common non-technical meaning is of an addictive drug, especially illegal, affecting mood and behaviour. Extensively used illegally.
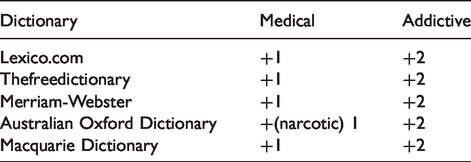
Meaning: A medication to treat disease, but also one that can affect a living organism and induce addiction. In the USA,
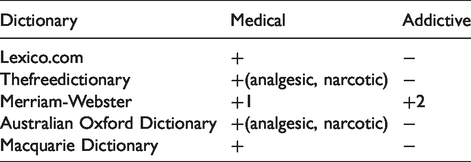
Meaning: A substance naturally derived from opium or related to it, and used medically for the relief of pain or for its soporific properties. Opiate has preserved its medical use better than
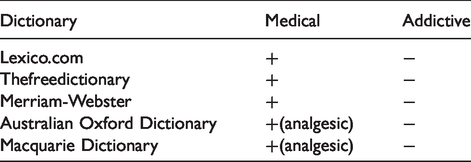
Meaning: Medicine, narcotic analgesic, but can create dependency.
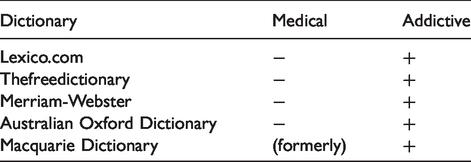
Meaning: First marketed by the German pharmaceutical company Bayer in 1895 as a non-addictive cough suppressant, and as an alternative to morphine. The name was chosen because heroin made one feel heroic (German
Meaning: A substance like opium:
These definition profiles across the five dictionaries allow us to establish a ranking of the six terms between medical and addictive definitions, bearing in mind that all six terms were originally medical in nature. In addition, it is important to remember that dictionaries are descriptive instruments. They describe current usage, though people often use dictionaries in prescriptive (what you should say and write) and proscriptive (what you should not) ways. There is an inevitable delay as dictionaries track changes in usage, and incorporate into their consolidated listings the changes that have shown themselves to be clearly established.
Opioid : lexical properties and usage
This brings us to the word
Indeed, a number of terms relating to OUD are not well understood by people outside the ranks of medical professionals.
And finally, as I have heard from a number of practising pain physicians, the word
The language of the opioid ‘epidemic’
This ‘epidemic’ status of GloWeB: 1.9 billion words, 1.8 million web pages, 340,000 websites, 20 different English-speaking countries iWeb: 10.6 billion words of web news since 2010 NOW: 12.3 billion words of journalistic English from the web.
With data sources as large as these we can be reasonably confident that skewing effects related to sample selection and distribution will be minimised. The different databases offer different analytical tools, which we use selectively for the purposes of the present analysis.
The NOW dataset, taken from web-accessible journalism, shows that the word
From 2011 to 2014
Incidence of the word opioid from 2010 to 2020.
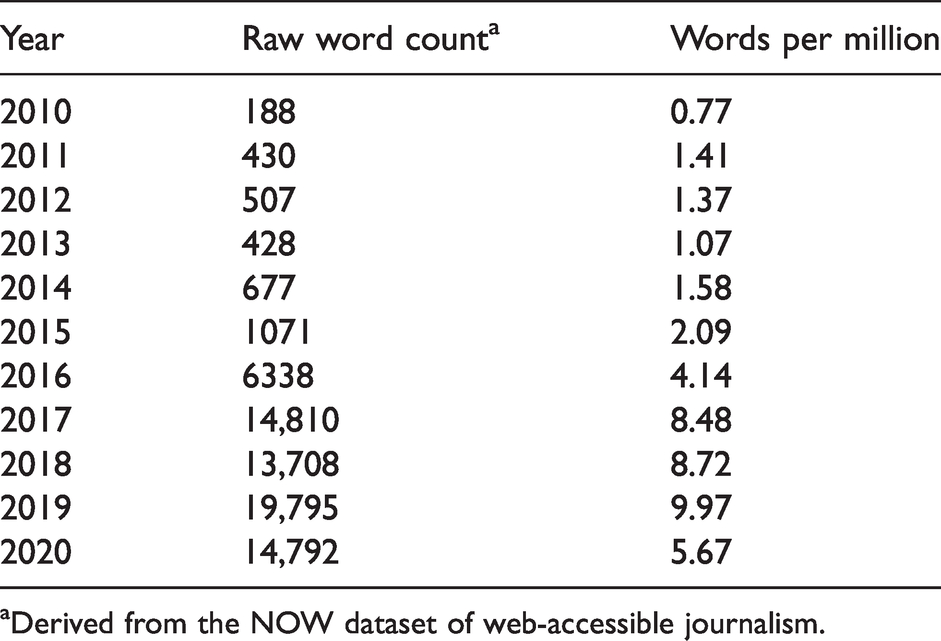
aDerived from the NOW dataset of web-accessible journalism.
Let us concentrate first on what happened up to and including 2019. It is not difficult, using key public pronouncements about
he discovered that the connections between the patients’ prefrontal lobes and their opioid systems had been damaged (Wired.com, 24 August, 2009). marketing trumped science and helped fuel the rapid increase in opioid use throughout the country (Healthnewsreview.org, 11 September, 2012). world's wealthiest country, the United States, faces an epidemic of suicide and opioid addiction – clear symptoms of rising unhappiness (newsroom.co.nz, 20 July, 2020). Although it’s rare in Canada to charge dealers with killing customers, the number of cases is increasing due to the opioid epidemic. Murder charges are much more common in the United States (https://www.cbc.ca/news/canada/london/london-ontairo-fentanyl-should-dealers-be-charged-with-manslaughter-1.5120166; 3 May, 2019). Struggling parents, domestic violence survivors, opioid users, and individuals with mental illness are hauled off to jail without treatment or assistance (https://slate.com/news-and-politics/2020/07/the-case-for-elizabeth-warren-for-vp.html, 10 July, 2020).
From 2020, however, there is a significant change:
Implications for clinical practice and public health
The word
First, if we agree that a more dispassionate tenor of discourse on opioids is desirable, it is necessary to moderate the current demonisation of opioids, while not discounting the dangerous effects of their use and misuse. This means counter-balancing the misinformation, stigma, rhetoric, rumour, taboo, shame, and embarrassment often associated with attitudes to opioids and discussions about them.
A related issue concerns placebos. There is already substantial experimental evidence of the efficacy of the placebo effect, though its actual mechanisms of operation are still being worked out. Part of the emotional domain of placebos has to do with the role of patient expectations.44 As I have argued,45 it is necessary to distinguish three kinds of placebo: Placebo1, the traditional ineffective medicine given in the hope that the patient’s belief will be therapeutically effective; Placebo2, an inert medication used in randomised trials; Placebo3, as part of caring interactions in routine clinical care.
If the placebo effect is to be allowed to work, it is necessary to address the stigma associated with opioids—in the spirit and actions of the OUD is seen not as a medical illness but as the consequence of moral weakness or willful choice; separating OUD treatment from the rest of health care can deflect the attention of the treating physician from other mental and physical conditions; language use: urine tests are ‘clean’ or ‘dirty’, as are patients; patients seeking to wind back their opioid use are described as ‘detoxifying’; people with OUD are called ‘junkies’; the criminal justice system often disallows access to methadone or buprenorphine as part of patients reducing their reliance on opioids.
These and other issues are addressed in the report of the American Medical Association’s Opioid Task Force,56,57 ‘The key to recovery is support and compassion. Patients in pain and patients with a substance use disorder need comprehensive treatment, not judgment’.56
And as Perry et al. report from a national survey58 while Americans do not consider OUD prescription disorder holders responsible for their addiction, they do subject them to social exclusion, including from jobs. And there is a washback effect from illegal or overuse patients to the clinical context, where bona fide doctors and patients are trying to achieve empathy and responsible strategies to address pain.
In this context, is it possible to talk about opioids in an objective and enabling light? First, and especially in public debate, it is necessary to modify the nexus between
Dissension in the medical profession
Establishing a more dispassionate baseline for discussion about opioids and their place in pain medicine may of itself be insufficient, as is demonstrated by a bitter recent interchange between pain physicians and patients in the professional literature.
In 2015 two pain specialists, Professor Jane Ballantyne and Dr Mark Sullivan, from the University of Washington’s School of Medicine, published a paper entitled ‘Intensity of CNCP – the wrong metric?’ in the prestigious
In their view it is therefore necessary to step back from the prescription of opioids, and look for more holistic solutions, certainly including suffering and quality of life rather than just numerical assessments of pain. They conclude that ‘For this purpose, nothing is more revealing or therapeutic than a conversation between a patient and a clinician, which allows the patient to be heard and the clinician to appreciate the patient's experiences and offer empathy, encouragement, mentorship, and hope’.59
There was an immediate and angry response from fellow pain specialists and people living with pain. Some of them even called for Ballantyne and Sullivan to be removed from their university positions, and were severely critical of their professional and ethical position as pain physicians; Ballantyne being President, and Sullivan a board member, of Physicians for Responsible Opioid Prescribing (PROP). One prominent pain physician was quoted as saying ‘To suggest that physicians should no longer treat pain intensity and let patients suffer goes beyond any sort of decency or concern for humanity’.60
This was far from being the end of what became a very public disagreement. Having professional bodies saying different things like this can only muddy the waters of discussion, and for people outside the healthcare domain, must surely be highly confusing.
PROP has advocated that opioids should not be used for long-term pain (Letter from Physicians 2021), and they attack the ‘scourge’ (their word) of the epidemic of opioids and deaths through overdoses from prescription opioids.61
The CDC has been focused more on controlling the epidemic and avoiding the overuse of opioids. Their 2016 Guideline25 included this important paragraph:
Nonpharmacologic therapy and nonopioid pharmacologic therapy are preferred for chronic pain. Clinicians should consider opioid therapy only if expected benefits for both pain and function are anticipated to outweigh risks to the patient. If opioids are used, they should be combined with nonpharmacologic therapy and nonopioid pharmacologic therapy, as appropriate.
The situation has been exacerbated by the other epidemic, actually pandemic: Covid-19. Patients have been unable to attend face-to-face consultations with their physicians to ensure continuing supplies of medications. The various regulatory bodies have scrambled to make these requirements more flexible, albeit with delays and again with opposition from PROP.
In addition, all of this has to be managed in the specific topology of medicine in the USA, with the need to synchronise federal and state governments, professional medical bodies, and insurance companies—who are reported to be less ready to go along with policy changes.
Looking back, there are some positive signs. From 2014 to 2019 opioid prescriptions fell by 37.1% in the USA.57 The American Medical Association’s Roadmap reports that from 2015 to 2019 deaths from the misuse of prescription opioids in the USA actually fell slightly, from 12,269 to 11,973. But deaths from the misuse of illegally acquired drugs were ominously gathering pace: fentanyl and derivatives (5,766 rising to 36,705), stimulants like methamphetamines (4,402 to 16,353), cocaine (5,486 to 16,055), and heroin (10,788 to 14,151). The media continue to write about the opioid ‘epidemic’, which is useful as a scare word, but without always separating prescription opioids from illegal opioids. The tone is confrontational, sometimes alarmist. For example, Yerby62 states, This catastrophe has unleashed death and misery across the country for over two decades, yet only recently have policymakers and the public begun to devote attention and greater resources to the problem. Opioid addiction is a terrible and life-threatening burden, one which no one chooses to bear.
Ultimately the common difficulty is the continuing lack of non-addictive pain medications, especially for CNCP. There are some early hopeful indications from EPPIC-Net, the Early Phase Pain Intervention Clinical Network.63 But these medications may take years to reach the market, unless they are propelled by the kind of shared purpose and urgency that accompanied the development of Coronavirus vaccines. That was one area where, at least in terms of the science, there was substantial consensus and sensible reporting. In contrast, the following health policies were mainly disasters of messaging, in different ways in different countries. If ‘disasters’ is apocalyptic, it is also arguably true. And it may well be what is needed to energise public discussion.
Conclusion
Opioids have different roles for different medical conditions. For the short-term relief of severe acute pain, for cancer pain, and for end-of-life pain, opioids administered under close medical supervision have a long and recognised role. Opioids are more controversial for other kinds of pain, especially CNCP. But opioids can unfortunately be misused in pain treatment by healthcare professionals and by patients, and misuse can shift to abuse. And in the domain of recreational drugs, opioid use can become opioid abuse. This has been picked up by a strong public and journalistic pushback against opioids in general over the last decade.
In current usage and in text databases the word
Footnotes
Author Contribution(s)
Acknowledgements
I warmly acknowledge critical contributions and advice from Meredith Craigie, Susan Evans, Damien Finniss, Laura Hamilton, Helen Keates, Geoffrey Mitchell, Frank New, Graham Rice and Joanna Sussex.
Declaration of Conflicting Interests
The author declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author received no financial support for the research, authorship, and/or publication of this article.
